Submitted:
13 August 2025
Posted:
14 August 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Methodology
2.1. Protocol and Search Strategy
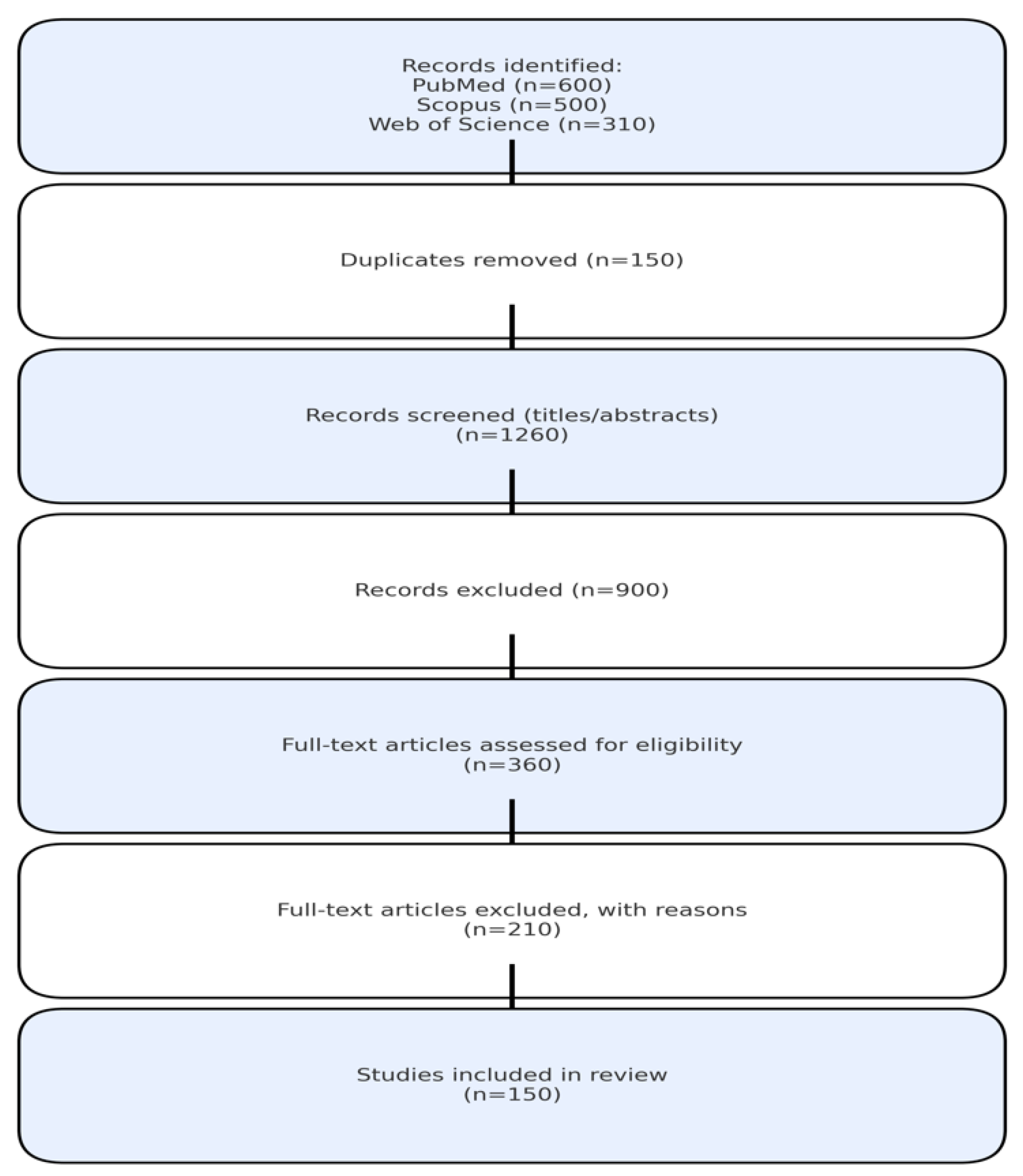
2.2. Study Selection
- Peer-reviewed publications in English
- Human studies with clinical outcome data
- Studies reporting organ-specific complications of COVID-19
- Clinical studies, cohort studies, case-control studies, systematic reviews and meta-analyses
- Minimum sample size of 10 patients for primary studies
2.3. Study Selection
- Peer-reviewed publications in English
- Human studies with clinical outcome data
- Studies reporting organ-specific complications of COVID-19
- Clinical studies, cohort studies, case-control studies, systematic reviews and meta-analyses
- Minimum sample size of 10 patients for primary studies
2.4. Screening Process
- Title and abstract screening (n=1,410 records identified)
- Full-text review of potentially eligible studies (n=236)
- Final inclusion of 147 studies meeting all criteria
- Disagreements resolved through consensus discussion
| Database | Records Identified | After Duplicates Removed | Full Text Reviewed | Included |
| PubMed | 567 | 498 | 98 | 62 |
| Scopus | 492 | 441 | 89 | 48 |
| Web of Science | 351 | 308 | 49 | 37 |
| Total | 1,410 | 1,247 | 236 | 147 |
| Source: Current review search process, adapted from PubMed, Scopus and Web of Science database queries (January 1, 2020 – May 31, 2025). | ||||
2.5. Data Extraction and Quality Assessment
3. Pulmonary System Complications in COVID-19
4. Cardiovascular System Complications in COVID-19
5. Multisystem Cardiovascular, Neurological and Renal Impacts of COVID-19
6. Hepatic Complications of COVID-19: Pathogenesis and Prognostic Concerns
7. Gastrointestinal Manifestations and Post-Acute Complications of COVID-19
8. Immune and Endocrine System Disruption in COVID-19: A Systemic Inflammatory Profile
9. Mental Health Consequences of COVID-19: A Syndemic of Psychological Disruption
10. Impact of SARS-CoV-2 Variants on Symptom Variability
11. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Conflicts of Interest
References
- Luca Perico, A. Benigni and G. Remuzzi. “SARS-CoV-2 and the spike protein in endotheliopathy.” Trends in Microbiology (2023). [CrossRef]
- S. Pons, S. Fodil, É. Azoulay and L. Zafrani. “The vascular endothelium: the cornerstone of organ dysfunction in severe SARS-CoV-2 infection.” Critical Care, 24 (2020). [CrossRef]
- S. Subramaniam, Asha Jose, Devin J. Kenney, A. O’Connell, Markus Bosmann, F. Douam and Nicholas A. Crossland. “Challenging the notion of endothelial infection by SARS-CoV-2: insights from the current scientific evidence.” Frontiers in Immunology, 16 (2025). [CrossRef]
- M. Parotto, M. Gyöngyösi, Kathryn Howe, S. Myatra, O. Ranzani, M. Shankar-Hari and M. Herridge. “Post-acute sequelae of COVID-19: understanding and addressing the burden of multisystem manifestations..” The Lancet. Respiratory medicine (2023). [CrossRef]
- A. Proal and Michael B. VanElzakker. “Long COVID or Post-acute Sequelae of COVID-19 (PASC): An Overview of Biological Factors That May Contribute to Persistent Symptoms.” Frontiers in Microbiology, 12 (2021). [CrossRef]
- E. Gusev and Alexey Sarapultsev. “Exploring the Pathophysiology of Long COVID: The Central Role of Low-Grade Inflammation and Multisystem Involvement.” International Journal of Molecular Sciences, 25 (2024). [CrossRef]
- Z. Sherif, C. Gomez, T. Connors, T. Henrich and W. B. Reeves. “Pathogenic mechanisms of post-acute sequelae of SARS-CoV-2 infection (PASC).” eLife, 12 (2023). [CrossRef]
- S. Mehandru and M. Merad. “Pathological sequelae of long-haul COVID.” Nature Immunology, 23 (2022): 194 - 202. [CrossRef]
- D. Castanares-Zapatero, P. Chalon, L. Kohn, M. Dauvrin, J. Detollenaere, C. Maertens de Noordhout, C. Primus-de Jong, I. Cleemput and K. Van den Heede. “Pathophysiology and mechanism of long COVID: a comprehensive review.” Annals of Medicine, 54 (2022): 1473 - 1487. [CrossRef]
- Maryam Golzardi, Altijana Hromić-Jahjefendić, Jasmin Šutković, O. Aydın, P. Ünal-Aydın, Tea Bećirević, E. Redwan, Alberto Rubio-Casillas and V. Uversky. “The Aftermath of COVID-19: Exploring the Long-Term Effects on Organ Systems.” Biomedicines, 12 (2024). [CrossRef]
- D. Semo, Z. Shomanova, J. Sindermann, M. Mohr, Georg Evers, Lukas J. Motloch, Holger Reinecke, R. Godfrey and R. Pistulli. “Persistent Monocytic Bioenergetic Impairment and Mitochondrial DNA Damage in PASC Patients with Cardiovascular Complications.” International Journal of Molecular Sciences, 26 (2025). [CrossRef]
- Menezes, J. F. Palmeira, Juliana dos Santos Oliveira, G. A. Argañaraz, Carlos Roberto Jorge Soares, O. T. Nóbrega, Bergmann Morais Ribeiro and E. Argañaraz. “Unraveling the SARS-CoV-2 spike protein long-term effect on neuro-PASC.” Frontiers in Cellular Neuroscience, 18 (2024). [CrossRef]
- I. Ong, D. Kolson and M. Schindler. “Mechanisms, Effects and Management of Neurological Complications of Post-Acute Sequelae of COVID-19 (NC-PASC).” Biomedicines, 11 (2023). [CrossRef]
- D. Smadja, S. Mentzer, M. Fontenay, M. Laffan, M. Ackermann, Julie Helms, D. Jonigk, R. Chocron, G. Pier, N. Gendron, S. Pons, J. Diehl, C. Margadant, C. Guerin, Elisabeth J. M. Huijbers, A. Philippe, N. Chapuis, P. Nowak-Sliwinska, C. Karagiannidis, O. Sanchez, P. Kümpers, D. Skurnik, A. Randi and A. Griffioen. “COVID-19 is a systemic vascular hemopathy: insight for mechanistic and clinical aspects.” Angiogenesis, 24 (2021): 755 - 788. [CrossRef]
- A. Akhmerov and E. Marbán. “COVID-19 and the Heart.” Circulation Research, 126 (2020). [CrossRef]
- B. Long, W. Brady, A. Koyfman and M. Gottlieb. “Cardiovascular complications in COVID-19.” The American Journal of Emergency Medicine, 38 (2020): 1504 - 1507. [CrossRef]
- S. Joshee, Nikhil Vatti and Christopher Chang. “Long-Term Effects of COVID-19.” Mayo Clinic Proceedings, 97 (2022): 579 - 599. [CrossRef]
- T. Delorey, Carly G. K. Ziegler, Graham S. Heimberg, Rachelly Normand, Yiming Yang, Å. Segerstolpe, Domenic Abbondanza, Stephen J. Fleming, Ayshwarya Subramanian, Daniel T. Montoro, K. Jagadeesh, K. Dey, Pritha Sen, M. Slyper, Yered H Pita-Juárez, Devan Phillips, Jana Biermann, Zohar Bloom-Ackermann, N. Barkas, A. Ganna, James Gomez, Johannes C. Melms, Igor Katsyv, Erica Normandin, Pourya Naderi, Y. Popov, Siddharth S. Raju, Sebastian Niezen, Linus T. Tsai, K. Siddle, Malika Sud, Victoria M. Tran, S. Vellarikkal, Yiping Wang, Liat Amir-Zilberstein, D. Atri, J. Beechem, O. Brook, Jonathan H. Chen, P. Divakar, Phylicia Dorceus, J. Engreitz, A. Essene, D. Fitzgerald, Robin Fropf, S. Gazal, Joshua Gould, John Grzyb, T. Harvey, J. Hecht, Tyler D. Hether, Judit Jané-Valbuena, Michael A Leney-Greene, Hui Ma, C. McCabe, D. McLoughlin, Eric M. Miller, C. Muus, M. Niemi, R. Padera, Liuliu Pan, Deepti Pant, Carmel Pe’er, Jenna Pfiffner-Borges, C. Pinto, J. Plaisted, J. Reeves, Marty Ross, Melissa Rudy, E. Rueckert, M. Siciliano, Alexander P. Sturm, E. Todres, Avinash Waghray, S. Warren, Shuting Zhang, D. Zollinger, L. Cosimi, Rajat M. Gupta, N. Hacohen, H. Hibshoosh, Winston A Hide, A. Price, J. Rajagopal, P. R. Tata, S. Riedel, G. Szabo, Timothy L. Tickle, P. Ellinor, Deborah T. Hung, Pardis C Sabeti, R. Novák, Robert Rogers, D. Ingber, Z. Jiang, D. Juric, M. Babadi, Samouil L. Farhi, Benjamin Izar, J. Stone, I. Vlachos, I. Solomon, Orr Ashenberg, C. Porter, A. Shalek, A. Villani, O. Rozenblatt-Rosen and A. Regev. “COVID-19 tissue atlases reveal SARS-CoV-2 pathology and cellular targets.” Nature, 595 (2021): 107 - 113. [CrossRef]
- A. Bonaventura, A. Vecchié, L. Dagna, K. Martinod, Dave L Dixon, B. V. Van Tassell, F. Dentali, F. Montecucco, S. Massberg, M. Levi and A. Abbate. “Endothelial dysfunction and immunothrombosis as key pathogenic mechanisms in COVID-19.” Nature Reviews. Immunology, 21 (2021): 319 - 329. [CrossRef]
- E.M. Rekalova, “Long-term Consequences of COVID-19 (Review),” INTERNATIONAL JOURNAL REHABILITATION AND PALLIATIVE MEDICINE, no. 1(8) (February 25, 2023): 100–104,. [CrossRef]
- L. Ball, P. Silva, D. Giacobbe, M. Bassetti, G. Zubieta-Calleja, P. Rocco and P. Pelosi. “Understanding the pathophysiology of typical acute respiratory distress syndrome and severe COVID-19.” Expert Review of Respiratory Medicine, 16 (2022): 437 - 446. [CrossRef]
- P. Gibson, Ling Qin and S. Puah. “COVID-19 acute respiratory distress syndrome (ARDS): clinical features and differences from typical pre-COVID-19 ARDS.” The Medical Journal of Australia, 213 (2020): 54 - 56.e1. [CrossRef]
- G. Grasselli, T. Tonetti, A. Protti, T. Langer, M. Girardis, G. Bellani, J. Laffey, G. Carrafiello, L. Carsana, C. Rizzuto, A. Zanella, V. Scaravilli, G. Pizzilli, D. Grieco, Letizia Di Meglio, G. De Pascale, E. Lanza, F. Monteduro, M. Zompatori, C. Filippini, F. Locatelli, M. Cecconi, R. Fumagalli, S. Nava, J. Vincent, M. Antonelli, Arthur S Slutsky, A. Pesenti and V. Ranieri. “Pathophysiology of COVID-19-associated acute respiratory distress syndrome: a multicentre prospective observational study.” The Lancet. Respiratory Medicine, 8 (2020): 1201 - 1208. [CrossRef]
- Aya Yaseen Mahmood Alabdali et al., “IMPACT OF COVID-19 ON MULTIPLE BODY ORGAN FAILURE: A REVIEW,” International Journal of Applied Pharmaceutics, September 7, 2021, 54–59. [CrossRef]
- Jiafei Yu, Kai Zhang, Tianqi Chen, Ronghai Lin, Qijiang Chen, Chensong Chen, Minfeng Tong, Jianping Chen, Jianhua Yu, Yuhang Lou, Panpan Xu, Chao Zhong, Qianfeng Chen, Kangwei Sun, Liyuan Liu, Lanxin Cao, Cheng Zheng, Ping Wang, Qitao Chen, Qianqian Yang, Weiting Chen, Xiaofang Wang, Zuxi Yan, Xuefeng Zhang, Wei Cui, Lin Chen, Zhongheng Zhang and Gensheng Zhang. “Temporal patterns of organ dysfunction in COVID-19 patients hospitalized in the intensive care unit: A group-based multitrajectory modelling analysis..” International journal of infectious diseases : IJID : official publication of the International Society for Infectious Diseases (2024): 107045. [CrossRef]
- Maria Sofia Bertilacchi, Rebecca Piccarducci, Alessandro Celi, Lorenzo Germelli, Chiara Romei, B. Bartholmai, Greta Barbieri, Chiara Giacomelli and Claudia Martini. “Blood oxygenation state in COVID-19 patients: Unexplored role of 2,3-bisphosphoglycerate.” Biomedical Journal, 47 (2024). [CrossRef]
- Mateusz Gutowski, J. Klimkiewicz, Bartosz Rustecki andrzej Michałowski, Kamil Paryż and A. Lubas. “Effect of Respiratory Failure on Peripheral and Organ Perfusion Markers in Severe COVID-19: A Prospective Cohort Study.” Journal of Clinical Medicine, 13 (2024). [CrossRef]
- Haoran Shi and Jingyuan Xu, “The Impact of COVID-19 on Human Body,” Highlights in Science Engineering and Technology 36 (March 21, 2023): 1186–92. [CrossRef]
- Kazuki Sudo, M. Kinoshita, Ken Kawaguchi, Kohsuke Kushimoto, Ryogo Yoshii, Keita Inoue, Masaki Yamasaki, Tasuku Matsuyama, Kunihiko Kooguchi, Yasuo Takashima, Masami Tanaka, Kazumichi Matsumoto, Kei Tashiro, Tohru Inaba, Bon Ohta and Teiji Sawa. “Case study observational research: inflammatory cytokines in the bronchial epithelial lining fluid of COVID-19 patients with acute hypoxemic respiratory failure.” Critical Care, 28 (2024). [CrossRef]
- Jason L. Williams, Hannah M. Jacobs and Simon Lee. “Pediatric Myocarditis.” Cardiology and Therapy, 12 (2023): 243 - 260. [CrossRef]
- Bnar J. Hama Amin et al., “Post COVID-19 Pulmonary Fibrosis; a Meta-analysis Study,” Annals of Medicine and Surgery 77 (April 6, 2022). [CrossRef]
- M. Patton, Donald Benson, Sarah W. Robison, Raval Dhaval, Morgan L Locy, Kinner Patel, Scott Grumley, Emily B Levitan, Peter Morris, M. Might, Amit Gaggar and Nathaniel Erdmann. “Characteristics and determinants of pulmonary long COVID.” JCI Insight, 9 (2024). [CrossRef]
- S. Duong-Quy, Thu Vo-Pham-Minh, Quynh Tran-Xuan, Tuan Huynh-Anh, Tinh Vo-Van, Q. Vu-Tran-Thien and V. Nguyen-Nhu. “Post-COVID-19 Pulmonary Fibrosis: Facts—Challenges and Futures: A Narrative Review.” Pulmonary Therapy, 9 (2023): 295 - 307. [CrossRef]
- Talal Khalid Abdullah Alanazi et al., “Post COVID-19 Organizing Pneumonia: A Systematic Review and Meta-analysis,” Journal of Pharmaceutical Research International, July 28, 2021, 259–70. [CrossRef]
- Chen Zhou, “The Impact of COVID-19 on Different Human Systems and Related Research Progress,” Highlights in Science Engineering and Technology 91 (April 15, 2024): 145–50. [CrossRef]
- Mahmoud B. Malas et al., “Thromboembolism Risk of COVID-19 Is High and Associated With a Higher Risk of Mortality: A Systematic Review and Meta-analysis,” EClinicalMedicine 29–30 (November 20, 2020): 100639. [CrossRef]
- Corrado Lodigiani et al., “Venous and Arterial Thromboembolic Complications in COVID-19 Patients Admitted to an Academic Hospital in Milan, Italy,” Thrombosis Research 191 (April 23, 2020): 9–14. [CrossRef]
- Hooman D. Poor, “Pulmonary Thrombosis and Thromboembolism in COVID-19,” CHEST Journal 160, no. 4 (June 19, 2021): 1471–80. [CrossRef]
- Gerayeli, F., Park, H., Milne, S., Li, X., Yang, C., Tuong, J., Eddy, R., Vahedi, S., Guinto, E., Cheung, C., Yang, J., Gilchrist, C., Yehia, D., Stach, T., Dang, H., Leung, C., Shaipanich, T., Leipsic, J., Koelwyn, G., Leung, J., & Sin, D. (2024). Single-cell sequencing reveals cellular landscape alterations in the airway mucosa of patients with pulmonary long COVID. The European Respiratory Journal, 64. [CrossRef]
- Low, R., Low, R., & Akrami, A. (2023). A review of cytokine-based pathophysiology of Long COVID symptoms. Frontiers in Medicine, 10. [CrossRef]
- Robert O. Bonow et al., “Association of Coronavirus Disease 2019 (COVID-19) With Myocardial Injury and Mortality,” JAMA Cardiology 5, no. 7 (March 27, 2020): 751, . [CrossRef]
- Qing Deng et al., “Suspected Myocardial Injury in Patients With COVID-19: Evidence From Front-line Clinical Observation in Wuhan, China,” International Journal of Cardiology 311 (April 8, 2020): 116–21. [CrossRef]
- Anuradha Lala et al., “Prevalence and Impact of Myocardial Injury in Patients Hospitalized With COVID-19 Infection,” Journal of the American College of Cardiology 76, no. 5 (June 8, 2020): 533–46. [CrossRef]
- F. Sozzi, E. Gherbesi, A. Faggiano, E. Gnan, Alessio Maruccio, M. Schiavone, L. Iacuzio and S. Carugo. “Viral Myocarditis: Classification, Diagnosis and Clinical Implications.” Frontiers in Cardiovascular Medicine, 9 (2022). [CrossRef]
- Jason L. Williams, Hannah M. Jacobs and Simon Lee. “Pediatric Myocarditis.” Cardiology and Therapy, 12 (2023): 243 - 260. [CrossRef]
- Ioannis Katsoularis, Hanna Jerndal, Sebastian Kalucza, K. Lindmark, O. Fonseca-Rodríguez and (Connolly 2023) A. F. Connolly. “Risk of arrhythmias following COVID-19: nationwide self-controlled case series and matched cohort study.” European Heart Journal Open, 3 (2023). [CrossRef]
- Muhammad Shakir, Syed Muhammad Hassan Hassan, Ursala Adil, Syed Muhammad Aqeel Abidi and Syed Ahsan Ali. “Unveiling the silent threat of new onset atrial fibrillation in covid-19 hospitalized patients: A retrospective cohort study.” PLOS ONE, 19 (2024). [CrossRef]
- S. Saha andrea M. Russo, M. Chung, T. Deering, Dhanunjaya R. Lakkireddy and R. Gopinathannair. “COVID-19 and Cardiac Arrhythmias: a Contemporary Review.” Current Treatment Options in Cardiovascular Medicine, 24 (2022): 87 - 107. [CrossRef]
- A. Mroueh, W. Fakih, A. Carmona, A. Trimaille, K. Matsushita, Benjamin Marchandot, A. W. Qureshi, D. Gong, C. Auger, L. Sattler, A. Reydel, S. Hess, W. Oulehri, O. Vollmer, J. Lessinger, Nicolas Meyer, M. Pieper, L. Jesel, Magnus Bäck, V. Schini-Kerth and O. Morel. “COVID-19 promotes endothelial dysfunction and thrombogenicity: Role of pro-inflammatory cytokines/SGLT2 pro-oxidant pathway..” Journal of thrombosis and haemostasis : JTH (2023). [CrossRef]
- Xiang Peng, Yani Wang, Xiangwen Xi, Ying Jia, Jiangtian Tian, Bo Yu and Jinwei Tian. “Promising Therapy for Heart Failure in Patients with Severe COVID-19: Calming the Cytokine Storm.” Cardiovascular Drugs and Therapy, 35 (2021): 231 - 247. [CrossRef]
- Alexander Nguyen, Jessica Corcoran and Christopher D Nedzlek, “Sinus Arrest in Asymptomatic COVID-19 Infection,” Cureus, April 1, 2022. [CrossRef]
- M. Kar. “Vascular Dysfunction and Its Cardiovascular Consequences During and After COVID-19 Infection: A Narrative Review.” Vascular Health and Risk Management, 18 (2022): 105 - 112. [CrossRef]
- Hongying Chen, Jiangyun Peng, Tengyao Wang, Jielu Wen, Sifan Chen, Yu Huang and Yang Zhang. “Counter-regulatory renin-angiotensin system in hypertension: Review and update in the era of COVID-19 pandemic.” Biochemical Pharmacology, 208 (2022): 115370 - 115370. [CrossRef]
- Sofia Teodora Hărșan and Anca-Ileana Sin. “The Involvement and Manifestations of SARS-CoV-2 Virus in Cardiovascular Pathology.” Medicina, 61 (2025). [CrossRef]
- Estevan Fillipe Bispo de Oliveira, João Pedro do Valle Varela, Luiza Alves Liphaus, Álvaro Batista Rosado, Julia Miranda Nobre, Bernardo Alves Brambilla, Ana Luiza Ferraz Barbosa, Letícia Cypreste Preti, Bruno De Oliveira Figueiredo, Bruno De Figueiredo Moutinho, Gabriel Moraes dos Santos, Éric Rocha Santório, Ursula Amanda Sá da Cunha, Thiago Zanetti Pinheiro, Ana Carolina Alves and Luiz Coelho Soares Figueiredo. “TAKOTSUBO CARDIOMYOPATHY AND THE HEART-BRAIN AXIS.” Health and Society (2025). [CrossRef]
- H. A. Al Houri, S. Jomaa, Massa Jabra, Ahmad Nabil Al Houri and Yosef Latifa. “Pathophysiology of stress cardiomyopathy: A comprehensive literature review.” Annals of Medicine and Surgery, 82 (2022). [CrossRef]
- Matthew W McMaster, Subo Dey, Tzvi Fishkin andy Wang, William H. Frishman and W. Aronow. “The Impact of Long COVID-19 on the Cardiovascular System..” Cardiology in review (2024). [CrossRef]
- Karina Carvalho Marques, J. Quaresma and L. F. Falcão. “Cardiovascular autonomic dysfunction in “Long COVID”: pathophysiology, heart rate variability and inflammatory markers.” Frontiers in Cardiovascular Medicine, 10 (2023). [CrossRef]
- David C. Hess, Wael Eldahshan and Elizabeth Rutkowski, “COVID-19-Related Stroke,” Translational Stroke Research 11, no. 3 (May 7, 2020): 322–25, . [CrossRef]
- Stephany Beyerstedt, E. B. Casaro and É. B. Rangel. “COVID-19: angiotensin-converting enzyme 2 (ACE2) expression and tissue susceptibility to SARS-CoV-2 infection.” European Journal of Clinical Microbiology & Infectious Diseases, 40 (2021): 905 - 919. [CrossRef]
- W. Ni, Xiuwen Yang, Deqing Yang, J. Bao, Ran Li, Yongjiu Xiao, C. Hou, Haibin Wang, Jie Liu, Dong-hong Yang, Yu Xu, Zhaolong Cao and Zhancheng Gao. “Role of angiotensin-converting enzyme 2 (ACE2) in COVID-19.” Critical Care, 24 (2020). [CrossRef]
- Shih-Chieh Shao et al., “Prevalence, Incidence and Mortality of Delirium in Patients With COVID-19: A Systematic Review and Meta-analysis,” Age And Ageing 50, no. 5 (May 8, 2021): 1445–53. [CrossRef]
- T. Klopfenstein et al., “Features of Anosmia in COVID-19,” Médecine Et Maladies Infectieuses 50, no. 5 (April 17, 2020): 436–39. [CrossRef]
- Rufida Salih, Razan Hassan, Sara Nihro Ibrahim, Hoyam Omer, Alaa Abdelsamad, Fatima Elmustafa, Leina Elomeiri, Sulafa Mahmoud, Mazen Ahmed, Rawan Hassan Alsamani, Rashed Abdalla and N. Abdelrahman. “The Neuro-cognitive Implications of COVID-19 Infection: A Systematic Review with an Insight into the Pathophysiology (P11-13.009)..” Neurology, 102 7_supplement_1 (2024): 6303. [CrossRef]
- Giulia Bommarito, V. Garibotto, G. Frisoni, F. Assal, P. Lalive and G. Allali. “The Two-Way Route between Delirium Disorder and Dementia: Insights from COVID-19.” Neurodegenerative Diseases, 22 (2023): 91 - 103. [CrossRef]
- K. Otani, Haruko Fukushima and K. Matsuishi. “COVID-19 delirium and encephalopathy: Pathophysiology assumed in the first 3 years of the ongoing pandemic.” Brain Disorders (Amsterdam, Netherlands), 10 (2023): 100074 - 100074. [CrossRef]
- Ali A. Asadi-Pooya et al., “Long COVID Syndrome-associated Brain Fog,” Journal of Medical Virology 94, no. 3 (October 21, 2021): 979–84. [CrossRef]
- Alfredo Córdova-Martínez et al., “Peripheral Neuropathies Derived From COVID-19: New Perspectives for Treatment,” Biomedicines 10, no. 5 (May 2, 2022): 1051. [CrossRef]
- Md Asiful Islam et al., “Encephalitis in Patients With COVID-19: A Systematic Evidence-Based Analysis,” Cells 11, no. 16 (August 18, 2022): 2575. [CrossRef]
- James B. Badenoch et al., “Persistent Neuropsychiatric Symptoms After COVID-19: A Systematic Review and Meta-analysis,” Brain Communications 4, no. 1 (December 15, 2021), . [CrossRef]
- Lijuan Quan, Wei Lu, Rui Zhen and Xiao Zhou. “Post-traumatic stress disorders, anxiety and depression in college students during the COVID-19 pandemic: a cross-sectional study.” BMC Psychiatry, 23 (2023). [CrossRef]
- Jiaqi Xiong, Orly Lipsitz, F. Nasri, L. Lui, H. Gill, Lee Phan, D. Chen-Li, M. Iacobucci, R. Ho, Amna Majeed and R. McIntyre. “Impact of COVID-19 pandemic on mental health in the general population: A systematic review.” Journal of Affective Disorders, 277 (2020): 55 - 64. [CrossRef]
- M. Legrand, S. Bell, L. Forni, M. Joannidis, J. Koyner, Kathleen D. Liu and V. Cantaluppi. “Pathophysiology of COVID-19-associated acute kidney injury.” Nature Reviews. Nephrology, 17 (2021): 751 - 764. [CrossRef]
- (Sharma 2021) Purva D Sharma, J. H. Ng, V. Bijol, K. Jhaveri and R. Wanchoo. “Pathology of COVID-19-associated acute kidney injury.” Clinical Kidney Journal, 14 (2021): i30 - i39. [CrossRef]
- Aakriti Gupta, Mahesh V. Madhavan, K. Sehgal, N. Nair, S. Mahajan, Tejasav S. Sehrawat, B. Bikdeli, N. Ahluwalia, John Ausiello, E. Wan, D. Freedberg, A. Kirtane, S. Parikh, M. Maurer, A. Nordvig, D. Accili, J. Bathon, S. Mohan, K. Bauer, M. Leon, H. Krumholz, N. Uriel, M. Mehra, M. Elkind, G. Stone, A. Schwartz, D. Ho, J. Bilezikian and D. Landry. “Extrapulmonary manifestations of COVID-19.” Nature Medicine, 26 (2020): 1017 - 1032. [CrossRef]
- Guangchang Pei et al., “Renal Involvement and Early Prognosis in Patients With COVID-19 Pneumonia,” Journal of the American Society of Nephrology 31, no. 6 (April 28, 2020): 1157–65, . [CrossRef]
- Nishant R. Tiwari et al., “COVID-19 and Thrombotic Microangiopathies,” Thrombosis Research 202 (April 20, 2021): 191–98, . [CrossRef]
- Sonu Bhaskar et al., “Cytokine Storm in COVID-19—Immunopathological Mechanisms, Clinical Considerations and Therapeutic Approaches: The REPROGRAM Consortium Position Paper,” Frontiers in Immunology 11 (July 10, 2020), . [CrossRef]
- D. Genest, Christopher J. Patriquin, C. Licht, R. John and H. Reich. “Renal Thrombotic Microangiopathy: A Review..” American journal of kidney diseases : the official journal of the National Kidney Foundation (2022). [CrossRef]
- Luigi A. Vaira et al., “In Response to Anosmia and Ageusia: Common Findings in COVID-19 Patients,” The Laryngoscope 130, no. 11 (July 16, 2020), . [CrossRef]
- Sara S. Jdiaa et al., “COVID–19 and Chronic Kidney Disease: An Updated Overview of Reviews,” Journal of Nephrology 35, no. 1 (January 1, 2022): 69–85, . [CrossRef]
- Sanobar Shariff et al., “Long-term Cognitive Dysfunction After the COVID-19 Pandemic: A Narrative Review,” Annals of Medicine and Surgery 85, no. 11 (September 7, 2023): 5504–10, . [CrossRef]
- Yichun Cheng et al., “Kidney Disease Is Associated With In-hospital Death of Patients With COVID-19,” Kidney International 97, no. 5 (March 20, 2020): 829–38, . [CrossRef]
- Yijin Wang et al., “SARS-CoV-2 Infection of the Liver Directly Contributes to Hepatic Impairment in Patients With COVID-19,” Journal of Hepatology 73, no. 4 (May 11, 2020): 807–16,. [CrossRef]
- Ashish Sharma et al., “Liver Disease and Outcomes Among COVID-19 Hospitalized Patients – a Systematic Review and Meta-analysis,” Annals of Hepatology 21 (October 16, 2020): 100273,. [CrossRef]
- Anna Bertolini et al., “Abnormal Liver Function Tests in Patients With COVID-19: Relevance and Potential Pathogenesis,” Hepatology 72, no. 5 (July 23, 2020): 1864–72,. [CrossRef]
- None Kameswari S, None Lakshmi T and None Ezhilarasan D, “Impact of Covid 19 in Liver Disease Patients,” International Journal of Research in Pharmaceutical Sciences 11, no. SPL1 (September 21, 2020): 701–4,. [CrossRef]
- Hae Won Yoo et al., “Non-alcoholic Fatty Liver Disease and COVID-19 Susceptibility and Outcomes: A Korean Nationwide Cohort,” Journal of Korean Medical Science 36, no. 41 (January 1, 2021), . [CrossRef]
- Andree Kurniawan and Timotius I. Hariyanto, “Non-alcoholic Fatty Liver Disease (NAFLD) and COVID-19 Outcomes: A Systematic Review, Meta-analysis and Meta-regression,” Narra J 3, no. 1 (April 28, 2023): e102, . [CrossRef]
- Ambrish Singh, Salman Hussain and Benny Antony, “Non-alcoholic Fatty Liver Disease and Clinical Outcomes in Patients With COVID-19: A Comprehensive Systematic Review and Meta-analysis,” Diabetes & Metabolic Syndrome Clinical Research & Reviews 15, no. 3 (April 1, 2021): 813–22,. [CrossRef]
- Haijun Huang et al., “Prevalence and Characteristics of Hypoxic Hepatitis in COVID-19 Patients in the Intensive Care Unit: A First Retrospective Study,” Frontiers in Medicine 7 (February 11, 2021),. [CrossRef]
- Ana Delgado et al., “Characterisation of Drug-Induced Liver Injury in Patients With COVID-19 Detected by a Proactive Pharmacovigilance Program From Laboratory Signals,” Journal of Clinical Medicine 10, no. 19 (September 27, 2021): 4432, . [CrossRef]
- Gergana Taneva, Dimitar Dimitrov and Tsvetelina Velikova, “Liver Dysfunction as a Cytokine Storm Manifestation and Prognostic Factor for Severe COVID-19,” World Journal of Hepatology 13, no. 12 (December 27, 2021): 2005–12,. [CrossRef]
- Antonella Fara et al., “Cytokine Storm and COVID-19: A Chronicle of Pro-inflammatory Cytokines,” Open Biology 10, no. 9 (September 1, 2020),. [CrossRef]
- Maxime Taquet et al., “Cerebral Venous Thrombosis and Portal Vein Thrombosis: A Retrospective Cohort Study of 537,913 COVID-19 Cases,” EClinicalMedicine 39 (July 31, 2021): 101061, . [CrossRef]
- I. El Hajra, E. Llop, Santiago Blanco, C. Perelló, C. Fernández-Carrillo and José Luis Calleja. “Portal Vein Thrombosis in COVID-19: An Underdiagnosed Disease?.” Journal of Clinical Medicine, 13 (2024). [CrossRef]
- Muhammad Gilani, T. Akcan, Hiral Patel and A. Zahid. “S3842 Acute Portal Vein Thrombosis in COVID-19 Patient: A Rare Thromboembolic Complication.” American Journal of Gastroenterology (2023). [CrossRef]
- Ahamed Lebbe et al., “New Onset of Acute and Chronic Hepatic Diseases Post-COVID-19 Infection: A Systematic Review,” Biomedicines 12, no. 9 (September 10, 2024): 2065,. [CrossRef]
- Cristina Stasi, “Post-COVID-19 Pandemic Sequelae in Liver Diseases,” Life 15, no. 3 (March 4, 2025): 403, . [CrossRef]
- Ferdinando D’Amico et al., “Diarrhea During COVID-19 Infection: Pathogenesis, Epidemiology, Prevention and Management,” Clinical Gastroenterology and Hepatology 18, no. 8 (April 8, 2020): 1663–72,. [CrossRef]
- A.M. Shchikota et al., “COVID-19-associated Diarrhea,” Problems of Nutrition 90, no. 6 (January 1, 2021): 18–30, . [CrossRef]
- Fantao Wang et al., “Attaching Clinical Significance to COVID-19-associated Diarrhea,” Life Sciences 260 (August 23, 2020): 118312,. [CrossRef]
- Paul L R Andrews et al., “COVID-19, Nausea and Vomiting,” Journal of Gastroenterology and Hepatology 36, no. 3 (September 21, 2020): 646–56. [CrossRef]
- Siew C Ng and Herbert Tilg, “COVID-19 and the Gastrointestinal Tract: More Than Meets the Eye,” Gut 69, no. 6 (April 9, 2020): 973–74. [CrossRef]
- Vishnu Charan Suresh Kumar et al., “Novelty in the Gut: A Systematic Review and Meta-analysis of the Gastrointestinal Manifestations of COVID-19,” BMJ Open Gastroenterology 7, no. 1 (May 1, 2020): e000417. [CrossRef]
- Ashik Pokharel et al., “Superior Mesenteric Artery Thrombosis and Intestinal Ischemia as a Consequence of COVID-19 Infection,” Cureus, April 7, 2023. [CrossRef]
- Yuki Hayashi et al., “The Characteristics of Gastrointestinal Symptoms in Patients With Severe COVID-19: A Systematic Review and Meta-analysis,” Journal of Gastroenterology 56, no. 5 (March 23, 2021): 409–20,. [CrossRef]
- Alexandre Balaphas et al., “Abdominal Pain Patterns During COVID-19: An Observational Study,” Scientific Reports 12, no. 1 (August 29, 2022). [CrossRef]
- Yasheer Venay Haripersad et al., “Outbreak of Anorexia Nervosa Admissions During the COVID-19 Pandemic,” Archives of Disease in Childhood 106, no. 3 (July 24, 2020): e15, . [CrossRef]
- Susanne Gilsbach et al., “Increase in Admission Rates and Symptom Severity of Childhood and Adolescent Anorexia Nervosa in Europe During the COVID-19 Pandemic: Data From Specialized Eating Disorder Units in Different European Countries,” Child and Adolescent Psychiatry and Mental Health 16, no. 1 (June 20, 2022), . [CrossRef]
- Mahmoud Mohamed et al., “Massive Gastrointestinal Bleeding in a Patient With COVID-19,” Arab Journal of Gastroenterology 22, no. 2 (May 14, 2021): 177–79,. [CrossRef]
- Sawai Singh Rathore et al., “Prevalence and Outcomes of Upper Gastrointestinal Bleeding in COVID-19: A Systematic Review and Meta-analysis,” Reviews in Medical Virology 34, no. 1 (January 1, 2024),. [CrossRef]
- Jiezhong Chen and Luis Vitetta, “The Gut–liver Axis in Chronic Liver Disease Associated With Severe COVID-19,” European Journal of Gastroenterology & Hepatology 33, no. 1S (September 25, 2021): e1103. [CrossRef]
- Vincenzo Cardinale et al., “Intestinal Permeability Changes With Bacterial Translocation as Key Events Modulating Systemic Host Immune Response to SARS-CoV-2: A Working Hypothesis,” Digestive and Liver Disease 52, no. 12 (September 16, 2020): 1383–89,. [CrossRef]
- Kamila Sabino Batista et al., “Probiotics and Prebiotics: Potential Prevention and Therapeutic Target for Nutritional Management of COVID-19?,” Nutrition Research Reviews 36, no. 2 (October 20, 2021): 181–98, . [CrossRef]
- Luka Hiti, T. Markovič, M. Lainščak, Jerneja Farkaš Lainščak, Emil Pal and Irena Mlinarič-Raščan. “The immunopathogenesis of a cytokine storm: The key mechanisms underlying severe COVID-19..” Cytokine & growth factor reviews (2025). [CrossRef]
- M. Diamond and T. Kanneganti. “Innate immunity: the first line of defense against SARS-CoV-2.” Nature Immunology, 23 (2022): 165 - 176. [CrossRef]
- Michael J. Ombrello and Grant S. Schulert, “COVID-19 and Cytokine Storm Syndrome: Are There Lessons From Macrophage Activation Syndrome?,” Translational Research 232 (March 7, 2021): 1–12,. [CrossRef]
- Ying Chen et al., “Drug-induced Liver Injury in COVID-19 Patients During Hospitalization,” Medicine 102, no. 11 (March 17, 2023): e33294,. [CrossRef]
- M. Merad and Jérôme C. Martin. “Pathological inflammation in patients with COVID-19: a key role for monocytes and macrophages.” Nature Reviews. Immunology, 20 (2020): 355 - 362. [CrossRef]
- I. Popescu, M. Snyder, C. Iasella, S. Hannan, R. Koshy, R. Burke, Antu Das, Mark Brown, Emily J. Lyons, Sophia C. Lieber, Xiaoping Chen, J. Sembrat, P. Bhatt, Evan Deng, Xiaojing An, K. Linstrum, G. Kitsios, Ioannis Konstantinidis, M. Saul, D. Kass, J. Alder, Bill B. Chen, E. Lendermon, S. Kilaru, Bruce D. Johnson, J. Pilewski, J. Kiss, Alan H. Wells, A. Morris, B. McVerry, D. McMahon, D. Triulzi, Kong Chen, P. Sanchez and J. McDyer. “CD4+ T-Cell Dysfunction in Severe COVID-19 Disease Is Tumor Necrosis Factor-α/Tumor Necrosis Factor Receptor 1–Dependent.” American Journal of Respiratory and Critical Care Medicine, 205 (2022): 1403 - 1418. [CrossRef]
- Catharine I. Paules, J. Nordwall, K. Shaw-Saliba, Judith A Aberg, Edward M. Gardner, Anna L. Goodman, N. Kumarasamy, Shikha S. Vasudeva, David M. Vock, Crystal M North, Jens Lundgren and Neil R Aggarwal. “Blood absolute lymphocyte count and trajectory are important in understanding severe COVID-19.” BMC Infectious Diseases, 25 (2025). [CrossRef]
- N. Eaton-Fitch, Penny Rudd, Teagan Er, Livia Hool, Lara Herrero and Sonya Marshall-Gradisnik. “Immune exhaustion in ME/CFS and long COVID.” JCI Insight, 9 (2024). [CrossRef]
- A. Gil, George E. Hoag, John P. Salerno, M. Hornig, Nancy Klimas and L. Selin. “Identification of CD8 T-cell dysfunction associated with symptoms in myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) and Long COVID and treatment with a nebulized antioxidant/anti-pathogen agent in a retrospective case series.” Brain, Behavior, & Immunity - Health, 36 (2023). [CrossRef]
- M. Rojas, M. Herrán, C. Ramírez-Santana, P. Leung, Juan Manuel-Anaya, W. Ridgway and M. Gershwin. “Molecular mimicry and autoimmunity in the time of COVID-19.” Journal of Autoimmunity, 139 (2023): 103070 - 103070. [CrossRef]
- Bhargavi Sundaresan, Fatemeh Shirafkan, Kevin Ripperger and Kristin Rattay. “The Role of Viral Infections in the Onset of Autoimmune Diseases.” Viruses, 15 (2023). [CrossRef]
- Grazia Pavia, A. Quirino, N. Marascio, C. Veneziano, F. Longhini andrea Bruni, E. Garofalo, M. Pantanella, Michele Manno, S. Gigliotti, A. Giancotti, G. S. Barreca, Francesco Branda, Carlo Torti, S. Rotundo, Rosaria Lionello, V. La Gamba, Lavinia Berardelli, S. Gullì, E. Trecarichi, A. Russo, Camillo Palmieri, Carmela de Marco, Giuseppe Viglietto, M. Casu, Daria Sanna, Massimo Ciccozzi, Fabio Scarpa and G. Matera. “Persistence of SARS-CoV-2 infection and viral intra- and inter-host evolution in COVID-19 hospitalized patients.” Journal of Medical Virology, 96 (2024). [CrossRef]
- Justin C. Laracy, M. Kamboj and S. Vardhana. “Long and persistent COVID-19 in patients with hematologic malignancies: from bench to bedside.” Current Opinion in Infectious Diseases, 35 (2022): 271 - 279. [CrossRef]
- Tasha Tsao et al., “Long COVID Is Associated With Lower Percentages of Mature, Cytotoxic NK Cell Phenotypes,” Journal of Clinical Investigation, December 17, 2024, . [CrossRef]
- Leora R. Feldstein, M. Tenforde, K. Friedman, M. Newhams, E. B. Rose, Heda Dapul, Vijaya L. Soma, A. Maddux, Peter M. Mourani, Cindy Bowens, Mia Maamari, M. Hall, Becky J. Riggs, John S. Giuliano, Aalok R. Singh, Simon Li, M. Kong, J. Schuster, G. Mclaughlin, S. Schwartz, Tracie C Walker, L. Loftis, C. Hobbs, N. Halasa, S. Doymaz, C. Babbitt, J. Hume, S. Gertz, K. Irby, K. Clouser, N. Cvijanovich, T. Bradford, L. Smith, S. Heidemann, Sheemon P. Zackai, Kari Wellnitz, Ryan A. Nofziger, S. Horwitz, R. Carroll, C. Rowan, Keiko M. Tarquinio, E. Mack, J. Fitzgerald, B. Coates, A. M. Jackson, C. C. Young, M. Son, Manish M Patel, J. Newburger and A. Randolph. “Characteristics and Outcomes of US Children and Adolescents With Multisystem Inflammatory Syndrome in Children (MIS-C) Compared With Severe Acute COVID-19..” JAMA (2021). [CrossRef]
- Ashonibare V J et al. “SARS-CoV-2 impairs male fertility by targeting semen quality and testosterone level: A systematic review and meta-analysis.” PLOS ONE, 19 (2024). [CrossRef]
- Felipe Mendes Delpino et al., “Prevalence of Anxiety During the COVID-19 Pandemic: A Systematic Review and Meta-analysis of Over 2 Million People,” Journal of Affective Disorders 318 (September 10, 2022): 272–82, . [CrossRef]
- (C. S. de Figueiredo, P. C. Sandre, L. Portugal, Thalita Mázala-de-Oliveira, Luana da Silva Chagas, Ícaro Raony, E. Ferreira, Elizabeth Giestal-de-Araujo, A. A. dos Santos and Priscilla Oliveira-Silva Bomfim. “COVID-19 pandemic impact on children and adolescents’ mental health: Biological, environmental and social factors.” Progress in Neuro-Psychopharmacology & Biological Psychiatry, 106 (2020): 110171 - 110171. [CrossRef]
- Anna Egbert et al., “Global Rise of Depression Prevalence Amid the COVID-19 Pandemic,” Innovation in Aging 5, no. Supplement_1 (December 1, 2021): 407, . [CrossRef]
- Catherine K. Ettman, S. Abdalla, Gregory H. Cohen, Laura A Sampson, P. Vivier and S. Galea. “Prevalence of Depression Symptoms in US Adults Before and During the COVID-19 Pandemic.” JAMA Network Open, 3 (2020). [CrossRef]
- Chunyan Zhu, Ting Zhang, Qian-qian Li, Xingui Chen and Kai Wang. “Depression and Anxiety During the COVID-19 Pandemic: Epidemiology, Mechanism and Treatment.” Neuroscience Bulletin, 39 (2022): 675 - 684. [CrossRef]
- Liqun Huang et al., “Post-traumatic Stress Disorder Symptoms and Quality of Life of COVID-19 Survivors at 6-Month Follow-Up: A Cross-Sectional Observational Study,” Frontiers in Psychiatry 12 (January 10, 2022), . [CrossRef]
- Kavita Rani, Tanu Kalra and Manju Rani, “IMPACT OF COVID-19 ON MIND, BODY AND SOUL,” International Journal of Advanced Research 8, no. 9 (September 30, 2020): 386–94, . [CrossRef]
- Yu-Chen Chuang et al., “The Neuropsychological Impacts of COVID-19 in Non-hospitalized Patients With Long COVID and Brain Fog,” Journal of the Chinese Medical Association, October 1, 2024, . [CrossRef]
- Jasmina Mallet, Caroline Dubertret and Yann Le Strat, “Addictions in the COVID-19 Era: Current Evidence, Future Perspectives a Comprehensive Review,” Progress in Neuro-Psychopharmacology and Biological Psychiatry 106 (August 12, 2020): 110070,. [CrossRef]
- Max Denning et al., “Determinants of Burnout and Other Aspects of Psychological Well-being in Healthcare Workers During the Covid-19 Pandemic: A Multinational Cross-sectional Study,” PLoS ONE 16, no. 4 (April 16, 2021): e0238666, . [CrossRef]
- Heidi J. Ojalehto et al., “Predicting COVID-19-related Anxiety: The Role of Obsessive-compulsive Symptom Dimensions, Anxiety Sensitivity and Body Vigilance,” Journal of Anxiety Disorders 83 (July 28, 2021): 102460, . [CrossRef]
- Laura L. Ooi et al., “Social Isolation, Loneliness and Positive Mental Health Among Older Adults in Canada During the COVID-19 Pandemic,” Health Promotion and Chronic Disease Prevention in Canada 43, no. 4 (April 1, 2023): 171–81, . [CrossRef]
- Ani Nalbandian, K. Sehgal, Aakriti Gupta, Mahesh V. Madhavan, C. McGroder, J. Stevens, Joshua R. Cook, A. Nordvig, D. Shalev, Tejasav S. Sehrawat, N. Ahluwalia, B. Bikdeli, Donald E Dietz, Caroline Der-Nigoghossian, Nadia A Liyanage-Don, G. Rosner, E. Bernstein, S. Mohan, Akinpelumi A. Beckley, D. Seres, T. Choueiri, N. Uriel, John Ausiello, D. Accili, D. Freedberg, M. Baldwin, A. Schwartz, D. Brodie, C. Garcia, M. Elkind, J. Connors, J. Bilezikian, D. Landry and E. Wan. “Post-acute COVID-19 syndrome.” Nature Medicine, 27 (2021): 601 - 615. [CrossRef]
- Vikram Thakur, R. Ratho, Pradeep Kumar, S. Bhatia, Ishani Bora, G. Mohi, S. K. Saxena, M. Devi, D. Yadav and Sanjeet Mehariya. “Multi-Organ Involvement in COVID-19: Beyond Pulmonary Manifestations.” Journal of Clinical Medicine, 10 (2021). [CrossRef]
- Zeinab Mohseni Afshar, Ali Tavakoli Pirzaman, Bardia Karim, Shiva Rahimipour Anaraki, R. Hosseinzadeh, Elaheh Sanjari Pireivatlou, A. Babazadeh, Dariush Hosseinzadeh, S. Miri, T. Sio, M. Sullman, M. Barary and S. Ebrahimpour. “SARS-CoV-2 Omicron (B.1.1.529) Variant: A Challenge with COVID-19.” Diagnostics, 13 (2023). [CrossRef]
- C. Menni, A. Valdes, L. Polidori, M. Antonelli, Satya Penamakuri, A. Nogal, P. Louca, A. May, J. Figueiredo, Christina Hu, E. Molteni, L. Canas, M. F. Österdahl, M. Modat, C. Sudre, B. Fox, A. Hammers, J. Wolf, J. Capdevila andrew T. Chan, S. David, C. Steves, S. Ourselin and T. Spector. “Symptom prevalence, duration and risk of hospital admission in individuals infected with SARS-CoV-2 during periods of omicron and delta variant dominance: a prospective observational study from the ZOE COVID Study.” Lancet (London, England), 399 (2022): 1618 - 1624. [CrossRef]
- P. Relan, N. V. Motaze, K. Kothari, Lisa Askie, O. le Polain de Waroux, M. V. Van Kerkhove, Janet Diaz and B. T. Tirupakuzhi Vijayaraghavan. “Severity and outcomes of Omicron variant of SARS-CoV-2 compared to Delta variant and severity of Omicron sublineages: a systematic review and metanalysis.” BMJ Global Health, 8 (2023). [CrossRef]
- Fei-Hong Hu, Yi-Jie Jia, Dan-Yan Zhao, Xue-Lei Fu, Wan Zhang, Wen Tang, Shixiang Hu, Hua Wu, Meng-Wei Ge, W. Du, Wang-Qin Shen, Bin Zhu and Hong-Lin Chen. “Clinical outcomes of the severe acute respiratory syndrome coronavirus 2 Omicron and Delta variant: systematic review and meta-analysis of 33 studies covering 6 037 144 coronavirus disease 2019–positive patients.” Clinical Microbiology and Infection, 29 (2023): 835 - 844. [CrossRef]
- T. Nyberg, N. Ferguson, S. Nash, H. Webster, S. Flaxman, N. Andrews, W. Hinsley, J. L. Bernal, M. Kall, S. Bhatt, P. Blomquist, A. Zaidi, E. Volz, N. A. Aziz, K. Harman, S. Funk, S. Abbott, R. Hope, A. Charlett, M. Chand, A. Ghani, S. Seaman, G. Dabrera, D. De Angelis, A. Presanis, S. Thelwall, T. Nyberg, N. Ferguson, S. Nash, H. Webster, S. Flaxman, N. Andrews, W. Hinsley, J. Lopez Bernal, M. Kall, S. Bhatt, P. Blomquist, A. Zaidi, E. Volz, N. A. Abdul Aziz, K. Harman, S. Funk, S. Abbott, R. Hope, A. Charlett, M. Chand, A. Ghani, S. Seaman, G. Dabrera, D. De Angelis, A. Presanis and S. Thelwall. “Comparative analysis of the risks of hospitalisation and death associated with SARS-CoV-2 omicron (B.1.1.529) and delta (B.1.617.2) variants in England: a cohort study.” Lancet (London, England), 399 (2022): 1303 - 1312. [CrossRef]
- Di Tian, Yang Pan, Z. Ge, Xiangjing Kong, Yao Zhang, Qing Zhang, Aibin Wang, P. Yang and Zhihai Chen. “Difference of Clinical Characteristics in Patients with Omicron and Delta Variants of SARS-CoV-2 in Beijing, China.” Infectious Diseases & Immunity, 3 (2023): 75 - 82. [CrossRef]
- A. Lauring, M. Tenforde, J. Chappell, M. Gaglani, A. Ginde, T. McNeal, S. Ghamande, D. Douin, H. Talbot, J. Casey, N. Mohr, A. Zepeski, N. Shapiro, K. Gibbs, D. Files, D. Hager, A. Shehu, M. Prekker, H. Erickson, M. Exline, M. Gong, A. Mohamed, N. Johnson, Vasisht Srinivasan, J. Steingrub, I. Peltan, Samuel M. Brown, E. Martin, A. Monto, Akram Khan, C. Hough, L. Busse, C. T. ten Lohuis, A. Duggal, Jennifer G. Wilson, A. J. Gordon, N. Qadir, Steven Y. Chang, Christopher Mallow, C. Rivas, H. Babcock, Jennie H. Kwon, N. Halasa, Carlos G. Grijalva, T. Rice, William B. Stubblefield, A. Baughman, K. Womack, J. Rhoads, C. Lindsell, K. Hart, Yuwei Zhu, K. Adams, S. Schrag, Samantha M. Olson, Miwako Kobayashi, J. Verani, M. Patel and W. Self. “Clinical severity of and effectiveness of mRNA vaccines against, covid-19 from omicron, delta and alpha SARS-CoV-2 variants in the United States: prospective observational study.” The BMJ, 376 (2022). [CrossRef]
- A. Şahin, Eda Karadag-Oncel, Osman Buyuksen, Yıldız Ekemen-Keles, Gulnihan Ustundag, Aysegul Elvan-Tuz, Selin Taşar, Elif Didinmez-Taskirdi, M. Baykan, Ahu Kara-Aksay, N. Yılmaz, Nihal Olgac-Dundar and Dilek Yılmaz. “The diversity in the clinical features of children hospitalized with COVID-19 during the nonvariant, Alpha (B.1.1.7), Delta (B.1.617.2) and Omicron (B.1.1.529) variant periods of SARS CoV-2: Caution for neurological symptoms in Omicron variant.” Journal of Medical Virology, 95 (2023). [CrossRef]
- M. Ellul, L. Benjamin, Bhagteshwar Singh, S. Lant, B. Michael, A. Easton, R. Kneen, S. Defres, J. Sejvar and T. Solomon. “Neurological associations of COVID-19.” The Lancet. Neurology, 19 (2020): 767 - 783. [CrossRef]
- C. Fernández-de-las-Peñas, K. Notarte, P. Peligro, Jacqueline Veronica Velasco, Miguel Joaquín Ocampo, B. Henry, L. Arendt-Nielsen, J. Torres-Macho and Gustavo Plaza-Manzano. “Long-COVID Symptoms in Individuals Infected with Different SARS-CoV-2 Variants of Concern: A Systematic Review of the Literature.” Viruses, 14 (2022). [CrossRef]
- (Hernández-Aceituno 2023) Ana Hernández-Aceituno, Abigail García-Hernández and E. Larumbe-Zabala. “COVID-19 long-term sequelae: Omicron versus Alpha and Delta variants.” Infectious Diseases Now, 53 (2023): 104688 - 104688. [CrossRef]
- Tziolos, N.-R.; Ioannou, P.; Baliou, S.; Kofteridis, D.P. Long COVID-19 Pathophysiology: What Do We Know So Far? Microorganisms 2023, 11, 2458. [CrossRef] [PubMed]
- Mistrulli, R.; Ferrera, A.; Muthukkattil, M.L.; Volpe, M.; Barbato, E.; Battistoni, A. SARS-CoV-2 Related Myocarditis: What We Know So Far. J. Clin. Med. 2023, 12, 4700. [Google Scholar] [CrossRef] [PubMed]
- Ursescu, C.; Teodoru, G.; Bucurica, S.; Nica, R.I.; Lazăr, Ș.D.; Popescu, M.N.; Ciobanu, I.; Berteanu, M. Using the ClinFIT COVID-19 Instrument to Assess the Functional Impairments Specific to Post-COVID-19 Patients in Romania. Diagnostics 2024, 14, 1540. [Google Scholar] [CrossRef] [PubMed]
- Ahuja, S.; Zaheer, S. From COVID-19 to Long COVID: The Forms of the Neurological Manifestations. J. Mind Med. Sci. 2023, 10, 209–216. [Google Scholar] [CrossRef]
- Vasichkina, E.; Alekseeva, D.; Kudryavtsev, I.; Glushkova, A.; Starshinova, A.Y.; Malkova, A.; Kudlay, D.; Starshinova, A. COVID-19 Heart Lesions in Children: Clinical, Diagnostic and Immunological Changes. Int. J. Mol. Sci. 2023, 24, 1147. [Google Scholar] [CrossRef] [PubMed]
| Study Type | Low Risk (%) | Moderate Risk (%) | High Risk (%) |
|---|---|---|---|
| Cohort Studies (n = 62) | 42 | 45 | 13 |
| Case-Control (n = 31) | 35 | 48 | 17 |
| Systematic Reviews (n = 28) | 46 | 43 | 11 |
| Case Series (n = 26) | 31 | 46 | 23 |
| Organ System | Acute Phase (%) | Long-term (6 mo) (%) | Key Biomarkers | Severity Association |
|---|---|---|---|---|
| Pulmonary | 78 | 24 | DLCO, CT findings | High |
| Cardiovascular | 32 | 11 | Troponin, NT-proBNP | High |
| Neurological | 43 | 32 | MRI changes, EEG | Moderate |
| Renal* | 28 | 35 | Creatinine, proteinuria | High |
| Hepatic | 38 | 8 | AST, ALT, bilirubin | Moderate |
| GI | 24 | 16 | Fecal calprotectin | Low–Moderate |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).




