2. The Patient Journey Touchpoints
The patient journey within a healthcare facility is composed of multiple moments, each point is an opportunity to either strengthen or weaken trust, comfort, and satisfaction. These touchpoints form a continuum that begins before the patient enters the hospital and continues long after discharge. Understanding and optimizing these stages is essential to delivering a seamless, empathetic healthcare experience.
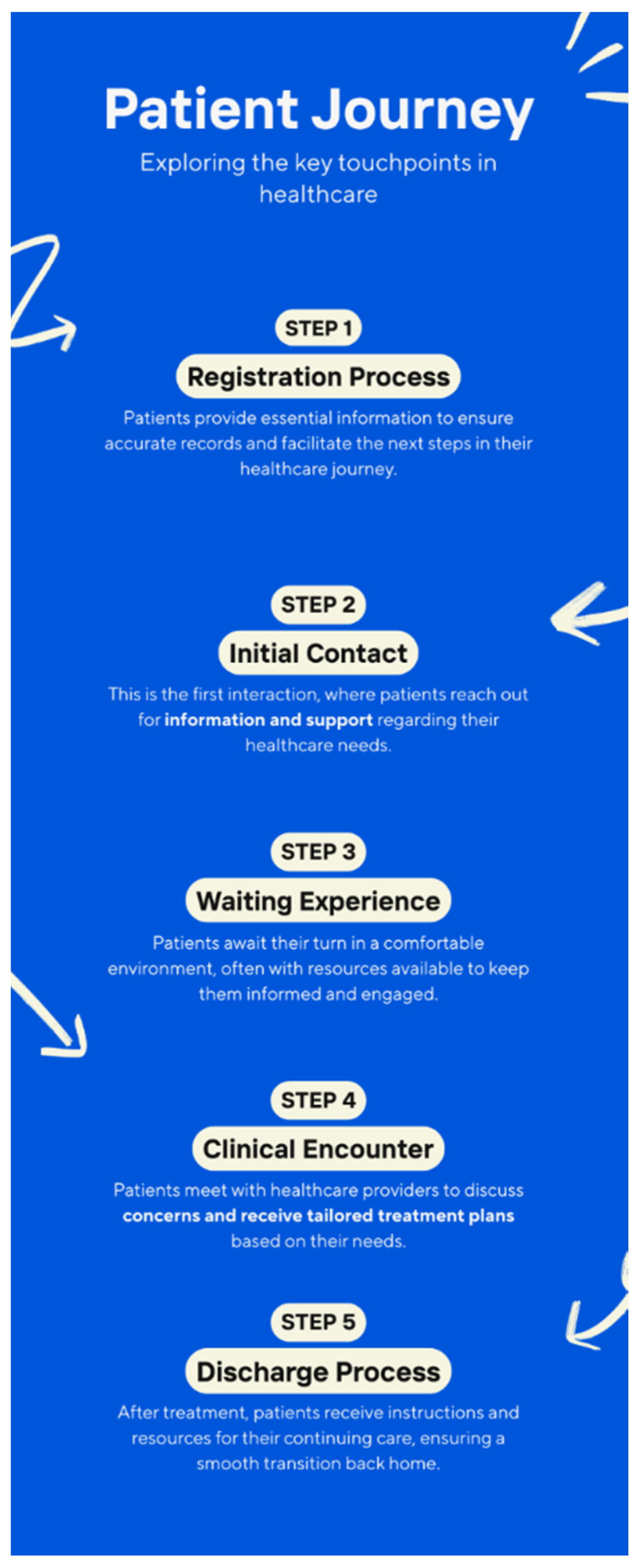
The journey often begins with initial contact, which could take the form of a phone call, website visit, or a walk-in inquiry. The tone, clarity, and helpfulness of this interaction set the stage for all future perceptions. If patients are met with confusion, indifference, or delays at this point, it undermines confidence and adds anxiety even before treatment begins.
Next is the registration and admission process. This phase often involves paperwork, identity verification, and financial information, elements that can be intimidating or stressful. Friendly, patient staff who guide individuals through this process with respect and transparency can help ease tensions and promote a sense of being cared for.
Once registered, patients move into the waiting experience, where emotions like worry and discomfort often surface. A clean, organized, and calming environment, paired with clear communication about waiting times and procedures, demonstrates respect for the patient’s time and dignity. This seemingly passive moment is, in reality, a powerful indicator of service quality.
The clinical encounter interactions with nurses, doctors, and other healthcare providers are the most critical touchpoint. It’s where trust is either deepened or eroded. Patients value clinicians who not only diagnose and treat but who also listen, explain, and empathize. Good customer service in this context means clear communication, cultural sensitivity, and a commitment to shared decision-making.
After treatment, the discharge process represents a crucial handover. It includes instructions, medications, follow-up appointments, and sometimes financial settlements. A rushed or unclear discharge can leave patients feeling unprepared and abandoned. Conversely, a well-orchestrated exit that anticipates questions and affirms continued support reflects a strong service culture.
The journey continues with post-care follow-up, which may include phone calls, emails, or telehealth check-ins. These interactions are often overlooked but play a vital role in recovery and ongoing patient satisfaction. They reassure patients that they have not been forgotten and that their healing remains a shared priority.
Each of these touchpoints is an opportunity to either reinforce or damage a patient’s trust in the healthcare system. Together, they form a mosaic of experience where attentive customer service transforms care from a clinical transaction into a meaningful, healing relationship. By mapping and intentionally improving these stages, healthcare institutions can design more compassionate, efficient, and patient-centered services that support long-term loyalty and better health outcomes.
Figure 1.
Five Critical Touchpoints.
Figure 1.
Five Critical Touchpoints.
2.1. Global Service Gaps in Healthcare
Despite advancements in healthcare delivery and the growing recognition of the importance of patient-centered care, service gaps persist across hospitals worldwide. These gaps often undermine the quality of patient experiences and can significantly impact health outcomes, even in well-resourced environments [
11]. Understanding these common service gaps is essential for identifying areas that require improvement and innovation [
21].
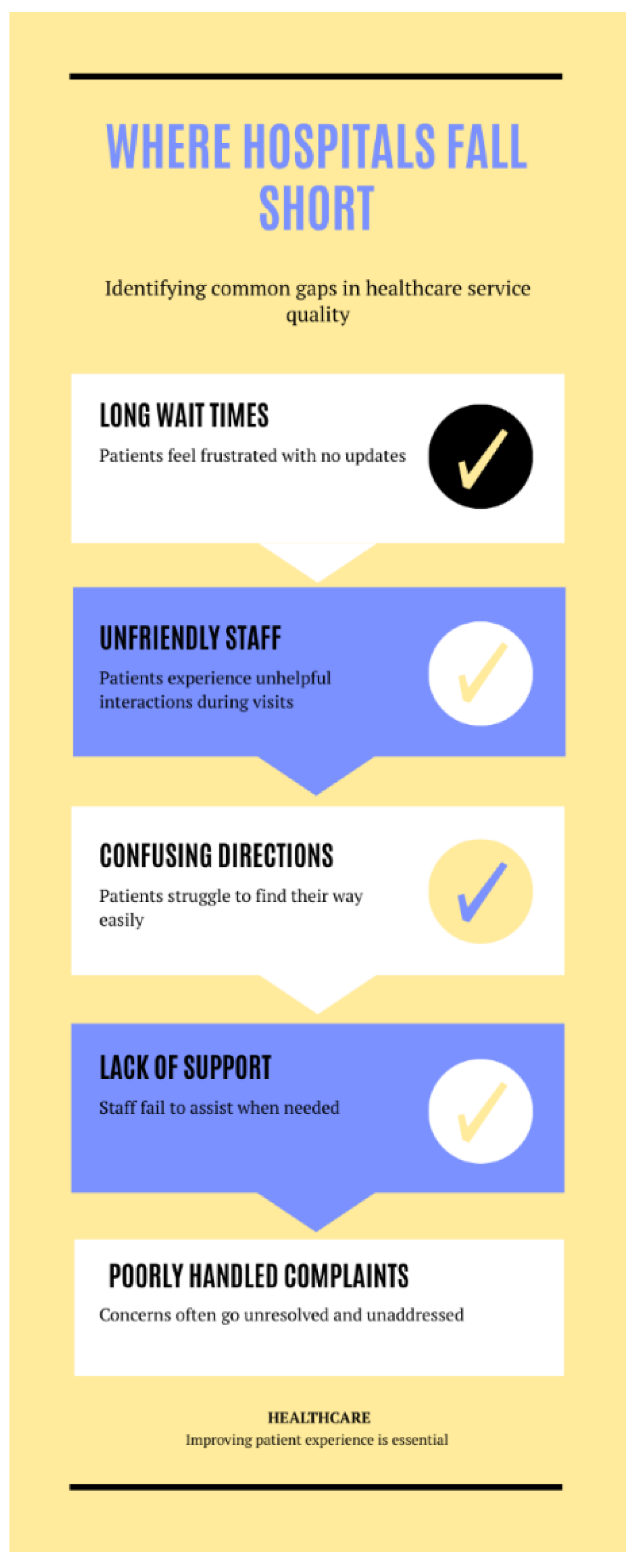
One of the most prevalent gaps is the lack of timely access to care. In many regions, patients encounter long waiting times for appointments, delays in emergency services, and extended periods before diagnostic results are available [
5,
6,
7,
8,
9,
10,
11,
12]. These delays not only cause frustration but also jeopardize health, especially in time-sensitive cases [
5].
Another widespread issue is poor communication between healthcare providers and patients. Patients frequently report not being adequately informed about their diagnoses, treatment options, or medication instructions. This communication gap can lead to confusion, non-compliance with medical advice, and a general sense of neglect. Cultural and language differences further compound this problem, especially in multicultural societies or countries with diverse populations.
There is also a global inconsistency in staff attitudes and emotional intelligence. While many healthcare professionals are highly skilled clinically, some lack the soft skills needed to interact with patients empathetically. Dismissive behavior, lack of courtesy, or indifference to patients’ concerns can create emotional distress and erode trust, regardless of the quality of the clinical care provided [
8].
Infrastructure and facility management are additional areas where service gaps are evident [
21]. Outdated equipment, insufficient cleanliness, lack of signage, or uncomfortable waiting areas can all contribute to a negative patient experience. In lower-income countries, this may stem from limited funding, while in higher-income regions, bureaucratic inefficiencies or poor planning may be to blame [
18].
Digital inequality represents another growing gap. As hospitals increasingly rely on technology for patient portals, telemedicine, and automated systems, not all patients are equally equipped to navigate these tools [
12]. Older adults, those with limited digital literacy, and patients in rural areas without strong internet connectivity often struggle to benefit from these technological innovations, creating a divide in access and service quality [
20].
Coordination between departments within hospitals is frequently cited as a pain point. A lack of internal communication can lead to misplaced test results, duplicate procedures, or misaligned care plans [
14]. Patients may feel like they are repeating themselves at every step or being passed from one department to another without proper handover or context [
6].
Lastly, follow-up care is a neglected area in many healthcare systems [
1]. After patients leave the hospital, they often receive little to no communication regarding their recovery, medication, or the need for further appointments [
7]. This absence of continuity increases the risk of readmissions, complications, or feelings of abandonment.
These common global service gaps highlight the importance of approaching healthcare not just as a clinical obligation but as a comprehensive human experience [
17]. Bridging these gaps requires commitment, innovation, and leadership from healthcare institutions and policymakers worldwide [
13]. The path to better healthcare begins with listening to patients, valuing their experiences, and acting decisively to eliminate the barriers that stand in the way of compassionate, efficient, and equitable service [
16].
Figure 2.
Five Global Service Gaps in Healthcare.
Figure 2.
Five Global Service Gaps in Healthcare.
2.2. Global Perspectives on Service Delivery
Healthcare service delivery varies widely across the globe, shaped by cultural values, economic resources, political systems, and public expectations [
2]. Yet, despite these differences, a common global aspiration persists: to provide care that is accessible, respectful, and responsive to the needs of every patient [
9]. By examining how different regions approach healthcare service delivery, valuable insights emerge into both innovative practices and shared challenges [
13].
In countries with universal healthcare systems such as the United Kingdom, Canada, and many in Western Europe, the focus often lies on equity and access. These systems are designed to ensure that all citizens receive care without financial hardship [
16]. However, they sometimes struggle with long wait times, overstretched resources, and bureaucracy, which can dilute the quality of the patient experience [
10]. Customer service initiatives in these regions often aim to improve efficiency, enhance provider communication, and personalize care within the constraints of a publicly funded system [
19].
In the United States, where healthcare is largely privatized, service delivery is often influenced by competition [
7]. Hospitals and clinics invest heavily in customer service to attract and retain patients. This has led to innovations such as concierge services, luxury birthing suites, digital patient engagement platforms, and personalized wellness plans [
12]. However, disparities in care remain a major issue, with access heavily dependent on insurance coverage and socioeconomic status.
Here, customer service excellence can coexist with unequal treatment access, highlighting the need for both structural reform and service refinement [
16].
In middle-income countries such as India, Brazil, and South Africa, a dual-system approach exists where both public and private sectors operate concurrently. While public hospitals aim to serve the masses, they often suffer from underfunding and congestion, resulting in lower service quality [
18]. In contrast, private facilities cater to those who can afford higher costs, offering faster, more comfortable, and more personalized services. The gap between these two tiers creates tension in service delivery, as national health goals strive to bring consistency and fairness across socioeconomic classes [
16].
Asian countries like Japan, South Korea, and Singapore offer compelling models of efficient service delivery. These nations combine strong government regulation, cutting-edge technology, and a cultural emphasis on respect and order [
2,
3,
4,
5,
6,
7,
8,
9,
10,
11,
12,
13]. In Japan, for example, the patient-provider interaction is guided by deep-rooted traditions of politeness and dignity, while Singapore’s digitized healthcare system ensures fast and coordinated care [
12]. These countries demonstrate that integrating cultural values with modern systems can produce highly effective service environments [
14].
In many parts of Africa and Southeast Asia, healthcare systems face enormous challenges, including workforce shortages, limited infrastructure, and funding constraints [
5]. Despite these hurdles, there are growing efforts to improve service delivery through community health initiatives, mobile health units, and international partnerships [
13]. Countries like Rwanda and Ghana have made significant strides in enhancing access and service quality through innovative health insurance models and community engagement. In these settings, customer service is increasingly recognized as essential, not secondary, to care delivery [
12].
Globally, the COVID-19 pandemic has acted as a catalyst for rethinking healthcare service models. It forced hospitals around the world to adopt virtual consultations, streamline patient flow, and strengthen communication channels - all key elements of good customer service [
16]. From urban hospitals in Europe to rural clinics in Latin America, the crisis exposed weaknesses and prompted systemic change toward more agile, patient-responsive care models [
5].
Ultimately, global perspectives on healthcare service delivery reveal that while each system has unique strengths and weaknesses, the human need for compassionate, respectful, and efficient care is universal [
17]. Learning from each other’s successes and failures offers a path forward - one where best practice can be adapted, scaled, and localized to improve service experiences across diverse healthcare landscapes.
Figure 3.
Perspectives on Service Delivery.
Figure 3.
Perspectives on Service Delivery.
2.3. Toward a Culture of Care
Transforming healthcare service delivery is not merely about systems and procedures. It is about shaping a deeper organizational ethos that consistently places the patient at the heart of every decision [
11]. A culture of care transcends transactional service encounters and embeds compassion, dignity, and responsiveness into the fabric of daily hospital life [
19]. While policies and technologies may guide structure, it is the people, values, and mindset within an institution that determine the real quality of care experienced by patients [
10].
At its core, a culture of care begins with leadership. When hospital leaders and administrators visibly champion empathy, fairness, and respect, they set the tone for everyone else [
21]. This culture cascades down through every department, influencing how staff interact with patients, how problems are solved, and how improvement is pursued. Leadership that listens to both patients and staff, that embraces feedback, and that remains open to change is essential to sustaining meaningful service transformation [
5].
A culture of care is also defined by shared ownership of the patient experience. It is not only the job of doctors and nurses to ensure that patients feel seen, heard, and valued [
4,
5]. Everyone be it receptionists, cleaners, pharmacists, porters, security personnel play a role in shaping how patients perceive and experience the healthcare environment [
7]. When every team member understands that they contribute to healing, a collective sense of purpose emerges [
9].
Training and education are critical enablers of this cultural shift. Soft skills such as active listening, conflict resolution, cultural competence, and emotional intelligence must be continually developed [
2]. These skills do not come automatically with medical expertise, yet they are crucial in fostering trust and comfort. Institutions that integrate customer service principles into clinical and non-clinical training tend to build stronger, more respectful relationships between caregivers and patients [
8].
Equally important is the way organizations recognize and reward compassionate service. Celebrating staff who go the extra mile reinforces the behaviors that embody a culture of care [
10]. Recognition programs, feedback loops, and open communication channels all help staff feel valued and motivated [
3]. When staff feel respected and supported, they are more likely to extend the same warmth and attentiveness to those in their care [
3].
Another hallmark of a culture of care is the continuous pursuit of patient feedback and co-design. Patients are not passive recipients; they are experts in their own experience [
12]. Institutions that invite patients to help shape services, participate in planning, and review systems from their perspective tend to deliver more responsive and meaningful care. This inclusivity builds mutual respect and strengthens trust in the healthcare system [
13,
14].
Lastly, a true culture of care is resilient and adaptable. In times of crisis like the COVID-19 pandemic healthcare systems were tested not only in terms of capacity but also in compassion [
7]. Those that had already invested in empathy-driven systems were better able to reassure, communicate with, and protect their patients and staff. Building a culture of care is thus not a luxury, but a necessity for preparedness, sustainability, and long-term success [
15].
In moving toward this vision, hospitals around the world must reflect not just on what services they provide, but how they provide them [
19]. The journey toward a culture of care is ongoing, but with intention and leadership, it can reshape the global standard for what healthcare truly means [
16].
Figure 4.
A Culture of Care.
Figure 4.
A Culture of Care.