Submitted:
06 March 2025
Posted:
07 March 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
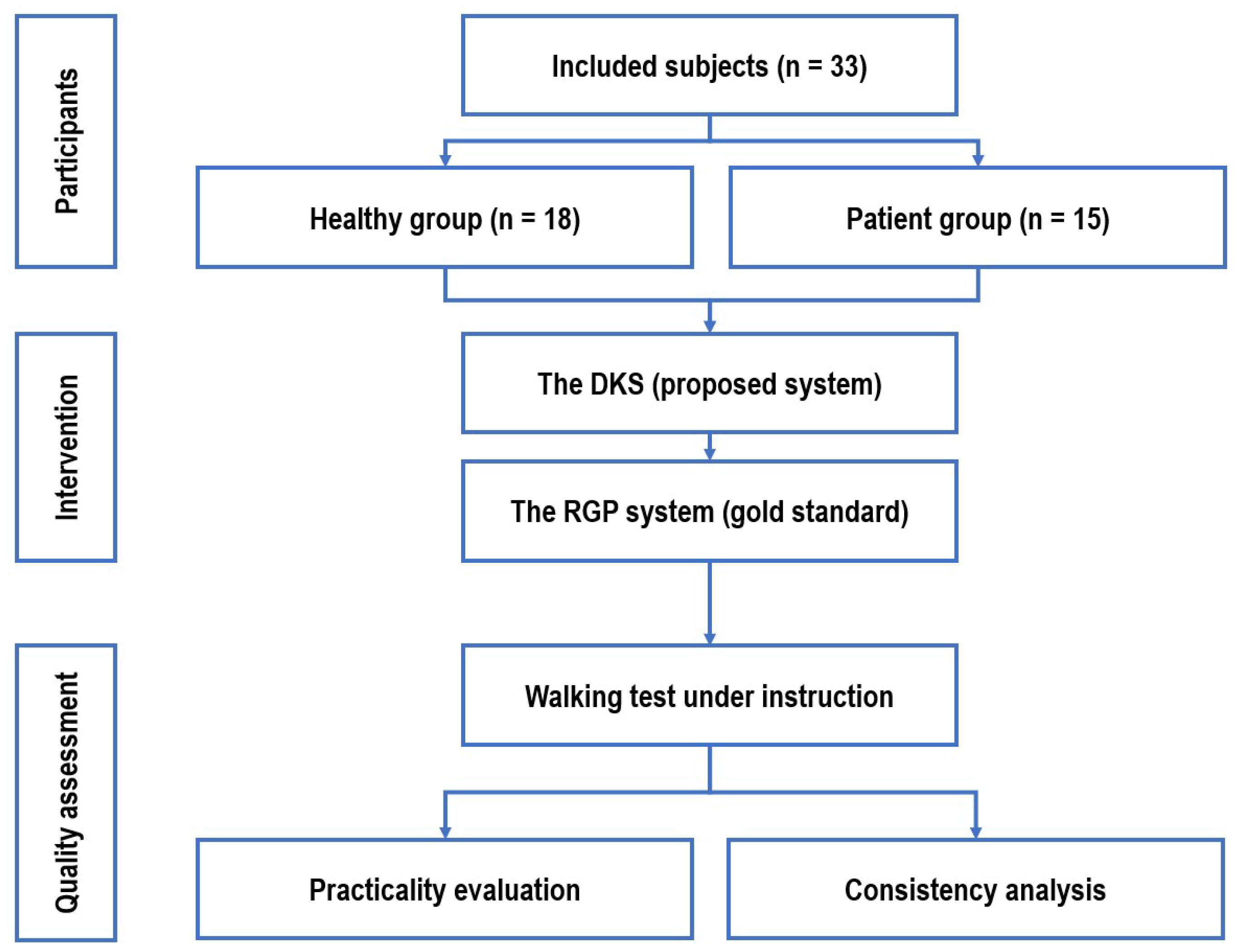
2.1. Participants
2.1.1. Inclusion Criteria
2.1.2. Exclusion Criteria
2.2. Apparatus
2.2.1. The Proposed Dual Kinect-V2 System (DKS)
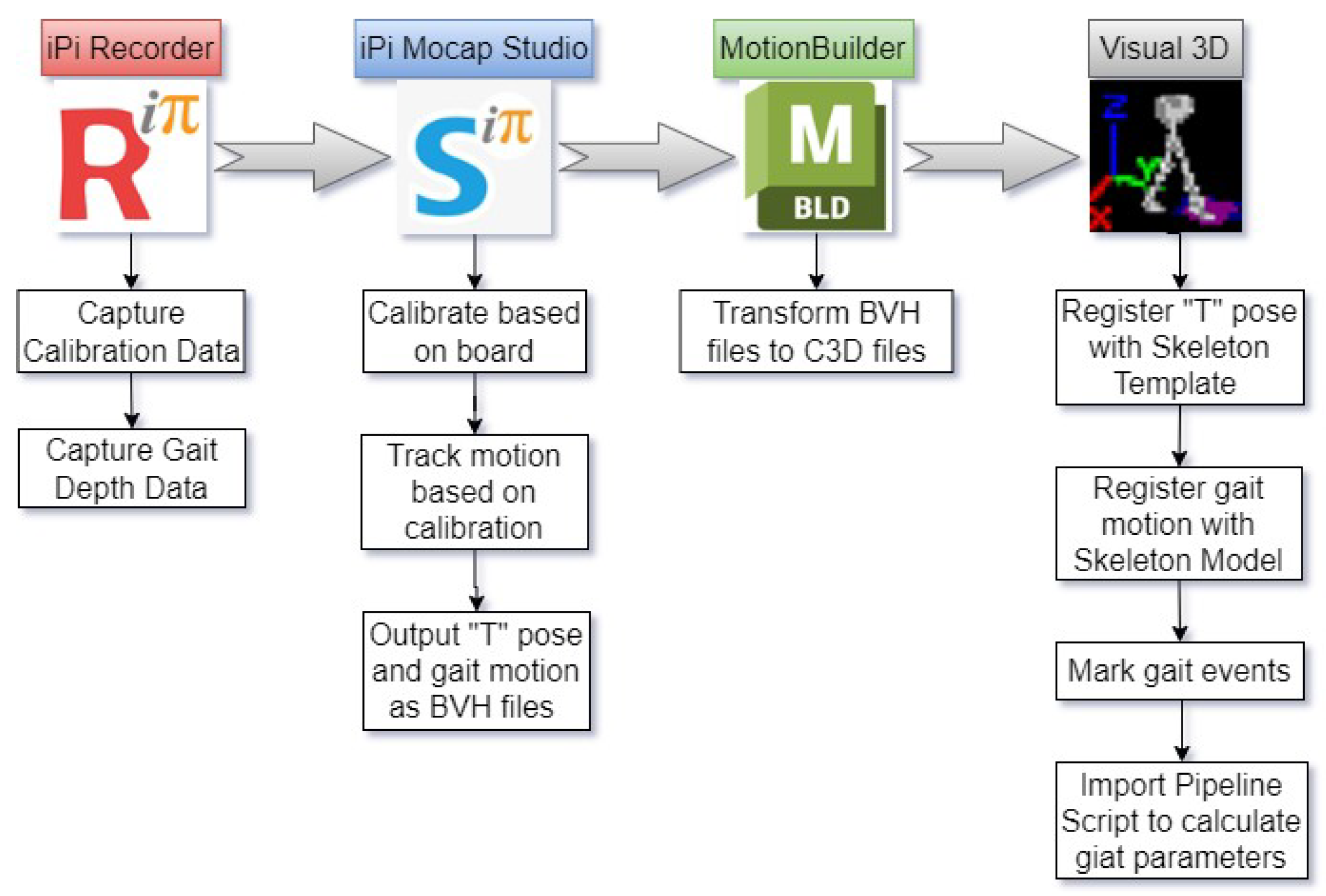
2.2.2. The Right Gait & Posture (RGP) System (Gold Standard)
2.3. Experimental Setup and Protocol
2.3.1. Experimental Setup
2.3.2. Testing Protocol
2.3.3. Data Collection and Comparison
2.4. Statistical analysis
3. Results
3.1. Participant Demography
3.2. Practicality Evaluation
3.3. Validation in the Healthy Group
3.4. Validation in the Patient Group
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| 10MWT | 10-Meter Walk Test |
| 2D | Two-Dimensional |
| 3D | Three-Dimensional |
| 95% LOA | Limits of Agreements |
| BVH | Biovision Hierarchy |
| CCC | Concordance Correlation Coefficients |
| DKS | Dual Kinect-V2 System |
| iNPH | Idiopathic Normal Pressure Hydrocephalus |
| PCC | earson’s correlation coefficien |
| POMA | Performance-Oriented Mobility Assessment |
| RGB | Red Green Blue |
| RGP | Right Gait & Posture |
| SDK | Software Development Kit |
| TUG | Timed Up and Go |
References
- Pirker, W.; Katzenschlager, R. Gait disorders in adults and the elderly: A clinical guide. Wiener Klinische Wochenschrift 2017, 129, 81–95. [Google Scholar] [PubMed]
- Osoba, M.Y.; Rao, A.K.; Agrawal, S.K.; Lalwani, A.K. Balance and gait in the elderly: A contemporary review. Laryngoscope investigative otolaryngology 2019, 4, 143–153. [Google Scholar] [PubMed]
- Mahlknecht, P.; Kiechl, S.; Bloem, B.R.; Willeit, J.; Scherfler, C.; Gasperi, A.; Rungger, G.; Poewe, W.; Seppi, K. Prevalence and burden of gait disorders in elderly men and women aged 60–97 years: a population-based study. PloS one 2013, 8, e69627. [Google Scholar]
- Stolze, H.; Klebe, S.; Baecker, C.; Zechlin, C.; Friege, L.; Pohle, S.; Deuschl, G. Prevalence of gait disorders in hospitalized neurological patients. Movement disorders: official journal of the Movement Disorder Society 2005, 20, 89–94. [Google Scholar]
- Jahn, K.; Zwergal, A.; Schniepp, R. Gait disturbances in old age: classification, diagnosis, and treatment from a neurological perspective. Deutsches Ärzteblatt International 2010, 107, 306. [Google Scholar]
- Kiprijanovska, I.; Gjoreski, H.; Gams, M. Detection of gait abnormalities for fall risk assessment using wrist-worn inertial sensors and deep learning. Sensors 2020, 20, 5373. [Google Scholar] [CrossRef]
- He, M.; Qi, Z.; Shao, Y.; Yao, H.; Zhang, X.; Zhang, Y.; Shi, Y.; E, Q.; Liu, C.; Hu, H.; et al. Quantitative evaluation of gait changes using APDM inertial sensors after the external lumbar drain in patients with idiopathic normal pressure hydrocephalus. Frontiers in Neurology 2021, 12, 635044. [Google Scholar]
- Relkin, N.; Marmarou, A.; Klinge, P.; Bergsneider, M.; Black, P.M. Diagnosing idiopathic normal-pressure hydrocephalus. Neurosurgery 2005, 57, S2–4. [Google Scholar]
- Gallagher, R.; Marquez, J.; Osmotherly, P. Clinimetric properties and minimal clinically important differences for a battery of gait, balance, and cognitive examinations for the tap test in idiopathic normal pressure hydrocephalus. Neurosurgery 2019, 84, E378–E384. [Google Scholar]
- Mori, E.; Ishikawa, M.; Kato, T.; Kazui, H.; Miyake, H.; Miyajima, M.; Nakajima, M.; Hashimoto, M.; Kuriyama, N.; Tokuda, T.; et al. Guidelines for management of idiopathic normal pressure hydrocephalus. Neurologia medico-chirurgica 2012, 52, 775–809. [Google Scholar]
- Petersen, G.; Ortega-Matute, E.; Perez-Nieto, D.; Inzunza, A.; Navarro, V.G. Diagnostic importance of disproportionately enlarged subarachnoid space hydrocephalus and Callosal Angle measurements in the context of normal pressure hydrocephalus: A useful tool for clinicians. Journal of the Neurological Sciences 2024, 466, 123250. [Google Scholar] [PubMed]
- Williams, M.A.; Malm, J. Diagnosis and treatment of idiopathic normal pressure hydrocephalus. Continuum: Lifelong Learning in Neurology 2016, 22, 579–599. [Google Scholar] [PubMed]
- Simon, S.R. Quantification of human motion: gait analysis—benefits and limitations to its application to clinical problems. Journal of biomechanics 2004, 37, 1869–1880. [Google Scholar] [PubMed]
- do Carmo Vilas-Boas, M.; Cunha, J.P.S. Movement quantification in neurological diseases: Methods and applications. IEEE reviews in biomedical engineering 2016, 9, 15–31. [Google Scholar]
- Bilney, B.; Morris, M.; Webster, K. Concurrent related validity of the GAITRite® walkway system for quantification of the spatial and temporal parameters of gait. Gait & posture 2003, 17, 68–74. [Google Scholar]
- Sharma, Y.; Cheung, L.; Patterson, K.K.; Iaboni, A.; et al. Factors influencing the clinical adoption of quantitative gait analysis technologies for adult patient populations with a focus on clinical efficacy and clinician perspectives: protocol for a scoping review. JMIR research protocols 2023, 12, e39767. [Google Scholar]
- Dubois, A.; Bresciani, J.P. Validation of an ambient system for the measurement of gait parameters. Journal of biomechanics 2018, 69, 175–180. [Google Scholar]
- Steinert, A.; Sattler, I.; Otte, K.; Röhling, H.; Mansow-Model, S.; Müller-Werdan, U. Using new camera-based technologies for gait analysis in older adults in comparison to the established GAITRite system. Sensors 2019, 20, 125. [Google Scholar] [CrossRef]
- Vilas-Boas, M.d.C.; Rocha, A.P.; Choupina, H.M.P.; Cardoso, M.N.; Fernandes, J.M.; Coelho, T.; Cunha, J.P.S. Validation of a single RGB-D camera for gait assessment of polyneuropathy patients. Sensors 2019, 19, 4929. [Google Scholar] [CrossRef]
- Ma, Y.; Mithraratne, K.; Wilson, N.C.; Wang, X.; Ma, Y.; Zhang, Y. The validity and reliability of a kinect v2-based gait analysis system for children with cerebral palsy. Sensors 2019, 19, 1660. [Google Scholar] [CrossRef]
- Summa, S.; Tartarisco, G.; Favetta, M.; Buzachis, A.; Romano, A.; Bernava, G.M.; Sancesario, A.; Vasco, G.; Pioggia, G.; Petrarca, M.; et al. Validation of low-cost system for gait assessment in children with ataxia. Computer methods and programs in biomedicine 2020, 196, 105705. [Google Scholar] [CrossRef] [PubMed]
- Springer, S.; Yogev Seligmann, G. Validity of the kinect for gait assessment: A focused review. Sensors 2016, 16, 194. [Google Scholar] [CrossRef] [PubMed]
- Usami, T.; Nishida, K.; Iguchi, H.; Okumura, T.; Sakai, H.; Ida, R.; Horiba, M.; Kashima, S.; Sahashi, K.; Asai, H.; et al. Evaluation of lower extremity gait analysis using Kinect V2® tracking system. SICOT-J 2022, 8, 27. [Google Scholar] [CrossRef] [PubMed]
- Oh, J.; Kuenze, C.; Jacopetti, M.; Signorile, J.F.; Eltoukhy, M. Validity of the Microsoft Kinect™ in assessing spatiotemporal and lower extremity kinematics during stair ascent and descent in healthy young individuals. Medical engineering & physics 2018, 60, 70–76. [Google Scholar]
- Guffanti, D.; Brunete, A.; Hernando, M.; Rueda, J.; Navarro Cabello, E. The accuracy of the Microsoft Kinect V2 sensor for human gait analysis. A different approach for comparison with the ground truth. Sensors 2020, 20, 4405. [Google Scholar] [CrossRef]
- Tanaka, R.; Kubota, T.; Yamasaki, T.; Higashi, A. Validity of the total body centre of gravity during gait using a markerless motion capture system. Journal of Medical Engineering & Technology 2018, 42, 175–181. [Google Scholar]
- Albert, J.A.; Owolabi, V.; Gebel, A.; Brahms, C.M.; Granacher, U.; Arnrich, B. Evaluation of the pose tracking performance of the azure kinect and kinect v2 for gait analysis in comparison with a gold standard: A pilot study. Sensors 2020, 20, 5104. [Google Scholar] [CrossRef]
- Tran, T.a.; Ruppert, T.; Eigner, G.; Abonyi, J. Assessing human worker performance by pattern mining of Kinect sensor skeleton data. Journal of Manufacturing Systems 2023, 70, 538–556. [Google Scholar] [CrossRef]
- Amdisen, A. Pearson’s correlation coefficient, p-value, and lithium therapy. Biological psychiatry 1987, 22, 926–928. [Google Scholar] [CrossRef]
- King, T.S.; Chinchilli, V.M.; Carrasco, J.L. A repeated measures concordance correlation coefficient. Statistics in medicine 2007, 26, 3095–3113. [Google Scholar] [CrossRef]
- Koo, T.K.; Li, M.Y. A guideline of selecting and reporting intraclass correlation coefficients for reliability research. Journal of chiropractic medicine 2016, 15, 155–163. [Google Scholar] [PubMed]
- Mehta, D.; Sridhar, S.; Sotnychenko, O.; Rhodin, H.; Shafiei, M.; Seidel, H.P.; Xu, W.; Casas, D.; Theobalt, C. Vnect: Real-time 3d human pose estimation with a single rgb camera. Acm transactions on graphics (tog) 2017, 36, 1–14. [Google Scholar] [CrossRef]
- Wallmann, H.W. Introduction to observational gait analysis. Home health care management & practice 2009, 22, 66–68. [Google Scholar]
- Rudisch, J.; Jöllenbeck, T.; Vogt, L.; Cordes, T.; Klotzbier, T.J.; Vogel, O.; Wollesen, B. Agreement and consistency of five different clinical gait analysis systems in the assessment of spatiotemporal gait parameters. Gait & posture 2021, 85, 55–64. [Google Scholar]
- Błażkiewicz, M. Muscle force distribution during forward and backward locomotion. Acta of Bioengineering and Biomechanics 2013, 15, 3–9. [Google Scholar]
- Naderi, S.; Mohammadipour, F.; Amir Seyfaddini, M.R. Kinematics of lower extremity during forward and backward walking on different gradients. Physical Treatments-Specific Physical Therapy Journal 2017, 7, 71–78. [Google Scholar]
- Yeung, L.F.; Yang, Z.; Cheng, K.C.C.; Du, D.; Tong, R.K.Y. Effects of camera viewing angles on tracking kinematic gait patterns using Azure Kinect, Kinect v2 and Orbbec Astra Pro v2. Gait & posture 2021, 87, 19–26. [Google Scholar]
- Jebeli, M.; Bilesan, A.; Arshi, A. A study on validating KinectV2 in comparison of Vicon system as a motion capture system for using in Health Engineering in industry. Nonlinear Engineering 2017, 6, 95–99. [Google Scholar] [CrossRef]



| Subgroup | Characteristics | Sex [M/F] | Age* [years] | Height* [cm] |
|---|---|---|---|---|
| Subgroup 1 | Healthy adults (n=9) | 5/4 | 30.67 ± 6.69 | 165.78 ± 9.36 |
| Subgroup 2 | Healthy older adults (n=9) | 5/4 | 69.67 ± 3.64 | 164.56 ± 7.16 |
| Idiopathic normal pressure hydrocephalus (n=7) | 4/3 | 69.29 ± 6.40 | 166.72 ± 4.53 | |
| Post-stroke mild hemiplegia (n=5) | 4/1 | 60.20 ± 12.11 | 170.40 ± 8.20 | |
| Subgroup 3 | Primary central nervous system vasculitis (n=1) | 1/0 | 38.00 | 184.00 |
| Syringomyelia (n=1) | 1/0 | 58.00 | 170.00 | |
| Paraneoplastic peripheral neuropathy (n=1) | 1/0 | 70.00 | 175.00 |
| Parameter | RGP* | DKS* | Mean Diff | 95% LoA | r | |
|---|---|---|---|---|---|---|
| Velocity [m/s] | 0.82 ± 0.15 | 0.83 ± 0.14 | -0.008 | -0.132 to 0.114 | 0.912 | 0.817 |
| L Velocity [m/s] | 0.80 ± 0.18 | 0.80 ± 0.16 | -0.001 | -0.177 to 0.174 | 0.863 | 0.765 |
| R Velocity [m/s] | 0.85 ± 0.13 | 0.86 ± 0.15 | -0.016 | -0.128 to 0.097 | 0.927 | 0.712 |
| L Cadence [step/min] | 87.01 ± 11.75 | 88.17 ± 11.93 | -1.163 | -7.169 to 4.843 | 0.967 | 0.882 |
| R Cadence [step/min] | 88.36 ± 11.61 | 85.76 ± 11.82 | 2.602 | -5.357 to 10.562 | 0.940 | 0.765 |
| Stride length [m] | 1.11 ± 0.13 | 1.14 ± 0.16 | -0.024 | -0.176 to 0.128 | 0.872 | 0.766 |
| L Step length [m] | 0.54 ± 0.09 | 0.55 ± 0.09 | -0.004 | -0.067 to 0.058 | 0.935 | 0.827 |
| R Step length [m] | 0.58 ± 0.08 | 0.58 ± 0.08 | 0.000 | -0.066 to 0.066 | 0.908 | 0.741 |
| Double-limb support phase [%] | 22.60 ± 2.24 | 22.63 ± 2.98 | -0.033 | -2.911 to 2.846 | 0.880 | 0.572 |
| Swing phase [%] | 38.49 ± 2.90 | 38.50 ± 2.66 | -0.017 | -2.817 to 2.784 | 0.871 | 0.603 |
| Stance phase [%] | 61.93 ± 2.73 | 62.00 ± 2.67 | -0.074 | -3.819 to 3.670 | 0.750 | 0.569 |
| Parameter | RGP* | DKS* | Mean Diff | 95% LoA | r | |
|---|---|---|---|---|---|---|
| Velocity [m/s] | 0.49 ± 0.25 | 0.47 ± 0.25 | 0.017 | -0.128 to 0.161 | 0.957 | 0.842 |
| L Velocity [m/s] | 0.49 ± 0.25 | 0.50 ± 0.30 | -0.003 | -0.209 to 0.203 | 0.941 | 0.733 |
| R Velocity [m/s] | 0.48 ± 0.25 | 0.44 ± 0.23 | 0.035 | -0.226 to 0.295 | 0.854 | 0.810 |
| L Cadence [step/min] | 81.79 ± 20.22 | 81.23 ± 20.64 | 0.563 | -6.395 to 7.521 | 0.985 | 0.943 |
| R Cadence [step/min] | 85.54 ± 13.87 | 84.65 ± 13.91 | 0.888 | -7.091 to 8.867 | 0.957 | 0.790 |
| Stride length [m] | 0.67 ± 0.25 | 0.65 ± 0.25 | 0.021 | -0.159 to 0.201 | 0.933 | 0.796 |
| L Step length [m] | 0.35 ± 0.13 | 0.35 ± 0.14 | 0.005 | -0.102 to 0.111 | 0.928 | 0.716 |
| R Step length [m] | 0.32 ± 0.14 | 0.31 ± 0.15 | 0.009 | -0.112 to 0.129 | 0.907 | 0.773 |
| Double-limb support phase [%] | 32.94 ± 9.23 | 27.62 ± 6.62 | 5.324 | -7.293 to 17.941 | 0.717 | 0.524 |
| Swing phase [%] | 28.35 ± 8.41 | 30.89 ± 8.08 | -2.539 | -14.906 to 9.828 | 0.708 | 0.352 |
| Stance phase [%] | 71.65 ± 8.41 | 69.31 ± 8.30 | 2.333 | -9.976 to 14.643 | 0.717 | 0.421 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




