Submitted:
30 June 2025
Posted:
02 July 2025
You are already at the latest version
Abstract
Keywords:
I. Introduction
II. Materials and Methods
2.1. Study Design and Setting
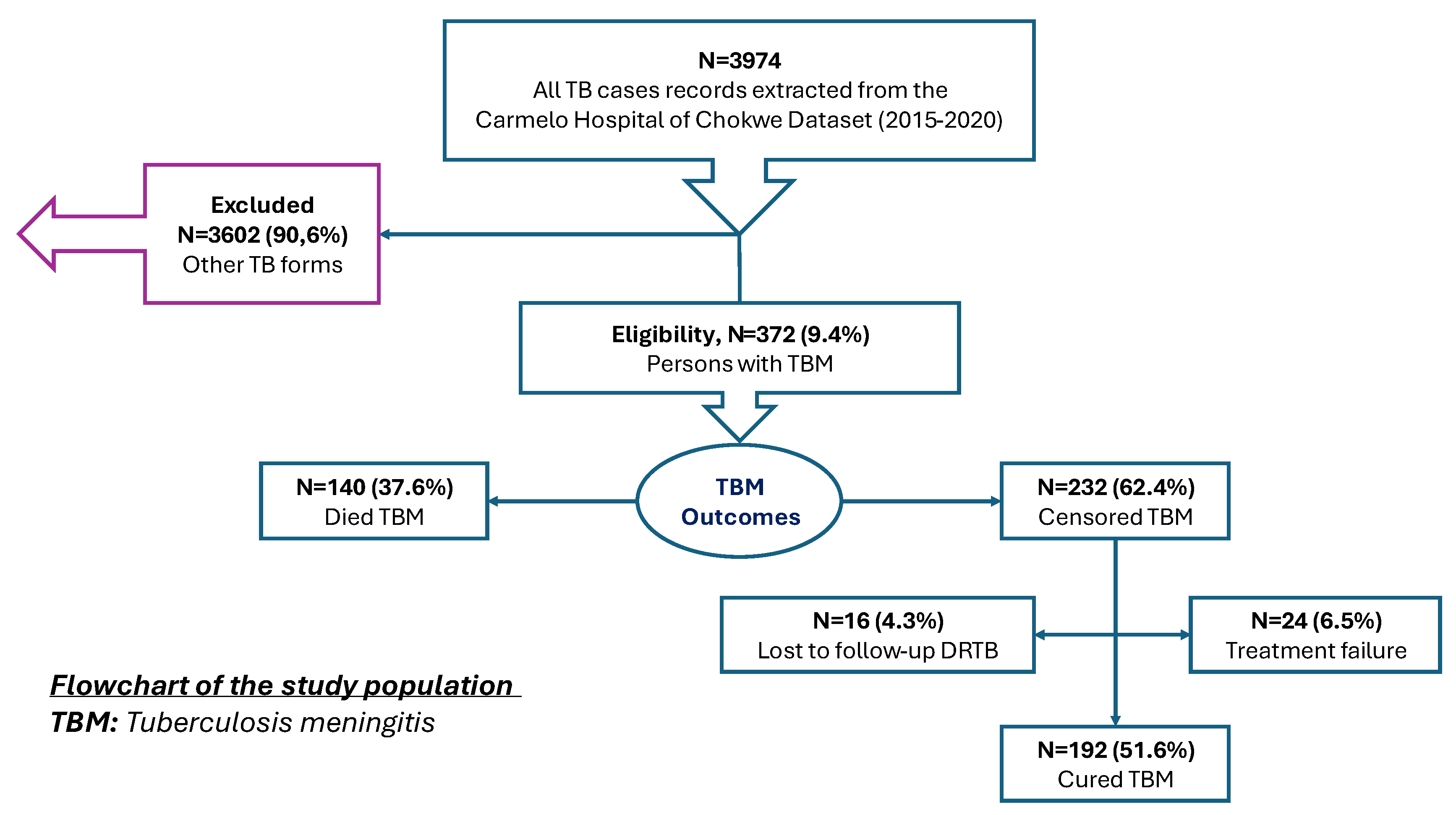
2.2. Study Population and Case Selection
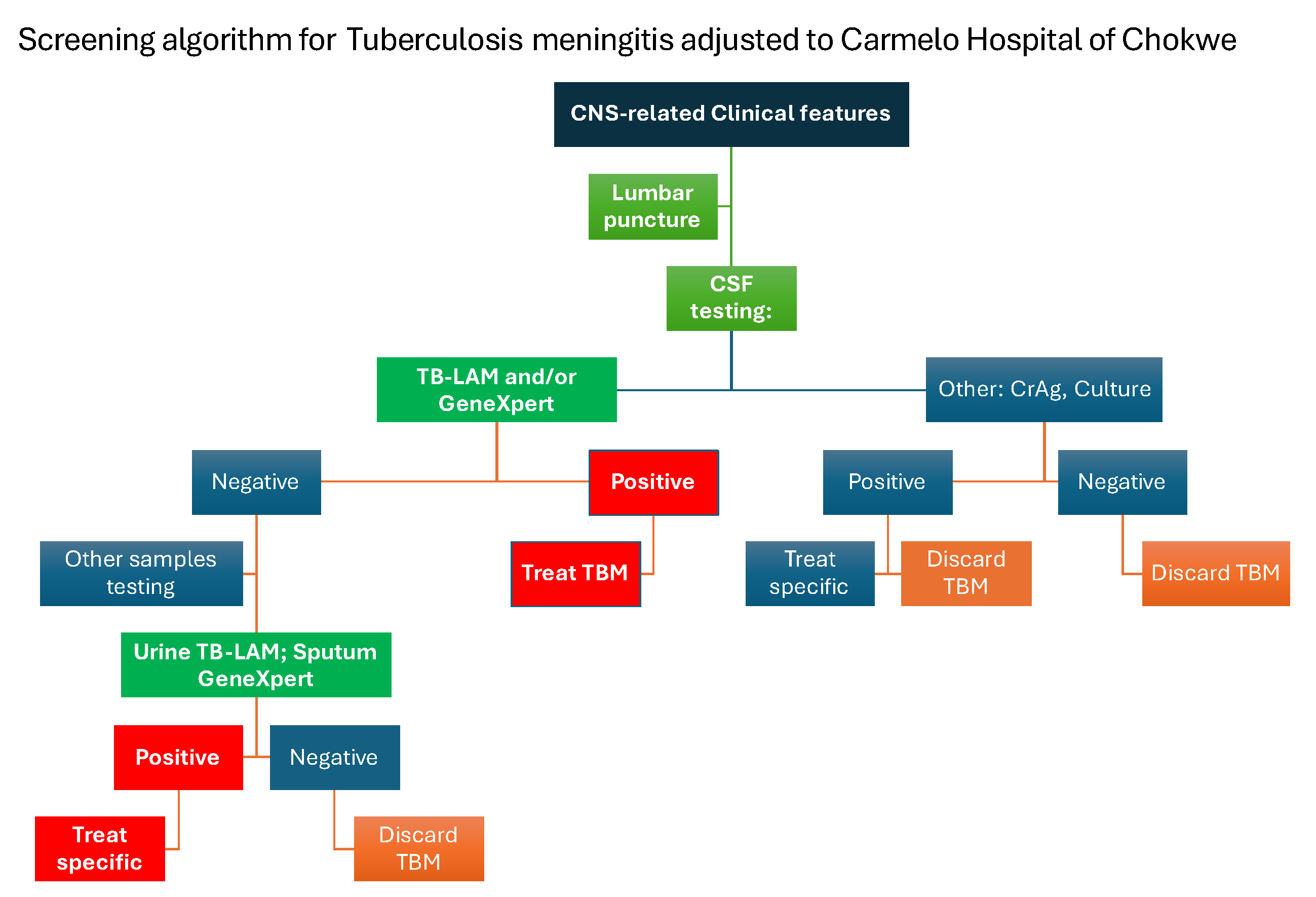
2.2.1. TBM Screening and Diagnostic Criteria
2.3. Data Collection and Variables
2.4. Outcomes definitions
- Died TBM: Patients with TBM who died during hospitalization or TB treatment.
- Cured TBM: Patients who completed treatment and had a documented favourable clinical response.
- Treatment failure: Clinical deterioration or persistent symptoms despite TB treatment.
- Lost to follow-up: Patients who discontinued treatment or were transferred to other facilities with unknown outcome.
- Censored: Patients still under treatment or with missing final outcome documentation.
2.5. Statistical Analysis
III. Results
3.1. Baseline Characteristics and Mortality Outcomes
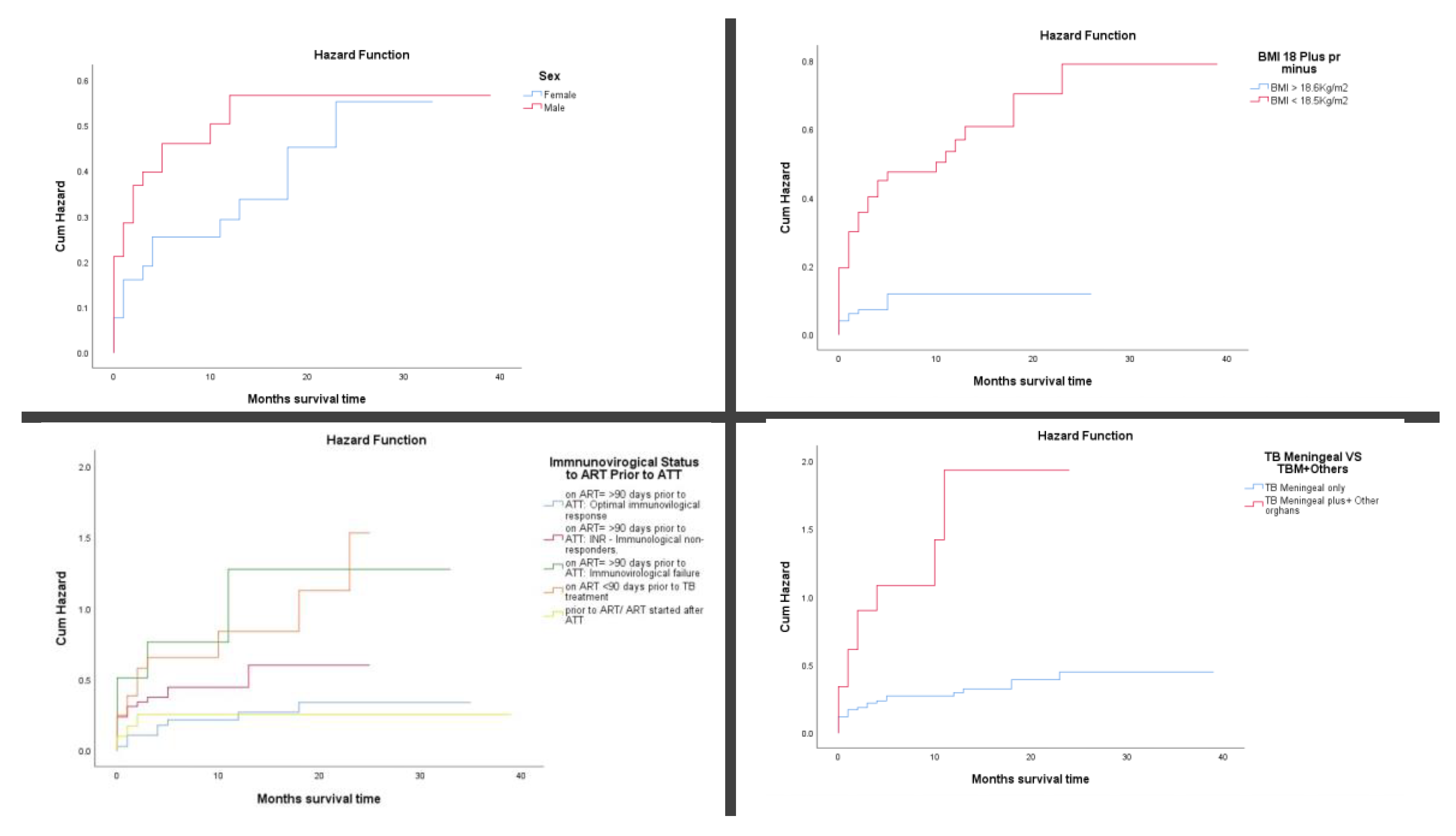
3.2. Predictors of Mortality in Patients with Tuberculous Meningitis
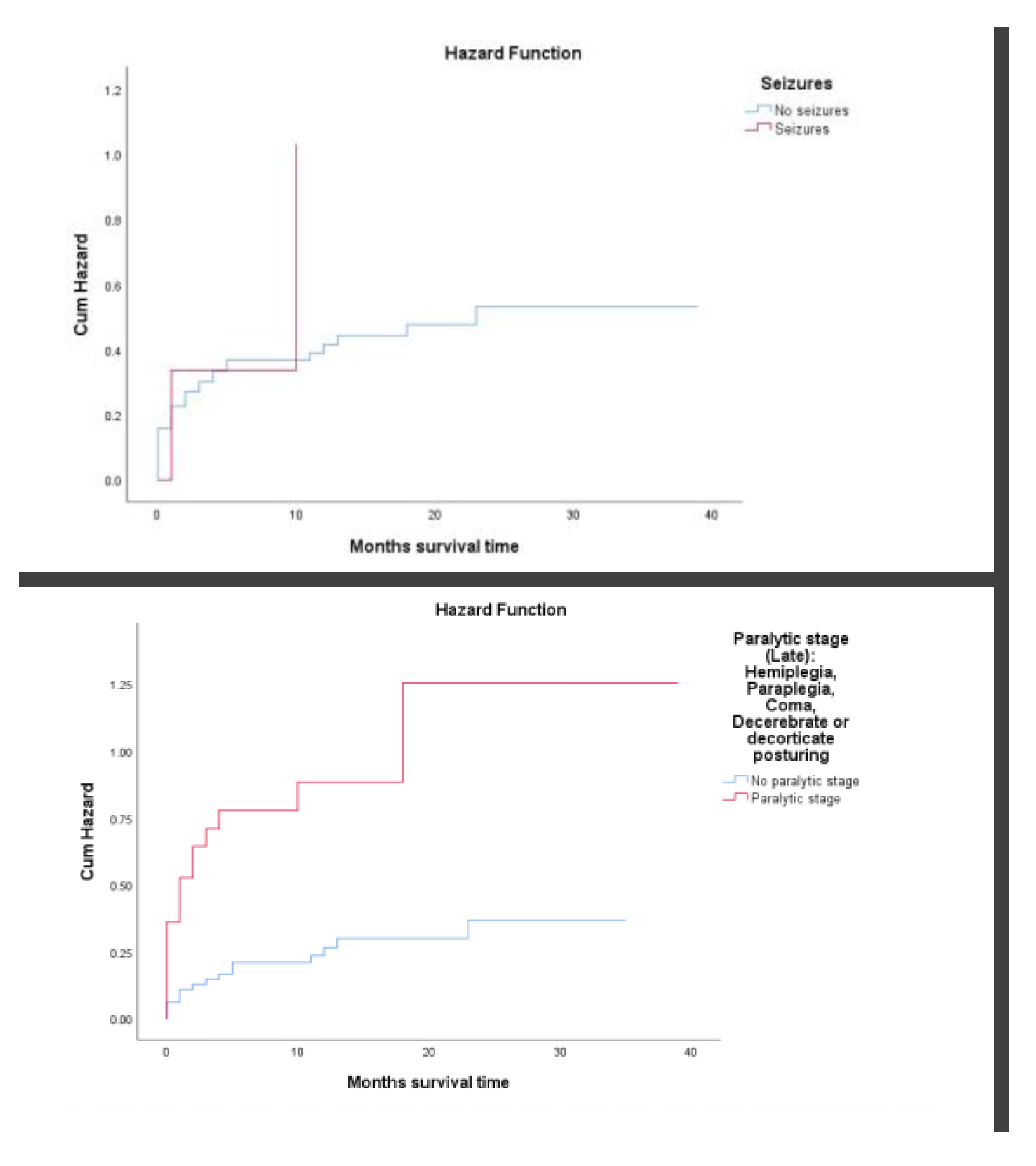
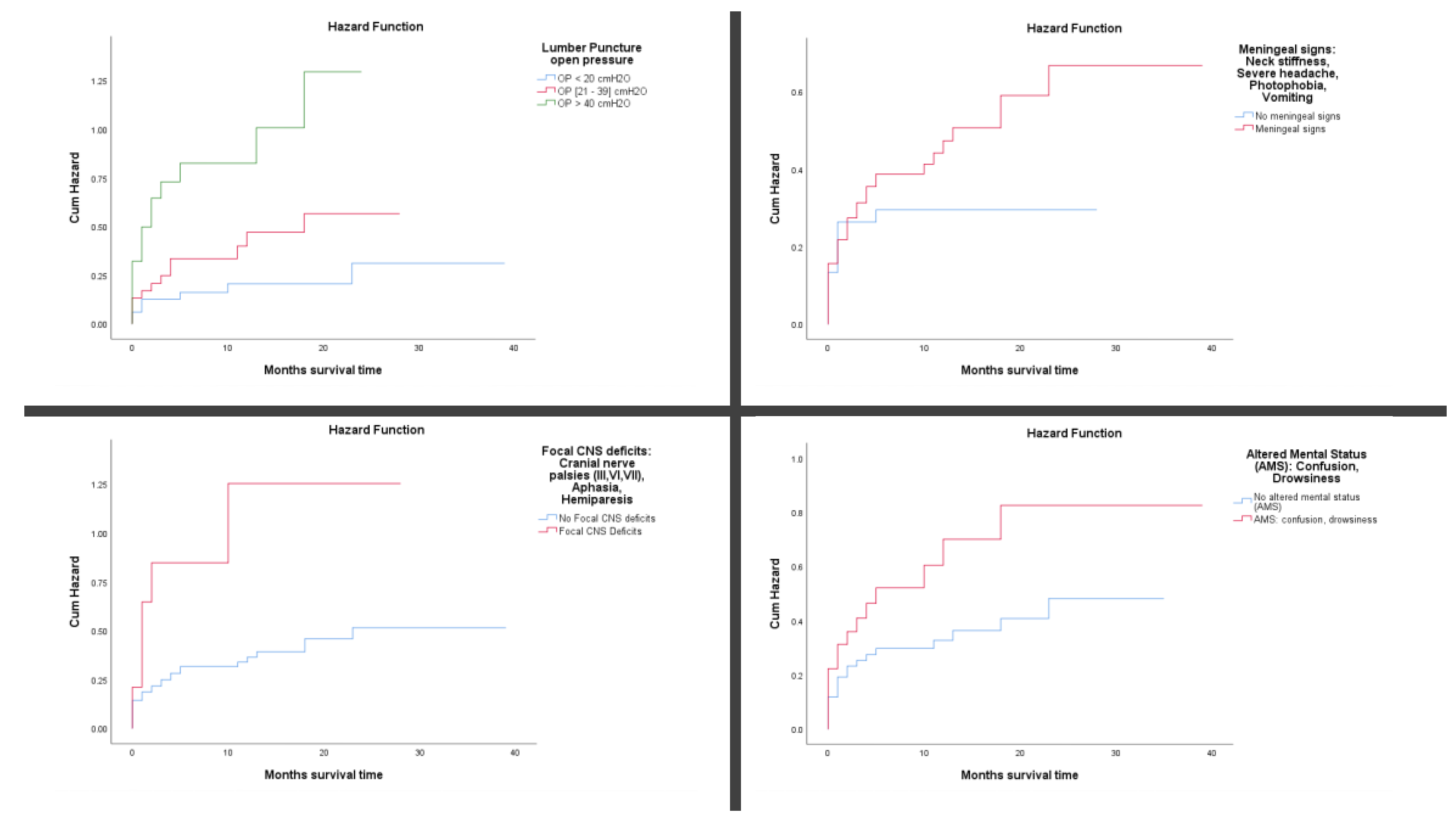
3.3. Cumulative Mortality Rate
IV. Discussion
4.1. Main Findings
4.2. Strength and Limitations
V. Conclusions and Recommendations
5.1. What the Bullet Points of This Study?
- Prioritize Early Diagnosis & Triage: Implement urgent lumbar puncture (LP) with cerebrospinal fluid (CSF) pressure measurement for patients presenting with central nervous system symptoms (e.g., headache, neck stiffness, altered mental status) in high TB/HIV burden areas. Expand access to and utilization of rapid point-of-care diagnostic tests like Xpert MTB/RIF Ultra and TB-LAM on CSF and other samples (e.g., urine, sputum) to confirm tuberculous meningitis (TBM) quickly. Actively use identified risk factors (male sex, malnutrition, disseminated disease) to flag high-risk patients for immediate, intensive management.
- Aggressively Manage Intracranial Hypertension: Routinely measure and actively manage elevated CSF pressure, identified as a critical predictor of death. Perform therapeutic LPs for pressures exceeding 40 cmH₂O. Train healthcare workers in managing intracranial hypertension using available interventions like acetazolamide or osmotic agents, especially where neurosurgical support is limited. Screen all TBM patients for signs of disseminated TB involving other organs, given its association with extremely high mortality.
- Integrate & Optimize HIV, TB, and Nutritional Care: Ensure timely initiation of antiretroviral therapy (ART) for HIV co-infected patients, generally within 2 weeks of starting TB treatment, while carefully weighing risks in severe neurological cases. Crucially, avoid starting ART less than 90 days before TB treatment initiation due to the associated higher mortality risk. Regularly monitor CD4 counts and viral loads to detect and promptly address immunovirological failure. Embed robust nutritional assessment and support, including therapeutic feeding programs, into routine TB/HIV care, particularly targeting patients with low BMI (<18.5 kg/m²).
- Standardize Neurological Assessment and Adjunctive Care: Develop and implement protocols for consistent staging of neurological severity at presentation. Train clinicians to recognize high-risk late-stage neurological signs (e.g., coma, decerebrate posturing, hemiplegia) that necessitate intensive monitoring and care. Ensure the consistent use of adjunctive corticosteroids per WHO guidelines in eligible TBM patients. Recognize focal neurological deficits and seizures as indicators of poor prognosis requiring heightened vigilance.
- Strengthen Health System Capacity: Invest in building sustainable diagnostic capacity in rural settings, including deploying affordable tools and maintaining reliable supplies of essential tests (Xpert, TB-LAM). Develop and disseminate context-specific clinical guidelines for TBM management tailored to the realities of resource-limited hospitals, emphasizing the critical steps identified (LP/pressure management, integrated care). Enhance training programs for frontline healthcare workers focusing on TBM recognition, safe LP procedures, complication management, and integrated HIV/TB/nutrition care. Strengthen referral pathways for complex cases requiring advanced care.
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Disclaimer
Abbreviations
| aHR | Adjusted hazard ratios |
| BMI | Body mass index |
| CI: | Confidence intervals |
| CSF | Cerebrospinal fluid |
| CHC: | Carmelo Hospital of Chókwè |
| CXR | Chest X-ray examination |
| ART | Antiretroviral therapy |
| IQR | Interquartile range |
| PLWH | People living with HIV |
| TBM | Tuberculous meningitis |
| WHO | World Health Organization |
References
- Lin, F.; Tuberculous meningitis diagnosis and treatment: classic approaches and high-throughput pathways. Front Immunol [Internet]. 2025 Jan 10 15. Available online: https://www.frontiersin.org/journals/immunology/articles/10.3389/fimmu.2024.1543009/full (accessed on 6 June 2025).
- Kalita J, Misra UK, Ranjan P. Predictors of long-term neurological sequelae of tuberculous meningitis: a multivariate analysis. European Journal of Neurology [Internet]. 2007, 14, 33–7. Available online: https://onlinelibrary.wiley.com/doi/abs/10.1111/j.1468-1331.2006.01534.x (accessed on 6 June 2025). [CrossRef] [PubMed]
- Manyelo CM, Solomons RS, Walzl G, Chegou NN. Tuberculous Meningitis: Pathogenesis, Immune Responses, Diagnostic Challenges, and the Potential of Biomarker-Based Approaches. Journal of Clinical Microbiology [Internet]. 2021, 18, 59. Available online: https://journals.asm.org/doi/10.1128/jcm.01771-20 (accessed on 6 June 2025).
- Isabel BE, Rogelio HP. Pathogenesis and immune response in tuberculous meningitis. Malays J Med Sci. 2014, 21, 4–10. [Google Scholar]
- Dastur DK, Manghani DK, Udani PM. Pathology and pathogenetic mechanisms in neurotuberculosis. Radiol Clin North Am. 1995, 33, 733–52. [Google Scholar] [CrossRef]
- Thwaites G, Chau TT, Mai NT, Drobniewski F, McAdam K, Farrar J. Tuberculous meningitis. J Neurol Neurosurg Psychiatry. 2000, 68, 289–99. [Google Scholar] [CrossRef] [PubMed]
- Cao WF, Leng EL, Liu SM, Zhou YL, Luo CQ, Xiang ZB, et al. Recent advances in microbiological and molecular biological detection techniques of tuberculous meningitis. Front Microbiol [Internet]. 2023. Available online: https://www.frontiersin.org/journals/microbiology/articles/10.3389/fmicb.2023.1202752/full (accessed on 6 June 2025).
- WHO. Global Tuberculosis Report 2024 [Internet]. Geneva: World Health Organization; 2024 Oct p. 68. Available online: https://www.who.int/teams/global-tuberculosis-programme/tb-reports/global-tuberculosis-report-2024 (accessed on 10 November 2024].
- Chin, JH. Tuberculous meningitis. Neurol Clin Pract [Internet]. 2014, 4, 199–205. Available online: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4121465/ (accessed on 6 June 2025). [CrossRef] [PubMed]
- Tenforde MW, Gertz AM, Lawrence DS, Wills NK, Guthrie BL, Farquhar C, et al. Mortality from HIV-associated meningitis in sub-Saharan Africa: a systematic review and meta-analysis. Journal of the International AIDS Society [Internet]. 2020, 23, e25416. Available online: https://onlinelibrary.wiley.com/doi/abs/10.1002/jia2.25416 (accessed on 6 June 2025). [CrossRef] [PubMed]
- Gottberg A von, Meintjes G. Meningitis: a frequently fatal diagnosis in Africa. The Lancet Infectious Diseases 2019, 19, 676–8. Available online: https://www.thelancet.com/journals/laninf/article/PIIS1473-3099(19)30111-2/fulltext (accessed on 6 June 2025). [CrossRef] [PubMed]
- PNCT. Relatorio Anual 2024. Maputo: MISAU; 2024 Maio p. 81.
- Programa Nacional de Controle da Tuberculose. Relatorio Anual 2023. Maputo: MISAU; 2023.
- PNCT. Plano Estratégico Nacional para acabar com a Tuberculose em Moçambique 2023 - 2030. Maputo: Ministério da Saúde; 2023 p. 129.
- Seid G, Alemu A, Dagne B, Gamtesa DF. Microbiological diagnosis and mortality of tuberculosis meningitis: Systematic review and meta-analysis. PLOS ONE 2023, 18, e0279203. Available online: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0279203 (accessed on 7 June 2025). [CrossRef] [PubMed]
- Maleki Rad M, Haddad M, Sheybani F, Shirazinia M, Dadgarmoghaddam M. Mortality predictors and diagnostic challenges in adult tuberculous meningitis: a retrospective cohort of 100 patients. Tropical Medicine and Health [Internet]. 2025, 53, 58. [CrossRef] [PubMed]
- Yasar KK, Pehlivanoglu F, Sengoz G. Predictors of mortality in tuberculous meningitis: a multivariate analysis of 160 cases. Int J Tuberc Lung Dis. 2010, 14, 1330–5. [Google Scholar]
- Kagimu E, Bangdiwala A, Kasibante J, Kabahubya M, Gakuru J, Timothy M, et al. Predictors of Early Mortality in HIV-associated Tuberculous Meningitis. Open Forum Infectious Diseases [Internet]. 2023, 10, ofad500. [CrossRef]
- George EL, Iype T, Cherian A, Chandy S, Kumar A, Balakrishnan A, et al. Predictors of mortality in patients with meningeal tuberculosis. Neurology India [Internet]. 2012, 60, 18, https://journals.lww.com/neur/fulltext/2012/60010/predictors_of_mortality_in_patients_with_meningeal.4.67aspx. [Google Scholar] [CrossRef]
- Wang L, Gu Z, Chen X, Yu X, Meng X. Analysis of risk factors for long-term mortality in patients with stage II and III tuberculous meningitis. BMC Infectious Diseases [Internet]. 2024, 24, 656. [Google Scholar] [CrossRef]
- Thao LTP, Heemskerk AD, Geskus RB, Mai NTH, Ha DTM, Chau TTH, et al. Prognostic Models for 9-Month Mortality in Tuberculous Meningitis. Clinical Infectious Diseases [Internet]. 2018, 66, 523–32. [Google Scholar] [CrossRef] [PubMed]
- Marais S, Pepper DJ, Schutz C, Wilkinson RJ, Meintjes G. Presentation and Outcome of Tuberculous Meningitis in a High HIV Prevalence Setting. PLOS ONE [Internet]. 2011, 6, e20077, https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0020077. [Google Scholar]
- Kalangi H, Boadla LR, Perlman DC, Yancovitz SR, George V, Salomon N. A true challenge: Disseminated tuberculosis with tuberculous meningitis in a patient with underlying chronic liver disease. IDCases [Internet]. 2024, 37, e02065, https://www.sciencedirect.com/science/article/pii/S2214250924001410. [CrossRef]
- Aslan S, Gulsun S, Atalay B. Disseminated tuberculosis complicated with tuberculous meningitis, miliary tuberculosis, and thoracal bone fracture while investigating a cervical lymphadenopathy. Tuberculosis: a hidden enemy? Neurosciences (Riyadh). 2010, 15, 129–30. [Google Scholar]
- Hilal T, Hurley P, McCormick M. Disseminated tuberculosis with tuberculous meningitis in an immunocompetent host. Oxf Med Case Reports [Internet]. 2014, 2014, 125–8, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4370030/. [Google Scholar] [CrossRef] [PubMed]
| Total N(%) | Death N(%) | Person-months (PM) |
Incidence per PM (95% CI) |
|
|---|---|---|---|---|
| Total | 372 (100.0) | 140 (37.63) | 3720 | 3.76 (3.14 - 3.76) |
| Sex | ||||
| Female | 162 (43.5) | 56 (40.0) | 2430 | 2.30 (1.92 - 2.66) |
| Male | 210 (56.5) | 84 (60.0) | 1890 | 4.44 (4.00 - 4.44) |
| BMI (Body Mass Index) | ||||
| BMI > 18.6Kg/m2 | 101 (27.2) | 11 (7.9) | 1111 | 0.99 (0.64 - 1.09) |
| BMI < 18.5Kg/m2 | 271 (72.8) | 129 (92.1) | 2710 | 4.76 (3.97 - 5.29) |
| Immnunovirogical Status to ART Prior to ATT | ||||
| on ART= >90 days prior to ATT: Optimal immunovilogical response | 139 (37.4) | 34 (24.3) | 1668 | 2.04 (1.29 - 2.22) |
| on ART= >90 days prior to ATT: INR - Immunological non-responders. | 90 (24.2) | 36 (25.7) | 810 | 4.44 (3.33 - 5.00) |
| on ART= >90 days prior to ATT: Immunovirological failure | 30 (8.1) | 20 (14.3) | 90 | 22.22 (6.06 - 22.22) |
| on ART <90 days prior to TB treatment | 50 (13.4) | 36 (25.7) | 450 | 8.00 (4.80 - 36.00) |
| prior to ART/ ART started after ATT | 63 (16.9) | 14 (10.0) | 693 | 2.02 (1.39 - 2.22) |
| TB Meningeal VS TBM+Others | ||||
| TB Meningeal only | 313 (84.1) | 93 (66.4) | 3756 | 2.48 (1.98 - 2.70) |
| TB Meningeal plus+ Other orghans | 59 (15.9) | 47 (33.6) | 118 | 39.83 (8.85 - 39.83) |
| Open Pressure Lumbar Puncture | ||||
| OP < 20 cmH2O | 136 (37.2) | 28 (20.0) | 1768 | 1.58 (1.08 - 1.87) |
| OP [21 - 39] cmH2O | 128 (35.0) | 48 (34.3) | 1344 | 3.57 (3.13 - 4.17) |
| OP > 40 cmH2O | 102 (27.9) | 64 (45.7) | 204 | 31.37 (12.55 - 62.75) |
|
Meningeal signs: (Neck stiffness, Severe headache, Photophobia, Vomiting) |
||||
| No meningeal signs | 96 (25.8) | 24 (17.1) | 864 | 2.78 (2.08 - 2.78) |
| Meningeal signs | 276 (74.2) | 116 (82.9) | 3036 | 3.82 (3.23 - 4.20) |
|
Focal CNS deficits: (Cranial nerve palsies [III,VI,VII], Aphasia, Hemiparesis) |
||||
| No Focal CNS deficits | 330 (88.7) | 112 (80.0) | 3630 | 3.09 (2.61 - 3.39) |
| Focal CNS Deficits | 42 (11.3) | 28 (20.0) | 84 | 33.33 (7.41 - 66.67) |
|
Altered Mental Status (AMS): Confusion, Drowsiness |
||||
| No altered mental status (AMS) | 252 (67.7) | 80 (57.1) | 2772 | 2.89 (2.44 - 2.89) |
| AMS: confusion, drowsiness | 120 (32.3) | 60 (42.9) | 1080 | 5.56 (4.17 - 5.56) |
| Seizures | ||||
| No seizures | 356 (96.2) | 128 (91.4) | 3916 | 3.27 (2.77 - 3.60) |
| Seizures | 14 (3.8) | 12 (8.6) | 140 | 8.57 (4.76 - 8.57) |
|
Paralytic stage (Late): Hemiplegia, Paraplegia, Coma, Decerebrate or decorticate posturing |
||||
| No paralytic stage | 250 (67.2) | 62 (44.3) | 3000 | 2.07 (1.65 - 2.25) |
| Paralytic stage | 122 (32.8) | 78 (55.7) | 366 | 21.31 (7.10 - 31.97) |
| Crude cHR (95% CI) | p-value | Adjusted aHR (95% CI) | p-value | |
|---|---|---|---|---|
| Sex | ||||
| Female | Reference | Reference | ||
| Male | 1.41 (1.00 - 1.98) | 0.048 | 1.80 (1.21 - 2.68) | 0.004 |
| BMI (Body Mass Index) | ||||
| BMI > 18.6Kg/m2 | Reference | Reference | ||
| BMI < 18.5Kg/m2 | 5.03 (2.72 - 9.32) | 0.000 | 2.75 (1.41 - 5.36) | 0.003 |
| Immnunovirogical Status to ART Prior to ATT | ||||
| on ART= >90 days prior to ATT: Optimal immunovilogical response | Reference | 0.000 | Reference | 0.000 |
| on ART= >90 days prior to ATT: INR - Immunological non-responders. | 1.99 (1.25 - 3.19) | 0.004 | 2.16 (1.29 - 3.62) | 0.003 |
| on ART= >90 days prior to ATT: Immunovirological failure | 3.88 (2.23 - 6.76) | 0.000 | 2.82 (1.54 - 5.16) | 0.001 |
| on ART <90 days prior to TB treatment | 3.55 (2.22 - 5.68) | 0.000 | 2.01 (1.19 - 3.38) | 0.009 |
| prior to ART/ ART started after ATT | 0.96 (0.51 - 1.78) | 0.886 | 0.69 (0.36 - 1.34) | 0.278 |
| TB Meningeal VS TBM+Others | ||||
| TB Meningeal only | Reference | Reference | ||
| TB Meningeal plus+ Other orghans | 4.27 (2.97 - 6.15) | 0.000 | 2.07 (1.31 - 3.29) | 0.002 |
| Open Pressure Lumbar Puncture | ||||
| OP < 20 cmH2O | Reference | 0.000 | Reference | 0.000 |
| OP [21 - 39] cmH2O | 2.01 (1.26 - 3.20) | 0.003 | 2.08 (1.25 - 3.46) | 0.005 |
| OP > 40 cmH2O | 4.47 (2.85 - 7.01) | 0.000 | 3.83 (2.33 - 6.31) | 0.000 |
|
Meningeal signs: (Neck stiffness, Severe headache, Photophobia, Vomiting) |
||||
| No meningeal signs | Reference | Reference | ||
| Meningeal signs | 1.59 (1.03 - 2.47) | 0.038 | 2.87 (1.74 - 4.75) | 0.000 |
|
Focal CNS deficits: (Cranial nerve palsies [III,VI,VII], Aphasia, Hemiparesis) |
||||
| No Focal CNS deficits | Reference | Reference | ||
| Focal CNS Deficits | 2.80 (1.83 - 4.26) | 0.000 | 1.46 (0.82 - 2.58) | 0.197 |
|
Altered Mental Status (AMS): (Confusion, Drowsiness) |
||||
| No altered mental status (AMS) | Reference | Reference | ||
| AMS: confusion, drowsiness | 1.78 (1.27 - 2.48) | 0.001 | 1.06 (0.69 - 1.62) | 0.793 |
| Seizures | ||||
| No seizures | Reference | Reference | ||
| Seizures | 2.50 (1.38 - 4.53) | 0.002 | 0.89 (0.44 - 1.81) | 0.748 |
|
Paralytic stage (Late): (Hemiplegia, Paraplegia, Coma, Decerebrate or decorticate posturing) |
||||
| No paralytic stage | Reference | Reference | ||
| Paralytic stage | 3.54 (2.53 - 4.96) | 0.000 | 2.15 (1.31 - 3.56) | 0.003 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




