Submitted:
19 September 2025
Posted:
30 September 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Symptom Domains Relative to PEM
2.1. Similarities
2.2. Separate Amplification Patterns Relative to PEM
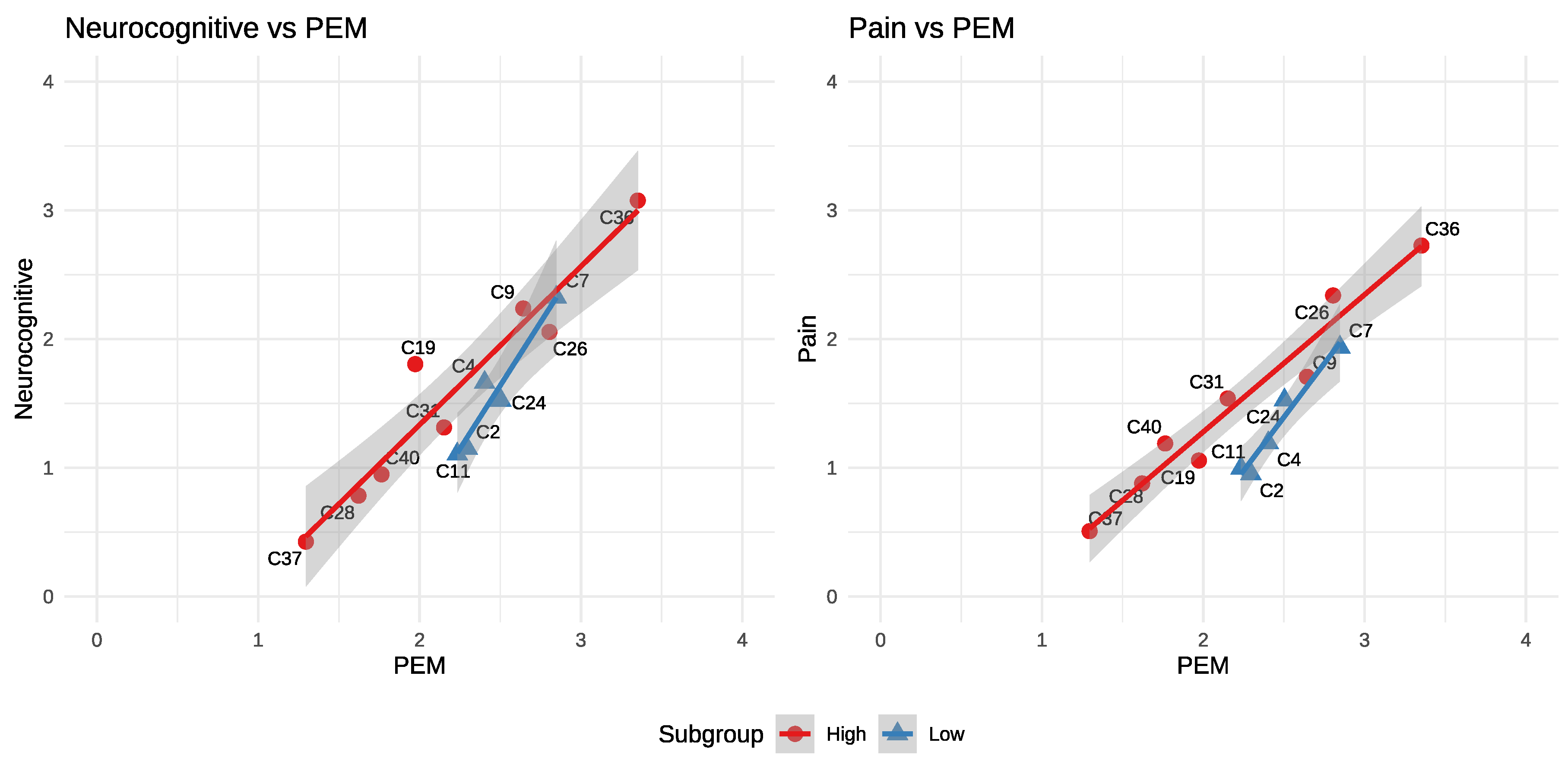
2.3. Weak Correlations Relative to PEM
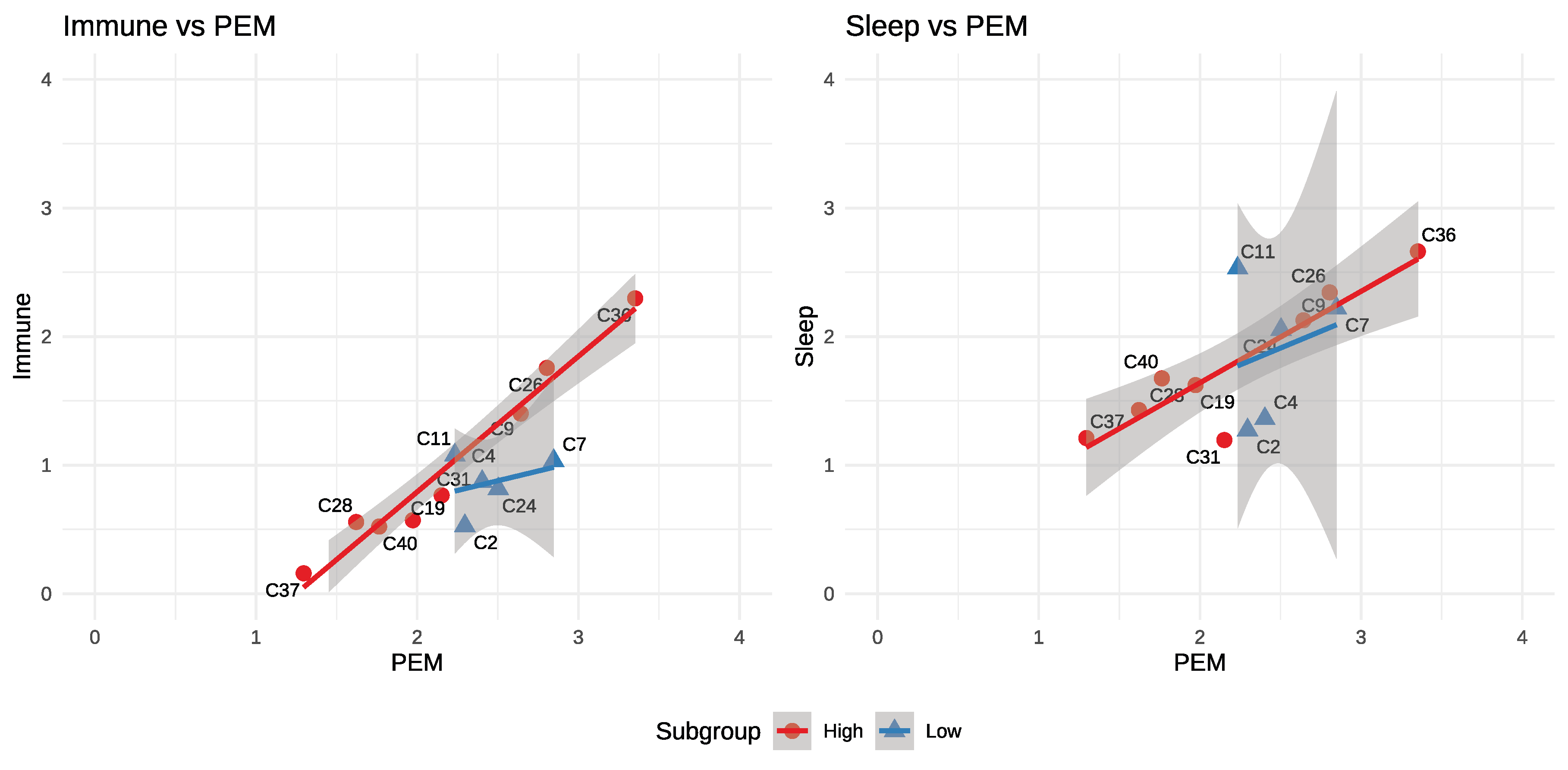
2.4. Summary of Differences
| Feature | High group | Low group |
|---|---|---|
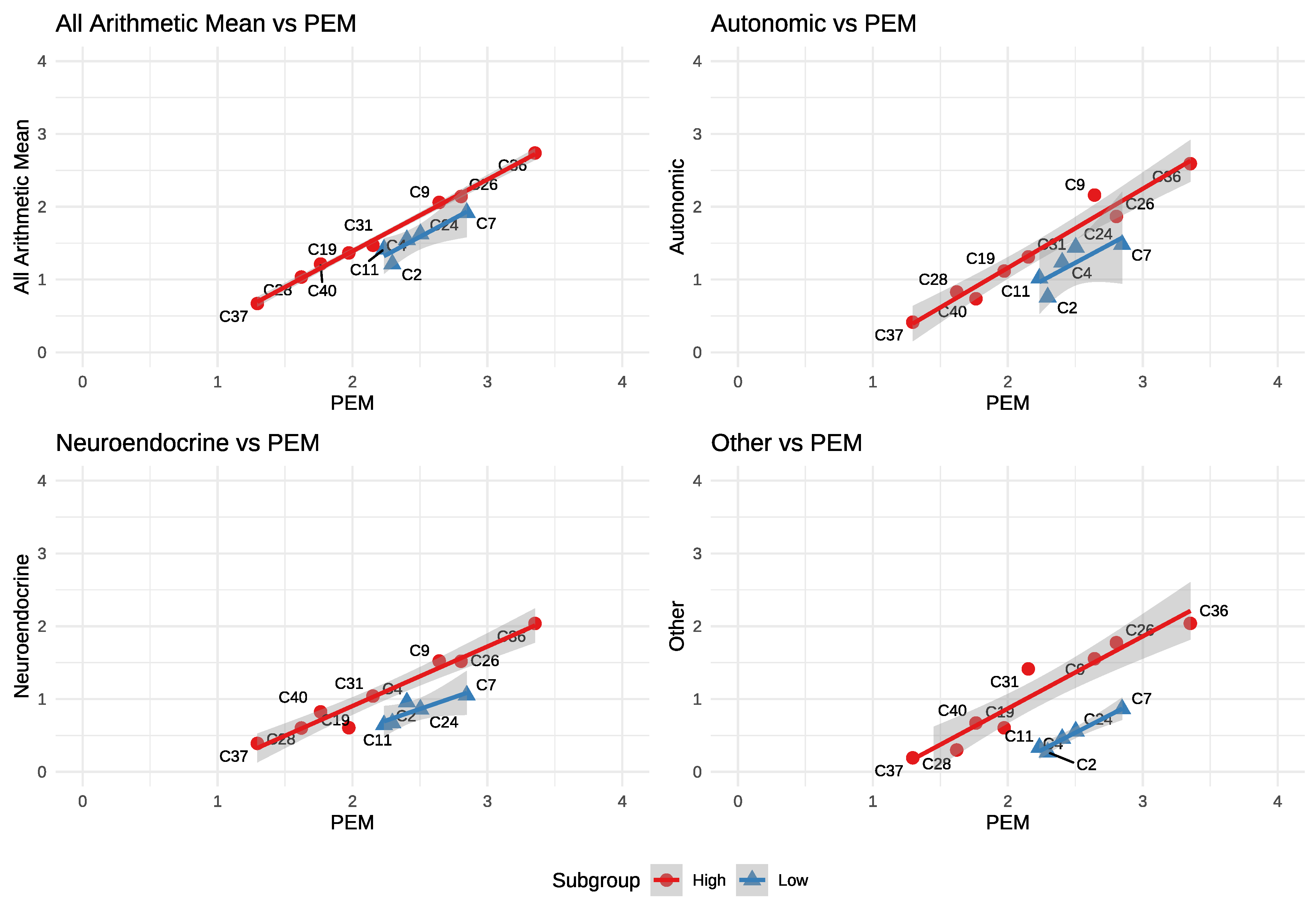
| Overall vs. PEM | Higher | Lower - esp. “Other” |
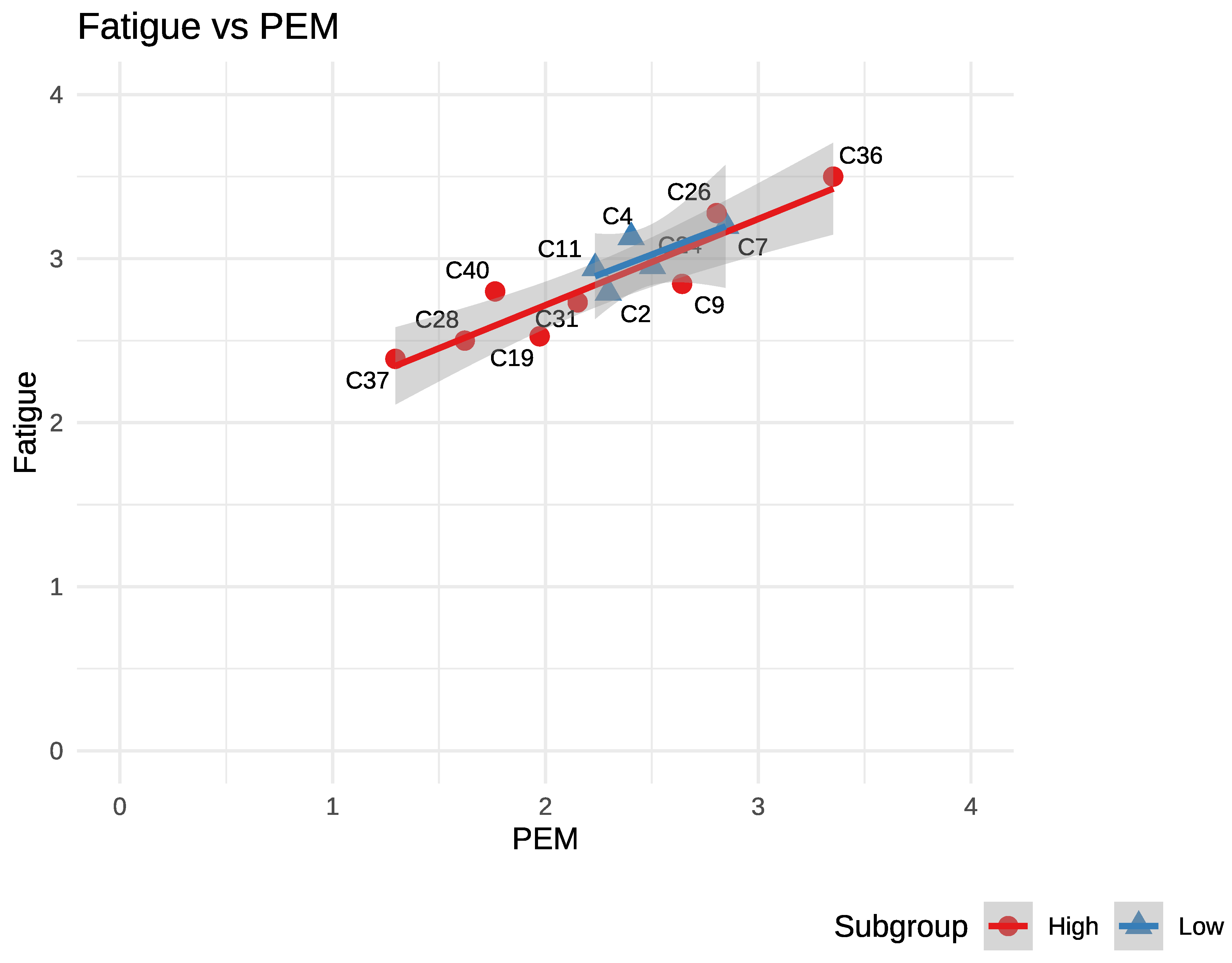
| Fatigue | R2 - 0.86 | Weaker R2 - 0.54 |
| PEM range | – 3.4 | Narrower – 2.9 |
| Neurocognitive | Tracks PEM | Elevated amplification |
| Pain | Tracks PEM | Elevated amplification |
| Immune | Tracks PEM | Flat at |
| Sleep | Tracks PEM | – 2.5, but uncorrelated |
3. Exploring the Low-intensity Subgroup
Almost 90% of the participants fulfilled the Fukuda case definition, compared to 80%, 59% and 39% fulfilling the IOM, CCC and ME-ICC case definitions, respectively. More than a quarter of the participants met the criteria for all four different case definitions, whilst 5% of the participants met none of the abovementioned case definitions,…
4. Characteristics of the Smallest Clusters
5. Discussion
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A. Cluster Summary Data
- Group each cluster by symptom domain and calculate geometric means for each symptom domain within each cluster.
- Rotate the table
- Add a new column, “all_mean” which is the arithmetic mean of all symptoms within each cluster.
- Save this file as cluster_grouped_tidy.csv
| Cluster | All | PEM | Fatigue | Auto | Immune | NC | NE | Pain | Other |
|---|---|---|---|---|---|---|---|---|---|
| C2 | 1.21 | 2.30 | 2.79 | 0.76 | 0.53 | 1.15 | 0.67 | 0.95 | 0.27 |
| C4 | 1.55 | 2.40 | 3.13 | 1.24 | 0.87 | 1.66 | 0.96 | 1.19 | 0.46 |
| C7 | 1.92 | 2.85 | 3.20 | 1.48 | 1.03 | 2.32 | 1.05 | 1.94 | 0.86 |
| C9 | 2.06 | 2.64 | 2.85 | 2.16 | 1.40 | 2.24 | 1.52 | 1.71 | 1.55 |
| C11 | 1.42 | 2.23 | 2.94 | 1.02 | 1.08 | 1.11 | 0.64 | 1.00 | 0.33 |
| C19 | 1.37 | 1.97 | 2.53 | 1.12 | 0.57 | 1.81 | 0.61 | 1.06 | 0.60 |
| C24 | 1.63 | 2.50 | 2.95 | 1.44 | 0.82 | 1.52 | 0.86 | 1.53 | 0.56 |
| C26 | 2.14 | 2.80 | 3.28 | 1.87 | 1.76 | 2.06 | 1.52 | 2.34 | 1.77 |
| C28 | 1.03 | 1.62 | 2.50 | 0.83 | 0.56 | 0.78 | 0.60 | 0.88 | 0.30 |
| C31 | 1.47 | 2.15 | 2.73 | 1.31 | 0.77 | 1.31 | 1.04 | 1.54 | 1.41 |
| C36 | 2.74 | 3.35 | 3.50 | 2.59 | 2.30 | 3.08 | 2.04 | 2.73 | 2.04 |
| C37 | 0.67 | 1.30 | 2.39 | 0.41 | 0.16 | 0.43 | 0.39 | 0.51 | 0.19 |
| C40 | 1.21 | 1.76 | 2.80 | 0.74 | 0.52 | 0.95 | 0.82 | 1.19 | 0.67 |
Appendix B. Statistical Descriptions
Appendix B.1. ANCOVA
| Domain | F statistic | p-value | Significance |
|---|---|---|---|
| Other | 33.3 | < 0.001 | *** |
| Neuroendocrine | 11.6 | 0.007 | ** |
| Fatigue | 5.2 | 0.046 | * |
| Autonomic | 3.8 | 0.08 | . |
| Pain | 3.1 | 0.108 | NA |
| Immune | 1.4 | 0.268 | NA |
| All_mean | 1.0 | 0.33 | NA |
| Sleep | 0.2 | 0.647 | NA |
| Neurocognitive | 0.0 | 0.849 | NA |
Appendix B.2. Leave-one-Out Analysis
| Cluster | Group | Domains Improved | Mean R2 |
|---|---|---|---|
| C2 | low | 9 | 0.0379 |
| C11 | low | 9 | 0.0271 |
| C4 | low | 8 | 0.0191 |
| C31 | high | 7 | 0.0163 |
| C7 | low | 5 | 0.0129 |
| C24 | low | 8 | 0.0126 |
Appendix B.3. R2 by Group
- Combined (all clusters)
- High-intensity group
- Low-intensity group
| Domain | Combined R2 | High-intensity R2 | Low-intensity R2 |
|---|---|---|---|
| All_mean | 0.91 | 1.00 | 0.84 |
| Autonomic | 0.79 | 0.96 | 0.62 |
| Fatigue | 0.84 | 0.86 | 0.54 |
| Immune | 0.78 | 0.96 | 0.11 |
| Neurocognitive | 0.85 | 0.92 | 0.93 |
| Neuroendocrine | 0.73 | 0.96 | 0.75 |
| Other | 0.52 | 0.92 | 0.96 |
| Pain | 0.81 | 0.95 | 0.95 |
| Sleep | 0.53 | 0.81 | 0.05 |
References
- Vaes, A. W. et al. Symptom-based clusters in people with ME/CFS: An illustration of clinical variety in a cross-sectional cohort. Journal of Translational Medicine. [CrossRef]
- Vaes, A. W. & collaborators. Supplementary dataset (excel): Additional file 3: Table S1 : 12967_2023_3946_MOESM3_ESM.xlsx. Journal of Translational Medicine, Springer Nature (2023). https://static-content.springer.com/esm/art%3A10.1186%2Fs12967-023-03946-6/MediaObjects/12967_2023_3946_MOESM3_ESM.
- Fall, E. A. et al. Chronic overlapping pain conditions in people with myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS): A sample from the multi-site clinical assessment of ME/CFS (MCAM) study. BMC Neurology. [CrossRef]
- Ramírez-Morales, R. , Bermúdez-Benítez, E., Martínez-Martínez, L.-A. & Martıínez-Lavín, M. Clinical overlap between fibromyalgia and myalgic encephalomyelitis: A systematic review and meta-analysis. Autoimmunity Reviews, 2022. [Google Scholar] [CrossRef]
- McManimen, S. L. & Jason, L. A. Post-exertional malaise in patients with ME and CFS with comorbid fibromyalgia. SRL Neurology & Neurosurgery, /: (2017). https, 2017. [Google Scholar]
- Vaes, A. W. & collaborators. Supplementary dataset (excel): Additional file 4 table S2 : 12967_2023_3946_MOESM4_ESM.xlsx. Journal of Translational Medicine, Springer Nature (2023). https://static-content.springer.com/esm/art%3A10.1186%2Fs12967-023-03946-6/MediaObjects/12967_2023_3946_MOESM4_ESM.
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




