Submitted:
15 June 2025
Posted:
17 June 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Subjects and Methods
2.1. Research Design
2.2. Study Participants
2.3. Minimal Sample Size Calculation
2.4. Measurement Tools
2.4.1. BMI
2.4.2. CRP
2.4.3. Family Support Scale (FSS)
2.5. Statistical Analysis
3. Results
3.1. General Characteristics of Participants and Scores on Outcome Variables
3.2. Correlations Among Continues Variables
3.3. Binary Logistic Regression Analysis Analyses
3.4. Moderated Binary Logistic Regression Analysis
4. Discussion
4. Conclusion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Khandaker, G.M.; Cousins, L.; Deakin, J.; Lennox, B.R.; Yolken, R.; Jones, P.B. (2015). Inflammation and immunity in schizophrenia: Implications for pathophysiology and treatment. Lancet Psychiatry 2, 258–270. [CrossRef]
- Müller, N.; Weidinger, E.; Leitner, B.; Schwarz, M.J. (2015) The role of inflammation in schizophrenia. Front. Neurosci. 9:372. [CrossRef]
- Sun, H.-L.; Bai, W.; Li, X.-H.; Huang, H.; Cui, X.-L.; Cheung, T.; Su, Z.-H.; Yuan, Z.; Ng, C.H.; Xiang, Y.-T. (2022). Schizophrenia and Inflammation Research: A Bibliometric Analysis. Front. Immunol. 13:907851. [CrossRef]
- Fond, G.; Lançon, C.; Auquier, P.; Boyer, L. (2018) C-Reactive Protein as a Peripheral Biomarker in Schizophrenia. An Updated Systematic Review. Front. Psychiatry, 9, 392. [CrossRef]
- Ullah, I.; Awan, H.A.; Aamir, A.; Diwan, M.N.; de Filippis, R.; Awan, S.; Irfan, M.; Fornaro, M.; Ventriglio, A.; Vellante, F.; Pettorruso, M.; Martinotti, G.; Di Giannantonio, M.; De Berardis, D. Role and Perspectives of Inflammation and C-Reactive Protein (CRP) in Psychosis: An Economic and Widespread Tool for Assessing the Disease. Int J Mol Sci. 2021 Dec 2;22(23):13032. [CrossRef]
- Moshage, H.J.; Roelofs, H.M.J.; van Pelt, J.F.; Hazenberg, B.P.C.; van Leeuwen, M.A.; Limburg, P.C.; Aarden, L.A.; Yap, S.H. (1988). The effect of interleukin-1, interleukin-6 and its interrelationship on the synthesis of serum amyloid A and C-reactive protein in primary cultures of adult human hepatocytes. Biochem. Biophys. Res. Commun. 155, 112–117. [CrossRef]
- Miller, B.J.; Culpepper, N.; Rapaport, M.H. C-reactive protein levels in schizophrenia: a review and meta-analysis. Clin Schizophr Relat Psychoses. 2014 Jan;7(4):223-30. [CrossRef] [PubMed]
- Fernandes, B.S.; et al. C-reactive protein is increased in schizophrenia but is not altered by antipsychotics: meta-analysis and implications. Mol Psychiatry. [CrossRef]
- Lestra, V.; Romeo, B.; Martelli, C.; Benyamina, A.; Hamdani, N. Could CRP be a differential biomarker of illness stages in schizophrenia? A systematic review and meta-analysis. Schizophr Res. 2022 Aug;246:175-186. [CrossRef] [PubMed]
- Metcalf, S.A.; Jones, P.B.; Nordstrom, T.; Timonen, M.; Mäki, P.; Miettunen, J.; Jääskeläinen, E.; Järvelin, M.R.; Stochl, J.; Murray, G.K.; Veijola, J.; Khandaker, G.M. Serum C-reactive protein in adolescence and risk of schizophrenia in adulthood: A prospective birth cohort study. Brain Behav Immun. 2017 Jan;59:253-259. [CrossRef] [PubMed] [PubMed Central]
- Osimo, E.F.; Baxter, L.; Stochl, J.; et al. Longitudinal association between CRP levels and risk of psychosis: a meta-analysis of population-based cohort studies. npj Schizophr 7, 31 (2021). [CrossRef]
- Hartwig, F.P.; Borges, M.C.; Horta, B.L.; Bowden, J.; Davey Smith, G. Inflammatory biomarkers and risk of schizophrenia: a 2-sample Mendelian randomization study. JAMA Psychiatry 2017;74: 1226–233. [CrossRef]
- Ligthart, S.; Vaez, A.; Vosa, U.; et al. Genome analyses of >200,000 individuals identify 58 loci for chronic inflammation and highlight pathways that link inflammation and complex disorders. Am J Hum Genet 2018;103:691–706. [CrossRef]
- Said, S.; Pazoki, R.; Karhunen, V.; Võsa, U.; Ligthart, S.; Bodinier, B.; Koskeridis, F.; Welsh, P.; Alizadeh, B.Z.; Chasman, D.I.; Sattar, N.; Chadeau-Hyam, M.; Evangelou, E.; Jarvelin, M.-R.; Elliott, P.; Tzoulaki, I.; Dehghan, A. 2022. Genetic analysis of over half a million people characterises C-reactive protein loci. Nat. Commun 13, 2198. [CrossRef]
- Gardner, R.M.; Dalman, C.; Wicks, S.; Lee, B.K.; Karlsson, H. Neonatal levels of acute phase proteins and later risk of non-affective psychosis. Transl. Psychiatry 3, e228. [CrossRef]
- Blomström, Å.; Gardner, R.; Dalman, C.; et al. Influence of maternal infections on neonatal acute phase proteins and their interaction in the development of non-affective psychosis. Transl Psychiatry 5, e502 (2015). [CrossRef]
- Ligthart, S. Commentary: CRP and schizophrenia: cause, consequence or confounding? Int J Epidemiol. 2019 Oct 1;48(5):1514-1515. [CrossRef] [PubMed]
- Jacomb, I.; Stanton, C.; Vasudevan, R.; Powell, H.; O’Donnell, M.; Lenroot, R.; Bruggemann, J.; Balzan, R.; Galletly, C.; Liu, D.; Weickert, C.S.; Weickert, T.W. (2018) C-Reactive Protein: Higher During Acute Psychotic Episodes and Related to Cortical Thickness in Schizophrenia and Healthy Controls. Front. Immunol. 9:2230. [CrossRef]
- Johnsen, E.; Fathian, F.; Korken, R.; Steen, V.; Jorgensen, H.; Gjestad, R.; et al. The serum level of C-reactive protein (CRP) is associated with cognitive performance in acute phase psychosis. BMC Psychiatry (2016) 16:1–11. [CrossRef]
- Fan, X.; Pristach, C.; Liu, E.Y.; Freudenreich, O.; Henderson, D.C.; Goff, D.C. Elevated serum levels of C-reactive protein are associated with more severe psychopathology in a subgroup of patients with schizophrenia. Psychiatry Res. (2007) 149:267–71. [CrossRef]
- Orsolini L, Sarchione F, Vellante F, Fornaro M, Matarazzo I, Martinotti G, Valchera A, Di Nicola M, Carano A, Di Giannantonio M, Perna G, Olivieri L, De Berardis D. Protein-C Reactive as Biomarker Predictor of Schizophrenia Phases of Illness? A Systematic Review. Curr Neuropharmacol. 2018;16(5):583-606. [CrossRef] [PubMed] [PubMed Central]
- Challa, F.; Seifu, D.; Sileshi, M.; Getahun, T.; Geto, Z.; Kassa, D.; Alemayehu, M.; Mesfin, M.; Fekadu, A.; Woldeamanuel, Y. Serum level of high sensitive C-reactive protein and IL - 6 markers in patients with treatment-resistant schizophrenia in Ethiopia: a comparative study. BMC Psychiatry. 2021 Aug 31;21(1):428. [CrossRef] [PubMed] [PubMed Central]
- Fawzi, M.H.; Fawzi, M.M.; Fawzi, M.M.; Said, N.S. C-reactive protein serum level in drug-free male Egyptian patients with schizophrenia. Psychiatry Res 190, 91–97 (2011). [CrossRef]
- Dimitrov, Dimitre H., Shuko Lee, Jesse Yantis, Craig Honaker, Nicole Braida, et Consuelo Walss-Bass. 2016. « Elevated Serum Levels of High-Sensitivity C-Reactive Proteins Are Associated with Severe Delusional Symptoms in a Subgroup of Patients with Schizophrenia ». The Journal of Clinical Psychiatry 77 (1): 131-32. [CrossRef]
- Garcia-Rizo, C.; Fernandez-Egea, E.; Oliveira, C.; Justicia, A.; Bernardo, M.; Kirkpatrick, B. Inflammatory markers in antipsychotic-naïve patients with nonaffective psychosis and deficit vs. nondeficit features. Psychiatry Res. 2012 Jul 30;198(2):212-5. Epub 2012 Mar 8. Erratum in: Psychiatry Res. 2013 Dec 30;210(3):1329. [CrossRef] [PubMed]
- Boozalis, Ted, Antonio L. Teixeira, Raymond Young-Jin Cho, et Olaoluwa Okusaga. 2017. « C-Reactive Protein Correlates with Negative Symptoms in Patients with Schizophrenia ». Frontiers in Public Health 5: 360. [CrossRef]
- Bulzacka, E.; Boyer, L.; Schurhoff, F.; Godin, O.; Berna, F.; Brunel, L.; et al. Chronic peripheral inflammation is associated with cognitive impairment in schizophrenia: results from the multicentric FACE-SZ dataset. Schizophr Bull. (2016) 42:1290–302. [CrossRef]
- Boozalis, Ted, Sridevi Devaraj, Olaoluwa O. Okusaga. 2019. « Correlations between Body Mass Index, Plasma High-Sensitivity C-Reactive Protein and Lipids in Patients with Schizophrenia ». The Psychiatric Quarterly 90 (1): 101-10. [CrossRef]
- Annamalai, A.; Kosir, U.; Tek, C. Prevalence of obesity and diabetes in patients with schizophrenia. World J Diabetes. 2017 Aug 15;8(8):390-396. [CrossRef] [PubMed] [PubMed Central]
- Cordes, J.; Bechdolf, A.; Engelke, C.; Kahl, K.G.; Balijepalli, C.; Lösch, C.; Klosterkötter, J.; Wagner, M.; Maier, W.; Heinz, A.; de Millas, W.; Gaebel, W.; Winterer, G.; Janssen, B.; Schmidt-Kraepelin, C.; Schneider, F.; Lambert, M.; Juckel, G.; Wobrock, T.; Riedel, M.; Moebus, S. Prevalence of metabolic syndrome in female and male patients at risk of psychosis. Schizophr Res. 2017 Mar;181:38-42. [CrossRef]
- Jeong, S.H.; Lee, N.Y.; Kim, S.H.; Chung, I.W.; Youn, T.; Kang, U.G.; et al. Long-term evolution of metabolic status in patients with schizophrenia stably maintained on second-generation antipsychotics. Psychiatry Investig. 2018;15:628–37. [CrossRef]
- Sugawara, N.; Yasui-Furukori, N.; Yamazaki, M.; Shimoda, K.; Mori, T.; Sugai, T.; Matsuda, H.; Suzuki, Y.; Ozeki, Y.; Okamoto, K.; Sagae, T.; Someya, T. Predictive Utility of Body Mass Index for Metabolic Syndrome Among Patients with Schizophrenia in Japan. Neuropsychiatr Dis Treat. 2020 Sep 30;16:2229-2236. [CrossRef]
- Liang, J.; Cai, Y.; Xue, X.; Li, X.; Li, Z.; Xu, C.; Xie, G.; Yu, Y. (2022) Does Schizophrenia Itself Cause Obesity? Front. Psychiatry 13:934384. [CrossRef]
- Chouinard, V.A.; Pingali, S.M.; Chouinard, G.; Henderson, D.C.; Mallya, S.G.; Cypess, A.M.; Cohen, B.M.; Öngür, D. Factors associated with overweight and obesity in schizophrenia, schizoaffective and bipolar disorders. Psychiatry Res. 2016 Mar 30;237:304-10. [CrossRef]
- Limosin, F.; Gasquet, I.; Leguay, D.; Azorin, J.M.; Rouillon, F. (2008). Body mass index and prevalence of obesity in a French cohort of patients with schizophrenia. Acta psychiatrica Scandinavica, 118(1), 19–25. [CrossRef]
- Allison, D.B.; Casey, D.E. Antipsychotic-induced weight gain: a review of the literature. J Clin Psychiatry. 2001;62 Suppl 7:22-31. [PubMed]
- Aoki, R.; Saito, T.; Ninomiya, K.; Shimasaki, A.; Ashizawa, T.; Ito, K.; Ikeda, M.; Iwata, N. Shared genetic components between metabolic syndrome and schizophrenia: Genetic correlation using multipopulation data sets. [CrossRef] [PubMed] [PubMed Central]
- Sørensen, H.J.; Gamborg, M.; Sørensen, T.I.A.; Baker, J.L.; Mortensen, E.L. Childhood body mass index and risk of schizophrenia in relation to childhood age, sex and age of first contact with schizophrenia. Eur Psychiatry. 2016 Apr;34:64-69. [CrossRef]
- Cameron, I.M.; Hamilton, R.J.; Fernie, G.; MacGillivray, S.A. Obesity in individuals with schizophrenia: a case controlled study in Scotland. BJPsych Open. 2017 Oct 17;3(5):254-256. [CrossRef]
- Zeng, M.; Wang, X.; Zhou, J.; Zhang, X.; Zhang, X.; Chi, J.; Lu, C.; Wang, L.; Li, S. Body mass index-specific metabolic profiles in schizophrenia: implications for cognitive dysfunction and psychopathology. J Neural Transm (Vienna). 2025 May 24. [CrossRef]
- Xiao, P.; Li, C.; Mi, J.; Wu, J. Evaluating the distinct effects of body mass index at childhood and adulthood on adult major psychiatric disorders. Sci Adv. 2024 Sep 13;10(37):eadq2452. [CrossRef] [PubMed]
- Choi, J.; Joseph, L.; Pilote, L. Obesity and C-reactive protein in various populations: a systematic review and meta-analysis. Obes Rev. 2013 Mar;14(3):232-44. [CrossRef]
- Timpson, N.J.; Nordestgaard, B.G.; Harbord, R.M.; Zacho, J.; Frayling, T.M.; Tybjærg-Hansen, A.; Smith, G.D. C-reactive protein levels and body mass index: elucidating direction of causation through reciprocal Mendelian randomization. Int J Obes (Lond). 2011 Feb;35(2):300-8. [CrossRef]
- Xu, H.; Barnes, G.T.; Yang, Q.; Tan, G.; Yang, D.; Chou, C.J.; et al. Chronic inflammation in fat plays a crucial role in the development of obesity-related insulin resistance. J Clin Invest (2003) 112(12):1821–30. [CrossRef]
- Kawai, T.; Autieri, M.V.; Scalia, R. Adipose tissue inflammation and metabolic dysfunction in obesity. Am J Physiol Cell Physiol (2021) 320(3):C375–c391. [CrossRef]
- Visser, M.; Bouter, L.M.; McQuillan, G.M.; Wener, M.H.; Harris, T.B. (1999). Elevated C-reactive protein levels in overweight and obese adults. JAMA 282, 2131–2135. [CrossRef]
- Wellen, K.E.; Hotamisligil, G.S. (2003). Obesity-induced inflammatory changes in adipose tissue. J. Clin. Invest. 112, 1785–1788. [CrossRef]
- Welsh, P.; Polisecki, E.; Robertson, M.; Jahn, S.; Buckley, B.M.; de Craen, A.J.; Ford, I.; Jukema, J.W.; Macfarlane, P.W.; Packard, C.J.; Stott, D.J.; Westendorp, R.G.; Shepherd, J.; Hingorani, A.D.; Smith, G.D.; Schaefer, E.; Sattar, N. Unraveling the directional link between adiposity and inflammation: a bidirectional Mendelian randomization approach. J Clin Endocrinol Metab. 2010 Jan;95(1):93-9. [CrossRef]
- Joseph, J.; Depp, C.; Martin, A.S.; Daly, R.E.; Glorioso, D.K.; Palmer, B.W.; Jeste, D.V. Associations of high sensitivity C-reactive protein levels in schizophrenia and comparison groups. Schizophr Res. 2015 Oct;168(1-2):456-60. [CrossRef]
- Van Dyne, A.; Wu, T.C.; Adamowicz, D.H.; Lee, E.E.; Tu, X.M.; Eyler, L.T. Longitudinal relationships between BMI and hs-CRP among people with schizophrenia. Schizophr Res. 2024 Sep;271:337-344. [CrossRef]
- McWhinney, S.R.; Brosch, K.; Calhoun, V.D.; Crespo-Facorro, B.; Crossley, N.A.; Dannlowski, U.; Dickie, E.; Dietze, L.M.F.; Donohoe, G.; Du Plessis, S.; Ehrlich, S.; Emsley, R.; Furstova, P.; Glahn, D.C.; Gonzalez-Valderrama, A.; Grotegerd, D.; Holleran, L.; Kircher, T.T.J.; Knytl, P.; Kolenic, M.; Lencer, R.; Nenadić, I.; Opel, N.; Pfarr, J.K.; Rodrigue, A.L.; Rootes-Murdy, K.; Ross, A.J.; Sim, K.; Škoch, A.; Spaniel, F.; Stein, F.; Švancer, P.; Tordesillas-Gutiérrez, D.; Undurraga, J.; Vázquez-Bourgon, J.; Voineskos, A.; Walton, E.; Weickert, T.W.; Weickert, C.S.; Thompson, P.M.; van Erp, T.G.M.; Turner, J.A.; Hajek, T. Obesity and brain structure in schizophrenia - ENIGMA study in 3021 individuals. Mol Psychiatry. 2022 Sep;27(9):3731-3737. Epub 2022 Jun 14. Erratum in: Mol Psychiatry. 2022 Sep;27(9):3738. doi: 10.1038/s41380-022-01696-3. Erratum in: Mol Psychiatry. 2024 Jan;29(1):56. [CrossRef]
- Nettis, M.A.; Pergola, G.; Kolliakou, A.; O'Connor, J.; Bonaccorso, S.; David, A.; Gaughran, F.; Di Forti, M.; Murray, R.M.; Marques, T.R.; Blasi, G.; Bertolino, A.; Pariante, C.M.; Dazzan, P.; Mondelli, V. Metabolic-inflammatory status as predictor of clinical outcome at 1-year follow-up in patients with first episode psychosis. Psychoneuroendocrinology. 2019 Jan;99:145-153. [CrossRef]
- Crump, C.; Winkleby, M.A.; Sundquist, K.; Sundquist, J. 2013. Comorbidities and mortality in persons with schizophrenia: a Swedish national cohort study. Am. J. Psychiatry 170(3),324–333. [CrossRef]
- Ratliff, J.C.; Palmese, L.B.; Reutenauer, E.L.; Srihari, V.H.; Tek, C. Obese schizophrenia spectrum patients have significantly higher 10-year general cardiovascular risk and vascular ages than obese individuals without severe mental illness. Psychosomatics. 2013 Jan-Feb;54(1):67-73. [CrossRef]
- Tsai, K.Y.; Lee, C.C.; Chou, Y.M.; Su, C.Y.; Chou, F.H. The incidence and relative risk of stroke in patients with schizophrenia: a five-year follow-up study. Schizophr Res. 2012 Jun;138(1):41-7. [CrossRef] [PubMed]
- Laursen, T.M.; Munk-Olsen, T.; Vestergaard, M. 2012. Life expectancy and cardio-vascular mortality in persons with schizophrenia. Curr.Opin.Psychiatry 25(2), 83–88. [CrossRef]
- Radhakrishnan, R.; Kaser, M.; Guloksuz, S. The Link Between the Immune System, Environment, and Psychosis. Schizophr Bull. 2017 Jul 1;43(4):693-697. [CrossRef]
- Mongan, D.; Ramesar, M.; Föcking, M.; Cannon, M.; Cotter, D. Role of inflammation in the pathogenesis of schizophrenia: A review of the evidence, proposed mechanisms and implications for treatment. Early Interv Psychiatry. 2020 Aug;14(4):385-397. [CrossRef]
- Miller, B.J.; Goldsmith, D.R. Evaluating the Hypothesis That Schizophrenia Is an Inflammatory Disorder. Focus (Am Psychiatr Publ). 2020 Oct;18(4):391-401. [CrossRef]
- Uchino, B.N. Social support and health: a review of physiological processes potentially underlying links to disease outcomes. J Behav Med. 2006 Aug;29(4):377-87. [CrossRef]
- McHugh Power, J.; Carney, S.; Hannigan, C.; Brennan, S.; Wolfe, H.; Lynch, M.; Kee, F.; Lawlor, B. Systemic inflammatory markers and sources of social support among older adults in the Memory Research Unit cohort. J Health Psychol. 2019 Mar;24(3):397-406. [CrossRef]
- Kiecolt-Glaser, J.K.; Gouin, J.P.; Hantsoo, L. Close relationships, inflammation, and health. Neurosci Biobehav Rev. 2010 Sep;35(1):33-8. [CrossRef]
- Hsiao, C.Y.; Lee, C.T.; Lu, H.L.; Tsai, Y.F. Living with schizophrenia: Health-related quality of life among primary family caregivers. J Clin Nurs. 2017;26(23–24):5151–9. [CrossRef]
- Chronister, J.; Fitzgerald, S.; Chou, C.C. The meaning of social support for persons with serious mental illness: A family member perspective. Rehabil Psychol. 2021 Feb;66(1):87-101. [CrossRef]
- Mueser, K.T.; Deavers, F.; Penn, D.L.; Cassisi, J.E. Psychosocial treatments for schizophrenia. Annu Rev Clin Psychol. 2013;9:465-97. [CrossRef]
- Verbiest, I.; Michels, N.; Tanghe, A.; Braet, C. Inflammation in obese children and adolescents: Association with psychosocial stress variables and effects of a lifestyle intervention. Brain Behav Immun. 2021 Nov;98:40-47. [CrossRef]
- O'Brien, J.R.; Loi, E.C.; Byrne, M.L.; Zalewski, M.; Casement, M.D. The Link Between Positive and Negative Parenting Behaviors and Child Inflammation: A Systematic Review. Child Psychiatry Hum Dev. 2023 Feb;54(1):51-65. [CrossRef]
- Diener, M.J.; Geenen, R.; Koelen, J.A.; Aarts, F.; Gerdes, V.E.; Brandjes, D.P.; Hinnen, C. (2016). The significance of attachment quality for obesity: A meta-analytic review. Canadian Journal of Behavioural Science, 48(4), 255. [CrossRef]
- Bernard, K.; Hostinar, C.E.; Dozier, M. Longitudinal associations between attachment quality in infancy, C-reactive protein in early childhood, and BMI in middle childhood: preliminary evidence from a CPS-referred sample. Attach Hum Dev. 2019 Feb;21(1):5-22. [CrossRef]
- Aas, M.; Dieset, I.; Hope, S.; Hoseth, E.; Mørch, R.; Reponen, E.; Steen, N.E.; Laskemoen, J.F.; Ueland, T.; Aukrust, P.; Agartz, I.; Andreassen, O.A.; Melle, I. Childhood maltreatment severity is associated with elevated C-reactive protein and body mass index in adults with schizophrenia and bipolar diagnoses. Brain Behav Immun. 2017 Oct;65:342-349. [CrossRef]
- Peritogiannis, V.; Ninou, A.; Samakouri, M. Mortality in Schizophrenia-Spectrum Disorders: Recent Advances in Understanding and Management. Healthcare (Basel). 2022 Nov 25;10(12):2366. [CrossRef]
- Yung, N.C.L.; Wong, C.S.M.; Chan, J.K.N.; Chen, E.Y.H.; Chang, W.C. Excess Mortality and Life-Years Lost in People With Schizophrenia and Other Non-affective Psychoses: An 11-Year Population-Based Cohort Study. Schizophr Bull. 2021 Mar 16;47(2):474-484. [CrossRef]
- Sicras-Mainar, A.; Rejas-Gutiérrez, J.; Navarro-Artieda, R.; Blanca-Tamayo, M. C-reactive protein as a marker of cardiovascular disease in patients with a schizophrenia spectrum disorder treated in routine medical practice. Eur Psychiatry. 2013 Mar;28(3):161-7. [CrossRef]
- Kelly, C.; McEvoy, J.P.; Miller, B.J. Total and differential white blood cell counts, inflammatory markers, adipokines, and incident metabolic syndrome in phase 1 of the clinical antipsychotic trials of intervention effectiveness study, (Schizophr. Res. 209 (2019) 193–197. [CrossRef]
- Mori, N.; McEvoy, J.P.; Miller, B.J. Total and differential white blood cell counts, inflammatory markers, adipokines, and the metabolic syndrome in phase 1 of the clinical antipsychotic trials of intervention effectiveness study, (Schizophr. Res. 169 (2015) 30–76. [CrossRef]
- Boyer, L.; Richieri, R.; Dassa, D.; Boucekine, M.; Fernandez, J.; Vaillant, R.; Padovani, R.; Auquier, P.; Lancon, C. Association of metabolic syndrome and inflammation with neurocognition in patients with schizophrenia, (Psychiatry Res. 210 (2013) 381– 386. [CrossRef]
- Osimo, E.F.; Perry, B.I.; Cardinal, R.N.; Lynall, M.E.; Lewis, J.; Kudchadkar, A.; Murray, G.K.; Perez, J.; Jones, P.B.; Khandaker, G.M. Inflammatory and cardiometabolic markers at presentation with first episode psychosis and long-term clinical outcomes: A longitudinal study using electronic health records. Brain Behav Immun. 2021 Jan;91:117-127. [CrossRef]
- Sarandol, E.; Sarandol, A.; Mercan, S.; Eker, S.S.; Surmen-Gur, E. Antipsychotic-Treated Schizophrenia Patients Develop Inflammatory and Oxidative Responses Independently From Obesity: However, Metabolic Disturbances Arise From Schizophrenia-Related Obesity. Hum Psychopharmacol. 2024 Nov;39(6):e2913. [CrossRef]
- Solmi, F.; Mascarell, M.C.; Zammit, S.; Kirkbride, J.B.; Lewis, G. Polygenic risk for schizophrenia, disordered eating behaviours and body mass index in adolescents. Br J Psychiatry. 2019 Jul;215(1):428-433. [CrossRef]
- Khosravi, M. Biopsychosocial factors associated with disordered eating behaviors in schizophrenia. Ann Gen Psychiatry 19, 67 (2020). [CrossRef]
- Tuncer, G.Z.; Çetinkaya Duman, Z. An examination of emotional eating behavior in individuals with a severe mental disorder. Arch Psychiatr Nurs. 2020 Dec;34(6):531-536. [CrossRef]
- Kouidrat, Y.; Amad, A.; Stubbs, B.; Louhou, R.; Renard, N.; Diouf, M.; Lalau, J.D.; Loas, G. Disordered eating behaviors as a potential obesogenic factor in schizophrenia. Psychiatry Res. 2018 Nov;269:450-454. [CrossRef]
- Tsofliou, F.; Casey, C.; Hughes, C. (2023). Stress and Disordered Eating Patterns. In: Patel, V.B., Preedy, V.R. (eds) Eating Disorders. Springer, Cham. [CrossRef]
- Prabhakaran, S.; Nagarajan, P.; Varadharajan, N.; et al. Relationship Between Quality of Life and Social Support Among Patients with Schizophrenia and Bipolar Disorder: A Cross-Sectional Study. J. Psychosoc. Rehabil. Ment. Health 8, 137–145 (2021). [CrossRef]
- Ospina, L.H.; Beck-Felts, K.; Ifrah, C.; Shagalow, S.; Lister, A.; Russo, S.J.; Gross, J.J.; Kimhy, D. Relationships among inflammation, social cognition, and social functioning in schizophrenia. Schizophr Res. 2022 Oct;248:366-367. [CrossRef]
- Carpentier, A.; Zampetas, D.; Durand, A.; Naassila, M.; Bralet, M.C. Relationships Between Immune-Inflammatory Features and Social Cognitive Impairments in Patients With Schizophrenia Spectrum Disorders: A Systematic Review. Brain Behav. 2025 Apr;15(4):e70384. [CrossRef]
- Lal, C.; Ul Haq, M.S.; Jaleel, F.A.; Jawed, D.N. Correlation Between Social Support, Patient Satisfaction, and Associated Factors in Patients with Schizophrenia. Cureus. 2025 Mar 26;17(3):e81222. [CrossRef]
- Palumbo, C.; Volpe, U.; Matanov, A.; Priebe, S.; Giacco, D. Social networks of patients with psychosis: a systematic review. BMC Res Notes. 2015 Oct 12;8:560. [CrossRef]
- Kang, H. Sample size determination and power analysis using the G*Power software. J Educ Eval Health Prof. 2021;18:17. [CrossRef]
- Yenipınar, A.; Koç, Ş.; Çanga, D.; Kaya, F. (2019). Determining Sample Size in Logistic Regression with G-Power. Black Sea Journal of Engineering and Science, 2(1), 16-22.
- Pearson, T.A.; Mensah, G.A.; Alexander, R.W.; Anderson, J.L.; Cannon, R.O., 3rd; Criqui, M.; Fadl, Y.Y.; Fortmann, S.P.; Hong, Y.; Myers, G.L.; Rifai, N.; Smith SCJr Taubert, K.; Tracy, R.P.; Vinicor, F.; Centers for Disease Control and Prevention; American Heart Association. Markers of inflammation and cardiovascular disease: application to clinical and public health practice: A statement for healthcare professionals from the Centers for Disease Control and Prevention and the American Heart Association. Circulation. 2003 Jan 28;107(3):499-511. [CrossRef]
- Tselebis, A.; Anagnostopoulou, T.; Bratis, D.; Moulou, A.; Maria, A.; Sikaras, C.; Ilias, I.; Karkanias, A.; Moussas, G.; Tzanakis, N. The 13 item Family Support Scale: Reliability and validity of the Greek translation in a sample of Greek health care professionals. Asia Pac Fam Med. 2011 Apr 13;10(1):3. [CrossRef]
- Ilias, I.; Tselebis, A.; Theotoka, I.; Hatzimichelakis, E. Association of perceived family support through glycemic control in native Greek patients managing diabetes with diet alone. Ethn Dis. 2004 Winter;14(1):2. [PubMed]
- Tselebis, A.; Bratis, D.; Pachi, A.; Moussas, G.; Karkanias, A.; Harikiopoulou, M.; Theodorakopoulou, E.; Kosmas, E.; Ilias, I.; Siafakas, N.; Vgontzas, A.; Tzanakis, N. [Chronic obstructive pulmonary disease: sense of coherence and family support versus anxiety and depression]. Psychiatriki. 2013 Apr-Jun;24(2):109-16. Greek, Modern. [PubMed]
- Templeton, Gary F. (2011) "A Two-Step Approach for Transforming Continuous Variables to Normal: Implications and Recommendations for IS Research," Communications of the Association for Information Systems: Vol. 28, Article 4. Available online: http://aisel.aisnet.org/cais/vol28/iss1/4.
- Firdous, S. Correlation of CRP, fasting serum triglycerides and obesity as cardiovascular risk factors. J Coll Physicians Surg Pak. 2014 May;24(5):308-13. [PubMed]
- Wensveen, F.M.; Valentić, S.; Šestan, M.; Turk Wensveen, T.; Polić, B. The "Big Bang" in obese fat: Events initiating obesity-induced adipose tissue inflammation. Eur J Immunol. 2015 Sep;45(9):2446-56. [CrossRef]
- Festa, A.; D'Agostino, R., Jr.; Williams, K.; et al. The relation of body fat mass and distribution to markers of chronic inflammation. Int J Obes 25, 1407–1415 (2001). [CrossRef]
- Goldsmith, D.R.; Massa, N.; Miller, B.J.; Miller, A.H.; Duncan, E. The interaction of lipids and inflammatory markers predict negative symptom severity in patients with schizophrenia. NPJ Schizophr. 2021 Oct 20;7(1):50. [CrossRef]
- Park, H.S.; Park, J.Y.; Yu, R. Relationship of obesity and visceral adiposity with serum concentrations of CRP, TNF-alpha and IL-6. Diabetes Res. Clin. Pr. 69, 29–35 (2005). [CrossRef]
- Popa, C.; Netea, M.G.; van Riel, P.L.; van der Meer, J.W.; Stalenhoef, A.F. The role of TNF-alpha in chronic inflammatory conditions, intermediary metabolism, and cardiovascular risk. J. Lipid Res. 48, 751–762 (2007). [CrossRef]
- Correll, C.U.; Stanford, A.D.; Claxton, A.; Du, Y.; Weiden, P.J. (2018). Social and functional outcomes with two doses of aripiprazole lauroxil vs placebo in patients with schizophrenia: A post-hoc analysis of a 12-week phase 3 efficacy study. Psychiatry Research, 2019(274), 176–181. [CrossRef]
- El-Monshed, A.; Amr, M. Association between perceived social support and recovery among patients with schizophrenia, International Journal of Africa Nursing Sciences, Volume 13, 2020, 100236. [CrossRef]
- Cha, H.Y.; Yang, S.J.; Kim, S.W. Higher Dietary Inflammation in Patients with Schizophrenia: A Case-Control Study in Korea. Nutrients. 2021 Jun 13;13(6):2033. [CrossRef]
- Bigseth, T.T.; Engh, J.A.; Andersen, E.; Bang-Kittilsen, G.; Egeland, J.; Falk, R.S.; Holmen, T.L.; Mordal, J.; Nielsen, J.; Ueland, T.; Vang, T.; Fredriksen, M. Alterations in inflammatory markers after a 12-week exercise program in individuals with schizophrenia-a randomized controlled trial. Front Psychiatry. 2023 May 11;14:1175171. [CrossRef]
- Tang, P.Y.; Tee, S.F.; Su, K.P. Editorial: The link between nutrition and schizophrenia. Front Psychiatry. 2022 Nov 21;13:1074120. [CrossRef]
- Yang, Y.C.; Schorpp, K.; Harris, K.M. Social support, social strain and inflammation: evidence from a national longitudinal study of U.S. adults. Soc Sci Med. 2014 Apr;107:124-35. [CrossRef]
- Wee, C.C.; Mukamal, K.J.; Huang, A.; Davis, R.B.; McCarthy, E.P.; Mittleman, M.A. (2008). Obesity and C-reactive protein levels among white, black, and hispanic US adults. Obesity (Silver Spring, Md.), 16(4), 875–880. [CrossRef]
- Lear, S.A.; Chen, M.M.; Birmingham, C.L.; Frohlich, J.J. (2003). The relationship between simple anthropometric indices and C-reactive protein: ethnic and gender differences. Metabolism, 52(12), 1542-1546. [CrossRef]
- Fond, G.; Godin, O.; Llorca, P.M.; Leboyer, M. (2015). Abnormal C-reactive protein (CRP) levels in schizophrenia and schizoaffective disorders. Results from the FACE-SZ dataset. European Psychiatry, 30(S2), S112–S112. [CrossRef]
- Gough, M.; Godde, K. A multifaceted analysis of social stressors and chronic inflammation. SSM Popul Health. 2018 Sep 12;6:136-140. [CrossRef]
- Guevara, J.E.; Murdock, K.W. High social strain and physical health: Examining the roles of anxious arousal, body mass index, and inflammation. Psychoneuroendocrinology. 2019 Aug;106:155-160. [CrossRef]
- Uchino, B.N.; Trettevik, R.; Kent de Grey, R.G.; Cronan, S.; Hogan, J.; Baucom, B.R.W. Social support, social integration, and inflammatory cytokines: A meta-analysis. Health Psychol. 2018 May;37(5):462-471. [CrossRef]
- Lachman, M.E.; Schiloski, K.A. The psychosocial anti-inflammatories: Sense of control, purpose in life, and social support in relation to inflammation, functional health and chronic conditions in adulthood. J Psychosom Res. 2024 Dec;187:111957. [CrossRef]
- Misra, S.; Johnson, K.A.; Parnarouskis, L.M.; Koenen, K.C.; Williams, D.R.; Gelaye, B.; Borba, C.P.C. How Early Life Adversities Influence Later Life Family Interactions for Individuals with Schizophrenia in Outpatient Treatment: A Qualitative Analysis. Community Ment Health J. 2020 Aug;56(6):1188-1200. [CrossRef]
- Hurtado, M.M.; Villena, A.; Quemada, C.; Morales-Asencio, J.M. Personal relationships during and after an initial psychotic episode. First-person experiences. J Ment Health. 2024 Sep 28:1-7. [CrossRef]
- Fagundes, C.P.; Bennett, J.M.; Derry, H.M.; Kiecolt-Glaser, J.K. Relationships and Inflammation across the Lifespan: Social Developmental Pathways to Disease. Soc Personal Psychol Compass. 2011 Nov;5(11):891-903. [CrossRef]
- Aldersey, H.M.; Whitley, R. Family Influence in Recovery from Severe Mental Illness. Community Ment Health J 51, 467–476 (2015). [CrossRef]
- van de Vyver, M. Immunology of chronic low-grade inflammation: relationship with metabolic function. J Endocrinol. 2023 Feb 23;257(1):e220271. [CrossRef]
- Valdearcos, M.; Xu, A.W.; Koliwad, S.K. Hypothalamic inflammation in the control of metabolic function. Annu Rev Physiol. 2015;77:131-60. [CrossRef]
- Cani, P.D.; Amar, J.; Iglesias, M.A.; Poggi, M.; Knauf, C.; Bastelica, D.; Neyrinck, A.M.; Fava, F.; Tuohy, K.M.; Chabo, C.; Waget, A.; Delmée, E.; Cousin, B.; Sulpice, T.; Chamontin, B.; Ferrières, J.; Tanti, J.F.; Gibson, G.R.; Casteilla, L.; Delzenne, N.M.; Alessi, M.C.; Burcelin, R. Metabolic endotoxemia initiates obesity and insulin resistance. Diabetes. 2007 Jul;56(7):1761-72. [CrossRef]
- Khovidhunkit, W.; Kim, M.S.; Memon, R.A.; Shigenaga, J.K.; Moser, A.H.; Feingold, K.R.; Grunfeld, C. Effects of infection and inflammation on lipid and lipoprotein metabolism: mechanisms and consequences to the host. J Lipid Res. 2004 Jul;45(7):1169-96. [CrossRef]
- Huet, L.; Delgado, I.; Dexpert, S.; Sauvant, J.; Aouizerate, B.; Beau, C.; Forestier, D.; Ledaguenel, P.; Magne, E.; Capuron, L. Relationship between body mass index and neuropsychiatric symptoms: Evidence and inflammatory correlates. Brain Behav Immun. 2021 May;94:104-110. [CrossRef]
- Sugai, T.; Suzuki, Y.; Yamazaki, M.; Shimoda, K.; Mori, T.; Ozeki, Y.; Matsuda, H.; Sugawara, N.; Yasui-Furukori, N.; Minami, Y.; Okamoto, K.; Sagae, T.; Someya, T. High Prevalence of Obesity, Hypertension, Hyperlipidemia, and Diabetes Mellitus in Japanese Outpatients with Schizophrenia: A Nationwide Survey. PLoS One. 2016 Nov 17;11(11):e0166429. [CrossRef]
- Catapano, L.; Castle, D. (2004). Obesity in schizophrenia: what can be done about it?. Australasian psychiatry: bulletin of Royal Australian and New Zealand College of Psychiatrists, 12(1), 23–25. [CrossRef]
- Bobes, J. (2007). Schizophrenia and overweight/obesity: Pathophysiology and medical consequences. European Psychiatry, 22(S1), S94–S94. [CrossRef]
- Chen, J.; Perera, G.; Shetty, H.; Broadbent, M.; Xu, Y.; Stewart, R. Body mass index and mortality in patients with schizophrenia spectrum disorders: a cohort study in a South London catchment area: General Psychiatry 2022;35:e100819.
- Arango, C.; Bobes, J.; Kirkpatrick, B.; Garcia-Garcia, M.; Rejas, J. Psychopathology, coronary heart disease and metabolic syndrome in schizophrenia spectrum patients with deficit versus non-deficit schizophrenia: findings from the CLAMORS study. Eur Neuropsychopharmacol. 2011 Dec;21(12):867-75. [CrossRef]
- Palmese, L.B.; DeGeorge, P.C.; Ratliff, J.C.; Srihari, V.H.; Wexler, B.E.; Krystal, A.D.; Tek, C. Insomnia is frequent in schizophrenia and associated with night eating and obesity. Schizophr Res. 2011 Dec;133(1-3):238-43. [CrossRef]
- Kolotkin, R.L.; Corey-Lisle, P.K.; Crosby, R.D.; Swanson, J.M.; Tuomari, A.V.; L'italien, G.J.; Mitchell, J.E. Impact of obesity on health-related quality of life in schizophrenia and bipolar disorder. Obesity (Silver Spring). 2008 Apr;16(4):749-54. [CrossRef]
- Storch Jakobsen, A.; Speyer, H.; Nørgaard, H.C.B.; Hjorthøj, C.; Krogh, J.; Mors, O.; Nordentoft, M. Associations between clinical and psychosocial factors and metabolic and cardiovascular risk factors in overweight patients with schizophrenia spectrum disorders - Baseline and two-years findings from the CHANGE trial. Schizophr Res. 2018 Sep;199:96-102. [CrossRef]
- Yong, N.; Pan, J.; Li, X.; Yu, L.; Hou, X. Influencing factors of obesity in community patients with deficit schizophrenia: a cross-sectional study. Eur J Med Res. 2022 Jun 11;27(1):90. [CrossRef]
- Kim, M.; Yang, S.J.; Kim, H.H.; Jo, A.; Jhon, M.; Lee, J.Y.; Ryu, S.H.; Kim, J.M.; Kweon, Y.R.; Kim, S.W. Effects of Dietary Habits on General and Abdominal Obesity in Community-dwelling Patients with Schizophrenia. Clin Psychopharmacol Neurosci. 2023 Feb 28;21(1):68-76. [CrossRef]
- Lundgren, J.D.; Rempfer, M.V.; Brown, C.E.; Goetz, J.; Hamera, E. The prevalence of night eating syndrome and binge eating disorder among overweight and obese individuals with serious mental illness. Psychiatry Res. 2010 Feb 28;175(3):233-6. [CrossRef]
- Anzengruber, D.; Klump, K.L.; Thornton, L.; Brandt, H.; Crawford, S.; Fichter, M.M.; Halmi, K.A.; Johnson, C.; Kaplan, A.S.; LaVia, M.; Mitchell, J.; Strober, M.; Woodside, D.B.; Rotondo, A.; Berrettini, W.H.; Kaye, W.H.; Bulik, C.M. Smoking in eating disorders. Eat Behav. 2006 Nov;7(4):291-9. [CrossRef]
- García-Mayor, R.V.; García-Soidán, F.J. Eating disoders in type 2 diabetic people: Brief review. Diabetes Metab Syndr. 2017 Jul-Sep;11(3):221-224. [CrossRef]
- Sankaranarayanan, A.; Johnson, K.; Mammen, S.J.; Wilding, H.E.; Vasani, D.; Murali, V.; Mitchison, D.; Castle, D.J.; Hay, P. Disordered Eating among People with Schizophrenia Spectrum Disorders: A Systematic Review. Nutrients. 2021 Oct 27;13(11):3820. [CrossRef]
- Tselebis, A.; Pachi, A. Primary Mental Health Care in a New Era. Healthcare (Basel). 2022 Oct 14;10(10):2025. [CrossRef]
- Cooper SJ, Reynolds GP; With expert co-authors (in alphabetical order):; Barnes T, England E, Haddad PM, Heald A, Holt R, Lingford-Hughes A, Osborn D, McGowan O, Patel MX, Paton C, Reid P, Shiers D, Smith J. BAP guidelines on the management of weight gain, metabolic disturbances and cardiovascular risk associated with psychosis and antipsychotic drug treatment. J Psychopharmacol. 2016 Aug;30(8):717-48. [CrossRef]
- DeJongh, B.M. Clinical pearls for the monitoring and treatment of antipsychotic induced metabolic syndrome. Ment Health Clin. 2021 Nov 8;11(6):311-319. https://doi.org/10.9740/mhc.2021.11.311. [CrossRef]
- Fernández-Abascal, B.; Suárez-Pinilla, P.; Cobo-Corrales, C.; Crespo-Facorro, B.; Suárez-Pinilla, M. (2021). In- and outpatient lifestyle interventions on diet and exercise and their effect on physical and psychological health: a systematic review and meta-analysis of randomised controlled trials in patients with schizophrenia spectrum disorders and first episode of psychosis. Neuroscience and biobehavioral reviews, 125, 535–568. [CrossRef]
- Mucheru, D.; Hanlon, M.C.; McEvoy, M.; Thakkinstian, A.; MacDonald-Wicks, L. (2019). Comparative efficacy of lifestyle intervention strategies targeting weight outcomes in people with psychosis: a systematic review and network meta-analysis. JBI database of systematic reviews and implementation reports, 17(9), 1770–1825. [CrossRef]
- Fernández-Abascal, B.; Suárez-Pinilla, M.; Cobo-Corrales, C.; Crespo-Facorro, B.; Suárez-Pinilla, P. (2023). Lifestyle intervention based on exercise and behavioural counselling and its effect on physical and psychological health in outpatients with schizophrenia spectrum disorders. An exploratory, pragmatic randomized clinical trial. Schizophrenia research, 261, 256–268. [CrossRef]
- Naylor, A.; Flood, A.; Keegan, R. (2024). The effectiveness of physical activity interventions that include both physical activity and psychosocial strategies in people living with a severe mental illness: a systematic review and meta-analysis. International Review of Sport and Exercise Psychology, 1–31. [CrossRef]
- Hahlweg, K.; Baucom, D.H. (2023). Family therapy for persons with schizophrenia: neglected yet important. European archives of psychiatry and clinical neuroscience, 273(4), 819–824. [CrossRef]
- Caqueo-Urízar, A.; Rus-Calafell, M.; Urzúa, A.; Escudero, J.; Gutiérrez-Maldonado, J. The role of family therapy in the management of schizophrenia: challenges and solutions. Neuropsychiatr Dis Treat. 2015 Jan 14;11:145-51. [CrossRef]
- Burbach, F.R. (2018). Family therapy and schizophrenia: a brief theoretical overview and a framework for clinical practice. BJPsych Advances, 24(4), 225–234. [CrossRef]
| Gender | Age | Illnessduration(in years) | BMI(kg/m2) | Family Support Scale (FSS) | CRP(mg/dl) | |||
|---|---|---|---|---|---|---|---|---|
| Male | Mean | 41.36* | 14.44 | 29.24 | 51.03 | Median | 0.17 | |
| N | 100 | 80 | 90 | 82 | N | 94 | ||
| S.D. | 10.79 | 11.01 | 4.22 | 10.62 | IQR | 0.30 | ||
| Female | Mean | 44.98* | 14.90 | 28.44 | 48.83 | Median | 0.19 | |
| N | 106 | 80 | 88 | 88 | N | 88 | ||
| S.D. | 14.37 | 10.01 | 5.44 | 10.23 | IQR | 0.41 | ||
| Total | Mean | 43.22 | 13.98 | 28.85 | 49.89 | Median | 0.17 | |
| N | 206 | 160 | 178 | 170 | N | 182 | ||
| S. D. | 12.85 | 11.97 | 4.86 | 10.45 | IQR | 0.39 | ||
| * t test p<0.05; IQR: interquartile rangeNotes: For illness duration, BMI & FSS the means from the Two-Step transformation are presented | ||||||||
| Pearson CorrelationN: 206 | Age | Illness duration(in years) | BMI(kg/m2) | |
|---|---|---|---|---|
| Illness duration(in years) | r | 0.659** | ||
| p | 0.000 | |||
| BMI(kg/m2) | r | 0.240** | 0.315** | |
| p | 0.001 | 0.000 | ||
| Family Support Scale (FSS) | r | -0.151 | -0.250 | -0.125 |
| p | 0.050 | 0.004 | 0.132 | |
| Spearman’s rhoN: 206 | Age | Illness duration(in years) | BMI(kg/m2) | Family Support Scale (FSS) | |
|---|---|---|---|---|---|
| CRP | rho | 0.140 | 0.038 | 0.213** | -0.510** |
| p | 0.060 | 0.638 | 0.005 | 0.000 | |
| Dependent Variables: | Predictor | B | SE | Wald | p | OR (95% CL) |
|---|---|---|---|---|---|---|
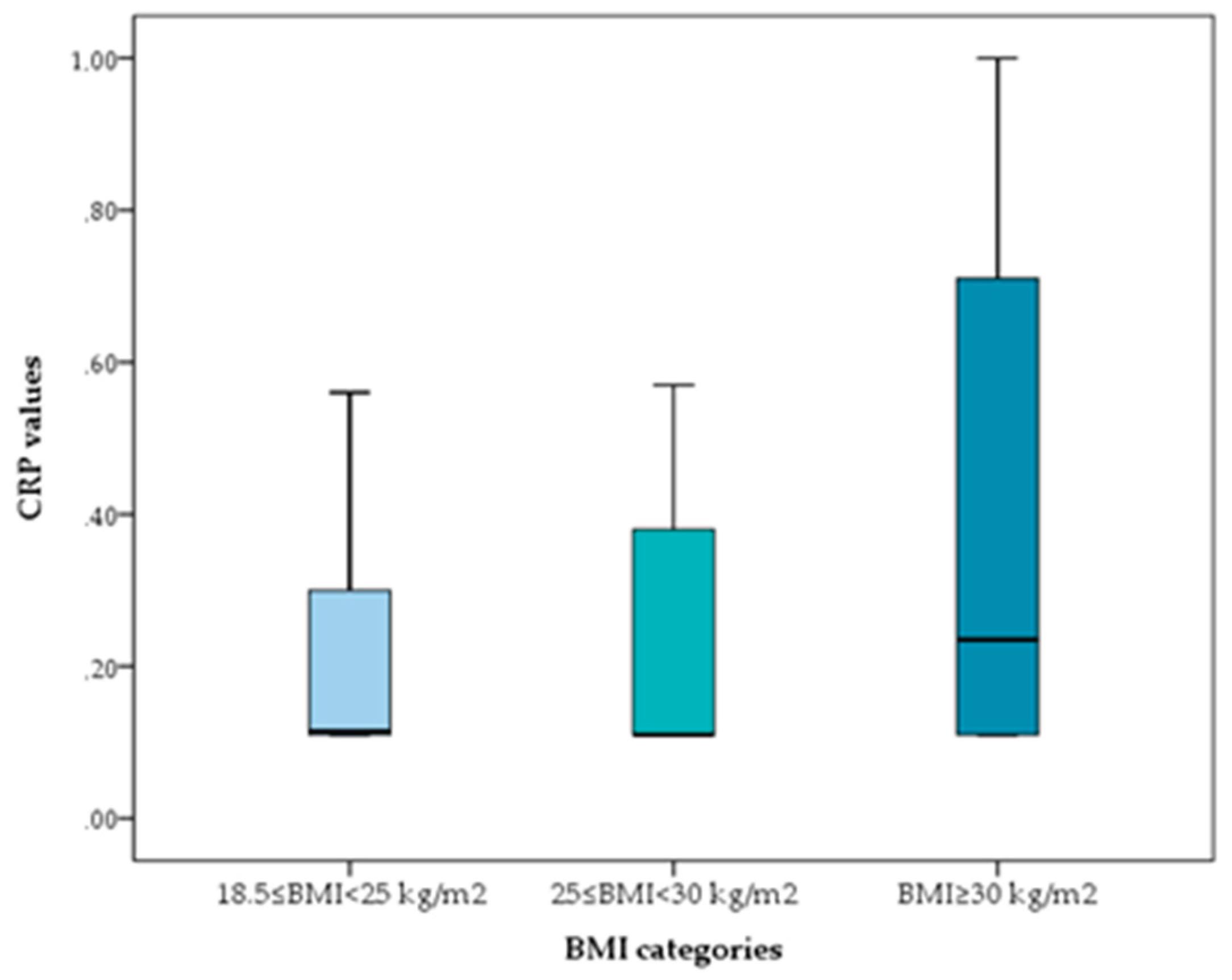
| CRP values ≥0.11mg/dl | ObesityBMI≥30 kg/m2 | 0.683 | 0.321 | 4.534 | 0.033* | 1.980 (1.056, 3.713) |
| CRP values >0.6mg/dl | 3.326 | 0.758 | 19.262 | 0.000** | 27.818 (6.300, 122.838) | |
| Notes: B = logistic regression coefficient;Correlations are statistically significant at the *p < 0.05, ** p <0.01 level. | ||||||
| Dependent Variable: CRP values >0.6mg/dl | B | SE | Wald | p | OR [95% CL] |
|---|---|---|---|---|---|
| Age | -0.047 | 0.049 | 0.923 | 0.337 | 0.954 [0.866, 1.051] |
| Gender | 0.552 | 0.616 | 0.805 | 0.370 | 1.738 [0.520, 5.811] |
| Illness duration | 0.088 | 0.052 | 2.817 | 0.093 | 1.092 [0.985, 1.210] |
| BMI | 0.158 | 0.068 | 5.396 | 0.020* | 1.171 [1.025, 1.337] |
| FSS | -0.090 | 0.037 | 6.086 | 0.014* | 0.914 [0.850, 0.982] |
| Notes: B = logistic regression coefficient;Correlations are statistically significant at the *p < 0.05, ** p <0.01 level. | |||||
| Dependent Variable: CRP values >0.6mg/dl | B | SE | Wald | p | Exp(B) [LLCL, ULCI] |
|---|---|---|---|---|---|
| Constant | -34.5617 | 15.2349 | 5.1465 | 0.0233 | |
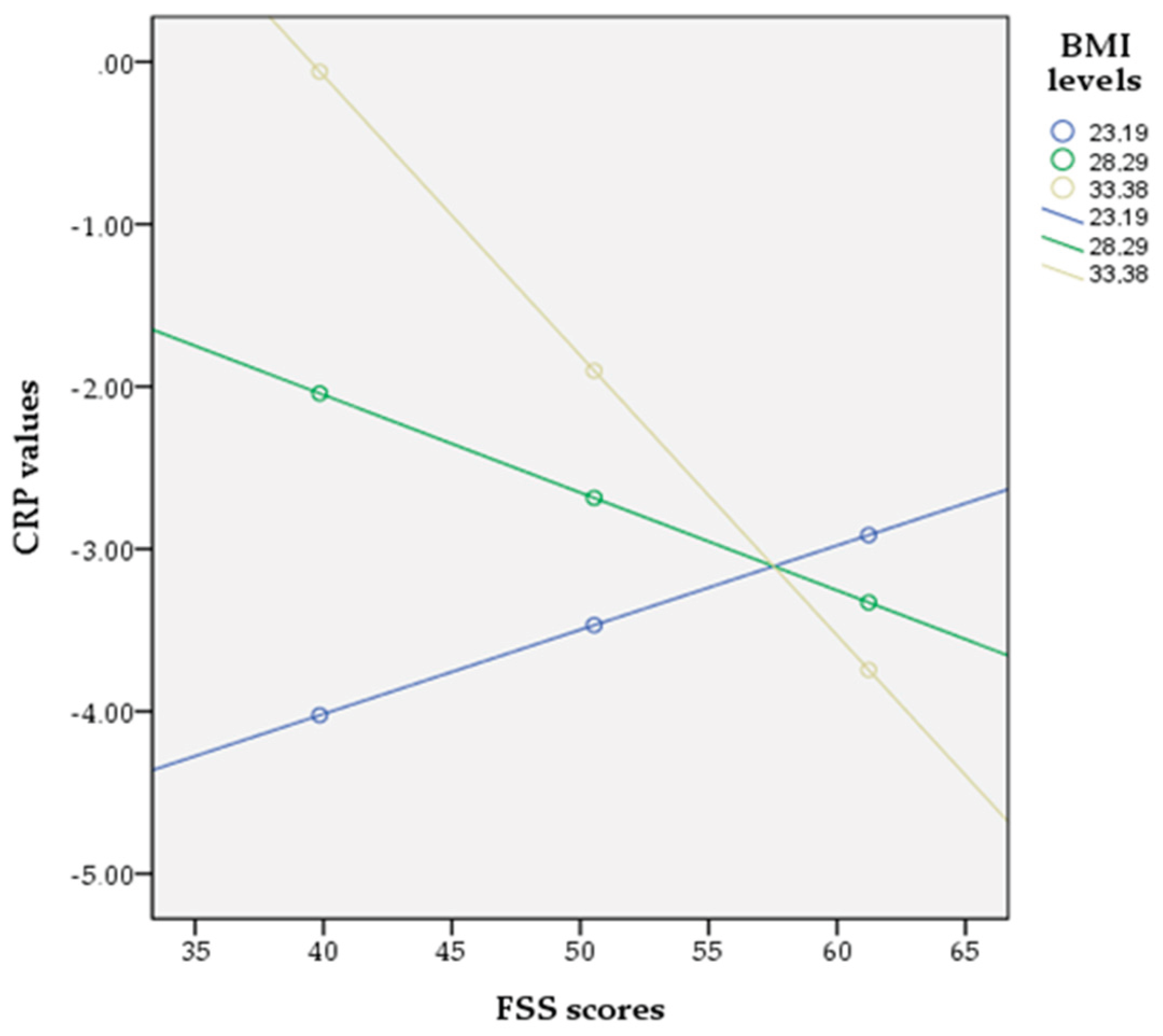
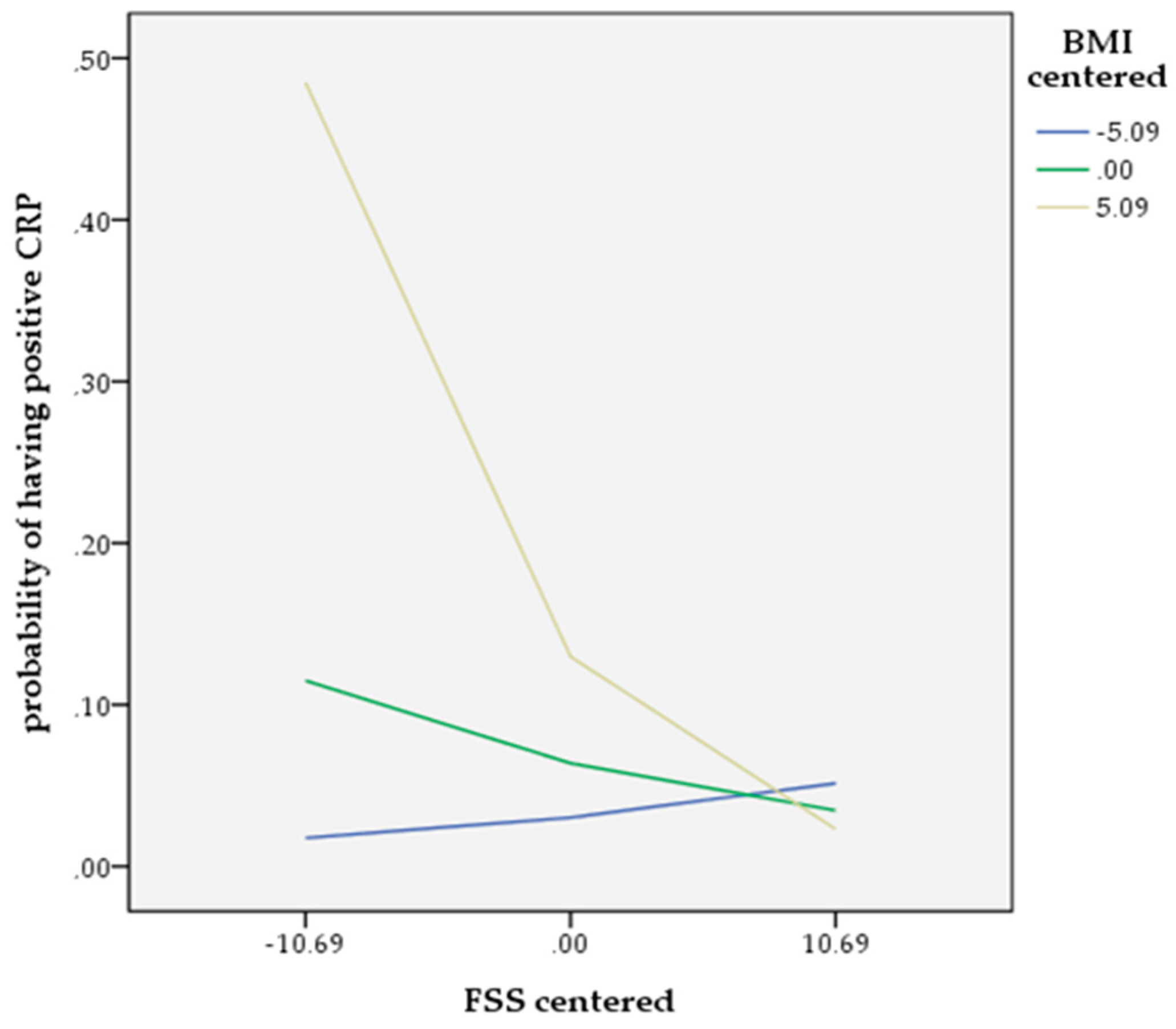
| FSS | 0.5624 | 0.2951 | 3.6332 | 0.0566 | 1.7548 [-0.0159, 1.1408] |
| Moderator (BMI) | 1.2664 | 0.5257 | 5.8028 | 0.0160* | 3.5480 [0.2360, 2.2967] |
| Interaction (FSS*BMI) | -0.0220 | 0.0100 | 4.8079 | 0.0283* | 0.9782 [-0.0417, -0.0023] |
| Covariates | |||||
| Age | -0.0687 | 0.0567 | 1.4648 | 0.2261 | 0.9336 [-0.1799, 0.0425] |
| Gender | 0.4568 | 0.6779 | 0.4541 | 0.5004 | 1.5790 [-0.8719, 1.7856] |
| Illness duration | 0.0897 | 0.0597 | 2.2570 | 0.1330 | 1.0938 [-0.0273, 0.2067] |
| Notes: B = logistic regression coefficient;Correlations are statistically significant at the *p < 0.05, ** p <0.01 level. | |||||
| BMI level | Effect of FSS on having positiveCRP values | SE | z | Wald | p | [95% CL] |
|---|---|---|---|---|---|---|
| Low (-1SD): 23.1927 | 0.0519 | 0.0709 | 0.7323 | 0.5362 | 0.4640 | [-0.0870, 0.1908] |
| Mean: 28.2865 | -0.0602 | 0.0390 | -1.5428 | 2.3802 | 0.1229 | [-0.1368, 0.0163] |
| High (+1SD): 33.3803 | -0.1724 | 0.0571 | -3.0197 | 9.1185 | 0.0025* | [-0.2842, -0.0605] |
| Notes: Correlations are statistically significant at the *p < 0.05, ** p <0.01 level. | ||||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




