Submitted:
20 February 2025
Posted:
21 February 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
Facility
Residents
- Period 1: Pre-COVID-19 pandemic, from January 1, 2018, to December 31, 2019
- Period 2: During the pandemic in Japan, when no COVID-19 cases were reported in the Toshiwakai LTCF, from January 1, 2020, to December 31, 2021
- Period 3: During the COVID-19 cluster outbreak at Toshiwakai LTCF, from January 1, 2022, to December 31, 2023
Prevention and Diagnostic Protocols
Treatment Protocols
Comparison of Demographic Parameters
Comparison of Symptoms
Survival Time Comparison
Statistical Analysis
3. Results
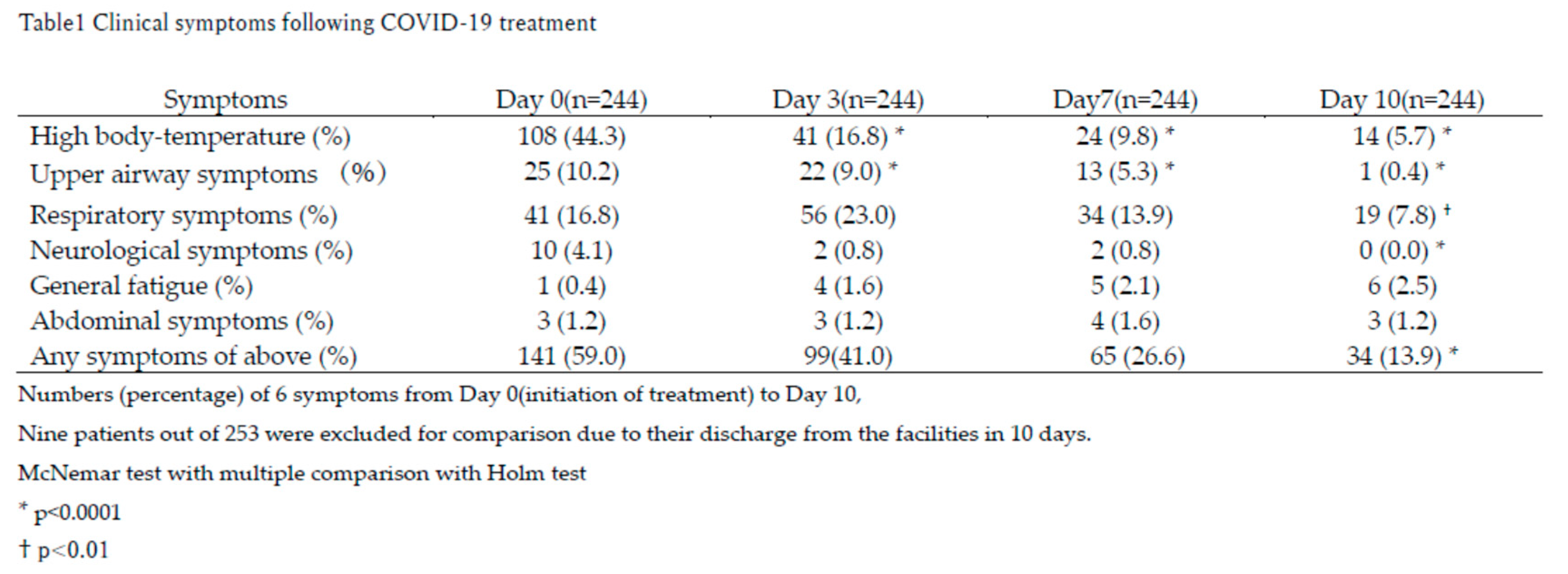
Comparison of Symptoms
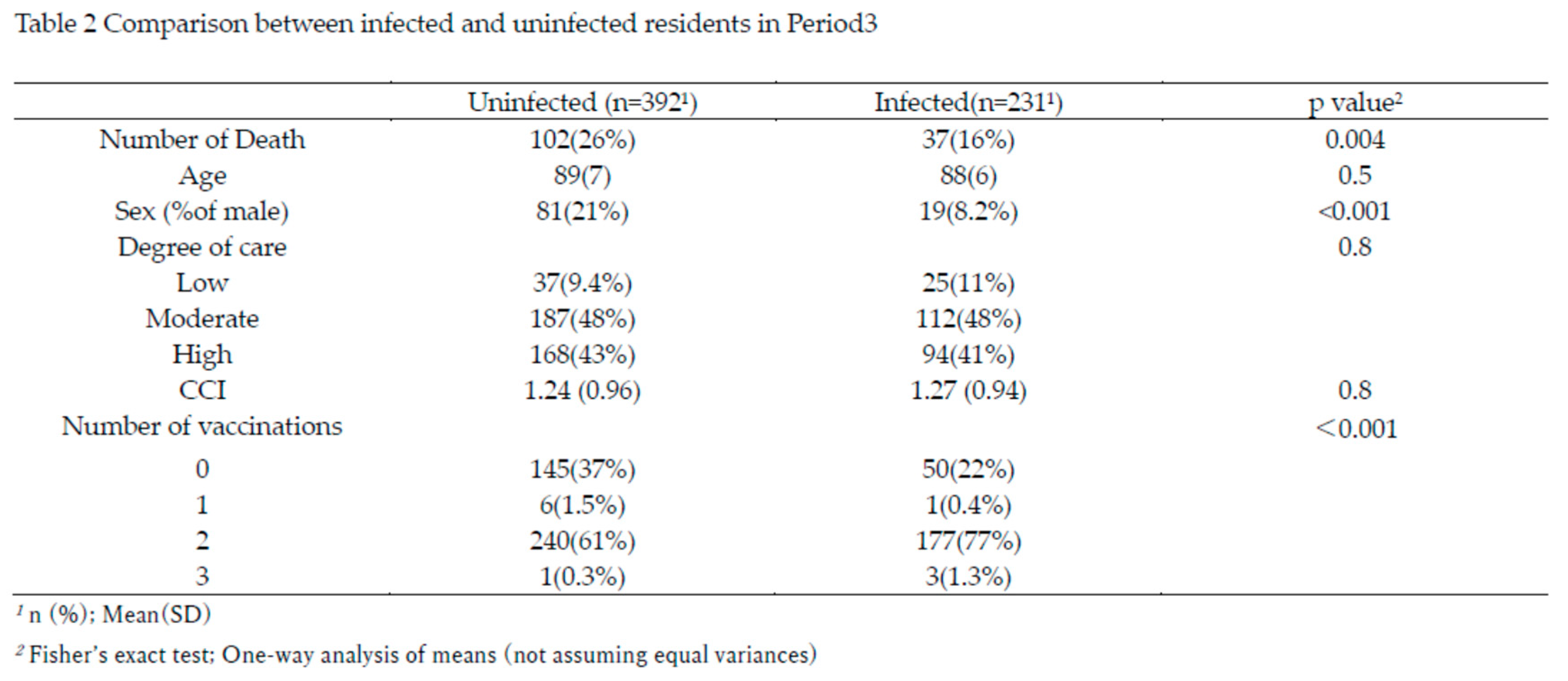
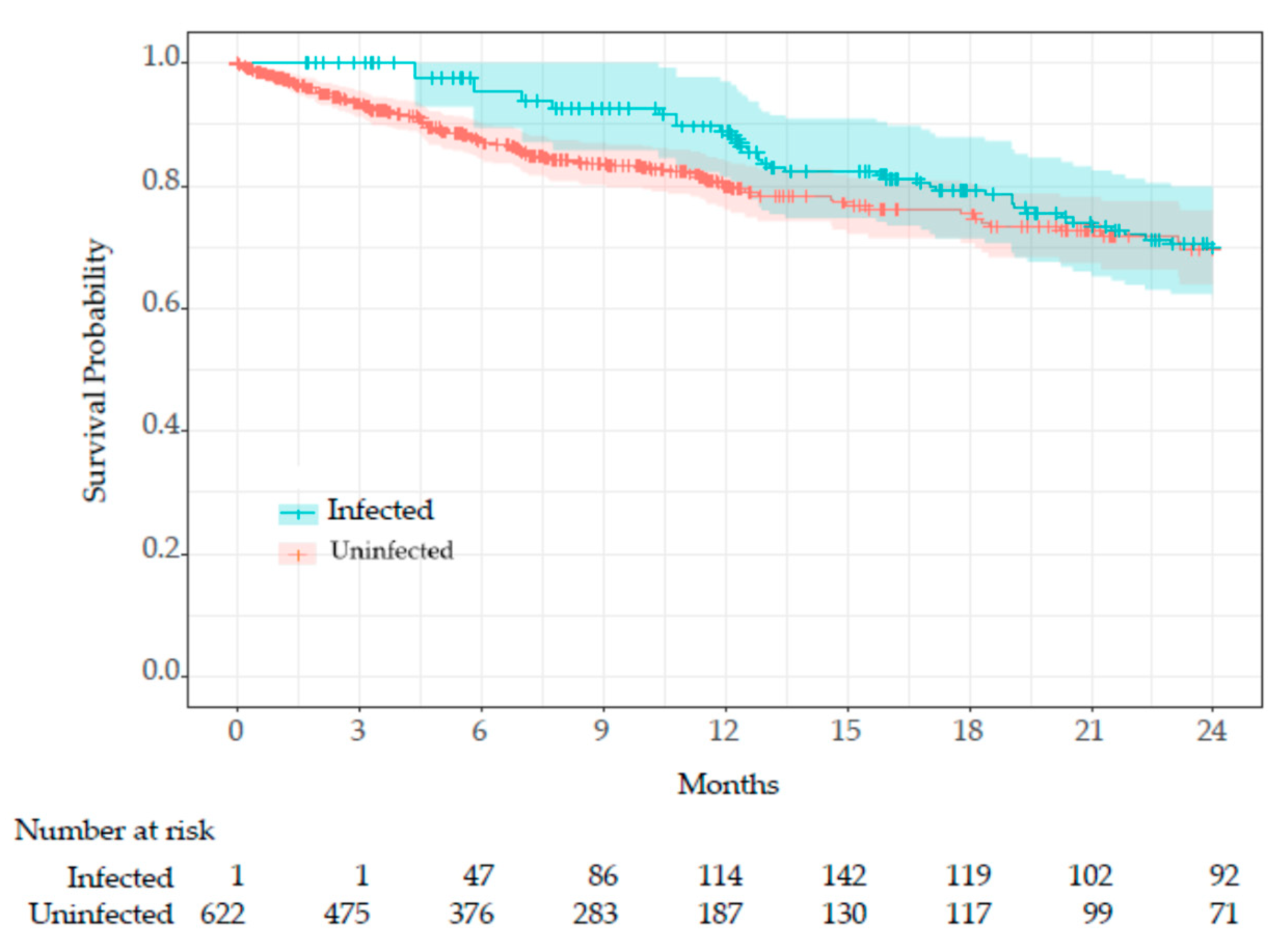
Comparison Between Infected and Uninfected Groups
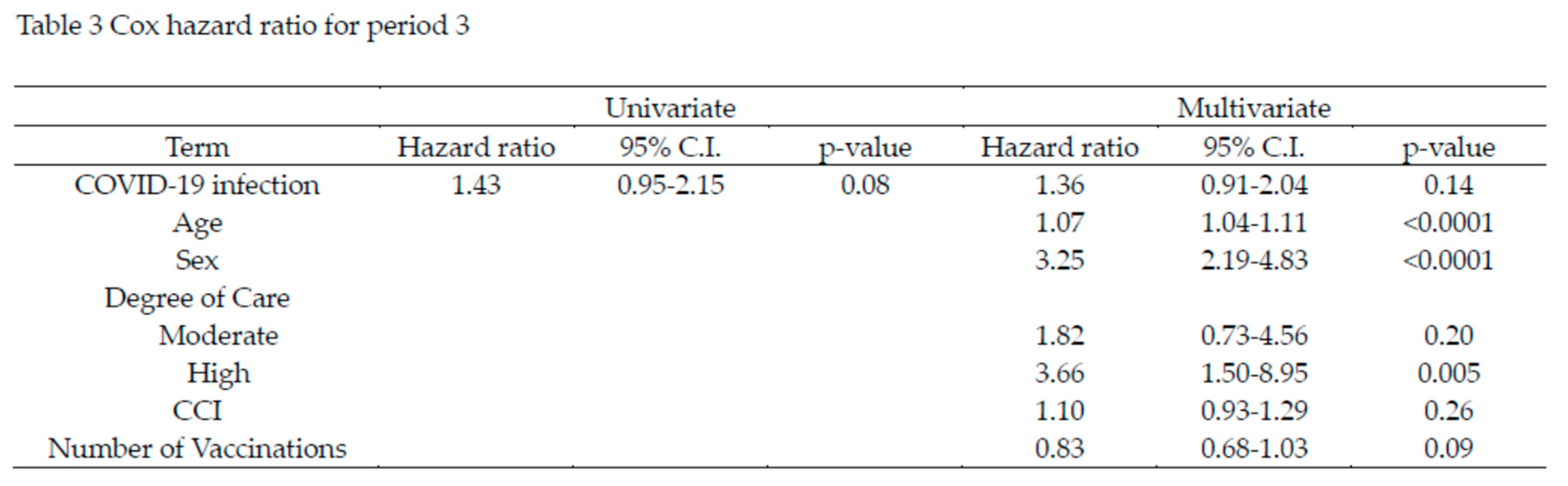
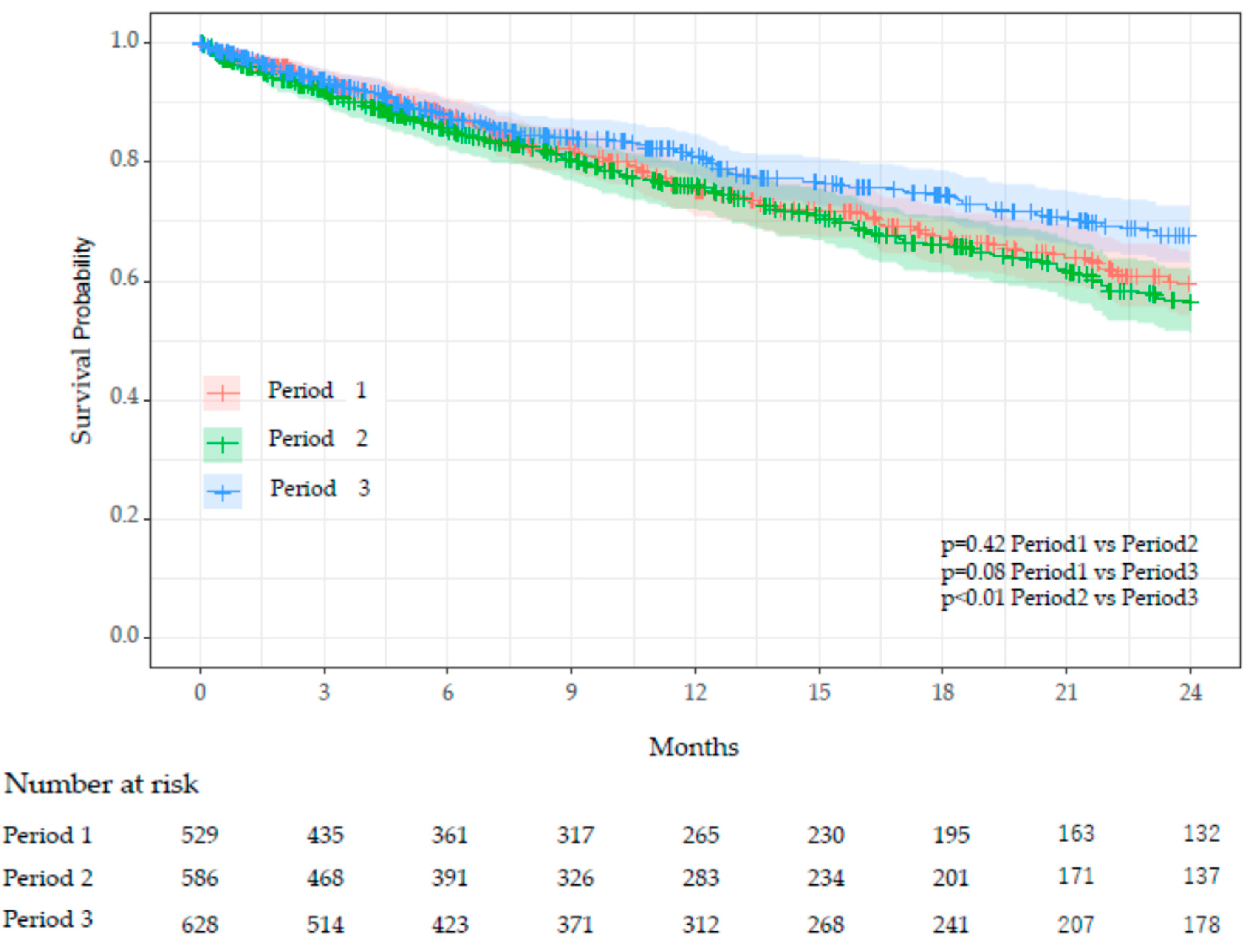
Comparison Between Periods
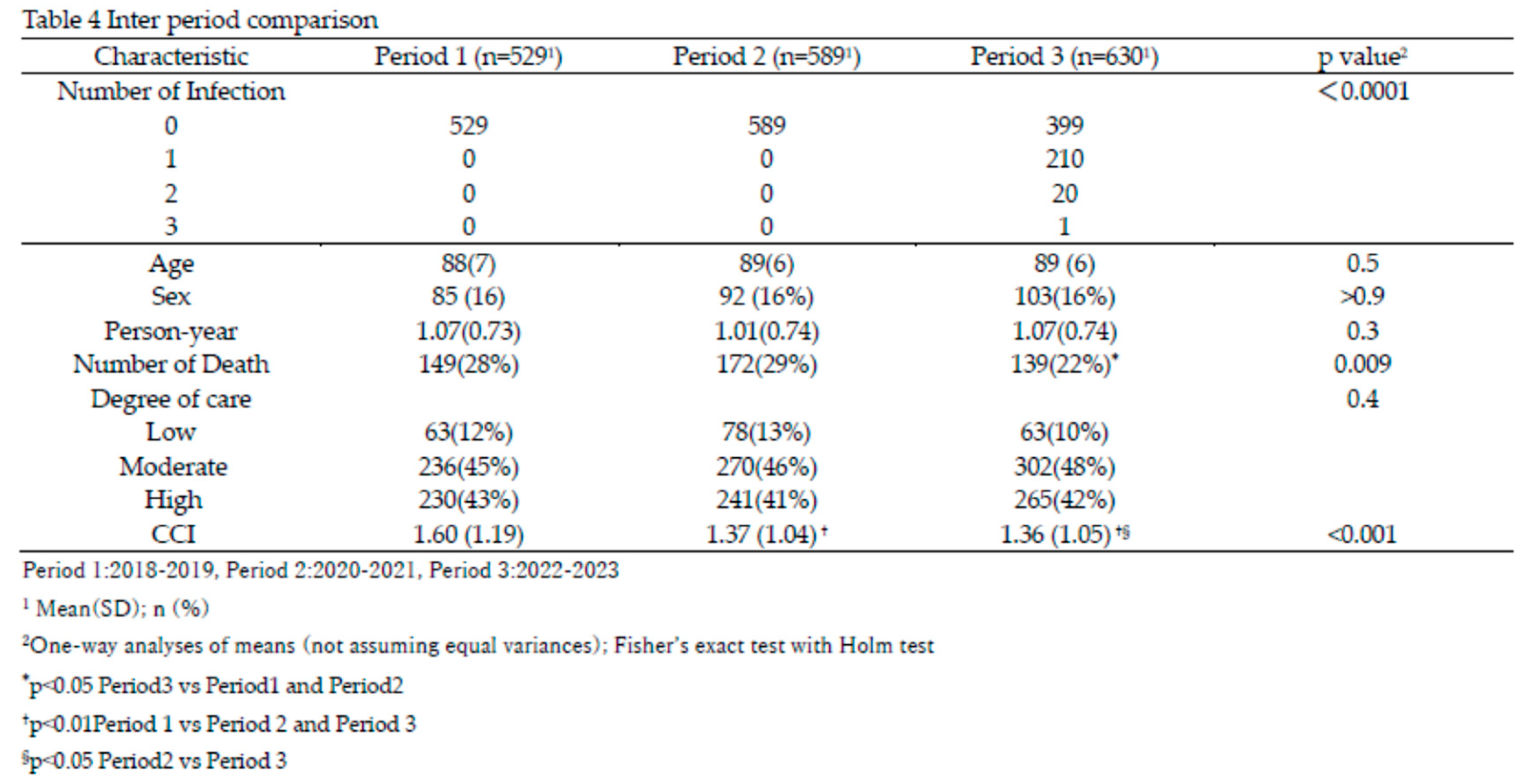
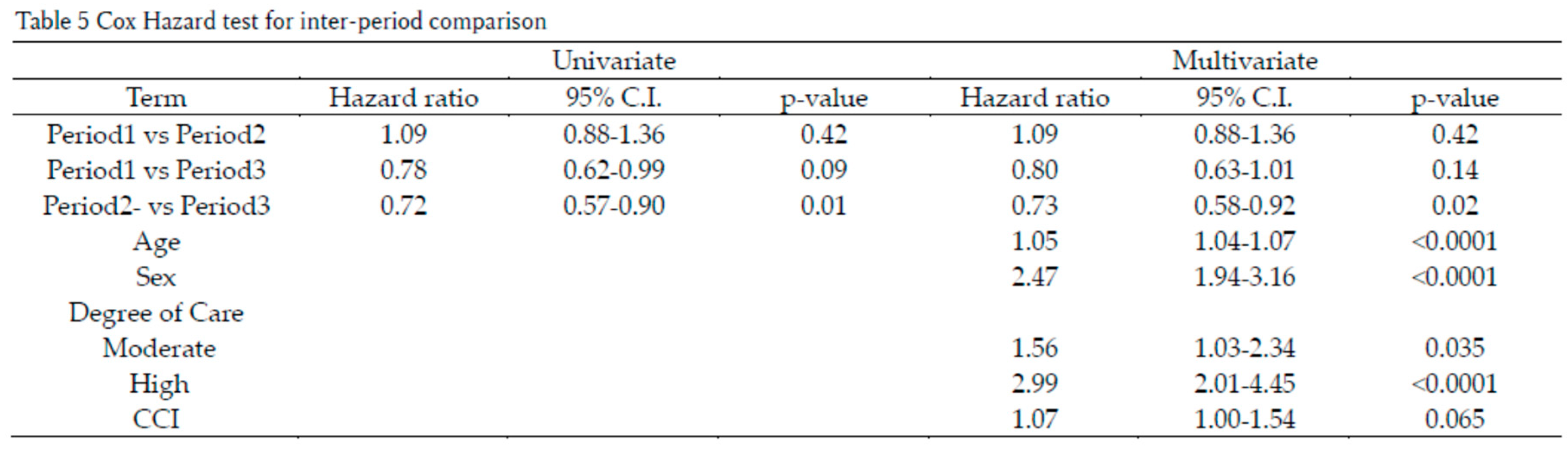
4. Discussion
5. Conclusions
6. Limitation
- Retrospective Design: This study utilized a retrospective observational approach, which may introduce inherent selection bias and limit the ability to establish causal relationships between interventions and outcomes.
- Single-Facility Data: The analysis was conducted in a single long-term care facility, potentially limiting the generalizability of the findings to other facilities with different demographic characteristics, healthcare systems, or infection control protocols.
- Unmeasured Confounding Factors: While efforts were made to adjust for age, sex, care levels, comorbidity index (CCI), and vaccination status, other potential confounders—such as undiagnosed asymptomatic infections or the presence of other comorbid conditions—were not comprehensively analyzed.
- Vaccination Effectiveness: The study observed significant differences in vaccination rates between infected and uninfected groups. However, the inability to directly compare vaccination timing and its potential confounding effect on outcomes limits the interpretation of its role in mitigating infection severity.
- Limited Scope on Respiratory Infections: The findings focus on SARS-CoV-2 outcomes. While preventive measures may mitigate the spread of other respiratory pathogens, this hypothesis was not directly examined.
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| LTCF | Long term care facility |
| SARS-CoV-2 | Severe acute respiratory syndrome coronavirus 2 |
| COVID-19 | Coronavirus disease-2019 |
| VOC | Variant of concern |
| C.I, | Confidence Interval |
References
- Worldometer. available at https://www.worldometers.info/coronavirus/.
- World Health Organization. WHO Coronavirus (COVID-19) Dashboard. available at https://data.who.int/dashboards/covid19/data.
- Harvey, W.T.; et al. SARS-CoV-2 variants, spike mutations and immune escape. Nat Rev Microbiol 2021, 19, 409–424. [Google Scholar] [CrossRef] [PubMed]
- Tao, K.; et al. The biological and clinical significance of emerging SARS-CoV-2 variants. Nat Rev Genet 2021, 22, 757–773. [Google Scholar] [CrossRef] [PubMed]
- Karim, S.S.A. and Q.A. Karim, Omicron SARS-CoV-2 variant: a new chapter in the COVID-19 pandemic. Lancet 2021, 398, 2126–2128. [Google Scholar] [CrossRef] [PubMed]
- Callaway, E.; Ledford, H. How bad is Omicron? What scientists know so far. Nature 2021, 600, 197–199. [Google Scholar] [CrossRef]
- Dejnirattisai, W.; et al. SARS-CoV-2 Omicron-B.1.1.529 leads to widespread escape from neutralizing antibody responses. Cell 2022, 185, 467–484. [Google Scholar] [CrossRef]
- Cao, Y.; et al. Omicron escapes the majority of existing SARS-CoV-2 neutralizing antibodies. Nature 2022, 602, 657–663. [Google Scholar] [CrossRef]
- Nyberg, T.; et al. Comparative analysis of the risks of hospitalisation and death associated with SARS-CoV-2 omicron (B.1.1.529) and delta (B.1.617.2) variants in England: a cohort study. Lancet 2022, 399, 1303–1312. [Google Scholar] [CrossRef]
- Singhal, T. ; The Emergence of Omicron: Challenging Times Are Here Again! Indian J Pediatr 2022, 89, 490–496. [Google Scholar] [CrossRef]
- Danielle-Iuliano, A.; Brunkard, J.M.; Boehmer,T.K. Peterson, E.; Adjei, A.; et al. Trends in Disease Severity and Health Care Utilization During the Early Omicron Variant Period Compared with Previous SARS-CoV-2 High Transmission Periods — United States, December 2020–January 2022, in Morbidity and Mortality Report. 2022, CDC. available at https://www.cdc.gov/mmwr/volumes/71/wr/mm7104e4.htm.
- Liu, Y.; et al. Reduction in the infection fatality rate of Omicron variant compared with previous variants in South Africa. Int J Infect Dis, 2022. 120: p. 146-149. [CrossRef]
- Ahmad, S.J.; et al. Fatality Rates After Infection With the Omicron Variant (B.1.1.529): How Deadly has it been? A Systematic Review and Meta-Analysis. J Acute Med 2024, 14, 51–60. [Google Scholar]
- Burton, J.K.; et al. Impact of COVID-19 on care-home mortality and life expectancy in Scotland. Age Ageing 2021, 50, 1029–1037. [Google Scholar] [CrossRef]
- Parra, P.N.B.; et al. The Effect of the COVID-19 Pandemic on the Elderly: Population Fatality Rates, COVID Mortality Percentage, and Life Expectancy Loss. Elder Law J 2022, 30, 33–80. [Google Scholar] [PubMed]
- Goldstein, J.R. and R.D. Lee, Demographic perspectives on the mortality of COVID-19 and other epidemics. Proc Natl Acad Sci U S A 2020, 117, 22035–22041. [Google Scholar] [CrossRef] [PubMed]
- Ma, B.H.; et al. Clinical Outcomes Following Treatment for COVID-19 With Nirmatrelvir/Ritonavir and Molnupiravir Among Patients Living in Nursing Homes. JAMA Netw Open 2023, 6, e2310887. [Google Scholar] [CrossRef] [PubMed]
- COVID-19 Treatment Clinical Care for Outpatients. CDC. available at https://www.cdc.gov/covid/hcp/clinical-care/outpatient-treatment.html.
- Shimizu, H.; et al. COVID-19 symptom-onset to diagnosis and diagnosis to treatment intervals are significant predictors of disease progression and hospitalization in high-risk patients: A real world analysis. Respir Investig 2023, 61, 220–229. [Google Scholar] [CrossRef]
- Chen, Y.J.; et al. Earlier diagnosis improves COVID-19 prognosis: a nationwide retrospective cohort analysis. Ann Transl Med 2021, 9, 941. [Google Scholar] [CrossRef]
- Huang, G.; et al. Timely Diagnosis and Treatment Shortens the Time to Resolution of Coronavirus Disease (COVID-19) Pneumonia and Lowers the Highest and Last CT Scores From Sequential Chest CT. AJR Am J Roentgenol 2020, 215, 367–373. [Google Scholar] [CrossRef]
- Konishi, T.; H. Inokuchi, and H. Yasunaga, Services in public long-term care insurance in Japan. Ann Clin Epidemiol 2024, 6, 1–4. [CrossRef]
- Nakazawa, E.; H. Ino, and A. Akabayashi Chronology of COVID-19 Cases on the Diamond Princess Cruise Ship and Ethical Considerations: A Report From Japan. Disaster Med Public Health Prep 2020, 14, 506–513. [CrossRef]
- Charlson, M.; et al. Validation of a combined comorbidity index. J Clin Epidemiol 1994, 47, 1245–1251. [Google Scholar] [CrossRef]
- Schultz, L.R.; E.L. Peterson, and N. Breslau, Graphing survival curve estimates for time-dependent covariates. Int J Methods Psychiatr Res 2002, 11, 68–74. [CrossRef]
- Zheng, Q.; et al. The influence of immortal time bias in observational studies examining associations of antifibrotic therapy with survival in idiopathic pulmonary fibrosis: A simulation study. Front Med (Lausanne) 2023, 10, 1157706. [Google Scholar] [CrossRef] [PubMed]
- Suissa, S. and S. Dell'Aniello, Time-related biases in pharmacoepidemiology. Pharmacoepidemiol Drug Saf 2020, 29, 1101–1110. [Google Scholar] [CrossRef] [PubMed]
- Hashan, M.R.; et al. Epidemiology and clinical features of COVID-19 outbreaks in aged care facilities: A systematic review and meta-analysis. EClinicalMedicine 2021, 33, 100771. [Google Scholar] [CrossRef] [PubMed]
- Duong, B.V.; et al. Is the SARS CoV-2 Omicron Variant Deadlier and More Transmissible Than Delta Variant? Int J Environ Res Public Health, 2022. 19(8). available at https://www.ncbi.nlm.nih.gov/pubmed/35457468.
- Severity of disease associated with Omicron variant as compared with Delta variant in hospitalized patients with suspected or confirmed SARS-CoV-2 infection. 2022. available at https://www.who.int/publications/i/item/9789240051829?utm_source=chatgpt.com.
- Guillermo V. Sanchez, G.V.; Biedron, C.; Fink, L.R.; Hatfield,K.M. , Polistico, J.M.F.; Meyer,M.P.;Noe,R.S. et al, Initial and Repeated Point Prevalence Surveys to Inform SARS-CoV-2 Infection Prevention in 26 Skilled Nursing Facilities — Detroit, Michigan, March–May 2020, in Morbidity and Mortality Weekly Report (MMWR). 2020, Center for Disease Control and Prevention. p. 882-886. available at ttps://www.cdc.gov/mmwr/volumes/69/wr/mm6927e1.htm?s_cid=mm6927e1_w.
- Madewell, Z.J.; et al. Rapid review and meta-analysis of serial intervals for SARS-CoV-2 Delta and Omicron variants. BMC Infect Dis 2023, 23, 429. [Google Scholar] [CrossRef]
- Xu, X.; et al. Assessing changes in incubation period, serial interval, and generation time of SARS-CoV-2 variants of concern: a systematic review and meta-analysis. BMC Med 2023, 21, 374. [Google Scholar] [CrossRef]
- Oksuzyan, A.; et al. Men: good health and high mortality. Sex differences in health and aging. Aging Clin Exp Res 2008, 20, 91–102. [Google Scholar] [CrossRef]
- Crimmins, E.M.; et al. Differences between Men and Women in Mortality and the Health Dimensions of the Morbidity Process. Clin Chem 2019, 65, 135–145. [Google Scholar] [CrossRef]
- Luy, M. and K. Gast, Do women live longer or do men die earlier? Reflections on the causes of sex differences in life expectancy. Gerontology 2014, 60, 143–153. [Google Scholar] [CrossRef]
- Pijls, B.G.; et al. Demographic risk factors for COVID-19 infection, severity, ICU admission and death: a meta-analysis of 59 studies. BMJ Open 2021, 11, e044640. [Google Scholar] [CrossRef]
- Yamaguchi, D.; et al. Potential Risk Factors to COVID-19 Severity: Comparison of SARS-CoV-2 Delta- and Omicron-Dominant Periods. Int J Environ Res Public Health 2024, 21. [Google Scholar] [CrossRef]
- Fan, Y.; et al. SARS-CoV-2 Omicron variant: recent progress and future perspectives. Signal Transduct Target Ther 2022, 7, 141. [Google Scholar] [CrossRef] [PubMed]
- Chidambaram, P.R.; R and Neuman,T.; Key Questions About Nursing Home Cases, Deaths, and Vaccinations as Omicron Spreads in the United States, in Coronavirus (COVID-19). 2022. available at https://www.cdc.gov/mmwr/volumes/73/wr/mm7312a5.htm.
- Link-Gelles, R.; Rowley,E.A.K.. DeSilva,M.B.; Dascomb,K.; Irving,S.A.; Klein,N.P. et al. Interim Effectiveness of Updated 2023–2024 (Monovalent XBB.1.5) COVID-19 Vaccines Against COVID-19–Associated Hospitalization Among Adults Aged ≥18 Years with Immunocompromising Conditions — VISION Network, September 2023–February 2024, M.a.M.W.R. (MMWR), Editor. 2024. p. 271–276. available at https://wwwnc.cdc.gov/eid/article/29/6/23-0130_article.
- Bloomfield, L.E. ; Ngeh,S.;Cadby,G.; Hutcheon,K. and Effle.P.V.; SARS-CoV-2 Vaccine Effectiveness against Omicron Variant in Infection-Naive Population, Australia, 2022. 2023, Center for Disease Control and Prevention.
- Chen, L.K.; et al. Predicting mortality of older residents in long-term care facilities: comorbidity or care problems? J Am Med Dir Assoc 2010, 11, 567–571. [Google Scholar] [CrossRef]
- Checovich, M.M.; et al. Evaluation of Viruses Associated With Acute Respiratory Infections in Long-Term Care Facilities Using a Novel Method: Wisconsin, 2016‒2019. J Am Med Dir Assoc 2020, 21, 29–33. [Google Scholar] [CrossRef] [PubMed]
- Influenza 2019/20 season, Japan, in Infectious Agents Surveillance Report. 2020, National Institute of Infectious Diseases. p. p191-193: November 2020.
- Otsuka, M.; et al. Respiratory syncytial virus infection notification trends and interpretation of the reported case data, 2018-2021, Japan. Jpn J Infect Dis, 2024.
- Sakamoto, H.; M. Ishikane, and P. Ueda, Seasonal Influenza Activity During the SARS-CoV-2 Outbreak in Japan. JAMA 2020, 323, 1969–1971. [CrossRef]
- Ujiie, M.; et al. Resurgence of Respiratory Syncytial Virus Infections during COVID-19 Pandemic, Tokyo, Japan. Emerg Infect Dis 2021, 27, 2969–2970. [Google Scholar] [CrossRef]
- Fukuda, Y.; et al. Resurgence of human metapneumovirus infection and influenza after three seasons of inactivity in the post-COVID-19 era in Hokkaido, Japan, 2022-2023. J Med Virol 2023, 95, e29299. [Google Scholar] [CrossRef]
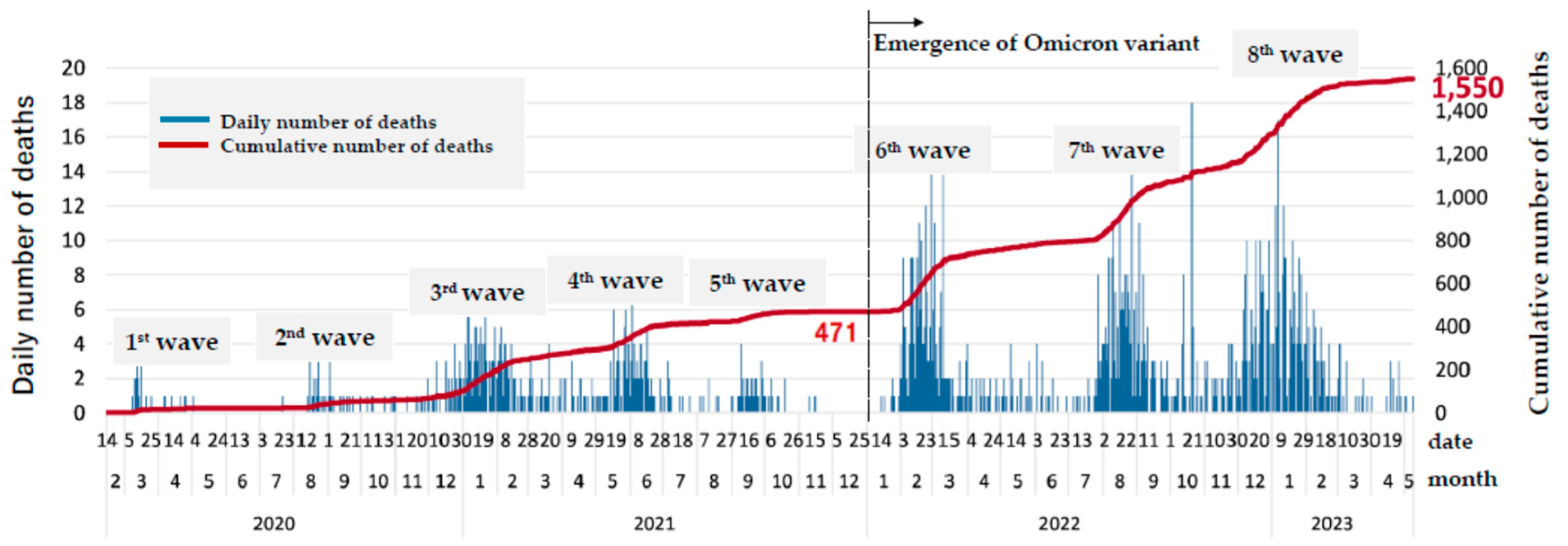
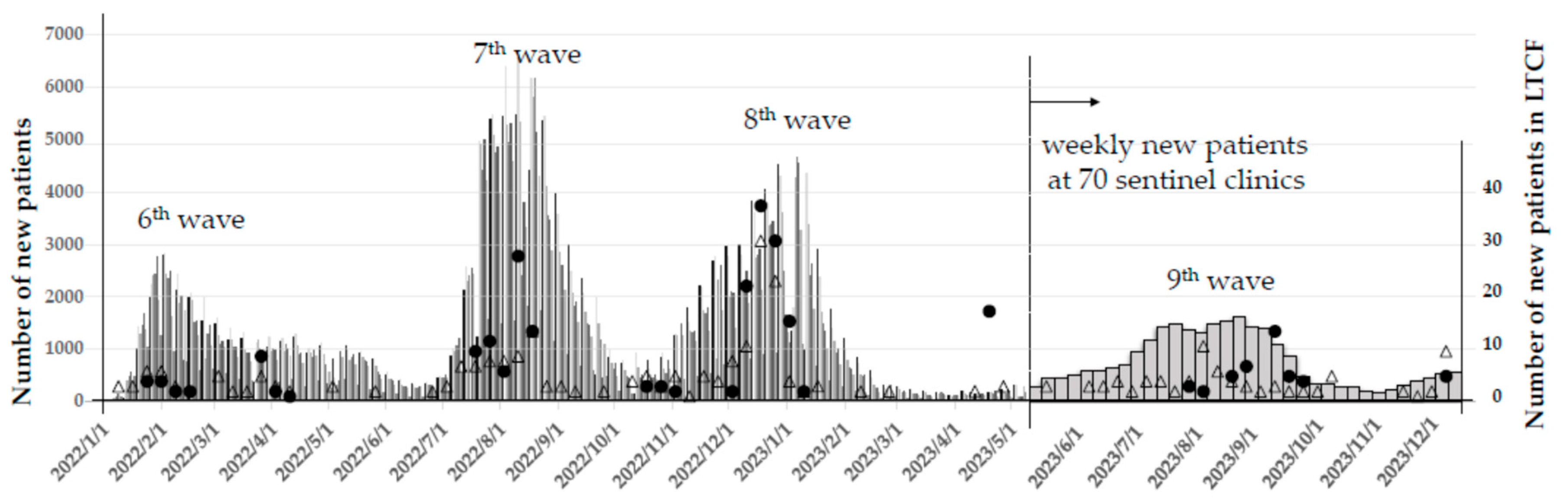
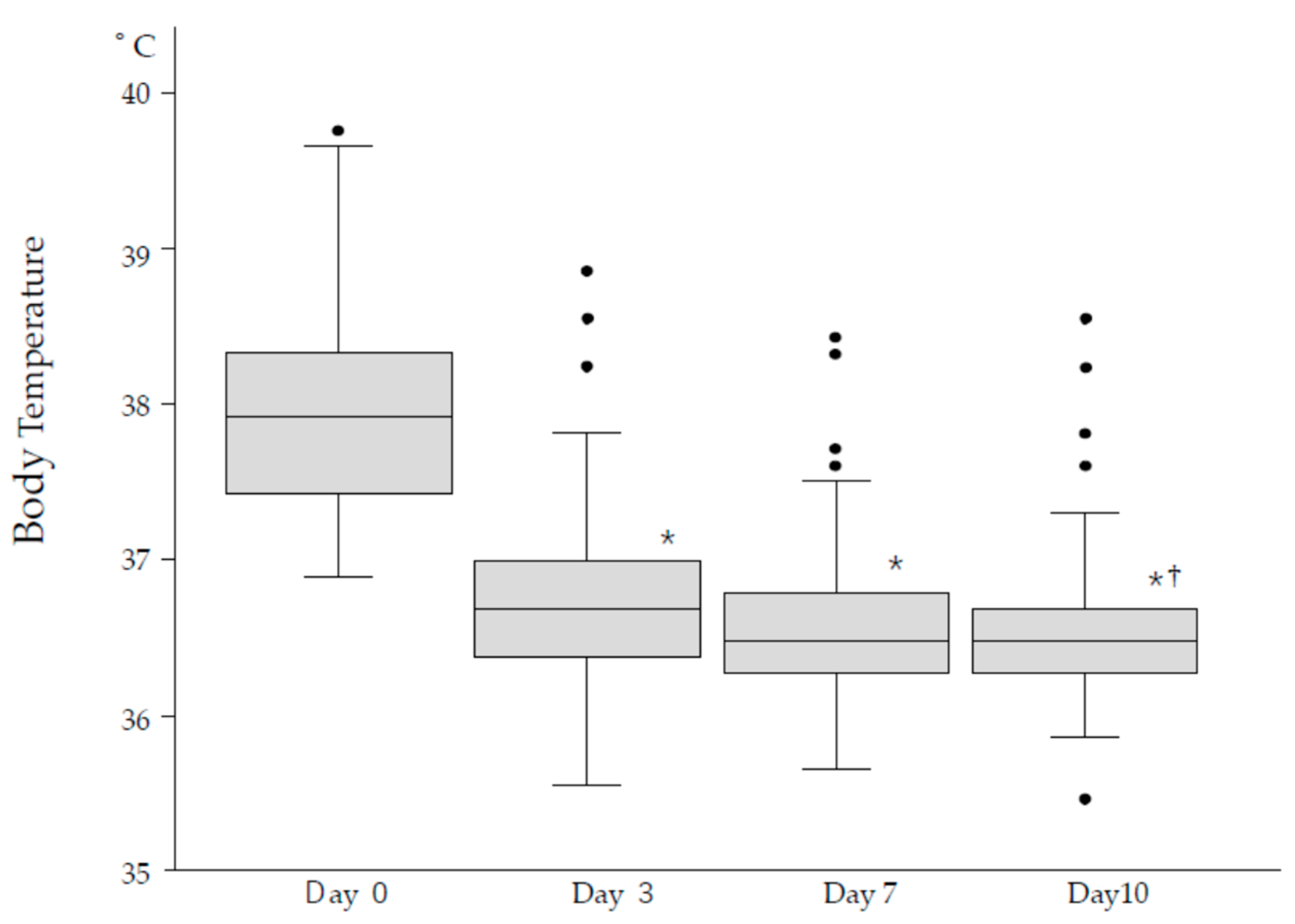
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



