Submitted:
04 July 2025
Posted:
07 July 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
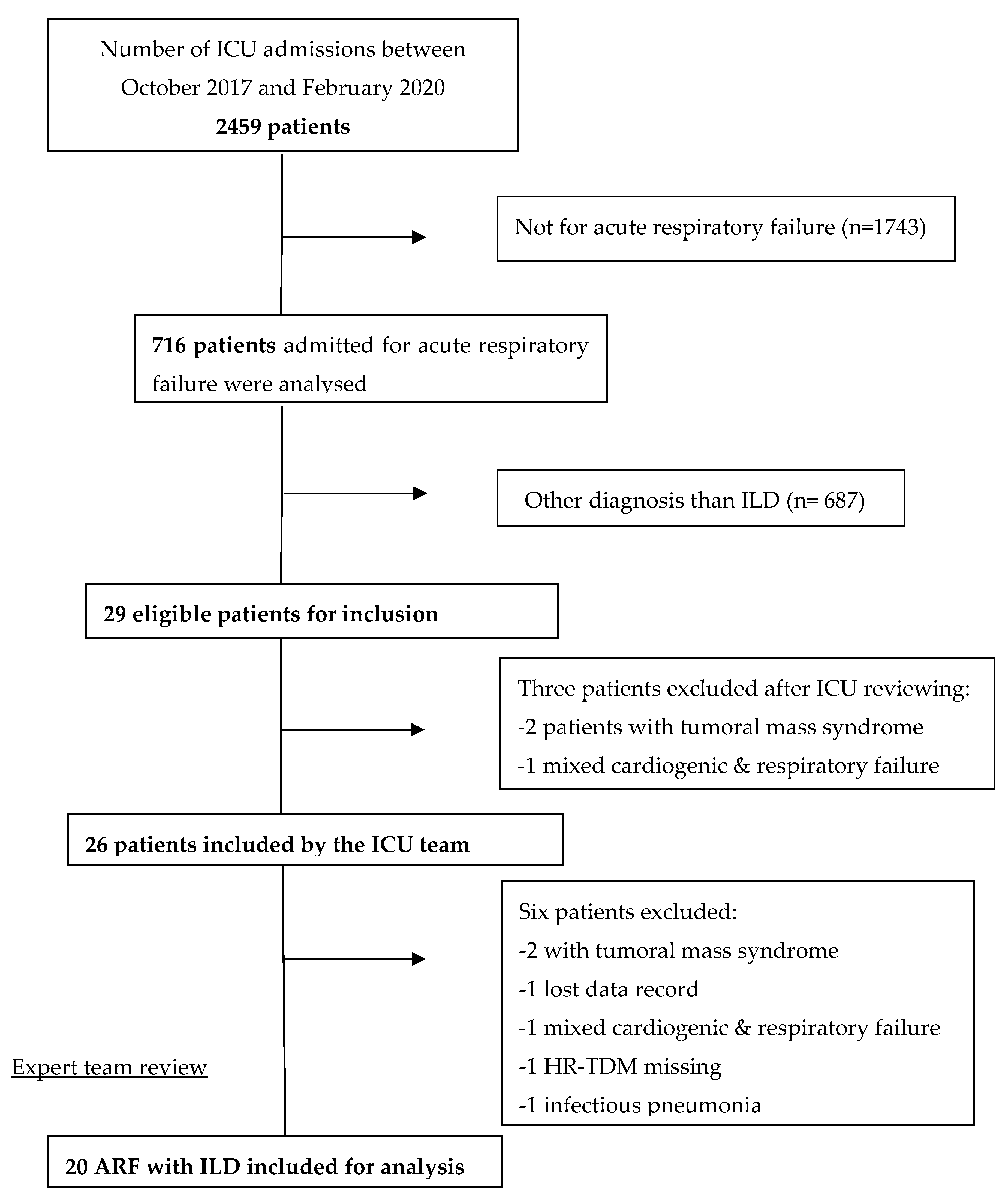
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Declarations
Conflicts of Interest
Abbreviations
| aMDA-5 | anti-MDA-5 antibodies |
| ATS | American Thoracic Society |
| ARDS | Acute Respiratory Distress Syndrom |
| ARF | Acute respiratory Failure |
| ATS | American Thoracic Society |
| BAL | bronchoalveolar lavage |
| CYC | cyclophosphamide |
| CTD | Connective tissue disease |
| COP | cryptogenic organizing pneumonia |
| DMD | Multidisciplinary discussion |
| ECMO | Extracorporeal membrane oxygenation |
| ERS | European Thoracic Society |
| HFNO | High-Flow nasal oxygen |
| HRCT | high-resolution computed tomography |
| ICU | Intensive Care Unit |
| ILD | Interstitial Lung Disease |
| MMF | mycophenolate mofetil |
| NSIP | Non-specific interstitial pneumonia |
| PaO2:FiO2 | ratio of the oxygen pressure to the fraction of inspired oxygen ratio |
| SOFA | Sepsis-related Organ Failure Assessment |
| PEP | Positive End-expiratory Pressure |
References
- American Thoracic Society, European Respiratory Society. American Thoracic Society/European Respiratory Society International Multidisciplinary Consensus Classification of the Idiopathic Interstitial Pneumonias. This joint statement of the American Thoracic Society (ATS), and the European Respiratory Society (ERS) was adopted by the ATS board of directors, June 2001 and by the ERS Executive Committee, June 2001. Am J Respir Crit Care Med 2002, 165, 277–304. [Google Scholar]
- Travis WD, Costabel U, Hansell DM, et al. An official American Thoracic Society/European Respiratory Society statement: Update of the international multidisciplinary classification of the idiopathic interstitial pneumonias. Am J Respir Crit Care Med 2013, 188, 733–748. [Google Scholar] [CrossRef] [PubMed]
- Coultas DB, Zumwalt RE, Black WC, Sobonya RE. The epidemiology of interstitial lung diseases. Am J Respir Crit Care Med 1994, 150, 967–972. [Google Scholar] [CrossRef]
- Huapaya JA, Wilfong EM, Harden CT, Brower RG, Danoff SK. Risk factors for mortality and mortality rates in interstitial lung disease patients in the intensive care unit. Eur Respir Rev 2018, 27, 180061. [Google Scholar] [CrossRef] [PubMed]
- Wijsenbeek M, Suzuki A, Maher TM. Interstitial lung diseases. Lancet 2022, 400, 769–786. [Google Scholar] [CrossRef]
- ARDS Definition Task Force, Ranieri VM, Rubenfeld GD, et al. Acute respiratory distress syndrome: the Berlin Definition. JAMA 2012, 307, 2526–2533. [Google Scholar]
- Bellani G, Laffey JG, Pham T, et al. Epidemiology, Patterns of Care, and Mortality for Patients With Acute Respiratory Distress Syndrome in Intensive Care Units in 50 Countries. JAMA 2016, 315, 788–800. [Google Scholar] [CrossRef]
- Meyer NJ, Gattinoni L, Calfee CS. Acute respiratory distress syndrome. Lancet 2021, 398, 622–637. [Google Scholar] [CrossRef]
- Gibelin A, Parrot A, Maitre B, et al. Acute respiratory distress syndrome mimickers lacking common risk factors of the Berlin definition. Intensive Care Med 2016, 42, 164–172. [Google Scholar] [CrossRef]
- Papazian L, Calfee CS, Chiumello D, et al. Diagnostic workup for ARDS patients. Intensive Care Med 2016, 42, 674–685. [Google Scholar] [CrossRef]
- Mikolasch TA, Garthwaite HS, Porter JC. Update in diagnosis and management of interstitial lung disease. Clin Med (Lond) 2017, 17, 146–153. [Google Scholar]
- Vincent JL, de Mendonça A, Cantraine F, et al. Use of the SOFA score to assess the incidence of organ dysfunction/failure in intensive care units: results of a multicenter, prospective study. Working group on “sepsis-related problems” of the European Society of Intensive Care Medicine. Crit Care Med 1998, 26, 1793–1800. [Google Scholar] [CrossRef] [PubMed]
- Amato MBP, Meade MO, Slutsky AS, et al. Driving pressure and survival in the acute respiratory distress syndrome. N Engl J Med 2015, 372, 747–755. [Google Scholar] [CrossRef] [PubMed]
- Gertler, R. Respiratory Mechanics. Anesthesiol Clin 2021, 39, 415–440. [Google Scholar] [CrossRef]
- Gannon WD, Lederer DJ, Biscotti M, et al. Outcomes and Mortality Prediction Model of Critically Ill Adults With Acute Respiratory Failure and Interstitial Lung Disease. Chest 2018, 153, 1387–1395. [Google Scholar] [CrossRef]
- Chang S-L, Tsai H-C, Lin F-C, Chao H-S, Chou C-W, Chang S-C. Clinical usefulness of bronchoalveolar lavage in patients with interstitial lung diseases: a pilot study. J Thorac Dis 2020, 12, 3125–3134. [Google Scholar] [CrossRef]
- Schnabel RM, van der Velden K, Osinski A, Rohde G, Roekaerts PMHJ, Bergmans DCJJ. Clinical course and complications following diagnostic bronchoalveolar lavage in critically ill mechanically ventilated patients. BMC Pulm Med 2015, 15, 107. [Google Scholar]
- Gerard L, Bidoul T, Castanares-Zapatero D, et al. Open Lung Biopsy in Nonresolving Acute Respiratory Distress Syndrome Commonly Identifies Corticosteroid-Sensitive Pathologies, Associated With Better Outcome. Crit Care Med 2018, 46, 907–914. [Google Scholar] [CrossRef]
- Maher, TM. Interstitial Lung Disease: A Review. JAMA 2024, 331, 1655–1665. [Google Scholar] [CrossRef]
- Raghu G, Remy-Jardin M, Richeldi L, et al. Idiopathic Pulmonary Fibrosis (an Update) and Progressive Pulmonary Fibrosis in Adults: An Official ATS/ERS/JRS/ALAT Clinical Practice Guideline. Am J Respir Crit Care Med 2022, 205, e18–47. [Google Scholar] [CrossRef]
- Petitpierre N, Beigelman C, Letovanec I, Lazor R. [Cryptogenic organizing pneumonia]. Rev Mal Respir 2016, 33, 703–717. [Google Scholar]
- Matsushita T, Mizumaki K, Kano M, et al. Antimelanoma differentiation-associated protein 5 antibody level is a novel tool for monitoring disease activity in rapidly progressive interstitial lung disease with dermatomyositis. Br J Dermatol 2017, 176, 395–402. [Google Scholar] [CrossRef] [PubMed]
- Chen Z, Wang X, Ye S. Tofacitinib in Amyopathic Dermatomyositis-Associated Interstitial Lung Disease. N Engl J Med 2019, 381, 291–293. [Google Scholar] [CrossRef]
- Naccache J-M, Jouneau S, Didier M, et al. Cyclophosphamide added to glucocorticoids in acute exacerbation of idiopathic pulmonary fibrosis (EXAFIP): a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Respir Med 2022, 10, 26–34. [Google Scholar] [CrossRef]
- Mankikian J, Caille A, Reynaud-Gaubert M, et al. Rituximab and mycophenolate mofetil combination in patients with interstitial lung disease (EVER-ILD): a double-blind, randomised, placebo-controlled trial. Eur Respir J 2023, 61, 2202071. [Google Scholar] [CrossRef]
- Urushiyama H, Jo T, Hasegawa W, et al. Effect of nintedanib on acute exacerbations of fibrosing interstitial lung diseases: a national database study in Japan. ERJ Open Res 2022, 8, 00209–02022. [Google Scholar]
- Mallick, S. Outcome of patients with idiopathic pulmonary fibrosis (IPF) ventilated in intensive care unit. Respir Med 2008, 102, 1355–1359. [Google Scholar] [CrossRef]
- Vuillard C, Pineton de Chambrun M, de Prost N, et al. Clinical features and outcome of patients with acute respiratory failure revealing anti-synthetase or anti-MDA-5 dermato-pulmonary syndrome: a French multicenter retrospective study. Ann Intensive Care 2018, 8, 87. [Google Scholar] [CrossRef]
- Radzikowska E, Fijolek J. Update on cryptogenic organizing pneumonia. Front Med (Lausanne) 2023, 10, 1146782. [Google Scholar]
- Dhanani Z, Gupta R. The Management of Interstitial Lung Disease in the ICU: A Comprehensive Review. J Clin Med 2024, 13, 6657. [Google Scholar] [CrossRef]
| Demographics | Median [IQR] or Mean (%) |
|---|---|
| Age | 70 [62–72] |
| Women | 5 (25) |
| Current smoker | 4 (20) |
| Allergic rhinitis | 1 (5) |
| Cardiovascular disease | 6 (30) |
| Obese | 2 (10) |
| Known cured or evolutive cancer disease | 5 (40) |
| Connective tissue disease | 3 (15) |
| Systemic sclerosis | 1 (5) |
| Rheumatoid arthritis | 1 (5) |
| Systemic lupus erythematosus | 1 (5) |
| Total ICU admission | 2459 |
| ILD initially diagnosed by the ICU team | 26 |
| Confirmed ILD among ICU’s team selection (%) | 20/26 (77) |
| Confirmed ILD among all ICU admission (%) | 20/2459 () |
| Confirmed ILD among ARF (%) | 20/687 ( |
| ILD disease | Related Main HRCT Pattern | N = 20 (%) |
|---|---|---|
| Idiopathic ILD | 7 (35) | |
| Idiopathic non-specific interstitial pneumonia | NSIP | 3 (15) |
| Cryptogenic organizing pneumonia | OP | 1 (5) |
| Idiopathic pulmonary fibrosis | UIP | 3 (15) |
| Auto-immune related ILD | 7 (35) | |
| CTD associated ILD | 6 (30) | |
| Systemic Lupus Erythematosus | Shrinking lung syndrome | 1 (5) |
| Rheumatoid arthritis | UIP | 1 (5) |
| Systemic sclerosis | Fibrotic NSIP | 2 (10) |
| Anti-synthetase syndrome | Fibrotic NSIP | 1 (5) |
| Anti-MDA5-antibody-associated amyopathic dermatomyositis |
NSIP | 1 (5) |
| Interstitial pneumonia with auto-immune features | Fibrotic NSIP | 1 (5) |
| Exposure-related | 3 (15) | |
| Hypersensitivity pneumonitis | HP | 1 (5) |
| Drug induced (docetaxel) | Fibrotic NSIP | 1 (5) |
| Radiation-induced lung injury | Fibrotic NSIP | 1 (5) |
| Others | 3 (15) | |
| Carcinomatous lymphangitis | Crazy paving | 3 (15) |
| Severity | Median [IQR] or Mean (%) |
|---|---|
| SOFA Score | 4 [3–7] |
| Criteria for ARDS | 19 (95) |
| Mild | 5 (25) |
| Moderate | 11 (55) |
| Severe | 3 (15) |
| Ventilatory support | |
| HFNO | 3 (15) |
| Invasive ventilation | 16 (80) |
| Veno-venous ECMO | 1 (5) |
| Ventilatory parameters | |
| PaO2:FiO2 | 174 [148–198] |
| PEP (cmH20) | 8 [8–10] |
| Driving Pressure (cmH20) | 19 [17–20] |
| Static compliance (mL/cmH20) | 21 [18–24] |
| Mortality | |
| Overall | 13 (65) |
| Among patient with invasive mechanical ventilation (n = 16) |
12 (75) |
| Among patient with auto-immune disease related ILD (n = 7) |
4 (57) |
| Among patient with steroid administration (n= 6) | 0 (0) |
| Confirmed ILD | ICU patients | p-value | |
|---|---|---|---|
| Number of patients | 20 | 2459 | |
| Deceased in the ICU | 13 | 632 | |
| Mortality rate (%) | 65 | 26 | <0.003 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




