Submitted:
20 June 2025
Posted:
24 June 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Foundations of Pre-Operative Planning
3. Generative Artificial Intelligence for Pre-Operative Planning
3.1. Predictive Analytics for Risk Stratification
3.2. AI-Driven Imaging
5. Surgical Education, Training and Patient Involvement
6. Current Challenges and Limitations
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AI | Artificial Intelligence |
| CRLM | Colorectal Liver Metastasis |
| CALI | Chemotherapy-Associated Liver Injury |
| GenAI | Generative Artificial Intelligence |
| HCC | Hepatocellular Carcinoma |
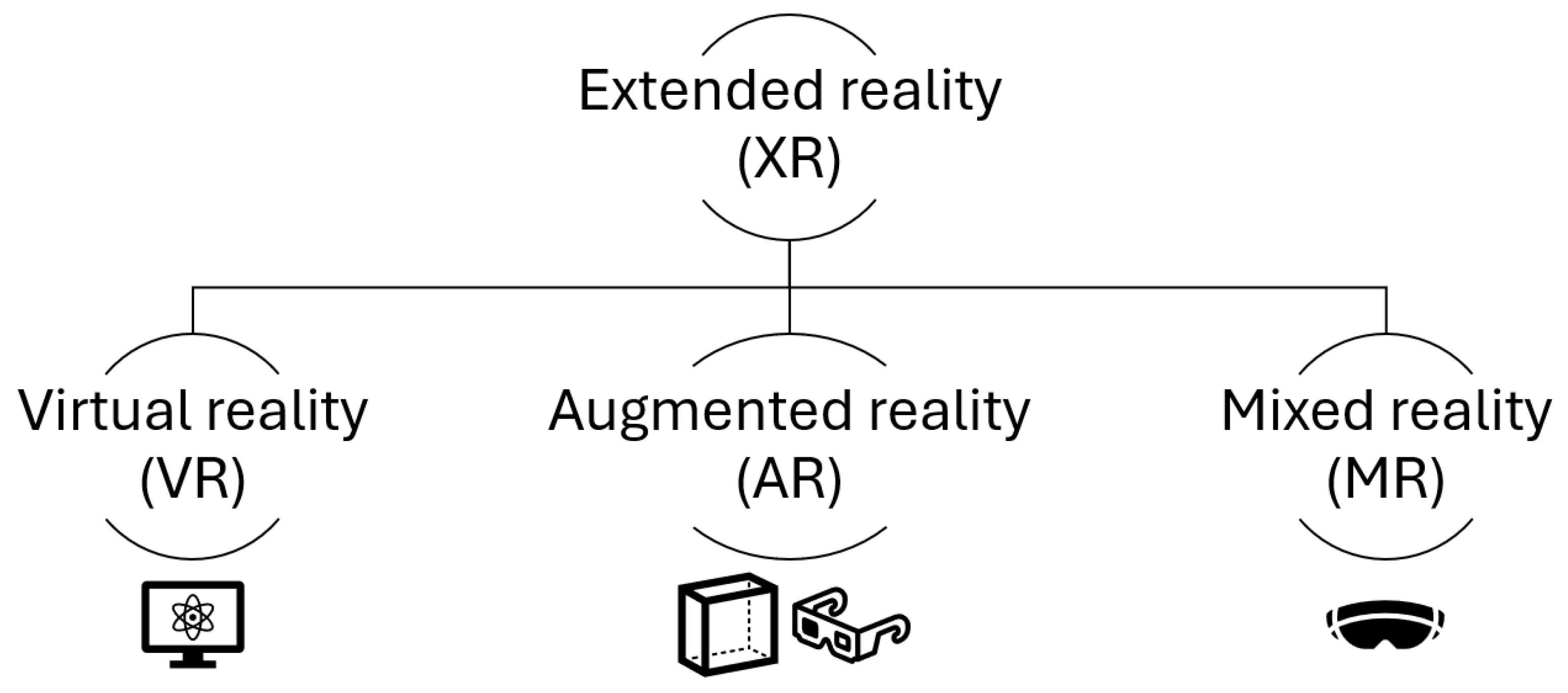
| XR | Extended Reality |
| PHLF | Post-hepatectomy liver failure |
| HPB | Hepato-pancreato-biliary |
| FLR | Future Liver Remnant |
| AUC | Area Under Curve |
| MDPI | Multidisciplinary Digital Publishing Institute |
| DOAJ | Directory of open access journals |
| TLA | Three letter acronym |
| LD | Linear dichroism |
| CT | Computed Tomography |
| MRI | Magnetic Resonance Imaging |
| MRCP | Magnetic Resonance Cholangiopancreatography |
| US | Ultrasound |
References
- International Surgical Outcomes Study g. Global patient outcomes after elective surgery: prospective cohort study in 27 low-, middle- and high-income countries. Br J Anaesth. 2016;117[5]:601-9. [CrossRef]
- Nepogodiev D, Martin J, Biccard B, Makupe A, Bhangu A, Nepogodiev D, et al. Global burden of postoperative death. The Lancet. 2019;393(10170):401. [CrossRef]
- Egeland C, Rostved AA, Schultz NA, Pommergaard HC, Daugaard TR, Thofner LB, et al. Morbidity and mortality after liver surgery for colorectal liver metastases: a cohort study in a high-volume fast-track programme. BMC Surg. 2021;21(1):312. [CrossRef]
- Topal H, Aerts R, Laenen A, Collignon A, Jaekers J, Geers J, Topal B. Survival After Minimally Invasive vs Open Surgery for Pancreatic Adenocarcinoma. JAMA Netw Open. 2022;5(12):e2248147. [CrossRef]
- Feussner H, Park A. Surgery 4.0: the natural culmination of the industrial revolution? Innov Surg Sci. 2017;2(3):105-8. [CrossRef]
- Raza MM, Venkatesh KP, Diao JA, Kvedar JC. Defining digital surgery for the future. NPJ Digit Med. 2022;5(1):155. [CrossRef]
- Gilg S, Sandstrom P, Rizell M, Lindell G, Ardnor B, Stromberg C, Isaksson B. The impact of post-hepatectomy liver failure on mortality: a population-based study. Scand J Gastroenterol. 2018;53(10-11):1335-9. [CrossRef]
- Primavesi F, Maglione M, Cipriani F, Denecke T, Oberkofler CE, Starlinger P, et al. E-AHPBA-ESSO-ESSR Innsbruck consensus guidelines for preoperative liver function assessment before hepatectomy. Br J Surg. 2023;110(10):1331-47. [CrossRef]
- Xu Y, Quan R, Xu W, Huang Y, Chen X, Liu F. Advances in Medical Image Segmentation: A Comprehensive Review of Traditional, Deep Learning and Hybrid Approaches. Bioengineering (Basel). 2024;11(10). [CrossRef]
- Gorgec B, Hansen IS, Kemmerich G, Syversveen T, Abu Hilal M, Belt EJT, et al. MRI in addition to CT in patients scheduled for local therapy of colorectal liver metastases (CAMINO): an international, multicentre, prospective, diagnostic accuracy trial. Lancet Oncol. 2024;25(1):137-46. [CrossRef]
- Aguiar JA, Riaz A, Thornburg B. Biliary Anatomy. Semin Intervent Radiol. 2021;38(3):251-4. [CrossRef]
- Strasberg SM, Hertl M, Soper NJ. An analysis of the problem of biliary injury during laparoscopic cholecystectomy. J Am Coll Surg. 1995;180(1):101-25. [PubMed]
- Kalata S, Thumma JR, Norton EC, Dimick JB, Sheetz KH. Comparative Safety of Robotic-Assisted vs Laparoscopic Cholecystectomy. JAMA Surg. 2023;158(12):1303-10. [CrossRef]
- Richardson MC, Bell G, Fullarton GM. Incidence and nature of bile duct injuries following laparoscopic cholecystectomy: an audit of 5913 cases. West of Scotland Laparoscopic Cholecystectomy Audit Group. Br J Surg. 1996;83(10):1356-60. [CrossRef]
- Broderick RC, Lee AM, Cheverie JN, Zhao B, Blitzer RR, Patel RJ, et al. Fluorescent cholangiography significantly improves patient outcomes for laparoscopic cholecystectomy. Surg Endosc. 2021;35(10):5729-39. [CrossRef]
- Kinami S, Maruyama K, Sannomiya Y, Saito H, Takamura H. Benefits, problems, and optimal timing of administration of indocyanine green fluorescence cholangiography in laparoscopic cholecystectomy. BMJ Surg Interv Health Technol. 2025;7(1):e000310. [CrossRef]
- Thirunavukarasu AJ, Ting DSJ, Elangovan K, Gutierrez L, Tan TF, Ting DSW. Large language models in medicine. Nat Med. 2023;29(8):1930-40. [CrossRef]
- Morley J, DeVito NJ, Zhang J. Generative AI for medical research. BMJ. 2023;382:1551. [CrossRef]
- Khurana D, Koli A, Khatter K, Singh S. Natural language processing: state of the art, current trends and challenges. Multimed Tools Appl. 2023;82(3):3713-44. [CrossRef]
- Kron P, Farid S, Ali S, Lodge P. Artificial Intelligence: A Help or Hindrance to Scientific Writing? Ann Surg. 2024;280(5):713-8. [CrossRef]
- Zhang M, Li J. A commentary of GPT-3 in MIT Technology Review 2021. Fundamental Research. 2021;1(6):831-3. [CrossRef]
- Vauthey JN, Pawlik TM, Ribero D, Wu TT, Zorzi D, Hoff PM, et al. Chemotherapy regimen predicts steatohepatitis and an increase in 90-day mortality after surgery for hepatic colorectal metastases. J Clin Oncol. 2006;24(13):2065-72. [CrossRef]
- Santol J, Kim S, Gregory LA, Baumgartner R, Murtha-Lemekhova A, Birgin E, et al. An APRI+ALBI-Based Multivariable Model as a Preoperative Predictor for Posthepatectomy Liver Failure. Ann Surg. 2025;281(5):861-71. [CrossRef]
- Mai RY, Lu HZ, Bai T, Liang R, Lin Y, Ma L, et al. Artificial neural network model for preoperative prediction of severe liver failure after hemihepatectomy in patients with hepatocellular carcinoma. Surgery. 2020;168(4):643-52. [CrossRef]
- Kowal M, Smith A, Pandanaboyana S, Pathak S. Editorial: Technological innovations and pancreatic cancer. Front Oncol. 2024;14:1497367. [CrossRef]
- Vela Ulloa J, King Valenzuela S, Riquoir Altamirano C, Urrejola Schmied G. Artificial intelligence-based decision-making: can ChatGPT replace a multidisciplinary tumour board? Br J Surg. 2023;110(11):1543-4. [CrossRef]
- Soga K, Ochiai J, Kassai K, Miyajima T, Itani K, Yagi N, Naito Y. Development of a novel fusion imaging technique in the diagnosis of hepatobiliary-pancreatic lesions. J Med Imaging Radiat Oncol. 2013;57(3):306-13. [CrossRef]
- Darzi F, Bocklitz T. A Review of Medical Image Registration for Different Modalities. Bioengineering (Basel). 2024;11(8). [CrossRef]
- Fang CH, Tao HS, Yang J, Fang ZS, Cai W, Liu J, Fan YF. Impact of three-dimensional reconstruction technique in the operation planning of centrally located hepatocellular carcinoma. J Am Coll Surg. 2015;220(1):28-37. [CrossRef]
- Andrews C, Southworth MK, Silva JNA, Silva JR. Extended Reality in Medical Practice. Current Treatment Options in Cardiovascular Medicine. 2019;21(4):18. [CrossRef]
- Zhang W, Zhu W, Yang J, Xiang N, Zeng N, Hu H, et al. Augmented Reality Navigation for Stereoscopic Laparoscopic Anatomical Hepatectomy of Primary Liver Cancer: Preliminary Experience. Front Oncol. 2021;11:663236. [CrossRef]
- Lou L., Zhang L., H. L. Application effect of contrast-enhanced ultrasound combined with mixed reality technology in laparoscopic anatomical hepatectomy. Medical Journal of Chinese People's Liberation Army. 2023;48(10):1208. [CrossRef]
- Onda S, Okamoto T, Kanehira M, Suzuki F, Ito R, Fujioka S, et al. Identification of inferior pancreaticoduodenal artery during pancreaticoduodenectomy using augmented reality-based navigation system. J Hepatobiliary Pancreat Sci. 2014;21(4):281-7. [CrossRef]
- Kitagawa M, Sugimoto M, Haruta H, Umezawa A, Kurokawa Y. Intraoperative holography navigation using a mixed-reality wearable computer during laparoscopic cholecystectomy. Surgery. 2022;171(4):1006-13. [CrossRef]
- Vedula SS, Ghazi A, Collins JW, Pugh C, Stefanidis D, Meireles O, et al. Artificial Intelligence Methods and Artificial Intelligence-Enabled Metrics for Surgical Education: A Multidisciplinary Consensus. J Am Coll Surg. 2022;234(6):1181-92. [CrossRef]
- Winkler-Schwartz A, Bissonnette V, Mirchi N, Ponnudurai N, Yilmaz R, Ledwos N, et al. Artificial Intelligence in Medical Education: Best Practices Using Machine Learning to Assess Surgical Expertise in Virtual Reality Simulation. J Surg Educ. 2019;76(6):1681-90. [CrossRef]
- Guerrero DT, Asaad M, Rajesh A, Hassan A, Butler CE. Advancing Surgical Education: The Use of Artificial Intelligence in Surgical Training. Am Surg. 2023;89(1):49-54. [CrossRef]
- Leon S, Lee S, Perez JE, Hashimoto DA. Artificial intelligence and the education of future surgeons. Am J Surg. 2025;246:116257. [CrossRef]
- Skorka P, Kargul M, Seemannova D, Gajek B, Gutowski P, Kazimierczak A, Rynio P. The Influence of Individualized Three-Dimensional Holographic Models on Patients' Knowledge Qualified for Intervention in the Treatment of Peripheral Arterial Disease (PAD). J Cardiovasc Dev Dis. 2023;10(11). [CrossRef]
- Clark K, Vendt B, Smith K, Freymann J, Kirby J, Koppel P, et al. The Cancer Imaging Archive (TCIA): maintaining and operating a public information repository. J Digit Imaging. 2013;26(6):1045-57. [CrossRef]
- Kondylakis H, Kalokyri V, Sfakianakis S, Marias K, Tsiknakis M, Jimenez-Pastor A, et al. Data infrastructures for AI in medical imaging: a report on the experiences of five EU projects. Eur Radiol Exp. 2023;7(1):20. [CrossRef]
- McCulloch P, Altman DG, Campbell WB, Flum DR, Glasziou P, Marshall JC, et al. No surgical innovation without evaluation: the IDEAL recommendations. Lancet. 2009;374(9695):1105-12. [CrossRef]
- Shiferaw KB, Roloff M, Balaur I, Welter D, Waltemath D, Zeleke AA. Guidelines and standard frameworks for artificial intelligence in medicine: a systematic review. JAMIA Open. 2025;8(1):ooae155. [CrossRef]
- Nathan H, Cameron JL, Choti MA, Schulick RD, Pawlik TM. The volume-outcomes effect in hepato-pancreato-biliary surgery: hospital versus surgeon contributions and specificity of the relationship. J Am Coll Surg. 2009;208(4):528-38. [CrossRef]
- Birkmeyer JD, Siewers AE, Finlayson EV, Stukel TA, Lucas FL, Batista I, et al. Hospital volume and surgical mortality in the United States. N Engl J Med. 2002;346(15):1128-37. [CrossRef]
| Ref. | n | Intervention / Surgery performed | Significant findings |
|---|---|---|---|
| [31] | |||
| 85 | Augmented reality navigation system / laparoscopic anatomical hepatectomy for primary liver cancer | Decreased length of stay and estimated blood loss in the augmented reality group | |
| [32] |
45 |
Mixed reality navigation combined with intra-operative ultrasound / laparoscopic anatomical hepatectomy for primary liver cancer |
Decreased estimated blood loss, complication rates and operative time in the mixed reality group |
| [33] |
7 |
Augmented reality navigation for pancreaticoduodenectomy |
No significant differences |
| [34] | 27 |
Augmented reality navigation for laparoscopic cholecystectomy |
No significant differences |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




