Submitted:
06 March 2025
Posted:
06 March 2025
You are already at the latest version
Abstract
Head and neck squamous cell carcinoma (HNSCC) poses a major challenge for global healthcare due to its high rates of mortality and morbidity. While radiotherapy remains a primary treatment option, its effectiveness can vary due to tumor heterogeneity. Advanc-es in artificial intelligence (AI) have enabled the application of radiomics to enhance cancer prognosis predictions. Method: This study proposes a stacking ensemble learning approach combined with deep learning models to predict prognosis in HNSCC patients. We utilized a dataset comprising 215 CT images with contoured Gross Tumor Volume (GTV) and Planning Target Volume (PTV) from HNSCC patients. Radiomics features were extracted and analyzed using a stacking ensemble machine learning (SEML) model, while deep learning machine learning (DLML) models were used to optimize prediction performance. Result: Our results indicated that the SEML model outperformed the DLML model in predicting prognosis outcomes, achieving an accuracy of 93%, sensitivity of 100%, and specificity of 83%. No significant difference was found between PTV and GTV for prediction performance (chi-square test, p > 0.05). Conclusion: This study highlights the effectiveness of the SEML model in improving prognostic accuracy for HNSCC pa-tients, with implications for enhancing clinical decision-making and personalizing treatment strategies.
Keywords:
1. Introduction
2. Methodology
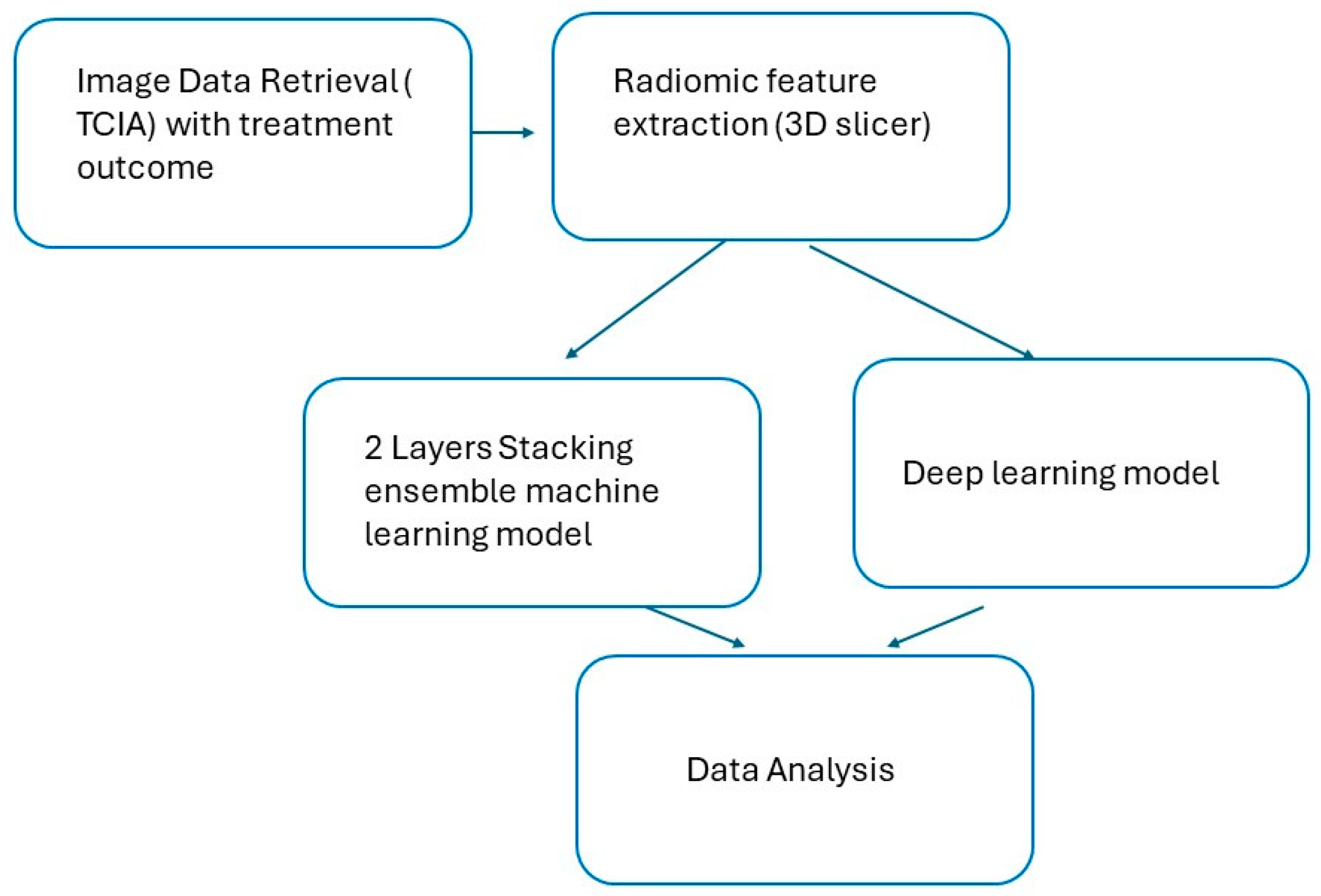
2.1. Research Workflow
2.2. Patient Data
2.3. Machine Learning Models
2.4. Machine Learning Process
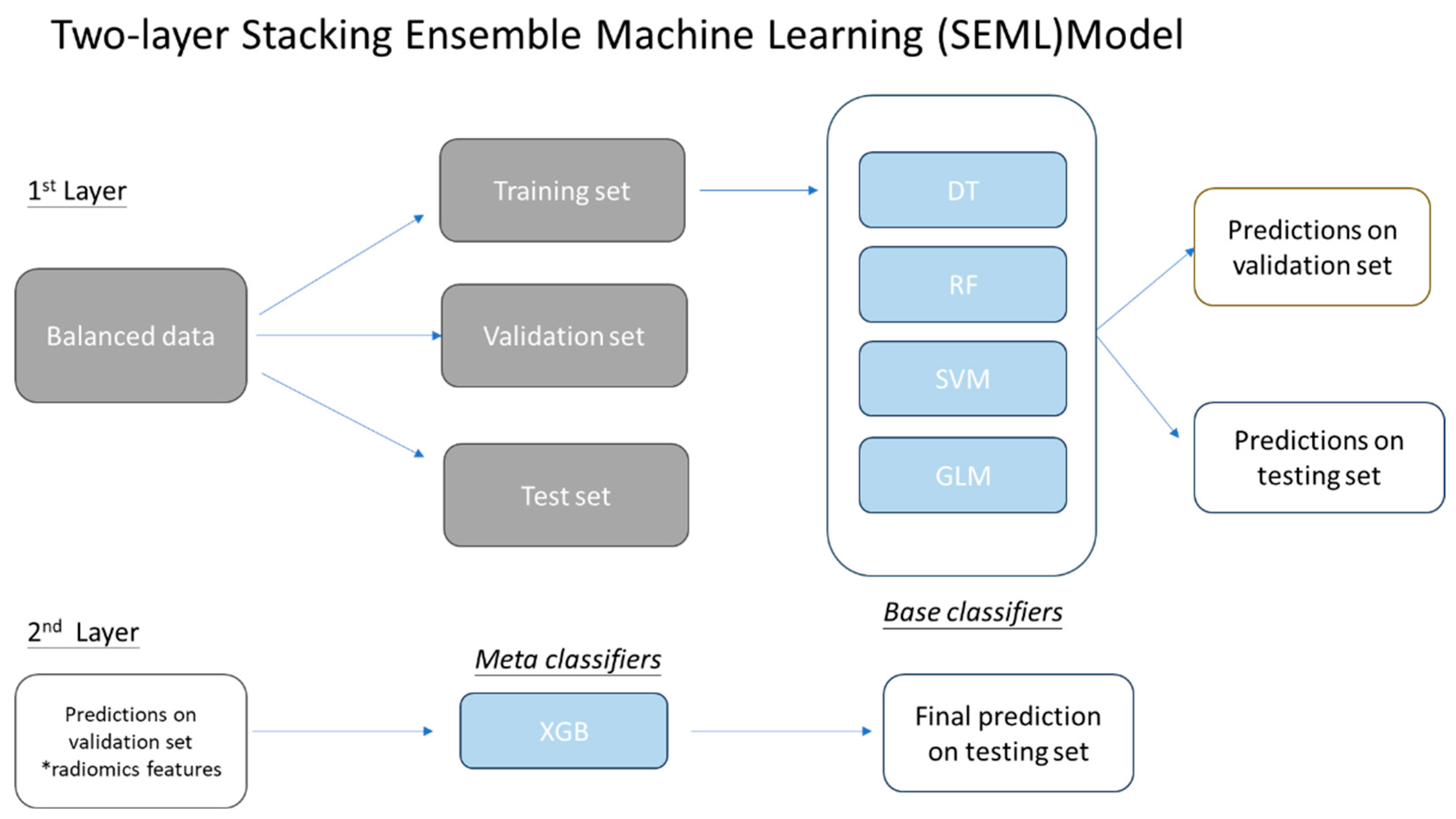
2.4.1. Two-layer Stacking Ensemble Machine Learning (SEML) Model
2.4.2. Overfitting Test
2.4.3. Deep Learning Machine Learning Models (DLML)
2.5. Data Analysis
3. Results
3.1. Demographic Cohort
3.2. Prediction Performance of SEML and DLML Models
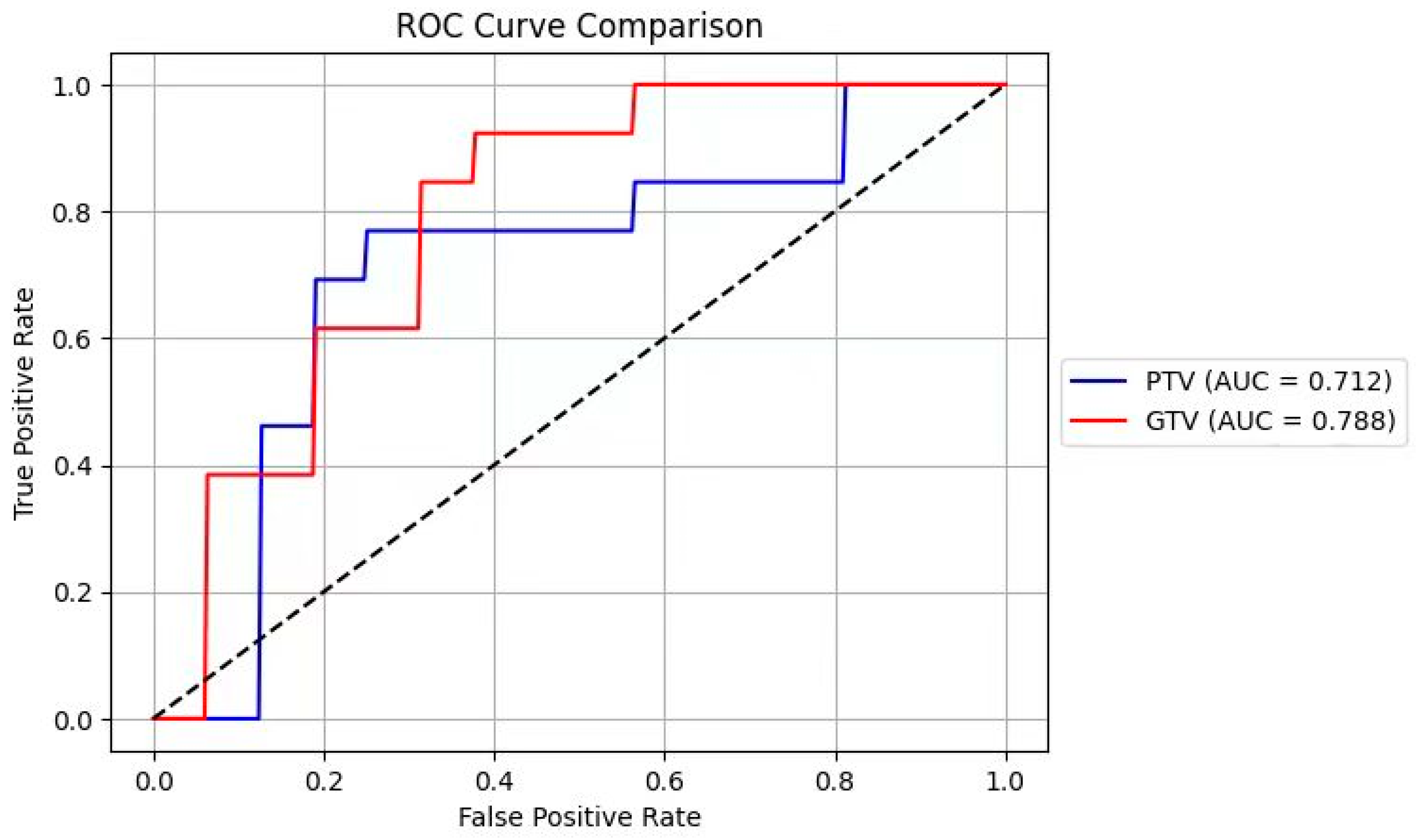
3.3. ROC Analysis
3.4. Comparison of SEML and DLML Models
4. Discussion
5. Conclusions
Author Contributions
Funding
Data Availability Statement
References
- Tsui, T., Cheung, K. M., Chow, J. C. H., & Wong, K. H. (2022). Risk Factors for Early Mortality in Head and Neck Cancer Patients Undergoing Definitive Chemoradiation. Hong Kong Journal of Radiology, 25(2), 127.
- Gormley M, Creaney G, Schache A, Ingarfield K, Conway DI. Reviewing the epidemiology of head and neck cancer: Definitions, trends and risk factors. Br Dent J 2022;233:780-786. [CrossRef]
- Huang S, Franc BL, Harnish RJ et al. Exploration of PET and MRI radiomic features for decoding breast cancer phenotypes and prognosis. NPJ Breast Cancer 2018;4:1-13. [CrossRef]
- Alabi, R. O., et al. (2021). Machine learning in oral squamous cell carcinoma: Current status, clinical concerns and prospects for future—A systematic review. Artificial Intelligence in Medicine, 115, 102060.
- Xiong, J., et al. (2018). The role of PET-based radiomic features in predicting local control of esophageal cancer treated with concurrent chemoradiotherapy. Scientific Reports, 8(1), 9902.
- Tang, F. H., et al. (2022). Radiomics from various tumour volume sizes for prognosis prediction of head and neck squamous cell carcinoma: a voted ensemble machine learning approach. Life, 12(9), 1380. [CrossRef]
- Feng, Y., et al. (2021). A heterogeneous ensemble learning method for neuroblastoma survival prediction. IEEE Journal of Biomedical and Health Informatics, 26(4), 1472-1483.
- Lui, V. W., et al. (2013). Frequent mutation of the PI3K pathway in head and neck cancer defines predictive biomarkers. Cancer Discovery, 3(7), 761-769.
- Yan, F., & Feng, Y. (2022). A two-stage stacked-based heterogeneous ensemble learning for cancer survival prediction. Complex Intelligent Systems, 8, 4619–4639. [CrossRef]
- Kumar, M., et al. (2022). Optimized stacking ensemble learning model for breast cancer detection and classification using machine learning. Sustainability, 14(21), 13998.
- Lee J, et al. (2023). Machine learning-based radiomics models for prediction of locoregional recurrence in patients with breast cancer. Oncology Letters, 26:1-10. [CrossRef]
- Zhao S, et al. (2023). Stacking ensemble learning-based [18F] FDG PET radiomics for outcome prediction in diffuse large B-cell lymphoma. J Nucl Med, 64:160-1609. [CrossRef]
- National Research Council. (2006). From Cancer Patient to Cancer Survivor: Lost in Transition. Washington, DC: The National Academies Press.
- Kwon, H., et al. (2019). Stacking ensemble technique for classifying breast cancer. Healthcare Informatics Research, 25(4), 283-288.
- Agarwal, A. (2020). Breast Cancer Prognosis Using Stacking Ensemble (Doctoral dissertation, State University of New York at Binghamton).
- Owusu DK, Nyarko PK. (2023). Stacked ensemble model for recurrent head and neck squamous cell carcinoma prognosis based on clinicopathologic and genomic markers. J Math Prob Equations Stat, 4:121-134.
- Marzorati, C., et al. (2017). Who is a cancer survivor? A systematic review of published definitions. Journal of Cancer Education, 32, 228-237.
- Parmar, C., et al. (2015). Radiomic machine-learning classifiers for prognostic biomarkers of head and neck cancer. Frontiers in Oncology, 5, 272.
- Chen, L., et al. (2020). Evaluation of CT-based radiomics signature and nomogram as prognostic markers in patients with laryngeal squamous cell carcinoma. Cancer Imaging, 20, 1-9. [CrossRef]
- ang FH, et al. (2021). Radiomics AI prediction for head and neck squamous cell carcinoma (HNSCC) prognosis and recurrence with target volume approach. BJR| Open, 3(1), 20200073.
- Bao D, et al. (2021). Prognostic and predictive value of radiomics features at MRI in nasopharyngeal carcinoma. Discov Oncol, 12:1-13. [CrossRef]
- Ching JCF, et al. (2023). Integrating CT-based radiomic model with clinical features improves long-term prognostication in high-risk prostate cancer. Front Oncol, 13:1-12. [CrossRef]
- Tang FH, et al. (2023). Radiomics-clinical AI model with probability weighted strategy for prognosis prediction in non-small cell lung cancer. Biomedicines, 11:1-12.

| Patient and Tumour Characteristics (All n = 164) |
Data |
|---|---|
| Age range (years) | 24–91 |
| Sex | |
| Female | 25 |
| Male | 139 |
| Staging | |
| Stage I | 3 |
| Stage II | 3 |
| Stage III | 23 |
| Stage IV | 135 |
| Diagnosis | |
| Ca Base of Tongue | 60 |
| Ca Tonsil | 58 |
| Ca others | 46 |
| Smoking status | |
| Smoker | 54 |
| Non-smoker | 110 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




