Submitted:
22 June 2025
Posted:
23 June 2025
You are already at the latest version
Abstract
Keywords:
Introduction
Methods
Study Population
ID Parameters Assessment and Definitions
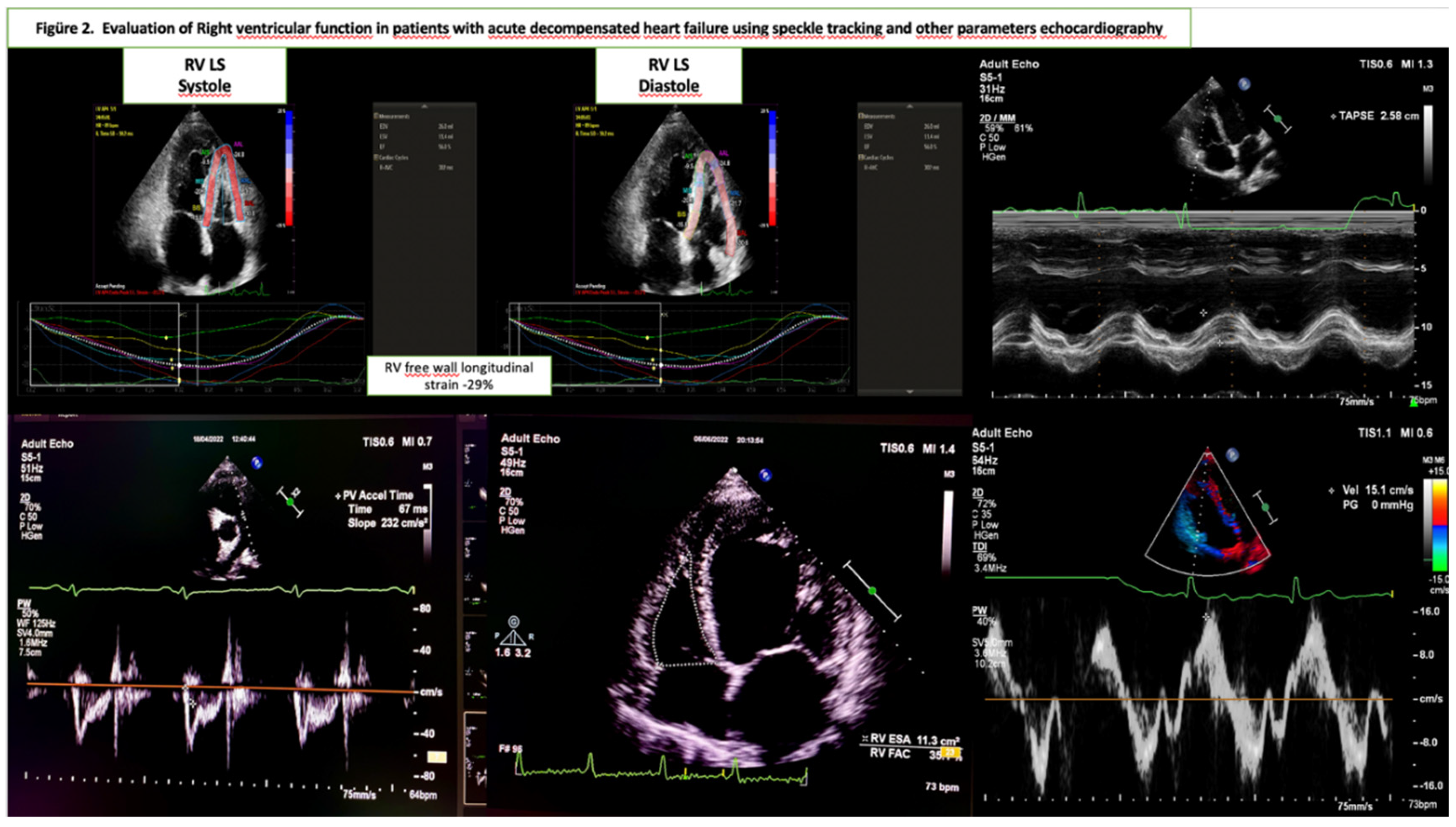
Echocardiographic Evaluation
- Tricuspid annular plane systolic excursion (TAPSE) measured via M-mode.
- Peak systolic tricuspid annular velocity (RV TDI S′) was obtained using tissue Doppler imaging.
- RV fractional area change (RV FAC) was calculated as the percentage of RV end-diastolic and end-systolic area changes.
- Systolic pulmonary artery pressure was estimated using the peak velocity gradient of tricuspid regurgitation flow, right atrial pressure derived from the inferior vena cava dimensions, and respiratory variability.
Statistical Analysis
Results
|
ANEMIA (-) ID (+) n:17 |
ANEMIA (+) ID (+) n:41 |
P value |
ANEMIA (-) ID(-) N:27 |
ANEMIA (-) ID(+) N:17 |
P value | |
| LVEF, (%) * | 35 (18-60) | 38 (18-60) | 0.41 | 30 (20-60) | 35 (18-60) | 0.42 |
| LAD (mm) * | 49 (44-60) | 46 (42-61) | 0.12 | 48 (40-61) | 49 (44-60) | 0.36 |
| TAPSE (mm) * | 18 (12-22) | 15.2 (12-22.9) | 0.08 | 17.3 (14.1-22.8) | 18 (12-22) | 0.90 |
| FAC (%) | 38.6 (20-50) | 36 (20-53) | 0.39 | 38 (18.5-50) | 38.6 (20.7-50) | 0.09 |
| RV-LS (%) * | -16.2 (6.3-26.8) | -14.7 (6.5-25.8) | 0.66 | -20.4 (-9.9 27) | -16.2((-6.3) - (-26.8)) | 0.05 |
| Pulmonaryacceleration time, (msn) | 92 (50-116) | 88 (56-132) | 0.91 | 96.9±22.1 | 86.9±21.1 | 0.20 |
| PASB, (mmHg) * | 50 (30-80) | 50 (28-70) | 0.72 | 45 (30-100) | 50 (30-80) | 0.68 |
| RV TDI S’ (CM/S) * | 10.3 (5.3-16.3) | 9.1 (6.4-17) | 0.78 | 012.2 (4.2-15.4) | 10.3 (5.3-16.3) | 0.21 |
|
Model |
Unstandardized coefficients | Standardized coefficients | P value | 95% CI | |
| B | Std. Error | Beta | |||
| Constant* | -0.961 | 7.507 | 0.89 | -15.872- 13.950 | |
| HGB | 0.652 | 0.248 | 0.252 | 0.01 | 0.160-1.145 |
| LV EF | 0.158 | 0.035 | 0.429 | <0.01 | 0.088 – 0.228 |
| Model | B | Partial correlations |
Collinearity statistics Tolerance |
P value | |
| eGFR | -0.010 | -0.047 | 0.924 | 0.66 | |
| Heart Rate | -0.046 | -0.164 | 0.881 | 0.12 | |
| DBP | 0.008 | 0.013 | 0.882 | 0.90 | |
| Troponin | 5.444 | 0.017 | 0.915 | 0.87 | |
| Ferritin | 0.007 | 0.150 | 0.843 | 0.15 | |
| LAD | 0.126 | 0.138 | 0.936 | 0.19 | |
Discussion
Limitations
Conclusions
References
- Magrì D, De Martino F, Moscucci F, Agostoni P, Sciomer S. Anemia and iron deficiency in heart failure: clinical and prognostic role. Heart Failure Clinics. 2019;15(3):359-69.
- Anand IS, Gupta P. Anemia and iron deficiency in heart failure: current concepts and emerging therapies. Circulation. 2018;138(1):80-98.
- Alnuwaysir RI, Hoes MF, van Veldhuisen DJ, van der Meer P, Grote Beverborg N. Iron deficiency in heart failure: mechanisms and pathophysiology. Journal of clinical medicine. 2021;11(1):125.
- Zhang H, Jamieson KL, Grenier J, Nikhanj A, Tang Z, Wang F, et al. Myocardial iron deficiency and mitochondrial dysfunction in advanced heart failure in humans. Journal of the American Heart Association. 2022;11(11):e022853.
- Loncar G, Obradovic D, Thiele H, von Haehling S, Lainscak M. Iron deficiency in heart failure. ESC heart failure. 2021;8(4):2368-79.
- Beale A, Carballo D, Stirnemann J, Garin N, Agoritsas T, Serratrice J, et al. Iron deficiency in acute decompensated heart failure. Journal of clinical medicine. 2019;8(10):1569.
- Palau P, Llàcer P, Domínguez E, Tormo JP, Zakarne R, Mollar A, et al. Iron deficiency and short-term adverse events in patients with decompensated heart failure. Clinical Research in Cardiology. 2021;110:1292-8.
- Enjuanes C, Klip IT, Bruguera J, Cladellas M, Ponikowski P, Banasiak W, et al. Iron deficiency and health-related quality of life in chronic heart failure: results from a multicenter European study. International journal of cardiology. 2014;174(2):268-75.
- Santas E, Miñana G, Cardells I, Palau P, Llàcer P, Fácila L, et al. Short-term changes in left and right systolic function following ferric carboxymaltose: a substudy of the Myocardial-IRON trial. ESC Heart Failure. 2020;7(6):4222-30.
- Martens, P. The effect of iron deficiency on cardiac function and structure in heart failure with reduced ejection fraction. Cardiac Failure Review. 2022;8.
- Miñana G, Santas E, de la Espriella R, Núñez E, Lorenzo M, Núñez G, et al. Right ventricular function and iron deficiency in acute heart failure. European Heart Journal Acute Cardiovascular Care. 2021;10(4):406-14.
- McDonagh TA, Metra M, Adamo M, Gardner RS, Baumbach A, Böhm M, et al. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: Developed by the Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC) With the special contribution of the Heart Failure Association (HFA) of the ESC. European heart journal. 2021;42(36):3599-726.
- Rudski LG, Lai WW, Afilalo J, Hua L, Handschumacher MD, Chandrasekaran K, et al. Guidelines for the echocardiographic assessment of the right heart in adults: a report from the American Society of Echocardiography: endorsed by the European Association of Echocardiography, a registered branch of the European Society of Cardiology, and the Canadian Society of Echocardiography. Journal of the American society of echocardiography. 2010;23(7):685-713.
- Badano LP, Kolias TJ, Muraru D, Abraham TP, Aurigemma G, Edvardsen T, et al. Standardization of left atrial, right ventricular, and right atrial deformation imaging using two-dimensional speckle tracking echocardiography: a consensus document of the EACVI/ASE/Industry Task Force to standardize deformation imaging. European Heart Journal-Cardiovascular Imaging. 2018;19(6):591-600.
- Lee J-H, Park J-H. Strain analysis of the right ventricle using two-dimensional echocardiography. Journal of cardiovascular imaging. 2018;26(3):111-24.
- Kobak KA, Radwańska M, Dzięgała M, Kasztura M, Josiak K, Banasiak W, et al. Structural and functional abnormalities in iron-depleted heart. Heart failure reviews. 2019;24:269-77.
- Chung YJ, Luo A, Park KC, Loonat AA, Lakhal-Littleton S, Robbins PA, et al. Iron-deficiency anemia reduces cardiac contraction by downregulating RyR2 channels and suppressing SERCA pump activity. JCI insight. 2019;4(7).
- Beck-da-Silva L, Piardi D, Soder S, Rohde LE, Pereira-Barretto AC, de Albuquerque D, et al. IRON-HF study: a randomized trial to assess the effects of iron in heart failure patients with anemia. International journal of cardiology. 2013;168(4):3439-42.
- Avni T, Leibovici L, Gafter-Gvili A. Iron supplementation for the treatment of chronic heart failure and iron deficiency: systematic review and meta-analysis. European journal of heart failure. 2012;14(4):423-9.
- Meyer P, Filippatos GS, Ahmed MI, Iskandrian AE, Bittner V, Perry GJ, et al. Effects of right ventricular ejection fraction on outcomes in chronic systolic heart failure. Circulation. 2010;121(2):252-8.
- Bosch L, Lam CS, Gong L, Chan SP, Sim D, Yeo D, et al. Right ventricular dysfunction in left-sided heart failure with preserved versus reduced ejection fraction. European journal of heart failure. 2017;19(12):1664-71.
- Raina A, Meeran T. Right ventricular dysfunction and its contribution to morbidity and mortality in left ventricular heart failure. Current Heart Failure Reports. 2018;15:94-105.
- Das P, Thandavarayan RA, Watanabe K, Velayutham R, Arumugam S. Right ventricular failure: a comorbidity or a clinical emergency? Heart failure reviews. 2021:1-15.
- Melenovsky V, Hwang S-J, Lin G, Redfield MM, Borlaug BA. Right heart dysfunction in heart failure with preserved ejection fraction. European heart journal. 2014;35(48):3452-62.
- Burns JA, Sanchez C, Beussink L, Daruwalla V, Freed BH, Selvaraj S, et al. Lack of association between anemia and intrinsic left ventricular diastolic function or cardiac mechanics in heart failure with preserved ejection fraction. The American journal of cardiology. 2018;122(8):1359-65.
- Oni O, Adebiyi A, Aje A, Akingbola T. Right ventricular function assessment in sickle cell anaemia patients using echocardiography. Haematol Int J. 2019;1:136.
- Barbosa MM, Vasconcelos MCM, Ferrari TCA, Fernandes BM, Passaglia LG, Silva CM, et al. Assessment of ventricular function in adults with sickle cell disease: role of two-dimensional speckle-tracking strain. Journal of the American Society of Echocardiography. 2014;27(11):1216-22.
- Maeder MT, Khammy O, Dos Remedios C, Kaye DM. Myocardial and systemic iron depletion in heart failure: implications for anemia accompanying heart failure. Journal of the American College of Cardiology. 2011;58(5):474-80.
- Zhang H, Zhabyeyev P, Wang S, Oudit GY. Role of iron metabolism in heart failure: From iron deficiency to iron overload. Biochimica et Biophysica Acta (BBA)-Molecular Basis of Disease. 2019;1865(7):1925-37.
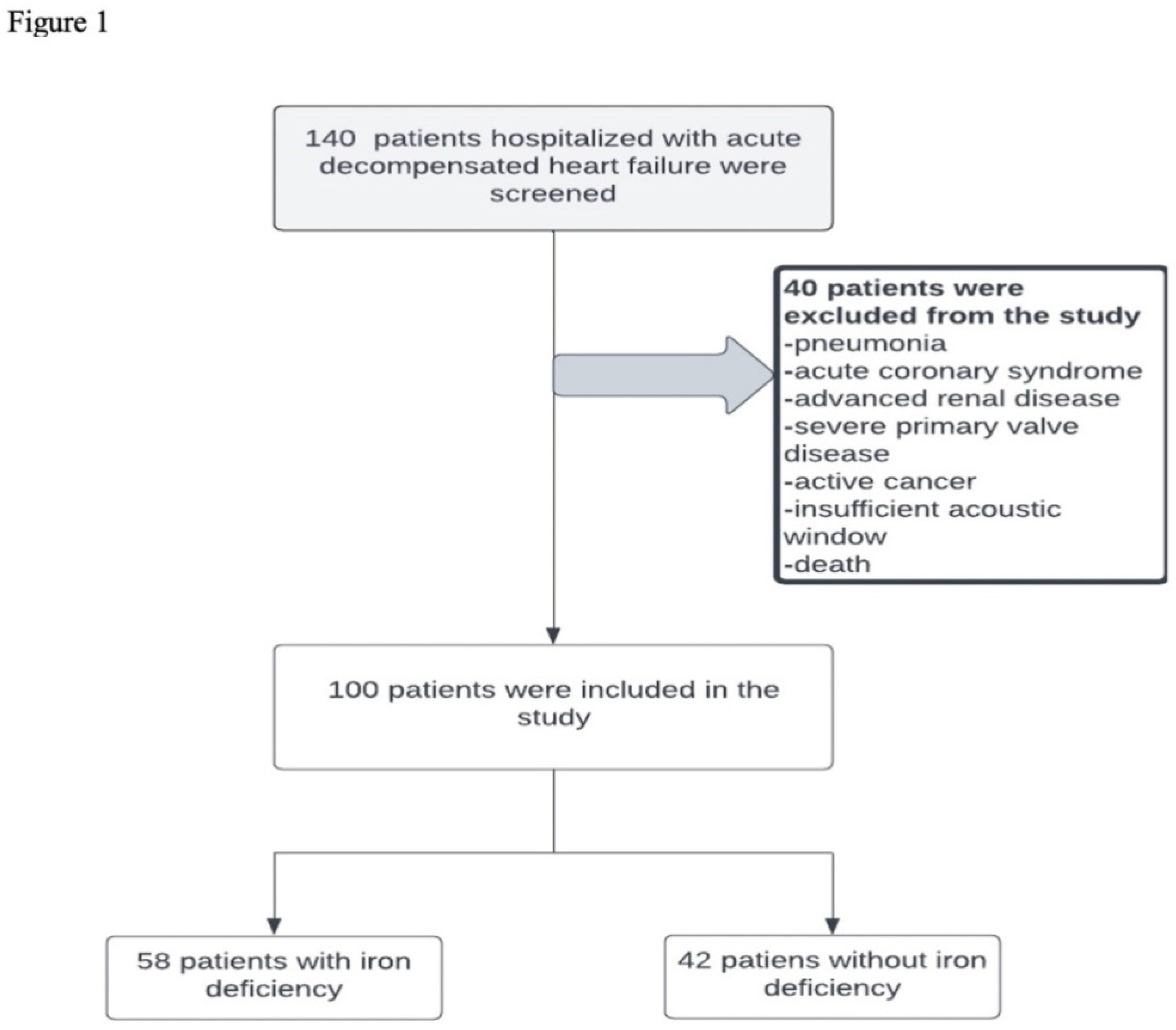
| Iron Deficiency (-) (n:42) |
Iron Deficiency (+) (n:58) |
P value | |
|---|---|---|---|
| Age, (years) | 68±10 | 70±11 | 0.65 |
| Gender (male), n (%) | 29 (69.0) | 35 (60.3) | 0.40 |
| Hypertension, n (%) | 33 (78.6) | 47 (81.0) | 0.80 |
| Diabetes Mellitus, n (%) | 19 (45.2) | 33 (56.9) | 0.31 |
| Ischaemicheartdisease, n (%) | 27 (64.3) | 44 (75.9) | 0.26 |
| Asthma/COPD, n (%) | 4 (9.5) | 14 (24.1) | 0.07 |
| Diuretictreatmentprior to admission, n (%) |
40 (95.2) | 57 (98.3) | 0.57 |
| Heart rate (b.p.m.) * | 76 (60-120) | 84 (55-115) | 0.38 |
| SBP, (mmHg) * | 130 (90-160) | 127 (100-155) | 0.67 |
| Severe TR, n (%) | 6 (14.3) | 15(25.9) | 0.21 |
| Haemoglobin, (g/dL) | 13.5±1.7 | 11.6±1.7 | |
| HTC, (%) | 40.2±5.7 | 34.7±5.4 | <0.01 |
| Serum Iron, (μg/dL) * |
50 (34-128) | 35 (16-198) | <0.01 |
| Ferritin, (ng/dL) * | 156.6 (112-954) | 61.9 (10.3-169) | <0.01 |
| TSAT, (%) * | 26.3 (17.7-60.1) | 14.5 (4.7-78.1) | <0.01 |
| WBC, (x103 /mL) * | 8.2 (4.5-64) | 8.1 (4.4-12) | 0.25 |
| CRP, (mg/dL) * | 5.0 (0.4-19) | 6.7 (0.6-32.4) | 0.23 |
| Creatinine, (mg/dL) | 1.2 (0.5-1.9) | 1.1 (0.6-2.0) | 0.98 |
| eGFR, (MDRD formula) (mL/min/1.73 m2) |
60.1 (30.5-120) | 53.4 (32.7-120) | 0.44 |
| Serum sodium, (mmol/L) | 139.2±3.8 | 138.1±3.8 | 0.55 |
| Serum potassium, (mmol/L) * | 4.3 (3.0-5.3) | 4.5 (3.2-5.43) | 0.56 |
| ALT, (U/L) * | 20.5 (6-46) | 17 (3-43) | 0.08 |
| NT-proBNP, (pg/mL) * | 4500 (1000-20000) | 3925 (1500-35000) | 0.79 |
| Troponin, (ng/mL) | 0.021 (0.007-0.05) | 0.018 (0.003-0.07) | 0.60 |
| Total cholesterol, (mg/dL) * | 142 (72-234) | 140 (91-298) | 0.68 |
| LDL-cholesterol, (mg/dL) * | 84 (34-156) | 75 (39-219) | 0.70 |
| HDL-cholesterol, (mg/dL) * | 40 (24-63) | 39.5 (21-93) | 0.46 |
| Echocardiographic findings | |||
| LVEF (%) * | 32.5 (20-60) | 36 (18-60) | 0.91 |
| LAD (mm) * | 48 (40-66) | 46.5 (42-61) | 0.59 |
| TAPSE (mm) * | 17.2 (13-22.8) | 15.6 (12-22.9) | 0.05 |
| RV FAC (%) * | 38.3±7.9 | 36.4±7.7 | 0.21 |
| RV-LS (%) * | -18.2 (8.6-27.2) | 14.7 (6.3-26.8) | 0.005 |
| Pulmonaryacceleration time (msn) | 97.8±23.8 | 88.8±20.9 | 0.05 |
| PASB (mmHg) * | 45 (30-100) | 50 (28-80) | 0.32 |
| RV TDI S’ (cm/s) | 10.7 (4.2-15.7) | 9.4 (5.3-17.0) | 0.09 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




