Submitted:
20 August 2025
Posted:
21 August 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
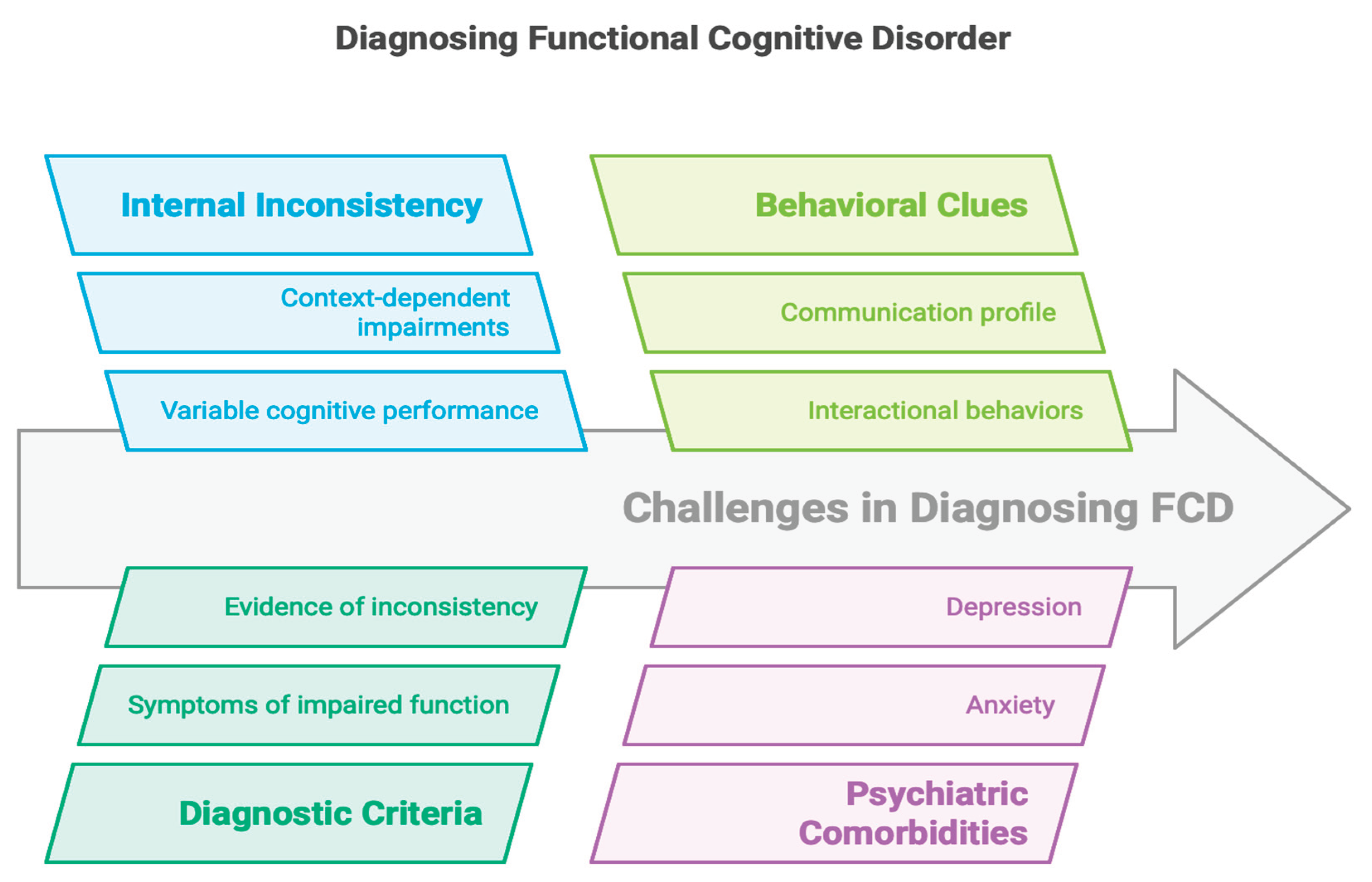
2. Definition and Diagnostic Challenges
3. Clinical Signs and Diagnostic Features
- One or more symptoms of impaired cognitive function;
- Evidence of internal inconsistency in performance;
- Symptoms not better explained by another medical, neurological, or psychiatric disorder;
- Symptoms that result in significant distress, impairment, or warrant clinical attention.
4. Communication Patterns and Interactional Profiles
- Longer response duration: In a study by Teodoro et al. [32], individuals with FCD spoke for a median of 124 seconds when describing their cognitive concerns, significantly longer than the 42 seconds observed in patients with neurodegenerative disorders. This verbosity may reflect intact working memory and linguistic fluency, characteristics inconsistent with progressive dementia.
- “Attending alone” behavior: A notable feature in FCD populations is the tendency to arrive unaccompanied at clinical appointments. These patients often bring written summaries or bullet-pointed notes detailing their concerns, behaviors seldom observed in individuals with dementia, who are frequently accompanied by family members who provide collateral information and support [1,12].
- Absence of the “head-turning sign”: In neurodegenerative conditions, patients often glance toward caregivers for reassurance or help during cognitive testing, a behavior that is rare in FCD, further reinforcing the functional, rather than organic, nature of their symptoms [28].
5. Metacognition and Psychological Factors
- Impaired metacognitive ability: Patients with FCD often overestimate their cognitive deficits, even in the context of normal or near-normal neuropsychological test results. They may misattribute benign lapses to serious dysfunction, due in part to poor calibration between subjective experiences and objective performance [1,16].
- Negative interpretation bias: Individuals with FCD may selectively attend to episodes of forgetfulness and interpret them as signs of progressive brain disease, reinforcing anxiety and worry [16]
- Memory-related anxiety and societal expectations: Cultural narratives and personal beliefs about aging or family history of dementia can exacerbate memory-related fears. Many patients report assuming that cognitive decline is inevitable, thereby interpreting normal lapses as harbingers of irreversible decline [32].
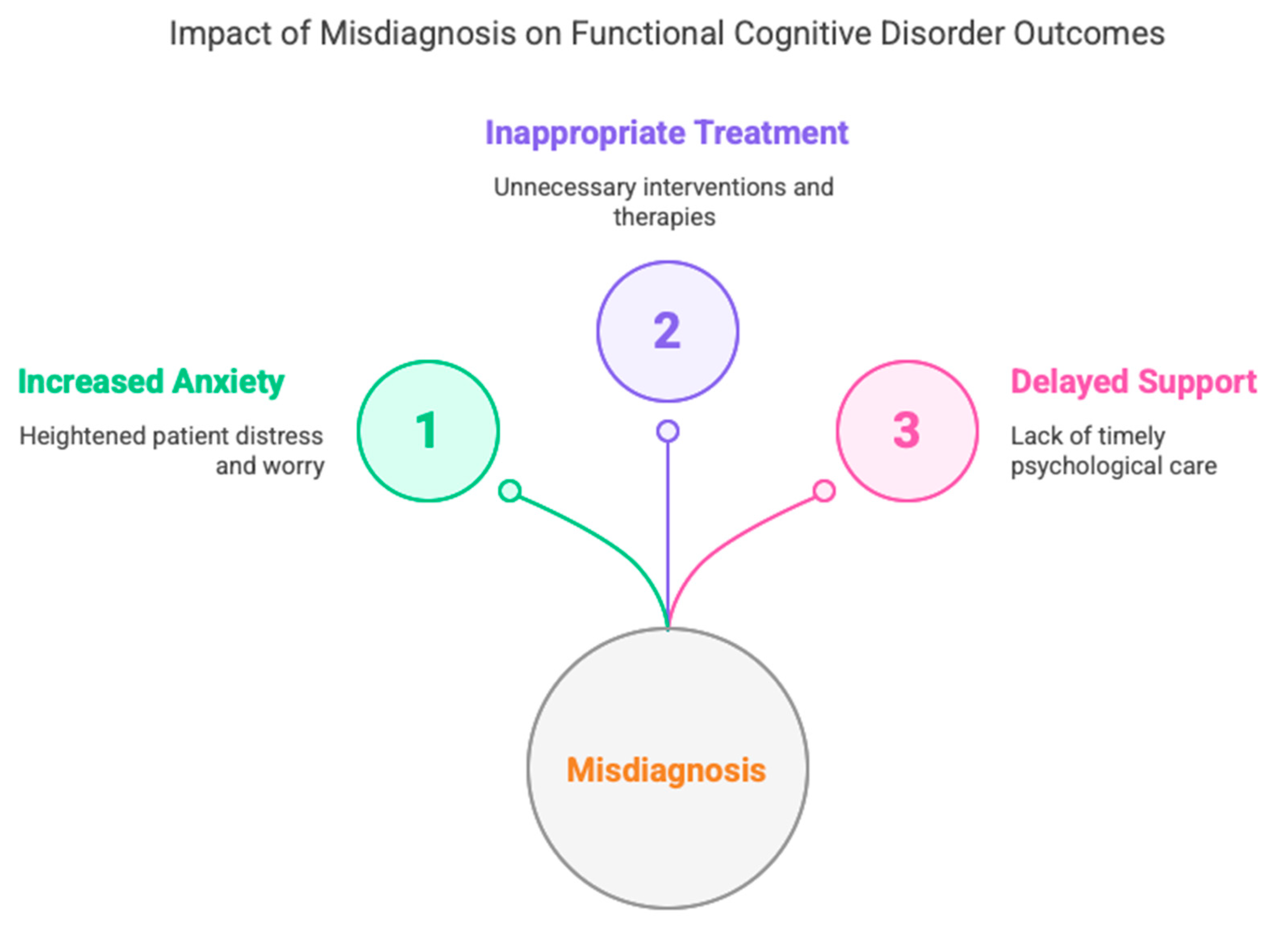
6. Long-Term Outcomes
7. Assessment Methods
7.1. Neuropsychological Testing
7.2. Cognitive Screening Instruments
7.3. Medical Symptom Validity Tests (MSVT)
7.4. Structured Questionnaires
7.5. Interactional and Conversational Assessment
7.6. Mini International Neuropsychiatric Interview
7.7. The Schmidtke Criteria
8. Related Concepts and Differential Diagnosis
8.1. Subjective Cognitive Decline
8.2. Pseudodementia
8.3.“Worried Well”
8.4. Cogniform Disorder
8.5. Functional Neurological Disorder
9. Conclusion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
Abbreviations
| PHQ-15 | Patient Health Questionnaire-15 |
| HADS | Hospital Anxiety and Depression Scale |
| PSQI | Pittsburgh Sleep Quality Index |
| MMQ | Multifactorial Memory Questionnaire |
| FCD | Functional Cognitive Disorder |
References
- Ball, H.A.; McWhirter, L.; Ballard, C.; Bhome, R.; Blackburn, D.J.; Edwards, M.J.; Fleming, S.M.; Fox, N.C.; Howard, R.; Huntley, J.; et al. Functional Cognitive Disorder: Dementia’s Blind Spot. Brain 2020, 143. [Google Scholar] [CrossRef]
- Poole, N.A.; Cope, S.R.; Bailey, C.; Isaacs, J.D. Functional Cognitive Disorders: Identification and Management. BJPsych Adv 2019, 25, 342–350. [Google Scholar] [CrossRef]
- Stone, J.; Pal, S.; Blackburn, D.; Reuber, M.; Thekkumpurath, P.; Carson, A. Functional (Psychogenic) Cognitive Disorders: A Perspective from the Neurology Clinic. Journal of Alzheimer’s Disease 2015, 48. [Google Scholar] [CrossRef] [PubMed]
- Marín-Medina, D.S.; Arenas-Vargas, P.A.; del Pilar Velásquez-Duque, M.; Bagnati, P.M. Functional Cognitive Disorder: Beyond Pseudodementia. Neurology Perspectives 2025, 5, 100179. [Google Scholar] [CrossRef]
- Pennington, C.; Ball, H.; Swirski, M. Functional Cognitive Disorder: Diagnostic Challenges and Future Directions. Diagnostics 2019, 9. [Google Scholar] [CrossRef]
- Cabreira, V.; Frostholm, L.; McWhirter, L.; Stone, J.; Carson, A. Clinical Signs in Functional Cognitive Disorders: A Systematic Review and Diagnostic Meta-Analysis. J Psychosom Res 2023, 173, 111447. [Google Scholar] [CrossRef]
- Bailey, C.; Bell, S.M.; Blackburn, D.M. How the UK Describes Functional Memory Symptoms. Psychogeriatrics 2017, 17. [Google Scholar] [CrossRef]
- Jessen, F.; Amariglio, R.E.; Van Boxtel, M.; Breteler, M.; Ceccaldi, M.; Chételat, G.; Dubois, B.; Dufouil, C.; Ellis, K.A.; Van Der Flier, W.M.; et al. A Conceptual Framework for Research on Subjective Cognitive Decline in Preclinical Alzheimer’s Disease. Alzheimer’s and Dementia 2014, 10. [Google Scholar] [CrossRef] [PubMed]
- Rahman-Filipiak, A.M.; Giordani, B.; Heidebrink, J.; Bhaumik, A.; Hampstead, B.M. Self- and Informant-Reported Memory Complaints: Frequency and Severity in Cognitively Intact Individuals and Those with Mild Cognitive Impairment and Neurodegenerative Dementias. Journal of Alzheimer’s Disease 2018, 65. [Google Scholar] [CrossRef]
- Pennington, C.; Newson, M.; Hayre, A.; Coulthard, E. Functional Cognitive Disorder: What Is It and What to Do about It? Pract Neurol 2015, 15, 436–444. [Google Scholar] [CrossRef] [PubMed]
- Cabreira, V.; McWhirter, L.; Carson, A. Functional Cognitive Disorder: Diagnosis, Treatment, and Differentiation from Secondary Causes of Cognitive Difficulties. Neurol Clin 2023, 41, 619–633. [Google Scholar] [CrossRef]
- Reuber, M.; Blackburn, D.J.; Elsey, C.; Wakefield, S.; Ardern, K.A.; Harkness, K.; Venneri, A.; Jones, D.; Shaw, C.; Drew, P. An Interactional Profile to Assist the Differential Diagnosis of Neurodegenerative and Functional Memory Disorders. Alzheimer Dis Assoc Disord 2018, 32. [Google Scholar] [CrossRef]
- Bharambe, V.; Larner, A.J. Functional Cognitive Disorders: Demographic and Clinical Features Contribute to a Positive Diagnosis. Neurodegener Dis Manag 2018, 8. [Google Scholar] [CrossRef]
- McWhirter, L.; Ritchie, C.; Stone, J.; Carson, A. Identifying Functional Cognitive Disorder: A Proposed Diagnostic Risk Model. CNS Spectr 2022, 27, 754–763. [Google Scholar] [CrossRef] [PubMed]
- Teodoro, T.; Edwards, M.J.; Isaacs, J.D. A Unifying Theory for Cognitive Abnormalities in Functional Neurological Disorders, Fibromyalgia and Chronic Fatigue Syndrome: Systematic Review. J Neurol Neurosurg Psychiatry 2018, 89, 1308–1319. [Google Scholar] [CrossRef]
- Bhome, R.; McWilliams, A.; Price, G.; Poole, N.A.; Howard, R.J.; Fleming, S.M.; Huntley, J.D. Metacognition in Functional Cognitive Disorder. Brain Commun 2022, 4. [Google Scholar] [CrossRef]
- Laukaityte, U.; Laukaityte, U. The Scope of Functional Neurological Disorder: Symptom Perception, Inference, and Psychiatry 2024.
- Tamilson, B.; Poole, N.; Agrawal, N. The Co-Occurrence of Functional Neurological Disorder and Autism Spectrum Disorder: A Systematic Literature Review and Meta-Analysis. Cogn Neuropsychiatry 2025. [Google Scholar] [CrossRef] [PubMed]
- Kemp, S.; Kapur, N.; Graham, C.D.; Reuber, M. Functional Cognitive Disorder: Differential Diagnosis of Common Clinical Presentations. Archives of Clinical Neuropsychology 2022, 37. [Google Scholar] [CrossRef] [PubMed]
- Bhome, R.; McWilliams, A.; Huntley, J.D.; Fleming, S.M.; Howard, R.J. Metacognition in Functional Cognitive Disorder- a Potential Mechanism and Treatment Target. Cogn Neuropsychiatry 2019, 24, 311–321. [Google Scholar] [CrossRef]
- Wakefield, S.J.; Blackburn, D.J.; Harkness, K.; Khan, A.; Reuber, M.; Venneri, A. Distinctive Neuropsychological Profiles Differentiate Patients with Functional Memory Disorder from Patients with Amnestic-Mild Cognitive Impairment. Acta Neuropsychiatr 2018, 30. [Google Scholar] [CrossRef]
- Silverberg, N.D.; Rush, B.K. Neuropsychological Evaluation of Functional Cognitive Disorder: A Narrative Review. Clinical Neuropsychologist 2024, 38, 302–325. [Google Scholar] [CrossRef]
- Schmidtke, K.; Metternich, B. Validation of Two Inventories for the Diagnosis and Monitoring of Functional Memory Disorder. J Psychosom Res 2009, 67. [Google Scholar] [CrossRef]
- Poole, N.A.; Cope, S.R.; Bailey, C.; Isaacs, J.D. Functional Cognitive Disorders: Identification and Management. BJPsych Adv 2019, 25. [Google Scholar] [CrossRef]
- Sabbagh, M.N.; Boada, M.; Borson, S.; Chilukuri, M.; Dubois, B.; Ingram, J.; Iwata, A.; Porsteinsson, A.P.; Possin, K.L.; Rabinovici, G.D.; et al. Early Detection of Mild Cognitive Impairment (MCI) in Primary Care. Journal of Prevention of Alzheimer’s Disease 2020, 7, 165–170. [Google Scholar] [CrossRef]
- Edmonds, E.C.; Delano-Wood, L.; Galasko, D.R.; Salmon, D.P.; Bondi, M.W. Subjective Cognitive Complaints Contribute to Misdiagnosis of Mild Cognitive Impairment. Journal of the International Neuropsychological Society 2014, 20. [Google Scholar] [CrossRef] [PubMed]
- Voros, V.; Fekete, S.; Tenyi, T.; Rihmer, Z.; Szili, I.; Osvath, P. Untreated Depressive Symptoms Significantly Worsen Quality of Life in Old Age and May Lead to the Misdiagnosis of Dementia: A Cross-Sectional Study. Ann Gen Psychiatry 2020, 19. [Google Scholar] [CrossRef] [PubMed]
- Ghadiri–Sani, M.; Larner, A. Head turning sign for diagnosis of dementia and mild cognitive impairment: a revalidation. J Neurol Neurosurg Psychiatry 2013, 84. [Google Scholar] [CrossRef]
- Elsey, C.; Drew, P.; Jones, D.; Blackburn, D.; Wakefield, S.; Harkness, K.; Venneri, A.; Reuber, M. Towards Diagnostic Conversational Profiles of Patients Presenting with Dementia or Functional Memory Disorders to Memory Clinics. Patient Educ Couns 2015, 98. [Google Scholar] [CrossRef]
- Soysal, P.; Usarel, C.; Ispirli, G.; Isik, A.T. Attended with and Head-Turning Sign Can Be Clinical Markers of Cognitive Impairment in Older Adults. Int Psychogeriatr 2017, 29. [Google Scholar] [CrossRef]
- McWhirter, L.; Ritchie, C.; Stone, J.; Carson, A. Functional Cognitive Disorders: A Systematic Review. Lancet Psychiatry 2020, 7, 191–207. [Google Scholar] [CrossRef]
- Teodoro, T.; Koreki, A.; Chen, J.; Coebergh, J.; Poole, N.; Ferreira, J.J.; Edwards, M.J.; Isaacs, J.D. Functional Cognitive Disorder Affects Reaction Time, Subjective Mental Effort and Global Metacognition. Brain 2023, 146. [Google Scholar] [CrossRef] [PubMed]
- Mascherek, A.; Zimprich, D.; Rupprecht, R.; Lang, F.R. What Do Cognitive Complaints in a Sample of Memory Clinic Outpatients Reflect? GeroPsych: The Journal of Gerontopsychology and Geriatric Psychiatry 2011, 24. [Google Scholar] [CrossRef]
- Van Patten, R.; Bellone, J.A. The Neuropsychology of Functional Neurological Disorders. J Clin Exp Neuropsychol 2023, 45, 957–969. [Google Scholar] [CrossRef]
- Picon, E.L.; Todorova, E. V.; Palombo, D.J.; Perez, D.L.; Howard, A.K.; Silverberg, N.D. Memory Perfectionism Is Associated with Persistent Memory Complaints after Concussion. Archives of Clinical Neuropsychology 2022, 37. [Google Scholar] [CrossRef]
- Zamarian, L.; Högl, B.; Delazer, M.; Hingerl, K.; Gabelia, D.; Mitterling, T.; Brandauer, E.; Frauscher, B. Subjective Deficits of Attention, Cognition and Depression in Patients with Narcolepsy. Sleep Med 2015, 16. [Google Scholar] [CrossRef]
- Larner, A.J. Screening Utility of the Attended Alone Sign for Subjective Memory Impairment. Alzheimer Dis Assoc Disord 2014, 28. [Google Scholar] [CrossRef]
- Larner, A.J. “Who Came with You?” A Diagnostic Observation in Patients with Memory Problems? [1]. J Neurol Neurosurg Psychiatry 2005, 76. [Google Scholar] [CrossRef]
- Tarik Elhadd, K. Functional Cognitive Disorders: Can Sleep Disturbance Contribute to a Positive Diagnosis? Article in Journal of Sleep Disorders & Therapy 2018. [Google Scholar] [CrossRef]
| Feature | Description | Clinical Relevance |
|---|---|---|
| Impaired metacognition | Difficulty accurately monitoring or evaluating cognitive performance. | Leads to overestimation of deficits despite intact objective testing. |
| Memory perfectionism | Unrealistically high standards for memory functioning. | Fosters hypervigilance and misinterpretation of benign lapses as pathological. |
| Negative interpretation bias | Tendency to selectively attend to and catastrophize normal forgetfulness. | Reinforces anxiety and distress about cognitive health. |
| Memory-related anxiety | Fear of inevitable decline due to aging or genetic predisposition. | Increases symptom salience and promotes maladaptive beliefs. |
| Cogniphobia | Avoidance of cognitively demanding activities. | Reduces exposure to corrective experiences, reinforcing dysfunctional beliefs. |
| Psychiatric comorbidity | Co-occurrence of anxiety, depression, or trauma history. | May perpetuate or exacerbate cognitive complaints but does not account for FCD alone. |
| Impaired metacognition | Difficulty accurately monitoring or evaluating cognitive performance. | Leads to overestimation of deficits despite intact objective testing. |
| Memory perfectionism | Unrealistically high standards for memory functioning. | Fosters hypervigilance and misinterpretation of benign lapses as pathological. |
| Negative interpretation bias | Tendency to selectively attend to and catastrophize normal forgetfulness. | Reinforces anxiety and distress about cognitive health. |
| Memory-related anxiety | Fear of inevitable decline due to aging or genetic predisposition. | Increases symptom salience and promotes maladaptive beliefs. |
| Cogniphobia | Avoidance of cognitively demanding activities. | Reduces exposure to corrective experiences, reinforcing dysfunctional beliefs. |
| Assessment Method | Purpose | Key Diagnostic Contribution |
|---|---|---|
| Neuropsychological Testing | Evaluates cognitive domains (e.g., memory, attention). | Reveals normal or inconsistent impairments not aligning with neuroanatomical patterns. |
| MoCA / MMSE | Brief cognitive screening tools. | Normal scores despite severe complaints suggest functional etiology. |
| Medical Symptom Validity Tests | Tests response consistency and effort. | Helps identify attentional interference or metacognitive disruption rather than malingering. |
| PHQ-15 / HADS / PSQI / MMQ | Questionnaires assessing somatic symptoms, mood, sleep, and memory beliefs. | Elevated scores without objective deficits support functional diagnosis. |
| Interactional Analysis | Observation of communication patterns and symptom narratives. | Features like verbosity, coherence, and “attending alone” behavior support FCD. |
| MINI Interview | Structured psychiatric interview. | Identifies comorbid depression, anxiety, or trauma relevant to FCD formulation. |
| Schmidtke Criteria | Symptom-based inventory. | Provides standardized diagnostic criteria with predictive value for non-progression. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




