Submitted:
20 February 2025
Posted:
21 February 2025
Read the latest preprint version here
Abstract
Keywords:
- Technological Progress: FHIR and ISO 23903:2021 present supplementary methodologies for data structuring and semantic compatibility, while blockchain and AI are being established to drive the secured, automated, and real-time exchange of healthcare information.
- Regulatory Landscape: The 2020–2025 WHO Strategy on Digital Health and the 2024 WHO Report on the Transformation of Digital Health underscore the need for harmonized interoperability frameworks, AI governance, and cybersecurity to deliver equitable access to digital healthcare innovations.
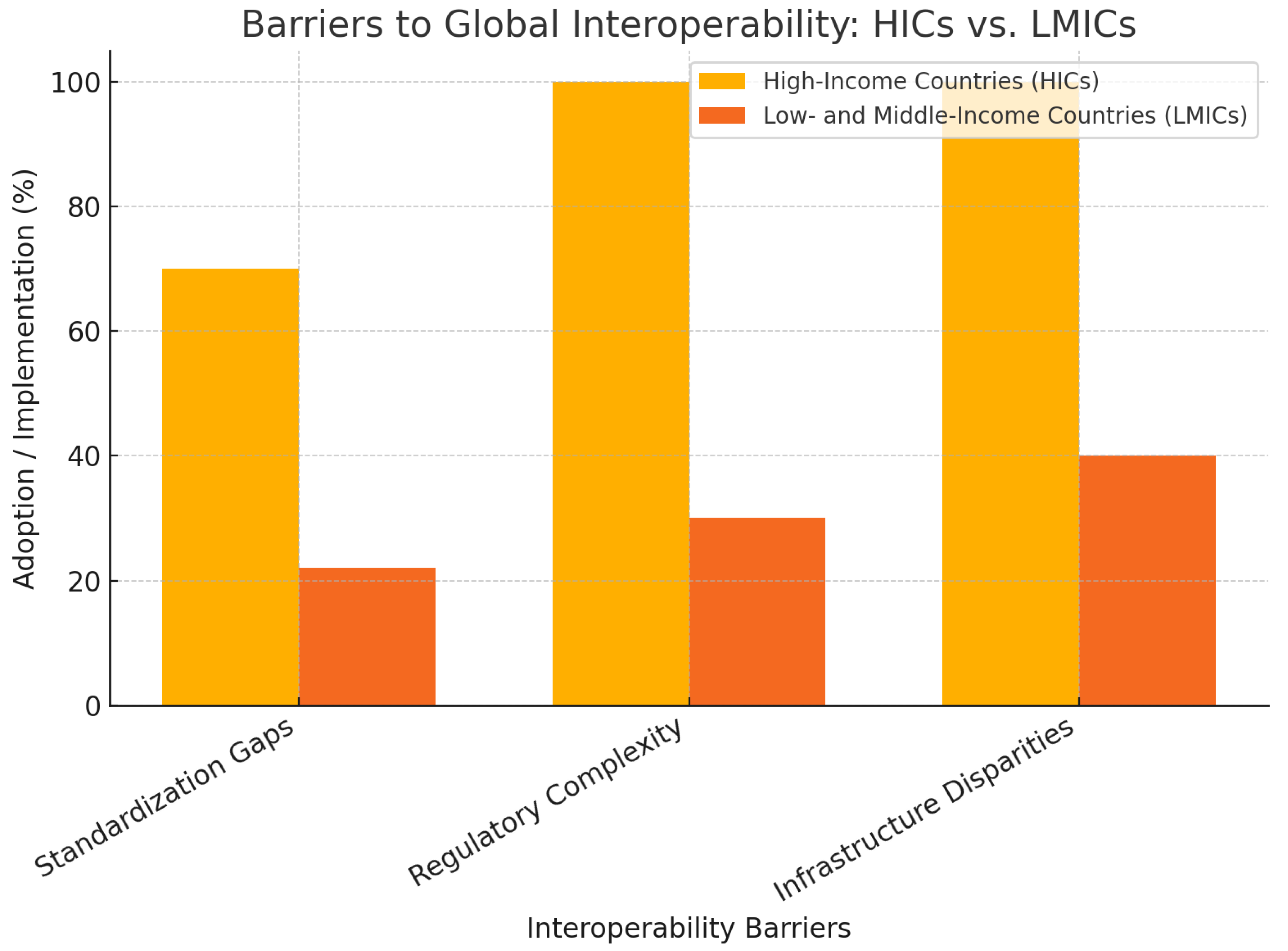
- Challenges and Barriers: Regulatory fragmentation, security risks, and infrastructure disparities in low- and middle-income countries (LMICs) remain key obstacles to achieving full interoperability.
- Future Directions: Expanding public-private partnerships, strengthening FHIR-TEFCA alignment, and implementing ISO 23903:2021-based integration models will be critical for ensuring scalable, cross-border health information exchange.
1. Introduction
- Technological Challenges – Electronic health record (EHR) architecture variability and the lack of standard protocols for data-sharing [8].
- Security & Privacy Issues – There is a need to balance the accessibility of information with robust patient information protection measures [10].
- Infrastructure Disparities – Inequal access to technologies that support Interoperability, particularly within resource-constrained environments [11].
Scope of this Paper
- Case Studies – Review the VHA’s successful experience integrating the EHR with other real applications [12].
| Region/Country | FHIR Adoption Rate | Key Implementations | Challenges | Source |
|---|---|---|---|---|
| United States | 65% | TEFCA integration, ONC mandates | Legacy EHRs, high implementation costs | [6,7] |
| European Union | 55% | EU Digital Health Action Plan, cross-border EHR exchange | Data privacy (GDPR), interoperability fragmentation | [9,13] |
| Canada | 48% | Pan-Canadian Health Data Strategy, FHIR-based national EHR | Uneven provincial adoption | [7,9] |
| Low/Middle-Income Countries (LMICs) | 22% | WHO interoperability frameworks, donor-funded projects | Infrastructure gaps, lack of regulatory enforcement | [9,16] |
2. Literature Review
3.1. Technological Foundations of Interoperability
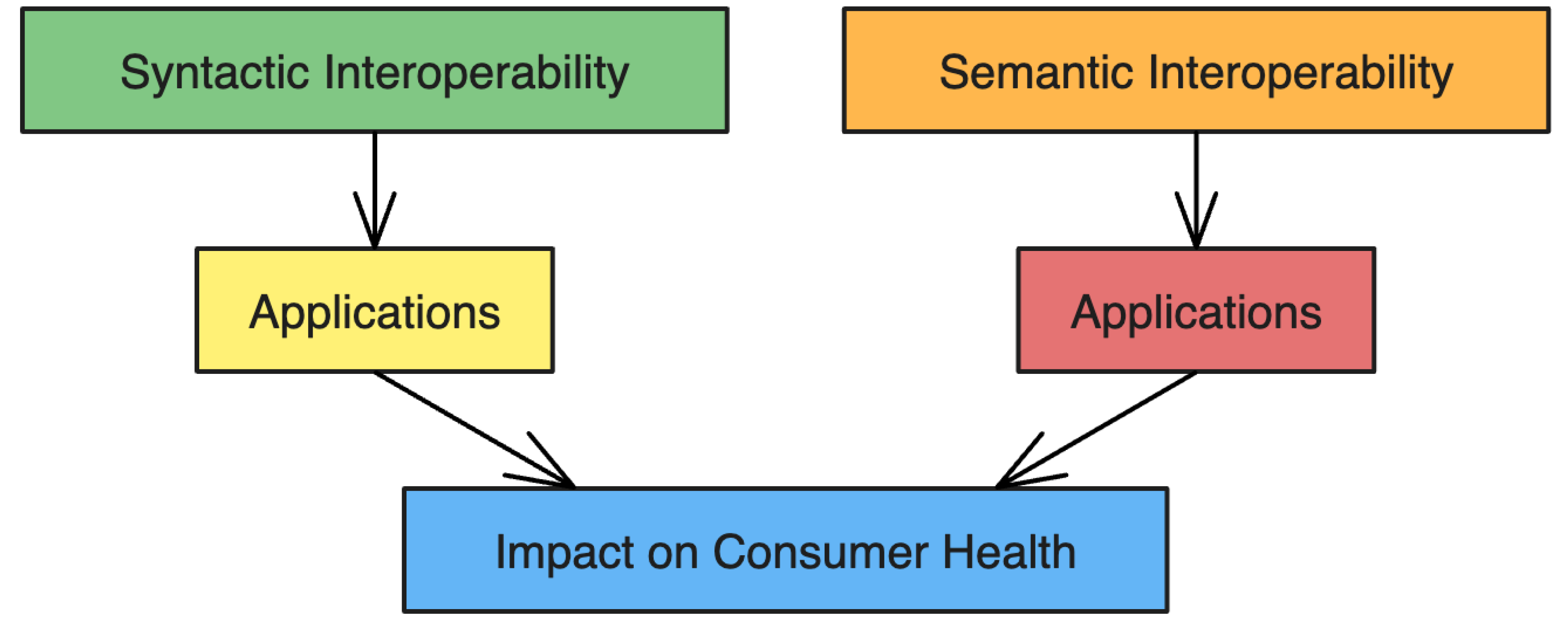
- Syntactic Interoperability: Assures that exchanging information is standard to allow systems to read and decode structured information. Tools like Fast Healthcare Interoperability Resources (FHIR) and Health Level Seven (HL7) allow standard structuring of information between healthcare systems [6].
- Semantic Interoperability: Assures that information is meaningful between systems. Shared vocabularies like Systematized Nomenclature of Medicine—Clinical Terms (SNOMED CT) and Logical Observation Identifiers, Names, and Codes (LOINC) provide shared terms that permit proper meaning to be understood between systems [6].
3.2. FHIR Activities of Standardization
3.2.1. Advantages of Using FHIR in Healthcare Interoperability
- Modular API Structure – FHIR employs a RESTful API structure to allow healthcare applications to securely access and update patient information between systems.
- Interoperability with Mobile Apps & Electronic Health Records – FHIR enables seamless interaction between mobile apps for healthcare, patient portals, and electronic health records (EHRs), enabling real-time information exchange [7].
- Standardized Data Formats – FHIR enables greater clinical workflow integration, usability, and healthcare provider decision-making by standardizing defined and coded data elements.
- Improved Scalability and Adaptability – It is compatible with structured and unstructured information to support bespoke applications per the requirements of healthcare providers.
3.2.2. Barriers to FHIR Adoption
- Technical Complexity – Many healthcare providers are still working with HL7 v2 and Clinical Document Architecture (CDA), necessitating other mapping frameworks to provide compatibility between current and FHIR-based systems [21].
- Variable Adoption Levels – Google, Microsoft, and Amazon have heavily invested in FHIR, while small to medium-sized providers are priced out by the cost due to a lack of IT capabilities and infrastructure [21].
- Integration Challenges – FHIR implementation requires extensive modifications to existing EHR systems, making interoperability efforts costly, time-consuming, and resource-intensive [21].
- Lack of a Common Oversight – The lack of a standard overseeing body to implement the adoption of FHIR results in varying levels of implementation within various healthcare environments, reducing Interoperability even further.
3.2.3. Complementary Strategies to Support FHIR Implementation
- Regulatory Enforcement through TEFCA – Conforming FHIR to the Trusted Exchange Framework and Common Agreement (TEFCA) would standardize the information exchange protocols between healthcare systems [8].
- Machine Learning to Standardise Data – Machine learning-enabled data harmonization software can enhance semantic Interoperability by automating non-standardized data into standard formats [5].
- Blockchain for Secure Data Sharing – Blockchain solutions can enhance the security of the data, auditability, and trust of the FHIR-enabled health data exchanges [14].
3.3. Policy and Governance Within Interoperability
3.3.1. TEFCA and the Rulemaking Structure
- Establish a Unified Platform of Data-Sharing – TEFCA establishes the infrastructure to provide smooth healthcare data exchange between clinics, insurers, government agencies, and hospitals.
- Encourage Private-Public Collaboration – With the backing of the TEFCA, both public and private healthcare organizations can access a shared healthcare data exchange network to aid increased adoption of Interoperability.
- Real-world comparison: VHA succeeded with its complete EHR system, while the LMICs lack digital infrastructure and regulation enforcement [9].
- Integration Costs – Aligning existing FHIR-based systems with TEFCA requires significant infrastructure upgrades, posing financial burdens for smaller providers.
| Policy Framework | United States (TEFCA, HIPAA) | European Union (GDPR, EHDS) | Canada (Pan-Canadian Strategy) | LMICs (WHO-led initiatives) |
|---|---|---|---|---|
| Standardization Approach | TEFCA mandates national EHR integration | GDPR-compliant cross-border data exchange | Province-led, limited national mandate | WHO global standards, inconsistent adoption |
| Data Privacy Regulation | HIPAA ensures PHI security | GDPR enforces strong patient consent | Provincial privacy laws | Varies widely, often weak security |
| Challenges | Limited enforcement, voluntary compliance | Fragmentation among member states | Uneven adoption across provinces | Infrastructure constraints, lack of funding |
3.3.2. Global Interoperability Efforts
- European Union’s Digital Health Action Plan – It aims to harmonize the models of the EHR at the EU member state levels to allow cross-border healthcare service delivery and the exchange of patient information [7].
- World Health Organization (WHO) Interoperability Framework – The WHO established international guidelines to standardize the requirements of Interoperability to provide equal access to low-resource countries to the technologies of shared healthcare information [9].
- ISO/TC 215 Health Informatics Standards – The International Organization for Standardization (ISO) established technical requirements to promote greater Interoperability, protection of personal information, and the security of healthcare information within multi-national healthcare environments [7,9].
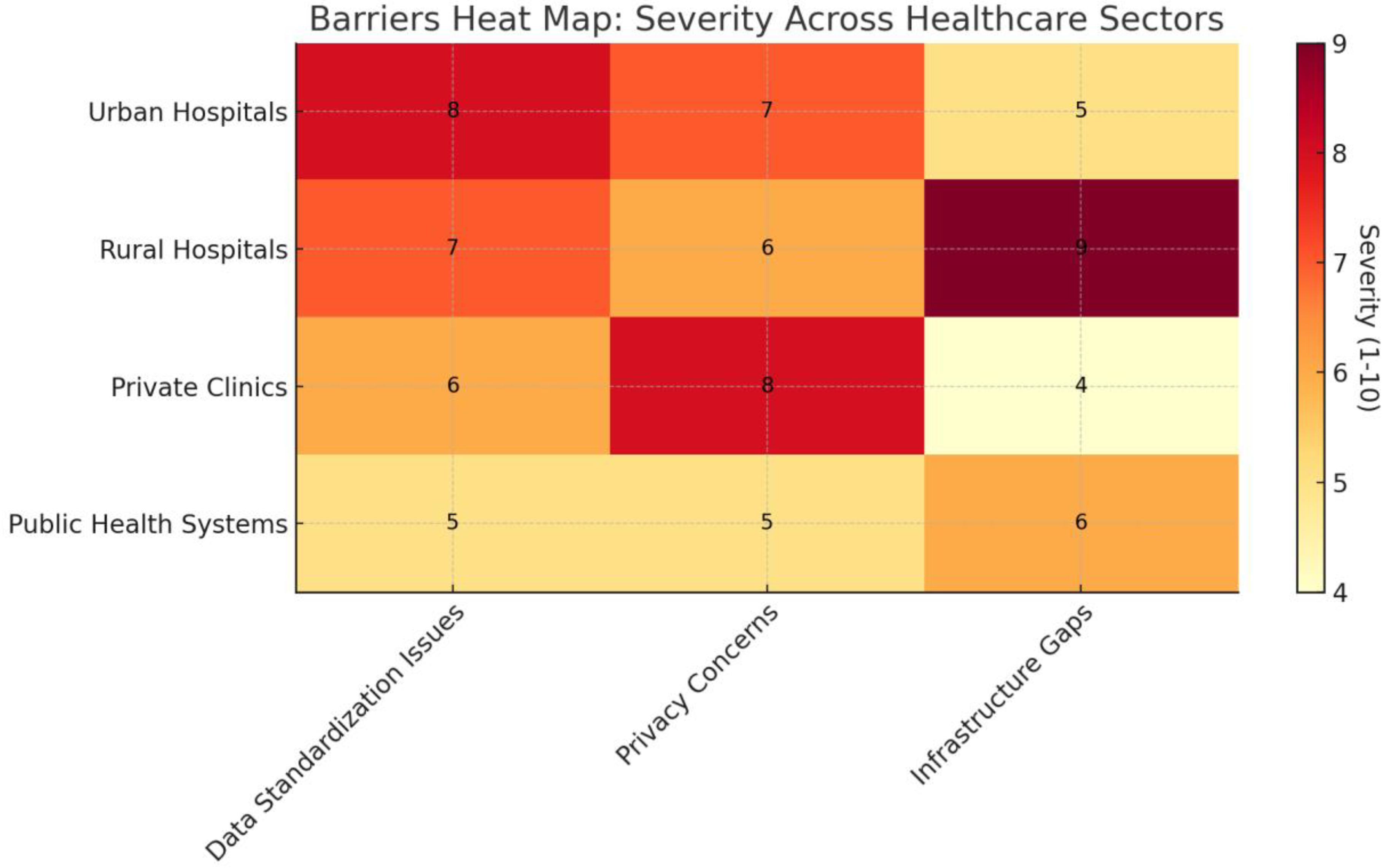
- Regulatory Fragmentation – Countries have unique data protection legislation and compliance models, with international compatibility a problem.
- Infrastructure Disparities – Low-income regions often lack the technological infrastructure to implement FHIR-compatible systems, creating a digital divide in health data exchange.
- Data Privacy and Cybersecurity Risks – Cross-border data transfer creates complex cybersecurity threats that necessitate strong governance frameworks to protect the information.
- Regulatory Harmonization – Governments must harmonize the data privacy legislation (e.g., HIPAA, GDPR, and country-wide healthcare policies) to allow secure international data exchange.
- Investment in digital infrastructure – Scaling up international opportunities to fund low-resource healthcare systems can bridge the digital divide while boosting the Interoperability of international health information.
- Privacy-Preserving Technologies – With AI-driven anonymization techniques and zero-knowledge proofs, confidential patient information can be maintained while enabling cross-border compatibility.
- AI-driven data harmonization tools, blockchain security models, and stronger regulatory mandates must complement FHIR adoption.
- TEFCA implementation requires enhanced policy enforcement, including mandatory compliance, financial incentives, and public-private collaboration.
- Global interoperability efforts must prioritize harmonizing the regulatory environment, investments in digital infrastructure, and adopting privacy-preserving technologies.
- Harmonizing National Laws – Different countries and jurisdictions have unique sets of legislation, such as HIPAA of the US and GDPR of the European Union, that have divergent healthcare information exchange policy frameworks.
- Ensuring Data Privacy – The secure transfer of confidential patient information between healthcare networks is a persistent issue, particularly with cross-border interoperability efforts. It is imperative to find a balance between the accessibility of the information and the protection of the information.
- Overcoming Infrastructure Inequalities – In low-resource settings, the digital infrastructure to accommodate FHIR-enabled interoperability solutions is not usually present. It creates inequitable access to technologies that allow the exchange of health information, particularly among low-income communities [21].
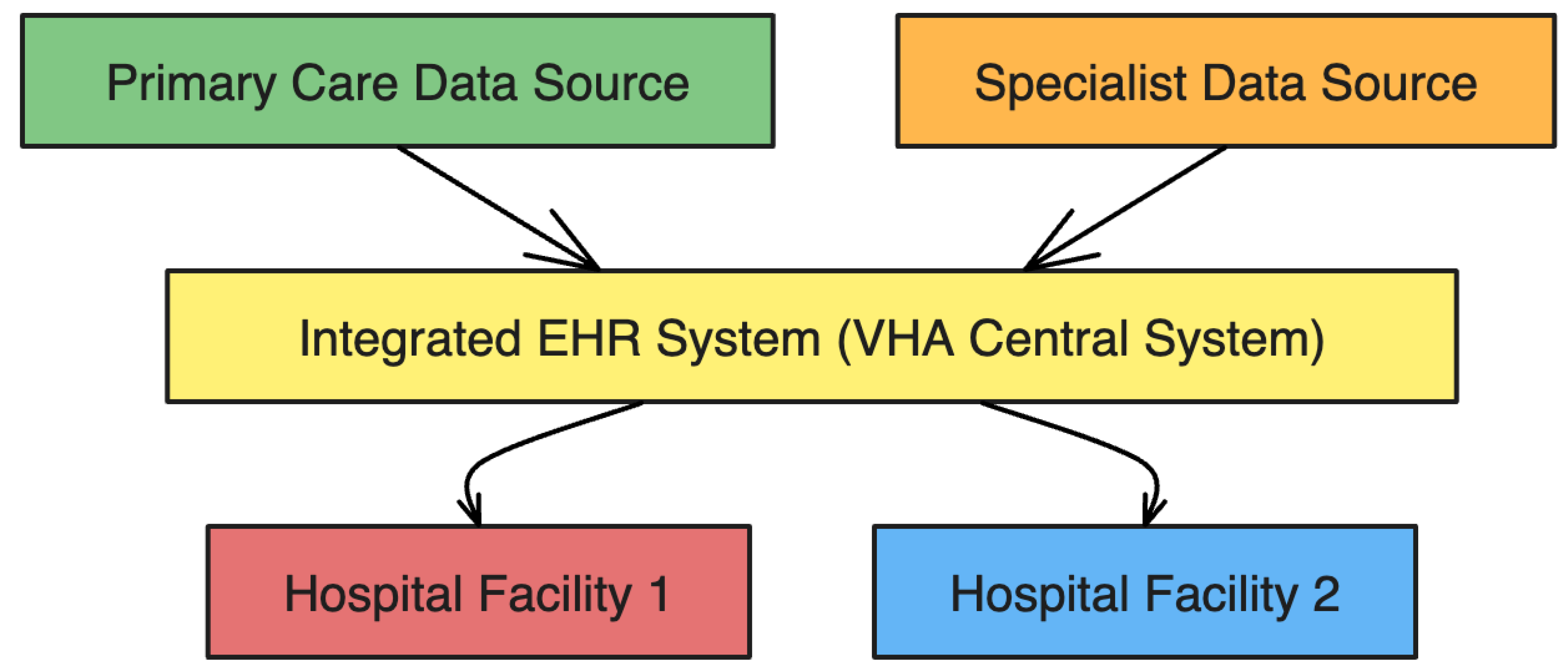
3.4. Real-World Case Study: Veterans Health Administration (VHA)
3.4.1. VHA’s Success with Integrated EHR
- Improved Care Coordination – Multiple care providers at various sites of the VHA can access, update, and share patient health information in real time to improve care coordination.
- Reduction in Redundant Tests and Medication Errors – Interoperability within the environment of the VHA avoids unnecessary tests, reduces error rates, and ultimately saves healthcare spending [10].
- Enhanced Provider Decision-Making – With the central health information exchange, clinicians can access complete patient histories to support more accurate treatment decisions and personalized treatment plans.
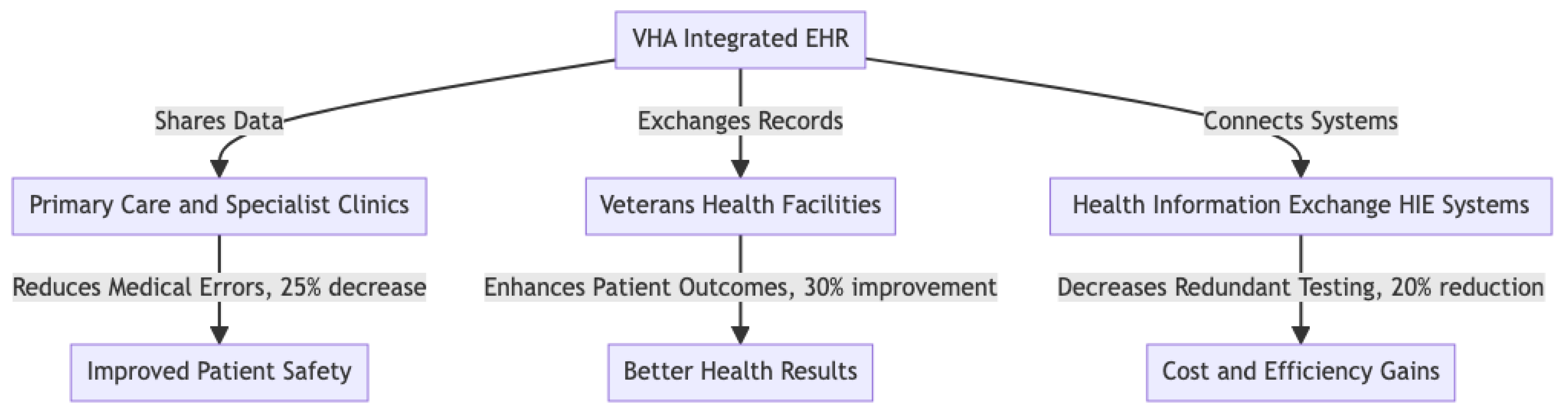
- Accelerating FHIR adoption to enhance data interoperability across VHA facilities.
- Improving HIE Tools to support information exchange with external healthcare providers
- Optimizing system usability to reduce workflow inefficiencies caused by data integration limitations.
3.4.2. Medication Reconciliation and Health Information Exchange (HIE) at the VHA
- Improved Clinician Access to External Medication Records – HIE adoption has led to fewer discrepancies in prescription histories, reducing medication errors and enhancing patient safety [11].
- Challenges in Interface Usability – Data glut, navigation intricacy, and impediments to integrating systems are among the challenges that impede clinicians' optimal usage of HIE solutions.
- Opportunities for Maximizing HIE Tools – Improved workflow architecture and real-time support of decisions can potentially simplify access to the data and enhance the results of Interoperability.
3.5. Identified Gaps and Future Directions
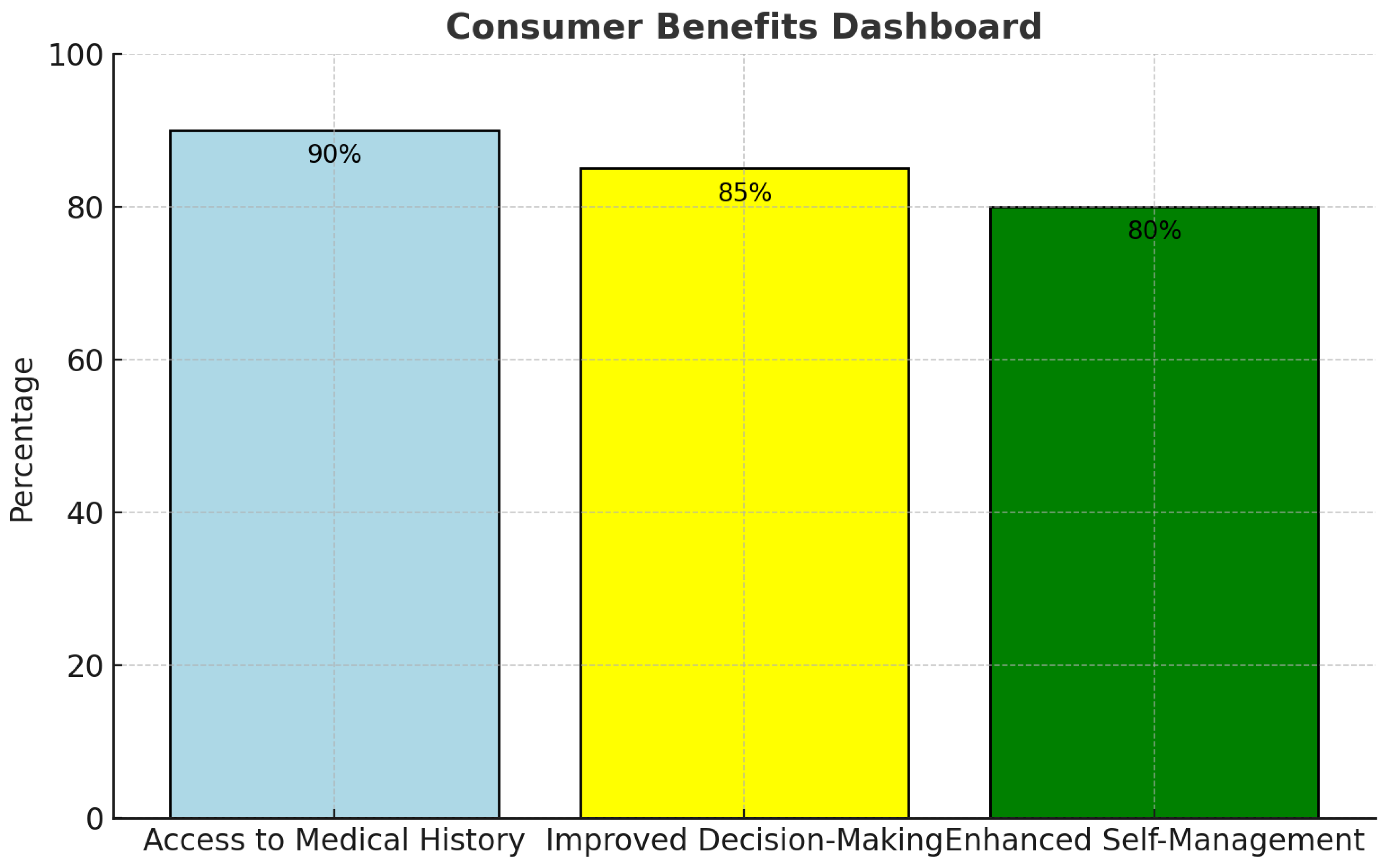
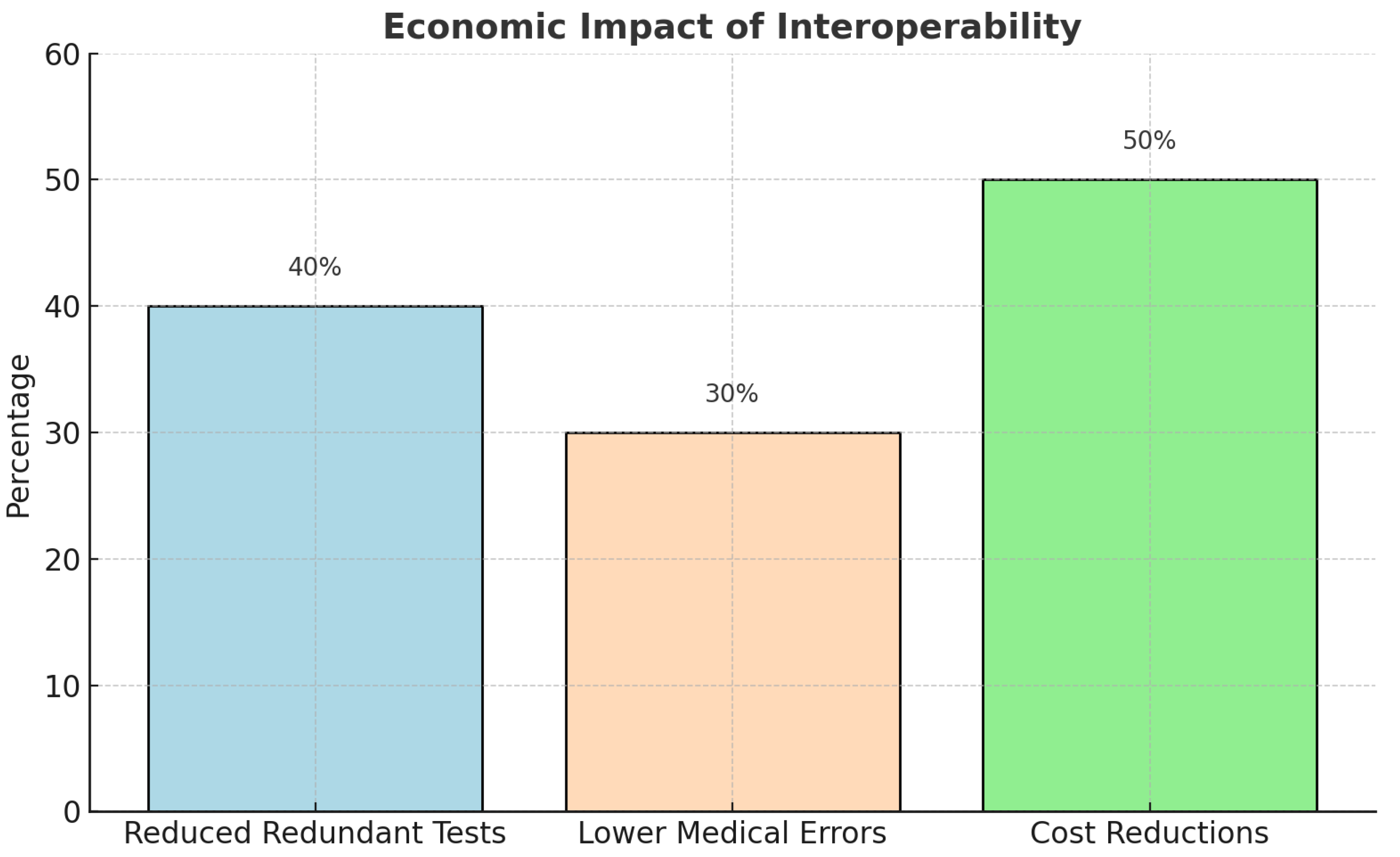
4. Challenges & Future Directions: Strengthening Policy and Technological Frameworks
4.1. Overcoming Standardization Gaps
4.2. Enhancing Security and Privacy Within Interoperability Networks
4.3. Bridging Infrastructure Disparities and Expanding Interoperability in Underserved Regions
4.4. Future Priorities of Research and Development
5. Emerging Technologies to Ensure Interoperability
5.1. Blockchain for Secure and Transparent Health Data Exchange
-
Patient-Controlled Data Ownership & Consent
-
Cross-System Data Consistency & Avoidance of Fraud
-
Cybersecurity & Ransomware Protection
5.2. AI for Data Standardization and Predictive Analytics
- Stakeholder engagement: All the major participants involved—including the healthcare providers, the patients, the policymakers, and the technologies' developers—will need to collaborate to craft AI solutions that address the ethics of the issue at hand, such as the issue of the algorithms being prejudiced and the issue of confidentiality of the information [5].
-
Natural Language Processing (NLP) to Enable Semantic Interoperability
-
Predictive Analytics to Manage Populations
-
Automated Data Mapping & FHIR Integration
| Technology | Key Benefits | Challenges & Barriers |
|---|---|---|
| AI & NLP | Improves semantic interoperability, automates data mapping | Bias in AI models, regulatory concerns |
| Blockchain | Enhances security, ensures patient-controlled consent | Scalability, lack of widespread implementation |
| FHIR & TEFCA | Enables real-time, standardized data exchange | Adoption barriers, costs of EHR integration |
5.3. FHIR and TEFCA: Future Directions in Data Sharing
- 1.
-
FHIR Advancements in Standardized Data Sharing
- 2.
-
TEFCA’s Role within the Governance & Compliance
- 3.
-
Global Harmonization of Interoperability Standards
-
Aligning AI & Blockchain with FHIR-Based TEFCA Models
-
Developing Scalable Interoperability Solutions for the Resource-Limited
-
Enhancing Cybersecurity & Data Privacy Governance
6. Policy and Governance Approaches
6.1. Regulatory Frameworks Supporting Interoperability
- 1.
-
Health Insurance Portability and Accountability Act (HIPAA) and General Data Protection Regulation (GDPR)
- 2.
-
HITECH Act & TEFCA (United States)
- o
- HITECH Act: Encourages the adoption of electronic health records (EHR) and enables the adoption of FHIR-based interoperability standards [17].
- o
-
Trusted Exchange Framework and Common Agreement (TEFCA):
- Establishes Health Information Networks (QHINs) to improve cross-organization information exchange
- Provides financial incentives to encourage the uptake of FHIR and TEFCA among healthcare providers [18].
- 3.
-
Medicare & Value-Based Care Policies
- Data-sharing incentives are minimal, creating challenges for small-and medium-sized providers [16].
6.2. Global Interoperability Initiatives
- 1.
-
European Union Digital Health Plan of Action
- 2.
-
World Health Organization (WHO) Global Interoperability Strategy
- 3.
-
ISO/TC 215 Health Informatics Standards
- o
- o
- o
| Standard/Framework | Focus Area | Key Contribution to Interoperability | Challenges |
|---|---|---|---|
| FHIR (HL7) | Technical data exchange | Defines API-based modular health data sharing | Limited semantic interoperability |
| TEFCA (ONC, USA) | Policy & Governance | Creates a federated framework for EHR data exchange | Voluntary adoption slows implementation |
| ISO 23903:2021 | Semantic interoperability | Provides an ontology-driven model for integrating multiple standards (FHIR, SNOMED CT, HL7) | Limited awareness and adoption |
| WHO Global Strategy on Digital Health (2020–2025) | International interoperability | Establishes governance models for cross-border health data exchange, AI adoption, and cybersecurity frameworks | Bridging the digital divide in LMICs |
| WHO European Digital Health Action Plan | Regional policy and implementation | Drives telemedicine expansion, AI ethics, and regulatory harmonization in the European Region | Requires further scalability beyond Europe |
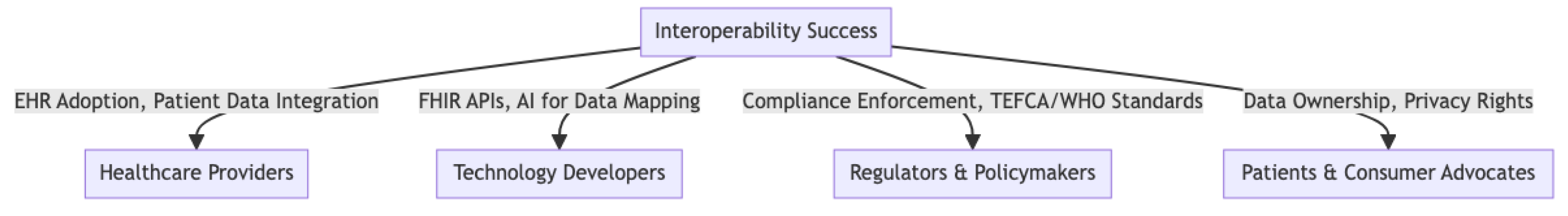
| Stakeholder Group | Key Role in Interoperability | Challenges |
|---|---|---|
| Healthcare Providers | Ensure seamless data exchange between institutions | EHR system fragmentation, lack of training |
| Technology Developers | Develop FHIR-compliant APIs, AI-driven data harmonization tools | Integration with legacy systems, security risks |
| Regulators & Policymakers | Enforce compliance (HIPAA, GDPR, TEFCA) | Cross-border policy misalignment |
| Patients & Consumer Groups | Advocate for patient data ownership and privacy | Lack of awareness, concerns about security |
6.3. Recommendations for Policymakers and Healthcare Institutions
- 1.
-
Align with the International Health Data Framework
- o
- o
- o
- 2.
-
Implement AI and blockchain Regulations to Ensure Interoperability
- o
- o
- o
- 3.
-
Expand the Funding of Health IT Adoption to the Underprivileged
- o
- o
- o
| Policy Framework | Key Contributions | Challenges |
|---|---|---|
| TEFCA (US) | Nationwide EHR data-sharing compliance | Voluntary adoption slows the impact |
| HIPAA & GDPR | Patient data privacy and security mandates | Regulatory fragmentation limits cross-border exchange |
| EU Digital Health Action Plan | FHIR-based cross-border EHR integration | Varying national policies hinder the full implementation |
| WHO Interoperability Strategy | Global standardization of health data-sharing | Infrastructure gaps in low-resource settings |
| ISO/TC 215 Health Informatics | Advances in global semantic interoperability | Limited enforcement across national health systems |
7. Conclusions and Future Directions
7.1. Summary of Main Conclusions
7.2. Call for Industry Collaboration and Investment
7.3. Next Steps for Research and Implementation
-
AI-Driven Semantic Interoperability Framework
-
Blockchain-Enabled Patient Data Governance
-
Cross-Border Regulatory Convergence
| Research Focus | Implementation Need | Potential Impact |
|---|---|---|
| AI for Semantic Interoperability | NLP for structured health data | Reduces data inconsistencies |
| Blockchain for Patient Data Ownership | Smart contracts for consent management | Enhances security, privacy compliance |
| Cross-Border Regulatory Harmonization | Aligning TEFCA, GDPR, and WHO standards | Facilitates seamless international data exchange |
Final Thoughts:
Conflict of Interest
| Abbreviation | Full Meaning |
|---|---|
| AI | Artificial Intelligence |
| API | Application Programming Interface |
| CDA | Clinical Document Architecture |
| EHR | Electronic Health Record |
| EU | European Union |
| FHIR | Fast Healthcare Interoperability Resources |
| GDPR | General Data Protection Regulation |
| HIE | Health Information Exchange |
| HIPAA | Health Insurance Portability and Accountability Act |
| HL7 | Health Level Seven International |
| HIT | Health Information Technology |
| ISO | International Organization for Standardization |
| LMICs | Low- and Middle-Income Countries |
| ML | Machine Learning |
| NLP | Natural Language Processing |
| ONC | Office of the National Coordinator for Health Information Technology |
| PHI | Protected Health Information |
| PPPs | Public-Private Partnerships |
| RBAC | Role-Based Access Control |
| SNOMED CT | Systematized Nomenclature of Medicine – Clinical Terms |
| TEFCA | Trusted Exchange Framework and Common Agreement |
| The US. | United States |
| VHA | Veterans Health Administration |
| WHO | World Health Organization |
References
- Lee AR, Kim IK, Lee E. Developing a transnational health record framework with level-specific interoperability guidelines based on a related literature review. Healthcare. 2021;9(1):67. [CrossRef]
- Palojoki S, Lehtonen L, Vuokko R. Semantic interoperability of electronic health records: Systematic review of alternative approaches for enhancing patient information availability. JMIR Med Inform. 2024;12:e53535. [CrossRef]
- Amatayakul M. Health IT and EHRs: Principles and practice. 6th ed. Chicago: American Health Information Management Association (AHIMA); 2016. Available online: https://bookshelf.vitalsource.com/books/9781584265610.
- Office of the National Coordinator for Health Information Technology (ONC). Trusted Exchange Framework and Common Agreement (TEFCA). 2024. Available online: https://www.healthit.gov/topic/interoperability/policy/trusted-exchange-framework-and-common-agreement-tefca.
- Amar F, April A, Abran A. Electronic health record and semantic issues using fast healthcare interoperability resources: Systematic mapping review. J Med Internet Res. 2024;26:e45209. [CrossRef]
- Health Level Seven International (HL7). Unpacking FHIR’s vital role in healthcare interoperability & TEFCA. 2024. https://blog.hl7.org/npacking-fhirs-vital-role-in-healthcare-interoperability-tefca-insights-from-fast-on-himsstv.
- European Commission. eHealth Network Guidelines on electronic exchange of health data. 2024. Available online: https://health.ec.europa.eu/document/download/d8f7955c-4a2c-4ba2-9aea-25f3044896e8_en?filename=ehealth_health-data_electronic-exchange_general-guidelines_en.pdf.
- Blanda Helena de Mello BH, Rigo SJ, da Costa CA, da Rosa Righi R, Donida B, Bez MR, et al. Semantic interoperability in health records standards: A systematic literature review. Health Technol. 2022;12(2):255–272. [CrossRef]
- Donahue M, Bouhaddou O, Hsing N, Turner T, Crandall G, Nelson J, et al. Veterans Health Information Exchange: Successes and Challenges of Nationwide Interoperability. AMIA Annu Symp Proc. 2018:385–394. Available online: https://pubmed.ncbi.nlm.nih.gov/30815078.
- Snyder ME, Nguyen KA, Patel H, Sanchez SL, Traylor M, Robinson MJ, et al. Clinicians' use of Health Information Exchange technologies for medication reconciliation in the U.S. Department of Veterans Affairs: a qualitative analysis. BMC Health Serv Res. 2024;24(1):1194. [CrossRef]
- Maldonado JA, Marcos M, Fernández-Breis JT, Giménez-Solano VM, Legaz-García MDC, Martínez-Salvador B. CLIN-IK-LINKS: A platform for the design and execution of clinical data transformation and reasoning workflows. Comput Methods Programs Biomed. 2020;197:105616. [CrossRef]
- HealthIT.gov. Interoperability in action: CMS rule builds on ONC initiatives. 2024. Available online: https://www.healthit.gov/buzz-blog/blog-series-cms-ipps-rule/interoperability-in-action-onc-informs-cms-ruling-on-hospital-measures-for-public-health-and-health-equity-reporting.
- Federal Register. Health data, technology, and interoperability: Trusted Exchange Framework and Common Agreement (TEFCA). 2024. Available online: https://www.federalregister.gov/documents/2024/12/16/2024-29163/health-data-technology-and-interoperability-trusted-exchange-framework-and-common-agreement-tefca.
- Centers for Disease Control and Prevention (CDC). Implementing public health interoperability. 2024. Available online: https://www.cdc.gov/data-interoperability/php/public-health-strategy/index.html.
- HealthIT.gov. FHIR roadmap for TEFCA exchange V.2: FHIR APIs are on their way into TEFCA exchange. 2024. Available online: https://www.healthit.gov/buzz-blog/tefca/fhir-roadmap-for-tefca-exchange-v-2.
- Blumenthal D, Tavenner M. The "meaningful use" regulation for electronic health records. N Engl J Med. 2010;363(6):501–504. Available online: https://pubmed.ncbi.nlm.nih.gov/20647183.
- Holmgren AJ, Patel V, Adler-Milstein J. Progress in interoperability: Measuring US hospitals' engagement in sharing patient data. Health Aff (Millwood). 2017;36(10):1820–1827. Available online: https://pubmed.ncbi.nlm.nih.gov/28971929.
- Mandel JC, Pollak JP, Mandl KD. The patient role in a federal national-scale health information exchange. J Med Internet Res. 2022;24(11):e41750. [CrossRef]
- Glandon GL, Slovensky DJ, Smaltz DH. Information technology for healthcare managers. 9th ed. Chicago: Health Administration Press; 2020.
- Institute of Medicine (US) Committee on Quality of Health Care in America.To Err is Human: Building a Safer Health System. Edited by Linda T. Kohn et al. National Academies Press (US); 2000. Available online: https://pubmed.ncbi.nlm.nih.gov/25077248.
- Ayaz M, Pasha MF, Alzahrani MY, Budiarto R, Stiawan D. The Fast Health Interoperability Resources (FHIR) Standard: Systematic Literature Review of Implementations, Applications, Challenges, and Opportunities. JMIR Med Inform. 2021;9(7):e21929. [CrossRef]
- International Organization for Standardization (ISO). Health informatics—Interoperability and integration reference architecture—Model and framework (ISO 23903:2021). ISO; 2021. Available online: https://www.iso.org/standard/77386.html.
- World Health Organization (WHO) Regional Office for Europe. Accelerating digital health transformation in Europe: a two-year progress report. WHO Europe. 2024 Oct 28. Available online: https://www.who.int/europe/news-room/28-10-2024-accelerating-digital-health-transformation-in-europe--a-two-year-progress-report.
- World Health Organization (WHO). Global strategy on digital health 2020–2025. WHO; 2021. Available online: https://www.who.int/publications/i/item/9789240020924.
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




