Submitted:
11 September 2025
Posted:
12 September 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
1.1. Endoscopic Ear Surgery in Cholesteatoma Management
1.2. Histopathology and Immunohistochemistry
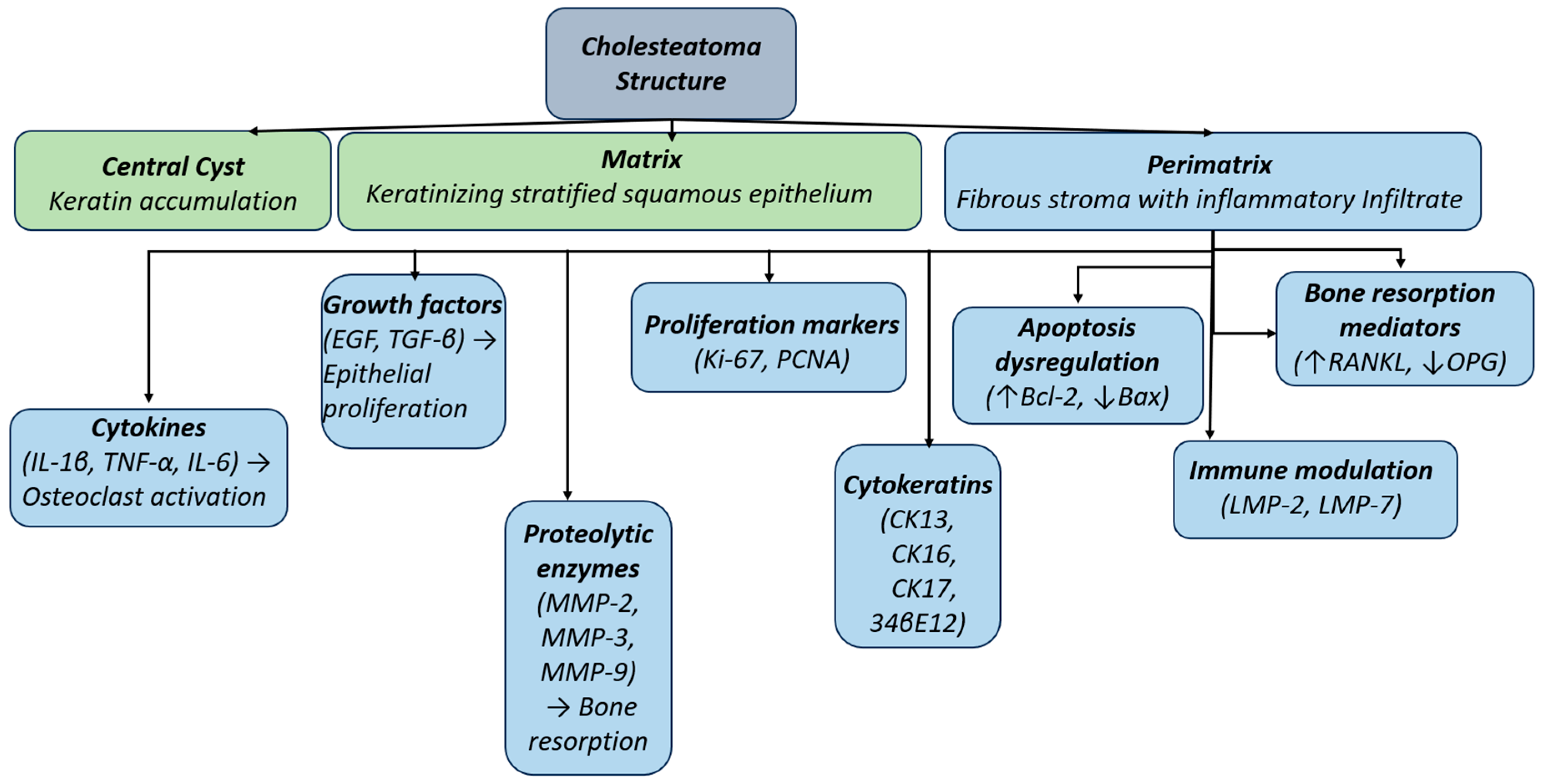
- Growth factors (EGF, TGF-β) promote epithelial proliferation.
- Proteolytic enzymes (MMP-2, MMP-3, MMP-9) enhance local bone destruction.
- Proliferation markers (Ki-67, PCNA) indicate the hyperproliferative nature of the epithelium.
- Cytokeratins (CK13, CK16, CK17, 34βE12) highlight altered epithelial differentiation.
- Apoptosis regulators (↑Bcl-2, ↓Bax) demonstrate dysregulation of programmed cell death.
- Immune modulation molecules (LMP-2, LMP-7) contribute to chronic inflammation.
- Bone resorption mediators (↑RANKL, ↓OPG) further accelerate osteoclastic activity[15].
1.3. Aim of the Present Study
|
Primary objective |
To assess the impact of endoscopic cholesteatoma surgery on health-related quality of life (QoL) using two validated PROMs: COMQ-12 and GBI. |
|
Secondary objectives |
|
|
Exploratory objective |
To contextualize PROMs findings with histological and immunohistochemical features of cholesteatoma (MMPs, cytokines, Ki-67, cytokeratins), highlighting potential links between biological aggressiveness and patient-perceived burden. |
2. Materials and Methods
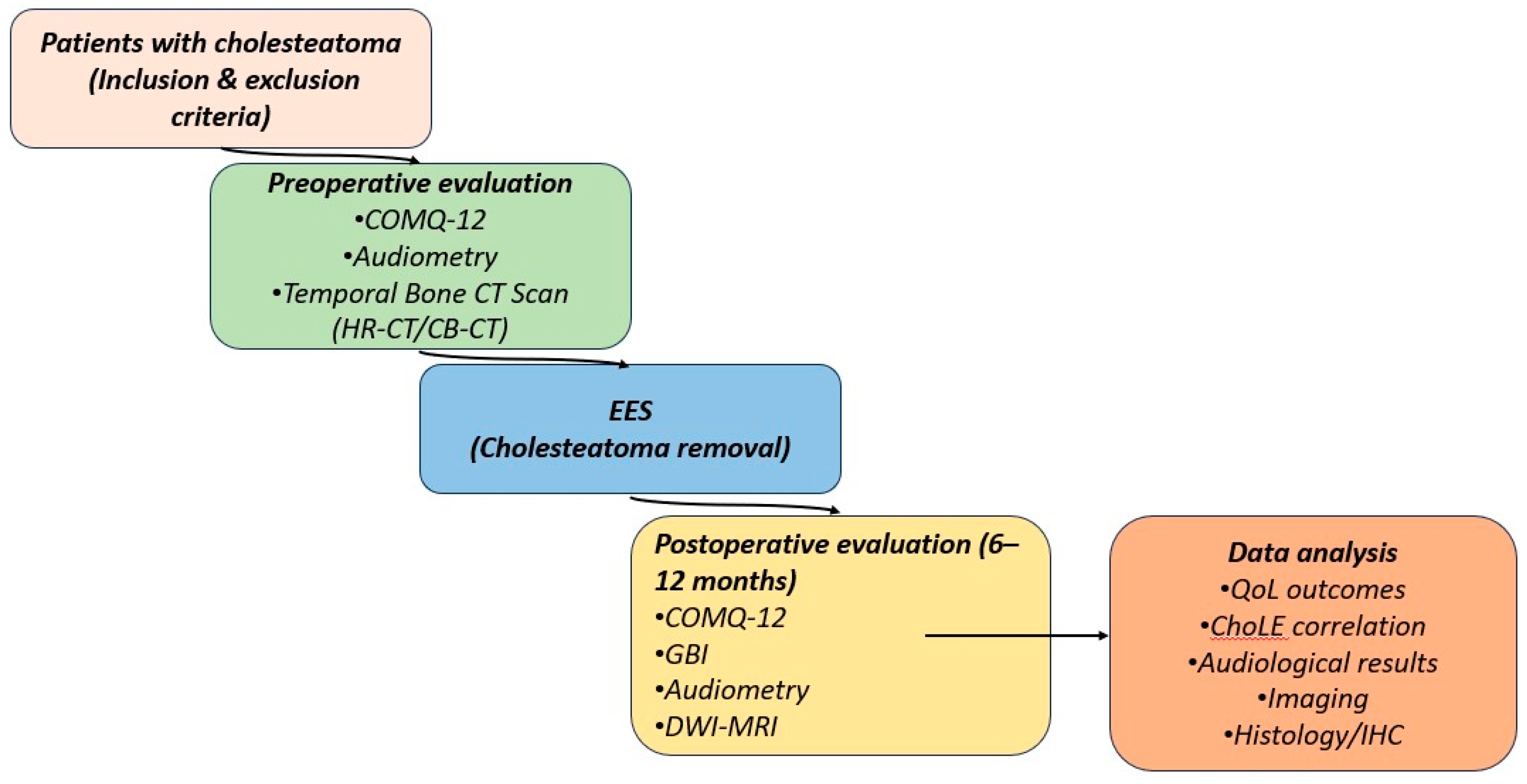
2.1. Study Design
2.2. Patient Selection and Eligibility Criteria
2.3. Sample Size Justification
2.4. Surgical Technique
2.4. Clinical and Audiological Assessment
2.5. Imaging Assessment
2.6. Quality of Life Assessment
2.7. Histological and Immunohistochemical Analysis (Exploratory)
2.8. Statistical Analysis
3. Results
3.1. Patient Characteristics
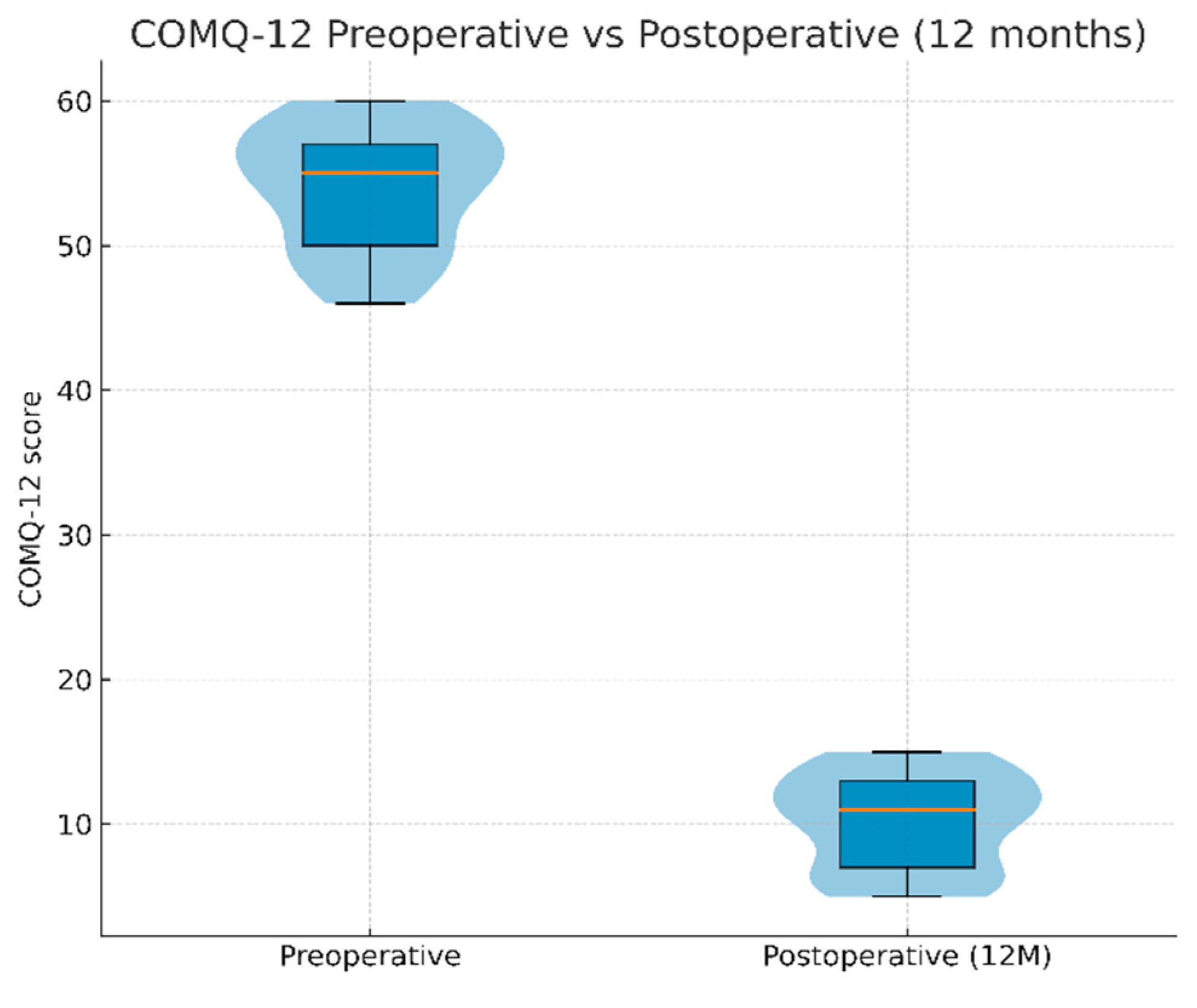
3.2. Quality of Life Outcomes
3.3. Audiological Results
3.4. Recurrence and Residual Disease
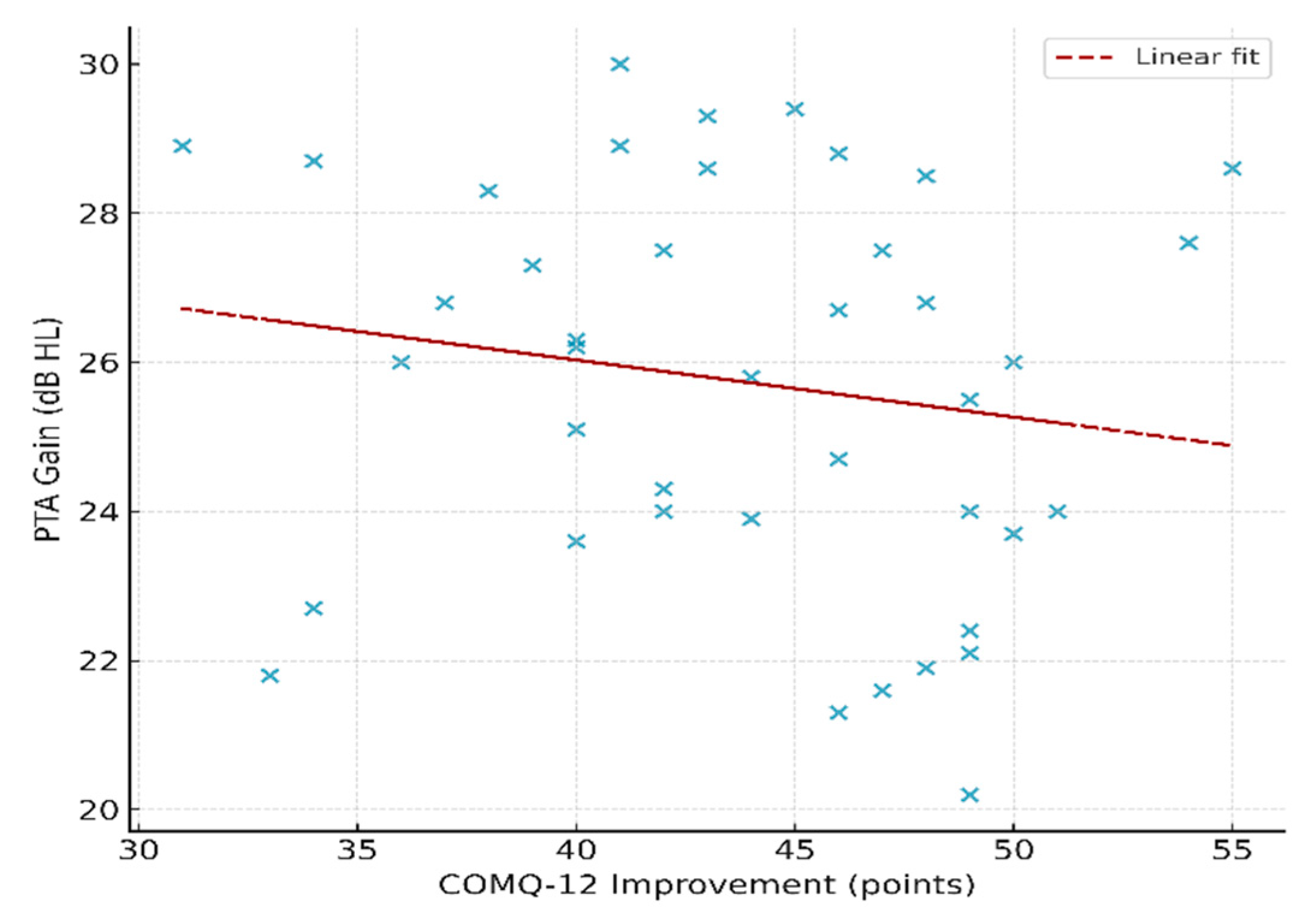
3.5. Correlations and Subgroup Analyses
| Variable 1 | Variable 2 | n | Method | Correlation (r/ρ) | p-value |
| COMQ-12 improvement | PTA gain (dB) | 41 | Pearson | –0.16 | 0.31 |
| GBI (12 months) | PTA gain (dB) | 41 | Spearman | 0.11 | 0.50 |
| GBI (12 months) | Age (years) | 41 | Spearman | –0.08 | 0.63 |
| COMQ-12 score (12 months) | Age (years) | 41 | Spearman | 0.17 | 0.30 |
3.6. Summary of Key Findings
4. Discussion
4.1. Interpretation of Findings
4.2. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| ABG | Air–Bone Gap |
| ANOVA | Analysis of Variance |
| Bax | Bcl-2-associated X protein |
| Bcl-2 | B-cell lymphoma 2 |
| CES | Endoscopic classification of the external auditory canal |
| ChOLE | Cholesteatoma extension, Ossicular chain status, Life-threatening complications, and Eustachian tube/mastoid status |
| COMQ-12 | Chronic Otitis Media Questionnaire-12 |
| CT | Computed Tomography |
| DWI-MRI | Diffusion-Weighted Magnetic Resonance Imaging |
| EAONO | European Academy of Otology and Neuro-Otology |
| EES | Endoscopic Ear Surgery |
| EGF | Epidermal Growth Factor |
| GBI | Glasgow Benefit Inventory |
| IHC | Immunohistochemistry |
| IL | Interleukin |
| IQR | Interquartile Range |
| JOS | Japanese Otological Society |
| LMP | Low Molecular Mass Polypeptide |
| MMP | Matrix Metalloproteinase |
| MRI | Magnetic Resonance Imaging |
| OPG | Osteoprotegerin |
| PCNA | Proliferating Cell Nuclear Antigen |
| PROMs | Patient-Reported Outcome Measures |
| PTA | Pure-Tone Average |
| QoL | Quality of Life |
| RANKL | Receptor Activator of Nuclear Factor Kappa-Β Ligand |
| RCT | Randomized Controlled Trial |
| SD | Standard Deviation |
| STAMCO | S – difficult visualisation areas, TAMCO - Tympanic cavity, Attic, Mastoid, Complications, and Ossicular chain involvement |
| TGF-β | Transforming Growth Factor-beta |
| TNF-α | Tumor Necrosis Factor-alpha |
References
- Kemppainen, H.O.; Puhakka, H.J.; Laippala, P.J.; Sipilä, M.M.; Manninen, M.P.; Karma, P.H. Epidemiology and Aetiology of Middle Ear Cholesteatoma. Acta Otolaryngol 1999, 119, 568–572, doi:10.1080/00016489950180801.
- Castle, J.T. Cholesteatoma Pearls: Practical Points and Update. Head Neck Pathol 2018, 12, 419–429, doi:10.1007/S12105-018-0915-5.
- Yung, M.; Tono, T.; Olszewska, E.; Yamamoto, Y.; Sudhoff, H.; Sakagami, M.; Mulder, J.; Kojima, H.; İncesulu, A.; Trabalzini, F.; et al. EAONO/JOS Joint Consensus Statements on the Definitions, Classification and Staging of Middle Ear Cholesteatoma. Journal of International Advanced Otology 2017, 13, 1–8, doi:10.5152/IAO.2017.3363.
- Linder, T.E.; Shah, S.; Martha, A.S.; Röösli, C.; Emmett, S.D. Introducing the “ChOLE” Classification and Its Comparison to the EAONO/JOS Consensus Classification for Cholesteatoma Staging. Otology and Neurotology 2019, 40, 63–72, doi:10.1097/MAO.0000000000002039,.
- Hu, Y.; Teh, B.M.; Hurtado, G.; Yao, X.; Huang, J.; Shen, Y. Can Endoscopic Ear Surgery Replace Microscopic Surgery in the Treatment of Acquired Cholesteatoma? A Contemporary Review. Int J Pediatr Otorhinolaryngol 2020, 131, doi:10.1016/J.IJPORL.2020.109872.
- Tarabichi, M.; Nogueira, J.F.; Marchioni, D.; Presutti, L.; Pothier, D.D.; Ayache, S. Transcanal Endoscopic Management of Cholesteatoma. Otolaryngol Clin North Am 2013, 46, 107–130, doi:10.1016/J.OTC.2012.10.001.
- Bonali, M.; Marchioni, D.; Bisi, N. Endoscopic Ear Surgery: Past and Future. Curr Otorhinolaryngol Rep 2022, 10, 343–348, doi:10.1007/S40136-022-00424-3/FIGURES/1.
- Bianconi, L.; Gazzini, L.; Laura, E.; De Rossi, S.; Conti, A.; Marchioni, D. Endoscopic Stapedotomy: Safety and Audiological Results in 150 Patients. European Archives of Oto-Rhino-Laryngology 2020, 277, 85–92, doi:10.1007/s00405-019-05688-y.
- Bassiouny, M.; Badour, N.; Omran, A.; Osama, H. Histopathological and Immunohistochemical Characteristics of Acquired Cholesteatoma in Children and Adults. Egyptian Journal of Ear, Nose, Throat and Allied Sciences 2012, 13, 7–12, doi:10.1016/j.ejenta.2012.02.007.
- Bologa, R.A.; Anghelina, F.; Mitroi, M.R.; Ciolofan, M.S.; Mogoantă, C.A.; Căpitănescu, A.N.; Grecu, A.F.; Anghelina, L.; Botezat, M.M.; Mogoş, A.A.; et al. Biology of Recurrent Cholesteatoma in a Romanian Young Patient – a Case Report. Romanian Journal of Morphology and Embryology 2024, 65, 775–780, doi:10.47162/RJME.65.4.24.
- Dornelles, C.; da Costa, S.S.; Meurer, L.; Schweiger, C. Correlation of Cholesteatomas Perimatrix Thickness with Patient’s Age. Braz J Otorhinolaryngol 2005, 71, 792–797, doi:10.1016/s1808-8694(15)31250-7.
- Kennedy, K.L.; Singh, A.K. Middle Ear Cholesteatoma. StatPearls 2024.
- Imai, R.; Sato, T.; Iwamoto, Y.; Hanada, Y.; Terao, M.; Ohta, Y.; Osaki, Y.; Imai, T.; Morihana, T.; Okazaki, S.; et al. Osteoclasts Modulate Bone Erosion in Cholesteatoma via RANKL Signaling. JARO - Journal of the Association for Research in Otolaryngology 2019, 20, 449–459, doi:10.1007/S10162-019-00727-1,.
- Espahbodi, M.; Samuels, T.L.; McCormick, C.; Khampang, P.; Yan, K.; Marshall, S.; McCormick, M.E.; Chun, R.H.; Harvey, S.A.; Friedland, D.R.; et al. Analysis of Inflammatory Signaling in Human Middle Ear Cell Culture Models of Pediatric Otitis Media. Laryngoscope 2021, 131, 410–416, doi:10.1002/LARY.28687.
- Bassiouny, M.; Badour, N.; Omran, A.; Osama, H. Histopathological and Immunohistochemical Characteristics of Acquired Cholesteatoma in Children and Adults. Egyptian Journal of Ear, Nose, Throat and Allied Sciences 2012, 13, 7–12, doi:10.1016/J.EJENTA.2012.02.007.
- Von Elm, E.; Altman, D.G.; Egger, M.; Pocock, S.J.; Gøtzsche, P.C.; Vandenbroucke, J.P. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) Statement: Guidelines for Reporting Observational Studies. PLoS Med 2007, 4, 1623–1627, doi:10.1371/journal.pmed.0040296.
- J, P.; Haggard, Y.M. Chronic Otitis Media Questionnaire-12 (COMQ-12).
- Glasgow Health Status Questionnaires Manual Available online: https://studylib.net/doc/8450311/the-health-status-questionnaires-manual (accessed on 23 August 2025).
- Quality of Life after Cholesteatoma Surgery: Comparison between Surgical Techniques. - Abstract - Europe PMC Available online: https://europepmc.org/article/PMC/9330745 (accessed on 23 August 2025).
- Phillips, J.S.; Tailor, B. V.; Nunney, I.; Yung, M.W.; Doruk, C.; Kara, H.; Kong, T.; Quaranta, N.; Peñaranda, A.; Bernardeschi, D.; et al. Impact of Hearing Disability and Ear Discharge on Quality-of-Life in Patients with Chronic Otitis Media: Data from the Multinational Collaborative COMQ-12 Study. Otology and Neurotology 2021, 42, E1507–E1512, doi:10.1097/MAO.0000000000003299.
- EL-Meselaty, K.; Badr-El-Dine, M.; Mandour, M.; Mourad, M.; Darweesh, R. Endoscope Affects Decision Making in Cholesteatoma Surgery. Otolaryngology - Head and Neck Surgery 2003, 129, 490–496, doi:10.1016/S0194-5998(03)01577-8.
- Van Der Toom, H.F.E.; Van Der Schroeff, M.P.; Janssen, J.M.H.; Westzaan, A.M.; Pauw, R.J. A Retrospective Analysis and Comparison of the STAM and STAMCO Classification and EAONO/JOS Cholesteatoma Staging System in Predicting Surgical Treatment Outcomes of Middle Ear Cholesteatoma. Otology and Neurotology 2020, 41, e468–e474, doi:10.1097/MAO.0000000000002549.
- ten Tije, F.A.; Merkus, P.; Buwalda, J.; Blom, H.M.; Kramer, S.E.; Pauw, R.J.; Nyst, H.J.; van der Putten, L.; Graveland, A.P.; Kingma, G.G.; et al. Practical Applicability of the STAMCO and ChOLE Classification in Cholesteatoma Care. European Archives of Oto-Rhino-Laryngology 2021, 278, 3777–3787, doi:10.1007/S00405-020-06478-7.
- Choi, J.E.; Kang, W.S.; Lee, J.D.; Chung, J.W.; Kong, S.K.; Lee, I.W.; Moon, I.J.; Hur, D.G.; Moon, I.S.; Cho, H.H. Outcomes of Endoscopic Congenital Cholesteatoma Removal in South Korea. JAMA Otolaryngol Head Neck Surg 2023, 149, 231, doi:10.1001/JAMAOTO.2022.4660.
- Yong, M.; Mijovic, T.; Lea, J. Endoscopic Ear Surgery in Canada: A Cross-Sectional Study. Journal of Otolaryngology - Head and Neck Surgery 2016, 45, doi:10.1186/S40463-016-0117-7,.
- Badr-El-Dine, M.; James, A.L.; Panetti, G.; Marchioni, D.; Presutti, L.; Nogueira, J.F. Instrumentation and Technologies in Endoscopic Ear Surgery. Otolaryngol Clin North Am 2013, 46, 211–225, doi:10.1016/J.OTC.2012.10.005.
- Couvreur, F.; Loos, E.; Desloovere, C.; Verhaert, N. Efficacy of Otoendoscopy for Residual Cholesteatoma Detection During Microscopic Chronic Ear Surgery. J Int Adv Otol 2024, 20, 225, doi:10.5152/IAO.2024.231122.
- Badr-el-Dine, M. Value of Ear Endoscopy in Cholesteatoma Surgery. Otology and Neurotology 2002, 23, 631–635, doi:10.1097/00129492-200209000-00004.
- Bächinger, D.; Rrahmani, A.; Weiss, N.M.; Mlynski, R.; Huber, A.; Röösli, C. Evaluating Hearing Outcome, Recidivism and Complications in Cholesteatoma Surgery Using the ChOLE Classification System. European Archives of Oto-Rhino-Laryngology 2020, 278, 1365, doi:10.1007/S00405-020-06208-Z.
- Henninger, B.; Kremser, C. Diffusion Weighted Imaging for the Detection and Evaluation of Cholesteatoma. World J Radiol 2017, 9, 217, doi:10.4329/WJR.V9.I5.217.
- Yiğiter, A.C.; Pınar, E.; İmre, A.; Erdoğan, N. Value of Echo-Planar Diffusion-Weighted Magnetic Resonance Imaging for Detecting Tympanomastoid Cholesteatoma. Journal of International Advanced Otology 2015, 11, 53–57, doi:10.5152/IAO.2015.447.
- Phillips, J.S.; Yung, M.W.; Nunney, I.; Doruk, C.; Kara, H.; Kong, T.; Quaranta, N.; Peñaranda, A.; Bernardeschi, D.; Dai, C.; et al. Multinational Appraisal of the Chronic Otitis Media Questionnaire 12 (COMQ-12). Otology and Neurotology 2021, 42, e45–e49, doi:10.1097/MAO.0000000000002845,.
- Bukurov, B.; Haggard, M.; Spencer, H.; Arsovic, N.; Grujicic, S.S. Can Short PROMs Support Valid Factor-Based Sub-Scores? Example of COMQ-12 in Chronic Otitis Media. PLoS One 2022, 17, doi:10.1371/journal.pone.0274513.
- Taneja, V.; Milner, T.D.; Iyer, A. Endoscopic Ear Surgery: Does It Have an Impact on Quality of Life? Our Experience of 152 Cases. Clinical Otolaryngology 2020, 45, 126–129, doi:10.1111/COA.13459;WGROUP:STRING:PUBLICATION.
- Rutkowska, J.; Kasacka, I.; Rogowski, M.; Olszewska, E. Immunohistochemical Identification and Assessment of the Location of Immunoproteasome Subunits LMP2 and LMP7 in Acquired Cholesteatoma. Int J Mol Sci 2023, 24, doi:10.3390/IJMS241814137,.
- Schürmann, M.; Oppel, F.; Shao, S.; Volland-Thurn, V.; Kaltschmidt, C.; Kaltschmidt, B.; Scholtz, L.U.; Sudhoff, H. Chronic Inflammation of Middle Ear Cholesteatoma Promotes Its Recurrence via a Paracrine Mechanism. Cell Commun Signal 2021, 19, 25, doi:10.1186/S12964-020-00690-Y.
- Ayache, S.; Beltran, M.; Guevara, N. Endoscopic Classification of the External Auditory Canal for Transcanal Endoscopic Ear Surgery. Eur Ann Otorhinolaryngol Head Neck Dis 2019, 136, 247–250, doi:10.1016/J.ANORL.2019.03.005.
- Yiannakis, C.P.; Sproat, R.; Iyer, A. Preliminary Outcomes of Endoscopic Middle-Ear Surgery in 103 Cases: A UK Experience. Journal of Laryngology and Otology 2018, 132, 493–496, doi:10.1017/S0022215118000695.
- Elfeky, A.E.M.; Khazbzk, A.O.; Nasr, W.F.; Emara, T.A.; Elanwar, M.W.; Amer, H.S.; Fouad, Y.A. Outcomes of Using Otoendoscopy During Surgery for Cholesteatoma. Indian Journal of Otolaryngology and Head and Neck Surgery 2019, 71, 1036–1039, doi:10.1007/S12070-017-1084-7.
- Barakate, M.; Bottrill, I. Combined Approach Tympanoplasty for Cholesteatoma: Impact of Middle-Ear Endoscopy. Journal of Laryngology and Otology 2008, 122, 120–124, doi:10.1017/S0022215107009346.
- Ayache, S.; Tramier, B.; Strunski, V. Otoendoscopy in Cholesteatoma Surgery of the Middle Ear: What Benefits Can Be Expected? Otology and Neurotology 2008, 29, 1085–1090, doi:10.1097/MAO.0B013E318188E8D7.
- Verma, B.; Dabholkar, Y.G. Role of Endoscopy in Surgical Management of Cholesteatoma: A Systematic Review. J Otol 2020, 15, 166, doi:10.1016/J.JOTO.2020.06.004.
- Sarcu, D.; Isaacson, G. Long-Term Results of Endoscopically Assisted Pediatric Cholesteatoma Surgery. Otolaryngology - Head and Neck Surgery (United States) 2016, 154, 535–539, doi:10.1177/0194599815622441.
- Li, B.; Zhou, L.; Wang, M.; Wang, Y.; Zou, J. Endoscopic versus Microscopic Surgery for Treatment of Middle Ear Cholesteatoma: A Systematic Review and Meta-Analysis. Am J Otolaryngol 2021, 42, 102451, doi:10.1016/J.AMJOTO.2020.102451.
- Nair, S.; Aishwarya, J.G.; Warrier, N.; Pavithra, V.; Jain, A.; Shamim, M.; Ramanathan, K.; Vasu, P.K. Endoscopic Ear Surgery in Middle Ear Cholesteatoma. Laparosc Endosc Robot Surg 2021, 4, 24–29, doi:10.1016/J.LERS.2021.01.004.
- Basonbul, R.A.; Ronner, E.A.; Kozin, E.D.; Lee, D.J.; Cohen, M.S. Systematic Review of Endoscopic Ear Surgery Outcomes for Pediatric Cholesteatoma. Otology and Neurotology 2021, 42, 108–115, doi:10.1097/MAO.0000000000002876,.
- Hamela, M.A.A.; Abd-Elnaseer, O.; El-Dars, M.M.; El-Antably, A. Comparison of the Outcomes of Endoscopic versus Microscopic Approach in Cholesteatoma Surgery: A Randomized Clinical Study. Egyptian Journal of Otolaryngology 2023, 39, 1–5, doi:10.1186/S43163-023-00492-2/TABLES/3.
- Migirov, L.; Shapira, Y.; Horowitz, Z.; Wolf, M. Exclusive Endoscopic Ear Surgery for Acquired Cholesteatoma: Preliminary Results. Otol Neurotol 2011, 32, 433–436, doi:10.1097/mao.0b013e3182096b39.
- Cohen, M.S.; Basonbul, R.A.; Kozin, E.D.; Lee, D.J. Residual Cholesteatoma during Second-Look Procedures Following Primary Pediatric Endoscopic Ear Surgery. Otolaryngology - Head and Neck Surgery (United States) 2017, 157, 1034–1040, doi:10.1177/0194599817729136.
- Bae, M.R.; Kang, W.S.; Chung, J.W. Comparison of the Clinical Results of Attic Cholesteatoma Treatment: Endoscopic versus Microscopic Ear Surgery. Clin Exp Otorhinolaryngol 2019, 12, 156–162, doi:10.21053/ceo.2018.00507.
- Raemy, Y.; Bächinger, D.; Peter, N.; Roosli, C. Health-Related Quality of Life in Patients after Endoscopic or Microscopic Cholesteatoma Surgery. European Archives of Oto-Rhino-Laryngology 2025, 282, 2275–2283, doi:10.1007/S00405-024-09097-8/FIGURES/5.
- Pollak, N. Endoscopic and Minimally-Invasive Ear Surgery: A Path to Better Outcomes. World J Otorhinolaryngol Head Neck Surg 2017, 3, 129–135, doi:10.1016/j.wjorl.2017.08.001.
- James, A.L. Endoscopic Middle Ear Surgery in Children. Otolaryngol Clin North Am 2013, 46, 233–244, doi:10.1016/J.OTC.2012.10.007.
- Tarabichi, M. Endoscopic Management of Limited Attic Cholesteatoma. Laryngoscope 2004, 114, 1157–1162, doi:10.1097/00005537-200407000-00005.
- Otsuka, A.; Koyama, H.; Kashio, A.; Matsumoto, Y.; Yamasoba, T. Comparison of Endoscopic and Microscopic Surgery for the Treatment of Acquired Cholesteatoma by EAONO/JOS Staging. Healthcare (Switzerland) 2024, 12, 1737, doi:10.3390/HEALTHCARE12171737/S1.
- Chiao, W.; Chieffe, D.; Fina, M. Endoscopic Management of Primary Acquired Cholesteatoma. Otolaryngol Clin North Am 2021, 54, 129–145, doi:10.1016/J.OTC.2020.09.014.
- Dalğıç, A.; Aksoy Yıldırım, G.; Zorlu, M.E.; Delice, O.; Aysel, A. Total Transcanal Endoscopic Ear Surgery for Cholesteatoma. Turk Arch Otorhinolaryngol 2023, 61, 1–7, doi:10.4274/TAO.2023.2022-11-6.
- Marchioni, D.; Alicandri-Ciufelli, M.; Piccinini, A.; Genovese, E.; Presutti, L. Inferior Retrotympanum Revisited: An Endoscopic Anatomic Study. Laryngoscope 2010, 120, 1880–1886, doi:10.1002/LARY.20995.
- Kuo, C.L.; Shiao, A.S.; Yung, M.; Sakagami, M.; Sudhoff, H.; Wang, C.H.; Hsu, C.H.; Lien, C.F. Updates and Knowledge Gaps in Cholesteatoma Research. Biomed Res Int 2015, 2015, doi:10.1155/2015/854024.
- Marchioni, D.; Soloperto, D.; Rubini, A.; Villari, D.; Genovese, E.; Artioli, F.; Presutti, L. Endoscopic Exclusive Transcanal Approach to the Tympanic Cavity Cholesteatoma in Pediatric Patients: Our Experience. Int J Pediatr Otorhinolaryngol 2015, 79, 316–322, doi:10.1016/J.IJPORL.2014.12.008.
- The Efficacy of Transcanal Endoscopic Ear Surgery in Children Compared to Adults - PubMed Available online: https://pubmed.ncbi.nlm.nih.gov/40310232/ (accessed on 23 August 2025).
- Dornhoffer, J.L.; Friedman, A.B.; Gluth, M.B. Management of Acquired Cholesteatoma in the Pediatric Population. Curr Opin Otolaryngol Head Neck Surg 2013, 21, 440–445, doi:10.1097/MOO.0B013E32836464BD.
- Kuo, C.L.; Liao, W.H.; Shiao, A.S. A Review of Current Progress in Acquired Cholesteatoma Management. European Archives of Oto-Rhino-Laryngology 2015, 272, 3601–3609, doi:10.1007/S00405-014-3291-0.
- Ito, T.; Kubota, T.; Watanabe, T.; Futai, K.; Furukawa, T.; Kakehata, S. Transcanal Endoscopic Ear Surgery for Pediatric Population with a Narrow External Auditory Canal. Int J Pediatr Otorhinolaryngol 2015, 79, 2265–2269, doi:10.1016/j.ijporl.2015.10.019.
- Miller, K.A.; Fina, M.; Lee, D.J. Principles of Pediatric Endoscopic Ear Surgery. Otolaryngol Clin North Am 2019, 52, 825–845, doi:10.1016/j.otc.2019.06.001.
- Dixon, P.R.; James, A.L. Evaluation of Residual Disease Following Transcanal Totally Endoscopic vs Postauricular Surgery among Children with Middle Ear and Attic Cholesteatoma. JAMA Otolaryngol Head Neck Surg 2020, 146, 408–413, doi:10.1001/jamaoto.2020.0001.
- Bovi, C.; Luchena, A.; Bivona, R.; Borsetto, D.; Creber, N.; Danesi, G. Recurrence in Cholesteatoma Surgery: What Have We Learnt and Where Are We Going? A Narrative Review. Acta Otorhinolaryngologica Italica 2023, 43, S48, doi:10.14639/0392-100X-SUPPL.1-43-2023-06.
- Tomlin, J.; Chang, D.; McCutcheon, B.; Harris, J. Surgical Technique and Recurrence in Cholesteatoma: A Meta-Analysis. Audiology and Neurotology 2013, 18, 135–142, doi:10.1159/000346140.
| Inclusion criteria | Exclusion criteria |
| Diagnosis of primary or recurrent cholesteatoma (confirmed by clinical exam and imaging) | Extensive disease requiring a retroauricular (mastoid) approach |
| Scheduled for exclusive endoscopic cholesteatoma surgery | Contraindication to general anesthesia |
| Ability to complete pre- and postoperative QoL questionnaires (COMQ-12 and GBI) | Cognitive impairment or inability to complete questionnaires |
| Minimum planned follow-up of ≥ 12 months | |
| Written informed consent obtained |
| Characteristic | Value |
| Age (mean ± SD, range) | 41.0 ± 14.4 (19–65) |
| Sex (M/F, %) | M: 16 (39.0%), F: 25 (61.0%) |
| Operated side (Right/Left, %) | Right: 23 (56.1%), Left: 18 (43.9%) |
| Chole classification | Stage 1: 41 (100%) |
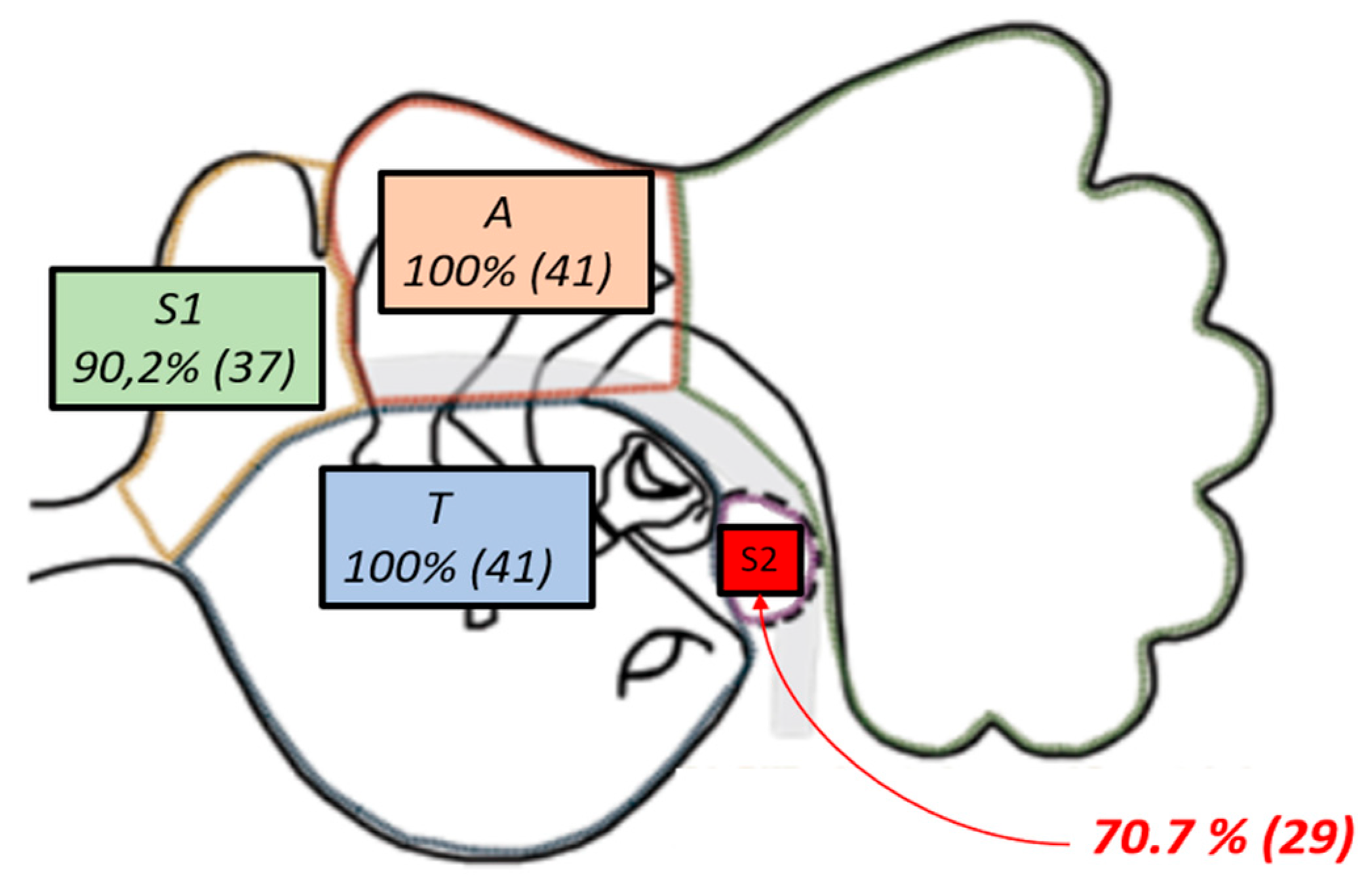
| STAMCO classification | Attic (A) and tympanic cavity (T) 100% (41) anterior difficult area (S1) 90.2% (37) posterior difficult area (S2) 70.7% (29) |
| Type of intervention | Exclusive EES: 41 (100%) |
| Type of reconstruction | Cartilage tympanoplasty: 12 (29.3%); Incus Interposition: 11 (26.8%); PORP: 10 (24.4%); TORP: 8 (19.5%) |
| Follow-up (mean, range) | 12 months (all patients) |
| Timepoint |
COMQ-12 Score (mean ± SD) |
p-value (vs. Preop) |
| Preoperative | 54.0 ± 4.2 | – |
| 3 months | 41.9 ± 7.2 | < 0.001 |
| 6 months | 38.0 ± 5.3 | < 0.001 |
| 12 months | 10.2 ± 3.3 | < 0.001 |
| Timepoint | GBI Score (mean ± SD) | p-value (12 vs 6 months) |
| 6 months | 82.6 ± 4.8 | – |
| 12 months | 84.1 ± 4.9 | < 0.001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




