Submitted:
28 February 2025
Posted:
03 March 2025
You are already at the latest version
Abstract
Kidney transplantation constitutes a pivotal intervention for patients experiencing end-stage renal disease (ESRD), offering significant enhancements in quality of life and longevity relative to dialysis. However, the residual prevalence of erectile dysfunction (ED) in male recipients, affecting approximately 20-50%, signals a pressing concern in post-transplant health management. This review investigates the intricate interplay between hormonal fluctuations, specifically testosterone and thyroid hormones, and the psychosocial dynamics encompassing anxiety, depression, and overall quality of life in this demographic. It explores the multifaceted etiologies of ED, encompassing neurovascular, hormonal, and psychological dimensions that converge post-transplant. Further, the review critically examines current therapeutic strategies, emphasizing an integrated, multidisciplinary approach that simultaneously addresses hormonal disruptions, psychosocial factors, and metabolic disturbances. The primary objective is to bridge the existing knowledge gap regarding the pre- and post-transplant experiences of ED among male patients, thereby informing clinical practices aimed at optimizing sexual health outcomes and enhancing the overall well-being of kidney transplant recipients. Through rigorous evaluation of contemporary studies, this work underscores the necessity for comprehensive interventions that prioritize both physiological and psychological health in addressing ED within this vulnerable population.
Keywords:
Introduction:
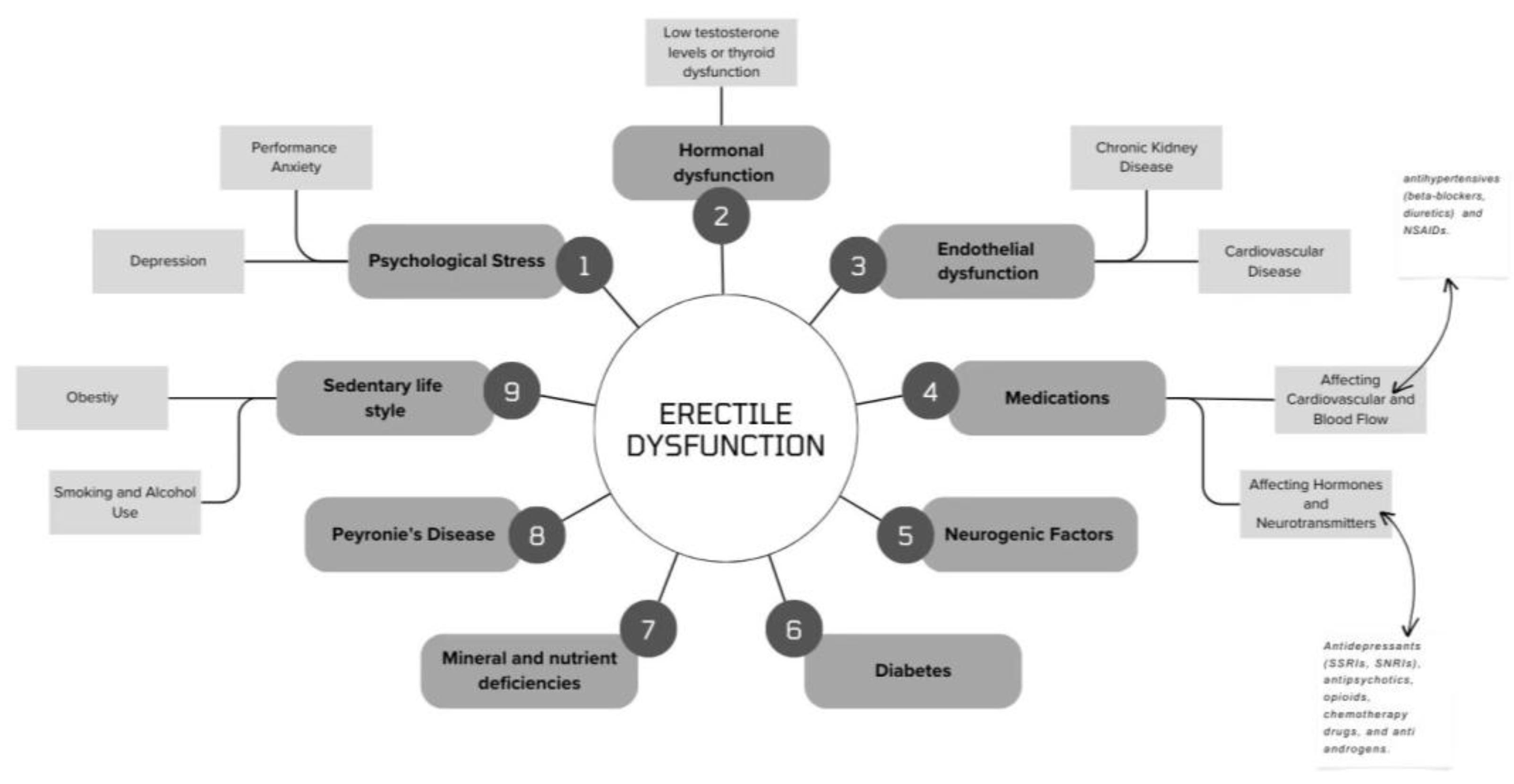
Pathophysiology of Erectile Dysfunction
Prevalence of Erectile Dysfunction
Comorbidities and Erectile dysfunction
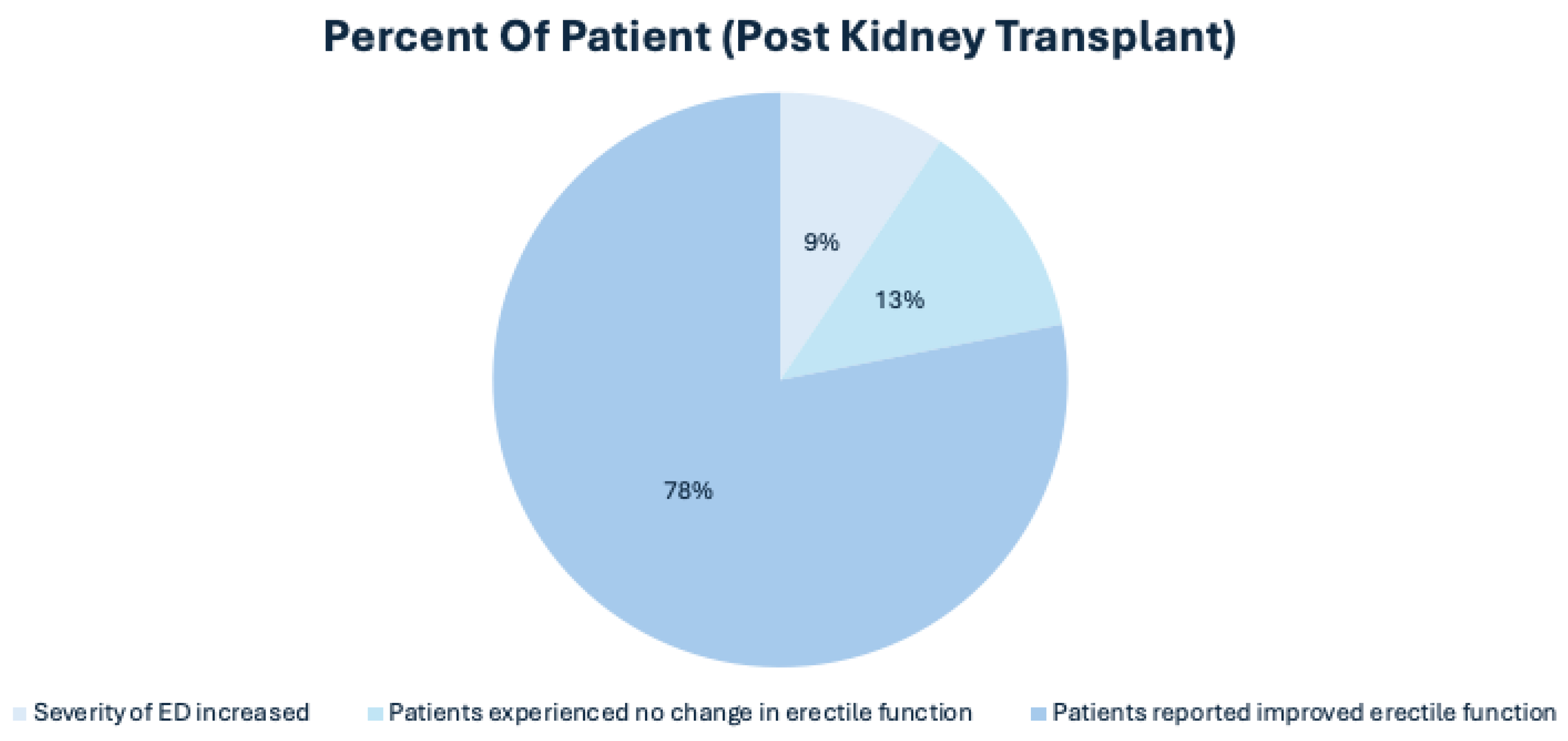
Erectile Dysfunction in Post-Transplant Patients
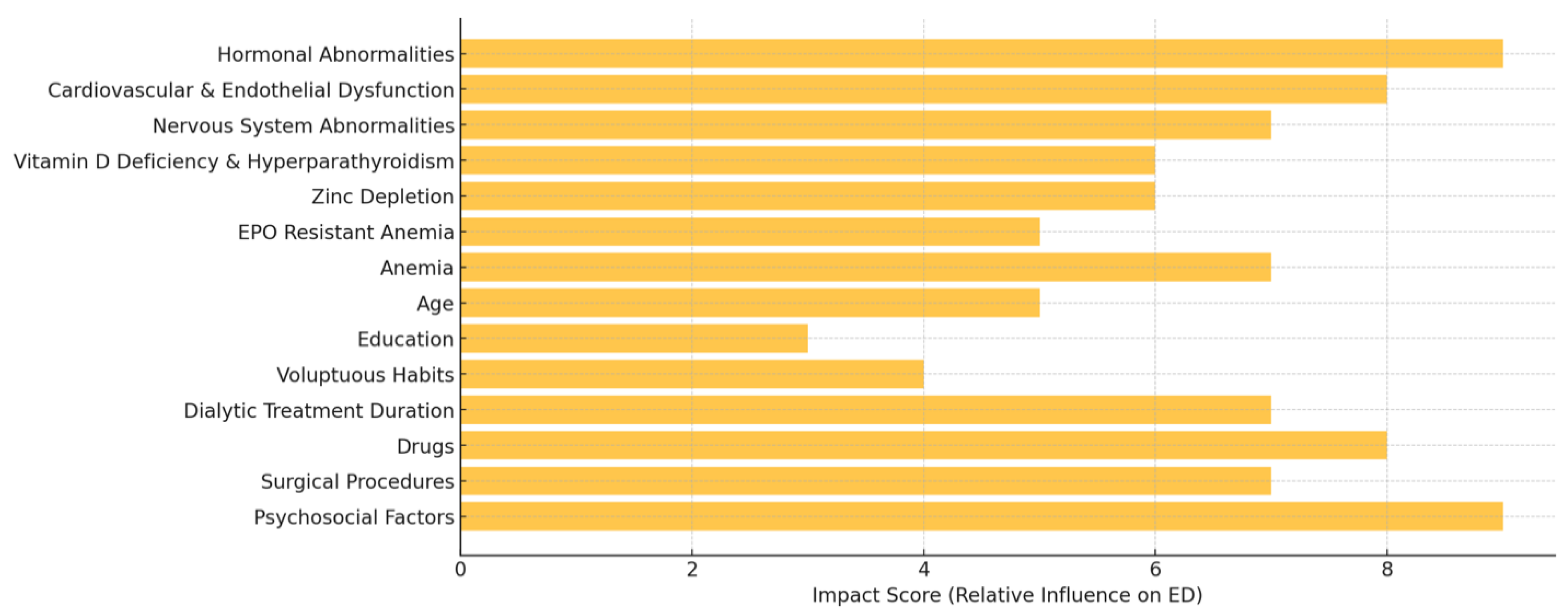
Medications and Nutritional Deficiencies Impacting Erectile Dysfunction in Post-Kidney Transplant Patients: Hormonal, Cardiovascular, and Neurogenic Factors
Current Therapeutic Approaches for Erectile Dysfunction in Post-Kidney Transplant Patients
Challenges and Future Directions
| Challenge | Key Issues | Research Gaps |
| Hormonal Therapy | Limited data on long-term TRT outcomes | Impact on rejection, metabolic health, CV risks |
| Psychosocial Factors | Anxiety, depression, body image concerns | Lack of transplant-specific interventions |
| Drug Interactions | TRT and immunosuppressants | Need for safety evaluations in transplant patients |
| Interdisciplinary Collaboration | Lack of coordinated care | Developing comprehensive care protocols |
Conclusion
Abbreviations:
| ED | Erectile Dysfunction |
| ESRD | (end-stage renal disease |
| KT | kidney transplantation |
| CKD | chronic kidney disease |
References
- Sharlip, I.D. Evaluation and nonsurgical management of erectile dysfunction. Urologic Clinics of North America 1998, 25, 647–659. [Google Scholar] [PubMed]
- Lewis, R.W.; et al. Definitions/epidemiology/risk factors for sexual dysfunction. J Sex Med 2010, 7 Pt 2, 1598–607. [Google Scholar] [PubMed]
- Shamloul, R.; Ghanem, H. Erectile dysfunction. Lancet 2013, 381, 153–65. [Google Scholar] [PubMed]
- Premužić, V.; Jelaković, B. ; Sexual dysfunction as a determinant of cardiovascular outcome in patients undergoing chronic hemodialysis. International Journal of Impotence Research 2018, 30, 14–20. [Google Scholar]
- Papadopoulou, E.; et al. Erectile dysfunction in chronic kidney disease: From pathophysiology to management. World Journal Of Nephrology 2015, 4, 379. [Google Scholar]
- Phé, V.; Rouprêt, M. Erectile dysfunction and diabetes: a review of the current evidence-based medicine and a synthesis of the main available therapies. Diabetes & metabolism 2012, 38, 1–13. [Google Scholar]
- Coban, S.; et al. , Does metabolic syndrome increase erectile dysfunction and lower urinary tract symptoms? Urology Journal 2014, 11, 1820–1824. [Google Scholar]
- Nunes, K.P.; Labazi, H.; Webb, R.C. ; New insights into hypertension-associated erectile dysfunction. Current opinion in nephrology and hypertension 2012, 21, 163–170. [Google Scholar]
- Bortolotti, A.; et al. , The epidemiology of erectile dysfunction and its risk factors. International journal of andrology 1998, 20, 323–334. [Google Scholar]
- Huri, H.Z.; et al. , Association of psychological factors, patients’ knowledge, and management among patients with erectile dysfunction. Patient preference and adherence 2016, 807–823. [Google Scholar]
- Fiuk, J.V.; Tadros, N.N. Erectile dysfunction in renal failure and transplant patients. Translational Andrology and Urology 2019, 8, 155. [Google Scholar] [PubMed]
- Salonia, A.; et al. European Association of Urology Guidelines on Sexual and Reproductive Health-2021 Update: Male Sexual Dysfunction. Eur Urol 2021, 80, 333–357. [Google Scholar] [PubMed]
- Laupacis, A.; et al. , A study of the quality of life and cost-utility of renal transplantation. Kidney international 1996, 50, 235–242. [Google Scholar] [PubMed]
- Rahman, I.A.; et al. , Effects of renal transplantation on erectile dysfunction: a systematic review and meta-analysis. International Journal of Impotence Research 2022, 34, 456–466. [Google Scholar]
- Jabali, S.S.; et al. Erectile dysfunction pre and post Kidney transplant recipients in Duhok city.
- Burnett, A.L. ; The role of nitric oxide in erectile dysfunction: implications for medical therapy. The Journal of Clinical Hypertension 2006, 8, 53–62. [Google Scholar]
- Manolis, A.; Doumas, M. ; Hypertension and sexual dysfunction. Archives of Medical Science Special Issues, 2009, 2009, 350–350. [Google Scholar]
- Leung, A.C.; Christ, G.J.; Melman, A. Physiology of penile erection and pathophysiology of erectile dysfunction. Atlas of Male Sexual Dysfunction 2004, 1–25. [Google Scholar]
- Manolis, A.; Doumas, M. ; Sexual dysfunction: the ‘prima ballerina’of hypertension-related quality-of-life complications. Journal of hypertension 2008, 26, 2074–2084. [Google Scholar]
- Steele, T.E.; et al. , Sexual experience of the chronic peritoneal dialysis patient. Journal of the American Society of Nephrology 1996, 7, 1165–1168. [Google Scholar]
- Levey, A.S.; et al. K/DOQI clinical practice guidelines for chronic kidney disease: evaluation, classification, and stratification. American Journal of Kidney Diseases 2002, 39 SUPPL. 1, i-ii+ S1-S266. [Google Scholar]
- Rebollo, P.; et al. , Factors associated with erectile dysfunction in male kidney transplant recipients. International journal of impotence research 2003, 15, 433–438. [Google Scholar] [CrossRef] [PubMed]
- Palmer, B.F. ; Outcomes associated with hypogonadism in men with chronic kidney disease. Advances in chronic kidney disease 2004, 11, 342–347. [Google Scholar] [CrossRef]
- Baylis, C. ; Arginine, arginine analogs and nitric oxide production in chronic kidney disease. Nature Clinical Practice Nephrology 2006, 2, 209–220. [Google Scholar] [CrossRef] [PubMed]
- Carrero, J.J.; et al. Testosterone deficiency is a cause of anaemia and reduced responsiveness to erythropoiesis-stimulating agents in men with chronic kidney disease. Nephrology Dialysis Transplantation 2012, 27, 709–715. [Google Scholar] [CrossRef]
- Dohle, G.R.; Elzanaty, S.; Van Casteren, N.J. Testicular biopsy: clinical practice and interpretation. Asian journal of andrology 2011, 14, 88. [Google Scholar] [CrossRef] [PubMed]
- Prem, A.; et al. , Male reproductive function in uraemia: efficacy of haemodialysis and renal transplantation. British journal of urology 1996, 78, 635–638. [Google Scholar] [CrossRef]
- Palmer, B.F. Sexual dysfunction in uremia. Journal of the American Society of Nephrology 1999, 10, 1381–1388. [Google Scholar] [CrossRef]
- Doumas, M.; et al. Factors affecting the increased prevalence of erectile dysfunction in Greek hypertensive compared with normotensive subjects. Journal of Andrology 2006, 27, 469–477. [Google Scholar] [CrossRef]
- Chang, S.W.; et al. The impact of diuretic therapy on reported sexual function. Archives of internal medicine 1991, 151, 2402–2408. [Google Scholar] [CrossRef]
- Rosen, R.C.; et al. The international index of erectile function (IIEF): a multidimensional scale for assessment of erectile dysfunction. Urology 1997, 49, 822–830. [Google Scholar] [CrossRef]
- Feldman, H.A.; et al. Erectile dysfunction and coronary risk factors: prospective results from the Massachusetts male aging study. Preventive medicine 2000, 30, 328–338. [Google Scholar]
- Messina, L.E.; et al. Erectile dysfunction in patients with chronic renal failure. International braz j urol 2007, 33, 673–678. [Google Scholar] [CrossRef] [PubMed]
- Türk, S.; et al. Quality of Life in Male Hemodialysis PatientsRole of Erectile Dysfunction. Nephron Clinical Practice 2004, 96, c21–c27. [Google Scholar] [PubMed]
- Mesquita, J.F.P.; et al. , Prevalence of erectile dysfunction in chronic renal disease patients on conservative treatment. Clinics 2012, 67, 181–183. [Google Scholar]
- Espinoza, R.; et al. Prevalence of erectile dysfunction in kidney transplant recipients. In Transplantation Proceedings; Elsevier, 2006. [Google Scholar]
- Rosas, S.E.; et al. Prevalence and determinants of erectile dysfunction in hemodialysis patients. Kidney international 2001, 59, 2259–2266. [Google Scholar]
- Cerqueira, J.; Moraes, M.; Glina, S. ; Erectile dysfunction: prevalence and associated variables in patients with chronic renal failure. International journal of impotence research 2002, 14, 65–71. [Google Scholar] [PubMed]
- Ponholzer, A.; et al. , Prevalence and risk factors for erectile dysfunction in 2869 men using a validated questionnaire. European urology 2005, 47, 80–86. [Google Scholar] [CrossRef]
- Giuliano, F.A.; et al. Prevalence of erectile dysfunction among 7689 patients with diabetes or hypertension, or both. Urology 2004, 64, 1196–1201. [Google Scholar]
- Johannes, C.B.; et al. Incidence of erectile dysfunction in men 40 to 69 years old: longitudinal results from the Massachusetts male aging study. The Journal of urology 2000, 163, 460–463. [Google Scholar] [CrossRef]
- Virag, R.; Bouilly, P.; Frydman, D. Is impotence an arterial disorder?: A study of arterial risk factors in 440 impotent men. The Lancet 1985, 325, 181–184. [Google Scholar]
- Lasaponara, F.; et al. Erectile dysfunction after kidney transplantation: our 22 years of experience. In Transplantation proceedings; Elsevier, 2004. [Google Scholar]
- Malavaud, B.; et al. High prevalence of erectile dysfunction after renal transplantation. Transplantation 2000, 69, 2121–2124. [Google Scholar] [PubMed]
- Barroso, L.; et al. Analysis of sexual function in kidney transplanted men. In Transplantation proceedings; Elsevier, 2008. [Google Scholar]
- Burgos, F.; et al. Effect of kidney transplantation and cyclosporine treatment on male sexual performance and hormonal profile: a prospective study. In Transplantation proceedings; Elsevier, 1997. [Google Scholar]
- Akbari, F.; et al. Effect of renal transplantation on sperm quality and sex hormone levels. BJU international 2003, 92, 281–283. [Google Scholar] [PubMed]
- Chu, S.; et al. Male sexual performance and hormonal studies in uremic patients and renal transplant recipients. In Transplantation proceedings; Elsevier Science Publishing Company, Inc., 1998. [Google Scholar]
- Tsujimura, A.; et al. Effect of renal transplantation on sexual function. Archives of andrology 2002, 48, 467–474. [Google Scholar]
- Levitan, D.; et al. Disturbances in the hypothalamic-pituitary-gonadal axis in male patients with acute renal failure. American journal of nephrology 1984, 4, 99–106. [Google Scholar]
- Corona, G.; et al. Endocrinologic control of men’s sexual desire and arousal/erection. The journal of sexual medicine 2016, 13, 317–337. [Google Scholar]
- Massry, S.; et al. Impotence in patients with uremia. Nephron 1977, 19, 305–310. [Google Scholar] [PubMed]
- Chou, F.-F.; et al. Improvement of sexual function in male patients after parathyroidectomy for secondary hyperparathyroidism. Journal of the American College of Surgeons 2001, 193, 486–492. [Google Scholar]
- Nikoobakht, M.R.; et al. The role of hypothyroidism in male infertility and erectile dysfunction. Urology Journal 2012, 9, 405–409. [Google Scholar] [PubMed]
- Cardinal, H.; Dieudé, M.; Hébert, M.-J. Endothelial dysfunction in kidney transplantation. Frontiers in immunology 2018, 9, 1130. [Google Scholar]
- Billups, K.L. Sexual dysfunction and cardiovascular disease: integrative concepts and strategies. The American journal of cardiology 2005, 96, 57–61. [Google Scholar]
- Foley, R.N.; Parfrey, P.S. Cardiovascular disease and mortality in ESRD. Journal of nephrology 1998, 11, 239–245. [Google Scholar] [PubMed]
- Federation, N.N.K. Sexual Problems Following a Transplant January 2024. Available online: https://www.kidney.org.uk/sexual-problems-following-a-transplant.
- Onder Canguven, A.H.A.M. Vitamin D and male erectile function: an updated review. The world journal of men's health, Jan 2020, 39, 31. [Google Scholar]
- Romejko, K.; et al. Testosterone deficiency as one of the major endocrine disorders in chronic kidney disease. Nutrients 2022, 14, 3438. [Google Scholar] [CrossRef]
- SEN*, S.; et al. Journal of Islamic Academy of Sciences Nephrology 1993.
- Majzoub, A.; Shoskes, D.A. A case series of the safety and efficacy of testosterone replacement therapy in renal failure and kidney transplant patients. Translational Andrology and Urology 2016, 5, 814. [Google Scholar] [PubMed]
- Basaria, S.; et al. Adverse events associated with testosterone administration. New England Journal of Medicine 2010, 363, 109–122. [Google Scholar] [PubMed]
- Krzastek, S.C.; et al. Long-term safety and efficacy of clomiphene citrate for the treatment of hypogonadism. The Journal of urology 2019, 202, 1029–1035. [Google Scholar]
- Guay, A.; et al. Clomiphene increases free testosterone levels in men with both secondary hypogonadism and erectile dysfunction: who does and does not benefit? International Journal of Impotence Research 2003, 15, 156–165. [Google Scholar]
- De Pasquale, C.; et al. Psychological and psychopathological aspects of kidney transplantation: a systematic review. Frontiers in psychiatry 2020, 11, 106. [Google Scholar]
- Kumar, B.A.; Mattoo, S.K. Organ transplant & the psychiatrist: An overview. Indian Journal of Medical Research 2015, 141, 408–416. [Google Scholar]
- Metz, M.; Epstein, N.; Mccarthy, B. Cognitive-behavioral therapy for sexual dysfunction; Routledge, 2017. [Google Scholar]

| Factor | Mechanism |
| Nitric Oxide Deficiency | Impaired vasodilation |
| Elevated ADMA | Competitive inhibition of NOS enzyme |
| Hypogonadism | Low testosterone, increased estrogen disrupts sexual function |
| Pituitary Axis Dysfunction | Elevated LH & FSH due to impaired feedback |
| Medications | Spironolactone, cimetidine, antidepressants contribute to ED |
| Study | Population | ED Prevalence |
| Massachusetts Male Aging Study (MMAS) | General Male Population | 8% (40s), 80% (70s) |
| Messina et al. | CKD Patients <50 years | Higher prevalence than >50 years |
| Mesquita et al. | CKD Patients | 72.3% (Stage 3), 81.5% (Stage 4), 87.5% (Stage 5) |
| Espinoza et al. | Kidney Transplant Recipients | 48.9% |
| Rosas et al. | Hemodialysis Patients | 82% |
| Rosas et al. | Hemodialysis Patients >50 years | 90% |
| Rosas et al. | Hemodialysis Patients <50 years | 63% |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




