Submitted:
21 August 2025
Posted:
22 August 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
1.1. Population Segmentation in Health & Healthcare Systems
1.2. International Context
1.3. Local Context
1.4. Care Model Implications for Health System Population Segmentation Models
1.5. Systemic Health System Population Segmentation—Singapore Case Study
- Introduce a novel Systemic Health System Population Segmentation Model approach that is person-centred and needs-based to enable health system redesign.
- Describe the Lifelong Care Segmentation and Sub-segmentation Models for the macrosystem and mesosystem levels of the Service Delivery System of a health system, based on the UCM.
- Describe the Episodic Care Segmentation Model for the mesosystem and microsystem levels of the Service Delivery System of a health system, based on the UCM.
- Illustrate the development process and evaluation results of these models.
2. Materials and Methods
2.1. Lifelong Care Segmentation (LS) Model Development
2.2. Further Needs-Based Sub-Segmentation Model (NBSSM) Development
2.3. Episodic Care Segmentation (ES) Model Development
2.4. Health System Population Segmentation Model Evaluation
3. Results
4. Discussion
5. Conclusions
Author Contributions
Acknowledgments
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Lynn, J. Using Population Segmentation to Provide Better Health Care for All: The “Bridges to Health” Model. The Milbank Quaterly 2007, 85, 185–208. [Google Scholar] [CrossRef]
- Vuil, S.I. Patient Segmentation Analysis Offeres Significant Benefits For Integrated Care And Support. Health Affaires. 2016, 35, 769–775. [Google Scholar]
- Chong, J.L. Do healthcare needs-based population segments predict outcomes among the elderly? Findings from a prospective cohort study in an urbabized low-income community. BMC Geriatrics. 2020, 20, 78. [Google Scholar] [CrossRef]
- Chong, J.L. Population Segmentation Based on Healthcare Needs: Validation of a Brief Clinician-Administered Tool. Society of General Internal Medicine 2020, 36, 9–16. [Google Scholar] [CrossRef]
- Suzman, R. Health in an ageing world--what do we know? Lancet. 2015, 385, 484–486. [Google Scholar] [CrossRef]
- Laberge, M. Population-based integrated care funding values and guiding principles: An empirical qualitative study. Heliyon. 2024, 10, e24904. [Google Scholar] [CrossRef]
- Beck da Silva Etges, A.P. Value-Based Reimbursement as a Mechanism to Achieve Social and Financial Impact in the Healthcare System. Journal of Health Economics and Outcomes Research. 2023, 10, 100–103. [Google Scholar] [CrossRef]
- Low, L.L. Assessing the validity of a data driven segmentation approach: A 4 year longitudinal study of healthcare utilization and mortality. PLoS ONE. 2018, 13, e0195243. [Google Scholar] [CrossRef]
- Balkrishnan, R. Capitation Payment, Length of Visit, and Preventive Services: Evidence From a National Sample of Outpatient Physicians. The American Journal of Managed Care. 2002, 8, 332–340. [Google Scholar]
- Teo, K.W. Health System Transformation Playbook & Yishun Health Unified Care Model: A Design, System and Complexity Thinking Enabled Approach to Health System and Services Transformation. 2022.
- Yan, S. A systematic review of the clinical application of data-driven population segmentation analysis. BMC Medical Research Methodology. 2018, 18, 121. [Google Scholar] [CrossRef]
- Mead, N. Patient-centredness: a conceptual framework and review of the empirical literature. Soc Sci Med. 2000, 51, 1087–1110. [Google Scholar] [CrossRef]
- Coulter, A. Person-centred care: what is it and how do we get there? Future Hospital Journal 2016, 3, 114–116. [Google Scholar] [CrossRef]
- Low, L.L. Evaluation of a pratical expert defined approach to patient population segmentation: a case study in Singapore. BMC Health Service Research. 2017, 17, 771. [Google Scholar] [CrossRef]
- NationaL Healthare Group. River of Life: NHG’s Perspectives on Population Health.; National Healthcare Group Pte Ltd.: Singapore, 2019. [Google Scholar]
- Ravaghi, H. A scoping review of community health needs and assets assessment: concepts, rationale, tools and uses. BMC Health Services Research. 2023, 23, 44. [Google Scholar] [CrossRef]
- Engel, G.L. The Need for a New Medical Model: A Challenge for Biomedicine. Psychodynamic Psychiatry. 2012, 40, 377–396. [Google Scholar] [CrossRef]
- Department of Statistics. Population and Population Structure 2019. https://www.singstat.gov.sg/find-data/search-by-theme/population/population-and-population-structure/latest-data. Accessed 17/11/2022.
- Arnetz, B.B. Enhancing healthcare efficiency to achieve the Quadruple Aim: an exploratory study. BMC Research Notes. 2020, 13, 362. [Google Scholar] [CrossRef]
- Bodenheimer, T. From Triple to Quadruple Aim: Care of the Patient Requires Care of the Provider. Annuals of Family Medicine. 2014, 12, 573–576. [Google Scholar] [CrossRef]
- Gibbs, J.F. Value-based focused global population health management. Journal of Gastrointestingal Oncology. 2021, 12 (Suppl 2), S275–S289. [Google Scholar] [CrossRef]
- Stevens, E.R. Measuring Population Health in a Large Integrated Health System to Guide Goal Setting and Resource Allocation: A Proof of Concept. Population Health Management. 2019, 22, 385–393. [Google Scholar] [CrossRef]
- Parrish, R.G. Measuring Population Health Outcomes. Precenting Chronic Disease Public Health Research, Practice, and Policy. 2010, 7. [Google Scholar]
- Kruse, C.S. The use of Electronic Health Records to Support Population Health: A Systematic Review of the Literature. Journal of Medical Systems. 2018, 42, 214. [Google Scholar] [CrossRef]
- Charlson, M.E. Charlson Comorbidity Index: A Critical Review of Clinimetric Properties. Psychother Psychosom. 2022, 8–35. [Google Scholar] [CrossRef]
- Yan, S. A systematic review of the clinical application of data-driven population segmentation analysis. BMC Med Res Methodol. 2018, 18, 121. [Google Scholar] [CrossRef]
- Choon, J.L. Population segmentation based on healthcare needs: a systematic review. Syst Rev. 2019, 8, 202. [Google Scholar] [CrossRef]
- Ekman, I. Person-Centered Care—Ready for Prime Time. European Journal of Cardiovascular Nursing. 2011, 248–251. [Google Scholar] [CrossRef]
- Hewner, S. Aligning population-based care management with chronic disease complexity. Nurs Outlook. 2014, 62, 250–258. [Google Scholar] [CrossRef]
- Hall, M.A. Liability Implications of Physician-Directed Care Coordination. Annals of Family Medicine. 2005, 3, 115–121. [Google Scholar] [CrossRef]
| Disease Description | ICD-10 | Disease Description | ICD-10 |
|---|---|---|---|
| Chronic liver disease | B18, K70-K77, Z94 | Cancer | C00-C75 |
| Solid tumor | C76-C80 | Lymphoma | C81-C90, C96 |
| Leukaemia | C91-C95 | Diabetes | E10-E14, O24 |
| Hyperlipidemia | E78 | Dementia | F00-F03 |
| Schizophrenia | F20 | Bipolar | F30-F31 |
| Depression | F32-F34, F38-F39 | Anxiety | F40-F45 |
| Paraplegia | G04, G11 | Parkinson | G20 |
| Alzheimer’s disease | G30 | Epilepsy | G40-G41 |
| Transient ischemic attacks | G45, I65-I66 | Stroke | G46 |
| Paraplegia | G81-G83 | Visual impairment | H53-H54, Z44, Z97 |
| Hearing impairment | H90-H91, Q16 | Hypertension | I10-I13, I15, O10-011 |
| Ischemic heart disease | I20-I25 | Atrial Fibrillation | I48 |
| Heart failure | I50 | Stroke | I60-I64, I67, I69 |
| Peripheral vascular disease | I70-I74, I77, I79 | COPD | J41-J44 |
| Asthma | J45-J46 | Peptic ulcer disease | K25-K28 |
| Psoriasis | L40 | Rheumatoid arthritis | M05-M06, M08 |
| Osteoarthritis | M15-M19 | Connective tissue | M30-M36 |
| Osteoporosis | M80-M82 | Nephritis | N02-N08, N11, N14-16 |
| Renal failure | N18-N19, N25, Z49, Z99 | Hyperplasia of prostate | N40 |
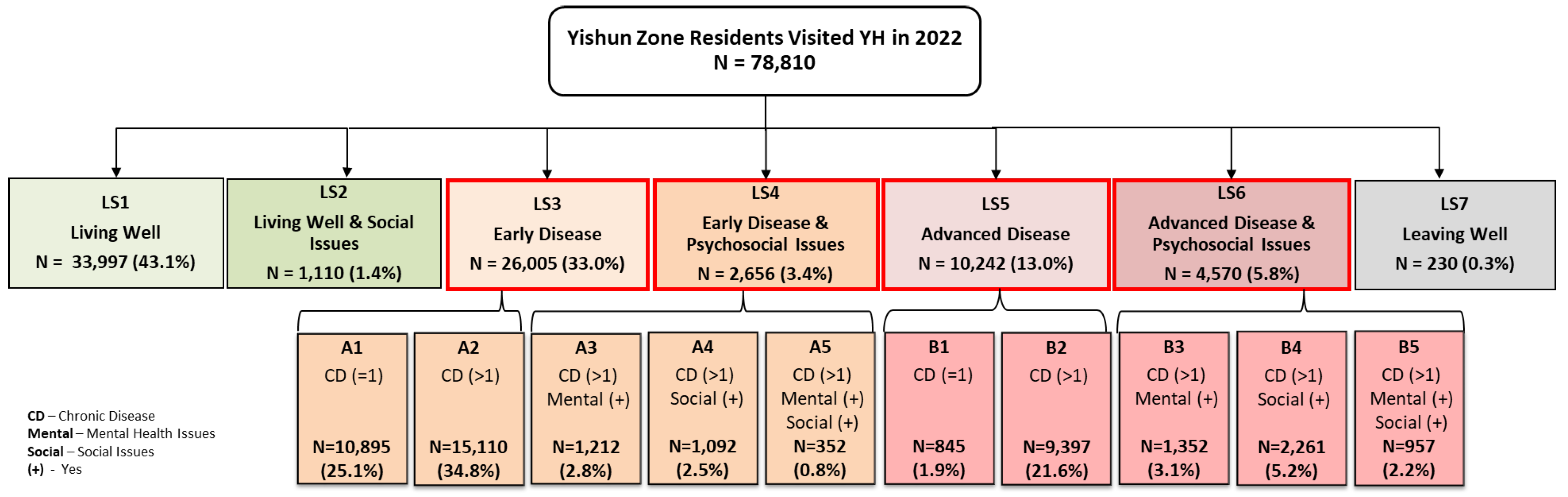
| A: Early Disease | B: Advanced Disease | ||
|---|---|---|---|
| 1 | Single Chronic Disease or Frail only |
A1)
|
B1)
|
| 2 | Multiple Chronic Diseases |
A2)
|
B2)
|
| 3 | Multiple Chronic Disease + Mental Issues |
A3)
|
B3)
|
| 4 | Multiple Chronic Diseases + Social Issues |
A4)
|
B4)
|
| 5 | Multiple Chronic Illness + Mental + Social Issues |
A5)
|
B5)
|
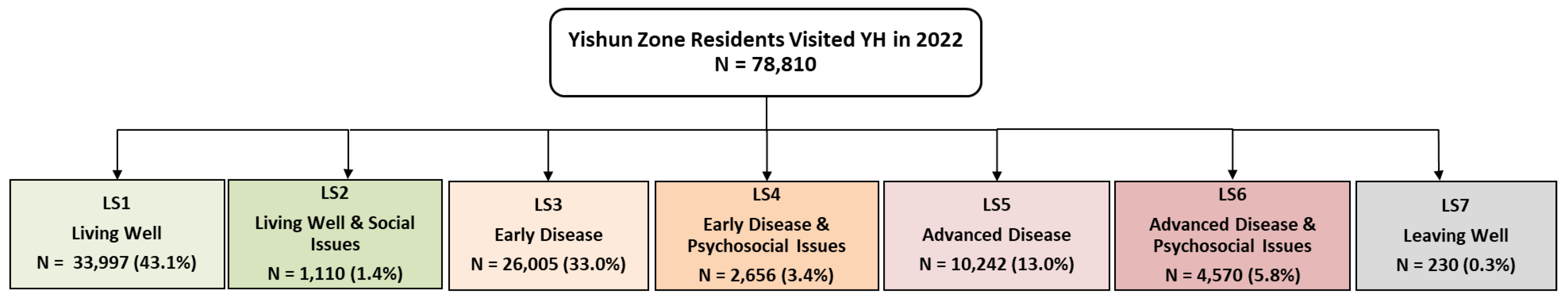
| LS1 | LS2 | LS3 | LS4 | LS5 | LS6 | LS7 | P-value | |
|---|---|---|---|---|---|---|---|---|
|
Mean Age (Years) |
38.9 | 37.2 | 56.7 | 61.4 | 63.7 | 67.6 | 76.9 | <0.001 |
| Gender | ||||||||
| Female % | 49.3% | 49.9% | 50.3% | 56.9% | 44.6% | 49.6% | 46.7% | <0.001 |
| Ethnicity | ||||||||
| Chinese, % | 59.9% | 30.3% | 68.8% | 65.9% | 62.2% | 60.6% | 69.6% | <0.001 |
| Malay, % | 11.5% | 39.0% | 11.9% | 16.3% | 16.5% | 18.8% | 13.1% | |
| Indian, % | 11.9% | 14.5% | 10.5% | 10.7% | 13.3% | 12.7% | 7.0% | |
| Others, % | 16.7% | 16.2% | 8.8% | 7.1% | 8.0% | 7.9% | 10.3% | |
| Average CCI score | 0.4 | 0.4 | 2.2 | 3.1 | 5.1 | 6.4 | 8.8 | <0.001 |
| A1 | A2 | A3 | A4 | A5 | B1 | B2 | B3 | B4 | B5 | P-value | |
|
Mean Age (Years) |
49.3 | 62.1 | 58.2 | 63.5 | 65.4 | 47.0 | 65.2 | 68.6 | 65.2 | 71.6 | <0.001 |
| Gender | |||||||||||
| Female % | 52.6% | 48.4% | 57.1% | 51.4% | 65.3% | 48.3% | 43.9% | 57.9% | 42.5% | 54.4% | <0.001 |
| Ethnicity | |||||||||||
| Chinese, % | 65.5% | 71.9% | 72.4% | 58.5% | 67.3% | 56.6% | 62.9% | 68.7% | 53.6% | 64.6% | <0.001 |
| Malay, % | 13.0% | 11.0% | 10.5% | 22.1% | 13.1% | 17.5% | 16.0% | 11.1% | 24.8% | 15.4% | |
| Indian, % | 11.0% | 10.0% | 9.8% | 11.8% | 12.5% | 13.4% | 13.7% | 13.6% | 12.7% | 14.2% | |
| Others, % | 10.5% | 7.0% | 7.3% | 7.6% | 7.1% | 12.5% | 7.3% | 6.6% | 8.9% | 5.9% | |
| Average CCI score | 1.2 | 2.9 | 2.7 | 3.3 | 3.7 | 1.8 | 5.4 | 6.1 | 6.2 | 7.3 | <0.001 |
| A1 | A2 | A3 | A4 | A5 | B1 | B2 | B3 | B4 | B5 | P-value | |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Average No. of ED visits | 0.6 | 0.4 | 0.9 | 0.9 | 1.6 | 0.7 | 0.7 | 1.3 | 1.1 | 2.1 | <0.001 |
| Average No. of SOC visits | 2.0 | 2.7 | 3.0 | 3.5 | 3.7 | 2.6 | 3.4 | 3.5 | 4.9 | 4.8 | <0.001 |
| Average No. of inpatient admission | 0.3 | 0.4 | 0.5 | 0.7 | 1.0 | 0.6 | 0.7 | 1.1 | 1.3 | 2.0 | <0.001 |
| Average annual hospitalization bed days | 0.7 | 0.8 | 2.3 | 4.8 | 9.5 | 2.8 | 2.7 | 8.1 | 9.9 | 22.6 | <0.001 |
| Average annual overall healthcare cost (SGD) | $1,941 | $2,538 | $3,981 | $6,955 | $10,682 | $5,432 | $6,018 | $10,399 | $14,524 | $23,356 | <0.001 |
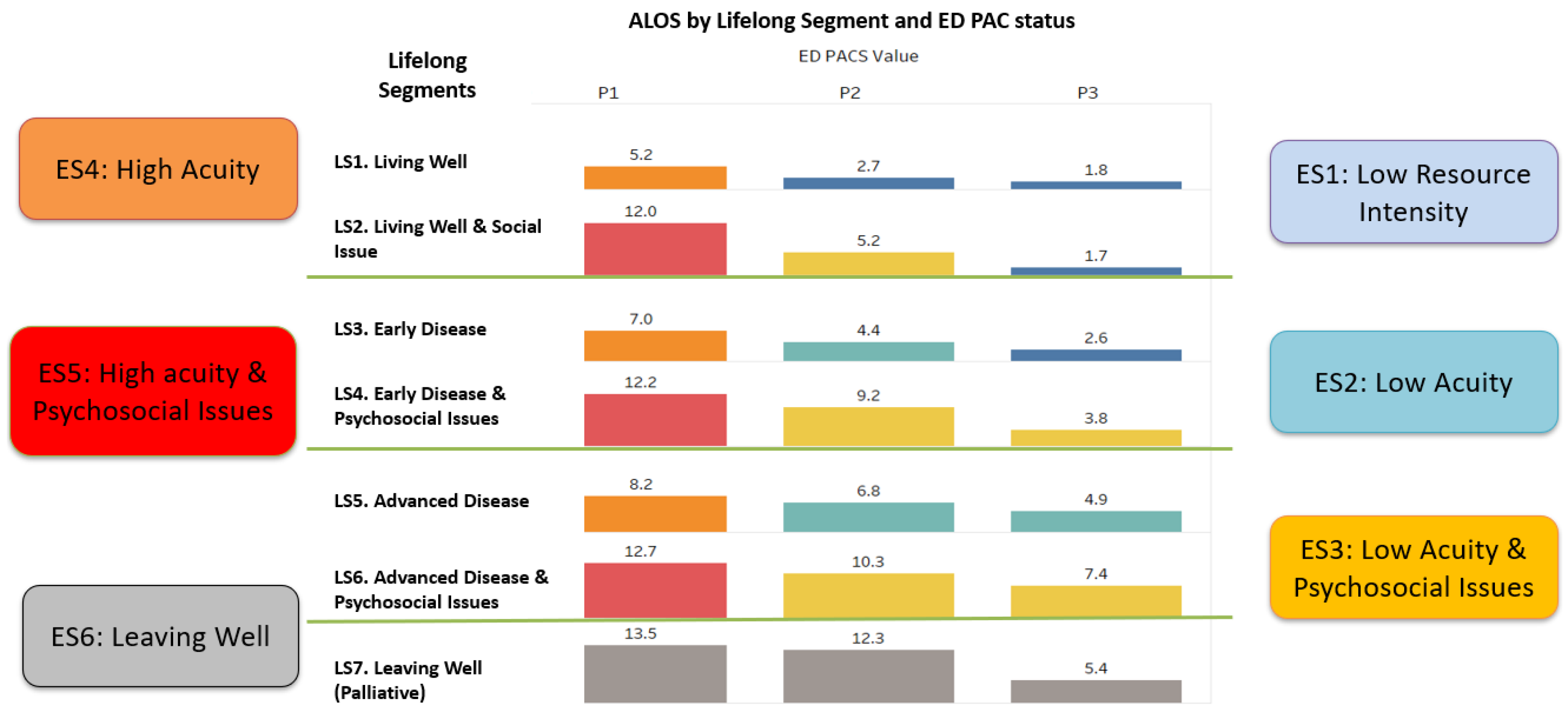
| ES1 | ES2 | ES3 | ES4 | ES5 | ES6 | P-value | |
|---|---|---|---|---|---|---|---|
|
Number of cases (%) |
1,966 (11.7%) |
5,807 (34.6%) |
4,215 (25.1%) |
1,274 (7.6%) |
722 (4.3%) |
351 (2.1%) |
|
| Average length of stay (Day) | 2.2 | 4.3 | 8.2 | 6.7 | 11.8 | 10.7 |
<0.001 |
| Average inpatient admission cost (SGD) | $3,283 | $5,571 | $8,384 | $14,314 | $17,298 | $10,655 | <0.001 |
| 30-day emergency readmission rate | 1.4% | 5.3% | 16.3% | 6.8% | 16.1% | 29.9% | <0.001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




