Submitted:
01 June 2025
Posted:
02 June 2025
Read the latest preprint version here
Abstract
Keywords:
1. Introduction
2. CCTA and Myocardial Bridging
3. Artificial Intelligence and Machine Learning in CCTA
4. Artificial Intelligence and Machine Learning in Myocardial Bridging
| Purpose | Type | Requirements | Functional or anatomical | |
|---|---|---|---|---|
| AI-enhanced segmentation and reconstruction | Analysis of images to identify regions of interest, enhance image quality and assess ischemia | Imaging + AI-based analysis | CT, MRI or US images | Functional, anatomical |
| CFD | Simulate and analyze blood flow dynamics within vessels or the heart | Imaging + simulation | CT scan with contrast agent, computational modeling | Functional |
| CT-FFR | Assessment of functional significance of stenosis by simulating blood flow | Imaging + simulation + ML-based analysis | CT scan with contrast agent, computational modeling | Functional |
4.1 AI-Enhanced Segmentation and Reconstruction
4.2 Computational Fluid Dynamics (CFD)
4.3 CT-Derived Fractional Flow Reserve (CT-FFR)
5. Challenges in Practical Implementation
5. Methods
6. Results
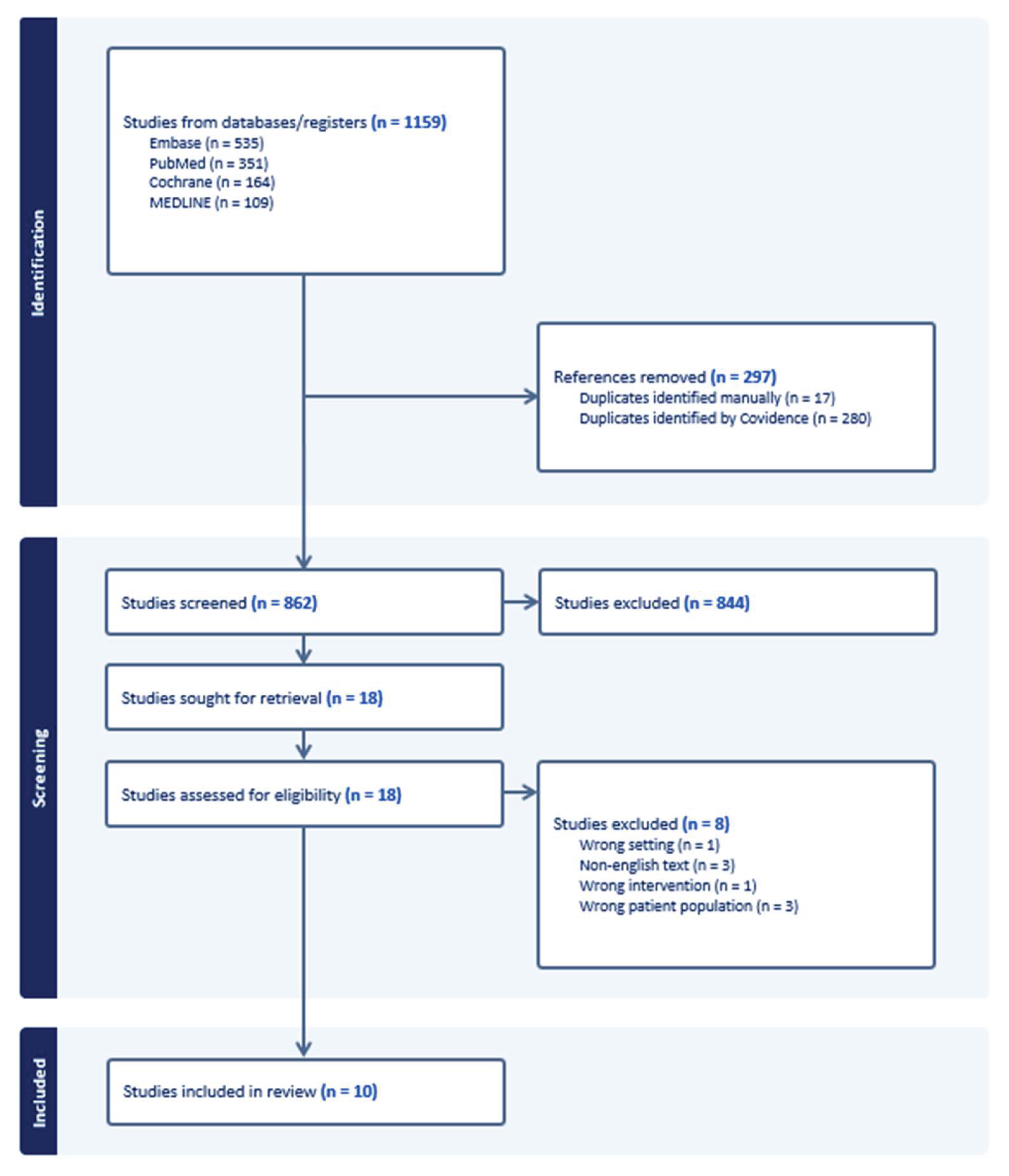
7. Discussion
| Study | Journal | Country | Study type | Study aim | Population | Total participants | Age | % Male | AI/ML technique | Purpose of AI | Findings |
| Martens 2024 [36] | European Heart Journal - Case Reports | Belgium | Case report | To report on a case showing improvement in CT-FFR following treatment of MB | A patient with LAD MB and abnormal CT-FFR which normalized after treatment with surgical unroofing of the MB | 1 | 55 | 100 | ML-based CT-FFR (HeartFlow) | Computation of CT-FFR | Normalization of CT-FFR from 0.76 pre-surgery to 0.92 post-surgery |
| Zhou 2019 [37] | European Radiology | China | Retrospective case-control | To evaluate the feasibility of CT-FFR derivation from CCTA in patients with MB, its relationship with MB anatomical features, and clinical relevance | Patients with LAD MB on CCTA with no atherosclerosis as compared with controls | 161; 120 cases; 40 controls |
Cases: 52.4 ± 11 Controls: 54.3 ± 11.5 |
Cases: 68 Controls: 54 |
ML-based CT-FFR (cFFR v3.0.0, Siemens Healthineers) | Computation of CT-FFR | MBs are associated with abnormal CT-FFR values. MB length and systolic stenosis are the main contributors to abnormal CT-FFR values with a combination of the two showing moderate predictive performance. Patients with abnormal FFR were less likely to be asymptomatic and more likely to have typical anginal chest pain |
| Zhou 2019 [34] | JACC: Cardiovascular Imaging | China | Retrospective cohort | To investigate the role of CT-FFR in predicting proximal plaque formation associated with MB in the LAD using ML approaches | Patients with MB in the LAD and no atherosclerosis on baseline CCTA who underwent follow-up CCTA with a minimum interval of 3 months | 188 | 55 ± 6 | 68.6 | ML-based CT-FFR (cFFR v3.0.0, Siemens Healthineers); ML-based prediction model using LASSO algorithms |
Computation of CT-FFR; ML models for prediction of plaque formation | CT-FFR distal to LAD MB and ΔCT-FFR significantly differed between patients with CT MB LAD who developed plaque and those who did not. ML algorithms further identified CT-FFR and ΔCT-FFR as the strongest predictors of plaque formation proximal to MB LAD |
| Zhou 2019 [35] | Canadian Journal of Cardiology | China | Retrospective cohort | To study the diagnostic performance of ML-based CT-FFR to detect functional ischemia in MB with iFFR as the reference standard | Patients who underwent CCTA for the evaluation of suspected or known CAD and were found to have LAD MB, who then underwent ICA within 60 days of CCTA | 104 | 61.2 ± 9.1 | 72.1 | ML-based CT-FFR (cFFR v3.2.0, Siemens Healthineers) | Automatic generation of centreline and luminal contours of coronary arteries; Computation of CT-FFR | CT-FFR has high diagnostic performance for functional ischemia in vessels with MB and concomitant proximal atherosclerotic disease compared with iFFR, regardless of length and depth of MB, with a low PPV for lesions of <70% stenosis |
| Jubran 2020 [39] | Circulation: Cardiovascular Imaging | United States | Retrospective cohort | To compare CT-FFR, dobutamine-stress dFFR, iFFR and IVUS in assessing the hemodynamic significance of MB | Patients with angina who had been found to have an MB in the LAD with ≤50% coronary artery stenosis by ICA and had undergone CCTA | CT-FFR: 49 dFFR: 43 iFFR: 28 IVUS: 46 |
47.5 ± 13.7 | 39 | ML-based CT-FFR (cFFR v3.1.2, Siemens Healthineers) | Computation of CT-FFR | CT-FFR values measured in LAD MB were lower than arteries without MB. CT-FFR values did not correlate with dobutamine-stress dFFR, iFFR or LAD systolic compression on IVUS. CT-FFR values were higher than dFFR and lower than iFFR. There was non-concordance between CT-FFR and dFFR, iFFR or degree of systolic compression measured by IVUS |
| Yu 2021 [38] | Korean Journal of Radiology | China | Cross sectional | To investigate the diagnostic performance of CT-FFR for MB-related ischemia using dynamic CT-MPI as a reference standard | Symptomatic patients with LAD MB and no obstructive stenosis on CCTA who also underwent CT-MPI | 75 | 62.7 ± 13.2 | 64 | ML-based CT-FFR (cFFR; version 3.0, Siemens Healthineers) | Computation of CT-FFR | ΔCT-FFRsystolic shows high sensitivity and NPV and reliably excludes MB-ischemia. All CT-FFR measurements had low PPV and other methodologies are needed to confirm positive CT-FFR results |
| Zhang 2024 [32] | Clinical Radiology | China | Retrospective Observational Comparative Study (Within-Subject) | To determine the effect of second-generation motion correction (MC2) on image quality and measurement reproducibility of CCTA images in patients with MB and mural coronary artery (MB-MCA) compared to standard (STD) images without motion correction and with first-generation motion correction (MC1) | Patients with known or suspected coronary artery disease who underwent CCTA and had MB-MCA in the LAD | 66 | 62 ± 11 | 45 | Deep learning image reconstruction algorithm (DLIR, GE Healthcare); First generation motion correction algorithm (MC1, GE Healthcare); Second generation motion correction algorithm (MC2, GE Healthcare) | Image reconstruction and motion correction | MC2 reduced motion artefacts and resulted in significant improvements of image quality and diagnostic confidence and measurement reproducibility for both MB and MCA in systolic and diastolic phases |
| Zhang 2024 [33] | Clinical Physiology and Functional Imaging | China | Retrospective case-control | To quantitatively investigate the effect of MB in the LAD on CT-FFR | Patients with confirmed LAD MB on CCTA with or without atherosclerosis in the LAD as compared with controls | 404; 300 cases; 104 controls |
Cases: 54 ± 6 Controls: 54 ± 7 |
Cases: 56 Controls: 24 |
ML-based CT-FFR (Shukun, ct-FFR, V1.17) | Automatic extraction of coronary artery tree; automatic segmentation, reconstruction and diagnosis of coronary artery stenosis; Computation of CT-FFR |
No differences in CT-FFR values between systolic and diastolic phases. MB (with or without atherosclerosis) is associated with greater ΔCT-FFR and lower CT-FFR compared with controls without MB. CT-FFR is significantly lower in MB with atherosclerosis than in MB without atherosclerosis. In MB with atherosclerosis, LAD stenosis severity is an independent risk factor significantly affecting CT-FFR values and abnormal CT-FFR (<0.80) is associated with more severe LAD stenosis. There was no significant difference detected in terms of clinical or anatomical features between the abnormal and normal CT-FFR groups |
| Chen 2024 [31] | European Heart Journal - Cardiovascular Imaging | China | Retrospective cohort and validation study | To develop and validate CCTA based radiomics models in predicting proximal plaque development in LAD MB | Patients with MB and no atherosclerotic plaque proximal to the MB segment on baseline CCTA | 295 | 55 ± 10 | 66 | ML models | Predictive modelling and analysis | The proximal MB cross-sectional radiomics model (pMB CS) is able to predict proximal atherosclerotic plaque development associated with LAD MB in an external validation set (AUC 0.75; P <0.001) and can be integrated with a clinical model to further improve performance (AUC 0.76; P <0.001) |
| Sun 2024 [30] | Clinical Imaging | China | Cross sectional | To compare the performance between CT-FFR and ΔCT-FFR in patients with deep LAD MB and explore predictors of discordance between the two measurements | Patients with deep LAD MB on CCTA and <50% stenosis of the LAD and/or left main stem | 175 | 60 ± 7 | 71.4 | Deep learning image reconstruction (TrueFidelity, GE Healthcare); ML-based CT-FFR (uAI Portal; United Imaging Intelligence) |
Image reconstruction; Automatic labelling of plaque and MB; Computation of CT-FFR |
30.9% of patients had discordance of CT-FFR and ΔCT-FFR with 94.4% of patients leaning towards CT-FFR positivity with a negative ΔCT-FFR. Proximal atherosclerosis and distance from the MB to the aorta were independent risk factors for discordance. Anatomic features (length and depth) of the MB were correlated with ΔCT-FFR rather than CT-FFR, suggesting ΔCT-FFR as a more specific tool for MB evaluation |
8. Conclusion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Rogers, I. S., Tremmel, J. A. & Schnittger, I. Myocardial bridges: Overview of diagnosis and management. Congenit Heart Dis 12, 619–623 (2017). [CrossRef]
- Poláček, P. Relation of myocardial bridges and loops on the coronary arteries to coronary occlusions. Am Heart J 61, 44–52 (1961). [CrossRef]
- Ishii, T., Asuwa, N., Masuda, S. & Ishikawa, Y. The effects of a myocardial bridge on coronary atherosclerosis and ischaemia. J Pathol 185, 4–9 (1998). [CrossRef]
- Möhlenkamp, S., Hort, W., Ge, J. & Erbel, R. Update on myocardial bridging. Circulation 106, 2616–2622 (2002). [CrossRef]
- Kawawa, Y. et al. Detection of myocardial bridge and evaluation of its anatomical properties by coronary multislice spiral computed tomography. Eur J Radiol 61, 130–138 (2007). [CrossRef]
- Rubinshtein, R. et al. Long-term prognosis and outcome in patients with a chest pain syndrome and myocardial bridging: a 64-slice coronary computed tomography angiography study. Eur Heart J Cardiovasc Imaging 14, 579–585 (2013). [CrossRef]
- Feld, H. et al. Exercise-induced ventricular tachycardia in association with a myocardial bridge. Chest 99, 1295–1296 (1991). [CrossRef]
- Nakanishi, R., Rajani, R., Ishikawa, Y., Ishii, T. & Berman, D. S. Myocardial bridging on coronary CTA: an innocent bystander or a culprit in myocardial infarction? J Cardiovasc Comput Tomogr 6, 3–13 (2012).
- Ge, J. et al. Comparison of intravascular ultrasound and angiography in the assessment of myocardial bridging. Circulation 89, 1725–1732 (1994). [CrossRef]
- Patricio, L. et al. Fractional flow reserve versus angiography for guiding percutaneous coronary intervention. Revista Portuguesa de Cardiologia 28, 229–230 (2009).
- Zimmermann, F. M. et al. Deferral vs. performance of percutaneous coronary intervention of functionally non-significant coronary stenosis: 15-year follow-up of the DEFER trial. Eur Heart J 36, 3182–3188 (2015). [CrossRef]
- Escaned, J. et al. Importance of diastolic fractional flow reserve and dobutamine challenge in physiologic assessment of myocardial bridging. J Am Coll Cardiol 42, 226–233 (2003). [CrossRef]
- Angelini, P., Uribe, C. & Raghuram, A. Coronary Myocardial Bridge Updates: Anatomy, Pathophysiology, Clinical Manifestations, Diagnosis, and Treatment Options. Tex Heart Inst J 52, (2025). [CrossRef]
- Ekeke, C. N., Noble, S., Mazzaferri, E. & Crestanello, J. A. Myocardial bridging over the left anterior descending: Myotomy, bypass, or both? J Thorac Cardiovasc Surg 149, e57–e58 (2015). [CrossRef]
- Tandar, A., Whisenant, B. K. & Michaels, A. D. Stent fracture following stenting of a myocardial bridge: Report of two cases. Catheterization and Cardiovascular Interventions 71, 191–196 (2008). [CrossRef]
- Kunamneni, P. B. et al. Outcome of intracoronary stenting after failed maximal medical therapy in patients with symptomatic myocardial bridge. Catheter Cardiovasc Interv 71, 185–190 (2008). [CrossRef]
- Bamberg, F. et al. Dynamic myocardial CT perfusion imaging for evaluation of myocardial ischemia as determined by MR imaging. JACC Cardiovasc Imaging 7, 267–277 (2014). [CrossRef]
- Ho, K. T., Chua, K. C., Klotz, E. & Panknin, C. Stress and rest dynamic myocardial perfusion imaging by evaluation of complete time-attenuation curves with dual-source CT. JACC Cardiovasc Imaging 3, 811–820 (2010). [CrossRef]
- Yang, J. et al. Stress Myocardial Blood Flow Ratio by Dynamic CT Perfusion Identifies Hemodynamically Significant CAD. JACC Cardiovasc Imaging 13, 966–976 (2020). [CrossRef]
- Li, Y., Dai, X., Lu, Z., Shen, C. & Zhang, J. Diagnostic performance of quantitative, semi-quantitative, and visual analysis of dynamic CT myocardial perfusion imaging: a validation study with invasive fractional flow reserve. Eur Radiol 31, 525–534 (2021). [CrossRef]
- Schicchi, N. et al. Stress-rest dynamic-CT myocardial perfusion imaging in the management of myocardial bridging: A ‘one-stop shop’ exam. J Cardiol Cases 28, 229–232 (2023). [CrossRef]
- Williams, M. C. et al. Artificial intelligence and machine learning for cardiovascular computed tomography (CCT): A white paper of the society of cardiovascular computed tomography (SCCT). J Cardiovasc Comput Tomogr 18, 519–532 (2024). [CrossRef]
- Slart, R. H. J. A. et al. Position paper of the EACVI and EANM on artificial intelligence applications in multimodality cardiovascular imaging using SPECT/CT, PET/CT, and cardiac CT. Eur J Nucl Med Mol Imaging 48, 1399–1413 (2021). [CrossRef]
- Sandeep, B. et al. Feasibility of artificial intelligence its current status, clinical applications, and future direction in cardiovascular disease. Curr Probl Cardiol 49, 102349 (2024). [CrossRef]
- Liao, J., Huang, L., Qu, M., Chen, B. & Wang, G. Artificial Intelligence in Coronary CT Angiography: Current Status and Future Prospects. Front Cardiovasc Med 9, 896366 (2022). [CrossRef]
- Lopez-Jimenez, F. et al. Artificial Intelligence in Cardiology: Present and Future. Mayo Clin Proc 95, 1015–1039 (2020). [CrossRef]
- Krittanawong, C., Zhang, H. J., Wang, Z., Aydar, M. & Kitai, T. Artificial Intelligence in Precision Cardiovascular Medicine. J Am Coll Cardiol 69, 2657–2664 (2017). [CrossRef]
- Tolu-Akinnawo, O. Z., Ezekwueme, F., Omolayo, O., Batheja, S. & Awoyemi, T. Advancements in Artificial Intelligence in Noninvasive Cardiac Imaging: A Comprehensive Review. Clin Cardiol 48, e70087 (2025). [CrossRef]
- Kwan, A. C., Salto, G., Cheng, S. & Ouyang, D. Artificial Intelligence in Computer Vision: Cardiac MRI and Multimodality Imaging Segmentation. Curr Cardiovasc Risk Rep 15, (2021). [CrossRef]
- Wu, Y., Tang, Z., Li, B., Firmin, D. & Yang, G. Recent Advances in Fibrosis and Scar Segmentation From Cardiac MRI: A State-of-the-Art Review and Future Perspectives. Front Physiol 12, (2021). [CrossRef]
- Alnasser, T. N. et al. Advancements in cardiac structures segmentation: a comprehensive systematic review of deep learning in CT imaging. Front Cardiovasc Med 11, (2024). [CrossRef]
- Liang, J. et al. Second-generation motion correction algorithm improves diagnostic accuracy of single-beat coronary CT angiography in patients with increased heart rate. Eur Radiol 29, 4215–4227 (2019). [CrossRef]
- Sun, J. et al. Further improving image quality of cardiovascular computed tomography angiography for children with high heart rates using second-generation motion correction algorithm. J Comput Assist Tomogr 44, 790–795 (2020). [CrossRef]
- Joshi, M. et al. Current and Future Applications of Artificial Intelligence in Cardiac CT. Curr Cardiol Rep 25, 109–117 (2023). [CrossRef]
- Sun, Q. et al. Predictors of discordance between CT-derived fractional flow reserve (CT-FFR) and △CT-FFR in deep coronary myocardial bridging. Clin Imaging 114, 110264 (2024). [CrossRef]
- Zhang, D. et al. Quantitative computed tomography angiography evaluation of the coronary fractional flow reserve in patients with left anterior descending artery myocardial bridging. Clin Physiol Funct Imaging 44, 251–259 (2024). [CrossRef]
- Zhang, Z., Liu, Z., Hong, N. & Chen, L. Effect of a second-generation motion correction algorithm on image quality and measurement reproducibility of coronary CT angiography in patients with a myocardial bridge and mural coronary artery. Clin Radiol 79, e462–e467 (2024). [CrossRef]
- Zhou, F. et al. Diagnostic Performance of Machine Learning Based CT-FFR in Detecting Ischemia in Myocardial Bridging and Concomitant Proximal Atherosclerotic Disease. Can J Cardiol 35, 1523–1533 (2019). [CrossRef]
- Gijsen, F. et al. Expert recommendations on the assessment of wall shear stress in human coronary arteries: existing methodologies, technical considerations, and clinical applications. Eur Heart J 40, 3421–3433 (2019). [CrossRef]
- Stone, P. H. et al. Role of Low Endothelial Shear Stress and Plaque Characteristics in the Prediction of Nonculprit Major Adverse Cardiac Events. JACC Cardiovasc Imaging 11, 462–471 (2018). [CrossRef]
- Kumar, A. et al. High Coronary Shear Stress in Patients With Coronary Artery Disease Predicts Myocardial Infarction. J Am Coll Cardiol 72, 1926–1935 (2018). [CrossRef]
- Candreva, A. et al. Current and Future Applications of Computational Fluid Dynamics in Coronary Artery Disease. Rev Cardiovasc Med 23, (2022). [CrossRef]
- Wojtas, K., Kozłowski, M., Orciuch, W. & Makowski, Ł. Computational Fluid Dynamics Simulations of Mitral Paravalvular Leaks in Human Heart. Materials 14, 7354 (2021). [CrossRef]
- Fezzi, S. et al. Integrated Assessment of Computational Coronary Physiology From a Single Angiographic View in Patients Undergoing TAVI. Circ Cardiovasc Interv 16, E013185 (2023). [CrossRef]
- Javadzadegan, A. et al. Development of a Computational Fluid Dynamics Model for Myocardial Bridging. J Biomech Eng 140, (2018). [CrossRef]
- Sharma, P. et al. A framework for personalization of coronary flow computations during rest and hyperemia. Annu Int Conf IEEE Eng Med Biol Soc 2012, 6665–6668 (2012).
- Gulati, M. et al. 2021 AHA/ACC/ASE/CHEST/SAEM/SCCT/ SCMR Guideline for the Evaluation and Diagnosis of Chest Pain: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation 144, E368–E454 (2021).
- Bittl, J. A. et al. Putting the 2021 ACC/AHA/SCAI Guideline for Coronary Artery Revascularization Into Practice. JACC Case Rep 4, 31–35 (2022). [CrossRef]
- Neumann, F.-J. & Sousa-Uva, M. ‘Ten commandments’ for the 2018 ESC/EACTS Guidelines on Myocardial Revascularization. Eur Heart J 40, 79–80 (2019).
- Yang, S. et al. Long-term prognostic implications of CT angiography-derived fractional flow reserve: Results from the DISCOVER-FLOW study. J Cardiovasc Comput Tomogr 18, 251–258 (2024). [CrossRef]
- Nørgaard, B. L. et al. Diagnostic performance of noninvasive fractional flow reserve derived from coronary computed tomography angiography in suspected coronary artery disease: the NXT trial (Analysis of Coronary Blood Flow Using CT Angiography: Next Steps). J Am Coll Cardiol 63, 1145–1155 (2014).
- Rajiah, P., Cummings, K. W., Williamson, E. & Young, P. M. CT Fractional Flow Reserve: A Practical Guide to Application, Interpretation, and Problem Solving. RadioGraphics 42, 340–358 (2022). [CrossRef]
- Tesche, C. et al. Coronary CT Angiography–derived Fractional Flow Reserve. Radiology 285, 17–33 (2017). [CrossRef]
- Seetharam, K., Brito, D., Farjo, P. D. & Sengupta, P. P. The Role of Artificial Intelligence in Cardiovascular Imaging: State of the Art Review. Front Cardiovasc Med 7, 618849 (2020). [CrossRef]
- Martens, B., Michiels, V., J.-F., A. & Cosyns, B. Normalization of FFR<ovid:inf>CT</ovid:inf> after surgical unroofing of a myocardial bridge: a case report. Eur Heart J Case Rep 8, ytae005- (2024).
- Zhou, F. et al. Fractional flow reserve derived from CCTA may have a prognostic role in myocardial bridging. Eur Radiol 29, 3017–3026 (2019). [CrossRef]
- Zhou, F. et al. Machine Learning Using CT-FFR Predicts Proximal Atherosclerotic Plaque Formation Associated With LAD Myocardial Bridging. JACC Cardiovasc Imaging 12, 1591–1593 (2019). [CrossRef]
- Jubran, A. et al. Computed Tomographic Angiography-Based Fractional Flow Reserve Compared With Catheter-Based Dobutamine-Stress Diastolic Fractional Flow Reserve in Symptomatic Patients With a Myocardial Bridge and No Obstructive Coronary Artery Disease. Circ Cardiovasc Imaging 13, e009576- (2020). [CrossRef]
- Yu, Y., Yu, L., Dai, X. & Zhang, J. CT Fractional Flow Reserve for the Diagnosis of Myocardial Bridging-Related Ischemia: A Study Using Dynamic CT Myocardial Perfusion Imaging as a Reference Standard. Korean J Radiol 22, 1964–1973 (2021). [CrossRef]
- Chen, Y. C. et al. Coronary CTA-based vascular radiomics predicts atherosclerosis development proximal to LAD myocardial bridging. Eur Heart J Cardiovasc Imaging 25, 1462–1471 (2024). [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




