Submitted:
18 June 2025
Posted:
20 June 2025
Read the latest preprint version here
Abstract
Keywords:
Part I: Muscle Weakness as a Psychoneurokinesiological Disorder
1. The Cost of Musculoskeletal Disorders
1.1. Non-Specific Musculoskeletal Dysfunction; a Major, Poorly Addressed Problem
1.2. Motor Control, Muscle Weakness, and nsMSDs
1.3. Clinically Interacting with Muscle Weakness and Motor Control
1.5. Maladaptive Neuroplasticity, a Missing Link in Motor Dysfunction?
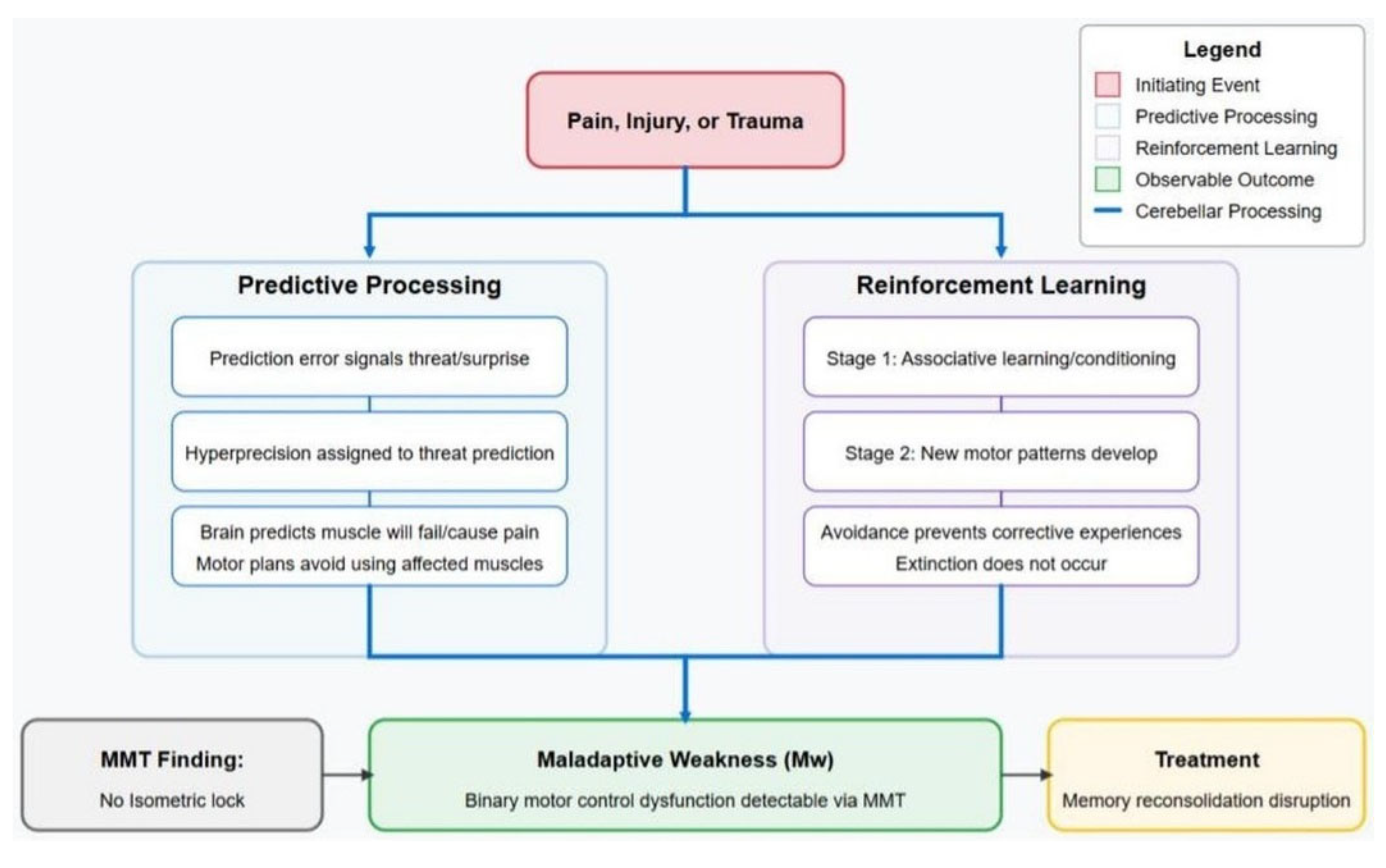
- Pain, stress, or trauma, occurring in temporal proximity to the contraction of a muscle, associates the sensory and motor events.
- The association leads to a prediction that use of the muscle will re-engage the experience of pain/trauma. Thus, use of the muscle is avoided, the first stage of the response.
- In the second stage, new combinations of muscles (muscle synergies) are developed. These new synergies, which avoid using muscles associated with pain or trauma, tend to be less efficient and potentially maladaptive, yet they become the preferred choice for functional activities.
- As in two-stage avoidance learning models often applied to PTSD, the habitual use of avoidance patterns prevents exposure to corrective experiences that could reintegrate the avoided muscles, once “healing” has occurred.
- The mechanism of action for (putatively) successful treatments for Mw is the elimination of muscle-pain/trauma associations through the blockage of memory reconsolidation.
1.6. Muscle, Motor, or Movement PTSD and Psychoneurokinesiology
1.7. Aims and Methods of This Theoretical Review
- Mw is a binary dysfunction.
- MMT outcomes reflect this binary nature.
- MMT directly assesses motor control integrity.
- Mw is a central feature of motor dysfunction in nsMSDs.
- Disruption of memory reconsolidation may resolve Mw.
2. Prevalence and Impact of Mw in nsMSDs
2.1. The Functional Impact of Muscle Weakness
- Chronicity and recurrence: Unresolved weakness may contribute to the progression from acute to chronic conditions and predispose to recurrence, even in asymptomatic individuals. [54].
2.2. Muscle Weakness and Chronic Pain
3. Predictive Processing; the First Theoretical Framework of Mw
3.1. Core Concepts of Predictive Processing
3.3. Trauma, Pain, and Predictive Processing
3.4. Motor Control and Active Inference
3.5. Arthrogenic Muscle Inhibition as Predictive Processing
3.6. Kinesiophobia, Mw, and Predictive Processing
3.7. Functional Weakness, Mw and Predictive Processing
4. Reinforcement Learning: The Second Theoretical Framework of Mw
4.1. How the Cerebellum Predicts Danger and Suppresses Movement
4.2. Implications of Maladaptive Motor Plasticity for Rehabilitation.
4.3. Freeze Responses and Passive Learning: Why Muscles Shut Down After Pain
4.4. Why Muscle Inhibition Persists: How New Movement Patterns Are Learned
5. Experimental Evidence for mPTSD and Its Treatment Principles
5.1. Disruption of Memory Reconsolidation as a Treatment Mechanism
Part II: MMT as a Neuropsychological Test
6. Adaptive Force and Its Relationship to Motor Control
6.1. When Does the Muscle Break? The Unengaged Controversy.
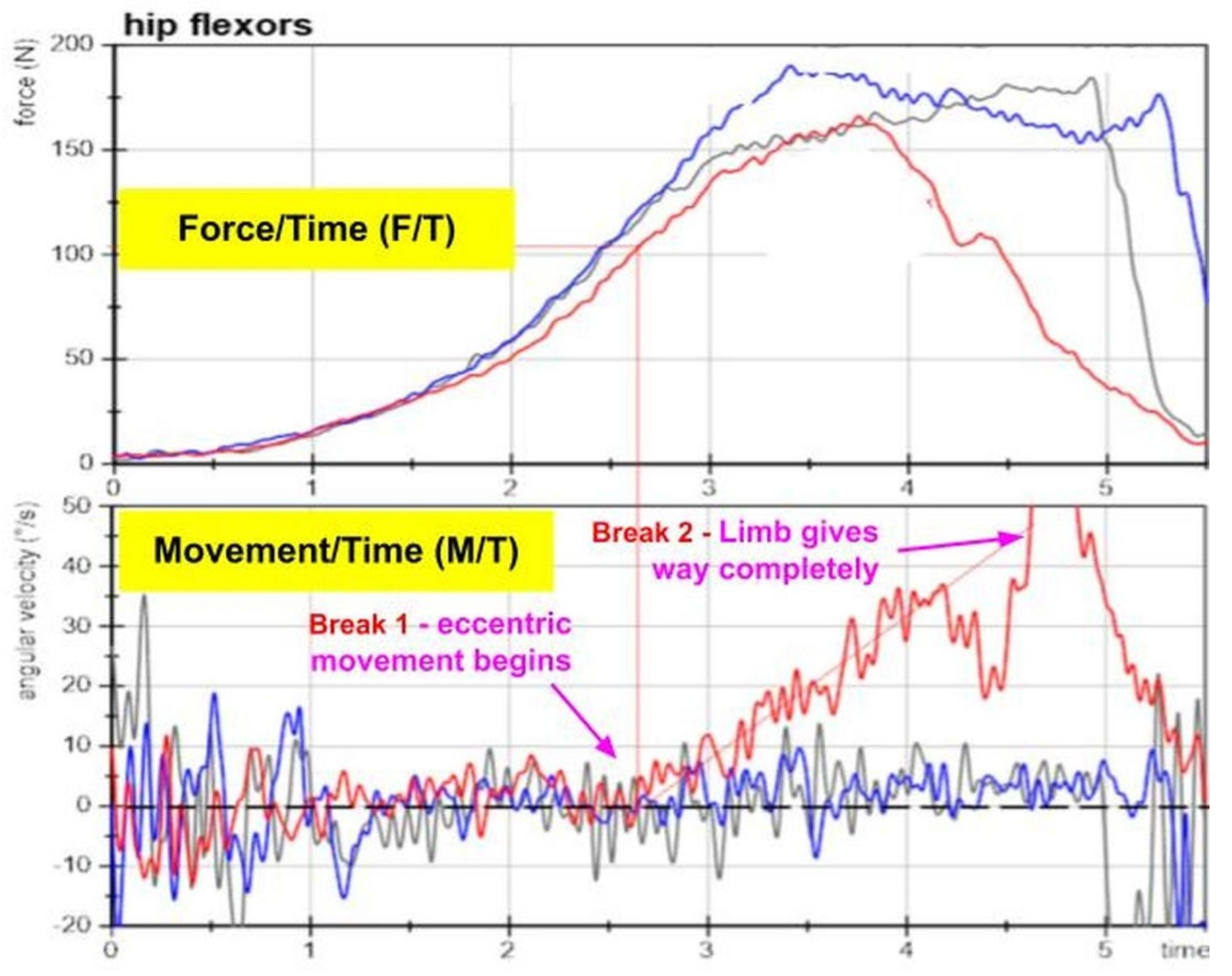
- All tracings in the bottom (movement) box show periodic oscillations — small up and down movements — but the blue and grey tracings are more regular than the red tracing.
- The blue and grey lines (neutral and positive imagery) maintain a flat trajectory, indicating isometric activity.
- Beginning at about 2.75 seconds, the red line (unpleasant imagery) begins to ascend. This represents the onset of eccentric movement. We call this Break 1.
- Between 4 and 5 seconds, more rapid movement temporarily brings the red line off the chart, as the limb completely gives way. We call this Break 2.
- The blue and grey tracings do not break at all.
- If MMT outcomes are based on the absence or presence of an isometric plateau, the test is essentially binary, and that binary outcome can be discerned at Break 1 based on movement; it is not necessary to take the test all the way to Break 2.
- Combining that with force tracings (top box), we observe that:
- The peak force of the red tracing is almost equal to that of the grey and blue tracings.
- The peak force of the grey and blue tracings is roughly sustained; peak force of the red tracing is more of a spike.
- The force of resistance of the red tracing continues to increase after the onset of eccentric movement.
- Eccentric resistance (force) is not primarily produced by active contraction. Instead, as the muscle is eccentrically lengthening, like a stretching rubber band, elastic elements of the muscle and tendon absorb the incoming force [265,266]. Moreover, the spinal reflex response to muscle spindle stretch as the muscle lengthens adds activation to the muscle independent of incoming motor commands (or predictions). [267]. If chronic muscle weakness is due to motor control deficits that limit active contraction, as we have posited, the force produced by passive or reflex functions is moot.
- Hand-held dynamometry (HHD) is often clinically used to detect the peak force (MVC) produced by a muscle using MMT. This could result in false negatives if the test continues to Break 2, since peak force of normal and weak muscles can be equivalent before Break 2 is reached.
- The concept of adaptive force implies that a muscle’s capacity to adapt is binary.
6.2. The Binary Nature of Muscle Function
6.3. The Binary Nature of Muscle Dysfunction
6.3.1. Temporary Reversal of AMI
6.3.2. Applied Kinesiology and Related Systems
6.4“. High Resolution” Muscle Testing; an Index of Motor Control Dysfunction?
6.5. Clinical Replication of These Results
- Step 1: Scan a subject for weak muscles using MMT according to the criteria set forth in Section 6.1, and create a list including each one found. These muscles do not all need to cross the same joint, so for instance, one might test ankle, knee, and hip muscles when attempting to address symptoms in any of the areas, though testing can be performed in asymptomatic areas as well. (In order to document symptomatic changes that could accompany muscle corrections, record symptoms and positive orthopedic tests before any testing is done.)
- Step 2: Starting from the top of the list, retest and immediately treat each muscle, one at a time using the following procedure: Within 7 seconds of (re)testing each muscle, have the subject follow your index finger from right to left and back with their eyes at about 1 complete cycle per second. Continue for 15 seconds (15 reps). Some weak muscles may have strengthened by the time they are reached on the list; this ‘spontaneous’ recovery should be noted as well.
- Step 3: Following Step 2, retest each muscle, noting whether it remains weak or strengthens. When all muscles have been addressed, previously noted symptoms or tests can be repeated, documenting changes.
- Step 4: At least 24 hours later, retest all muscles that were originally found to be weak. Also review symptoms and tests from Step 1.
7. Summary and Conclusion
7.1. Limitations
Funding
Conflicts of Interest
Abbreviations
| AInf | Active inference |
| AK | Applied Kinesiology |
| AMI | Arthrogenic muscle inhibition |
| CK | Clinical Kinesiology |
| CNS | Central nervous system |
| CR | Conditioned response |
| CS | Conditioned stimulus |
| EMDR | Eye Movement Desensitization and Reprocessing |
| EMG | Electromyography |
| FEP | Free energy principle |
| FM/T | Force and Motion over Time |
| FMD | Functional motor disorder |
| FND | Functional neurologic disorder |
| FW | Functional weakness |
| HHD | Hand-held dynamometry |
| HR | High resolution |
| MCE | Motor control exercise |
| MMT | Manual muscle testing |
| motorPPC | Motor prediction, planning, and control |
| mPTSD | Muscle, motor, or movement post-traumatic stress disorder |
| MVC/MVIC | Maximum voluntary (isometric) contraction |
| nsMSD | Non-specific musculoskeletal disorder |
| PAG | Periaqueductal grey |
| PNK | Psychoneurokinesiology |
| PP | Predictive processing |
| PTSD | Post-traumatic stress disorder |
| RL | Reinforcement learning |
| TENS | Transcutaneous electrical nerve stimulation |
| TMS | Transcranial magnetic stimulation |
| TPJ | Temporo-parietal junction |
| US | Unconditioned stimulus |
References
- Balagué F, Mannion AF, Pellisé F, Cedraschi C. Non-specific low back pain. The Lancet. 2012;379:482–91.
- Fougeront N, Fleiter B. Temporomandibular disorder and comorbid neck pain: Facts and hypotheses regarding pain-induced and rehabilitation-induced motor activity changes. Canadian Journal of Physiology and Pharmacology. 2018;96.
- Jepsen JR. Can testing of six individual muscles represent a screening approach to upper limb neuropathic conditions? BMC Neurol. 2014;14:90.
- Maher C, Underwood M, Buchbinder R. Non-specific low back pain. The Lancet. 2017;389:736–47.
- Moradi A, Ebrahimzadeh MH, Ring D. Nonspecific Arm Pain. Arch Bone Jt Surg. 2013;1:53–8.
- Oliveira CB, Maher CG, Pinto RZ, Traeger AC, Lin C-WC, Chenot J-F, et al. Clinical practice guidelines for the management of non-specific low back pain in primary care: an updated overview. Eur Spine J. 2018;27:2791–803.
- O’Sullivan P. It’s time for change with the management of non-specific chronic low back pain. Br J Sports Med. 2012;46:224–7.
- Patel DR, Villalobos A. Evaluation and management of knee pain in young athletes: overuse injuries of the knee. Transl Pediatr. 2017;6:190–8.
- O’Sullivan P. Diagnosis and classification of chronic low back pain disorders: maladaptive movement and motor control impairments as underlying mechanism. Man Ther. 2005;10:242–55.
- Casser H-R, Seddigh S, Rauschmann M. Acute Lumbar Back Pain. Dtsch Arztebl Int. 2016;113:223–34.
- Meier ML, Vrana A, Schweinhardt P. Low Back Pain: The Potential Contribution of Supraspinal Motor Control and Proprioception. Neuroscientist. 2019;25:583–96.
- Schmid S, Bangerter C, Schweinhardt P, Meier ML. Identifying Motor Control Strategies and Their Role in Low Back Pain: A Cross-Disciplinary Approach Bridging Neurosciences With Movement Biomechanics. Front Pain Res. 2021;2.
- Darnall BD, Carr DB, Schatman ME. Pain Psychology and the Biopsychosocial Model of Pain Treatment: Ethical Imperatives and Social Responsibility. Pain Medicine. 2017;18:1413–5.
- Sarno JE. The Divided Mind: The Epidemic of Mindbody Disorders. 1 edition. New York: Harper Perennial; 2007.
- Sullivan MJ. Toward a biopsychomotor conceptualization of pain: implications for research and intervention. The Clinical journal of pain. 2008;24:281–90.
- Saxena A, Godena E, Maggio J, Perez DL. Towards an Outpatient Model of Care for Motor Functional Neurological Disorders: A Neuropsychiatric Perspective. Neuropsychiatr Dis Treat. 2020;16:2119–34.
- Karartı C, Basat HÇ, Özsoy İ, Özyurt F, Özsoy G, Kodak Mİ, et al. Biopsychosocial Approach in Identifying Risk Factors of Kinesiophobia in Persons with Subacromial Pain Syndrome and Developing a Clinical Prediction Tool. Indian J Orthop. 2022;57:124–36.
- Hides JA, Richardson CA, Jull GA. Multifidus Muscle Recovery Is Not Automatic After Resolution of Acute, First-Episode Low Back Pain. Spine. 1996;21:2763–9.
- Falla DL, Jull GA, Hodges PW. Patients With Neck Pain Demonstrate Reduced Electromyographic Activity of the Deep Cervical Flexor Muscles During Performance of the Craniocervical Flexion Test. Spine. 2004;29:2108.
- MacDonald D, Moseley GL, Hodges PW. Why do some patients keep hurting their back? Evidence of ongoing back muscle dysfunction during remission from recurrent back pain. PAIN®. 2009;142:183–8.
- Werner S. Anterior knee pain: an update of physical therapy. Knee Surg Sports Traumatol Arthrosc. 2014;22:2286–94.
- Russo M, Deckers K, Eldabe S, Kiesel K, Gilligan C, Vieceli J, et al. Muscle Control and Non-specific Chronic Low Back Pain. Neuromodulation. 2018;21:1–9.
- Nijs J, Daenen L, Cras P, Struyf F, Roussel N, Oostendorp RAB. Nociception affects motor output: a review on sensory-motor interaction with focus on clinical implications. Clin J Pain. 2012;28:175–81.
- Hodges PW, Butler J, Tucker K, MacDonell CW, Poortvliet P, Schabrun S, et al. Non-uniform Effects of Nociceptive Stimulation to Motoneurones during Experimental Muscle Pain. Neuroscience. 2021;463:45–56.
- Schilaty ND, McPherson AL, Nagai T, Bates NA. Arthrogenic muscle inhibition manifests in thigh musculature motor unit characteristics after anterior cruciate ligament injury. European Journal of Sport Science. 2023;23:840–50.
- McPherson AL, Schilaty ND, Anderson S, Nagai T, Bates NA. Arthrogenic muscle inhibition after anterior cruciate ligament injury: Injured and uninjured limb recovery over time. Front Sports Act Living. 2023;5.
- Sherman DA, Rush J, Glaviano NR, Norte GE. Knee joint pathology and efferent pathway dysfunction: Mapping muscle inhibition from motor cortex to muscle force. Musculoskeletal Science and Practice. 2024;74:103204.
- van Dieën JH, Moseley GL, Hodges PW. Chapter 18 - Motor control changes and low back pain: cause or effect? In: Hodges PW, Cholewicki J, van Dieën JH, editors. Spinal Control. Churchill Livingstone; 2013. p. 207–17.
- Mok NW, Brauer SG, Hodges PW. Failure to use movement in postural strategies leads to increased spinal displacement in low back pain. Spine (Phila Pa 1976). 2007;32:E537-543.
- Hodges PW, Tucker K. Moving differently in pain: a new theory to explain the adaptation to pain. Pain. 2011;152 3 Suppl:S90–8.
- Cowan SM, Schache AG, Brukner P, Bennell KL, Hodges PW, Coburn P, et al. Delayed onset of transversus abdominus in long-standing groin pain. Medicine and science in sports and exercise. 2004;36:2040–5.
- Hodges PW, Richardson CA. Delayed postural contraction of transversus abdominis in low back pain associated with movement of the lower limb. J Spinal Disord. 1998;11:46–56.
- Löfvenberg R, Kärrholm J, Sundelin G, Ahlgren O. Prolonged Reaction Time in Patients with Chronic Lateral Instability of the Ankle. Am J Sports Med. 1995;23:414–7.
- Neige C, Mavromatis N, Gagné M, Bouyer LJ, Mercier C. Effect of movement-related pain on behaviour and corticospinal excitability changes associated with arm movement preparation. The Journal of Physiology. 2018;596:2917–29.
- Oliveira DG, Kirkwood RN, Oliveira GM. Clinimetric Properties of the Applied Kinesiology Manual Muscle Test in Adults With and Without Pain: A Methodological Study. Journal of Chiropractic Medicine. 2022. [CrossRef]
- van Dieën JH, Selen LPJ, Cholewicki J. Trunk muscle activation in low-back pain patients, an analysis of the literature. J Electromyogr Kinesiol. 2003;13:333–51.
- Stergiou N, Decker LM. Human Movement Variability, Nonlinear Dynamics, and Pathology: Is There A Connection? Hum Mov Sci. 2011;30:869–88.
- Hodges PW. Motor control and pain. In: Sluka K, editor. Mechanisms and Management of Pain for the Physical Therapist. Philadelphia, PA: Wolters Kluwer Health; 2016.
- Moseley GL, Hodges PW. Are the changes in postural control associated with low back pain caused by pain interference? Clin J Pain. 2005;21:323–9.
- Larsson C, Ekvall Hansson E, Sundquist K, Jakobsson U. Impact of pain characteristics and fear-avoidance beliefs on physical activity levels among older adults with chronic pain: a population-based, longitudinal study. BMC Geriatr. 2016;16:50.
- Núñez-Cortés R, Horment-Lara G, Tapia-Malebran C, Castro M, Barros S, Vera N, et al. Role of kinesiophobia in the selective motor control during gait in patients with low back-related leg pain. J Electromyogr Kinesiol. 2023;71:102793.
- Picavet HSJ, Vlaeyen JWS, Schouten JSAG. Pain Catastrophizing and Kinesiophobia: Predictors of Chronic Low Back Pain. Am J Epidemiol. 2002;156:1028–34.
- Lund JP, Donga R, Widmer CG, Stohler CS. The pain-adaptation model: a discussion of the relationship between chronic musculoskeletal pain and motor activity. Canadian Journal of Physiology and Pharmacology. 1991;69:683–94.
- Merkle SL, Sluka KA, Frey-Law LA. The interaction between pain and movement. J Hand Ther. 2020;33:60–6.
- Andersen OK, Sonnenborg FA, Arendt-Nielsen L. Reflex receptive fields for human withdrawal reflexes elicited by non-painful and painful electrical stimulation of the foot sole. Clin Neurophysiol. 2001;112:641–9.
- Dimitrova A, Kolb FP, Elles HG, Maschke M, Forsting M, Diener HC, et al. Cerebellar Responses Evoked by Nociceptive Leg Withdrawal Reflex as Revealed by Event-Related fMRI. Journal of Neurophysiology. 2003;90:1877–86.
- Jarrell F, Jacks A, Faubert J. An introduction to Spinal Reflex Analysis. Journal of the Australian Association of Massage Therapists. 2009;7:6–11.
- Ogden P, Minton K, Pain C, Siegel DJ, van der Kolk BA. Trauma and the Body: A Sensorimotor Approach to Psychotherapy. 1 edition. New York: W. W. Norton & Company; 2006.
- Levine PA. Trauma and memory: Brain and body in a search for the living past: A practical guide for understanding and working with traumatic memory. North Atlantic Books; 2015.
- Payne P, Levine PA, Crane-Godreau MA. Somatic experiencing: using interoception and proprioception as core elements of trauma therapy. Front Psychol. 2015;6:93.
- van der Kolk BA. The Body Keeps the Score: Brain, Mind, and Body in the Healing of Trauma. Reprint edition. New York, NY: Penguin Books; 2015.
- Binder MD, Hirokawa N, Windhorst U, editors. Sherrington’s Law of Reciprocal Innervation. In: Encyclopedia of Neuroscience. Springer Berlin Heidelberg; 2009. p. 3687–3687.
- Dankaerts W, O’Sullivan P, Burnett A, Straker L. Altered Patterns of Superficial Trunk Muscle Activation During Sitting in Nonspecific Chronic Low Back Pain Patients: Importance of Subclassification. Spine. 2006;31:2017–23.
- Summers SJ, Chipchase LS, Hirata R, Graven-Nielsen T, Cavaleri R, Schabrun SM. Motor adaptation varies between individuals in the transition to sustained pain. PAIN. 2019;160:2115–25.
- Brumagne S, Janssens L, Janssens E, Goddyn L. Altered postural control in anticipation of postural instability in persons with recurrent low back pain. Gait & Posture. 2008;28:657–62.
- Mientjes MI, Frank JS. Balance in chronic low back pain patients compared to healthy people under various conditions in upright standing. Clin Biomech (Bristol). 1999;14:710–6.
- Luomajoki H, Kool J, de Bruin ED, Airaksinen O. Movement control tests of the low back; evaluation of the difference between patients with low back pain and healthy controls. BMC Musculoskeletal Disorders. 2008;9:170.
- Revel M, Andre-Deshays C, Minguet M. Cervicocephalic kinesthetic sensibility in patients with cervical pain. Arch Phys Med Rehabil. 1991;72:288–91.
- Brandt M, Danneels L, Meirezonne H, Oosterwijck JV, Willems T, Matheve T. Clinically assessed lumbopelvic sensorimotor control tests in low back pain: are they actually valid? A systematic review according to COSMIN guidelines. Musculoskeletal Science & Practice. 2024;71.
- Schulz J, Vitt E, Niemier K. A systematic review of motor control tests in low back pain based on reliability and validity. J Bodyw Mov Ther. 2022;29:239–50.
- Saragiotto BT, Maher CG, Yamato TP, Costa LOP, Menezes Costa LC, Ostelo RWJG, et al. Motor control exercise for chronic non-specific low-back pain. Cochrane Database Syst Rev. 2016;:CD012004.
- Mapinduzi J, Ndacayisaba G, Mahaudens P, Hidalgo B. Effectiveness of motor control exercises versus other musculoskeletal therapies in patients with pelvic girdle pain of sacroiliac joint origin: A systematic review with meta-analysis of randomized controlled trials. Journal of Back and Musculoskeletal Rehabilitation. 2022;35:713–28.
- Goertz CM, Xia T, Long CR, Vining RD, Pohlman KA, DeVocht JW, et al. Effects of spinal manipulation on sensorimotor function in low back pain patients--A randomised controlled trial. Man Ther. 2016;21:183–90.
- Christiansen TL, Niazi IK, Holt K, Nedergaard RW, Duehr J, Allen K, et al. The effects of a single session of spinal manipulation on strength and cortical drive in athletes. Eur J Appl Physiol. 2018;118:737–49.
- Kendall JC, Vindigni D, Polus BI, Azari MF, Harman SC. Effects of manual therapies on stability in people with musculoskeletal pain: a systematic review. Chiropr Man Therap. 2020;28:13.
- Hopkins JT, Ingersoll CD, Edwards J, Klootwyk TE. Cryotherapy and Transcutaneous Electric Neuromuscular Stimulation Decrease Arthrogenic Muscle Inhibition of the Vastus Medialis After Knee Joint Effusion. J Athl Train. 2002;37:25–31.
- Hart JM, Kuenze CM, Pietrosimone BG, Ingersoll CD. Quadriceps function in anterior cruciate ligament-deficient knees exercising with transcutaneous electrical nerve stimulation and cryotherapy: a randomized controlled study. Clin Rehabil. 2012;26:974–81.
- Hart JM, Kuenze CM, Diduch DR, Ingersoll CD. Quadriceps Muscle Function After Rehabilitation With Cryotherapy in Patients With Anterior Cruciate Ligament Reconstruction. Journal of Athletic Training. 2014;49:733–9.
- Rush JL, Sherman DA, Bazett-Jones DM, Ingersoll CD, Norte GE. Understanding Athletic Trainers’ Knowledge, Intervention, and Barriers Toward Arthrogenic Muscle Inhibition. Journal of Sport Rehabilitation. 2021;1 aop:1–9.
- Norte G, Rush J, Sherman D. Arthrogenic Muscle Inhibition: Best Evidence, Mechanisms, and Theory for Treating the Unseen in Clinical Rehabilitation. Journal of Sport Rehabilitation. 2021;:1–19.
- Hopkins JT, Ingersoll CD, Cordova ML, Edwards JE. Intrasession and intersession reliability of the soleus H-reflex in supine and standing positions. Electromyogr Clin Neurophysiol. 2000;40:89–94.
- Hurley MV. The effects of joint damage on muscle function, proprioception and rehabilitation. Manual therapy. 1997;2:11–7.
- Hurley MV, Jones DW, Newham DJ. Arthrogenic quadriceps inhibition and rehabilitation of patients with extensive traumatic knee injuries. Clinical Science. 1994;86:305–10.
- McVey ED, Palmieri RM, Docherty CL, Zinder SM, Ingersoll CD. Arthrogenic muscle inhibition in the leg muscles of subjects exhibiting functional ankle instability. Foot and Ankle International. 2005;26:1055.
- Needle AR, Lepley AS, Grooms DR. Central nervous system adaptation after ligamentous injury: a summary of theories, evidence, and clinical interpretation. Sports Medicine. 2017;47:1271–88.
- Park J, Grindstaff TL, Hart JM, Hertel JN, Ingersoll CD. Knee-Extension Exercise’s Lack of Immediate Effect on Maximal Voluntary Quadriceps Torque and Activation in Individuals with Anterior Knee Pain. Journal of Sport Rehabilitation. 2012;21:119–26.
- Mense S, Gerwin RD, editors. Muscle Pain: Diagnosis and Treatment. 2010 edition. Heidelberg ; New York: Springer; 2010.
- Tayfur B, Charuphongsa C, Morrissey D, Miller SC. Neuromuscular Function of the Knee Joint Following Knee Injuries: Does It Ever Get Back to Normal? A Systematic Review with Meta-Analyses. Sports Medicine (Auckland, N.z). 2020;51:321.
- Capin JJ, Bade MJ, Jennings JM, Snyder-Mackler L, Stevens-Lapsley JE. Total Knee Arthroplasty Assessments Should Include Strength and Performance-Based Functional Tests to Complement Range-of-Motion and Patient-Reported Outcome Measures. Physical Therapy. 2022;102:pzac033.
- Makkuva A, Surve P, Makkuva A, Surve P. Exploring physiotherapy strategies in arthrogenic muscle inhibition: A scoping review. International Journal of Science and Research Archive. 2024;12:2609–20.
- Gin R, Green B. George Goodheart, Jr., D.C., and a history of applied kinesiology. J Manipulative Physiol Ther. 1997;20:331–7.
- Walther DS. Applied Kinesiology Synopsis 2nd Edition. Systems DC Pueblo, CO; 2000.
- Goodheart GJ. You’ll Be Better: The Story of Applied Kinesiology. 2005.
- Frost R. Applied kinesiology: a training manual and reference book of basic principles and practices. Berkeley, Calif.: North Atlantic Books; 2013.
- Mercola, Joe, Buhler CF. AMIT: An Effective Treatment for Muscle Injuries and Pain. Mercola.com. 2013. http://fitness.mercola.com/sites/fitness/archive/2013/01/04/advanced-muscle-integration-technique.aspx. Accessed 7 Jan 2013.
- Weissfeld RK. Mind, trauma & muscle inhibition Part I: Experiment and case history yield novel theory of muscular PTSD [Hypothesis]. 2021;2.
- Kelly MA, Freeman LK, Dornan T. Family Physicians’ Experiences of Physical Examination. Ann Fam Med. 2019;17:304–10.
- ICD-10-CM. ICD-10-CM Official Guidelines for Coding and Reporting FY 2024 -- UPDATED April 1, 2024 (April 1, 2024 - September 30, 2024). 2024.
- Nijs J, Paul van Wilgen C, Van Oosterwijck J, van Ittersum M, Meeus M. How to explain central sensitization to patients with “unexplained” chronic musculoskeletal pain: practice guidelines. Man Ther. 2011;16:413–8.
- Woolf CJ. Central sensitization: Implications for the diagnosis and treatment of pain. Pain. 2011;152 3 Suppl:S2-15.
- Bonin RP, De Koninck Y. A spinal analog of memory reconsolidation enables reversal of hyperalgesia. Nat Neurosci. 2014;17:1043–5.
- Pelletier R, Higgins J, Bourbonnais D. Is neuroplasticity in the central nervous system the missing link to our understanding of chronic musculoskeletal disorders? BMC Musculoskelet Disord. 2015;16.
- Ader R. Psychoneuroimmunology. In: Smelser NJ, Baltes PB, editors. International Encyclopedia of the Social & Behavioral Sciences. Oxford: Pergamon; 2001. p. 12422–8.
- Furuya S, Hanakawa T. The curse of motor expertise: Use-dependent focal dystonia as a manifestation of maladaptive changes in body representation. Neurosci Res. 2016;104:112–9.
- Tomporowski PD, Qazi AS. Cognitive-Motor Dual Task Interference Effects on Declarative Memory: A Theory-Based Review. Front Psychol. 2020;11.
- Prushansky T, Gepstein R, Gordon C, Dvir Z. Cervical muscles weakness in chronic whiplash patients. Clin Biomech (Bristol, Avon). 2005;20:794–8.
- Barton CJ, Lack S, Malliaras P, Morrissey D. Gluteal muscle activity and patellofemoral pain syndrome: a systematic review. Br J Sports Med. 2013;47:207–14.
- Palmieri-Smith RM, Hopkins JT, Brown TN. Peroneal activation deficits in persons with functional ankle instability. The American journal of sports medicine. 2009;37:982–8.
- Dong S, Liu Y, Liu Z, Shen P, Sun H, Zhang P, et al. Can Arthrogenic Muscle Inhibition Exist in Peroneal Muscles Among People with Chronic Ankle Instability? A Cross-sectional Study. Sports Medicine - Open. 2024;10:35.
- Lee JH, Jung HW, Jang WY. A prospective study of the muscle strength and reaction time of the quadriceps, hamstring, and gastrocnemius muscles in patients with plantar fasciitis. BMC Musculoskeletal Disorders. 2020;21:722.
- Cuthbert S, Blum C, Rosner A. The Association of Manual Muscle Tests and Treatment Outcomes With Headache and Cranial Dysfunctions: A Retrospective Case Series Report. Altern Ther Health Med. 2018;24:8–21.
- Wilder RP, Sethi S. Overuse injuries: tendinopathies, stress fractures, compartment syndrome, and shin splints. Clinics in Sports Medicine. 2004;23:55–81.
- Schaefer LV, Dech S, Wolff LL, Bittmann FN. Emotional Imagery Influences the Adaptive Force in Young Women: Unpleasant Imagery Reduces Instantaneously the Muscular Holding Capacity. Brain Sciences. 2022;12:1318.
- Chen Y, Chen XY, Jakeman LB, Schalk G, Stokes BT, Wolpaw JR. The Interaction of a New Motor Skill and an Old One: H-Reflex Conditioning and Locomotion in Rats. J Neurosci. 2005;25:6898–906.
- Hurley MV. The role of muscle weakness in the pathogenesis of osteoarthritis. Rheumatic Disease Clinics of North America. 1999;25:283–98.
- Pietrosimone BG, Hertel J, Ingersoll CD, Hart JM, Saliba SA. Voluntary quadriceps activation deficits in patients with tibiofemoral osteoarthritis: a meta-analysis. PM R. 2011;3:153–62; quiz 162.
- Pietrosimone B, Blackburn JT, Harkey MS, Luc BA, Pamukoff DN, Hart JM. Clinical Strategies for Addressing Muscle Weakness Following Knee Injury. Clinics in sports medicine. 2015;34:285–300.
- Palermi S, Vittadini F, Vecchiato M, Corsini A, Demeco A, Massa B, et al. Managing Lower Limb Muscle Reinjuries in Athletes: From Risk Factors to Return-to-Play Strategies. Journal of Functional Morphology and Kinesiology. 2023;8:155.
- de Sousa CS, de Jesus FLA, Machado MB, Ferreira G, Ayres IGT, de Aquino LM, et al. Lower limb muscle strength in patients with low back pain: a systematic review and meta-analysis. J Musculoskelet Neuronal Interact. 2019;19:69–78.
- Reed-Jones RJ, Vallis LA. Proprioceptive deficits of the lower limb following anterior cruciate ligament deficiency affect whole body steering control. Exp Brain Res. 2007;182:249–60.
- Hodges PW. Pain and motor control: from the laboratory to rehabilitation. Journal of Electromyography and Kinesiology. 2011;21:220–8.
- Wang HK, Cochrane T. Mobility impairment, muscle imbalance, muscle weakness, scapular asymmetry and shoulder injury in elite volleyball athletes. Journal of sports medicine and physical fitness. 2001;41:403.
- Schmitt LC, Paterno MV, Hewett TE. The Impact of Quadriceps Femoris Strength Asymmetry on Functional Performance at Return to Sport Following Anterior Cruciate Ligament Reconstruction. Journal of Orthopaedic & Sports Physical Therapy. 2012;42:750–9.
- Munn J, Sullivan SJ, Schneiders AG. Evidence of sensorimotor deficits in functional ankle instability: A systematic review with meta-analysis. Journal of Science and Medicine in Sport. 2010;13:2–12.
- Lewek M, Rudolph K, Axe M, Snyder-Mackler L. The effect of insufficient quadriceps strength on gait after anterior cruciate ligament reconstruction. Clinical Biomechanics. 2002;17:56–63.
- Kim K-M, Kim J-S, Needle AR. Soleus arthrogenic muscle inhibition following acute lateral ankle sprain correlates with symptoms and ankle disability but not with postural control. Journal of Sport and Health Science. 2024. [CrossRef]
- O’Reilly S, Jones A, Doherty M. Muscle weakness in osteoarthritis. Current opinion in rheumatology. 1997;9:259–62.
- Roos EM, Herzog W, Block JA, Bennell KL. Muscle weakness, afferent sensory dysfunction and exercise in knee osteoarthritis. Nature Reviews Rheumatology. 2010;7:57–63.
- Roth R. A Warning Signal to the Body. Dtsch Arztebl Int. 2016;113:562–3.
- Pontén M, Fust J, D’Onofrio P, Dorp R van, Sunnergård L, Ingre M, et al. The pain alarm response - an example of how conscious awareness shapes pain perception. Sci Rep. 2019;9:12478.
- Stegemann A, Liu S, Retana Romero OA, Oswald MJ, Han Y, Beretta CA, et al. Prefrontal engrams of long-term fear memory perpetuate pain perception. Nat Neurosci. 2023;26:820–9.
- Staud R. Evidence for shared pain mechanisms in osteoarthritis, low back pain, and fibromyalgia. Curr Rheumatol Rep. 2011;13:513–20.
- Cerritelli F 1, Esteves JE 2 1 C-BHRD, osteojorge@gmail. com 2 Clinical-Based Human Research Department FCC, osteojorge@gmail.com, Malta ICOM Educational G 1071 G. An Enactive–Ecological Model to Guide Patient-Centered Osteopathic Care. 2022;:1092.
- Friston K. The free-energy principle: a unified brain theory? Nature Reviews Neuroscience. 2010;11:127–38.
- Adams RA, Shipp S, Friston KJ. Predictions not commands: active inference in the motor system. Brain Structure and Function. 2013;218:611–43.
- Parr T, Friston K, Pezzulo G. Generative models for sequential dynamics in active inference. Cogn Neurodyn. 2024;18:3259–72.
- Parr T, Friston KJ. The Anatomy of Inference: Generative Models and Brain Structure. Front Comput Neurosci. 2018;12:90.
- Ongaro G, Kaptchuk TJ. Symptom perception, placebo effects, and the Bayesian brain. Pain. 2019;160:1–4.
- Suttie J. Eight Ways Your Perception of Reality Is Skewed. Greater Good. 2020. https://greatergood.berkeley.edu/article/item/eight_reasons_to_distrust_your_own_perceptions. Accessed 29 Mar 2025.
- Bohlen L, Shaw R, Cerritelli F, Esteves JE. Osteopathy and Mental Health: An Embodied, Predictive, and Interoceptive Framework. Front Psychol. 2021;12:767005.
- Kuperman P, Talmi D, Katz N, Treister R. Certainty in ascending sensory signals – The unexplored driver of analgesic placebo response. Medical Hypotheses. 2020;143:110113.
- Linson A, Parr T, Friston KJ. Active inference, stressors, and psychological trauma: A neuroethological model of (mal)adaptive explore-exploit dynamics in ecological context. Behavioural Brain Research. 2020;380:112421.
- Seriès P. Post-traumatic stress disorder as a disorder of prediction. Nat Neurosci. 2019;22:334–6.
- Barrett LF, Simmons WK. Interoceptive predictions in the brain. Nature Reviews Neuroscience. 2015;16:419.
- Kozlowska K, Walker P, McLean L, Carrive P. Fear and the Defense Cascade: Clinical Implications and Management. Harv Rev Psychiatry. 2015;23:263–87.
- Harricharan S, McKinnon MC, Lanius RA. How Processing of Sensory Information From the Internal and External Worlds Shape the Perception and Engagement With the World in the Aftermath of Trauma: Implications for PTSD. Front Neurosci. 2021;15.
- Kube T, Berg M, Kleim B, Herzog P. Rethinking post-traumatic stress disorder - A predictive processing perspective. Neurosci Biobehav Rev. 2020;113:448–60.
- Van den Bergh O, Witthöft M, Petersen S, Brown RJ. Symptoms and the body: Taking the inferential leap. Neuroscience & Biobehavioral Reviews. 2017;74:185–203.
- Barrett LF. How Emotions Are Made. Pan Macmillan; 2017.
- Castejón J, Chen F, Yasoda-Mohan A, Ó Sé C, Vanneste S. Chronic pain – A maladaptive compensation to unbalanced hierarchical predictive processing. NeuroImage. 2024;297:120711.
- Edwards MJ, Adams RA, Brown H, Pareés I, Friston KJ. A Bayesian account of ‘hysteria.’ Brain. 2012;135:3495–512.
- Clark A. Predictions, precision, and agentive attention. Consciousness and Cognition. 2017;56:115–9.
- Dehne E. The Spinal Adaptation Syndrome (A Theory Based on the Study of Sprains). Clinical Orthopaedics and Related Research®. 1955;5:211–20.
- Gabel CP, Guy B, Mokhtarinia HR, Melloh M. Slacklining: A narrative review on the origins, neuromechanical models and therapeutic use. World J Orthop. 2021;12:360–75.
- Stokes M, Young A. The contribution of reflex inhibition to arthrogenous muscle weakness. Clinical Science. 1984;67:7–14.
- Criss CR, Lepley AS, Onate JA, Clark BC, Simon JE, France CR, et al. Brain activity associated with quadriceps strength deficits after anterior cruciate ligament reconstruction. Sci Rep. 2023;13:8043.
- Frissora KN. Reliability of Measuring Voluntary Quadriceps Activation Using the Burst Superimposition and Interpolated Twitch Techniques. 2014.
- Hart JM, Pietrosimone B, Hertel J, Ingersoll CD. Quadriceps activation following knee injuries: a systematic review. J Athl Train. 2010;45:87–97.
- Patel HH, Berlinberg EJ, Nwachukwu B, Williams RJ, Mandelbaum B, Sonkin K, et al. Quadriceps Weakness is Associated with Neuroplastic Changes Within Specific Corticospinal Pathways and Brain Areas After Anterior Cruciate Ligament Reconstruction: Theoretical Utility of Motor Imagery-Based Brain-Computer Interface Technology for Rehabilitation. Arthrosc Sports Med Rehabil. 2022;5:e207–16.
- Sonnery-Cottet B, Saithna A, Quelard B, Daggett M, Borade A, Ouanezar H, et al. Arthrogenic muscle inhibition after ACL reconstruction: a scoping review of the efficacy of interventions. Br J Sports Med. 2018;:bjsports-2017-098401.
- Sonnery-Cottet B, Hopper GP, Gousopoulos L, Vieira TD, Thaunat M, Fayard J-M, et al. Arthrogenic Muscle Inhibition Following Knee Injury or Surgery: Pathophysiology, Classification, and Treatment. Video Journal of Sports Medicine. 2022;2:26350254221086295.
- Javadian Y, Adabi M, Heidari B, Babaei M, Firouzjahi A, Ghahhari BY, et al. Quadriceps Muscle Strength Correlates With Serum Vitamin D and Knee Pain in Knee Osteoarthritis. Clin J Pain. 2017;33:67–70.
- Lepley AS, Lepley LK. Mechanisms of Arthrogenic Muscle Inhibition. Journal of Sport Rehabilitation. 2021;1 aop:1–10.
- Durfee WK, Iaizzo PA. Rehabilitation and muscle testing. Encyclopedia of Medical Devices and Instrumentation. 2006.
- Conroy VM, Murray JBN, Alexopulos QT, McCreary J. Kendall’s Muscles: Testing and Function with Posture and Pain. 6th edition. Wolters Kluwer Health; 2022.
- Avers D, Lott DJ, Brown M. Daniels and Worthingham’s Muscle Testing. 11th edition. Saunders; 2024.
- Nakajima T, Sakamoto M, Endoh T, Komiyama T. Location-specific and task-dependent modulation of cutaneous reflexes in intrinsic human hand muscles. Clinical Neurophysiology. 2006;117:420–9.
- Oishi K, Kimura M, Yasukawa M, Yoneda T, Maeshima T. Amplitude reduction of H-reflex during mental movement simulation in elite athletes. Behav Brain Res. 1994;62:55–61.
- Behm D, Power K, Drinkwater E. Comparison of interpolation and central activation ratios as measures of muscle inactivation. Muscle & Nerve. 2001;24:925–34.
- Fukunaga T, Johnson CD, Nicholas SJ, McHugh MP. Muscle hypotrophy, not inhibition, is responsible for quadriceps weakness during rehabilitation after anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc. 2019;27:573–9.
- Verbunt JA, Seelen HA, Vlaeyen JW, Bousema EJ, van der Heijden GJ, Heuts PH, et al. Pain-related factors contributing to muscle inhibition in patients with chronic low back pain: an experimental investigation based on superimposed electrical stimulation. The Clinical journal of pain. 2005;21:232–40.
- Osan R, Tort ABL, Amaral OB. A Mismatch-Based Model for Memory Reconsolidation and Extinction in Attractor Networks. PLoS One. 2011;6:e23113.
- Pedreira ME, Pérez-Cuesta LM, Maldonado H. Mismatch Between What Is Expected and What Actually Occurs Triggers Memory Reconsolidation or Extinction. Learn Mem. 2004;11:579–85.
- Ploghaus A, Tracey I, Clare S, Gati JS, Rawlins JNP, Matthews PM. Learning about pain: The neural substrate of the prediction error for aversive events. PNAS. 2000;97:9281–6.
- Wacongne C, Changeux J-P, Dehaene S. A Neuronal Model of Predictive Coding Accounting for the Mismatch Negativity. J Neurosci. 2012;32:3665–78.
- Dancey E. The effect of experimental pain on neural function and motor learning. 2017.
- McNally GP, Westbrook RF. Predicting danger: The nature, consequences, and neural mechanisms of predictive fear learning. Learn Mem. 2006;13:245–53.
- Meulders A, Vansteenwegen D, Vlaeyen JWS. The acquisition of fear of movement-related pain and associative learning: A novel pain-relevant human fear conditioning paradigm. PAIN. 2011;152:2460–9.
- Salomoni SE, Marinovic W, Carroll TJ, Hodges PW. Motor Strategies Learned during Pain Are Sustained upon Pain-free Reexposure to Task. Med Sci Sports Exerc. 2019;51:2334–43.
- Palmieri RM, Weltman A, Edwards JE, Tom JA, Saliba EN, Mistry DJ, et al. Pre-synaptic modulation of quadriceps arthrogenic muscle inhibition. Knee Surgery, Sports Traumatology, Arthroscopy. 2005;13:370–6.
- Brown H, Friston KJ, Bestmann S. Active Inference, Attention, and Motor Preparation. Front Psychol. 2011;2.
- Ocampo B, Painter DR, Kritikos A. Event coding and motor priming: how attentional modulation may influence binding across action properties. Experimental Brain Research. 2012;219:139–50.
- Hapidou EG, O’Brien MA, Pierrynowski MR, de las Heras E, Patel M, Patla T. Fear and Avoidance of Movement in People with Chronic Pain: Psychometric Properties of the 11-Item Tampa Scale for Kinesiophobia (TSK-11). Physiother Can. 2012;64:235–41.
- Larsson C, Ekvall Hansson E, Sundquist K, Jakobsson U. Kinesiophobia and its relation to pain characteristics and cognitive affective variables in older adults with chronic pain. BMC Geriatr. 2016;16.
- Nijs J, Lluch Girbés E, Lundberg M, Malfliet A, Sterling M. Exercise therapy for chronic musculoskeletal pain: Innovation by altering pain memories. Manual Therapy. 2015;20:216–20.
- Santi M, Diener I, Oostendorp R. Assessment and treatment of patients with kinesiophobia: A Delphi consensus. Journal of Novel Physiotherapy and Rehabilitation. 2022;6:023–8.
- Gabler C, Kitzman PH, Mattacola CG. Targeting quadriceps inhibition with electromyographic biofeedback: a neuroplastic approach. Critical ReviewsTM in Biomedical Engineering. 2013;41:125–35.
- Pietrosimone B, McLeod MM, Florea D, Gribble PA, Tevald MA. Immediate increases in quadriceps corticomotor excitability during an electromyography biofeedback intervention. J Electromyogr Kinesiol. 2015;25:316–22.
- Stone J, Warlow C, Sharpe M. The symptom of functional weakness: a controlled study of 107 patients. Brain. 2010;133:1537–51.
- Mayo Clinic. Functional neurologic disorder/conversion disorder - Symptoms and causes. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/conversion-disorder/symptoms-causes/syc-20355197. Accessed 21 Apr 2023.
- Bühler J, Weber S, Loukas S, Walther S, Aybek S. Non-invasive neuromodulation of the right temporoparietal junction using theta-burst stimulation in functional neurological disorder. BMJ Neurol Open. 2024;6.
- Moccia L, di Luzio M, Conte E, Modica M, Ambrosecchia M, Ardizzi M, et al. Sense of agency and its disturbances: A systematic review targeting the intentional binding effect in neuropsychiatric disorders. Psychiatry and Clinical Neurosciences. 2024;78:3–18.
- Welniarz Q, Worbe Y, Gallea C. The Forward Model: A Unifying Theory for the Role of the Cerebellum in Motor Control and Sense of Agency. Frontiers in Systems Neuroscience. 2021;15:22.
- Halicka M, Vittersø AD, Proulx MJ, Bultitude JH. Neuropsychological Changes in Complex Regional Pain Syndrome (CRPS). Behavioural Neurology. 2020;2020:4561831.
- Filbrich L, Verfaille C, Vannuscorps G, Berquin A, Barbier O, Libouton X, et al. Atypical influence of biomechanical knowledge in Complex Regional Pain Syndrome-towards a different perspective on body representation. Sci Rep. 2023;13:520.
- Bennett K, Diamond C, Hoeritzauer I, Gardiner P, McWhirter L, Carson A, et al. A practical review of functional neurological disorder (FND) for the general physician. Clin Med (Lond). 2021;21:28–36.
- Balsam PD, Gallistel CR. Temporal maps and informativeness in associative learning. Trends Neurosci. 2009;32:73–8.
- Bouton ME. Learning and Behavior: A Contemporary Synthesis. 1st edition. Sunderland, Mass: Sinauer Associates; 2006.
- Eliassen JC, Souza T, Sanes JN. Experience-Dependent Activation Patterns in Human Brain during Visual-Motor Associative Learning. J Neurosci. 2003;23:10540–7.
- Brown TH, Kairiss EW, Keenan CL. Hebbian synapses: biophysical mechanisms and algorithms. Annual review of neuroscience. 1990;13:475–511.
- Kim JJ, Thompson RF. Cerebellar circuits and synaptic mechanisms involved in classical eyeblink conditioning. Trends in neurosciences. 1997;20:177–81.
- Schreurs BG, Burhans LB. Eyeblink Classical Conditioning and Post-Traumatic Stress Disorder – A Model Systems Approach. Front Psychiatry. 2015;6.
- Koch C. What Is Consciousness? Nature. 2018;557:S8–12.
- Ernst TM, Brol AE, Gratz M, Ritter C, Bingel U, Schlamann M, et al. The cerebellum is involved in processing of predictions and prediction errors in a fear conditioning paradigm. eLife. 2019;8:e46831.
- Hwang K-D, Kim SJ, Lee Y-S. Cerebellar Circuits for Classical Fear Conditioning. Frontiers in Cellular Neuroscience. 2022;16.
- Blithikioti C, Nuño L, Guell X, Pascual-Diaz S, Gual A, Balcells-Olivero Μ, et al. The cerebellum and psychological trauma: A systematic review of neuroimaging studies. Neurobiology of Stress. 2022;17:100429.
- Blithikioti C, Duek O, Gordon C, Krystal JH, Levy I, Harpaz-Rotem I, et al. Cerebellar Contributions to Traumatic Autobiographical Memory in People with Post-Traumatic Stress Disorder. Cerebellum. 2024;23:2332–40.
- Terpou BA, Densmore M, Thome J, Frewen P, McKinnon MC, Lanius RA. The Innate Alarm System and Subliminal Threat Presentation in Posttraumatic Stress Disorder: Neuroimaging of the Midbrain and Cerebellum. Chronic Stress. 2019;3:2470547018821496.
- R.C. Miall. The cerebellum, predictive control and motor coordination. In: Sensory Guidance of Movement. John Wiley & Sons; 2008.
- Shadmehr R, Smith MA, Krakauer JW. Error correction, sensory prediction, and adaptation in motor control. Annual review of neuroscience. 2010;33:89–108.
- Angel RW. Efference copy in the control of movement. Neurology. 1976;26:1164–1164.
- Chabrol FP, Blot A, Mrsic-Flogel TD. Cerebellar Contribution to Preparatory Activity in Motor Neocortex. Neuron. 2019;103:506-519.e4.
- Gao Z, Davis C, Thomas AM, Economo MN, Abrego AM, Svoboda K, et al. A cortico-cerebellar loop for motor planning. Nature. 2018;563:113–6.
- Ito M. Bases and implications of learning in the cerebellum—adaptive control and internal model mechanism. Progress in brain research. 2005;148:95–109.
- Welman M, Smit AE, Jongen JLM, Tibboel D, van der Geest JN, Holstege JC. Pain Experience is Somatotopically Organized and Overlaps with Pain Anticipation in the Human Cerebellum. Cerebellum. 2018;17:447–60.
- Boillat Y, Bazin P-L, van der Zwaag W. Whole-body somatotopic maps in the cerebellum revealed with 7T fMRI. NeuroImage. 2020;211:116624.
- Coombes SA, Tandonnet C, Fujiyama H, Janelle CM, Cauraugh JH, Summers JJ. Emotion and motor preparation: A transcranial magnetic stimulation study of corticospinal motor tract excitability. Cogn Affect Behav Neurosci. 2009;9:380–8.
- Koutsikou S, Crook JJ, Earl EV, Leith JL, Watson TC, Lumb BM, et al. Neural substrates underlying fear-evoked freezing: the periaqueductal grey–cerebellar link. The Journal of Physiology. 2014;592:2197–213.
- Roelofs K. Freeze for action: neurobiological mechanisms in animal and human freezing. Philos Trans R Soc Lond B Biol Sci. 2017;372.
- da Silva GN, Seiffert N, Tovote P. Cerebellar contribution to the regulation of defensive states. Front Syst Neurosci. 2023;17.
- Rosner AL, Leisman G, Gilchriest J, Charles E, Keschner MG, Minond M. Reliability and validity of therapy localization as determined from multiple examiners and instrumentation. Functional Neurology, Rehabilitation, and Ergonomics. 2015;5:365.
- Jensen AM, Stevens RJ, Burls AJ. Estimating the accuracy of muscle response testing: two randomised-order blinded studies. BMC complementary and alternative medicine. 2016;16:492.
- De Peuter S, Diest I, Vansteenwegen D, Bergh O, Vlaeyen JW. Understanding fear of pain in chronic pain: interoceptive fear conditioning as a novel approach. European journal of pain. 2011;15:889–94.
- Zaman J, De Peuter S, Van Diest I, Van den Bergh O, Vlaeyen JWS. Interoceptive cues predicting exteroceptive events. Int J Psychophysiol. 2016;109:100–6.
- Li CN, Keay KA, Henderson LA, Mychasiuk R. Re-examining the Mysterious Role of the Cerebellum in Pain. J Neurosci. 2024;44:e1538232024.
- Manda O, Hadjivassiliou M, Varrassi G, Zavridis P, Zis P. Exploring the Role of the Cerebellum in Pain Perception: A Narrative Review. Pain Ther. 2025. [CrossRef]
- Kharrazian D, Brock B. Cerebellum and Immunity. In: Functional Neuroloty Seminars, 2016. 2016.
- Benagiano V, Rizzi A. Autonomic functions of the cerebellum: Anatomical bases and clinical implications. Italian Journal of Anatomy and Embryology. 2024;128:113–23.
- Cornwell BR, Overstreet C, Krimsky M, Grillon C. Passive avoidance is linked to impaired fear extinction in humans. Learn Mem. 2013;20:164–9.
- Jarvik ME, Kopp R. An improved one-trial passive avoidance learning situation. Psychological reports. 1967;21:221–4.
- Linson A, Friston K. Reframing PTSD for computational psychiatry with the active inference framework. Cognitive Neuropsychiatry. 2019;24:347–68.
- Kozlowska K. The Developmental Origins of Conversion Disorders. Clin Child Psychol Psychiatry. 2007;12:487–510.
- Matzel LD, Han YR, Grossman H, Karnik MS, Patel D, Scott N, et al. Individual Differences in the Expression of a “General” Learning Ability in Mice. J Neurosci. 2003;23:6423–33.
- Ferrara NC, Kwapis JL, Trask S. Memory retrieval, reconsolidation, and extinction: Exploring the boundary conditions of post-conditioning cue exposure. Front Synaptic Neurosci. 2023;15.
- Liew BXW, Vecchio AD, Falla D. The influence of musculoskeletal pain disorders on muscle synergies—A systematic review. PLOS ONE. 2018;13:e0206885.
- Doyon J, Penhune V, Ungerleider LG. Distinct contribution of the cortico-striatal and cortico-cerebellar systems to motor skill learning. Neuropsychologia. 2003;41:252–62.
- Hull C. Prediction signals in the cerebellum: Beyond supervised motor learning. eLife. 2020;9:e54073.
- de Silva P, Rachman S. Does escape behaviour strengthen agoraphobic avoidance? A preliminary study. Behav Res Ther. 1984;22:87–91.
- Hamm AO, Richter J, Pané-Farré C, Westphal D, Wittchen H-U, Vossbeck-Elsebusch AN, et al. Panic disorder with agoraphobia from a behavioral neuroscience perspective: Applying the research principles formulated by the Research Domain Criteria (RDoC) initiative: Panic disorder with agoraphobia. Psychophysiology. 2016;53:312–22.
- Krypotos A-M, Effting M, Kindt M, Beckers T. Avoidance learning: a review of theoretical models and recent developments. Front Behav Neurosci. 2015;9.
- Chen XY, Wolpaw JR. Ablation of cerebellar nuclei prevents H-reflex down-conditioning in rats. Learn Mem. 2005;12:248–54.
- Thompson AK, Wolpaw JR. The Simplest Motor Skill: Mechanisms and Applications of Reflex Operant Conditioning. Exercise and Sport Sciences Reviews. 2014;42:82–90.
- Wolpaw JR, Chen XY. The cerebellum in maintenance of a motor skill: A hierarchy of brain and spinal cord plasticity underlies H-reflex conditioning. Learn Mem. 2006;13:208–15.
- Lewis C, Roberts NP, Andrew M, Starling E, Bisson JI. Psychological therapies for post-traumatic stress disorder in adults: systematic review and meta-analysis. Eur J Psychotraumatol. 2020;11:1729633.
- Rikkert M, van Rood Y, de Roos C, Ratter J, van den Hout M. A trauma-focused approach for patients with tinnitus: the effectiveness of eye movement desensitization and reprocessing – a multicentre pilot trial. Eur J Psychotraumatol. 2018;9:1512248.
- Novo Navarro P, Landin-Romero R, Guardiola-Wanden-Berghe R, Moreno-Alcázar A, Valiente-Gómez A, Lupo W, et al. 25 years of Eye Movement Desensitization and Reprocessing (EMDR): The EMDR therapy protocol, hypotheses of its mechanism of action and a systematic review of its efficacy in the treatment of post-traumatic stress disorder. Rev Psiquiatr Salud Ment (Engl Ed). 2018;11:101–14.
- Schubert SJ, Lee CW, Drummond PD. The efficacy and psychophysiological correlates of dual-attention tasks in eye movement desensitization and reprocessing (EMDR). J Anxiety Disord. 2011;25:1–11.
- Agren T. Human reconsolidation: A reactivation and update. Brain Research Bulletin. 2014;105:70–82.
- LeDoux JE. Consolidation: challenging the traditional view. In: Dudai Y, Roediger HL, Fitzpatrick SM, editors. Science of Memory: Concepts. London ; New York: Oxford University Press; 2007. p. 171–5.
- van den Hout MA, Engelhard IM. How does EMDR work? Journal of Experimental Psychopathology. 2012;3:724–38.
- Propper RE, Christman SD. Interhemispheric interaction and saccadic horizontal eye movements: Implications for episodic memory, EMDR, and PTSD. Journal of EMDR Practice and Research. 2008;2:269–81.
- Armstrong MS, Vaughan K. An orienting response model of eye movement desensitization. J Behav Ther Exp Psychiatry. 1996;27:21–32.
- Chamberlin DE. The Predictive Processing Model of EMDR. Frontiers in Psychology. 2019;10:2267.
- Sinclair AH, Manalili GM, Brunec IK, Adcock RA, Barense MD. Prediction errors disrupt hippocampal representations and update episodic memories. Proceedings of the National Academy of Sciences. 2021;118:e2117625118.
- Sevenster D, Beckers T, Kindt M. Prediction error demarcates the transition from retrieval, to reconsolidation, to new learning. Learn Mem. 2014;21:580–4.
- Hoff M, Schaefer L, Heinke N, Bittmann F. Report on Adaptive Force, A Specific Neuromuscular Function. Eur J Transl Myol. 2015;25:5183.
- Bittmann FN, Dech S, Schaefer LV. Another Way to Confuse Motor Control: Manual Technique Supposed to Shorten Muscle Spindles Reduces the Muscular Holding Stability in the Sense of Adaptive Force in Male Soccer Players. Brain Sciences. 2023;13:1105.
- Schaefer LV, Dech S, Aehle M, Bittmann FN. Disgusting odours affect the characteristics of the Adaptive Force in contrast to neutral and pleasant odours. Scientific Reports. 2021;11:1–16.
- Schaefer LV, Bittmann FN. Are there two forms of isometric muscle action? Results of the experimental study support a distinction between a holding and a pushing isometric muscle function. BMC Sports Sci Med Rehabil. 2017;9:11.
- Schaefer LV, Carnarius F, Dech S, Bittmann FN. Repeated measurements of Adaptive Force: Maximal holding capacity differs from other maximal strength parameters and preliminary characteristics for non-professional strength vs. endurance athletes. Front Physiol. 2023;14:1020954.
- Bittmann FN, Dech S, Aehle M, Schaefer LV. Manual Muscle Testing—Force Profiles and Their Reproducibility. Diagnostics. 2020;10.
- Courtemanche R, Robinson JC, Aponte DI. Linking oscillations in cerebellar circuits. Front Neural Circuits. 2013;7.
- D’Angelo E, Koekkoek SKE, Lombardo P, Solinas S, Ros E, Garrido J, et al. Timing in the cerebellum: oscillations and resonance in the granular layer. Neuroscience. 2009;162:805–15.
- McAuley JH, Marsden CD. Physiological and pathological tremors and rhythmic central motor control. Brain. 2000;123 ( Pt 8):1545–67.
- Schaefer LV, Bittmann FN. Two forms of isometric muscle function: Interpersonal motor task supports a distinction between a holding and a pushing isometric muscle action. 2020;:2020.08.17.253633.
- Schaefer LV, Dech S, Bittmann FN. Adaptive Force and emotionally related imaginations – preliminary results suggest a reduction of the maximal holding capacity as reaction to disgusting food imagination. Heliyon. 2021;7:e07827.
- Lobo I, Campagnoli RR, Figueira JS, Andrade I, Figueira I, Gama C, et al. Hidden wounds of violence: Abnormal motor oscillatory brain activity is related to posttraumatic stress symptoms. NeuroImage. 2021;224:117404.
- Bohannon RW. Reliability of manual muscle testing: A systematic review. Isokinetics and Exercise Science. 2018;26:245–52.
- Conable K, Corneal J, Hambrick T, Marquina N, Zhang J. Investigation of Methods and Styles of Manual Muscle Testing by AK Practitioners. J Chiropr Med. 2005;4:1–10.
- Bohannon RW. Make tests and break tests of elbow flexor muscle strength. Phys Ther. 1988;68:193–4.
- Schmitt W, Cuthbert S. Common errors and clinical guidelines for manual muscle testing: Chiropractic & Manual Therapies. 2008;16:16.
- Stratford PW, Balsor BE. A comparison of make and break tests using a hand-held dynamometer and the Kin-Com. J Orthop Sports Phys Ther. 1994;19:28–32.
- Van der Ploeg RJ, Oosterhuis HJ. The" make/break test" as a diagnostic tool in functional weakness. Journal of Neurology, Neurosurgery & Psychiatry. 1991;54:248–51.
- Caruso W, Leisman G. A Force/Displacement Analysis of Muscle Testing. Perceptual and Motor Skills. 2000;91:683–92.
- Radák Z. Chapter 2 - Skeletal Muscle, Function, and Muscle Fiber Types. In: Radák Z, editor. The Physiology of Physical Training. Academic Press; 2018. p. 15–31.
- Roberts TJ, Azizi E. The series-elastic shock absorber: tendons attenuate muscle power during eccentric actions. J Appl Physiol (1985). 2010;109:396–404.
- Macefield VG, Knellwolf TP. Functional properties of human muscle spindles. Journal of Neurophysiology. 2018;120:452–67.
- Conable KM. Intraexaminer comparison of applied kinesiology manual muscle testing of varying durations: a pilot study. Journal of Chiropractic Medicine. 2010;9:3–10.
- Caruso W, Leisman G. The clinical utility of force/displacement analysis of muscle testing in applied kinesiology. International journal of neuroscience. 2001;106:147–57.
- Nguyen TV, Hsu C-Y, Jaiswal S, Muggleton NG, Liang W-K, Juan C-H. To Go or Not to Go: Degrees of Dynamic Inhibitory Control Revealed by the Function of Grip Force and Early Electrophysiological Indices. Front Hum Neurosci. 2021;15.
- Mayr S, Buchner A, Dentale S. Prime retrieval of motor responses in negative priming. Journal of Experimental Psychology: Human Perception and Performance. 2009;35:408.
- Praamstra P, Seiss E. The neurophysiology of response competition: motor cortex activation and inhibition following subliminal response priming. J Cogn Neurosci. 2005;17:483–93.
- Klaassen FH, Held L, Figner B, O’Reilly JX, Klumpers F, de Voogd LD, et al. Defensive freezing and its relation to approach–avoidance decision-making under threat. Sci Rep. 2021;11:12030.
- Riskind JH, Sagliano L, Trojano L, Conson M. Dysfunctional Freezing Responses to Approaching Stimuli in Persons with a Looming Cognitive Style for Physical Threats. Front Psychol. 2016;7.
- Gangemi SC. A newly discovered muscle-organ relationship: the pectoralis minor and the parotid gland. Collected Papers International College of Applied Kinesiology. 2006;2005–2006:75–7.
- Hoffman J, Mendel R, Carpenter. Evaluation of Muscle-Organ Association, Part II. J Clin Chiro. 1977;III:42–60.
- Pollard HP, Bablis P, Bonello R, others. Commentary: The Ileocecal valve point and muscle testing: A possible mechanism of action. Chiropractic Journal of Australia. 2006;36:122.
- Iravani B, Schaefer M, Wilson DA, Arshamian A, Lundström JN. The human olfactory bulb processes odor valence representation and cues motor avoidance behavior. Proc Natl Acad Sci U S A. 2021;118:e2101209118.
- Price RS, Maples WC. Physiological Effects of Low-Plus Lenses: Manual Muscle Testing and Nearpoint Lens Prescription. 2005;36:93. https://cdn.ymaws.com/www.covd.org/resource/resmgr/ovd36/93_98_PriceMaples.pdf. Accessed 21 Jan 2025.
- Nicholas JA, Melvin M, Saraniti AJ. Neurophysiologic inhibition of strength following tactile stimulation of the skin. Am J Sports Med. 1980;8:181–6.
- Levinsson A, Holmberg H, Broman J, Zhang M, Schouenborg J. Spinal Sensorimotor Transformation: Relation between Cutaneous Somatotopy and a Reflex Network. J Neurosci. 2002;22:8170–82.
- Fallon JB, Bent LR, McNulty PA, Macefield VG. Evidence for strong synaptic coupling between single tactile afferents from the sole of the foot and motoneurons supplying leg muscles. J Neurophysiol. 2005;94:3795–804.
- Monti DA, Sinnott J, Marchese M, Kunkel EJ, Greeson JM. Muscle test comparisons of congruent and incongruent self-referential statements. Perceptual and Motor Skills. 1999;88:1019–28.
- Rice DA, McNair PJ, Lewis GN. Mechanisms of quadriceps muscle weakness in knee joint osteoarthritis: the effects of prolonged vibration on torque and muscle activation in osteoarthritic and healthy control subjects. Arthritis Res Ther. 2011;13:R151.
- Jensen AM. Estimating the prevalence of use of kinesiology-style manual muscle testing: A survey of educators. Advances in Integrative Medicine. 2015;2:96–102.
- Beardall AG. Clinical Kinesiology, Vols. I, II, III, IV, V. Beardall, DC. Inc., Lake Oswego, OR; 1980.
- Buhler CF, Williams S. Muscles of the neck. 2013.
- Weissfeld RK. Mind, trauma & muscle inhibition Part II: When muscle inhibition is not ignored. Evidence of effectiveness from the NBA. Asia-Pacific Chiropractic Journal. 2021;2.
- Wilczynski M. 20-Year History of Missed Games in the NBA. Weak Side Awareness. 2011. https://weaksideawareness.wordpress.com/2011/11/28/20-year-history-of-missed-games-in-the-nba/. Accessed 14 Feb 2020.
- Buckley T. Battle on Wounded Knee Doctors are in awe, teammates are amazed, yet Hornacek insists he’s just doing his job. Deseret News. 2000. https://www.deseret.com/2000/4/21/19557822/jeff-hornacek-battle-on-wounded-knee. Accessed 12 Feb 2020.
- Dorausch M. NBA Star John Stockton Attributes Longevity to Team Chiropractor. 2002. http://www.planetc1.com/cgi-bin/n/v.cgi?id=1018295924. Accessed 17 Feb 2018.
- Jarvis, Kelly B. Chiropractic and all that Jazz. Dynamic Chiropractic. 1998;16.
- Franklin DW, Wolpert DM. Computational Mechanisms of Sensorimotor Control. Neuron. 2011;72:425–42.
- Welling H. Transformative emotional sequence: Towards a common principle of change. Journal of Psychotherapy Integration. 2012;22:109.
- Assouline A, Mendelsohn A, Reshef A. Memory-directed acupuncture as a neuromodulatory treatment for PTSD: Theory, clinical model and case studies. Transl Psychiatry. 2022;12:1–9.
- Clinical Kinesiology. Studio Version of the Muscle Testing Series by Dr. Alan G. Beardall, DC. Clinical Kinesiology. https://www.clinicalkinesiology.com/collections/studio-version-of-the-muscle-testing-series-by-dr-alan-g-beardall-dc-3-part-series-in-color. Accessed 13 Feb 2023.
- Buhler C, Williams S. Amit Seminars. https://www.amitseminars.com/. Accessed 19 May 2025.
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



