Submitted:
04 February 2025
Posted:
05 February 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Intervention and Data Collection
2.3. Blood-Based Biomarker Analysis
2.4. Outcome Measures
2.5. Statistical Analysis
3. Results
3.1. Clinical parameters
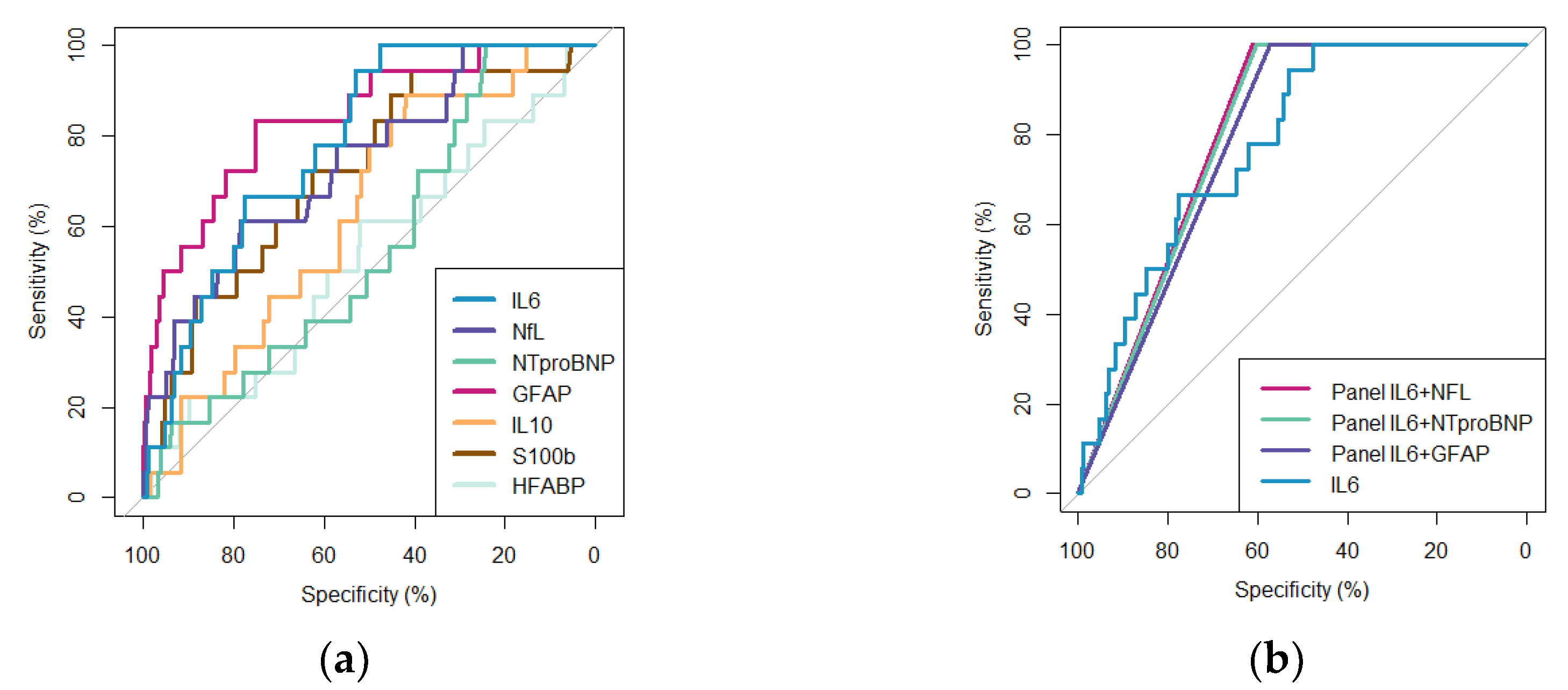
3.2. Individuals’ Biomarkers Performances
3.3. Combinations of Biomarkers Performances
3.4. Age-Correlation in the Healthy Population
4. Discussion
Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AUC | Area Under the Curve |
| BBB | Blood-Brain Barrier |
| CT | Computed Tomography |
| CV | Coefficient of Variation |
| ECI | ExtraCranial Injuries |
| ELISA | Enzyme-Linked Immunoassay |
| GCS | Glasgow Coma Scale |
| GFAP | Glial Fibrillary Acidic Protein |
| HFABP | Heart Fatty-Acid-Binding Protein |
| HFR | Fribourg Hospital |
| HUG | Hopitaux Universitaires de Genève |
| IC | Confidence Interval |
| ICI | Intracranial injury |
| IL10 | Interleukin 10 |
| IL8 | Interleukin 8 |
| IL6 | Interleukin 6 |
| IQR | Inter Quartile Range |
| LLD | Lower Limit of Detection |
| LLOQ | Lower Limit of Quantification |
| LOC | Loss of Consciousness |
| Max | Maximum |
| Min | Minimum |
| mTBI | mild Traumatic Brain Injury |
| NfL | Neurofilament Light chain |
| NPV | Negative Predictive Value |
| NTproBNP | N-terminal prohormone of brain natriuretic peptide |
| PECARN | Pediatric Emergency Care Applied Research Network |
| PED | Pediatric Emergency Department |
| PTA | Post Traumatic Amnesia |
| RHNE | Neuchâtel Hospital |
| ROC | Receiver Operating Characteristic |
| S100b | S100 calcium-binding protein B |
| SE | Sensitivity |
| SD | Standard Deviation |
| SP | Specificity |
| TBI | Traumatic Brain Injury |
| UCHL-1 | Ubiquitin Carboxy-terminal Hydrolase L1 |
References
- Lumba-Brown A, Yeates KO, Sarmiento K, et al. Centers for Disease Control and Prevention Guideline on the Diagnosis and Management of Mild Traumatic Brain Injury Among Children. JAMA Pediatr. 2018, 172, e182853. [Google Scholar] [CrossRef] [PubMed]
- Dewan MC, Mummareddy N, Wellons JC, 3rd, Bonfield CM. Epidemiology of Global Pediatric Traumatic Brain Injury: Qualitative Review. World Neurosurg. 2016, 91, 497–509 e1. [Google Scholar] [CrossRef] [PubMed]
- Kuppermann N, Holmes JF, Dayan PS, et al. Identification of children at very low risk of clinically-important brain injuries after head trauma: a prospective cohort study. Lancet. 2009, 374, 1160–70. [Google Scholar] [CrossRef] [PubMed]
- Babl FE, Borland ML, Phillips N, et al. Accuracy of PECARN, CATCH, and CHALICE head injury decision rules in children: a prospective cohort study. Lancet 2017, 389, 2393–2402. [Google Scholar] [CrossRef]
- Borg J, Holm L, Cassidy JD, et al. Diagnostic procedures in mild traumatic brain injury: results of the WHO Collaborating Centre Task Force on Mild Traumatic Brain Injury. J Rehabil Med 2004, (Suppl. 43), 61–75. [Google Scholar] [CrossRef]
- Haydel MJ, Preston CA, Mills TJ, Luber S, Blaudeau E, DeBlieux PM. Indications for computed tomography in patients with minor head injury. N Engl J Med. 2000, 343, 100–5. [Google Scholar] [CrossRef]
- Brenner DJ, Hall EJ. Computed tomography--an increasing source of radiation exposure. N Engl J Med. 2007, 357, 2277–84. [Google Scholar] [CrossRef]
- Carroll LJ, Cassidy JD, Holm L, Kraus J, Coronado VG, Injury WHOCCTFoMTB. Methodological issues and research recommendations for mild traumatic brain injury: the WHO Collaborating Centre Task Force on Mild Traumatic Brain Injury. J Rehabil Med 2004, (43 Suppl), 113–25. [CrossRef]
- Levin HS, Diaz-Arrastia RR. Diagnosis, prognosis, and clinical management of mild traumatic brain injury. Lancet Neurol. 2015, 14, 506–17. [Google Scholar] [CrossRef]
- Jarrahi A, Braun M, Ahluwalia M, et al. Revisiting Traumatic Brain Injury: From Molecular Mechanisms to Therapeutic Interventions. Biomedicines 2020, 8. [CrossRef]
- Zetterberg H, Smith DH, Blennow K. Biomarkers of mild traumatic brain injury in cerebrospinal fluid and blood. Nature Reviews Neurology. 2013, 9, 201–210. [Google Scholar] [CrossRef] [PubMed]
- Sapin V, Gaulmin R, Aubin R, Walrand S, Coste A, Abbot M. Blood biomarkers of mild traumatic brain injury: State of art. Neurochirurgie. 2021, 67, 249–254. [Google Scholar] [CrossRef] [PubMed]
- Bouvier D, Oris C, Brailova M, Durif J, Sapin V. Interest of blood biomarkers to predict lesions in medical imaging in the context of mild traumatic brain injury. Clinical Biochemistry. 2020, 85, 5–11. [Google Scholar] [CrossRef]
- Siman R, Toraskar N, Dang A, et al. A Panel of Neuron-Enriched Proteins as Markers for Traumatic Brain Injury in Humans. Journal of Neurotrauma. 2009, 26, 1867–1877. [Google Scholar] [CrossRef] [PubMed]
- Lagerstedt L, Egea-Guerrero JJ, Bustamante A, et al. Combining H-FABP and GFAP increases the capacity to differentiate between CT-positive and CT-negative patients with mild traumatic brain injury. PLoS One. 2018, 13, e0200394. [Google Scholar] [CrossRef]
- Bazarian JJ, Welch RD, Caudle K, et al. Accuracy of a rapid glial fibrillary acidic protein/ubiquitin carboxyl-terminal hydrolase L1 test for the prediction of intracranial injuries on head computed tomography after mild traumatic brain injury. Acad Emerg Med. 2021, 28, 1308–1317. [Google Scholar] [CrossRef]
- Bazarian JJ, Biberthaler P, Welch RD, et al. Serum GFAP and UCH-L1 for prediction of absence of intracranial injuries on head CT (ALERT-TBI): a multicentre observational study. Lancet Neurology. 2018, 17, 782–789. [Google Scholar] [CrossRef]
- Lagerstedt L, Egea-Guerrero JJ, Bustamante A, et al. H-FABP: A new biomarker to differentiate between CT-positive and CT-negative patients with mild traumatic brain injury. PLoS One. 2017, 12, e0175572. [Google Scholar] [CrossRef]
- Oris C, Kahouadji S, Durif J, Bouvier D, Sapin V. S100B, Actor and Biomarker of Mild Traumatic Brain Injury. Int J Mol Sci 2023, 24. [CrossRef]
- Oris C, Pereira B, Durif J, et al. The Biomarker S100B and Mild Traumatic Brain Injury: A Meta-analysis. Pediatrics 2018, 141. [CrossRef]
- Unden J, Ingebrigtsen T, Romner B, Scandinavian Neurotrauma C. Scandinavian guidelines for initial management of minimal, mild and moderate head injuries in adults: an evidence and consensus-based update. BMC Med. 2013, 11, 50. [Google Scholar] [CrossRef]
- Gil-Jardine C, Payen JF, Bernard R, et al. Management of patients suffering from mild traumatic brain injury 2023. Anaesth Crit Care Pain Med. 2023, 42, 101260. [Google Scholar] [CrossRef] [PubMed]
- Calcagnile O, Anell A, Undén J. The addition of S100B to guidelines for management of mild head injury is potentially cost saving. Bmc Neurol. 2016, 16, 200. [Google Scholar] [CrossRef]
- Unden L, Calcagnile O, Unden J, Reinstrup P, Bazarian J. Validation of the Scandinavian guidelines for initial management of minimal, mild and moderate traumatic brain injury in adults. BMC Med. 2015, 13, 292. [Google Scholar] [CrossRef]
- Manzano S, Holzinger IB, Kellenberger CJ, et al. Diagnostic performance of S100B protein serum measurement in detecting intracranial injury in children with mild head trauma. Emerg Med J. 2016, 33, 42–6. [Google Scholar] [CrossRef]
- Chiollaz AC, Pouillard V, Spigariol F, et al. Management of Pediatric Mild Traumatic Brain Injury Patients: S100b, Glial Fibrillary Acidic Protein, and Heart Fatty-Acid-Binding Protein Promising Biomarkers. Neurotrauma Rep. 2024, 5, 529–539. [Google Scholar] [CrossRef]
- Bouvier D, Castellani C, Fournier M, et al. Reference ranges for serum S100B protein during the first three years of life. Clin Biochem. 2011, 44, 927–9. [Google Scholar] [CrossRef]
- Reyes J, Spitz G, Major BP, et al. Utility of Acute and Subacute Blood Biomarkers to Assist Diagnosis in CT-Negative Isolated Mild Traumatic Brain Injury. Neurology. 2023, 101, E1992–E2004. [Google Scholar] [CrossRef]
- Posti JP, Takala RSK, Lagerstedt L, et al. Correlation of Blood Biomarkers and Biomarker Panels with Traumatic Findings on Computed Tomography after Traumatic Brain Injury. Journal of Neurotrauma. 2019, 36, 2178–2189. [Google Scholar] [CrossRef]
- Hossain I, Marklund N, Czeiter E, Hutchinson P, Buki A. Blood biomarkers for traumatic brain injury: A narrative review of current evidence. Brain Spine 2024, 4.
- Ryan E, Kelly L, Stacey C, et al. Mild-to-severe traumatic brain injury in children: altered cytokines reflect severity. J Neuroinflamm 2022, 19.
- Harris PA, Taylor R, Minor BL, et al. The REDCap consortium: Building an international community of software platform partners. J Biomed Inform. 2019, 95, 103208. [Google Scholar] [CrossRef]
- Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG. Research electronic data capture (REDCap)--a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009, 42, 377–81. [Google Scholar] [CrossRef] [PubMed]
- Chiollaz AC, Pouillard V, Habre C, et al. Diagnostic potential of IL6 and other blood-based inflammatory biomarkers in mild traumatic brain injury among children. Front Neurol. 2024, 15, 1432217. [Google Scholar] [CrossRef]
- Chiollaz AC, Pouillard V, Habre C, et al. Evaluating NfL and NTproBNP as predictive biomarkers of intracranial injuries after mild traumatic brain injury in children presenting to emergency departments. Front Neurol. 2025, 16. [Google Scholar] [CrossRef]
- Robin, X. PanelomiX for the Combination of Biomarkers. Methods Mol Biol. 2019, 1959, 261–273. [Google Scholar] [CrossRef]
- Robin X, Turck N, Hainard A, et al. PanelomiX: A threshold-based algorithm to create panels of biomarkers. Translational Proteomics. 2013, 1, 57–64. [Google Scholar] [CrossRef]
- Crowe L, Babl F, Anderson V, Catroppa C. The epidemiology of paediatric head injuries: Data from a referral centre in Victoria, Australia. J Paediatr Child H. 2009, 45, 346–350. [Google Scholar] [CrossRef]
- Sönnerqvist C, Brus O, Olivecrona M. Validation of the scandinavian guidelines for initial management of minor and moderate head trauma in children. Eur J Trauma Emerg S. 2021, 47, 1163–1173. [Google Scholar] [CrossRef]
- Bressan S, Eapen N, Phillips N, et al. PECARN algorithms for minor head trauma: Risk stratification estimates from a prospective PREDICT cohort study. Academic Emergency Medicine. 2021, 28, 1124–1133. [Google Scholar] [CrossRef]
- Nigrovic LE, Kuppermann N. Children With Minor Blunt Head Trauma Presenting to the Emergency Department. Pediatrics. 2019, 144. [Google Scholar] [CrossRef]
- Unden J, Dalziel SR, Borland ML, et al. External validation of the Scandinavian guidelines for management of minimal, mild and moderate head injuries in children. BMC Med. 2018, 16, 176. [Google Scholar] [CrossRef]
- Giza CC, Gioia G, Cook LJ, et al. CARE4Kids Study: Endophenotypes of Persistent Post-Concussive Symptoms in Adolescents: Study Rationale and Protocol. J Neurotrauma. 2024, 41, 171–185. [Google Scholar] [CrossRef] [PubMed]
- Haber M, Amyot F, Kenney K, et al. Vascular Abnormalities within Normal Appearing Tissue in Chronic Traumatic Brain Injury. Journal of Neurotrauma. 2018, 35, 2250–2258. [Google Scholar] [CrossRef]
| N=419 mTBI |
CT- (N=79) or Obs. (N=322) (N=401) 96% of total cohort |
CT+ (N=18) 19% of CT-scanned 4% of total cohort |
P-value |
| INCLUSION CRITERIA: | |||
| Severity of injury, n (%) | |||
| GCS14 | 54 (13.5%) | 6 (33.3%) | 0.044 |
| GCS15* | 347 (86.5%) | 12 (66.7%) | |
| Sign of basilar skull fracture, n (%) | 10 (2.5%) | 6 (33.3%) | <0.001 |
| Severe mechanism of injury◊, n (%) | 175 (43.6%) | 14 (77.8%) | 0.009 |
| *Symptoms at admission (within GCS 15), n (%) | |||
| Loss of consciousness | 85 (21.2%) | 2 (11.1%) | 0.772 |
| Post-traumatic amnesia | 116 (28.9%) | 1 (5.6%) | 0.127 |
| Persistent headaches | 105 (26.2%) | 6 (33.3%) | 0.268 |
| More than three episodes of vomiting | 64 (16.0%) | 4 (22.2%) | 0.367 |
| Vertigo | 37 (9.2%) | 0 (0%) | 0.471 |
| Confusion | 46 (11.5%) | 1 (5.6%) | 0.936 |
| Convulsion | 8 (2.0%) | 0 (0%) | 1 |
| OTHER CLINICAL VARIABLES: | |||
| Age (yo) | |||
| Mean (SD) | 8.8 (4.40) | 7.8 (4.27) | 0.338 |
| Median [Min, Max] | 9.1 [0.1, 16.0] | 7.1 [0.9, 15.0] | |
| Sex, n (%) | |||
| Boys | 234 (58.4%) | 12 (66.7%) | 0.669 |
| Girls | 167 (41.6%) | 6 (33.3%) | |
| Extracranial injuries (ECI), n (%) | |||
| mTBI + either body/face fractures | 13 CT- (16.5%); 13 Obs. (4%) |
4 (22.2%) | 0.031 |
| Skull fracture (on CT), n (%) | |||
| Simple skull fracture (not PECARN criterion) | 14 CT- (17.7%) | 15 (83.3%) | <0.001 |
| N=419 mTBI |
CT- & Obs. (N=401) |
CT+ (N=18) |
P-value (Mann–Whitney U test) |
| TimelapsTBI-blood (hours) | |||
| Mean (SD) | 6.43 (4.98) | 8.44 (7.11) | 0.298 |
| Median [Min, Max] | 5.00 [0, 24.0] | 6.50 [2.00, 24.0] | |
| IL6 (pg/ml) | |||
| Mean (SD) | 2.45 (7.66) | 5.55 (8.20) | <0.001 |
| Median [Min, Max] | 1.05 [0.0385, 99.4] | 2.64 [0.932, 34.2] | |
| NfL (pg/ml) | |||
| Mean (SD) | 23.2 (19.2) | 49.8 (41.6) | <0.001 |
| Median [Min, Max] | 17.7 [0.119, 127] | 31.3 [13.5, 141] | |
| NTproBNP (pg/ml) | |||
| Mean (SD) | 98.5 (90.6) | 112 (96.0) | 0.433 |
| Median [Min, Max] | 69.9 [0.471, 709] | 67.8 [36.0, 337] | |
| GFAP (pg/ml) | |||
| Mean (SD) | 559 (910) | 3140 (3450) | <0.001 |
| Median [Min, Max] | 208 [0.746, 8770] | 2080 [75.7, 11200] | |
| IL10 (pg/ml) | |||
| Mean (SD) | 1.21 (5.16) | 1.34 (2.09) | 0.061 |
| Median [Min, Max] | 0.423 [0.0634, 94.9] | 0.587 [0.211, 9.27] | |
| S100b (pg/ml) | |||
| Mean (SD) | 56.7 (66.5) | 125 (137) | 0.002 |
| Median [Min, Max] | 41.5 [0.108, 672] | 74.6 [2.05, 582] | |
| HFABP (pg/ml) | |||
| Mean (SD) | 3390 (3250) | 3810 (3210) | 0.629 |
| Median [Min, Max] | 2480 [20.2, 32200] | 2730 [1220, 13200] |
| (a) | ||||
| Individuals |
Sensibility (%) (95%CI) |
Specificity (%) (95%CI) |
AUC (%) (95%CI) |
Threshold(pg/ml) |
| IL6 |
100 (100 - 100) |
47.6 (42.9 – 52.4) |
78.1 (69.6 – 86.6) |
> 0.93 |
| NfL |
100 (100 - 100) |
29.4 (25.1 – 33.8) |
73.9 (61.9 – 85.8) |
> 13.53 |
| NTproBNP |
100 (100 - 100) |
24.4 (20.3 – 28.6) |
55.5 (43.2 – 67.7) |
> 35.97 |
| GFAP |
100 (100 - 100) |
25.7 (21.5 – 29.9) |
83.9 (74.0 – 93.8) |
> 75.36 |
| (b) | ||||
| Combinations (duplex) |
Sensibility (%) (95%CI) |
Specificity (%) (95%CI) |
AUC (%) (95%CI) |
Threshold(pg/ml) |
| IL6 + NfL |
100 (100 - 100) |
61,1 (56,4 – 65,8) |
80.55 (78.2 – 83.0) |
> 0.93 > 13.52 |
| IL6 + NTproBNP |
100 (100 - 100) |
60,1 (55,4 – 64,8) |
80.05 (77.7 – 82.5) |
> 0.93 > 35.07 |
| IL6 + GFAP |
100 (100 - 100) |
57,4 (52,6 – 62,1) |
78.68 (76.3 – 81.1) |
> 0.93 > 75.36 |
| (c) | ||||
| Confusion matrix | CT− & Obs. | CT+ | Total | |
|
Predicted CT− & Obs. |
245 (33 CT− and 212 Obs.) True Negative : 61% |
0 | 245 | |
|
Predicted CT+ |
156 (46 CT− and 110 Obs.) |
18 True Positive : 100% |
174 | |
| Total | 401 | 18 | 419 | |
| Biomarkers | Spearman coefficient (r) | p-value |
|---|---|---|
| IL6 | 0.17 | 0.09 |
| GFAP | -0.73 | <0.001 |
| NTproBNP | 0.00 | 0.52 |
| NfL | -0.22 | 0.028 |
| HFABP | -0.22 | 0.029 |
| S100b | -0.44 | <0.001 |
| IL10 | -0.55 | <0.001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




