Submitted:
09 June 2025
Posted:
10 June 2025
You are already at the latest version
Abstract
Keywords:
Introduction
The External Violence Incident Report
Materials and Methods
Overview
Setting and Context
Data Collection
Measures and Outcomes
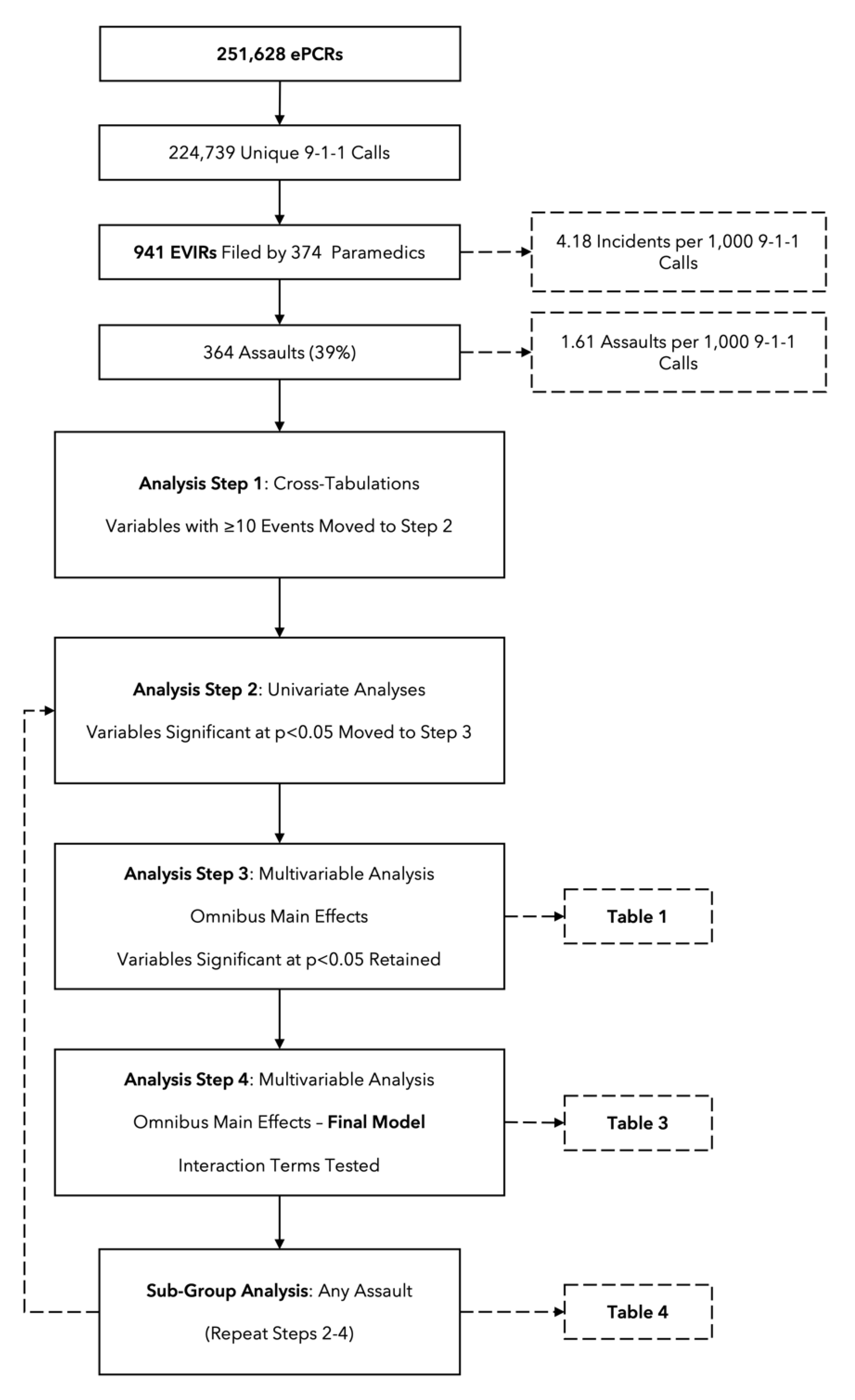
Analysis
Results
Overview
Univariate Analyses
Adjusted Models
Secondary Outcome: Any Assault
Discussion
Limitations
Conclusion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Maguire, B.J.; O’Meara, P.; O’Neill, B.J.; Brightwell, R. Violence against emergency medical services personnel: A systematic review of the literature. Am J Ind Med 2018, 61, 167–180. [Google Scholar] [CrossRef]
- Maguire, B.J.; O’Neill, B.J. Emergency Medical Service Personnel’s Risk From Violence While Serving the Community. Am J Public Health 2017, 107, 1770–1775. [Google Scholar] [CrossRef]
- Murray, R.M.; Davis, A.L.; Shepler, L.J.; Moore-Merrell, L.; Troup, W.J.; Allen, J.A.; Taylor, J.A. A Systematic Review of Workplace Violence Against Emergency Medical Services Responders. New Solut 2020, 29, 487–503. [Google Scholar] [CrossRef] [PubMed]
- Maguire, B.J.; Browne, M.; O’Neill, B.J.; Dealy, M.T.; Clare, D.; O’Meara, P. International Survey of Violence Against EMS Personnel: Physical Violence Report. Prehospital and disaster medicine 2018, 33, 526–531. [Google Scholar] [CrossRef]
- Olschowka, N.; Möckel, L. Aggression and violence against paramedics and the impact on mental health: A survey study. Journal of Emergency Medicine, Trauma and Acute Care 2021, 2021. [CrossRef]
- Taylor, J.; Murray, R.; Binzer, M.; Robert Borse, C.; Davis, A.; Gallogly, V.; Ghanbari, R.; Diane McKinsey, L.; Chief David Picone, B.; Gary Wingrove, P. EMERG-ing data: Multi-city surveillance of workplace violence against EMS responders. Journal of Safety Research 2023. [CrossRef]
- Bigham, B.; Jensen, J.L.; Tavares, W.; Drennan, I.; Saleem, H.; Dainty, K.N.; Munro, G. Paramedic self-reported exposure to violence in the emergency medical services (EMS) workplace: A mixed-methods cross sectional survey. Prehospital Emergency Care 2014, 18, 489–494. [Google Scholar] [CrossRef] [PubMed]
- Mausz, J.; Johnston, M.; Arseneau-Bruneau, D.; Batt, A.M.; Donnelly, E.A. Prevalence and Characteristics of Violence against Paramedics in a Single Canadian Site. International Journal of Environmental Research and Public Health 2023, 20. [Google Scholar] [CrossRef] [PubMed]
- McGuire, S.S.; Bellolio, F.; Buck, B.J.; Liedl, C.P.; Stuhr, D.D.; Mullan, A.F.; Buffum, M.R.; Clements, C.M. Workplace Violence Against Emergency Medical Services (EMS): A Prospective 12-Month Cohort Study Evaluating Prevalence and Risk Factors Within a Large, Multistate EMS Agency. Prehospital Emergency Care 2024, 1–8. [Google Scholar] [CrossRef]
- McGuire, S.S.; Bellolio, F.; Sztajnkrycer, M.D.; Sveen, M.J.; Liedl, C.P.; Mullan, A.F.; Clements, C.M. Use of Body Armor by EMS Clinicians, Workplace Violence, and Racial and Ethnic Disparities in Care. JAMA Netw Open 2025, 8, e2456528. [Google Scholar] [CrossRef]
- Schosler, B.; Bang, F.S.; Mikkelsen, S. The extent of physical and psychological workplace violence experienced by prehospital personnel in Denmark: a survey. Scand J Trauma Resusc Emerg Med 2024, 32, 136. [Google Scholar] [CrossRef]
- Maguire, B.J.; Al Amiry, A.; O’Neill, B.J. Occupational Injuries and Illnesses among Paramedicine Clinicians: Analyses of US Department of Labor Data (2010 - 2020). Prehospital and Disaster Medicine 2023, 38, 581–588. [Google Scholar] [CrossRef]
- McGuire, S.S.; Lampman, M.A.; Smith, O.A.; Clements, C.M. Impact of Workplace Violence Against Emergency Medical Services (EMS). Prehospital Emergency Care 2025, 29, 129–137. [Google Scholar] [CrossRef] [PubMed]
- Setlack, J.; Brais, N.; Keough, M.; Johnson, E.A. Workplace violence and psychopathology in paramedics and firefighters: Mediated by posttraumatic cognitions. Canadian Journal of Behavioural Science 2021, 53, 211–220. [Google Scholar] [CrossRef]
- Viking, M.; Hugelius, K.; Kurland, L. Experiences of exposure to workplace violence among ambulance personnel. International Emergency Nursing 2022, 65, 101220. [Google Scholar] [CrossRef]
- Carleton, R.N.; Afifi, T.O.; Turner, S.; Taillieu, T.; Duranceau, S.; LeBouthillier, D.M.; Sareen, J.; Ricciardelli, R.; MacPhee, R.; Groll, D.; et al. Mental disorder symptoms among public safety personnel in Canada. Can J Psychiatry 2018, 63, 54–64. [Google Scholar] [CrossRef]
- Reardon, M.; Abrahams, R.; Thyer, L.; Simpson, P. Review article: Prevalence of burnout in paramedics: A systematic review of prevalence studies. Emergency medicine Australasia 2020, 32, 182–189. [Google Scholar] [CrossRef] [PubMed]
- Crowe, R.P.; Bower, J.K.; Cash, R.E.; Panchal, A.R.; Rodriguez, S.A.; Olivo-Marston, S.E. Association of Burnout with Workforce-Reducing Factors among EMS Professionals. Prehospital Emergency Care 2018, 22, 229–236. [Google Scholar] [CrossRef]
- Carleton, R.N.; Afifi, T.O.; Taillieu, T.; Turner, S.; El-Gabalawy, R.; Sareen, J.; Asmundson, G.J.G. Anxiety-related psychopathology and chronic pain comorbidity among public safety personnel. J Anxiety Disord 2018, 55, 48–55. [Google Scholar] [CrossRef]
- Koopmans, E.; Wagner, S.L.; Schmidt, G.; Harder, H. Emergency Response Services Suicide: A Crisis in Canada? . Journal of Loss and Trauma 2017, 22, 527–539. [Google Scholar] [CrossRef]
- Shen, K.; Eddelbuettel, J.C.P.; Eisenberg, M.D. Job Flows Into and Out of Health Care Before and After the COVID-19 Pandemic. JAMA Health Forum 2024, 5, e234964. [Google Scholar] [CrossRef]
- Poon, Y.R.; Lin, Y.P.; Griffiths, P.; Yong, K.K.; Seah, B.; Liaw, S.Y. A global overview of healthcare workers’ turnover intention amid COVID-19 pandemic: a systematic review with future directions. Hum Resour Health 2022, 20, 70. [Google Scholar] [CrossRef] [PubMed]
- Mausz, J.; Johnston, M.; Donnelly, E.A. The role of organizational culture in normalizing paramedic exposure to violence. Journal of Aggression, Conflict and Peace Research 2021, 14, 112–122. [Google Scholar] [CrossRef]
- Boyle, M.; McKenna, L. Paramedic student exposure to workplace violence during clinical placements - A cross-sectional study. Nurse Educ Pract 2017, 22, 93–97. [Google Scholar] [CrossRef] [PubMed]
- Braun, D.; Reifferscheid, F.; Kerner, T.; Dressler, J.L.; Stuhr, M.; Wenderoth, S.; Petrowski, K. Association between the experience of violence and burnout among paramedics. Int Arch Occup Environ Health 2021, 94, 1559–1565. [Google Scholar] [CrossRef]
- Gormley, M.A.; Crowe, R.P.; Bentley, M.A.; Levine, R. A National Description of Violence toward Emergency Medical Services Personnel. Prehospital Emergency Care 2016, 20, 439–447. [Google Scholar] [CrossRef]
- Maguire, B.J.; Hunting, K.L.; Smith, G.S.; Levick, N.R. Occupational fatalities in emergency medical services: a hidden crisis. Annals of Emergency Medicine 2002, 40, 625–632. [Google Scholar] [CrossRef]
- Maguire, B.J.; Smith, S. Injuries and fatalities among emergency medical technicians and paramedics in the United States. Prehospital and Disaster Medicine 2013, 28, 376–382. [Google Scholar] [CrossRef]
- Mausz, J.; Donnelly, E.A. Violence Against Paramedics: Protocol for Evaluating 2 Years of Reports Through a Novel, Point-of-Event Reporting Process. JMIR Res Protoc 2023, 12, e37636. [Google Scholar] [CrossRef]
- Mausz, J.; Johnston, M.; Donnelly, E. Development of a reporting process for violence against paramedics. Canadian Paramedicine 2021, 44. [Google Scholar]
- Ding, Y.; Park, E.; Nagarajan, M.; Grafstein, E. Patient prioritization in emergency department triage systems: An empirical study of Canadian triage and acuity scale (CTAS). Manufacturing & Service Operations Management 2017, 24, 713–948. [Google Scholar] [CrossRef]
- Kim, S.C.; Dunn, K.; Youells, C.; Whitmore, G.; McComack, A.; Dievendorf, E.; Bell, C.; Burnett, S.J.; Kim, S.; Clemency, B. Aggressive Behavior Risk Assessment Tool for Emergency Medical Services. J Am Coll Emerg Physicians Open 2025, 6, 100095. [Google Scholar] [CrossRef] [PubMed]
- Strum, R.P.; Tavares, W.; Worster, A.; Griffith, L.E.; Costa, A.P. Identifying patient characteristics associated with potentially redirectable paramedic transported emergency department visits in Ontario, Canada: a population-based cohort study. BMJ Open 2021, 11, e054625. [Google Scholar] [CrossRef] [PubMed]
- Tavares, W.; Kaas-Mason, S.; Spearen, C.; Kedzierski, N.; Watts, J.; Moran, P.; Leyenaar, M.S. Redesigning paramedicine systems in Canada with “IMPACC”. Paramedicine 2024. [CrossRef]
- Drew, P.; Devenish, S.; Tippett, V. Paramedic occupational violence: A qualitative examination of aggressive behaviour during out-of-hospital care. Paramedicine 2024, 21. [Google Scholar] [CrossRef]
- Bolster, J.; Armour, R.; O’Toole, M.; Lysko, M.; Batt, A.M. The paramedic role in caring for people who use illicit and controlled drugs: A scoping review. Paramedicine 2023, 20, 117–127. [Google Scholar] [CrossRef]
- Bolster, J.L.; Batt, A.M. An Analysis of Drug Use-Related Curriculum Documents for Paramedic Students in British Columbia. Cureus 2023, 15, e48515. [Google Scholar] [CrossRef]
- Ford-Jones, P.C. Enhancing Safety and Mitigating Violence on Prehospital Mental Health Calls: For the Care Providers and Care Recipients. Canadian Journal of Community Mental Health 2023, 42, 17–31. [Google Scholar] [CrossRef]
- Meijer, P.; Ford-Jones, P.; Carter, D.; Duhaney, P.; Adam, S.; Pomeroy, D.; Thompson, S. Examining an Alternate Care Pathway for Mental Health and Addiction Prehospital Emergencies in Ontario, Canada: A Critical Analysis. International Journal of Environmental Research and Public Health 2024, 21. [Google Scholar] [CrossRef]
- Ford-Jones, P.; Thompson, S.; Pomeroy, D.; Duhaney, P.; Adam, S.; Gebremikael, L.; Carter, D.; Iheanacho, C.; Meijer, P. An Integrated Crisis Care Framework: A Community-Informed Approach; Humber Polytechnic: Ontario, Canada, 2024. [Google Scholar]
- Bruton, L.; Johnson, H.; MacKey, L.; Farok, A.; Thyer, L.; Simpson, P.M. The impact of body-worn cameras on the incidence of occupational violence towards paramedics: a systematic review. Journal of Aggression, Conflict and Peace Research 2022, 14, 133–142. [Google Scholar] [CrossRef]
- Mausz, J.; Piquette, D.; Bradford, R.; Johnston, M.; Batt, A.M.; Donnelly, E. Hazard flagging as a risk mitigation strategy for violence against emergency medical services. Healthcare 2024, 21, 1–8. [Google Scholar] [CrossRef]
- Garner, D.G., Jr.; DeLuca, M.B.; Crowe, R.P.; Cash, R.E.; Rivard, M.K.; Williams, J.G.; Panchal, A.R.; Cabanas, J.G. Emergency medical services professional behaviors with violent encounters: A prospective study using standardized simulated scenarios. J Am Coll Emerg Physicians Open 2022, 3, e12727. [Google Scholar] [CrossRef] [PubMed]
- Chirico, F.; Afolabi, A.A.; Ilesanmi, O.S.; Nucera, G.; Ferrari, G.; Szarpak, L.; Yildirim, M.; Magnavita, N. Workplace violence against healthcare workers during the COVID-19 pandemic: A systematic review. Journal of Health and Social Sciences 2022, 7, 14–35. [Google Scholar] [CrossRef]
| Category | Covariate | OR | 95% CI | p-value | Decision |
|---|---|---|---|---|---|
|
Dispatch Priority |
Priority 3 (‘Prompt’) | 1.21 | 0.91, 1.62 | 0.17 | Dropped |
| Priority 4 (‘Urgent’) | 1.34 | 1.02, 1.77 | 0.03 | Retained | |
|
Call Location Code |
Other Location (Reference) | ||||
| Private Residence | 0.99 | 0.81, 1.22 | 0.97 | Dropped | |
| Store | 2.02 | 1.42, 2.87 | <0.001 | Retained | |
| Long-Term Care Home | 0.82 | 0.56, 1.20 | 0.31 | Dropped | |
| Hotel | 3.17 | 2.07, 4.84 | <0.001 | Retained | |
| Street/Intersection | 1.91 | 1.50, 2.44 | <0.001 | Retained | |
| Restaurant/Bar | 5.55 | 3.58, 8.60 | <0.001 | Retained | |
|
Shift |
Day Shift (Reference) | Retained | |||
| Afternoon Shift | 1.52 | 1.30, 1.77 | <0.001 | Retained | |
| Overnight Shift | 1.59 | 1.33, 1.90 | <0.001 | Retained | |
|
Acuity |
CTAS 5 (Non-Urgent; Reference) |
Reclassified into “High Acuity” variable (i.e., CTAS 1 or 2) |
|||
| CTAS 4 (Less Urgent) | 0.66 | 0.85, 1.71 | 0.05 | ||
| CTAS 3 (Urgent) | 1.20 | 0.85, 1.71 | 0.28 | ||
| CTAS 2 (Emergent) | 2.02 | 1.41, 2.88 | <0.001 | ||
| CTAS 1 (Resuscitation) | 1.64 | 1.02, 2.66 | 0.04 | ||
|
Primary Problem Code |
Other Problem (Reference) | ||||
| General Problem | 1.18 | 0.92, 1.52 | 0.18 | Dropped | |
| Intoxication | 16.54 | 13.34, 20.48 | <0.001 | Retained | |
| Abdominal Pain | 1.35 | 0.95, 1.93 | 0.09 | Dropped | |
| Mental Health | 12.71 | 10.29, 15.69 | <0.001 | Retained | |
| Dyspnea | 1.01 | 0.67, 1.54 | 0.93 | Dropped | |
| Trauma/Injury | 2.02 | 1.58, 2.58 | <0.001 | Retained | |
| Chest Pain | 1.58 | 1.09, 6.56 | 0.01 | Retained | |
| Altered Mental Status | 4.77 | 3.47, 6.56 | <0.001 | Retained | |
|
Patient Age |
Seniors (65+ Years; Reference) | ||||
| Working Age (25-64 Years) | 2.40 | 2.05, 2.80 | <0.001 | Retained | |
| Youth (15-24 Years) | 1.69 | 1.31, 2.17 | <0.001 | Retained | |
| Children (0-14 Years) | 0.38 | 0.21, 0.68 | 0.001 | Retained |
| Patient Age/Sex Groups | OR | 95% CI | p-value |
|---|---|---|---|
| Children - Female | 0.42 | 0.19, 0.90 | 0.026 |
| Children - Male | 0.24 | 0.10, 0.59 | 0.002 |
| Youth - Female | 1.20 | 0.83, 1.74 | 0.324 |
| Youth - Male | 1.64 | 1.18, 2.29 | 0.003 |
| Working Age - Female | 1.22 | 0.96, 1.54 | 0.094 |
| Working Age - Male | 2.73 | 2.23, 3.38 | <0.001 |
| Senior - Female | 0.69 | 0.53, 0.90 | 0.007 |
| Senior - Male (Reference) |
| Variable Category | Covariate | OR | 95% CI | p-value |
|---|---|---|---|---|
|
Pick Up Location |
Other Location (Reference) | |||
| Hotel | 1.50 | 1.01, 2.24 | 0.041 | |
| Street | 1.33 | 1.11, 1,60 | <0.001 | |
| Restaurant/Bar | 2.84 | 1.64, 3.76 | <0.001 | |
| Shift | Day Shift (Reference) | |||
| Afternoon Shift | 1.26 | 1.08, 1.48 | 0.003 | |
| Overnight Shift | 1.25 | 1.05, 1.50 | 0.011 | |
|
Primary Problem |
Other Problem (Reference) | |||
| Intoxication | 9.06 | 7.49, 10.95 | <0.001 | |
| Mental Health | 10.59 | 8.89, 12.61 | <0.001 | |
| Trauma | 1.67 | 1.34, 2.08 | <0.001 | |
| Altered Mental Status | 3.27 | 2.43, 4.40 | <0.001 | |
| Acuity | High Acuity | 1.86 | 1.62, 2.15 | <0.001 |
|
Patient Demographics |
Other Age/Gender Group (Reference) | |||
| Youth - Male | 0.31 | 0.12, 0.75 | 0.009 | |
| Working Age - Male | 1.78 | 1.54, 2.04 | <0.001 |
| Variable Category | Covariate | p-value | OR | 95% CI |
|---|---|---|---|---|
| Pick-Up Location | Long-Term Care | <0.001 | 2.51 | 1.71, 3.70 |
|
Shift |
Day Shift (Reference) | |||
| Afternoon Shift | 0.042 | 1.28 | 1.00, 1.64 | |
| Overnight Shift | 0.693 | 1.06 | 0.79, 1.42 | |
|
Primary Problem |
Other Problem (Reference) | |||
| Intoxication | <0.001 | 21.37 | 15.43, 29.58 | |
| Mental Health | <0.001 | 30.37 | 22.67, 40.80 | |
| Trauma/Injury | <0.001 | 2.19 | 1.47, 3.27 | |
| Altered Mental Status | <0.001 | 6.06 | 4.02, 9.14 | |
| Acuity | High Acuity | <0.001 | 2.86 | 2.30, 3.56 |
|
Patient Demographics |
Senior - Male (Reference) | |||
| Children - Female | 0.036 | 0.22 | 0.05, 0.90 | |
| Children - Male | 0.037 | 0.12 | 0.01, 0.88 | |
| Youth - Female | 0.036 | 0.57 | 0.34, 0.96 | |
| Youth - Male | 0.318 | 0.77 | 0.47, 1.27 | |
| Working Age - Female | 0.187 | 0.78 | 0.54, 1.12 | |
| Working Age - Male | 0.210 | 0.80 | 0.56, 1.13 | |
| Senior - Female | 0.019 | 0.63 | 0.43, 0.92 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




