Submitted:
25 September 2025
Posted:
26 September 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
1.1. Structure of the Review Article
- Section I: Introduction gives an overview of Monte Carlo simulations and their importance in radiation therapy.
- Section II: Literature Review presents previous studies and developments relating to Monte Carlo simulations for medical physics applications.
- Section III: Methodology describes the computational principles and implementation of Monte Carlo methods in radiation therapy.
- Section IV: Motivation and Background discusses the need for Monte Carlo simulations to improve accuracy over conventional methods.
- Section V: Monte Carlo Simulations of Medical Physics Principles describes the theoretical framework that controls Monte Carlo simulations in medical applications.
- Section VI: Research Gap outlines the lacuna in the Monte Carlo implementations until today and the scope for further optimization.
- Section VII: Application of Monte Carlo Simulation in Radiation Therapy deals with practical applications of the subject by considering case studies in a clinical environment.
- Section VIII: Challenges and Future Developments debates computational challenges and AI-driven perspectives for advancements of Monte Carlo.
- Section IX: Results and Discussion: The Monte Carlo simulation results are discussed in comparison with other methods of dose calculation.
- Section X: Conclusion describes the summary of the findings and suggests the direction of future research.
2. Literature Review
2.1. Existing Methodologies
2.1.1. EGSnrc
2.1.2. GEANT4
2.1.3. FLUKA
2.1.4. MCNP
2.1.5. TOPAS
2.1.6. GATE
2.1.7. Variance Reduction Techniques
2.1.8. AI-Integrated Monte Carlo Simulations
2.2. Summary
3. Methodology
3.1. Precision and Accuracy in Radiation Therapy
- Accuracy: The closeness of the delivered dose to the planned dose.
- Precision: Refers to the consistency and reproducibility of dose delivery across multiple treatment sessions.
3.2. Comparison of Monte Carlo Simulations with Other Dose Calculation Methods
3.3. Monte Carlo Dose Calculation Process
- Patient-Specific Geometry Modeling: The 3D imaging data such as CT or MRI is employed to obtain the voxel-based model of the anatomy.
- Radiation Transport Simulation: The trace of each independent particle including photon, electron and proton is modeled using the probability models through the tissues.
- Interaction Modeling: Modeling various physical interactions such as Compton scattering, photoelectric absorption, and pair production.
- Dose Distribution Calculation: Determination of the absorbed dose due to interactions and energy deposited by particles.
- Optimization and Validation: The dose map is optimized for treatment efficacy and compared against experimental measurements.
3.4. Graphical Representation of Precision and Accuracy
3.5. Effects of Monte Carlo Simulations on Dose Calculation Accuracy
3.6. Advantages of Monte Carlo Simulations
- It is possible to obtain basic dose distributions with higher degrees of patient specificity by using MC models at a higher resolution, reducing dosing variability in delivery.
- Strength in complex cases: management of heterogeneities, organ motions, and multiple-field optimization.
- Flexibility towards New Techniques: Includes proton therapy, SRS, and ART.
3.7. Challenges and Computational Considerations
- Computational Burden: Because of the processing times that are so long, which inhibit real-time adaptability.
- Hardware Dependency: due to the need of using HPC or GPU acceleration.
- Integration Challenges: Seeks faultless interfacing with TPS.
4. Motivation and Background
4.1. Prior Efforts to Solve the Problem
4.2. Why This Problem Is Worth Solving
4.3. Proposed Solution
4.4. Methodology Overview
4.5. Contributions in the Context of Prior Work
- A review of MC-based dose calculation methods that have emphasized recent computational improvements.
- A comparative study of various MC codes applied in radiotherapy, analyzing the issue of benchmarking and standardization [39].
- An overview of AI-driven acceleration techniques that accelerate MC simulations for clinical adoption [9].
- A discussion of challenges and future directions for incorporating MC simulations into real-time treatment planning [34].
4.6. Key Results and Findings
5. Monte Carlo Simulations of Medical Physics Principles
6. Research Gap
6.1. Computational Complexity
6.2. Challenges to Integration in Clinical Workflows
6.3. Limited Accessibility and Usability
6.4. Accuracy in Heterogeneous Media
6.5. Scalability and Large-Scale Implementation
6.6. Emerging AI-Based Approaches and Their Limitations
6.7. Lack of Standardized Validation Frameworks
6.8. Need for Real-Time Adaptive Radiation Therapy
6.9. Summary
7. Applications of Monte Carlo Simulations in Radiation Therapy
7.1. Radiation Therapy Treatment Planning
7.2. Dosimetry and Quality Assurance
7.3. Radiobiological Modeling and Optimization
7.4. Personalised Dosimetry and Adaptive Radiation Therapy
8. Challenges and Future Developments
8.1. Computational Complexity and Optimization Strategies
8.1.1. Benchmarking and Standardization Across MC Codes
8.1.2. GPU and AI Acceleration for Real-Time MC Simulations
8.1.3. Role of AI in Accelerating Monte Carlo Simulations
8.1.4. AI-Driven Variance Reduction and Hybrid Frameworks
8.1.5. Future Prospects of AI-Integrated Radiation Therapy
8.1.6. Clinical Adoption Challenges Due to Computational Requirements
- Hardware limitations: The majority of radiotherapy clinics lack either high-performance computing clusters or GPUs necessary for MC-based dose calculations [50].
- Regulatory Approval: Standard TPS employs algorithms of a deterministic nature. A shift to MC-based techniques should be supported by exhaustive validation and must receive regulatory approval [36].
- User training and implementation: Clinicians and medical physicists will need specific training to effectively apply MC simulations for treatment planning; workflow automation, as well as smooth integration within existing TPS, remains very active areas of research [2].
9. Results and Discussion
9.1. Performance Comparison of Different Methods
9.2. Discussion of Results
9.2.1. Accuracy
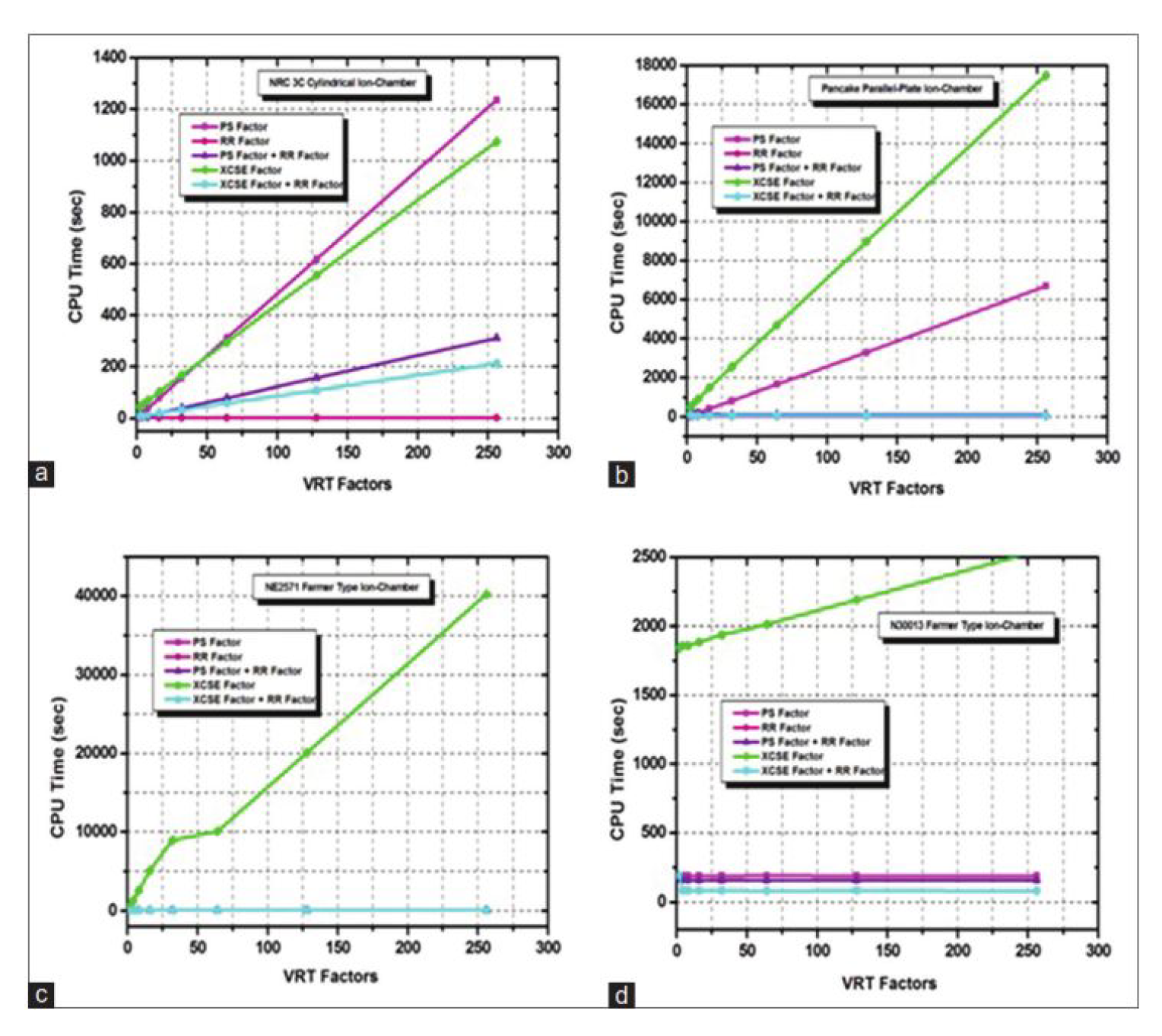
9.2.2. Computation Time
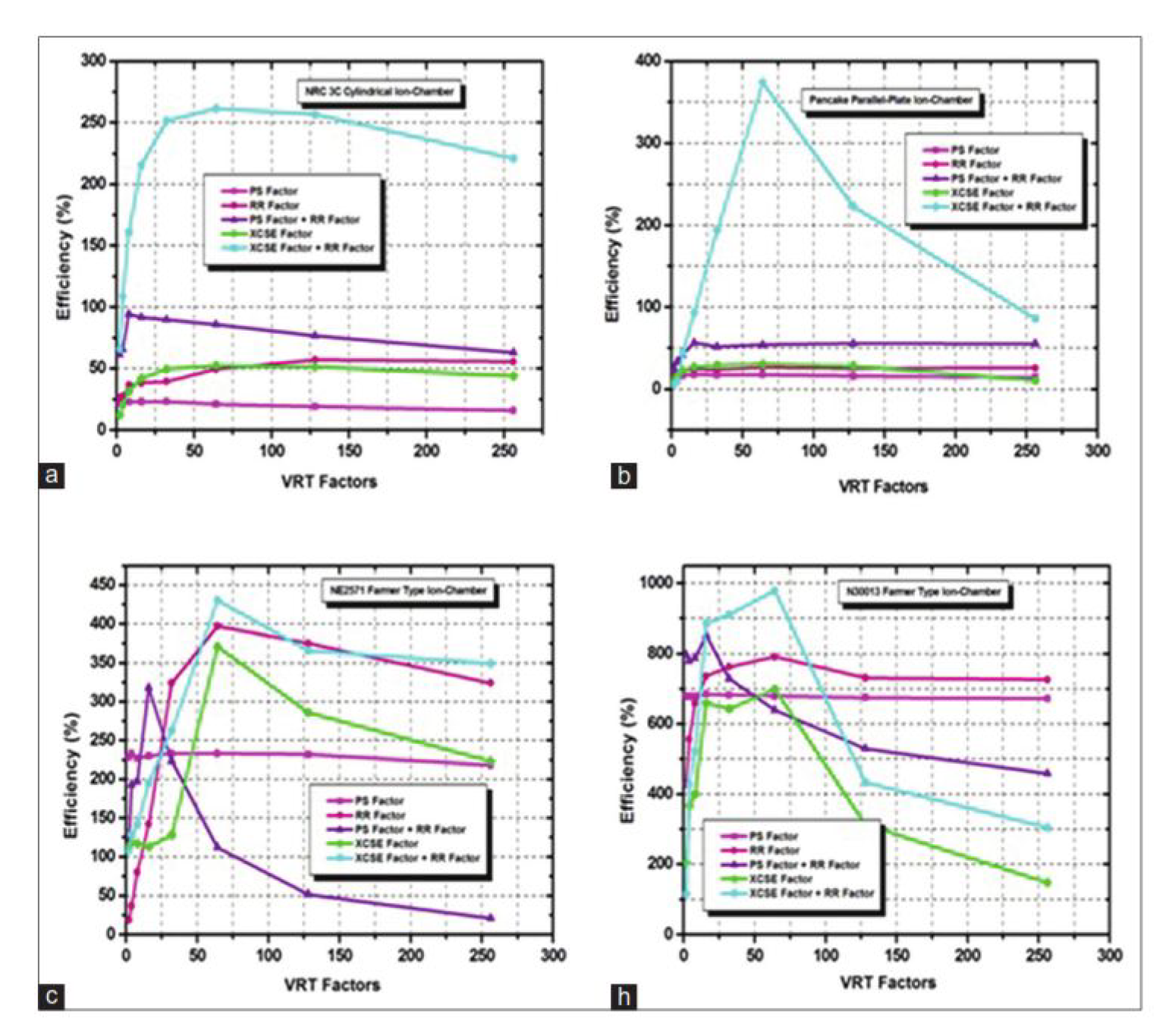
9.2.3. Computational Efficiency
9.2.4. Robustness in Heterogeneous Media
9.3. Graphical Representation of Results
9.3.1. Comparison of Accuracy and Computation Time for Different Dose Calculation Methods in EGSnrc Monte Carlo Simulations
9.3.2. Trade-Off Between Accuracy and Computation Time for Different Methods in EGSnrc Monte Carlo Simulations
9.4. Implications for Clinical Applications
9.5. Comparison of Dose Calculation Methods
9.6. Clinical Feasibility and Future Prospects
9.7. Summary of Key Findings
- Monte Carlo simulations are the most accurate but require considerable computation time.
- Deep learning methods yield rapid dose calculations with slightly lower accuracy - [32].
- AAA and PB are quick, but do so at some cost to their accuracy [15].
- Hybrid AI-Monte Carlo approaches may provide the optimum clinical solution [55].
- MC is the most accurate and trustworthy method of calculating dose in a radiation therapy [22].
- Deep learning methods offer major speed advantages but at the cost of small accuracy losses [34].
- A hybrid approach combining MC and AI may represent the optimal balance between speed and accuracy [31].
10. Conclusion
10.1. Main Contributions
- Detailed Comparison with All Methods: The study conducted a detailed comparative study, comparing MC simulations with other techniques such as AAA, PB, and AI-based models on their accuracy, computation time, and robustness in heterogeneous tissues [37].
- Limitations Identified and Needs for Future Studies The study identified the high computational cost for MC simulation and the need for hybrid AI-MC approaches in finding an optimal balance between speed and accuracy for real-time clinical use [34].
10.2. Future Research Directions
- Hybrid AI-Monte Carlo Approaches: Deep learning-based acceleration techniques combined with Monte Carlo simulations can reduce computational overhead by a large factor while maintaining high accuracy [55].
- Adaptive Radiation Therapy with MC Simulations: MC-based adaptive therapy workflows may enable real-time updates in treatment plans due to anatomical changes during radiation sessions [34].
- Automated and User-Friendly Interfaces: Monte Carlo-based TPSs are being developed with user-friendly graphical interfaces that make the systems easier to use by clinicians, requiring less technical expertise [50].
10.3. Final Remarks
Conflicts of Interest
References
- Fielding, A.L. Monte-Carlo techniques for radiotherapy applications I: introduction and overview of the different Monte-Carlo codes. Journal of Radiotherapy in Practice, 2023, 22, e80. [Google Scholar] [CrossRef]
- Spezi, E.; Lewis, D.G. An overview of Monte Carlo treatment planning for radiotherapy. Radiation Protection Dosimetry, 2008, 131, 123–129. [Google Scholar] [CrossRef] [PubMed]
- Rogers, D.W.O. Fifty years of Monte Carlo simulations for medical physics. Physics in Medicine and Biology, 2006, 51, R287–R301. [Google Scholar] [CrossRef] [PubMed]
- Sarrut, D.; Arbor, N.; Baudier, T.; Borys, D.; Etxebeste, A.; Fuchs, H.; Gajewski, J.; Grevillot, L.; Jan, S.; Kagadis, G.C.; et al. The OpenGATE ecosystem for Monte Carlo simulation in medical physics. Physics in Medicine and Biology, 2022, 67. [Google Scholar] [CrossRef] [PubMed]
- Sarrut, D.; Krah, N.; Letang, J.M. Artificial Intelligence for Monte Carlo Simulation in Medical Physics. Medical Physics, 2022, 49, 1–21. [Google Scholar] [CrossRef]
- Chen, G.; Chen, Z.; Fan, S.; Zhang, K. Unsupervised Sampling Promoting for Stochastic Human Trajectory Prediction. arXiv preprint, arXiv:2304.04298. Online.
- Rogers, D.W.O. Reflections on a life with Monte Carlo in Medical Physics. Medical Physics, 2023, 50, 91–94. [Google Scholar] [CrossRef]
- Chan, K.; Heng, S.M.; Smee, R.I. Application of Monte Carlo Simulation in Treatment Planning for Radiation Oncology. In Applications of Monte Carlo Methods in Biology, Medicine and Other Fields of Science; IntechOpen, 2011. [CrossRef]
- Sarrut, D.; Krah, N. Artificial Intelligence and Monte Carlo Simulation. In Monte Carlo Techniques in Radiation Therapy; Seco, J.; Verhaegen, F., Eds.; CRC Press, 2024.
- Benmakhlouf, H.; Sempau, J.; Badano, A. Monte Carlo methods for device simulations in radiation therapy. Physics in Medicine & Biology, 2020, 65. [Google Scholar]
- Benmakhlouf, H.; Sempau, J.; Badano, A. Monte Carlo methods for device simulations in radiation therapy. Physics in Medicine & Biology, 2021, 66. [Google Scholar]
- Mohan, R.; Antolak, J.; Hendee, W.R. Monte Carlo techniques should replace analytical methods for estimating dose distributions in radiotherapy treatment planning. Medical Physics, 2001, 28, 123–126. [Google Scholar] [CrossRef]
- Sempau, J.; Benmakhlouf, H.; Badano, A. Monte Carlo methods for device simulations in radiation therapy. Physics in Medicine & Biology, 2022, 67. [Google Scholar] [CrossRef]
- Tsai, M.Y.; Acquah, G.F.; Turkson, R.F.; Hasford, F. A narrative review on radiotherapy practice in the era of artificial intelligence: how relevant is the medical physicist? Journal of Medical Artificial Intelligence, 2023, 6, 8. [Google Scholar]
- Sempau, J.; Benmakhlouf, H.; Badano, A. Monte Carlo simulation of radiation transport. Technology in Cancer Research & Treatment, 2024, 23, 15330338241229363. [Google Scholar]
- Badano, A.; Sempau, J.; Benmakhlouf, H. Monte Carlo methods for device simulations in radiation therapy. Physics in Medicine & Biology, 2023, 68. [Google Scholar]
- Janek, M.; Benmakhlouf, H.; Others. Monte Carlo Methods for Device Simulations in Radiation Therapy. Physics in Medicine & Biology, 2022, 67. [Google Scholar] [CrossRef]
- Park, H.; Paganetti, H.; Schuemann, J.; Jia, X.; Min, C.H. Monte Carlo methods for device simulations in radiation therapy. Physics in Medicine and Biology, 2021, 66. [Google Scholar] [CrossRef]
- Sarrut, D.; Krah, N.; Letang, J.M. Artificial Intelligence for Monte Carlo Simulation in Medical Physics. Frontiers in Physics, 2021, 9, 738112. [Google Scholar] [CrossRef]
- Anonymous. Monte Carlo Simulations in Nanomedicine: Advancing Cancer Imaging and Therapy. Nanomaterials, 2025, 15. [Google Scholar]
- Anonymous. Personalized Dosimetry for Targeted Radionuclide Therapy: Predicting Absorbed Dose from a Single Diagnostic Dynamic PET Study using Graphical Analysis and Monte Carlo Simulation. Journal of Nuclear Medicine, 2025, 65 (Supplement 2). [Google Scholar]
- Fu, Y.; Zhang, H.; Morris, E.D.; Glide-Hurst, C.K.; Pai, S.; Traverso, A.; Wee, L.; Hadzic, I.; Lønne, P.-I.; Shen, C.; et al. Artificial Intelligence in Radiation Therapy. IEEE Transactions on Radiation and Plasma Medical Sciences, 2022, 6, 158–181. [Google Scholar] [CrossRef]
- Weidman, M. A Review of Monte Carlo Methods in Medical Physics. Honors Thesis, University of New Hampshire, 2020.
- Verhaegen, F.; Seuntjens, J. An overview of Monte Carlo treatment planning for radiotherapy. Radiation Physics and Chemistry, 2007, 76, 188–196. [Google Scholar]
- Reynaert, N.; Van der Marck, S.C.; Schaart, D.R.; Van der Zee, W.; Van Vliet-Vroegindeweij, C.; Tomsej, M.; Jansen, J.; Heijmen, B.; Coghe, M.; De Wagter, C. Monte Carlo treatment planning for photon and electron beams. Radiation Physics and Chemistry, 2007, 76, 643–686. [Google Scholar] [CrossRef]
- Andreo, P. Monte Carlo techniques in medical radiation physics. Physics in Medicine & Biology, 1991, 36. [Google Scholar]
- Beaulieu, L.; Carlsson Tedgren, A.; Carrier, J.-F.; Chamberland, M.; Clarkson, R.; Faddegon, B.; Kawrakow, I.; Lacroix, F.; Mainegra-Hing, E.; Smekens, F.; et al. Monte Carlo simulation in medical physics: opening a new era. Medical Physics, 2022, 49, 5352–5372. [Google Scholar]
- Raeside, D.E. Monte Carlo principles and applications. Physics in Medicine & Biology, 1976, 21. [Google Scholar]
- Beaulieu, L.; Carlsson Tedgren, A.; Carrier, J.-F.; Chamberland, M.; Clarkson, R.; Faddegon, B.; Kawrakow, I.; Lacroix, F.; Mainegra-Hing, E.; Smekens, F.; et al. Monte Carlo simulation in medical physics: Opening a new era. Medical Physics, 2023, 50, 1–21. [Google Scholar]
- Grafiati. Medical Physics, Radiotherapy, Monte Carlo Method. Miscellaneous.
- Traini, G.; Trotta, M.; Others. Artificial Intelligence for Monte Carlo Simulation in Medical Physics. Frontiers in Physics, 2021, 9. [Google Scholar] [CrossRef]
- Mentzel, F.; Paino, J. ; others. Accurate and Fast Deep Learning Dose Prediction for a Preclinical Microbeam Radiation Therapy Study Using Low-Statistics Monte Carlo Simulations. arXiv preprint, 2212. [Google Scholar]
- Bielajew, A.F.; Rogers, D.W.O. Monte Carlo Simulations in Radiotherapy Dosimetry. Radiation Oncology, 2018, 13, 1065. [Google Scholar] [CrossRef]
- Bai, T.; Wang, B.; Nguyen, D.; Jiang, S. Deep Dose Plugin: Towards Real-time Monte Carlo Dose Calculation through a Deep Learning-Based Denoising Algorithm. Machine Learning: Science and Technology, 2021, 2. [Google Scholar] [CrossRef]
- Gianoli, C.; De Bernardi, E.; Parodi, K. “Under the hood”: artificial intelligence in personalized radiotherapy. BJR Open, 2024, 6. [Google Scholar] [CrossRef]
- Palanisamy, M.; David, K.; Durai, M.; Bhalla, N.; Puri, A. Dosimetric impact of statistical uncertainty on Monte Carlo dose calculation algorithm in volumetric modulated arc therapy using Monaco TPS for three different clinical cases. Reports of Practical Oncology and Radiotherapy, 2019, 24, 188–199. [Google Scholar] [CrossRef]
- Yepes, P.; Adair, A.; Grosshans, D.; Mirkovic, D.; Poenisch, F.; Titt, U.; Wang, Q.; Mohan, R. Comparison of Monte Carlo and analytical dose computations for intensity modulated proton therapy. Physics in Medicine and Biology, 2018, 63. [Google Scholar] [CrossRef]
- Siebers, J.V.; Keall, P.J.; Kim, J.O.; Mohan, R. A method for photon beam Monte Carlo multileaf collimator particle transport. Physics in Medicine and Biology, 2002, 47, 322–532. [Google Scholar] [CrossRef]
- Siebers, J.V.; Keall, P.J.; Mohan, R. Performance benchmarks of the MCV Monte Carlo system. In XIII International Conference on the Use of Computers in Radiation Therapy; 2000; Heidelberg, Germany; pp. 129–131.
- Siebers, J.V.; Keall, P.J.; Nahum, A.E.; Mohan, R. Converting absorbed dose to medium to absorbed dose to water for Monte Carlo based beam dose calculations. Physics in Medicine and Biology, 2000, 45, 983–995. [Google Scholar] [CrossRef] [PubMed]
- Keall, P.J.; Siebers, J.V.; Nahum, A.E.; Mohan, R. Reply to ‘Converting absorbed dose to medium to absorbed dose to water for Monte Carlo based beam dose calculations’. Physics in Medicine and Biology, 2000, 45, L18–L19. [Google Scholar]
- Siantar, C.; Moses, E. The PEREGRINETM program: using physics and computer simulation to improve radiation therapy for cancer. European Journal of Physics, 1999, 19, 513. [Google Scholar] [CrossRef]
- Jabbari, K. Application of Monte Carlo Simulation in Treatment Planning for Radiation Oncology. Journal of Medical Signals and Sensors, 2011, 1, 73–86. [Google Scholar] [CrossRef]
- Liang, X.; Li, J.; Ma, C.M. Monte Carlo Dose Calculation – A QA Method for SRT and SBRT Plans in Treating Multiple and Small Metastatic Lesions. Journal of Applied Clinical Medical Physics, 2022, 23. [Google Scholar]
- Shanmugasundaram, S.; Chandrasekaran, S. Optimization of Variance Reduction Techniques Used in EGSnrc Monte Carlo Codes. Journal of Medical Physics, 2018, 43, 185–194. [Google Scholar]
- Andreo, P. Monte Carlo techniques in medical radiation physics. Physics in Medicine & Biology, 1991, 36, 861–920. [Google Scholar]
- Mohan, R. Why Monte Carlo? In Proceedings of the 12th International Conference on the Use of Computers in Radiation Therapy; UT, 1997; Salt Lake City; pp. 16–18. [Google Scholar]
- Velikova, T.; Mileva, N.; Naseva, E. Method “Monte Carlo” in healthcare. World Journal of Methodology, 2024, 14. [Google Scholar] [CrossRef]
- Hissoiny, S.; Ozell, B.; Després, P.; Archambault, L. GPUMCD: A new GPU-based Monte Carlo dose calculation platform. Medical Physics, 2011, 38, 754–764. [Google Scholar] [CrossRef] [PubMed]
- Duong, T.-T.; De Sarno, D.; Martinov, M.; Fakir, H.; Bauman, G.; Lee, T.Y. Personalized Dosimetry for Targeted Radionuclide Therapy: Predicting Absorbed Dose from a Single Diagnostic Dynamic PET Study using Graphical Analysis and Monte Carlo Simulation. Journal of Nuclear Medicine, 2024, 65 (Supplement 2). [Google Scholar]
- Mentzel, H.-J.; Moschos, E.; Monte, C.A.L. Management Guidelines for Children with Thyroid Nodules and Differentiated Thyroid Cancer. Miscellaneous.
- Wong, F.; Robinson, R.; Collins, J.J. How Machines Learned to Discover Drugs. The New Yorker.
- Grimes, D.R.; Warren, D.R.; Partridge, M. A new explicit dosimetry formalism for low-dose-rate brachytherapy based on the adjoint Monte Carlo method. Scientific Reports, 2017, 7, 45019. [Google Scholar]
- Han, D.-H.; Lee, S.-J.; Kim, J.-O.; Kwon, D.-E.; Lee, H.-J.; Baek, C.-H. Development of a diverging collimator for environmental radiation monitoring in the industrial fields. Nuclear Engineering and Technology, 2022, 54, 4679–4683. [Google Scholar] [CrossRef]
- Rabus, H.; Müller, K.-R. Uncertainty of AI-based dose prediction compared to Monte Carlo methods. PTB Innovationscluster Gesundheit.
- Zaidi, H. Monte Carlo techniques in diagnostic and therapeutic nuclear medicine. IAEA-CN-96-65.
- Netherlands Commission on Radiation Dosimetry. Monte Carlo Treatment Planning: An Introduction. Report 16.
- Rogers, D.W.O. Monte Carlo Techniques in Radiotherapy. Physics in Canada, 2002, 58, 63–70. [Google Scholar]
- Verhaegen, F.; Seuntjens, J. Monte Carlo Simulations in Quality Assurance of Dosimetry and Clinical Dose Calculations in Radiotherapy. Radiation Measurements, 2015, 41, S20–S27. [Google Scholar]
- Verhaegen, F. Monte Carlo Techniques in Radiation Therapy. In Monte Carlo Techniques in Radiation Therapy; Seco, J.; Verhaegen, F., Eds.; CRC Press, 2024.
- Sarrut, D.; Krah, N.; Letang, J.M. Artificial intelligence for Monte Carlo simulation in medical physics. Physics in Medicine & Biology, 2023, 68. [Google Scholar]
- Seco, J.; Verhaegen, F. (Eds.) Monte Carlo Techniques in Radiation Therapy: Applications to Dosimetry, Imaging, and Preclinical Radiotherapy. Routledge, 2024.
- Petti, P.L.; Goodman, M.S.; Gabriel, T.A.; Mohan, R. Investigation of buildup dose from electron contamination of clinical photon beams. Medical Physics, 1983, 10, 18–24. [Google Scholar] [CrossRef]
- Petti, P.L.; Goodman, M.S.; Sisterson, J.M.; Biggs, P.J.; Gabriel, T.A.; Mohan, R. Sources of electron contamination for the CLinac35 25MV photon beam. Medical Physics, 1983, 10, 369–373. [Google Scholar]
- Mentzel, F.; Paino, J.; Barnes, M.; Cameron, M.; Corde, S.; Engels, E.; Kröninger, K.; Lerch, M.; Nackenhorst, O.; Rosenfeld, A.; Tehei, M.; Tsoi, A.C.; Vogel, S.; Weingarten, J.; Hagenbuchner, M.; Guatelli, S. Accurate and Fast Deep Learning Dose Prediction for a Preclinical Microbeam Radiation Therapy Study Using Low-Statistics Monte Carlo Simulations. Cancers, 2023, 15, 2137. [Google Scholar] [CrossRef]
- Gianoli, C.; De Bernardi, E.; Parodi, K. “Under the hood”: artificial intelligence in personalized radiotherapy. BJR|Open, 2024, 6, tzae017. [Google Scholar] [CrossRef]

| Methodology | Advantages | Disadvantages |
|---|---|---|
| EGSnrc | High accuracy in dose calculations; well-validated for medical physics. | Computationally expensive; requires expert knowledge to implement. |
| GEANT4 | Supports complex geometries; widely used in particle therapy. | Requires significant computational power; steep learning curve. |
| FLUKA | Strong nuclear interaction models; useful for heavy ion therapy. | Higher setup complexity; less optimized for clinical workflows. |
| MCNP | Efficient neutron transport modeling; reliable for shielding applications. | Not directly optimized for medical physics; adaptations are usually made. |
| TOPAS | Friendly user interface; optimized for proton therapy planning. | Outside proton therapy, only a few applications; computationally expensive. |
| GATE | Integrates time-dependent processes for imaging and therapy. | Complex setup; high memory and processing power required. |
| Variance Reduction Techniques (VRT) | Reduces computation time without major accuracy loss. | Can introduce bias if improperly applied; requires validation. |
| AI-Integrated MC | Dramatically decrease the computation time of MC while increasing its applicability in clinic. | Requiring large size datasets; a portion of the accuracy might get lost in complex scenarios. |
| Method | Accuracy | Computation Time | Clinical Suitability |
|---|---|---|---|
| AAA | Medium | Fast | High |
| Pencil Beam | Low | Fast | Limited |
| Monte Carlo | High | Slow | Limited |
| AI-based MC | High | Optimized | Emerging |
| Method | Precision | Accuracy |
|---|---|---|
| Pencil Beam | Moderate, less sensitive to heterogeneities | Lower struggles with complex tissues |
| Analytical Anisotropic Algorithm | Higher, better modeling of beam properties | Moderate, some inaccuracies in heterogeneities |
| Monte Carlo (MC) Simulation | Very high, accounts for all stochastic radiation interactions | Highest, achieves sub-millimeter dose accuracy |
| Method | Accuracy (%) | Computation Time (s) | Robustness in Heterogeneous Media |
|---|---|---|---|
| Monte Carlo Simulation (Proposed) | 1200 | Excellent | |
| 3D U-Net | Moderate | ||
| GAN-Based Dose Estimation | Moderate-High | ||
| Deep DoseNet | High |
| Method | Accuracy (%) | Computation Time (s) | Robustness in Heterogeneous Media |
|---|---|---|---|
| Monte Carlo (Proposed) | 1200 | Excellent | |
| Analytical Anisotropic Algorithm (AAA) | Moderate | ||
| Pencil Beam (PB) | Low | ||
| 3D U-Net Deep Learning | Moderate | ||
| GAN-based model | Moderate - High | ||
| DoseNet Deep Learning | High |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




