Submitted:
08 May 2025
Posted:
09 May 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Study Scope
2.3. Data Collection and Information Sources
2.4. Study Population
2.5. Inclusion and Exclusion Criteria:
2.5.1. Inclusion Criteria:
2.5.2. Exclusion Criteria:
2.6. Variables
2.7. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AF | Atrial Fibrillation |
| OAC | Oral Anticoagulants |
| ESC-EACTS Guidelines | Guidelines developed by the European Society of Cardiology (ESC) and the European Association for Cardio-Thoracic Surgery (EACTS) |
| GECATE | Acronym for “Gender perspective on cardiovascular diseases in the Terres de l'Ebre” |
| ICS | Acronym for “Catalan Health Institute” |
| EAPs | Acronym for “Primary Care teams” |
| HCC3 | Acronym for “Shared clinical record of Catalonia” |
| SIRE | Acronym for “Integrated Electronic Prescription System” |
| COPD | Chronic Obstructive Pulmonary Disease |
| BMI | Body Mass Index |
| OSAHS | Obstructive Sleep Apnea/Hypopnea Syndrome |
| VKAs | Vitamin K antagonists |
| NOACs | Non-vitamin K oral anticoagulants |
Appendix A
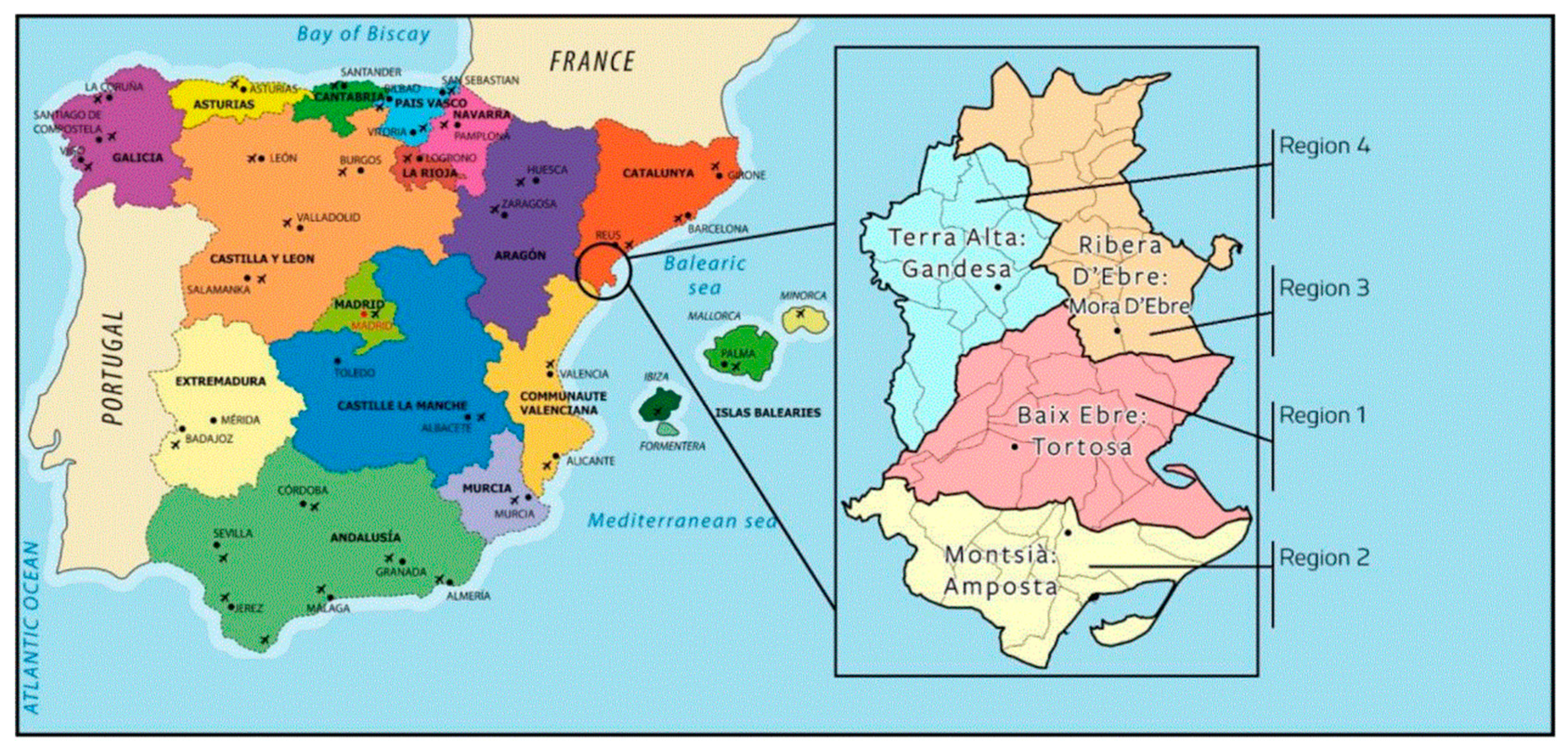
References
- van der Endt VHW, Milders J, Penning de Vries BBL, Trines SA, Groenwold RHH, Dekkers OM, Trevisan M, Carrero JJ, van Diepen M, Dekker FW, de Jong Y. Comprehensive comparison of stroke risk score performance: a systematic review and meta-analysis among 6 267 728 patients with atrial fibrillation. Europace. 2022 Nov 22;24(11):1739-1753. [CrossRef]
- {2]. Boriani G, Vitolo M, Mei DA. CHA2DS2-VA instead of CHA2DS2-VASc for stroke risk stratification in patients with atrial fibrillation: not just a matter of sex. Europace. 2024 Nov 1;26(11):euae281. [CrossRef]
- Kalarus Z, Mairesse GH, Sokal A, Boriani G, Średniawa B, Casado-Arroyo R, Wachter R, Frommeyer G, Traykov V, Dagres N, Lip GYH, Boersma L, Peichl P, Dobrev D, Bulava A, Blomström-Lundqvist C, de Groot NMS, Schnabel R, Heinzel F, Van Gelder IC, Carbucicchio C, Shah D, Eckardt L. Searching for atrial fibrillation: looking harder, looking longer, and in increasingly sophisticated ways. An EHRA position paper. Europace. 2023 Feb 8;25(1):185-198. Erratum in: Europace. 2024 Jun 3;26(6):euae167. doi: 10.1093/europace/euae167. [CrossRef]
- Wilkinson C, Wu J, Clegg A, Nadarajah R, Rockwood K, Todd O et al. Impact of oral anticoagulation on the association between frailty and clinical outcomes in people with atrial fibrillation: nationwide primary care records on treatment analysis. Europace 2022;24:1065–75.
- Yoshimura H, Providencia R, Finan C, Schmidt AF, Lip GYH. Refining the CHA2DS2VASc risk stratification scheme: shall we drop the sex category criterion? Europace. 2024 Nov 1;26(11):euae280. [CrossRef]
- Lip GYH, Teppo K, Nielsen PB. CHA2DS2-VASc or a non-sex score (CHA2DS2-VA) for stroke risk prediction in atrial fibrillation: contemporary insights and clinical implications. Eur Heart J. 2024 Sep 29;45(36):3718-3720. [CrossRef]
- Teppo K, Lip GYH, Airaksinen KEJ, Halminen O, Haukka J, Putaala J et al. Comparing CHA2DS2-VA and CHA2DS2-VASc scores for stroke risk stratification in patients with atrial fibrillation: a temporal trends analysis from the retrospective Finnish AntiCoagulation in Atrial Fibrillation (FinACAF) cohort. Lancet Reg Health Eur 2024;43:100967.
- Van Gelder IC, Rienstra M, Bunting KV, Casado-Arroyo R, Caso V, Crijns HJGM, De Potter TJR, Dwight J, Guasti L, Hanke T, Jaarsma T, Lettino M, Løchen ML, Lumbers RT, Maesen B, Mølgaard I, Rosano GMC, Sanders P, Schnabel RB, Suwalski P, Svennberg E, Tamargo J, Tica O, Traykov V, Tzeis S, Kotecha D; ESC Scientific Document Group. 2024 ESC Guidelines for the management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (EACTS). Eur Heart J. 2024 Sep 29;45(36):3314-3414. [CrossRef]
- Wu VC, Wu M, Aboyans V, Chang SH, Chen SW, Chen MC, Wang CL, Hsieh IC, Chu PH, Lin YS. Female sex as a risk factor for ischaemic stroke varies with age in patients with atrial fibrillation. Heart. 2020 Apr;106(7):534-540. [CrossRef]
- Rienstra M, Tzeis S, Bunting KV, Caso V, Crijns HJGM, De Potter TJR, Sanders P, Svennberg E, Casado-Arroyo R, Dwight J, Guasti L, Hanke T, Jaarsma T, Lettino M, Løchen ML, Lumbers RT, Maesen B, Mølgaard I, Rosano GMC, Schnabel RB, Suwalski P, Tamargo J, Tica O, Traykov V, Kotecha D, Van Gelder IC. Spotlight on the 2024 ESC/EACTS management of atrial fibrillation guidelines: 10 novel key aspects. Europace. 2024 Dec 3;26(12):euae298. [CrossRef]
- Ictus: Plan de Actuación en Europa (2018-2030). Ed Stroke Alliance for Europe (SAFE). 2018. www.safestroke.eu (accessed on 25 April 2025).
- Pla de salut de la Regió Sanitària Terres de l’Ebre 2021-2025. Tortosa: Direcció General de Planificació i Recerca en Salut;2022. https://scientiasalut.gencat.cat/handle/11351/7964 (accessed on 5 May 2025).
- Idescat. Indicadors Demogràfics i de Territori. Estructura per Edats, Envelliment i Dependència. Comarques i Aran. Available online: http://www.idescat.cat/pub/?id=inddt&n=915&by=com (accessed on 5 May 2025).
- Generalitat de Catalunya. Projeccions de Població Principals Resultats 2013–2051. 2008. Available online: https://www.idescat.cat/serveis/biblioteca/docs/cat/pp2021-2041pr.pdf (accessed on 25 April 2025).
- Alshehri AM. Stroke in atrial fibrillation: Review of risk stratification and preventive therapy. J Family Community Med. 2019 May-Aug;26(2):92-97. [CrossRef]
- Heidbuchel H, Van Gelder IC, Desteghe L; EHRA-PATHS Investigators. ESC and EHRA lead a path towards integrated care for multimorbid atrial fibrillation patients: the Horizon 2020 EHRA-PATHS project. Eur Heart J. 2022 Apr 14;43(15):1450-1452. [CrossRef]
- Steven Ho Man Lam, Giulio Francesco Romiti, Bernadette Corica, Tommaso Bucci, Brian Olshansky, Tze-Fan Chao, Menno V Huisman, Gregory Y H Lip, on behalf of the GLORIA-AF Investigators, Stroke risk stratifications according to CHA2DS2-VASc vs. CHA2DS2-VA in patients with Atrial Fibrillation: insights from the GLORIA-AF registry, European Heart Journal - Cardiovascular Pharmacotherapy, 2025;, pvaf031. [CrossRef]
- Clua-Espuny JL, Hernández-Pinilla A, Gentille-Lorente D, Muria-Subirats E, Forcadell-Arenas T, de Diego-Cabanes C, Ribas-Seguí D, Diaz-Vilarasau A, Molins-Rojas C, Palleja-Millan M, Satué-Gracia EM, Martín-Luján F; PREFATE Project-Group. Evidence Gaps and Lessons in the Early Detection of Atrial Fibrillation: A Prospective Study in a Primary Care Setting (PREFATE Study). Biomedicines. 2025 Jan 7;13(1):119. [CrossRef]
- Romiti, G.F., Corica, B., Mei, D.A. et al. Patterns of comorbidities in patients with atrial fibrillation and impact on management and long-term prognosis: an analysis from the Prospective Global GLORIA-AF Registry. BMC Med 22, 151 (2024). [CrossRef]
- Lip GYH, Teppo K, Nielsen PB. CHA2DS2-VASc or a non-sex score (CHA2DS2-VA) for stroke risk prediction in atrial fibrillation: contemporary insights and clinical implications. Eur Heart J. 2024 Sep 29;45(36):3718-3720. [CrossRef]
- Champsi A, Mobley AR, Subramanian A, Nirantharakumar K, Wang X, Shukla D, Bunting KV, Molgaard I, Dwight J, Arroyo RC, Crijns HJGM, Guasti L, Lettino M, Lumbers RT, Maesen B, Rienstra M, Svennberg E, Țica O, Traykov V, Tzeis S, van Gelder I, Kotecha D. Gender and contemporary risk of adverse events in atrial fibrillation. Eur Heart J. 2024 Sep 29;45(36):3707-3717. [CrossRef]
- Lu J, Hutchens R, Hung J, Bennamoun M, McQuillan B, Briffa T, Sohel F, Murray K, Stewart J, Chow B, Sanfilippo F, Dwivedi G. Performance of multilabel machine learning models and risk stratification schemas for predicting stroke and bleeding risk in patients with non-valvular atrial fibrillation. Comput Biol Med. 2022 Nov;150:106126. [CrossRef]
- Moltó-Balado, P.; Reverté-Villarroya, S.; Alonso-Barberán, V.; Monclús-Arasa, C.; Balado-Albiol, M.T.; Clua-Queralt, J.; Clua-Espuny, J.-L. Machine Learning Approaches to Predict Major Adverse Cardiovascular Events in Atrial Fibrillation. Technologies 2024, 12, 13. [Google Scholar] [CrossRef]
- Giner-Soriano M, Prat-Vallverdú O, Ouchi D, Vilaplana-Carnerero C, Morros R. Sex and gender differences in the use of oral anticoagulants for non-valvular atrial fibrillation: A population-based cohort study in primary health care in catalonia. Front Pharmacol. 2023 Feb 7;14:1110036. [CrossRef]
- Teppo K, Airaksinen KEJ, Jaakkola J, Halminen O, Salmela B, Kalatsova K, Kouki E, Haukka J, Putaala J, Linna M, Aro AL, Mustonen P, Hartikainen J, Lehto M. Temporal trends of gender disparities in oral anticoagulant use in patients with atrial fibrillation. Eur J Clin Invest. 2024 Jan;54(1):e14107. [CrossRef]
- Nielsen PB, Overvad TF. Female Sex as a Risk Modifier for Stroke Risk in Atrial Fibrillation: Using CHA2DS2-VASc versus CHA2DS2-VA for Stroke Risk Stratification in Atrial Fibrillation: A Note of Caution. Thromb Haemost. 2020 Jun;120(6):894-898. [CrossRef]
- Salmasi S, Loewen PS, Tandun R, Andrade JG, De Vera MA. Adherence to oral anticoagulants among patients with atrial fibrillation: a systematic review and meta-analysis of observational studies. BMJ Open. 2020 Apr 8;10(4):e034778. [CrossRef]
| Variables | Men | (%) | Women | (%) | p | ALL (%) |
|---|---|---|---|---|---|---|
| All (n %) | 19,531 | 48.7% | 20,548 | 51.3% | - | 40,077 |
| FA | 1,928 | 9.9% | 1,442 | 7.0% | < 0.001 | 3,370 (8.4%) |
| Age average | 77.28±6.56 | 77.6±6.63 | < 0.001 | 77.4±6.60 | ||
| CHA2DS2-VASc | 2.7±1.1 | 3.6±1.1 | < 0.001 | 3.2±1.2 | ||
| CHA2DS2-VA | 2.8±1.1 | 2.6±1.1 | < 0.001 | 2.68±1.1 | ||
| Heart failure | 1,790 | 9.2% | 1,558 | 7.6.·% | < 0.001 | 3,348 (8.4%) |
| Hypertension arterial | 11,526 | 59.0% | 12,218 | 59.5% | 0.360 | 23,744 (59.2%) |
| Age 65 to 74 years | 7,748 | 39.6% | 7,765 | 37.8% | < 0.001 | 15,513 (38.7%) |
| Age ≥75 years | 11,783 | 60.3% | 12,783 | 62.6% | < 0.001 | 24,566 (61.3%) |
| Diabetes mellitus | 5,763 | 29.5% | 4,498 | 21.9% | < 0.001 | 10,261 (25.6%) |
| Stroke/TIA/Systemic embolism | 843 | 4.7% | 724 | 3.5% | < 0.001 | 1567 (3.9%) |
| Vascular peripheral disease | 1,983 | 10.2% | 798 | 3.9% | < 0.001 | 2,781 (6.9%) |
| Ischemic cardiomyopathy | 2,073 | 10.6% | 917 | 4.5% | < 0.001 | 2,990 (7.5%) |
| BMI1 (kg/m2) | 28.1±4.5 | 28.4±5.7 | < 0.001 | 28.3±5.2 | ||
| Charlson index | 1.5±1.4 | 1.2±1.2 | < 0.001 | 1.38±1.9 | ||
| Dementia/cognitive impairment | 1,452 | 7.4% | 2,225 | 10.8% | < 0.001 | 3,677 (9.2%) |
| Pfeiffer score | 2.72±3.20 | 3.63±3.35 | < 0.001 | 3.23±3.3 | ||
| Chronic Kidney Disease | 3,181 | 16.3% | 3,080 | 15.0% | < 0.001 | 6,261 (15.6%) |
| Glomerular filtration rate (ml/min/1.73 m2) |
72.2±18.0 | 73.4±17.6 | < 0.001 | 72.9±17.7 | ||
| COPD2/asthma/bronchitis | 2,895 | 14,8% | 2,224 | 10.8% | < 0.001 | 5,119 (12.8%) |
| OSAHS3 | 966 | 4.9% | 473 | 2.3% | < 0.001 | 1,439 (3.6%) |
| Dyslipidemia | 8,394 | 43.0% | 10,623 | 51.7% | < 0.001 | 19,017 (47.5%) |
| Statins | 6,006 | 30.8% | 6,326 | 30.8% | 0.940 | 12,332 (30.8%) |
| Antiaggregants | 3,411 | 17.5% | 2,335 | 11.4% | < 0,001 | 5,746 (14.3%) |
| Anticoagulation | 1,977 | 10.1% | 1,468 | 7.1% | < 0.001 | 3,445 (8.6%) |
| Hospital visits | 0.36±1.3 | 0.27±0.95 | < 0.001 | 0.31±1,15 | ||
| Active medications | 5.17±4.3 | 5.76±4.40 | < 0.001 | 5.48±4.36 | ||
| Exitus | 14,492 | 74.2% | 17,173 | 83.6% | < 0.001 | 31,665 (79.0%) |
| Variables | Men | (%) | Women | (%) | p | ALL (%) |
|---|---|---|---|---|---|---|
| All (n %) | 1,928 | 57.2% | 1,442 | 42.8% | < 0.001 | 3,370 |
| Age average | 79.5±6.23 | 80.9±6.1 | < 0.001 | 80.1±6.24 | ||
| CHA2DS2-VASc | 3.58±1.18 | 4.51±1.12 | < 0.001 | 3.98±1.24 | ||
| CHA2DS2-VA | 3.58±1.18 | 3,51±1.12 | 0.071 | 3.55±1.16 | ||
| Heart failure | 690 | 35.8% | 543 | 37.7% | 0.278 | 1,233 (36.6%) |
| Hypertension arterial | 1,439 | 74.6% | 1,091 | 75.7% | 0.520 | 2,530 (75.1%) |
| Age 65 to 74 years | 460 | 23.8% | 246 | 17.1% | < 0.001 | 706 (20.94%) |
| Age ≥75 years | 1,468 | 76.1% | 1,196 | 82.9% | < 0.001 | 2,664 (79.1%) |
| Diabetes mellitus | 727 | 37.7% | 461 | 32.0% | 0.001 | 1,188 (35.3%) |
| Stroke/TIA/Systemic embolism | 194 | 10.1% | 137 | 9.5% | 0.599 | 331 (9.8%) |
| Vascular peripheral disease | 351 | 18.2% | 119 | 8.3% | < 0.001 | 470 (13.8%) |
| Ischemic cardiomyopathy | 375 | 19.5% | 162 | 11.2% | < 0.001 | 537 (15.8%) |
| BMI1 (kg/m2) | 29.07±5.1 | 28.53±6.2 | 0.022 | 29.2±5.5 | ||
| Charlson index | 2.27±1.5 | 1.91±1.38 | < 0.001 | 2.10±1.45 | ||
| Dementia/cognitive impairment | 196 | 10.2% | 212 | 14.7% | < 0.001 | 408 (12.1%) |
| Pfeiffer score | 2.14±2.7 | 3.31±3.0 | < 0.001 | 2.71±2.9 | ||
| Chronic Kidney Disease | 58155 | 30.1% | 417 | 28.9% | 0.446 | 998 (29.6%) |
| Glomerular filtration rate (ml/min/1.73 m2) |
65.5±20.0 | 64.7±19.8 | 0.356 | 65.16±19.9 | ||
| COPD3/asthma/bronchitis | 454 | 23.5% | 223 | 15.5% | < 0.001 | 677 (20.1%) |
| OSAHS2 | 170 | 8.8% | 54 | 3.7% | < 0.001 | 224 (6.6%) |
| Dyslipidemia | 933 | 48.4% | 774 | 53.7% | 0.002 | 1707 (50.7%) |
| Statins | 721 | 37.4% | 505 | 35.0% | 0.158 | 1,226 (36.4%) |
| Antiaggregants | 122 | 6.3% | 48 | 3.3% | < 0,001 | 170 (5.0%) |
| Anticoagulation VKAs4 NOACs5 |
1,522 492 1,030 |
78.9% 32.3% 67.6% |
1,140 378 762 |
79.0% 33.1% 66.8% |
0.9694 0.6810 0-6810 |
2,662 (78.9%) 870 (32.6%) 1,792 (67.3%) |
| Hospital visits | 0.68±1.7 | 0.58±1.51 | 0.070 | 0.64±1.64 | ||
| Active medications | 8.03±4.6 | 8.57±4.7 | 0.001 | 8.26±4.68 | ||
| Exitus | 1,445 | 74.9% | 1,125 | 78.0% | 0.095 | 2,570 (76.3%) |
| Tab | CHA2DS2VASc | CHA2DS2VA | |||||
| score | WOMEN N1 (%) |
MEN n1 (%) |
p | WOMEN N2 (%) |
MEN n2 (%) |
P | Total registered stroke |
| 1 | - | 61 (3.1%) | < 0.001 | 46 (3.2%) | 61 (3.1%) | 0.9549 | - |
| 2 | 46 (3.2%) | 276 (14.3%) | < 0.001 | 210 (14.5%) | 276 (14.3%) | 0.8784 | 10 (3.02%) |
| 3 | 210 (14.6%) | 593 (30.7%) | <0.001 | 459 (31.8%) | 593 (30.8%) | 0.5301 | 48 (14.50%) |
| 4 | 459 (31.8%) | 589 (30.5%) | 0.4489 | 481 (33.3%) | 589 (30.5%) | 0.0902 | 112 (33.83%) |
| 5 | 481 (33.5%) | 307 (15.9%) | < 0.001 | 183 (12.7%) | 307 (15.9%) | 0.0098 | 84 (25.37%) |
| 6 | 183 (12.6%) | 88 (4.5%) | < 0.001 | 58 (4.0%) | 88 (4.5%) | 0.4969 | 58 (17.52%) |
| 7 | 58 (4.0%) | 14 (0.7%) | < 0.001 | 5 (0.3%) | 14 (0.7%) | 0.2214 | 19 (5.74%) |
| 8 | 5 (0.3%) | - | 0.0327 | - | - | - | |
| 9 | - | - | - | - | - | ||
| Total | 1,442 (7.0%) | 1,928 (9.9%) | < 0.001 | 1,442 (7.0%) | 1,928 (9.9%) | < 0.001 | 331 |
| CHA2DS2VASc | CHA2DS2VA | |||||
| score | FA (N) |
Stroke (n) |
Incidence rate per 100 person-years CI95% | FA (N) |
Incidence rate per 100 person-years CI95% | Razon de tasas CI95% |
| 1 | 61 | - | 107 | - | ||
| 2 | 322 | 10 | 1.41 [0.68-2.59] | 486 | 0.93 [0.45-1.71] | 1.51 [0.63-3.64] |
| 3 | 803 | 48 | 2.80 [2.06-3.71] | 1052 | 2.16 [1.59-2.86] | 1.29 [0.86-1.93] |
| 4 | 1048 | 112 | 4.85 [3.99-5.83] | 1070 | 4.67 [3.85-5.62] | 1.03 [0.79-1.34] |
| 5 | 788 | 84 | 4.82 [3.84-5.96] | 490 | 7.58 [6.05-9.39] | 0.63 [0.46-0.85] |
| 6 | 271 | 58 | 9.49 [7.21-12.27] | 146 | 19.3 [14.68-24.99] | 0.49 [0.34-0.70] |
| 7 | 72 | 19 | 13.10 [7.89-20.46] | 19 | 50.0 [30.1-78.0] | 0.26 [0.13-0.49] |
| 8 | 5 | - | - | - | ||
| 9 | - | - | - | - | ||
| Total | 3370 | 331 | 4,51 [4.03-5.02] | 3370 | 4,51 [4.03-5.02] | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




