Submitted:
22 April 2025
Posted:
22 April 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Data Collection
2.2. Measures
2.3. Mental Health Assessment
2.3.1. Connor-Davidson Resilience Scale (CD-RISC 10)
2.3.2. Brief Resilience Coping Scale (BRCS)
2.3.3. The APGAR Family Scale
2.3.4. AUDIT-C Questionnaire
2.3.5. Generalized Anxiety Disorder-2 (GAD-2) and Patient Health Questionnaire-2 (PHQ-2)
2.3.6. Posttraumatic Stress Disorder (PTSD)-8
2.3.7. Subjective Happiness Scale (SHS)
2.4. Statistical Analysis
3. Results
3.1. Sample Characteristics
3.1.1. Sociodemographic Descriptive Data
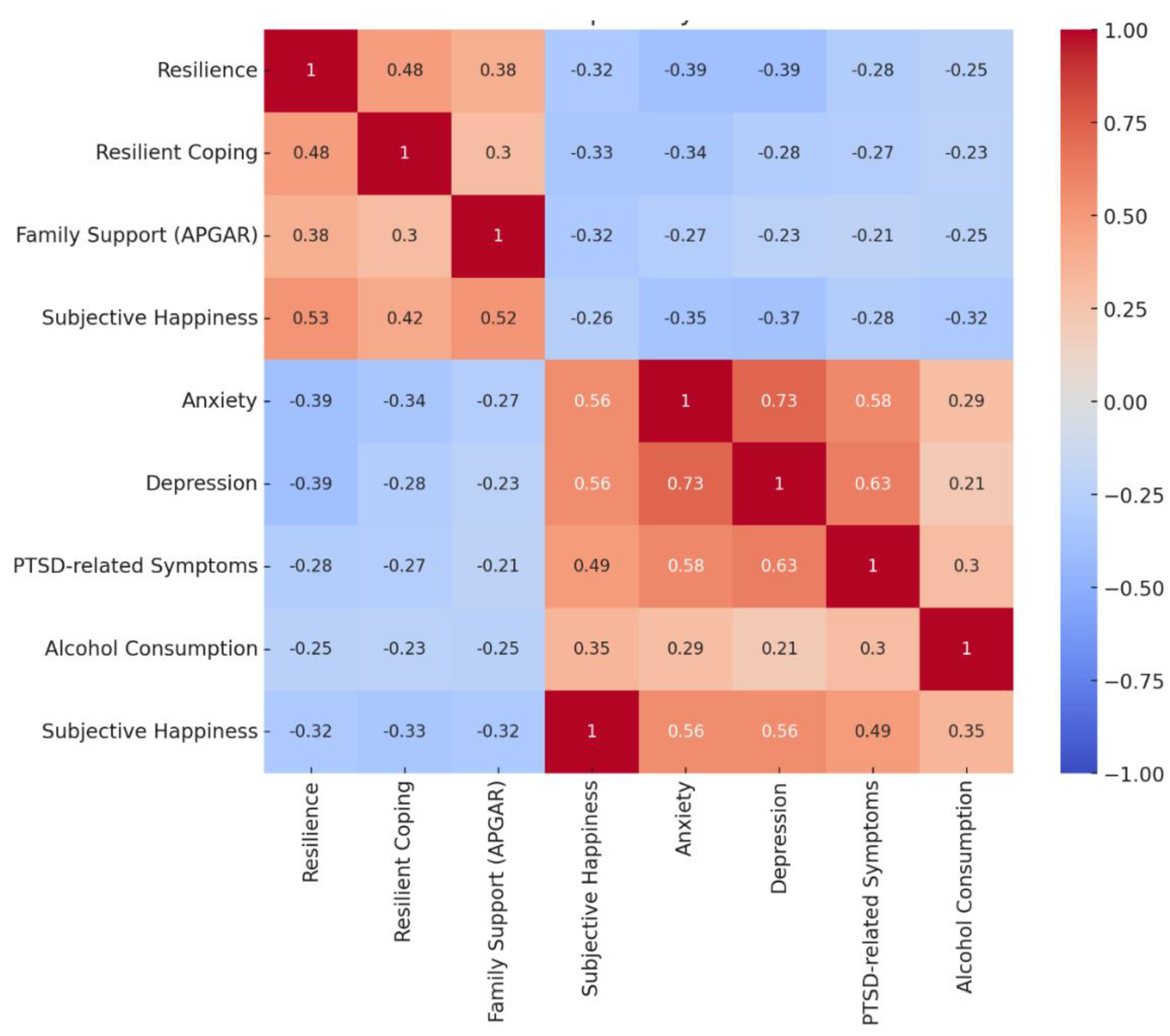
3.1.2. Bivariate Analysis
3.1.3. Factors Related to Armed Conflict Exposure
3.2. Normality Tests
3.3. Group Differences (Resilient vs. Non-Resilient Individuals)
3.4. Multivariate Analysis (MANOVA)
3.5. Predictive Models of Resilience
Interpretation of Odds Ratios, Model Fit, and Predictive Ability
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Bell, V., Méndez, F., Martínez, C., Palma, P. P., & Bosch, M. (2012). Characteristics of the Colombian Armed Conflict and the Mental Health of Civilians Living in Active Conflict Zones. Conflict and Health, 6, 1–8. [CrossRef]
- Restrepo, M. T., & Padilla-Medina, D. (2023). Armed conflict exposure and mental health: Examining the role of imperceptible violence. Medicine, Conflict and Survival, 39, 199–221. [CrossRef]
- Gómez-Restrepo, C., Tamayo-Martínez, N., Buitrago, G., Guarnizo-Herreño, C. C., Garzón-Orjuela, N., Eslava-Schmalbach, J., & Rincón, C. J. (2016). Violencia por conflicto armado y prevalencias de trastornos del afecto, ansiedad y problemas mentales en la población adulta colombiana. Revista Colombiana de Psiquiatría, 45(2), 147–153.
- Bonilla-Escobar, F. J., Osorio-Cuéllar, G. V., Pacichana-Quinayaz, S. G., Rangel-Gómez, A. N., Gomes-Pereira, L. D., Fandiño-Losada, A., & Gutiérrez-Martínez, M. I. (2021). Impacts of violence on the mental health of Afro-descendant survivors in Colombia. Medicine, Conflict and Survival, 37, 124–145. [CrossRef]
- Bonanno, G. A. (2004). Loss, trauma, and human resilience: Have we underestimated the human capacity to thrive after extremely aversive events? American Psychologist, 59(1), 20–28. [CrossRef]
- Masten, A. S. (2014). Global perspectives on resilience in children and youth. Child Development, 85(4), 1244–1259. [CrossRef]
- Adams, R. E., & Boscarino, J. A. (2006). Predictors of PTSD and delayed PTSD after disaster: The impact of exposure and psychosocial resources. Journal of Nervous and Mental Disease, 194(7), 485–493. [CrossRef]
- Benight, C. C., & Bandura, A. (2004). Social cognitive theory of posttraumatic recovery: The role of perceived self-efficacy. Behavior Research and Therapy, 42(10), 1129–1148. [CrossRef]
- Tol, W. A., Barbui, C., Galappatti, A., Silove, D., Betancourt, T. S., Souza, R., & Van Ommeren, M. (2011). Mental health and psychosocial support in humanitarian settings: Linking practice and research. The Lancet, 378(9802), 1581–1591. [CrossRef]
- Oviedo, L., Seryczyńska, B., Torralba, J., Roszak, P., Del Angel, J., Vyshynska, O., & Churpita, S. (2022). Coping and resilience strategies among Ukraine war refugees. International Journal of Environmental Research and Public Health, 19(20), 13094. [CrossRef]
- Gómez-Restrepo, C., Sarmiento-Suárez, M. J., Alba-Saavedra, M., Calvo-Valderrama, M. G., Rincón-Rodríguez, C. J., González-Ballesteros, L. M., & van Loggerenberg, F. (2023). Mental health problems and resilience in adolescents during the COVID-19 pandemic in a post-armed conflict area in Colombia. Scientific Reports, 13, 9743. [CrossRef]
- Connor, K. M., & Davidson, J. R. (2003). Development of a new resilience scale: The Connor-Davidson resilience scale (CD-RISC). Depression and Anxiety, 18(2), 76–82. [CrossRef]
- Notario-Pacheco, B., Martínez-Vizcaíno, V., Trillo-Calvo, E., Pérez-Yus, M. C., Serrano-Parra, D., & García-Campayo, J. (2014). Validity and reliability of the Spanish version of the 10-item Connor-Davidson Resilience Scale (CD-RISC-10) in patients with fibromyalgia. Health and Quality of Life Outcomes, 12, 14. [CrossRef]
- Bakic, H., & Ajdukovic, D. (2019). Stability and change post-disaster: Dynamic relations between individual, interpersonal, and community resources and psychosocial functioning. European Journal of Psychotraumatology, 10(1), 1614821. [CrossRef]
- Sinclair, V. G., & Wallston, K. A. (2004). The development and psychometric evaluation of the Brief Resilient Coping Scale. Assessment, 11(1), 94–101. [CrossRef]
- Limonero, J. T., Tomás-Sábado, J., Gómez-Romero, M. J., Maté-Méndez, J., Sinclair, V. G., Wallston, K. A., & Gómez-Benito, J. (2014). Evidence for validity of the Brief Resilient Coping Scale in a young Spanish sample. The Spanish Journal of Psychology, 17, E34. [CrossRef]
- Calderón, C., Lorenzo-Seva, U., Ferrando, P. J., Sorribes, E., Rodríguez-González, A., Obispo, B. M., & Jiménez-Fonseca, P. (2022). Measurement properties of the Spanish version of the Brief Resilient Coping Scale (BRCS) in cancer patients. International Journal of Clinical and Health Psychology, 22(3), 100313. [CrossRef]
- Arias, L. (1994). El APGAR familiar en el cuidado primario de salud. Colombia Médica, 25(1), 26-28.
- Smilkstein, G., Ashworth, C., & Montano, D. (1982). Validity and reliability of the family APGAR as a test of family function. Journal of Family Practice, 15(2), 303–311.
- Díaz-Cárdenas, S., Tirado-Amador, L., & Simancas-Pallares, M. (2017). Validez de constructo y confiabilidad de la APGAR familiar en pacientes odontológicos adultos de Cartagena, Colombia. Revista Universidad Industrial de Santander Salud, 49(4), 541–548.
- Smilkstein, G. (1978). The family APGAR: A proposal for a family function test and its use by physicians. Journal of Family Practice, 6(6), 1231–1239.
- Babor, T. F., Higgins-Biddle, J. C., Saunders, J. B., & Monteiro, M. G. (2001). Cuestionario de Identificación de los Trastornos debidos al Consumo de Alcohol (AUDIT). Organización Mundial de la Salud.
- Kroenke, K., Spitzer, R. L., & Williams, J. B. W. (2003). The PHQ-9: Validity of a brief depression severity measure. Journal of General Internal Medicine, 16(9), 606–613. [CrossRef]
- Errazuriz, A., Beltrán, R., Torres, R., & Passi-Solar, A. (2022). The validity and reliability of the PHQ-9 and PHQ-2 on screening for Major Depression in Spanish-speaking immigrants in Chile: A cross-sectional study. International Journal of Environmental Research and Public Health, 19(21), 13975. [CrossRef]
- Löwe, B., Kroenke, K., & Gräfe, K. (2005). Detecting and monitoring depression with a two-item questionnaire (PHQ-2). Journal of Psychosomatic Research, 58(2), 163–171. [CrossRef]
- Plummer, F., Manea, L., Trepel, D., & McMillan, D. (2016). Screening for anxiety disorders with the GAD-7 and GAD-2: A systematic review and diagnostic metaanalysis. General Hospital Psychiatry, 39, 24–31. [CrossRef]
- Andersen, T. E., Hansen, M., Ravn, S. L., Seehuus, R., Nielsen, M., & Vaegter, H. B. (2018). Validation of the PTSD-8 scale in chronic pain patients. Pain Medicine, 19(7), 1365-1372. [CrossRef]
- Forrest, W., & Steel, Z. (2023). The impact of immigration detention on the mental health of refugees and asylum seekers. Journal of Traumatic Stress, 36(3), 642–653. [CrossRef]
- Extremera, N., & Fernández-Berrocal, P. (2014). The Subjective Happiness Scale: Translation and preliminary psychometric evaluation of a Spanish version. Social Indicators Research, 119(1), 473–481. [CrossRef]
- Extremera, N., & Fernández-Berrocal, P. (2014). The Subjective Happiness Scale: Translation and preliminary psychometric evaluation of a Spanish version. Social Indicators Research, 119(1), 473–481. [CrossRef]
- Lyubomirsky, S., & Lepper, H. S. (1999). A measure of subjective happiness: Preliminary reliability and construct validation. Social Indicators Research, 46(2), 137–155. [CrossRef]
- Purgato, M., Tedeschi, F., Bonetto, C., de Jong, J., Jordans, M. J., Tol, W. A., & Barbui, C. (2020). Trajectories of psychological symptoms and resilience in conflict-affected children in low-and middle-income countries. Clinical Psychology Review, 82, 101935. [CrossRef]
- Meyer, E. C., Kotte, A., Kimbrel, N. A., DeBeer, B. B., Elliott, T. R., Gulliver, S. B., & Morissette, S. B. (2019). Predictors of lower-than-expected posttraumatic symptom severity in war veterans: The influence of personality, self-reported trait resilience, and psychological flexibility. Behavior Research and Therapy, 113, 1–8. [CrossRef]
- Zamora-Moncayo, E., Burgess, R. A., Fonseca, L., González-Gort, M., & Kakuma, R. (2021). Gender, mental health, and resilience in armed conflict: Listening to life stories of internally displaced women in Colombia. BMJ Global Health, 6, e005770. [CrossRef]
- Vera-Bachmann, D. (2015). Resiliencia, pobreza y ruralidad. Revista Médica de Chile, 143(5), 677–678. [CrossRef]
- Miller-Suchet, L., Camargo, N., Sangraula, M., Castellar, D., Diaz, J., Meriño, V., Chamorro Coneo, A. M., Chávez, D., Venegas, M., Cristobal, M., Bonz, A. G., Ramirez, C., Trejos Herrera, A. M., Ventevogel, P., Brown, A. D., Schojan, M., Greene, M. C. (2024). Comparing mediators and moderators of mental health outcomes from the implementation of Group Problem Management Plus (PM+) among Venezuelan refugees and migrants and Colombian returnees in Northern Colombia. International Journal of Environmental Research and Public Health, 21(5), 527. [CrossRef]
- Perdomo, M., Sánchez, F., & Blanco, A. (2021). Effects of a community resilience intervention program on victims of forced displacement: A case study. Journal of Community Psychology, 49(6), 1630–1647. [CrossRef]
- Özmete, E., & Pak, M. (2023). Family functioning and community resilience during the COVID-19 lockdown period in Turkey. Social Work in Public Health, 38(5-8), 437–449. [CrossRef]
- Nam, B., Kim, J. Y., DeVylder, J. E., & Song, A. (2016). Family functioning, resilience, and depression among North Korean refugees. Psychiatry Research, 245, 451–457. [CrossRef]
- Aldwin, C. M. (2009). Stress, coping, and development: An integrative perspective. Guilford Press.
- Cosco, T. D., Howse, K., & Brayne, C. (2017). Healthy ageing, resilience and wellbeing. Epidemiology and Psychiatric Sciences, 26(6), 579–583. [CrossRef]
- Wei, J., Gong, Y., Wang, X., Shi, J., Ding, H., Zhang, M., & Han, J. (2021). Gender differences in the relationships between different types of childhood trauma and resilience on depressive symptoms among Chinese adolescents. Preventive Medicine, 148, 106523. [CrossRef]
- Watters, E. R., Aloe, A. M., & Wojciak, A. S. (2021). Examining the associations between childhood trauma, resilience, and depression: A multivariate meta-analysis. Trauma, Violence, & Abuse, 24(1), 231–244. [CrossRef]
- Saghin, D., Lupchian, M. M., & Lucheș, D. (2022). Social cohesion and community resilience during the COVID-19 pandemic in northern Romania. International Journal of Environmental Research and Public Health, 19(8), 4587. [CrossRef]
- Nuwayhid, I., Zurayk, H., Yamout, R., & Cortas, C. S. (2011). Summer 2006 war on Lebanon: A lesson in community resilience. Global Public Health, 6(5), 505–519. [CrossRef]
- Wong, R., DeGraff, D. S., & Orozco-Rocha, K. (2023). Economic resources and health: A bi-directional cycle for resilience in old age. Journal of Aging and Health, 35(10), 767–780. [CrossRef]
- Weitzel, E. C., Glaesmer, H., Hinz, A., et al. (2023). Soziodemografische und soziale Korrelate selbstberichteter Resilienz im Alter – Ergebnisse der populationsbasierten LIFE-Adult-Studie. Bundesgesundheitsblatt - Gesundheitsforschung - Gesundheitsschutz, 66(4), 402–409. [CrossRef]
- Bonanno, G. A., & Westphal, M. (2024). The three axioms of resilience. Journal of Trauma and Stress, 37(5), 717–723. [CrossRef]
- Blanc, J., Rahill, G. J., Laconi, S., & Mouchenik, Y. (2016). Religious beliefs, PTSD, depression and resilience in survivors of the 2010 Haiti earthquake. Journal of Affective Disorders, 190, 697–703. [CrossRef]
- Cusack, S. E., Wright, A. W., & Amstadter, A. B. (2023). Resilience and alcohol use in adulthood in the United States: A scoping review. Preventive Medicine, 168, 107442. [CrossRef]
- Nielsen, B., & Andersen, K. (2022). Alkohol, angst og depression. Ugeskrift for Læger, 184, V10210816.
- Scheffer, M., Bockting, C. L., Borsboom, D., Cools, R., Delecroix, C., Hartmann, J. A., Kendler, K. S., van de Leemput, I., van der Maas, H. L. J., van Nes, E., Mattson, M., McGorry, P. D., & Nelson, B. (2024). A dynamical systems view of psychiatric disorders—theory: A review. JAMA Psychiatry, 81(6), 618–623. [CrossRef]
- Camargo, A., Olmos, J., Higuera-Dagovett, E., Vargas, R., & Barreto, R. (2019). Papel de los profesionales de la salud en el diseño, obtención y entendimiento del consentimiento informado: Una revisión. Revista U.D.C.A Actualidad & Divulgación Científica, 22(2), e1164. [CrossRef]
| Variable | Kolmogorov-Smirnov (p-value) | Shapiro-Wilk (p-value) |
|---|---|---|
| Resilience | 0.200 | 0.156 |
| APGAR Family Support | 0.003 | 0.002 |
| Anxiety | 0.000 | 0.000 |
| Depression | 0.000 | 0.000 |
| Subjective Happiness | 0.001 | 0.001 |
| Variable | Resilient (M ± SD) | Non-Resilient (M ± SD) | F-value | p-value | η² parcial |
|---|---|---|---|---|---|
| APGAR | 15.60 ± 4.469 | 12.10 ± 5.434 | 17.749 | <0.001 | 0.082 |
| Anxiety | 1.21 ± 1.419 | 2.16 ± 1.771 | 12.518 | 0.001 | 0.059 |
| Depression | 1.09 ± 1.535 | 1.90 ± 1.538 | 10.644 | 0.001 | 0.051 |
| Subjective Happiness | 21.51 ± 4.685 | 16.98 ± 5.603 | 27.649 | <0.001 | 0.123 |
| Predictor | Exp(B) | p-value |
|---|---|---|
| Resilient Coping | 0.772 | <0.001 |
| Subjective Happiness | 0.864 | 0.001 |
| Anxiety | 1.447 | 0.010 |
| Alcohol Consumption | 0.813 | 0.014 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




