Submitted:
15 July 2025
Posted:
16 July 2025
Read the latest preprint version here
Abstract
Keywords:
Introduction
Methods
Study design and participants inclusion
Cognitive assessment
Video-polysomnography (V-PSG) and sleep architecture
Statistical Analysis
Results
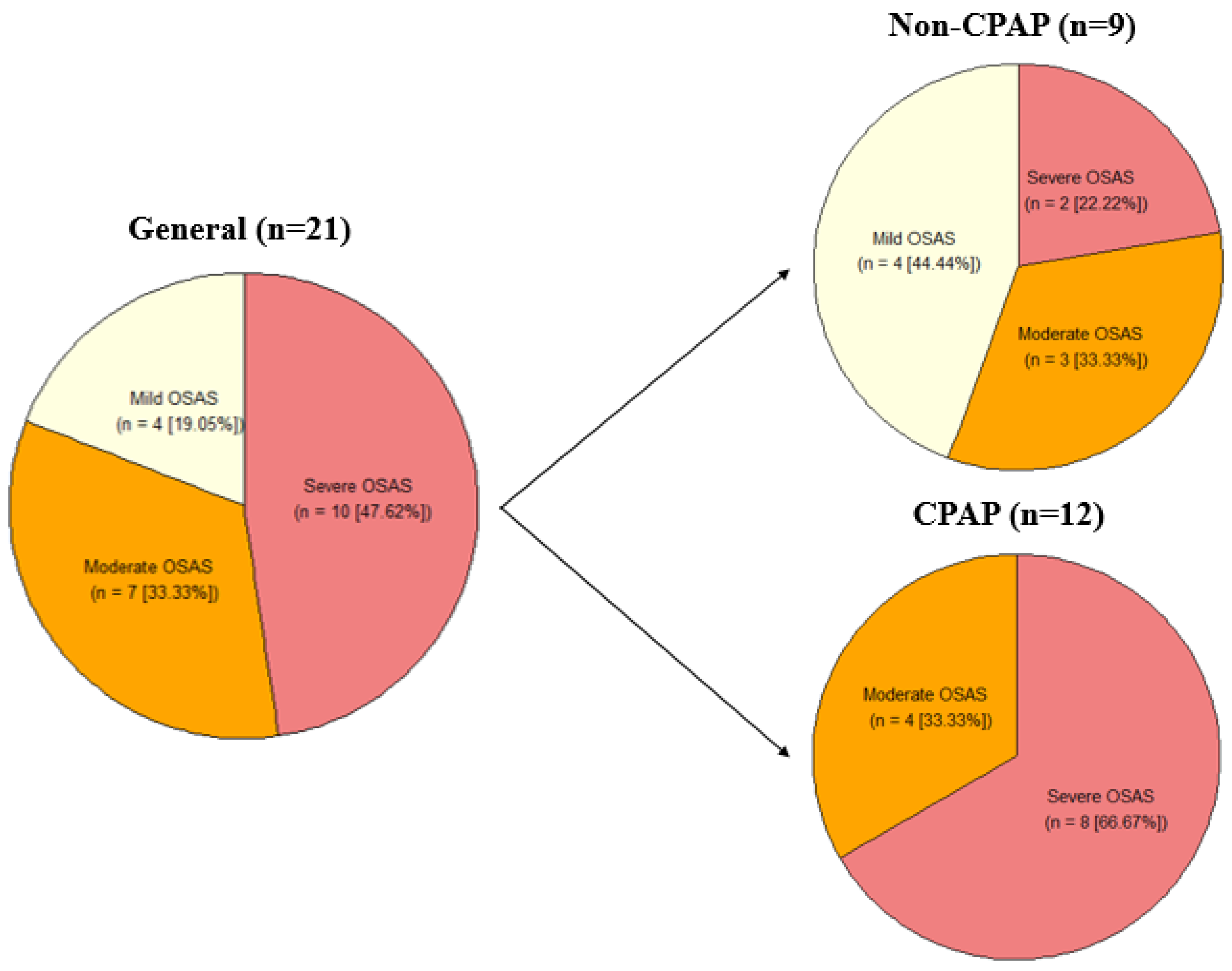
Demographic description of the CPAP and non-CPAP groups
CPAP results
Longitudinal Cognitive Status
Effect of sleep in cognitive progression.
Discussion
Cognitive Progression in the full cohort
Impact of the CPAP on Cognitive Progression
Effect of sleep parameters on Cognitive Progression
Study Limitations
Conclusion
Author Contributions
References
- Jiao, B.; Li, R.; Zhou, H.; Qing, K.; Liu, H.; Pan, H.; Lei, Y.; Fu, W.; Wang, X.; Xiao, X.; Liu, X.; Yang, Q.; Liao, X.; Zhou, Y.; Fang, L.; Dong, Y.; Yang, Y.; Jiang, H.; Huang, S.; Shen, L. Neural biomarker diagnosis and prediction to mild cognitive impairment and Alzheimer's disease using EEG technology. Alzheimers Res Ther. 2023 Feb 10;15, 32. [CrossRef] [PubMed]
- Mayer, G.; Frohnhofen, H.; Jokisch, M.; Hermann, D.M.; Gronewold, J. Associations of sleep disorders with all-cause MCI/dementia and different types of dementia - clinical evidence, potential pathomechanisms and treatment options: A narrative review. Front Neurosci. 2024. [CrossRef]
- Thipani Madhu, M.; Balaji, O.; Kandi, V.; Ca, J.; Harikrishna, G.V.; Metta, N.; Mudamanchu, V.K.; Sanjay, B.G.; Bhupathiraju, P. Role of the Glymphatic System in Alzheimer's Disease and Treatment Approaches: A Narrative Review. Cureus. 2024 Jun 29;16, e63448. [CrossRef]
- Hussain, R.; Graham, U.; Elder, A.; Nedergaard, M. Air pollution, glymphatic impairment, and Alzheimer's disease. Trends Neurosci. 2023 Nov;46, 901-911. [CrossRef]
- Ekanayake, A.; Peiris, S.; Ahmed, B.; Kanekar, S.; Grove, C.; Kalra, D.; Eslinger, P.; Yang, Q.; Karunanayaka, P. A Review of the Role of Estrogens in Olfaction, Sleep and Glymphatic Functionality in Relation to Sex Disparity in Alzheimer's Disease. Am J Alzheimers Dis Other Demen. 2024 Jan-Dec;39:15333175241272025. [CrossRef]
- Huang, Z.; Jordan, J.D.; Zhang, Q. Early life adversity as a risk factor for cognitive impairment and Alzheimer's disease. Transl Neurodegener. 2023 May 12;12, 25. [CrossRef]
- Heutz, R.; Claassen, J.; Feiner, S.; Davies, A.; Gurung, D.; Panerai, R.B.; Heus, R.; Beishon, L.C. Dynamic cerebral autoregulation in Alzheimer's disease and mild cognitive impairment: A systematic review. J Cereb Blood Flow Metab. 2023 Aug;43, 1223-1236. [CrossRef]
- Zhang, Q.; Coury, R.; Tang, W. Prediction of conversion from mild cognitive impairment to Alzheimer's disease and simultaneous feature selection and grouping using Medicaid claim data. Alzheimers Res Ther. 2024 Mar 9;16, 54. [CrossRef]
- Matuskova, V.; Veverova, K.; Jester, D.J.; Matoska, V.; Ismail, Z.; Sheardova, K.; Horakova, H.; Cerman, J.; Laczó, J.; Andel, R.; Hort, J.; Vyhnalek, M. Mild behavioral impairment in early Alzheimer's disease and its association with APOE and BDNF risk genetic polymorphisms. Alzheimers Res Ther. 2024 Jan 26;16, 21. [CrossRef]
- Astara, K.; Tsimpolis, A.; Kalafatakis, K.; Vavougios, G.D.; Xiromerisiou, G.; Dardiotis, E.; Christodoulou, N.G.; Samara, M.T.; Lappas, A.S. Sleep disorders and Alzheimer's disease pathophysiology: The role of the Glymphatic System. A scoping review. Mech Ageing Dev. 2024 Feb;217:111899. [CrossRef]
- Gao, Y.; Liu, K.; Zhu, J. Glymphatic system: an emerging therapeutic approach for neurological disorders. Front Mol Neurosci. 2023 Jul 6;16:1138769. [CrossRef]
- Voumvourakis, K.I.; Sideri, E.; Papadimitropoulos, G.N.; Tsantzali, I.; Hewlett, P.; Kitsos, D.; Stefanou, M.; Bonakis, A.; Giannopoulos, S.; Tsivgoulis, G.; Paraskevas, G.P. The Dynamic Relationship between the Glymphatic System, Aging, Memory, and Sleep. Biomedicines. 2023 Jul 25;11, 2092. [CrossRef]
- Örzsik, B.; Palombo, M.; Asllani, I.; Dijk, D.J.; Harrison, N.A.; Cercignani M. Higher order diffusion imaging as a putative index of human sleep-related microstructural changes and glymphatic clearance. Neuroimage. 2023 Jul 1;274:120124. [CrossRef]
- Simmonds, E.; Levine, K.S.; Han, J.; Iwaki, H.; Koretsky, M.J.; Kuznetsov, N.; Faghri, F.; Solsberg, C.W.; Schuh, A.; Jones, L.; Bandres-Ciga, S.; Blauwendraat, C.; Singleton, A.; Escott-Price, V.; Leonard, H.L.; Nalls, M.A. Sleep disturbances as risk factors for neurodegeneration later in life. medRxiv [Preprint]. 2023 Nov 9:2023.11.08.23298037. [CrossRef]
- Oliver, C.; Li, H.; Biswas, B.; Woodstoke, D.; Blackman, J.; Butters, A.; Drew, C.; Gabb, V.; Harding, S.; Hoyos, C.M.; Kendrick, A.; Rudd, S.; Turner, N.; Coulthard, E. A systematic review on adherence to continuous positive airway pressure (CPAP) treatment for obstructive sleep apnoea (OSA) in individuals with mild cognitive impairment and Alzheimer's disease dementia. Sleep Med Rev. 2024 Feb;73:101869. [CrossRef]
- Richards, K.C.; Lozano, A.J.; Morris, J.; Moelter, S.T.; Ji, W.; Vallabhaneni, V.; Wang, Y.; Chi, L.; Davis, E.M.; Cheng, C.; Aguilar, V.; Khan, S.; Sankhavaram, M.; Hanlon, A.L.; Wolk, D.A.; Gooneratne, N. Predictors of Adherence to Continuous Positive Airway Pressure in Older Adults With Apnea and Amnestic Mild Cognitive Impairment. J Gerontol A Biol Sci Med Sci. 2023 Oct 9;78, 1861-1870. [CrossRef]
- Ke, S., Luo, T., Ding, Y. et al. Does Obstructive sleep apnea mediate the risk of cognitive impairment by expanding the perivascular space?. Sleep Breath 29, 130 (2025). [CrossRef]
- Ozturk, B.; Koundal, S.; Al Bizri, E.; Chen, X.; Gursky, Z.; Dai, F.; Lim, A.; Heerdt, P.; Kipnis, J.; Tannenbaum, A.; Lee, H.; Benveniste, H. Continuous positive airway pressure increases CSF flow and glymphatic transport. JCI Insight. 2023 Jun 22;8, e170270. [CrossRef]
- Kapur, V.K.; Auckley, D.H.; Chowdhuri, S.; Kuhlmann, D.C.; Mehra, R.; Ramar, K.; Harrod, C.G. Clinical Practice Guideline for Diagnostic Testing for Adult Obstructive Sleep Apnea: An American Academy of Sleep Medicine Clinical Practice Guideline. J Clin Sleep Med. 2017 Mar 15;13, 479-504. [CrossRef]
- Duff, K.; Suhrie, K.R.; Hammers, D.B.; Dixon, A.M.; King, J.B.; Koppelmans, V.; Hoffman, J.M. Repeatable battery for the assessment of neuropsychological status and its relationship to biomarkers of Alzheimer's disease. Clin Neuropsychol. 2023 Jan;37, 157-173. [CrossRef]
- Liu, W.T.; Huang, H.T.; Hung, H.Y.; Lin, S.Y.; Hsu, W.H.; Lee, F.Y.; Kuan, Y.C.; Lin, Y.T.; Hsu, C.R.; Stettler, M.; Yang, C.M.; Wang, J.; Duh, P.J.; Lee, K.Y.; Wu, D.; Lee, H.C.; Kang, J.H.; Lee, S.S.; Wong, H.J.; Tsai, C.Y.; Majumdar, A. Continuous Positive Airway Pressure Reduces Plasma Neurochemical Levels in Patients with OSA: A Pilot Study. Life (Basel). 2023 Feb 22;13, 613. [CrossRef]
- Grimmer, T.; Riemenschneider, M.; Förstl, H.; Henriksen, G.; Klunk, W.E.; Mathis, C.A.; Shiga, T.; Wester, H.J.; Kurz, A.; Drzezga, A. Beta amyloid in Alzheimer's disease: increased deposition in brain is reflected in reduced concentration in cerebrospinal fluid. Biol Psychiatry. 2009 Jun 1;65, 927-34. [CrossRef]
- Claudio Liguori, Agostino Chiaravalloti, Francesca Izzi, Marzia Nuccetelli, Sergio Bernardini, Orazio Schillaci, Nicola Biagio Mercuri, Fabio Placidi, Sleep apnoeas may represent a reversible risk factor for amyloid-β pathology, Brain, Volume 140, Issue 12, December 2017, Page e75, . [CrossRef]
- Ma, J., Chen, M., Liu, GH. et al. Effects of sleep on the glymphatic functioning and multimodal human brain network affecting memory in older adults. Mol Psychiatry (2024). [CrossRef]
- Jackson, M.L.; Howard, M.E.; Barnes, M. Cognition and daytime functioning in sleep-related breathing disorders. Prog Brain Res. 2011;190:53-68. [CrossRef]
- Lee, H.J.; Lee, D.A.; Shin, K.J.; Park, K.M. Glymphatic system dysfunction in obstructive sleep apnea evidenced by DTI-ALPS. Sleep Med. 2022 Jan;89:176-181. [CrossRef]
- Kamagata K, Andica C, Takabayashi K, Saito Y, Taoka T, Nozaki H, Kikuta J, Fujita S, Hagiwara A, Kamiya K, Wada A, Akashi T, Sano K, Nishizawa M, Hori M, Naganawa S, Aoki S; Alzheimer's Disease Neuroimaging Initiative. Association of MRI Indices of Glymphatic System With Amyloid Deposition and Cognition in Mild Cognitive Impairment and Alzheimer Disease. Neurology. 2022 Dec 12;99, e2648-e2660. [CrossRef] [PubMed]
- Ren, L.; Wang, K.; Shen, H.; Xu, Y.; Wang, J.; Chen, R. Effects of continuous positive airway pressure (CPAP) therapy on neurological and functional rehabilitation in Basal Ganglia Stroke patients with obstructive sleep apnea: A prospective multicenter study. Medicine (Baltimore). 2019 Jul;98, e16344. [CrossRef]
- Bubu, O.M.; Andrade, A.G.; Umasabor-Bubu, O.Q.; Hogan, M.M.; Turner, A.D.; de Leon, M.J.; Ogedegbe, G.; Ayappa, I.; Jean-Louis, G.G.; Jackson, M.L.; Varga, A.W.; Osorio, R.S. Obstructive sleep apnea, cognition and Alzheimer's disease: A systematic review integrating three decades of multidisciplinary research. Sleep Med Rev. 2020 Apr;50:101250. [CrossRef]
- Richards K.C., Gooneratne N., Dicicco B., et. al.: CPAP adherence may slow 1-year cognitive decline in older adults with mild cognitive impairment and apnea. J Am Geriatr Soc 2019; 67: pp. 558-564.
- Ancoli-Israel S., Palmer B.W., Cooke J.R., et. al.: Cognitive effects of treating obstructive sleep apnea in Alzheimer's disease: a randomized controlled study. J Am Geriatr Soc 2008; 56: pp. 2076-2081.
- Cooke J.R., Ayalon L., Palmer B.W., et. al.: Sustained use of CPAP slows deterioration of cognition, sleep, and mood in patients with Alzheimer's disease and obstructive sleep apnea: a preliminary study. J Clin Sleep Med 2009; 5: pp. 305-309.
- Lajoie, A.C.; Lafontaine, A.L.; Kimoff, R.J.; Kaminska, M. Obstructive Sleep Apnea in Neurodegenerative Disorders: Current Evidence in Support of Benefit from Sleep Apnea Treatment. J Clin Med. 2020 Jan 21;9, 297. [CrossRef]
- Djonlagic, I.; Guo, M.; Matteis, P.; Carusona, A.; Stickgold, R.; Malhotra, A. First night of CPAP: impact on memory consolidation attention and subjective experience. Sleep Med. 2015 Jun;16, 697-702. [CrossRef]
- Fernandes, M.; Chiaravalloti, A.; Manfredi, N.; Placidi, F.; Nuccetelli, M.; Izzi, F.; Camedda, R.; Bernardini, S.; Schillaci, O.; Mercuri, N.B.; Liguori, C. Nocturnal Hypoxia and Sleep Fragmentation May Drive Neurodegenerative Processes: The Compared Effects of Obstructive Sleep Apnea Syndrome and Periodic Limb Movement Disorder on Alzheimer's Disease Biomarkers. J Alzheimers Dis. 2022;88, 127-139. [CrossRef]
- Liguori, C.; Mercuri, N.B.; Izzi, F.; Romigi, A.; Cordella, A.; Sancesario, G.; Placidi, F. Obstructive Sleep Apnea is Associated With Early but Possibly Modifiable Alzheimer's Disease Biomarkers Changes. Sleep. 2017 May 1;40(5). [CrossRef]
- Reddy, O.C.; van der Werf, Y.D. The Sleeping Brain: Harnessing the Power of the Glymphatic System through Lifestyle Choices. Brain Sci. 2020 Nov 17;10, 868. [CrossRef]
- Scullin, M.K.; Bliwise, D.L. Is cognitive aging associated with levels of REM sleep or slow wave sleep? Sleep. 2015 Mar 1;38, 335-6. [CrossRef]
- Song Y, Blackwell T, Yaffe K, Ancoli-Israel S, Redline S, Stone KL; Osteoporotic Fractures in Men (MrOS) Study Group. Relationships between sleep stages and changes in cognitive function in older men: the MrOS Sleep Study. Sleep. 2015 Mar 1;38, 411-21. [CrossRef] [PubMed]
- Lo, J.C.; Groeger, J.A.; Cheng, G.H.; Dijk, D.J.; Chee, M.W. Self-reported sleep duration and cognitive performance in older adults: a systematic review and meta-analysis. Sleep Med. 2016 Jan;17:87-98. [CrossRef]
- Wang, Q.; Zhu, H.; Dai, R.; Zhang, T. Associations Between Total Sleep Duration and Cognitive Function Among Middle-Aged and Older Chinese Adults: Does Midday Napping Have an Effect on It? Int J Gen Med. 2022 Feb 10;15:1381-1391. [CrossRef]
- Nelson, K.L.; Davis, J.E.; Corbett, C.F. Sleep quality: An evolutionary concept analysis. Nurs Forum. 2022 Jan;57, 144-151. [CrossRef]
- Barami, K. Cerebral venous overdrainage: an under-recognized complication of cerebrospinal fluid diversion. Neurosurg Focus. 2016 Sep;41, E9. [CrossRef]
- Gleadhill, I.C.; Schwartz, A.R.; Schubert, N.; Wise, R.A.; Permutt, S.; Smith, P.L. Upper airway collapsibility in snorers and in patients with obstructive hypopnea and apnea. Am Rev Respir Dis. 1991 Jun;143, 1300-3. [CrossRef]
- Wellman, A.; Genta, P.R.; Owens, R.L.; Edwards, B.A.; Sands, S.A.; Loring, S.H.; White, D.P.; Jackson, A.C.; Pedersen, O.F.; Butler, J.P. Test of the Starling resistor model in the human upper airway during sleep. J Appl Physiol (1985). 2014 Dec 15;117, 1478-85. [CrossRef]
- Thomas Penzel Marion Möller Heinrich, F. Becker, Lennart Knaack, Jörg-Hermann Peter, Effect of Sleep Position and Sleep Stage on the Collapsibility of the Upper Airways in Patients with Sleep Apnea, Sleep, Volume 24, Issue 1, January 2001, Pages 90–95, . [CrossRef]
- Landry, S.A.; Beatty, C.; Thomson, L.D.J.; Wong, A.M.; Edwards, B.A.; Hamilton, G.S.; Joosten, S.A. A review of supine position related obstructive sleep apnea: Classification, epidemiology, pathogenesis and treatment. Sleep Med Rev. 2023 Dec;72:101847. [CrossRef]
- Kuo, C.D.; Chen, G.Y.; Lo, H.M. Effect of different recumbent positions on spectral indices of autonomic modulation of the heart during the acute phase of myocardial infarction. Crit Care Med. 2000 May;28, 1283-9. [CrossRef]
- Yang, J.L.; Chen, G.Y.; Kuo, C.D. Comparison of effect of 5 recumbent positions on autonomic nervous modulation in patients with coronary artery disease. Circ J. 2008 Jun;72, 902-8. [CrossRef]
- Muppidi, S.; Gupta, P.K.; Vernino, S. Reversible right vagal neuropathy. Neurology. 2011 Oct 18;77, 1577-9. [CrossRef]
- Cheng, K.P.; Brodnick, S.K.; Blanz, S.L.; Zeng, W.; Kegel, J.; Pisaniello, J.A.; Ness, J.P.; Ross, E.; Nicolai, E.N.; Settell, M.L.; Trevathan, J.K.; Poore, S.O.; Suminski, A.J.; Williams, J.C.; Ludwig, K.A. Clinically-derived vagus nerve stimulation enhances cerebrospinal fluid penetrance. Brain Stimul. 2020 Jul-Aug;13, 1024-1030. [CrossRef]
- Kim, D.J.; Lee, H.P.; Kim, M.S.; Park, Y.J.; Go, H.J.; Kim, K.S.; Lee, S.P.; Chae, J.H.; Lee, C.T. The effect of total sleep deprivation on cognitive functions in normal adult male subjects. Int J Neurosci. 2001 Jul;109(1-2):127-37. [CrossRef]
- Pilcher, J.J.; McClelland, L.E.; DeWayne, D.; Henk, M.; Jaclyn, H.; Thomas, B.; Wallsten, S.; McCubbin, J.A. Language performance under sustained work and sleep deprivation conditions. Aviation, Space, and Environmental Medicine. 2007 May 1;78, B25-38.
- Crowley, R.; Alderman, E.; Javadi, A.H.; Tamminen, J. A systematic and meta-analytic review of the impact of sleep restriction on memory formation. Neurosci Biobehav Rev. 2024 Dec;167:105929. [CrossRef]
- Chua, E.C.; Fang, E.; Gooley, J.J. Effects of total sleep deprivation on divided attention performance. PLoS One. 2017 Nov 22;12, e0187098. [CrossRef]
- Menon, R.N.; Radhakrishnan, A.; Sreedharan, S.E.; Sarma, P.S.; Kumari, R.S.; Kesavadas, C.; Sasi, D.; Lekha, V.S.; Justus, S.; Unnikrishnan, J.P. Do quantified sleep architecture abnormalities underlie cognitive disturbances in amnestic mild cognitive impairment? J Clin Neurosci. 2019 Sep;67:85-92. [CrossRef]
| Features | Non-CPAP (n = 9) | CPAP (n = 12) | P-value |
| Age, yrs | 79 (72-81) | 74 (60-78) | 0.010 |
| Sex |
1.000 |
||
| Females | 6 (66.67%) | 9 (75.00%) | |
| Males | 3 (33.33%) | 3 (25.00%) | |
| Education, yrs | 12 (5-18) | 9 (2-20) | 0.327 |
|
Abbreviation: Yrs, Years. | |||
| Neurocognitive Test / Assessment |
Score T0 (Baseline) (mean ± SD) |
Score T1 (12 Months) (mean ± SD) |
P-value |
| CDR | 0.64 ± 0.36 | 0.71 ± 0.37 | 0.223 |
| MMSE | 22.67 ± 5.35 | 20.71 ± 5.51 | < 0.001 |
| RBANS Total | 66.24 ± 14.77 | 64.24 ± 15.48 | < 0.001 |
| RBANS IMI | 65.05 ± 15.50 | 61.29 ± 15.25 | < 0.001 |
| RBANS LL | 17.90 ± 5.51 | 16.50 ± 6.07 | < 0.001 |
| RBANS SM | 7.24 ± 4.33 | 6.33 ± 4.82 | 0.001 |
| RBANS VSPI | 85.89 ± 19.38 | 87.95 ± 17.08 | 0.056 |
| RBANS FC | 16.65 ± 2.66 | 17.10 ± 1.92 | 0.365 |
| RBANS LO | 13.00 ± 4.24 | 13.05 ± 4.05 | 0.031 |
| RBANS LNGI | 74.21 ± 19.12 | 77.68 ± 16.45 | < 0.001 |
| RBANS PN | 7.84 ± 2.14 | 8.58 ± 1.71 | 0.016 |
| RBANS SF | 11.71 ± 5.58 | 11.38 ± 5.16 | < 0.001 |
| RBANS ATI | 69.42 ± 18.14 | 69.11 ± 18.59 | < 0.001 |
| RBANS DDS | 4.86 ± 1.28 | 4.48 ± 1.33 | 0.005 |
| RBANS IDS | 2.82 ± 2.83 | 4.47 ± 1.55 | 0.768 |
| RBANS C | 21.00 ± 14.15 | 20.00 ± 14.86 | < 0.001 |
| RBANS DMI | 64.75 ± 19.35 | 57.30 ± 19.49 | 0.003 |
| RBANS LR | 1.10 ± 1.67 | 1.33 ± 2.20 | 0.003 |
| RBANS LRe | 14.90 ± 4.38 | 14.50 ± 2.70 | 0.349 |
| RBANS SR | 2.57 ± 2.77 | 1.86 ± 2.41 | 0.002 |
| RBANS FR | 5.86 ± 5.08 | 5.48 ± 5.71 | 0.003 |
| Neuropsychological Test / Assessment | Non-CPAP (n = 9) | CPAP (n = 12) | P-value |
|
T1 (12 Months) – T0 (Baseline) (mean ± SD) |
T1 (12 Months) – T0 (Baseline) (mean ± SD) |
||
| CDR | 0.06 ± 0.17 | 0.08 ± 0.19 | 0.838 |
| MMSE | -3.78 ± 2.54 | -0.58 ± 3.42 | 0.016 |
| RBANS Total | -6.38 ± 7.73 | 1.89 ± 9.09 | 0.028 |
| RBANS IMI | -4.78 ± 9.96 | -3.00 ± 14.52 | 0.229 |
| RBANS LL | -2.56 ± 4.10 | -0.45 ± 4.91 | 0.589 |
| RBANS SM | -0.78 ± 2.91 | -1.00 ± 4.59 | 0.495 |
| RBANS VSPI | -6.11 ± 14.83 | 9.40 ± 20.59 | 0.119 |
| RBANS FC | -1.11 ± 2.09 | 1.73 ± 2.97 | 0.010 |
| RBANS LO | -0.33 ± 2.74 | 0.40 ± 4.81 | 0.988 |
| RBANS LNGI | 2.44 ± 12.27 | 4.40 ± 15.68 | 0.177 |
| RBANS PN | 0.67 ± 1.41 | 0.80 ± 1.99 | 0.643 |
| RBANS SF | -1.67 ± 2.69 | 0.67 ± 4.10 | 0.045 |
| RBANS ATI | -1.38 ± 6.80 | 0.45 ± 8.49 | 0.834 |
| RBANS DDS | -0.33 ± 0.87 | -0.42 ± 0.79 | 0.961 |
| RBANS IDS | 2.00 ± 3.16 | 1.33 ± 4.27 | 0.151 |
| RBANS C | -3.38 ±6.07 | 0.73 ± 6.31 | 0.135 |
| RBANS DMI | -18.00 ± 13.87 | 1.18 ± 15.52 | 0.064 |
| RBANS LR | -0.44 ± 0.88 | 0.75 ± 2.18 | 0.326 |
| RBANS LRe | -2.67 ± 3.43 | 1.45 ± 4.95 | 0.145 |
| RBANS SR | -0.78 ± 1.09 | -0.67 ± 1.87 | 0.211 |
| RBANS FR | -0.67 ± 4.09 | -0.17 ± 4.93 | 0.802 |
| Sleep Stages | Sleep Quality | Sleep Position | |||||||
| N2 | N3 | REM | TST | SE | W | ST | RST | ||
| Δ MMSE | p-value | 0.038 | 0.022 | 0.879 | 0.856 | 0.673 | 0.655 | 0.023 | 0.011 |
| r | -0.41 | 0.51 | 0.14 | 0.01 | 0.01 | -0.02 | -0.44 | 0.56 | |
| Δ RBANS Total | p-value | 0.415 | 0.299 | 0.766 | 0.055 | 0.090 | 0.094 | 0.549 | 0.076 |
| r | 0.19 | 0.21 | 0.03 | 0.35 | 0.29 | -0.29 | -0.10 | 0.35 | |
| Δ RBANS IMI | p-value | 0.106 | 0.977 | 0.044 | 0.014 | 0.038 | 0.048 | 0.420 | 0.966 |
| r | 0.32 | -0.17 | 0.42 | 0.38 | 0.29 | -0.27 | 0.25 | -0.12 | |
| Δ RBANS LL | p-value | 0.393 | 0.628 | 0.015 | 0.024 | 0.036 | 0.041 | 0.705 | 0.866 |
| r | 0.18 | 0.01 | 0.53 | 0.40 | 0.36 | -0.35 | 0.12 | -0.02 | |
| Δ RBANS SM | p-value | 0.106 | 0.865 | 0.294 | 0.038 | 0.118 | 0.148 | 0.329 | 0.877 |
| r | 0.35 | -0.17 | 0.20 | 0.39 | 0.26 | -0.23 | 0.28 | -0.07 | |
| Δ RBANS LO | p-value | 0.928 | 0.249 | 0.985 | 0.214 | 0.294 | 0.360 | 0.041 | 0.002 |
| r | -0.08 | 0.28 | -0.13 | 0.10 | 0.07 | -0.06 | -0.43 | 0.54 | |
| Δ RBANS LNGI | p-value | 0.280 | 0.509 | 0.682 | 0.098 | 0.183 | 0.194 | 0.579 | 0.679 |
| r | 0.42 | -0.04 | -0.27 | 0.31 | 0.27 | -0.26 | 0.26 | -0.03 | |
| Δ RBANS PN | p-value | 0.216 | 0.683 | 0.893 | 0.235 | 0.379 | 0.390 | 0.153 | 0.410 |
| r | 0.49 | -0.32 | -0.19 | 0.25 | 0.21 | -0.21 | 0.46 | -0.30 | |
| Δ RBANS SF | p-value | 0.191 | 0.281 | 0.266 | 0.032 | 0.018 | 0.016 | 0.882 | 0.656 |
| r | 0.37 | 0.09 | 0.11 | 0.33 | 0.39 | -0.41 | 0.12 | -0.02 | |
| Δ RBANS ATI | p-value | 0.291 | 0.625 | 0.955 | 0.278 | 0.456 | 0.465 | 0.855 | 0.615 |
| r | 0.24 | 0.13 | -0.02 | 0.22 | 0.15 | -0.14 | -0.04 | 0.10 | |
| Δ RBANS DDS | p-value | 0.178 | 0.154 | 0.781 | 0.242 | 0.328 | 0.344 | 0.014 | 0.058 |
| r | -0.33 | 0.36 | -0.12 | -0.30 | -0.25 | 0.24 | -0.53 | 0.39 | |
| Δ RBANS C | p-value | 0.064 | 0.348 | 0.993 | 0.020 | 0.016 | 0.014 | 0.445 | 0.937 |
| r | 0.42 | 0.21 | -0.02 | 0.47 | 0.49 | -0.50 | 0.19 | -0.03 | |
| Δ RBANS DMI | p-value | 0.227 | 0.536 | 0.759 | 0.427 | 0.317 | 0.300 | 0.632 | 0.639 |
| r | 0.32 | 0.03 | 0.09 | 0.24 | 0.29 | -0.31 | -0.04 | 0.04 | |
| Δ RBANS LR | p-value | 0.196 | 0.515 | 0.769 | 0.191 | 0.121 | 0.109 | 0.084 | 0.271 |
| r | 0.32 | 0.06 | 0.09 | 0.29 | 0.35 | -0.36 | 0.43 | -0.30 | |
| Δ RBANS SR | p-value | 0.181 | 0.360 | 0.079 | 0.019 | 0.055 | 0.073 | 0.776 | 0.216 |
| r | 0.40 | -0.10 | 0.45 | 0.51 | 0.40 | -0.37 | 0.24 | 0.05 | |
| Δ RBANS FR | p-value | 0.328 | 0.035 | 0.473 | 0.549 | 0.253 | 0.196 | 0.273 | 0.207 |
| r | 0.25 | 0.46 | -0.11 | 0.13 | 0.25 | -0.28 | -0.24 | 0.30 | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




