Submitted:
13 February 2025
Posted:
14 February 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
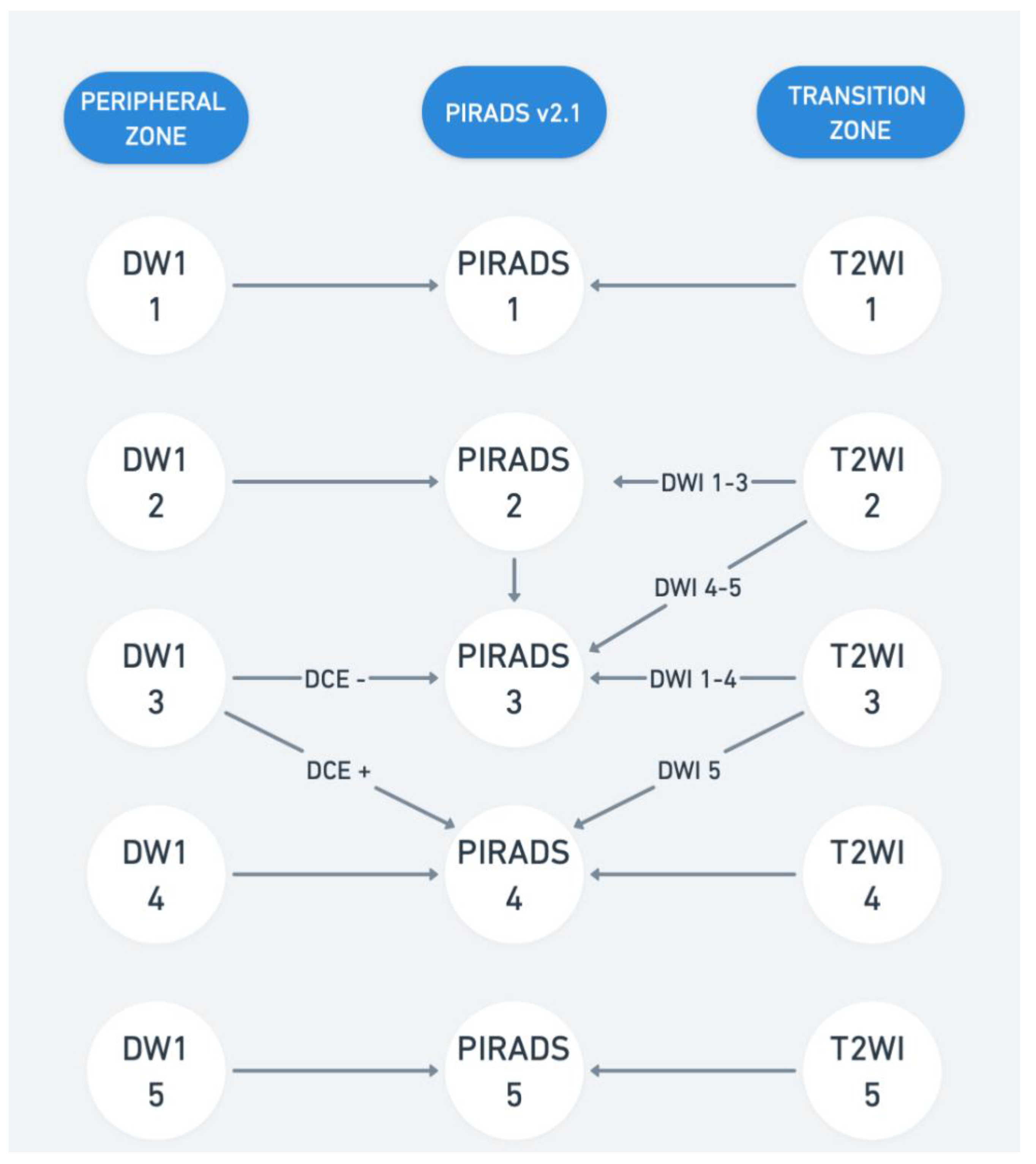
2. Magnetic Resonance Imaging (MRI)
3. MRI PCa Diagnosis in Biopsy-Naïve Patients
4. MRI PCa Diagnosis in Repeat Biopsy Settings
- For PI-RADS 3, csPCa detection ranged from 2.5% to 22%.
- For PI-RADS 4, csPCa detection ranged from 7.7% to 45%.
- For PI-RADS 5, csPCa detection reached up to 50%.
5. MRI and Active Surveillance
5. MRI and Staging
6. Benefits and Pitfalls of MRI
7. Micro-Ultrasound (MicrotUS)
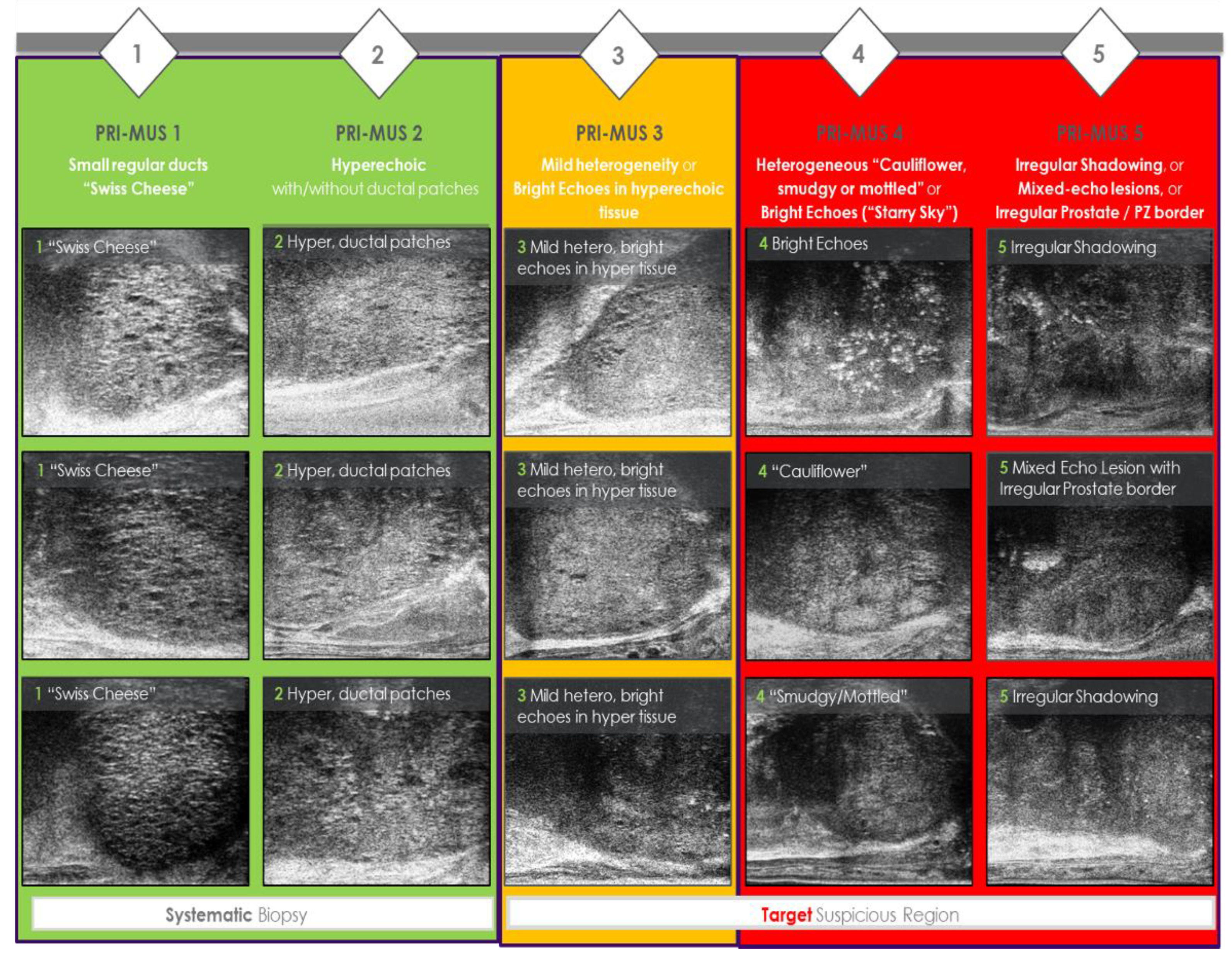
7. MicroUS Image Interpretation and PRI-MUS Scoring
- Anterior Prostate: Anterior tumors lack ducts, have a hypoechoic stroma, and are longer than tall. Larger lesions may show irregular borders or loss of surrounding fat. Benign prostatic hyperplasia (BPH) nodules, in contrast, appear as taller-than-long structures with smooth, hyperechoic capsules and occasional ducts or cysts.
- Central Zone: Rarely affected by cancer (3%), this zone serves as a reference for evaluating echogenicity. Identifying midline landmarks, such as the verumontanum, helps differentiate normal ducts from cancerous areas.
- Peripheral Zone: Large, visible ducts indicate no cancer (PRI-MUS 1). As ducts shrink or disappear, the lesion progresses to PRI-MUS 2 or higher. A mixed or mottled echogenic background suggests PRI-MUS 4, while a hypoechoic or isoechoic background relative to the central zone suggests PRI-MUS 5. Larger cancers may disrupt adjacent tissue or the prostate capsule.
8. Microus and Pca Diagnosis in Biopsy-Naïve Patients
9. Microus and PCa Diagnosis in Repeat Biopsy Settings
10. Microus and Active Suirveillance
10. Microus and Staging
- Visible breach of the prostate capsule
- Capsular bulging
- Obliteration of the prostatic-seminal vesicle angle
- Presence of a hypoechoic halo
- Capsular contact length ≥15 mm
11. Benefits and Pitfalls of Microus
12. Conclusion
Funding
Conflicts of Interest
References
- Panebianco, V.; Barchetti, F.; Sciarra, A.; Ciardi, A.; Indino, E.L.; Papalia, R.; et al. Multiparametric magnetic resonance imaging vs. standard care in men being evaluated for prostate cancer: A randomized study. Urologic Oncology: Seminars and Original Investigations 2015, 33, 17.e1–17.e7. [Google Scholar] [CrossRef]
- Haffner, J.; Lemaitre, L.; Puech, P.; Haber, G.-P.; Leroy, X.; Jones, J.S.; et al. Role of magnetic resonance imaging before initial biopsy: comparison of magnetic resonance imaging-targeted and systematic biopsy for significant prostate cancer detection. BJU International 2011, 108, E171–8. [Google Scholar] [CrossRef]
- van der Leest, M.; Cornel, E.; Israël, B.; Hendriks, R.; Padhani, A.R.; Hoogenboom, M.; et al. Head-to-head Comparison of Transrectal Ultrasound-guided Prostate Biopsy Versus Multiparametric Prostate Resonance Imaging with Subsequent Magnetic Resonance-guided Biopsy in Biopsy-naïve Men with Elevated Prostate-specific Antigen: A Large Prospective Multicenter Clinical Study. European Urology 2019, 75, 570–8. [Google Scholar] [CrossRef] [PubMed]
- Kasivisvanathan, V.; Rannikko, A.S.; Borghi, M.; Panebianco, V.; Mynderse, L.A.; Vaarala, M.H.; et al. MRI-Targeted or Standard Biopsy for Prostate-Cancer Diagnosis. New England Journal of Medicine 2018, 378, 1767–77. [Google Scholar] [CrossRef]
- Klotz, L.; Chin, J.; Black, P.C.; Finelli, A.; Anidjar, M.; Bladou, F.; et al. Comparison of Multiparametric Magnetic Resonance Imaging–Targeted Biopsy With Systematic Transrectal Ultrasonography Biopsy for Biopsy-Naive Men at Risk for Prostate Cancer: A Phase 3 Randomized Clinical Trial. JAMA Oncology 2021, 7, 534–42. [Google Scholar] [CrossRef] [PubMed]
- Klotz, L.; Chin, J.; Black, P.C.; Finelli, A.; Anidjar, M.; Machado, A.; et al. Magnetic Resonance Imaging–Targeted Versus Systematic Prostate Biopsies: 2-year Follow-up of a Prospective Randomized Trial (PRECISE). European Urology Oncology 2024, 7, 456–61. [Google Scholar] [CrossRef] [PubMed]
- Shaw, G.L.; Thomas, B.C.; Dawson, S.N.; Srivastava, G.; Vowler, S.L.; Gnanapragasam, V.J.; et al. Identification of pathologically insignificant prostate cancer is not accurate in unscreened men. Br J Cancer 2014, 110, 2405–11. [Google Scholar] [CrossRef]
- Abraham, N.E.; Mendhiratta, N.; Taneja, S.S. Patterns of Repeat Prostate Biopsy in Contemporary Clinical Practice. Journal of Urology 2015, 193, 1178–84. [Google Scholar] [CrossRef]
- Drost, F.-J.H.; Osses, D.; Nieboer, D.; Bangma, C.H.; Steyerberg, E.W.; Roobol, M.J.; et al. Prostate Magnetic Resonance Imaging, with or Without Magnetic Resonance Imaging-targeted Biopsy, and Systematic Biopsy for Detecting Prostate Cancer: A Cochrane Systematic Review and Meta-analysis. European Urology 2020, 77, 78–94. [Google Scholar] [CrossRef]
- Barkovich, E.J.; Shankar, P.R.; Westphalen, A.C. A Systematic Review of the Existing Prostate Imaging Reporting and Data System Version 2 (PI-RADSv2) Literature and Subset Meta-Analysis of PI-RADSv2 Categories Stratified by Gleason Scores. American Journal of Roentgenology 2019, 212, 847–54. [Google Scholar] [CrossRef]
- Zawaideh, J.P.; Sala, E.; Pantelidou, M.; Shaida, N.; Koo, B.; Caglic, I.; et al. Comparison of Likert and PI-RA DS version 2 MRI scoring systems for the detection of clinically significant prostate cancer. British Journal of Radiology 2020, 93. [Google Scholar] [CrossRef] [PubMed]
- Grivas, N.; Lardas, M.; Espinós, E.L.; Lam, T.B.; Rouviere, O.; Mottet, N.; et al. Prostate Cancer Detection Percentages of Repeat Biopsy in Patients with Positive Multiparametric Magnetic Resonance Imaging (Prostate Imaging Reporting and Data System/Likert 3–5) and Negative Initial Biopsy. A Mini Systematic Review. European Urology 2022, 82, 452–7. [Google Scholar] [CrossRef] [PubMed]
- Diagnosing prostate cancer: PROGENSA PCA3 assay and Prostate Health Index | Guidance | NICE 2015. https://www.nice.org.uk/guidance/dg17 (accessed June 18, 2024).
- Rajwa, P.; Pradere, B.; Quhal, F.; Mori, K.; Laukhtina, E.; Huebner, N.A.; et al. Reliability of Serial Prostate Magnetic Resonance Imaging to Detect Prostate Cancer Progression During Active Surveillance: A Systematic Review and Meta-analysis. Eur Urol 2021, 80, 549–63. [Google Scholar] [CrossRef]
- Oliveira, T.; Ferreira, L.A.; Marto, C.M.; Marques, C.; Oliveira, C.; Donato, P. The Role of Multiparametric MRI in the Local Staging of Prostate Cancer. FBE 2023, 15, 21. [Google Scholar] [CrossRef] [PubMed]
- Westphalen, A.C.; McCulloch, C.E.; Anaokar, J.M.; Arora, S.; Barashi, N.S.; Barentsz, J.O.; et al. Variability of the Positive Predictive Value of PI-RADS for Prostate MRI across 26 Centers: Experience of the Society of Abdominal Radiology Prostate Cancer Disease-focused Panel. Radiology 2020, 296, 76–84. [Google Scholar] [CrossRef]
- Murray, J.; Tree, A.C. Prostate cancer – Advantages and disadvantages of MR-guided RT. Clinical and Translational Radiation Oncology 2019, 18, 68–73. [Google Scholar] [CrossRef]
- Ahmed, H.U.; El-Shater Bosaily, A.; Brown, L.C.; Gabe, R.; Kaplan, R.; Parmar, M.K.; et al. Diagnostic accuracy of multi-parametric MRI and TRUS biopsy in prostate cancer (PROMIS): a paired validating confirmatory study. Lancet 2017, 389, 815–22. [Google Scholar] [CrossRef]
- Rosenkrantz, A.B.; Taneja, S.S. Radiologist, Be Aware: Ten Pitfalls That Confound the Interpretation of Multiparametric Prostate MRI. American Journal of Roentgenology 2014, 202, 109–20. [Google Scholar] [CrossRef]
- Lughezzani, G.; Saita, A.; Lazzeri, M.; Paciotti, M.; Maffei, D.; Lista, G.; et al. Comparison of the Diagnostic Accuracy of Micro-ultrasound and Magnetic Resonance Imaging/Ultrasound Fusion Targeted Biopsies for the Diagnosis of Clinically Significant Prostate Cancer. European Urology Oncology 2019, 2, 329–32. [Google Scholar] [CrossRef]
- Ghai, S.; Perlis, N.; Atallah, C.; Jokhu, S.; Corr, K.; Lajkosz, K.; et al. Comparison of Micro-US and Multiparametric MRI for Prostate Cancer Detection in Biopsy-Naive Men. Radiology 2022, 305, 390–8. [Google Scholar] [CrossRef]
- Cotter, F.; Perera, S.; Sathianathen, N.; Lawrentschuk, N.; Murphy, D.; Bolton, D. Comparing the Diagnostic Performance of Micro- Ultrasound-Guided Biopsy Versus Multiparametric Magnetic Resonance Imaging-Targeted Biopsy in the Detection of Clinically Significant Prostate Cancer: A Systematic Review and Meta-Analysis. Société Internationale d’Urologie Journal 2023, 4, 465–79. [Google Scholar] [CrossRef]
- Sountoulides, P.; Pyrgidis, N.; Polyzos, S.A.; Mykoniatis, I.; Asouhidou, E.; Papatsoris, A.; et al. Micro-Ultrasound–Guided vs Multiparametric Magnetic Resonance Imaging-Targeted Biopsy in the Detection of Prostate Cancer: A Systematic Review and Meta-Analysis. The Journal of Urology 2021. [Google Scholar] [CrossRef]
- Avolio, P.P.; Lughezzani, G.; Paciotti, M.; Maffei, D.; Uleri, A.; Frego, N.; et al. The use of 29 MHz transrectal micro-ultrasound to stratify the prostate cancer risk in patients with PI-RADS III lesions at multiparametric MRI: A single institutional analysis. Urologic Oncology: Seminars and Original Investigations 2021, 39, e1–e832. [Google Scholar] [CrossRef] [PubMed]
- Klotz, L.; Andriole, G.; Cash, H.; Cooperberg, M.; Crawford, E.D.; Emberton, M.; et al. Optimization of prostate biopsy - Micro-Ultrasound versus MRI (OPTIMUM): A 3-arm randomized controlled trial evaluating the role of 29 MHz micro-ultrasound in guiding prostate biopsy in men with clinical suspicion of prostate cancer. Contemporary Clinical Trials 2022, 112, 106618. [Google Scholar] [CrossRef]
- Beatrici, E.; Frego, N.; Chiarelli, G.; Sordelli, F.; Mancon, S.; Saitta, C.; et al. A Comparative Evaluation of Multiparametric Magnetic Resonance Imaging and Micro-Ultrasound for the Detection of Clinically Significant Prostate Cancer in Patients with Prior Negative Biopsies. Diagnostics 2024, 14, 525. [Google Scholar] [CrossRef] [PubMed]
- Klotz, L. Active surveillance in intermediate-risk prostate cancer. BJU International 2020, 125, 346–54. [Google Scholar] [CrossRef]
- Klotz, L.; Vesprini, D.; Sethukavalan, P.; Jethava, V.; Zhang, L.; Jain, S.; et al. Long-Term Follow-Up of a Large Active Surveillance Cohort of Patients With Prostate Cancer. Journal of Clinical Oncology 2015. [Google Scholar] [CrossRef]
- Chen, R.C.; Rumble, R.B.; Loblaw, D.A.; Finelli, A.; Ehdaie, B.; Cooperberg, M.R.; et al. Active Surveillance for the Management of Localized Prostate Cancer (Cancer Care Ontario Guideline): American Society of Clinical Oncology Clinical Practice Guideline Endorsement. JCO 2016, 34, 2182–90. [Google Scholar] [CrossRef]
- Mahal, B.A.; Butler, S.; Franco, I.; Spratt, D.E.; Rebbeck, T.R.; D’Amico, A.V.; et al. Use of Active Surveillance or Watchful Waiting for Low-Risk Prostate Cancer and Management Trends Across Risk Groups in the United States, 2010-2015. JAMA 2019, 321, 704–6. [Google Scholar] [CrossRef]
- Tosoian, J.J.; Mamawala, M.; Epstein, J.I.; Landis, P.; Macura, K.J.; Simopoulos, D.N.; et al. Active Surveillance of Grade Group 1 Prostate Cancer: Long-term Outcomes from a Large Prospective Cohort. European Urology 2020, 77, 675–82. [Google Scholar] [CrossRef]
- Klotz, L.; Pond, G.; Loblaw, A.; Sugar, L.; Moussa, M.; Berman, D.; et al. Randomized Study of Systematic Biopsy Versus Magnetic Resonance Imaging and Targeted and Systematic Biopsy in Men on Active Surveillance (ASIST): 2-year Postbiopsy Follow-up. European Urology 2020, 77, 311–7. [Google Scholar] [CrossRef]
- Albers, P.; Wang, B.; Broomfield, S.; Medina Martín, A.; Fung, C.; Kinnaird, A. Micro-ultrasound Versus Magnetic Resonance Imaging in Prostate Cancer Active Surveillance. European Urology Open Science 2022, 46, 33–5. [Google Scholar] [CrossRef] [PubMed]
- Maffei, D.; Fasulo, V.; Avolio, P.P.; Saitta, C.; Paciotti, M.; De Carne, F.; et al. Diagnostic performance of microUltrasound at MRI-guided confirmatory biopsy in patients under active surveillance for low-risk prostate cancer. Prostate 2023, 83, 886–95. [Google Scholar] [CrossRef] [PubMed]
- Regis, F.; Casale, P.; Persico, F.; Colombo, P.; Cieri, M.; Guazzoni, G.; et al. Use of 29-MHz Micro-ultrasound for Local Staging of Prostate Cancer in Patients Scheduled for Radical Prostatectomy: A Feasibility Study. European Urology Open Science 2020, 19, 20–3. [Google Scholar] [CrossRef] [PubMed]
- Fasulo, V.; Buffi, N.M.; Regis, F.; Paciotti, M.; Persico, F.; Maffei, D.; et al. Use of high-resolution micro-ultrasound to predict extraprostatic extension of prostate cancer prior to surgery: a prospective single-institutional study. World J Urol 2022, 40, 435–42. [Google Scholar] [CrossRef]
- Pedraza, A.M.; Parekh, S.; Joshi, H.; Grauer, R.; Wagaskar, V.; Zuluaga, L.; et al. Side-specific, Microultrasound-based Nomogram for the Prediction of Extracapsular Extension in Prostate Cancer. European Urology Open Science 2023, 48, 72–81. [Google Scholar] [CrossRef]
- Claros, O.R.; Tourinho-Barbosa, R.R.; Fregeville, A.; Gallardo, A.C.; Muttin, F.; Carneiro, A.; et al. Comparison of Initial Experience with Transrectal Magnetic Resonance Imaging Cognitive Guided Micro-Ultrasound Biopsies versus Established Transperineal Robotic Ultrasound Magnetic Resonance Imaging Fusion Biopsies for Prostate Cancer. The Journal of Urology 2020. [CrossRef]
- Lorusso, V.; Kabre, B.; Pignot, G.; Branger, N.; Pacchetti, A.; Thomassin-Piana, J.; et al. Comparison Between Micro-Ultrasound and Multiparametric MRI Regarding the Correct Identification of Prostate Cancer Lesions. Clin Genitourin Cancer 2022, 20, e339–45. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).