Submitted:
07 February 2025
Posted:
10 February 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Material and Methods
2.1. Inclusion Criteria
2.2. Exclusion Criteria
2.3. Clinical Evaluation
2.4. Risk Factor Evaluation
2.5. Investigations
2.6. MRI and MR Venography
2.7. Mechanical Ventilation
- (a)
- PaO2 < 60 mm of Hg on venti musk
- (b)
- PaCO2 > 50mm of Hg
- (c)
- pH< 7.3
2.8. Treatment
2.9. Outcome
2.10. Statistical Analysis
3. Results
3.1. Comparison of MV and Non-MV Patients
3.2. Comparison of Clinical Parameters
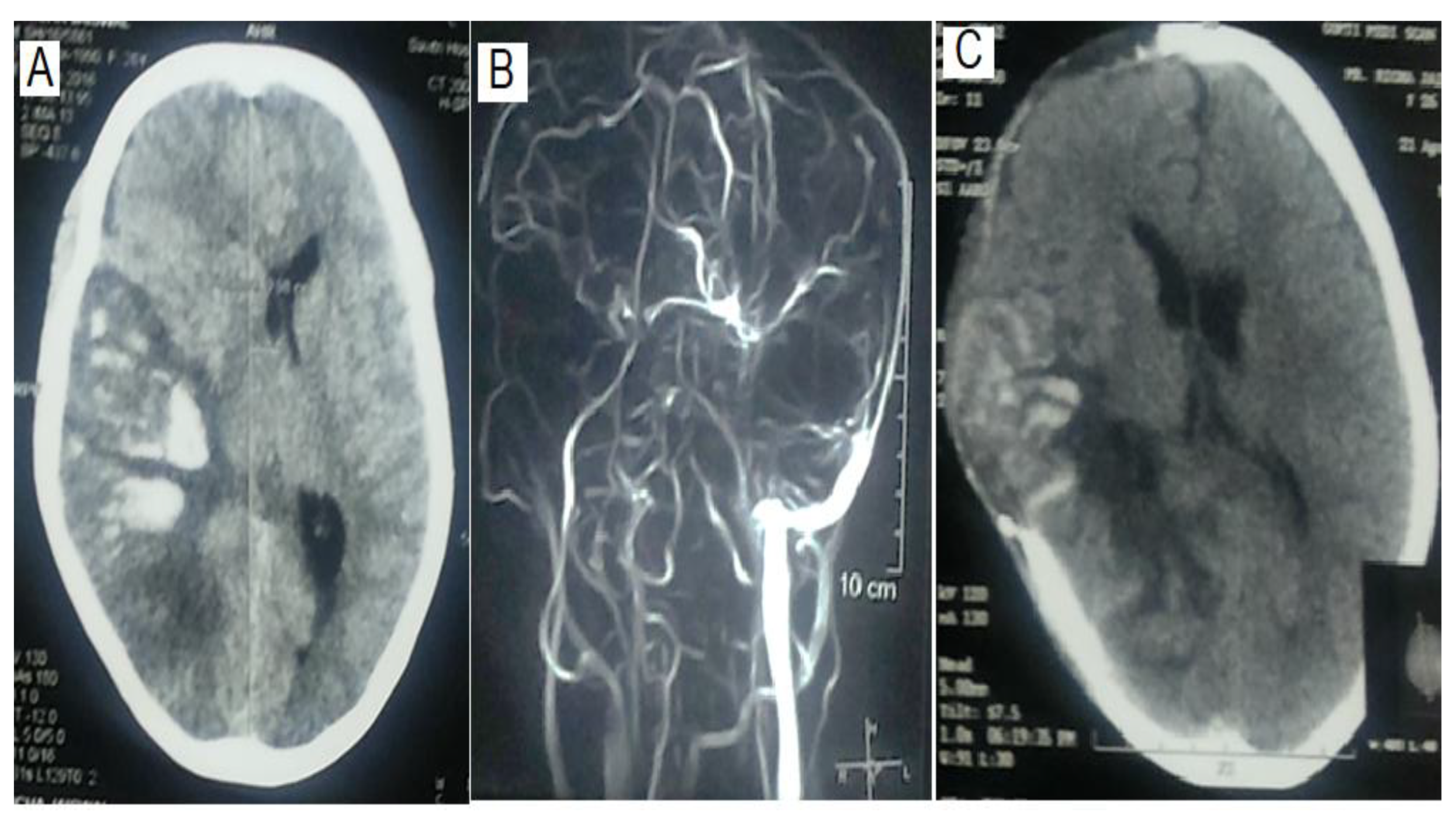
3.3. Comparison of MRV and MRI Findings
3.4. Comparison of Risk Factors
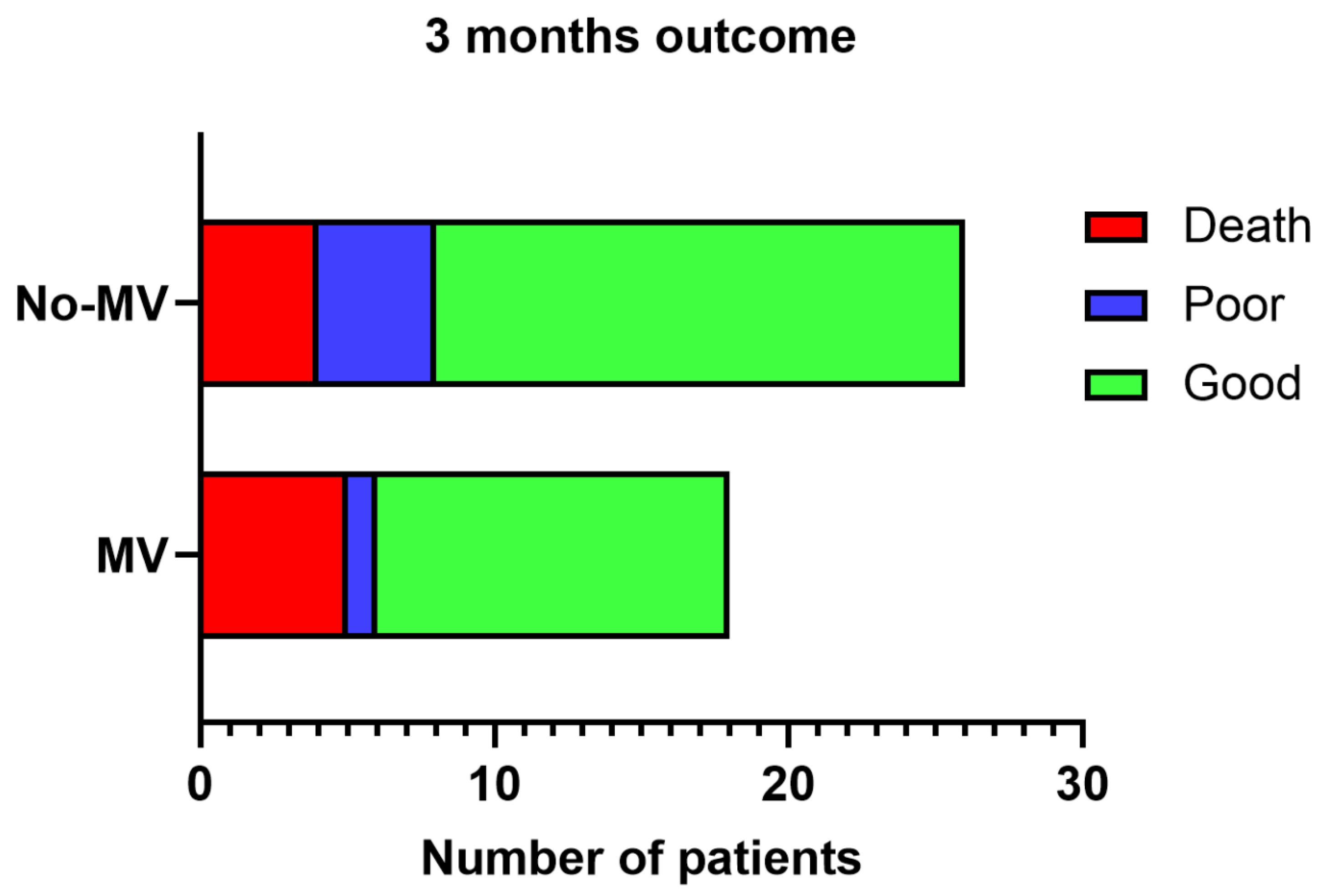
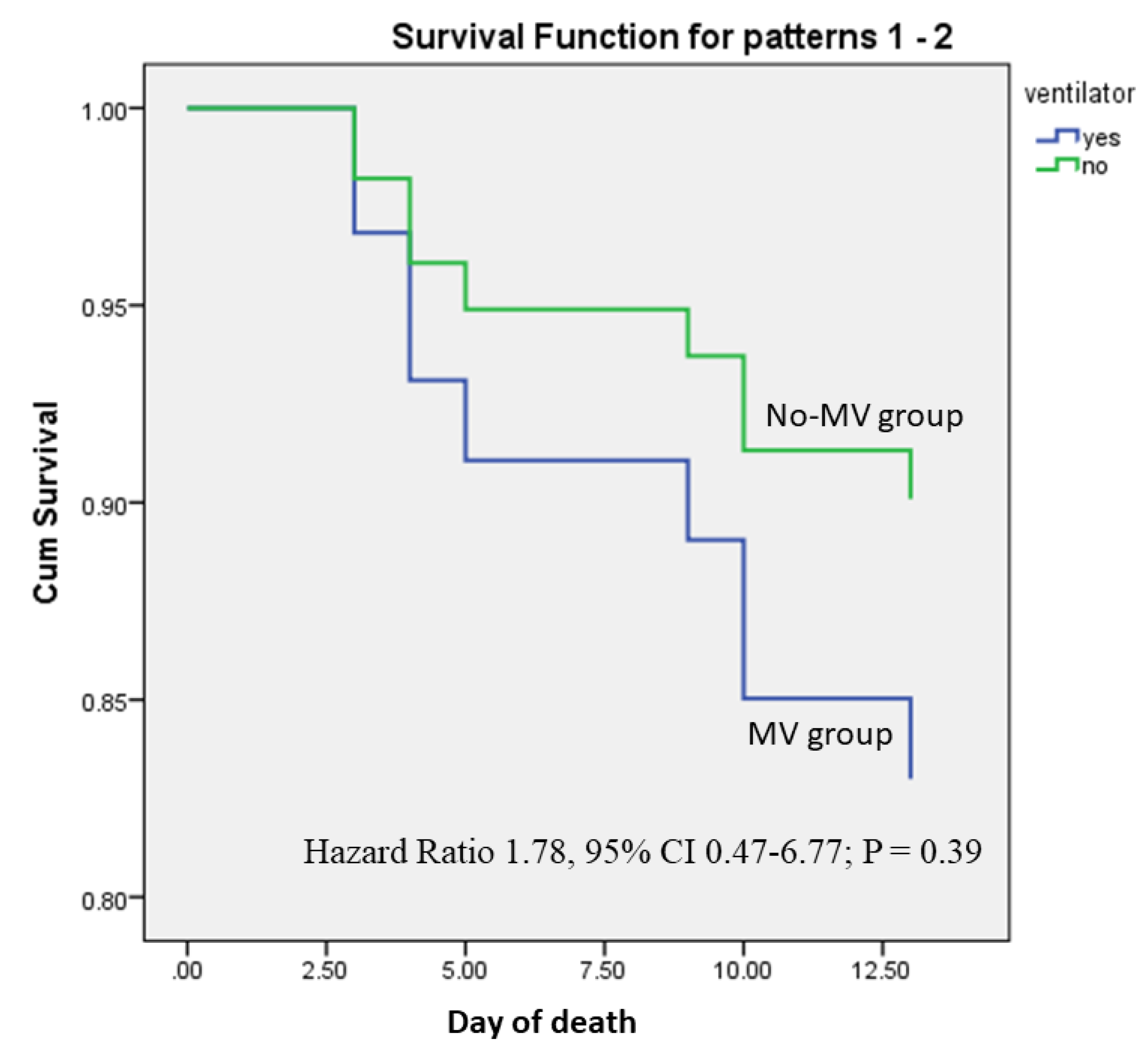
3.5. Outcome
3.6. Predictors of Death
4. Discussion
5. Limitation
6. Conclusion
Funding
Author’s contribution
Acknowledgments
Ethical Approval
Informed consent form
Conflicts of Interest
Data Statement
References
- GBD 2019 Stroke Collaborators. Global, regional, and national burden of stroke and its risk factors, 1990-2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet. Neurol. 2021, 20, 795–820. [Google Scholar] [CrossRef]
- de Montmollin, E. , Terzi, N., Dupuis, C., Garrouste-Orgeas, M., da Silva, D., Darmon, M., Laurent, V., Thiéry, G., Oziel, J., Marcotte, G., Gainnier, M., Siami, S., Sztrymf, B., Adrie, C., Reignier, J., Ruckly, S., Sonneville, R., Timsit, J. F., & OUTCOMEREA Study Group One-year survival in acute stroke patients requiring mechanical ventilation: a multicenter cohort study. Ann. Intensive Care 2020, 10, 53. [Google Scholar]
- Lahiri, S.; Mayer, S.A.; Fink, M.E.; Lord, A.S.; Rosengart, A.; Mangat, H.S.; Segal, A.Z.; Claassen, J.; Kamel, H. Mechanical Ventilation for Acute Stroke: A Multi-state Population-Based Study. Neurocritical Care 2015, 23, 28–32. [Google Scholar] [CrossRef] [PubMed]
- Young, P. , Beasley, R. , Bailey, M., Bellomo, R., Eastwood, G. M., Nichol, A., Pilcher, D. V., Yunos, N. M., Egi, M., Hart, G. K., Reade, M. C., Cooper, D. J., & Study of Oxygen in Critical Care (SOCC) Group. The association between early arterial oxygenation and mortality in ventilated patients with acute ischaemic stroke. Critical care and resuscitation : journal of the Australas. Acad. Crit. Care Med. 2012, 14, 14–9. [Google Scholar]
- Popat, C.; Ruthirago, D.; Shehabeldin, M.; Yang, S.; Nugent, K. Outcomes in Patients With Acute Stroke Requiring Mechanical Ventilation: Predictors of Mortality and Successful Extubation. The American journal of the medical sciences 2018, 356, 3–9. [Google Scholar] [CrossRef] [PubMed]
- Schielke, E.; Busch, M.A.; Hildenhagen, T.; Holtkamp, M.; Küchler, I.; Harms, L.; Masuhr, F. Functional, cognitive and emotional long-term outcome of patients with ischemic stroke requiring mechanical ventilation. J. Neurol. 2005, 252, 648–54. [Google Scholar] [CrossRef] [PubMed]
- Steiner, T.; Mendoza, G.; De Georgia, M.; Schellinger, P.; Holle, R.; Hacke, W. Prognosis of stroke patients requiring mechanical ventilation in a neurological critical care unit. Stroke. 1997, 28, 711–5. [Google Scholar] [CrossRef] [PubMed]
- Santoli, F.; De Jonghe, B.; Hayon, J.; Tran, B.; Piperaud, M.; Merrer, J.; Outin, H. Mechanical ventilation in patients with acute ischemic stroke: survival and outcome at one year. Intensive Care Med. 2001, 27, 1141–6. [Google Scholar] [CrossRef] [PubMed]
- Milhaud, D. , Popp, J. , Thouvenot, E., Heroum, C., & Bonafé, A. Mechanical ventilation in ischemic stroke. Journal of stroke and cerebrovascular diseases: the official journal of Natl. Stroke Assoc. 2004, 13, 183–8. [Google Scholar]
- Burtin, P.; Bollaert, P.E.; Feldmann, L.; Nace, L.; Lelarge, P.; Bauer, P.; Larcan, A. Prognosis of stroke patients undergoing mechanical ventilation. Intensive Care Med. 1994, 20, 32–6. [Google Scholar] [CrossRef] [PubMed]
- Saposnik, G. , Barinagarrementeria, F., Brown, R. D., Jr, Bushnell, C. D., Cucchiara, B., Cushman, M., deVeber, G., Ferro, J. M., Tsai, F. Y., & American Heart Association Stroke Council and the Council on Epidemiology and Prevention Diagnosis and management of cerebral venous thrombosis: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 2011, 42, 1158–92. [Google Scholar] [PubMed]
- Qureshi, A.I. A Classification Scheme for Assessing Recanalization and Collateral Formation following Cerebral Venous Thrombosis. J. Vasc. Interv. Neurol. 2010, 3, 1. [Google Scholar] [PubMed]
- Ferro, J. M.; Canhão, P.; Stam, J.; Bousser, M.G.; Barinagarrementeria, F. ISCVT Investigators Prognosis of cerebral vein and dural sinus thrombosis: results of the International Study on Cerebral Vein and Dural Sinus Thrombosis (ISCVT). Stroke 2004, 35, 664–70. [Google Scholar] [CrossRef]
- Kalita, J.; Misra, U.K.; Singh, R.K. Do the Risk Factors Determine the Severity and Outcome of Cerebral Venous Sinus Thrombosis? Transl. Stroke Res. 2018, 9, 575–581. [Google Scholar] [CrossRef] [PubMed]
- Triquenot Bagan, A.; Crassard, I.; Drouet, L.; Barbieux-Guillot, M.; Marlu, R.; Robinet-Borgomino, E.; Morange, P.E.; Wolff, V.; Grunebaum, L.; Klapczynski, F.; André-Kerneis, E.; Pico, F.; Martin-Bastenaire, B.; Ellie, E.; Menard, F.; Rouanet, F.; Freyburger, G.; Godenèche, G.; Allano, H.A.; Moulin, T.; … Le Cam Duchez, V. Cerebral Venous Thrombosis: Clinical, Radiological, Biological, and Etiological Characteristics of a French Prospective Cohort (FPCCVT)-Comparison With ISCVT Cohort. Front. Neurol. 2021, 12, 753110. [Google Scholar] [CrossRef] [PubMed]
- Soyer, B.; Rusca, M.; Lukaszewicz, A.C.; Crassard, I.; Guichard, J.P.; Bresson, D.; Mateo, J.; Payen, D. Outcome of a cohort of severe cerebral venous thrombosis in intensive care. Ann. Intensive Care 2016, 6, 29. [Google Scholar] [CrossRef] [PubMed]
- Wall, J.; Enblad, P. Neurointensive care of patients with cerebral venous sinus thrombosis and intracerebral haemorrhage. Journal of clinical neuroscience : official journal of the Neurosurg. Soc. Australas. 2018, 58, 83–88. [Google Scholar] [CrossRef]
- Kalita, J.; Singh, V.K.; Jain, N.; Misra, U.K.; Kumar, S. Cerebral Venous Sinus Thrombosis Score and its Correlation with Clinical and MRI Findings. Journal of stroke and cerebrovascular diseases. Off. J. Natl. Stroke Natl. Stroke Assoc. 2019, 28, 104324. [Google Scholar] [CrossRef] [PubMed]
- Kalita, J.; Misra, U.K.; Singh, V.K.; Dubey, D. Predictors and outcome of status epilepticus in cerebral venous thrombosis. J. Neurol. 2019, 266, 417–425. [Google Scholar] [CrossRef] [PubMed]
- Kalita, J.; Ranjan, A.; Misra, U.K. Outcome of Guillain-Barre syndrome patients with respiratory paralysis. QJM: monthly journal of the Association of Physicians, 2016, 109, 319–323. [Google Scholar] [CrossRef] [PubMed]
- \Ruiz-Sandoval, J. L. , Chiquete, E. , Bañuelos-Becerra, L. J., Torres-Anguiano, C., González-Padilla, C., Arauz, A., León-Jiménez, C., Murillo-Bonilla, L. M., Villarreal-Careaga, J., Barinagarrementería, F., Cantú-Brito, C., & RENAMEVASC investigators Cerebral venous thrombosis in a Mexican multicenter registry of acute cerebrovascular disease: the RENAMEVASC study. Journal of stroke and cerebrovascular diseases. Off. J. Natl. Stroke Assoc. 2012, 21, 395–400. [Google Scholar]
- Kalita, J.; Singh, V.K.; Misra, U.K. A study of hyperhomocysteinemia in cerebral venous sinus thrombosis. Indian J. Med. Res. 2020, 152, 584–594. [Google Scholar] [CrossRef] [PubMed]
- Abdo, R.; Abboud, H.; Salameh, P.; El Hajj, T.; Hosseini, H. Mortality and Predictors of Death Poststroke: Data from a Multicenter Prospective Cohort of Lebanese Stroke Patients. Journal of stroke and cerebrovascular diseases. Off. J. Natl. Stroke Assoc. 2019, 28, 859–868. [Google Scholar] [CrossRef]
- Hénon, H.; Godefroy, O.; Leys, D.; Mounier-Vehier, F.; Lucas, C.; Rondepierre, P.; Duhamel, A.; Pruvo, J.P. Early predictors of death and disability after acute cerebral ischemic event. Stroke. 1995, 26, 392–8. [Google Scholar] [CrossRef]
- Stolz, E.; Trittmacher, S.; Rahimi, A.; Gerriets, T.; Röttger, C.; Siekmann, R.; Kaps, M. Influence of recanalization on outcome in dural sinus thrombosis: a prospective study. Stroke 2004, 35, 544–7. [Google Scholar] [CrossRef]
- Baumgartner, R.W.; Studer, A.; Arnold, M.; Georgiadis, D. Recanalisation of cerebral venous thrombosis. J. Neurol. Neurosurg. Psychiatry 2003, 74, 459–61. [Google Scholar] [CrossRef]
- Golestanian, E.; Liou, J.I.; Smith, M.A. Long-term survival in older critically ill patients with acute ischemic stroke. Crit. Care Med. 2009, 37, 3107–13. [Google Scholar] [CrossRef] [PubMed]
- Meyfroidt, G.; Bollaert, P.E.; Marik, P.E. Acute ischemic stroke in the ICU: to admit or not to admit? Intensive Care Med. 2014, 40, 749–51. [Google Scholar] [CrossRef] [PubMed]
- Aguiar de Sousa, D.; Lucas Neto, L.; Canhão, P.; Ferro, J.M. Recanalization in Cereb. Venous Thrombosis. Stroke 2018, 49, 1828–1835. [Google Scholar]
- Singh, V.K.; Jain, N.; Kalita, J.; Misra, U.K.; Kumar, S. Significance of recanalization of sinuses and resolution of parenchymal lesion in cerebral venous sinus thrombosis. Journal of clinical neuroscience: official journal of the Neurosurg. Soc. Australas. 2020, 77, 175–180. [Google Scholar] [CrossRef]
|
Total (n=45) |
MV (n=18) |
Non-MV (n=27) |
P | |
| Age (yrs) | 34.07±12.56 | 29.44±11.91 | 36.67±13.31 | 0.07 |
| Females | 22 | 6(33.3%) | 16(59.2%) | 0.13 |
| Duration of illness (Days) | 11.47±13.08 | 12.66±15.02 | 10.67±11.87 | 0.62 |
|
Onset Acute (≤ 2 days) Sub-acute (3-30 days) Chronic >30 days |
7 35 3 |
4(22.2%) 12(65.7%) 2(11.1%) |
3(11.1%) 23(85.2%) 1(3.7%) |
0.33 |
| Seizures | 40 | 16(88.9%) | 24(88.9%) | 1.00 |
| Status epilepticus | 16 | 8(44.4%) | 8(29.6%) | 0.54 |
| Focal deficit | 33 | 14(77.8%) | 19(70.4%) | 0.73 |
| GCS score | 8.08±3.02 | 8.39±3.22 | 9.11±2.91 | 0.44 |
| Risk factor Hereditary prothrombotic states |
||||
| MTHFR CC CT TT |
16 14 1 |
3(75%) 1(25%) 0(0%) |
13(76.5%) 3(17.6%) 1(5.9%) |
0.32 |
| Antithrombin III Normal Deficient |
20 2 |
9(81.8%) 2(18.2%) |
11(100% 0(0%) |
0.48 |
| Protein S Normal Deficient |
21 11 |
10(71.4%) 4(28.6%) |
11(61.1%) 7(38.9%) |
0.71 |
| Protein C Normal Deficient |
24 8 |
7(58.8%) 6(41.2%) |
17(89.5%) 2(10.5%) |
0.04 |
| Acquired prothrombotic state Homocysteine µmol/l <15 ≥15 |
17 11 |
4(66.7%) 2(33.3%) |
13(59.1%) 9(40.9%) |
0.10 |
| APLA syndrome Yes No |
8 23 |
3(33.3%) 6(66.4%) |
5((22.7%) 17(77.3%) |
0.66 |
| Vitamin B12 pg/ml <200 200-500 >500 |
11 6 17 |
3(25%) 1(8.3%) 8(66.7%) |
8(36.4%) 5(22.7%) 9(40.9%) |
0.79 |
| Folic acid ng/ml <3.5 >3.5 |
8 23 |
3(33.3%) 6(66.7%) |
5(22.7%) 17(77.3%) |
0.66 |
| Female Specific risk Puerperium Yes No |
7 15 |
2(33.3%) 4(66.4%) |
5(31.2%) 11(68.8%) |
1.00 |
| Oral contraceptives pill Yes No |
2 20 |
1(16.7%) 5(83.3%) |
1(6.2%) 15(93.8%) |
0.48 |
| Number of risk factor | 1.67±0.83 | 1.25±0.5 | 1.67±6.76 | 0.06 |
| No risk factor | 5 | 1(20%) | 4(80%) | 0.63 |
| Parameter |
All n=45 |
MV n=18 |
Non-MV n=27 |
P |
| Parenchymal lesion on MRI Infarct Hemorrhagic |
39 7 32 |
16(88.9%) 1(5.5%) 15(83.3%) |
23(85.2%) 6((22.2%) 17(63.0%) |
1.00 0.21 |
| Thrombosis on MRV Superficial system Deep system Both |
37 2 6 |
15(83.3%) 1(5.5%) 2(11.0%) |
22(81.5%) 1(3.7%) 4(14.8%) |
0.91 |
| Superior saggital sinus | 31 | 13(72.2%) | 18(66.7%) | 0.75 |
| Inferior saggital sinus | 2 | 0(0%) | 2(7.4%) | 0.51 |
| Transverse sinus | 29 | 13(72.2%) | 16((59.2%) | 0.53 |
| Sigmoid sinus | 19 | 9(50%) | 10(3.7.0%) | 0.54 |
| Number of sinus involved | 1.29±0.46 | 1.33±0.48 | 1.26±0.45` | 0.60 |
|
Death N=9 |
Survived N=36 |
P | |
| Age (yrs) |
29.67±12.93 | 35.17±12.41 | 0.24 |
| Gender (Male/Female) | 6(66.7%)/3(33.3%) | 17(47.2%)/19(52.8%) | 0.46 |
| Duration (days) Acute/ Sub/chronic |
6.44±5.43 3(33.3%)/6(66.7%)/0(0%) |
12.72±14.15 4(11.1%)/29(80.5%)/3(8.3%) |
0.04 0.20 |
| Status epilepticus |
3(33.3%) | 1438.9%) | 1.00 |
| Motor deficit | 8(88.9%) | 25(97.2%) | 0.41 |
| Number of risk factor | 5.67±4.47 | 8.91±7.27 | |
| MRI parenchymal lesion | 9(100%) | 30(83.3%) | 0.32 |
| MRV Deep/Superficial/Both |
7((77.8%)/0(0%)/2(22.2%) |
30(83.3%)/2(5.5%)/4(11.1%) |
0.55 |
| GCS score | 6.89±2.62 | 9.31±2.95 | 0.03 |
| Mechanical ventilation | 5(55.5%) | 13(36.1%) | 0.45 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




