Submitted:
22 February 2025
Posted:
24 February 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Clinical Characterstics and Fluid Administration Strategy
2.2. Statistical analysis
3. Results
3.1. Clinical Characteristics of the ELBW Cohort
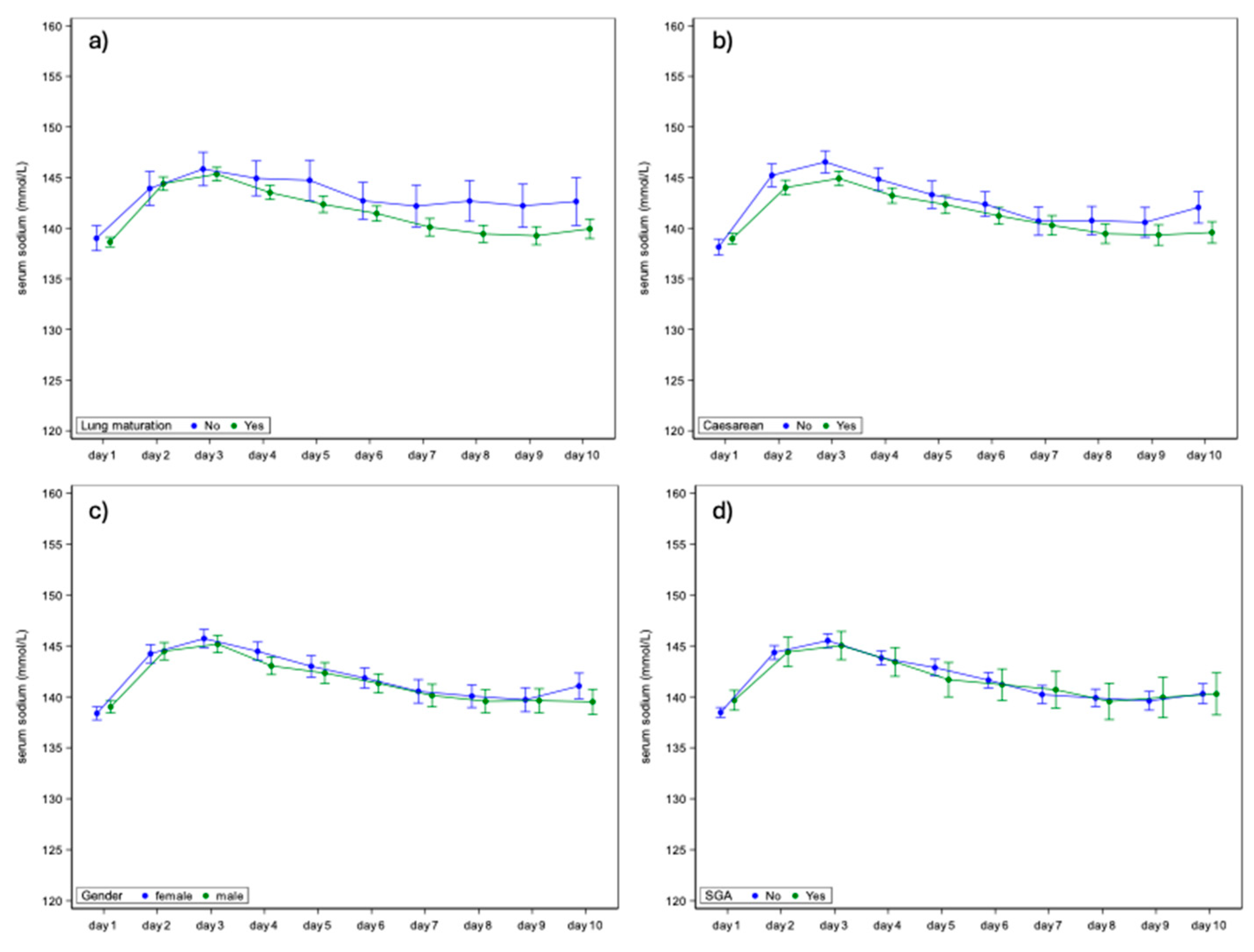
3.2. Perinatal Variables
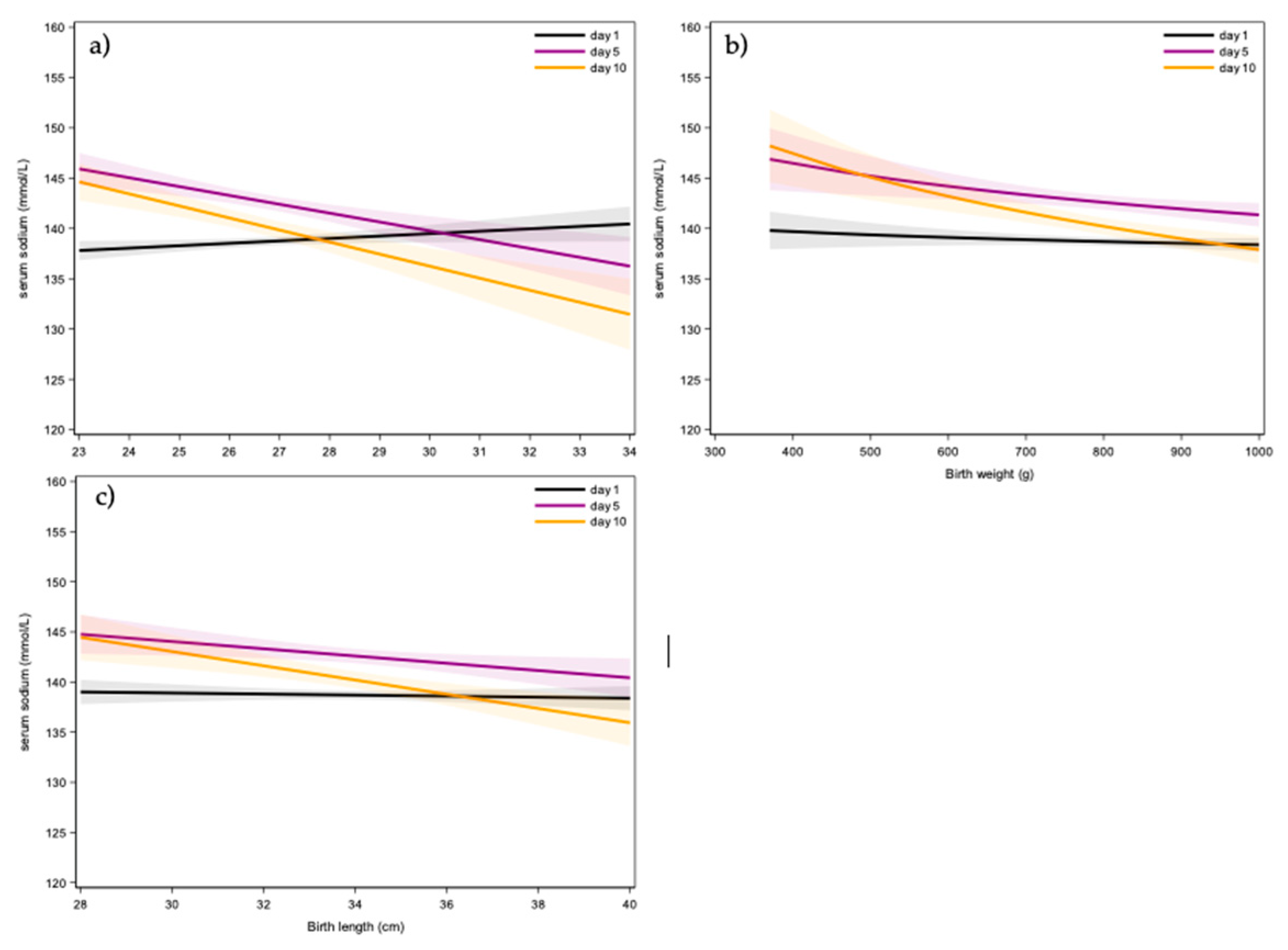
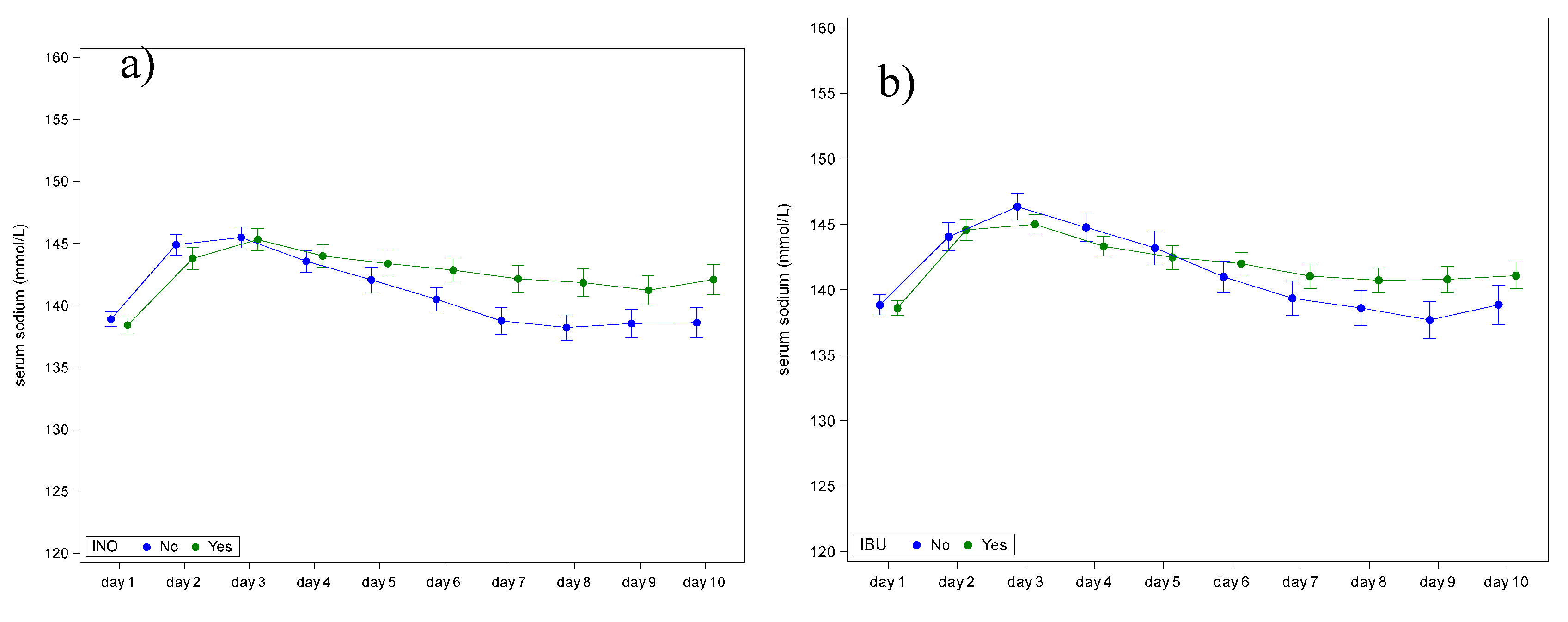
3.3. Neonatal Variables
4. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Wada, M.; Kusuda, S.; Takahashi, N.; Nishida, H. Fluid and electrolyte balance in extremely preterm infants < 24 weeks of gestation in the first week of life. Pediatr. Int. 2008, 50, 331–336. [Google Scholar] [CrossRef] [PubMed]
- Stritzke, A.; Thomas, S.; Amin, H.; Fusch, C.; Lodha, A. Renal consequences of preterm birth. Mol. Cell. Pediatr. 2017, 4, 2. [Google Scholar] [CrossRef] [PubMed]
- Monnikendam, C.S.; Mu, T.S.; Aden, J.K.; Lefkowitz, W.; Carr, N.R.; Aune, C.N.; Ahmad, K.A. Dysnatremia in extremely low birth weight infants is associated with multiple adverse outcomes. J. Perinatol. 2019, 39, 842–847. [Google Scholar] [CrossRef] [PubMed]
- Pace, M.; van Sas, S.; Salaets, T. , Laenen, A.; Raaijmakers, A.; Allegaert, K. Hypo- and hypernatriemia in extremely low birth weight infants in the first 10 days of life: a review. Children 2025, 12, 231. [Google Scholar] [CrossRef] [PubMed]
- van Donge, T.; Allegaert, K.; Gotta, V; Smits, A.; Levtchenko, E.; Mekahli, D.; van den Anker, J.; Pfister, M. Characterizing dynamics of serum creatinine and creatinine clearance in extremely low birth weight neonates during the first 6 weeks of life. Pediatric Nephrology. 2021, 36, 649–659. [Google Scholar] [CrossRef] [PubMed]
- Allegaert, K.; Hildebrand, H.; Singh, K.; Turner, M.A. The publication quality of laboratory values in clinical studies in neonates. Pediatr. Res. 2023, 94, 96–98. [Google Scholar] [CrossRef] [PubMed]
- Devlieger, H.; De Pourcq, L.; Casneuf, A.; Vanhole, C.; de Zegher, F.; Jaeken, J.; Eggermont, E. Standard two-compartment formulation for total parenteral nutrition in the neonatal intensive care unit: a fluid tolerance based system. Clin. Nutr. 1993, 12, 282–286. [Google Scholar] [CrossRef] [PubMed]
- SAS Institute Inc. SAS software 9.4; SAS Institute Inc.: Cary, NC, USA, 2014. [Google Scholar]
- Gawlowski, Z.; Aladangady, N.; Coen, P.G. Hypernatraemia in preterm infants born at less than 27 weeks gestation. J. Paediatr. Child. Health. 2006, 42, 771–774. [Google Scholar] [CrossRef] [PubMed]
- Segar, J.L. A physiological approach to fluid and electrolyte management of the preterm infant: Review. J Neonatal Perinatal Med. 2020, 13, 11–19. [Google Scholar] [CrossRef] [PubMed]
- Costarino, A.T.; Gruskay, J.A.; Corcoran, L.; Polin, R.A.; Baumgart, S. Sodium restriction versus daily maintenance replacement in very low birth weight premature neonates: A randomized, blind therapeutic trial. J Pediatr. 1992, 120, 99–106. [Google Scholar] [CrossRef] [PubMed]
- Eibensteiner, F.; Laml-Wallner, G.; Thanhaeuser, M.; Ristl, R.; Ely, S.; Jilma, B.; Berger, A.; Haiden, N. ELBW infants receive inadvertent sodium load above the recommended intake. Pediatr Res. 2020, 88, 412–420. [Google Scholar] [CrossRef] [PubMed]
- Boubred, F.; Herlenius, E.; Bartocci, M.; Jonsson, B.; Vanpée, M. Extremely preterm infants who are small for gestational age have a high risk of early hypophosphatemia and hypokalemia. Acta Paediatr. 2015, 104, 1077–1083. [Google Scholar] [CrossRef] [PubMed]
- Stritzke, A.; Ismail, R.; Rose, M.S.; Lyon, A.W.; Tenton, T.R. Cord-Blood Derived Chemistry Reference Values in Preterm Infants for Sodium, Chloride, Potassium, Glucose, and Creatinine. Am. J. Perinatol. 2024, 41, 722–729. [Google Scholar] [CrossRef] [PubMed]
- Ohkawa, N.; Shoji, H.; Ikeda, N.; Murano, Y.; Okuno, T.; Kantake, M.; Yokomizo, T.; Shimizu, T. The impact of cyclooxygenase inhibitor use on urinary prostaglandin metabolites in preterm infants. Pediatr. Neonatol. 2024, 65, 123–126. [Google Scholar] [CrossRef] [PubMed]
- Agakidou, E.; Chatziioannadis, I.; Kontou, A.; Stathopoulou, T.; Chotas, W.; Sarafidis, K. An update on pharmacologic management of neonatal hypotension: when, why, and which medication. Children (Basel) 2024, 11, 490. [Google Scholar] [CrossRef] [PubMed]
- Dimitriou, G.; Kavvadia, V.; Marcou, M.; Greenough, A. Antenatal steroids and fluid balance in very low birth weight infants. Arch. Dis. Child. Fetal Neonatal Ed. 2005, 90, F509–F513. [Google Scholar] [CrossRef] [PubMed]
| Variable | Statistic | All | |
|---|---|---|---|
| Birth weight (g) | N Mean Std Median IQR Range |
211 807 135 830 (715; 910) (370;1000) |
|
| Length (cm) | N Mean Std Median IQR Range |
200 34 2.4 34 (32; 36) (28; 40) |
|
| Growth category | AGA SGA |
n/N (%) n/N (%) |
170/211 (80.6%) 41/211 (19.4%) |
| Gestational age (weeks) | N Mean Std Median IQR Range |
211 26.7 1.9 26 (25; 28) (23; 34) |
|
| Sex | Female Male Unknown |
n/N (%) n/N (%) n/N (%) |
99/211 (46.9%) 111/211 (52.6%) 1/211 (0.5%) |
| Neonatal death | No Yes |
n/N (%) n/N (%) |
183/211 (86.7%) 28/211 (13.3%) |
| Lung maturation | No Yes |
n/N (%) n/N (%) |
28/207 (13.5%) 179/207 (86.5%) |
| Caesarean | No Yes |
n/N (%) n/N (%) |
63/209 (30.1%) 146/209 (69.9%) |
| Ibuprofen | No Yes |
n/N (%) n/N (%) |
79/209 (37.8%) 130/209 (62.2%) |
| Inotropic agents | No Yes |
n/N (%) n/N (%) |
111/208 (53.4%) 97/208 (46.6%) |
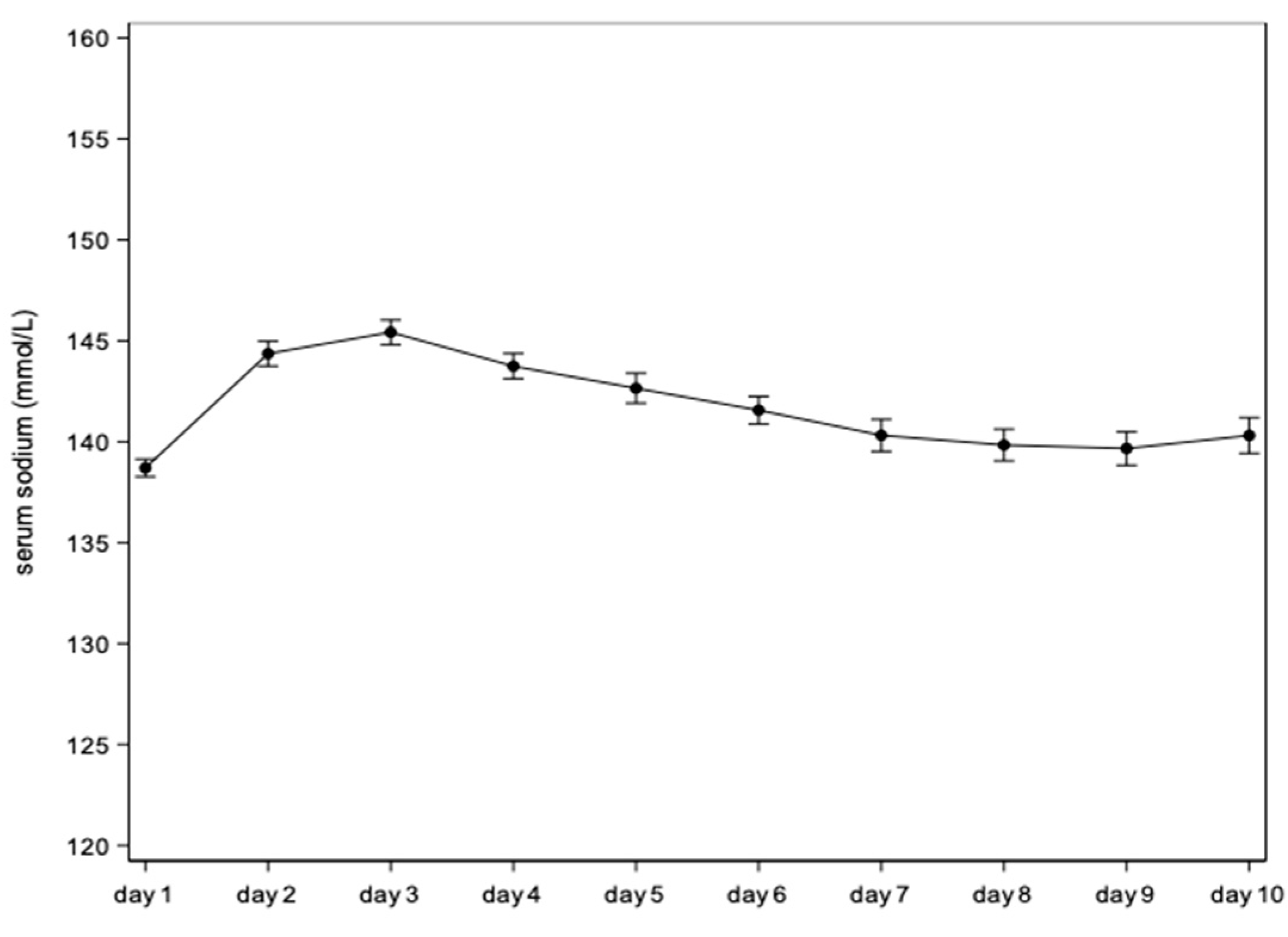
| Day | Mean estimate (95% CI) | Mean difference vs Day 1 (95% CI) | P-value |
|---|---|---|---|
| Day 1 | 138.7 (138.3;139.1) | 0 | . |
| Day 2 | 144.4 (143.7;145.0) | 5.7 (5.0;6.3) | <.0001 |
| Day 3 | 145.4 (144.8;146.0) | 6.7 (6.0;7.5) | <.0001 |
| Day 4 | 143.7 (143.1;144.4) | 5.0 (4.3;5.8) | <.0001 |
| Day 5 | 142.6 (141.9;143.4) | 3.9 (3.1;4.8) | <.0001 |
| Day 6 | 141.6 (140.9;142.2) | 2.9 (2.0;3.7) | <.0001 |
| Day 7 | 140.3 (139.5;141.1) | 1.6 (0.7;2.5) | 0.0005 |
| Day 8 | 139.8 (139.0;140.6) | 1.1 (0.2;2.0) | 0.0141 |
| Day 9 | 139.7 (138.8;140.5) | 1.0 (0.0;1.9) | 0.0422 |
| Day 10 | 140.3 (139.4;141.2) | 1.6 (0.6;2.6) | 0.0015 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




