Submitted:
25 August 2025
Posted:
26 August 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
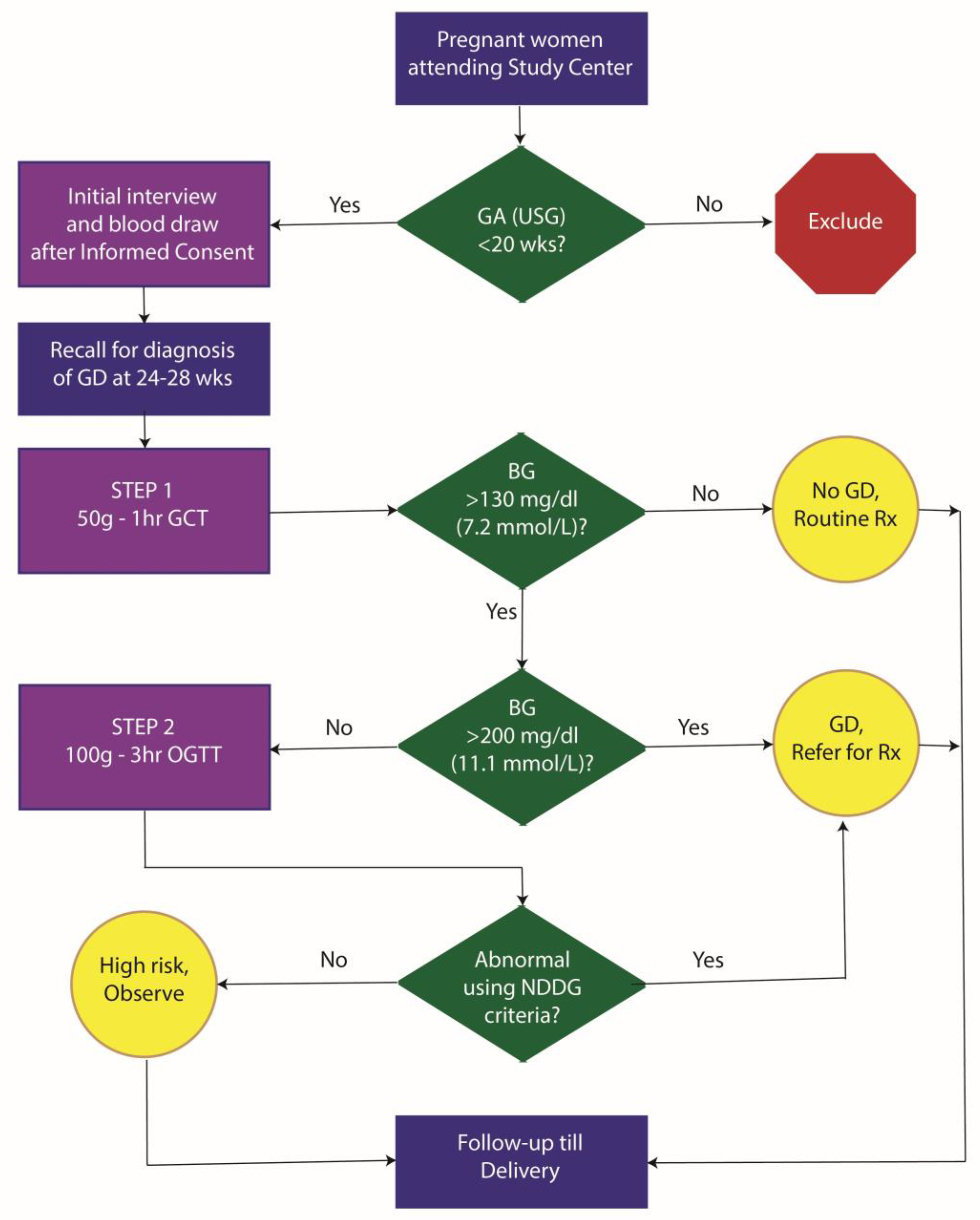
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| ACOG | American College of Obstetrics and Gynecology |
| AMPM | Automated Multi-Pass Method |
| BMI | Body mass index |
| C&C | Carpenter-Coustan |
| GCT | Glucose Challenge Test |
| GD | Gestational Diabetes |
| HDL | High density lipoprotein |
| LDL | Low density lipoprotein |
| MERGD | Markers of Early Risk-stratification of Gestational Diabetes |
| MET | Metabolic equivalents |
| NDDG | National Diabetes Data Group |
| OGTT | Oral Glucose Tolerance Test |
| PPAQ | Pregnancy Physical Activity Questionnaire |
| TG | Triglycerides |
| VLDL | Very low density lipoprotein |
| WHO | World Health Organization |
References
- Lain, K.Y.; Catalano, P.M. Metabolic changes in pregnancy. Clinical obstetrics and gynecology. 2007, 50, 938–948. [Google Scholar] [CrossRef] [PubMed]
- WHO Diagnostic criteria and classification of hyperglycaemia first detected in pregnancy; World Health Organization: Geneva, 2013.
- Group, H.S.C.R. Hyperglycemia and Adverse Pregnancy Outcome (HAPO) Study: associations with neonatal anthropometrics. Diabetes. 2009, 58, 453–459. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Group, H.S.C.R.; Metzger, B.E.; Lowe, L.P.; Dyer, A.R.; Trimble, E.R.; Chaovarindr, U.; Coustan, D.R.; Hadden, D.R.; McCance, D.R.; Hod, M.; McIntyre, H.D.; Oats, J.J.; Persson, B.; Rogers, M.S.; Sacks, D.A. Hyperglycemia and adverse pregnancy outcomes. The New England journal of medicine. 2008, 358, 1991–2002. [Google Scholar] [CrossRef] [PubMed]
- Li-Zhen, L.; Yun, X.; Xiao-Dong, Z.; Shu-Bin, H.; Zi-Lian, W.; Adrian Sandra, D.; Bin, L. Evaluation of guidelines on the screening and diagnosis of gestational diabetes mellitus: systematic review. BMJ open. 2019, 9, e023014. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- ACOG Practice Bulletin No. 190: Gestational Diabetes Mellitus. Obstetrics and gynecology. 2018, 131, e49–e64. [CrossRef] [PubMed]
- Mohan, V.; Usha, S.; Uma, R. Screening for gestational diabetes in India: Where do we stand? Journal of postgraduate medicine. 2015, 61, 151–154. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Coustan, D.R.; Lowe, L.P.; Metzger, B.E.; Dyer, A.R.; International Association of, D.; Pregnancy Study, G. The Hyperglycemia and Adverse Pregnancy Outcome (HAPO) study: paving the way for new diagnostic criteria for gestational diabetes mellitus. American journal of obstetrics and gynecology. 2010, 202, 654–e1. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Langer, O.; Umans, J.G.; Miodovnik, M. Perspectives on the proposed gestational diabetes mellitus diagnostic criteria. Obstetrics and gynecology. 2013, 121, 177–182. [Google Scholar] [CrossRef] [PubMed]
- Bodmer-Roy, S.; Morin, L.; Cousineau, J.; Rey, E. Pregnancy outcomes in women with and without gestational diabetes mellitus according to the International Association of the Diabetes and Pregnancy Study Groups criteria. Obstetrics and gynecology. 2012, 120, 746–752. [Google Scholar] [CrossRef] [PubMed]
- Fuller, K.P.; Borgida, A.F. Gestational diabetes mellitus screening using the one-step versus two-step method in a high-risk practice. Clinical diabetes : a publication of the American Diabetes Association. 2014, 32, 148–150. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Li, K.T.; Naik, S.; Alexander, M.; Mathad, J.S. Screening and diagnosis of gestational diabetes in India: a systematic review and meta-analysis. Acta diabetologica. 2018, 55, 613–625. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Dawood FS, Hunt D, Patel A, Kittikraisak W, Tinoco Y, Kurhe K, Soto G, Hombroek D, Garg S, Chotpitayasunondh T, Gonzales O, Bhargav S, Thompson MG, Chotpitayasunondh B, Florian R, Prakash A, Arriola S, Macareo L, Das P, Cabrera S, La Rosa S, Azziz-Baumgartner E, Pregnancy, Influenza Multinational Epidemiologic Study Working G. The Pregnancy and Influenza Multinational Epidemiologic (PRIME) study: a prospective cohort study of the impact of influenza during pregnancy among women in middle-income countries. Reproductive health. 2018, 15, 159. [CrossRef] [PubMed] [PubMed Central]
- Dawood, F.S.; Kittikraisak, W.; Patel, A.; Rentz Hunt, D.; Suntarattiwong, P.; Wesley, M.G.; Thompson, M.G.; Soto, G.; Mundhada, S.; Arriola, C.S.; Azziz-Baumgartner, E.; Brummer, T.; Cabrera, S.; Chang, H.H.; Deshmukh, M.; Ellison, D.; Florian, R.; Gonzales, O.; Kurhe, K.; Kaoiean, S.; Rawangban, B.; Lindstrom, S.; Llajaruna, E.; Mott, J.A.; Saha, S.; Prakash, A.; Mohanty, S.; Sinthuwattanawibool, C.; Tinoco, Y. Incidence of influenza during pregnancy and association with pregnancy and perinatal outcomes in three middle-income countries: a multisite prospective longitudinal cohort study. The Lancet Infectious diseases. 2021, 21, 97–106. [Google Scholar] [CrossRef] [PubMed]
- American Diabetes, A. 2. Classification and Diagnosis of Diabetes: Standards of Medical Care in Diabetes-2018. Diabetes care 2018, 41, S13–S27. [Google Scholar] [CrossRef] [PubMed]
- Carpenter, M.W.; Coustan, D.R. Criteria for screening tests for gestational diabetes. American journal of obstetrics and gynecology. 1982, 144, 768–773. [Google Scholar] [CrossRef] [PubMed]
- Raper, N.R.; Perloff, B.; Ingwersen, L.; Steinfeldt, L.; Anand, J. An overview of USDA's dietary intake data system. J Foof Compos Anal. 2004, 17, 545–555. [Google Scholar] [CrossRef]
- Gopalan, C.; Rama Sastri, B.V.; Balasubramanian, S.C. Nutritive value of Indian Foods; National Institute of Nutrition: Hyderabad, India, 2012. [Google Scholar]
- Chasan-Taber, L.; Schmidt, M.D.; Roberts, D.E.; Hosmer, D.; Markenson, G.; Freedson, P.S. Development and validation of a Pregnancy Physical Activity Questionnaire. Medicine and science in sports and exercise. 2004, 36, 1750–1760. [Google Scholar] [CrossRef] [PubMed]
- Chowdhury Salian, S.; Singh, J. Reliability and validity of the Indian version of the Pregnancy Physical Activity Questionnaire (PPAQ). Int J Curr Res Modern Ed. 2017, 2, 89–92. [Google Scholar]
- VanderWeele, T.J.; Ding, P. Sensitivity Analysis in Observational Research: Introducing the E-Value. Annals of internal medicine. 2017, 167, 268–274. [Google Scholar] [CrossRef] [PubMed]
- Consultation, W.H.O.E. Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet. 2004, 363, 157–163. [Google Scholar] [CrossRef] [PubMed]
- Ryan, E.A.; Savu, A.; Yeung, R.O.; Moore, L.E.; Bowker, S.L.; Kaul, P. Elevated fasting vs post-load glucose levels and pregnancy outcomes in gestational diabetes: a population-based study. Diabetic medicine : a journal of the British Diabetic Association. 2020, 37, 114–122. [Google Scholar] [CrossRef] [PubMed]
- Kaul, P.; Savu, A.; Yeung, R.O.; Ryan, E.A. Association between maternal glucose and large for gestational outcomes: Real-world evidence to support Hyperglycaemia and Adverse Pregnancy Outcomes (HAPO) study findings. Diabetic medicine : a journal of the British Diabetic Association. 2022, 39, e14786. [Google Scholar] [CrossRef] [PubMed]
- Roeckner, J.T.; Sanchez-Ramos, L.; Jijon-Knupp, R.; Kaunitz, A.M. Single abnormal value on 3-hour oral glucose tolerance test during pregnancy is associated with adverse maternal and neonatal outcomes: a systematic review and metaanalysis. American journal of obstetrics and gynecology. 2016, 215, 287–297. [Google Scholar] [CrossRef] [PubMed]
- Levin, G.; Tsur, A.; Shai, D.; Cahan, T.; Shapira, M.; Meyer, R. Prediction of adverse neonatal outcome among newborns born through meconium-stained amniotic fluid. International journal of gynaecology and obstetrics: the official organ of the International Federation of Gynaecology and Obstetrics. 2021, 154, 515–520. [Google Scholar] [CrossRef] [PubMed]
- Oral, S.; Celik, S.; Akpak, Y.K.; Golbasi, H.; Bayraktar, B.; Unver, G.; Sahin, S.; Yurtcu, N.; Soyer Caliskan, C. Prediction of gestational diabetes mellitus and perinatal outcomes by plasma zonulin levels. Archives of gynecology and obstetrics 2022. [Google Scholar] [CrossRef] [PubMed]
- Modzelewski, R.; Stefanowicz-Rutkowska, M.M.; Matuszewski, W.; Bandurska-Stankiewicz, E.M. Gestational Diabetes Mellitus-Recent Literature Review. Journal of clinical medicine 2022, 11. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Ye, W.; Luo, C.; Huang, J.; Li, C.; Liu, Z.; Liu, F. Gestational diabetes mellitus and adverse pregnancy outcomes: systematic review and meta-analysis. . 2022;377:e067946. Epub 2022/05/26. Bmj 2022, 377, e067946, at www.icmje.org/disclosure-of-interest/ and declare: support from the National Natural Science Foundation of China and the Natural Science Foundation for Young Scientist of Hunan Province, China for the submitted work; no financial relationships with any organisations that might have an interest in the submitted work in the previous three years; no other relationships or activities that could appear to have influenced the submitted work. [Google Scholar] [CrossRef] [PubMed]
- Liu, H.; Liu, J. Improved support vector machine algorithm based on the influence of Gestational Diabetes Mellitus on the outcome of perinatal outcome by ultrasound imaging. Pakistan journal of medical sciences. 2021, 37, 1625–1629. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Xu, H.; Arkema, E.V.; Cnattingius, S.; Stephansson, O.; Johansson, K. Gestational weight gain and delivery outcomes: A population-based cohort study. Paediatric and perinatal epidemiology. 2021, 35, 47–56. [Google Scholar] [CrossRef] [PubMed]
- Glazer, K.B.; Danilack, V.A.; Field, A.E.; Werner, E.F.; Savitz, D.A. Term Labor Induction and Cesarean Delivery Risk among Obese Women with and without Comorbidities. American journal of perinatology. 2022, 39, 154–164. [Google Scholar] [CrossRef] [PubMed]
- Pouliot, A.; Elmahboubi, R.; Adam, C. Incidence and Outcomes of Gestational Diabetes Mellitus Using the New International Association of Diabetes in Pregnancy Study Group Criteria in Hopital Maisonneuve-Rosemont. Canadian journal of diabetes. 2019, 43, 594–599. [Google Scholar] [CrossRef] [PubMed]
- Lennestal, R.; Otterblad Olausson, P.; Kallen, B. Maternal use of antihypertensive drugs in early pregnancy and delivery outcome, notably the presence of congenital heart defects in the infants. European journal of clinical pharmacology. 2009, 65, 615–625. [Google Scholar] [CrossRef] [PubMed]
- Ramezani Tehrani, F.; Rahmati, M.; Farzadfar, F.; Abedini, M.; Farahmand, M.; Hosseinpanah, F.; Hadaegh, F.; Torkestani, F.; Valizadeh, M.; Azizi, F.; Behboudi-Gandevani, S. One-step versus two-step screening for diagnosis of gestational diabetes mellitus in Iranian population: A randomized community trial. Frontiers in endocrinology 2022, 13, 1039643. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Zera, C.A.; Seely, E.W. Controversies in Gestational Diabetes. TouchREVIEWS in endocrinology. 2021, 17, 102–107. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Saccone, G.; Khalifeh, A.; Al-Kouatly, H.B.; Sendek, K.; Berghella, V. Screening for gestational diabetes mellitus: one step versus two step approach. A meta-analysis of randomized trials. The journal of maternal-fetal & neonatal medicine : the official journal of the European Association of Perinatal Medicine, the Federation of Asia and Oceania Perinatal Societies, the International Society of Perinatal Obstet. 2020, 33, 1616–1624. [Google Scholar] [CrossRef] [PubMed]
- Khalifeh, A.; Eckler, R.; Felder, L.; Saccone, G.; Caissutti, C.; Berghella, V. One-step versus two-step diagnostic testing for gestational diabetes: a randomized controlled trial. The journal of maternal-fetal & neonatal medicine : the official journal of the European Association of Perinatal Medicine, the Federation of Asia and Oceania Perinatal Societies, the International Society of Perinatal Obstet. 2020, 33, 612–617. [Google Scholar] [CrossRef] [PubMed]
- Brown, F.M.; Wyckoff, J. Application of One-Step IADPSG Versus Two-Step Diagnostic Criteria for Gestational Diabetes in the Real World: Impact on Health Services, Clinical Care, and Outcomes. Current diabetes reports. 2017, 17, 85. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Sevket, O.; Ates, S.; Uysal, O.; Molla, T.; Dansuk, R.; Kelekci, S. To evaluate the prevalence and clinical outcomes using a one-step method versus a two-step method to screen gestational diabetes mellitus. The journal of maternal-fetal & neonatal medicine : the official journal of the European Association of Perinatal Medicine, the Federation of Asia and Oceania Perinatal Societies, the International Society of Perinatal Obstet. 2014, 27, 36–41. [Google Scholar] [CrossRef] [PubMed]
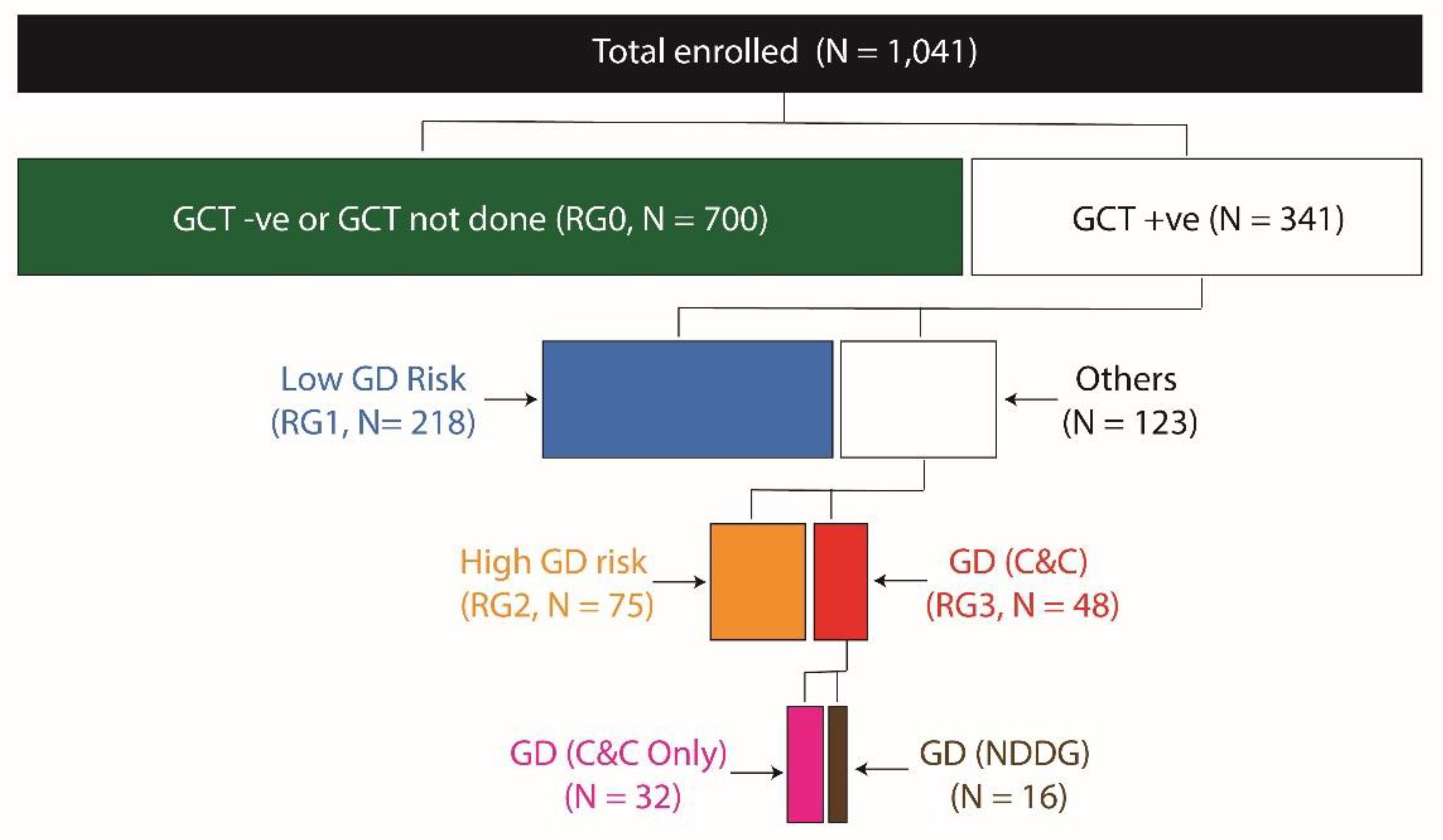
| Characteristic | GD Risk group | P | |||
| 0 | 1 | 2 | 3 | ||
| (n = 700) | (n = 218) | (n = 75) | (n = 48) | ||
| Enrollment characteristics | |||||
| Maternal age at enrollment | 25.08 (0.15) | 25.85 (0.27) | 25.91 (0.56) | 27.56 (0.58) | 0.0001 |
| Gestational age at enrollment | 16.25 (0.11) | 16.17 (0.19) | 15.47 (0.38) | 15.76 (0.46) | 0.2204 |
| Singleton pregnancy | 688 (98.29) | 212 (97.25) | 75 (100.00) | 47 (97.92) | 0.4742 |
| Demographics | |||||
| Maternal education | 0.1490 | ||||
| Never schooled / kindergarten only | 5 (0.72) | 2 (0.92) | 2 (2.67) | 2 (4.17) | |
| Class 1-8 | 109 (15.62) | 39 (17.89) | 16 (21.33) | 4 (8.33) | |
| Class 9-10 | 235 (33.67) | 78 (35.78) | 24 (32.00) | 13 (27.08) | |
| Class 11-12 | 194 (27.79) | 54 (24.77) | 20 (26.67) | 17 (35.42) | |
| College 1-3 years | 106 (15.19) | 35 (16.06) | 11 (14.67) | 6 (12.50) | |
| College >3 years | 35 (5.01) | 8 (3.67) | 2 (2.67) | 6 (12.50) | |
| Degree / Masters | 14 (2.01) | 2 (0.92) | 0 (0.00) | 0 (0.00) | |
| Family income | 0.0228 | ||||
| INR <100,000 per annum | 287 (41.41) | 84 (39.25) | 31 (41.47) | 23 (48.94) | |
| INR 100,000-<200,000 per annum | 312 (45.02) | 102 (47.66) | 29 (39.73) | 12 (25.33) | |
| INR 200,000-<300,000 per annum | 68 (9.81) | 26 (12.15) | 8 (10.96) | 8 (17.02) | |
| INR 300,000-<400,000 per annum | 20 (2.89) | 1 (0.47) | 3 (4.11) | 2 (4.26) | |
| INR 400,000-<600,000 per annum | 4 (0.58) | 0 (0.00) | 2 (2.74) | 1 (2.13) | |
| INR 600,000-<1,000,000 per annum | 1 (0.14) | 1 (0.47) | 0 (0.00) | 0 (0.00) | |
| INR >=1,000,000 per annum | 1 (0.14) | 0 (0.00) | 0 (0.00) | 1 (2.13) | |
| Caste | 0.0752 | ||||
| Open | 205 (29.33) | 70 (32.11) | 33 (44.00) | 22 (45.83) | |
| Other backward classes | 244 (34.91) | 78 (35.78) | 24 (32.00) | 14 (29.17) | |
| Scheduled caste | 166 (23.75) | 42 (19.27) | 13 (17.33) | 4 (8.33) | |
| Scheduled tribe | 33 (4.72) | 15 (6.88) | 2 (2.67) | 4 (8.33) | |
| Nomadic tribe / Vimukta Jaati | 29 (4.15) | 8 (3.67) | 2 (2.67) | 4 (8.33) | |
| Other | 22 (3.15) | 5 (2.29) | 1 (1.33) | 0 (0.00) | |
| Religion | 0.1956 | ||||
| Hindu | 427 (61.17) | 136 (62.67) | 41 (54.67) | 26 (54.17) | |
| Buddhist | 123 (17.62) | 34 (15.67) | 12 (16.00) | 4 (8.33) | |
| Muslim | 145 (20.77) | 44 (20.28) | 22 (29.33) | 18 (37.50) | |
| Sikh | 3 (0.43) | 1 (0.46) | 0 (0.00) | 0 (0.00) | |
| Christian | 0 (0.00) | 1 (0.46) | 0 (0.00) | 0 (0.00) | |
| Other | 0 (0.00) | 1 (0.46) | 0 (0.00) | 0 (0.00) | |
| Obstetric history | |||||
| Previous pregnancies | 0.2560 | ||||
| 0 | 316 (45.21) | 98 (44.95) | 43 (57.33) | 22 (45.83) | |
| 1 | 251 (35.91) | 67 (30.73) | 18 (24.00) | 15 (31.25) | |
| 2 | 105 (15.02) | 39 (17.89) | 8 (10.67) | 10 (20.83) | |
| 3 | 20 (2.86) | 12 (5.50) | 4 (5.33) | 1 (2.08) | |
| 4 | 5 (0.72) | 1 (0.46) | 1 (1.33) | 0 (0.00) | |
| 5 | 2 (0.29) | 0 (0.00) | 1 (1.33) | 0 (0.00) | |
| 6 | 0 (0.00) | 1 (0.46) | 0 (0.00) | 0 (0.00) | |
| Previous livebirths | 0.6558 | ||||
| 0 | 68 (17.75) | 20 (16.67) | 7 (21.88) | 6 (23.08) | |
| 1 | 265 (69.19) | 84 (70.00) | 19 (59.38) | 14 (53.85) | |
| 2 | 44 (11.19) | 15 (12.50) | 6 (18.75) | 6 (23.08) | |
| 3 | 6 (1.57) | 1 (0.83) | 0 (0.00) | 0 (0.00) | |
| Previous cesarean section | 102 (14.57) | 35 (16.06) | 12 (16.00) | 7 (14.58) | 0.9490 |
| Body mass index (Kg/m2) | 21.31 (0.14) | 21.51 (0.30) | 22.18 (0.45) | 23.66 (0.70) | 0.0010 |
| Obesity (BMI≥27.5 Kg/m2) | 45 (6.43) | 19 (8.72) | 8 (10.67) | 11 (22.92) | 0.0005 |
| Blood pressure | |||||
| Systolic (mmHg) | 100.63 (0.31) | 103.30 (0.55) | 102.74 (0.99) | 105.70 (1.50) | 4.40x10-6 |
| Diastolic (mmHg) | 63.24 (0.23) | 65.61 (0.44) | 65.58 (0.80) | 66.99 (1.07) | 3.38x10-8 |
| Pulse pressure (mmHg) | 37.43 (0.22) | 37.69 (0.40) | 37.75 (0.72) | 37.77 (0.93) | 0.8629 |
| Mean arterial pressure (mmHg) | 75.68 (0.24) | 78.17 (0.44) | 77.57 (0.75) | 80.52 (1.19) | 1.48x10-8 |
| Hypertension | 7 (1.01) | 7 (3.21) | 1 (1.35) | 3 (6.25) | 0.0133 |
| Blood lipid profile | |||||
| Total serum cholesterol (mg/dl) | 157.07 (1.21) | 162.39 (2.17) | 159.72 (3.73) | 163.19 (4.27) | 0.1133 |
| Serum triglycerides (mg/dl) | 104.83 (1.80) | 112.13 (2.67) | 114.15 (5.84) | 125.88 (5.91) | 0.0001 |
| Serum high density lipoprotein (mg/dl) | 50.90 (0.34) | 50.25 (0.59) | 48.35 (0.92) | 50.77 (1.30) | 0.1423 |
| Serum low density lipoprotein (mg/dl) | 85.21 (1.06) | 89.71 (1.94) | 88.54 (3.21) | 87.24 (3.78) | 0.2076 |
| Serum very low density lipoprotein (mg/dl) | 20.97 (0.36) | 22.43 (0.53) | 22.83 (1.17) | 25.18 (1.18) | 0.0001 |
| Characteristic | GD Risk group | P | |||
| 0 | 1 | 2 | 3 | ||
| (n = 700) | (n = 218) | (n = 75) | (n = 48) | ||
| Dietary characteristics | |||||
| Total calories (Kcal/d) | 1510.26 (28.75) | 1489.70 (42.63) | 1419.60 (69.90) | 1560.37 (83.98) | 0.4785 |
| Total proteins (g/d) | 50.47 (1.29) | 53.04 (2.51) | 50.00 (4.54) | 56.49 (5.29) | 0.5188 |
| Total carbohydrates (g/d) | 220.91 (3.48) | 214.90 (5.39) | 203.73 (8.58) | 222.68 (11.91) | 0.5581 |
| Total fats (g/d) | 46.19 (1.50) | 45.33 (2.11) | 44.02 (3.30) | 47.70 (3.28) | 0.1557 |
| Total dietary fiber (g/d) | 7.14 (0.20) | 6.63 (0.29) | 6.53 (0.46) | 7.81 (0.61) | 0.1258 |
| Dietary iron (mg/d) | 15.41 (0.31) | 13.89 (0.48) | 14.25 (0.81) | 16.92 (1.07) | 0.0136 |
| Dietary calcium (mg/d) | 482.24 (10.29) | 473.98 (16.71) | 485.82 (28.45) | 548.71 (50.73) | 0.5046 |
| Water intake (L/d) | 1.13 (0.02) | 1.16 (0.04) | 1.11 (0.06) | 1.09 (0.06) | 0.9137 |
| Physical activity (per week) | |||||
| Total METs | 59.22 (0.88) | 57.42 (1.41) | 56.71 (1.84) | 56.31 (2.83) | 0.5037 |
| Sedentary METs | 1.18 (0.07) | 1.02 (0.12) | 0.84 (0.13) | 1.26 (0.24) | 0.3199 |
| Light intensity activity METs | 49.73 (0.62) | 48.44 (1.03) | 49.53 (1.52) | 48.64 (2.21) | 0.7153 |
| Moderate intensity activity METs | 8.29 (0.37) | 7.95 (0.58) | 6.35 (0.52) | 6.41 (0.99) | 0.5379 |
| Vigourous intensity activity METs | 0.02 (0.01) | 0.01 (0.01) | 0.00 (0.00) | 0.00 (0.00) | 0.6339 |
| Household/ caregiving activity METs | 55.65 (0.84) | 54.06 (1.38) | 53.65 (1.78) | 52.67 (2.67) | 0.5665 |
| Occupational activity METs | 0.04 (0.02) | 0.10 (0.05) | 0.00 (0.00) | 0.00 (0.00) | 0.2556 |
| Sports activity METs | 1.14 (0.04) | 1.11 (0.06) | 1.07 (0.10) | 1.20 (0.13) | 0.9246 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




