Submitted:
01 April 2025
Posted:
03 April 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
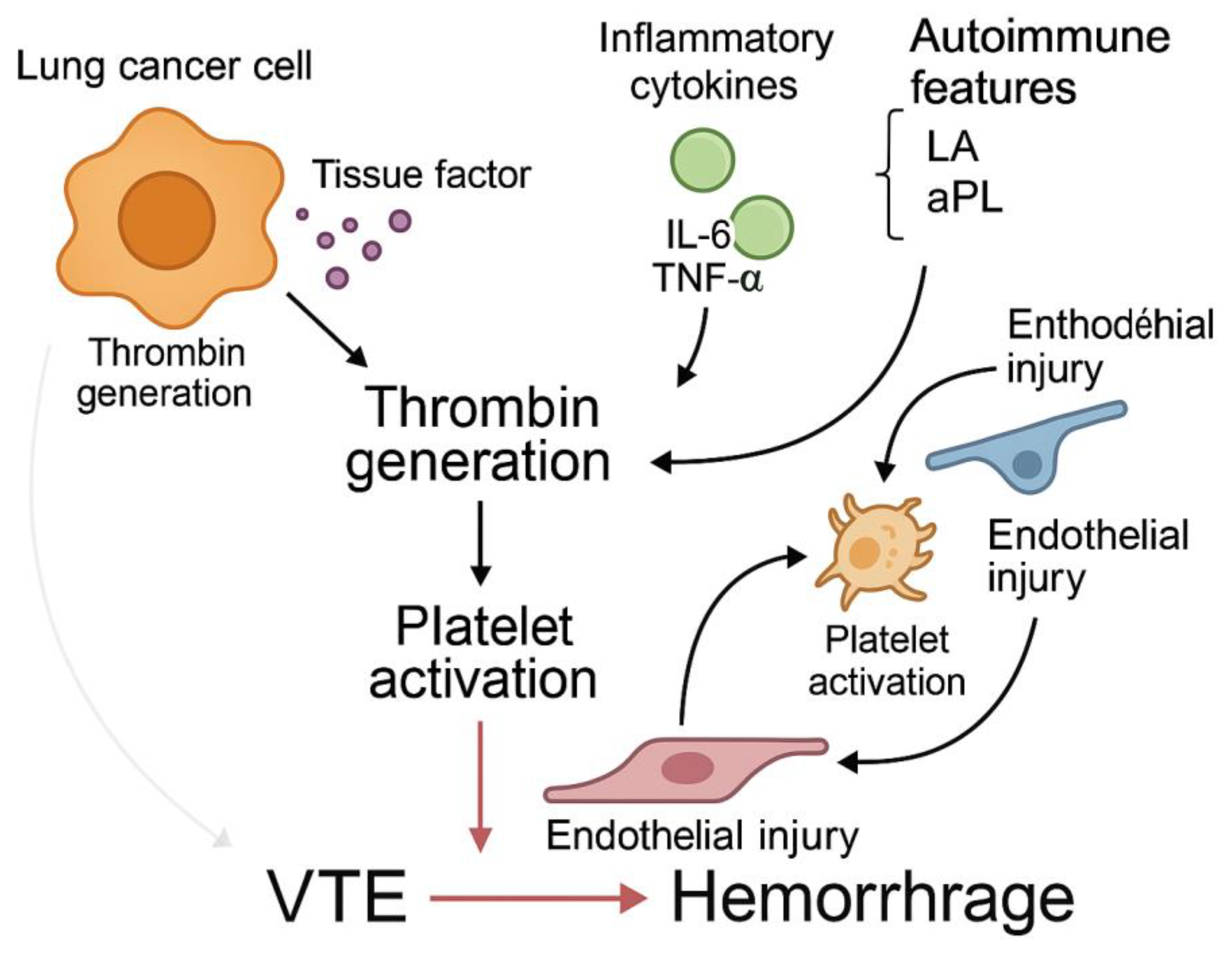
2. Mechanisms of Hypercoagulability in Lung Cancer
2.1. Tumor-Derived Procoagulants
2.2. Inflammatory Cytokine Activation
2.3. Endothelial Dysfunction and Platelet Activation
2.4. Autoimmunity and Acquired Inhibitors
2.5. Treatment-Related Risks
3. Diagnostic Strategies in Cancer-Associated Coagulopathy
3.1. Laboratory Assessment
3.2. Biomarker Evaluation
3.3. Imaging Modalities
4. Management of Coagulation Abnormalities
4.1. Anticoagulation in Lung Cancer
4.2. Management of Acquired Coagulation Inhibitors
4.3. Multidisciplinary Monitoring and Follow-Up
5. Conclusion and Future Directions
5.1. Clinical Integration: Practical Recommendations
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| VTE | venous thromboembolism |
| DVT | deep vein thrombosis |
| PE | pulmonary embolism |
| CAT | cancer-associated thrombosis |
References
- Siegel RL, Miller KD, Fuchs HE, Jemal A. Cancer statistics, 2023. CA Cancer J Clin. 2023;73(1):17–48. [CrossRef]
- Khorana AA, Kuderer NM, Culakova E, et al. Development and validation of a predictive model for chemotherapy-associated thrombosis. Blood. 2008;111(10):4902–4907. [CrossRef]
- Tagalakis V, Kavan P, Zukor D, et al. Clinical predictors of venous thromboembolism in patients with cancer. Curr Oncol. 2022;29(1):13–24. PMID: 35069530.
- Varki A. Trousseau's syndrome: multiple definitions and multiple mechanisms. Blood. 2007;110(6):1723–1729. [CrossRef]
- Blom JW, Doggen CJ, Osanto S, Rosendaal FR. Malignancies, prothrombotic mutations, and the risk of venous thrombosis. JAMA. 2005;293(6):715–722. PMID: 15701913.
- Thaler J, Ay C, Pabinger I. Venous thromboembolism and cancer: a risk factor for poor prognosis in cancer patients. Semin Thromb Hemost. 2014;40(7):791–803. [CrossRef]
- Grilz E, Königsbrügge O, Posch F, et al. Cancer-associated thrombosis is associated with mortality in a prospective cohort study. Thromb Res. 2018;164(Suppl 1): S112–S117. PMID: 30100232.
- Caine GJ, Stonelake PS, Lip GY, Kehoe ST. The hypercoagulable state of malignancy: pathogenesis and current debate. Neoplasia. 2002;4(6):465–473. [CrossRef]
- Pengo V, Banzato A, Bison E, et al. What have we learned about antiphospholipid syndrome from patients presenting with isolated lupus anticoagulant? Autoimmun Rev. 2018;17(8):810–812. [CrossRef]
- Ay C, Dunkler D, Marosi C, et al. Prediction of venous thromboembolism in cancer patients. Blood. 2010;116(24):5377–5382. [CrossRef]
- Levi M, van der Poll T. Endothelial injury in sepsis. Intensive Care Med. 2013;39(10):1839–1842. [CrossRef]
- Kumar S, Kim CW, Simmons RD, Jo H. Role of flow-sensitive microRNAs in endothelial dysfunction and atherosclerosis: mechanosensitive athero-miRs. Arterioscler Thromb Vasc Biol. 2014;34(10):2206–2216. [CrossRef]
- Hisada Y, Mackman N. Tissue factor and cancer: regulation, tumor growth, and metastasis. Semin Thromb Hemost. 2019;45(4):385–395. PMID: 30810753.
- Tesselaar ME, Romijn FP, Van Der Linden IK, et al. Microparticle-associated tissue factor activity: a link between cancer and thrombosis? J Thromb Haemost. 2007;5(3):520–527. PMID: 17155953.
- Franchini M, Lippi G. Acquired factor VIII inhibitors. Blood. 2008;112(2):250–255. [CrossRef]
- Liu F, Song D, Xie H, et al. Interleukin-6, tumor necrosis factor-alpha, and interleukin-1 beta as diagnostic biomarkers for sepsis: a meta-analysis. PLoS One. 2016;11(7): e0159065. [CrossRef]
- Kwaan HC. Role of plasma plasminogen activator inhibitor-1 in vascular disease. Am J Med. 1992;92(6A):62S–68S. [CrossRef]
- Labelle M, Begum S, Hynes RO. Direct signaling between platelets and cancer cells induces an epithelial-mesenchymal-like transition and promotes metastasis. Cancer Cell. 2011;20(5):576–590. [CrossRef]
- Verbruggen B, Novakova I, Wessels H, et al. The Nijmegen modification of the Bethesda assay for factor VIII inhibitors: improved specificity and reliability. Thromb Haemost. 1995;73(2):247–251.
- Moore RA, Adel N, Riedel E, et al. High incidence of thromboembolic events in patients treated with cisplatin-based chemotherapy: a large retrospective analysis. J Clin Oncol. 2011;29(25):3466–3473. PMID: 21788568.
- Agnelli G, Becattini C, Meyer G, et al. Apixaban for the treatment of venous thromboembolism associated with cancer. N Engl J Med. 2020;382(17):1599–1607. PMID: 32320558.
- van Es N, Di Nisio M, Cesarman G, et al. Biomarkers for cancer-associated venous thromboembolism. J Thromb Haemost. 2022;20(2):375–385. PMID: 34770794.
- Mulder FI, Bosch FT, Young AM, et al. Validation of the Khorana score for prediction of VTE in cancer patients: a pooled analysis. Thromb Haemost. 2021;121(3):328–335. PMID: 32920774.
- Carrier M, Righini M, Wells PS, et al. Subsegmental pulmonary embolism diagnosed by CT: a systematic review and meta-analysis. Chest. 2010;138(6):1093–1099. PMID: 20424131.
- Lee AY, Peterson EA. Treatment of cancer-associated thrombosis. Blood. 2013;122(14):2310–2317. PMID: 23908473.
- Tiede A, Scharf RE, Werwitzke S, et al. Diagnosis and treatment of acquired hemophilia A: guidelines from the German, Austrian, and Swiss Thrombosis and Hemostasis Society. Blood. 2020;135(7):551–564. PMID: 31871163.
- Collins PW, Hirsch S, Baglin TP, et al. Acquired hemophilia A in the UK: a 2-year national surveillance study. Blood. 2007;109(5):1870–1877. PMID: 17047148.
- Yaoita K, Takasaki T, Ito S, et al. Large Cell Neuroendocrine Carcinoma with Acquired Hemophilia a Diagnosed by Endobronchial Biopsy: A Case Report. Cureus. 2024 Oct 1;16(10): e70623. PMID: 39483578; PMCID: PMC11526768. [CrossRef]
- Lahiri A, Maji A, Potdar PD, et al. Lung cancer immunotherapy: progress, pitfalls, and promises. Mol Cancer. 2023 Feb 21;22(1):40. PMID: 36810079; PMCID: PMC9942077. [CrossRef]
- Lyman GH. Thromboprophylaxis with low-molecular-weight heparin in medical patients with cancer. Cancer. 2009 Dec 15;115(24):5637-50. PMID: 19827150; PMCID: PMC3714853. [CrossRef]
| Mechanism | Key Features | Clinical Impact |
|---|---|---|
| Tumor-derived procoagulants | Tissue factor (TF) expression, microparticle release | Initiation of coagulation cascade, increased VTE risk |
| Inflammatory cytokines | IL-6, TNF-α, IL-1β upregulation; PAI-1 elevation | Enhanced thrombin generation, suppressed fibrinolysis |
| Endothelial dysfunction | ↓ Thrombomodulin/tPA; ↑ E-selectin, ICAM-1 | Promotes leukocyte and platelet adhesion, vascular inflammation |
| Platelet activation | Tumor–platelet interaction, VEGF-mediated stimulation | Platelet aggregation, tumor protection, immune evasion |
| Autoimmune features (LA) | Prolonged aPTT, lupus anticoagulant, antiphospholipid antibodies | Diagnostic complexity; risk of both thrombosis and bleeding |
| Treatment-related factors | Chemotherapy, immunotherapy, surgery | Exacerbates hypercoagulability, increases thrombotic/bleeding risk |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




