Submitted:
27 January 2025
Posted:
28 January 2025
You are already at the latest version
Abstract
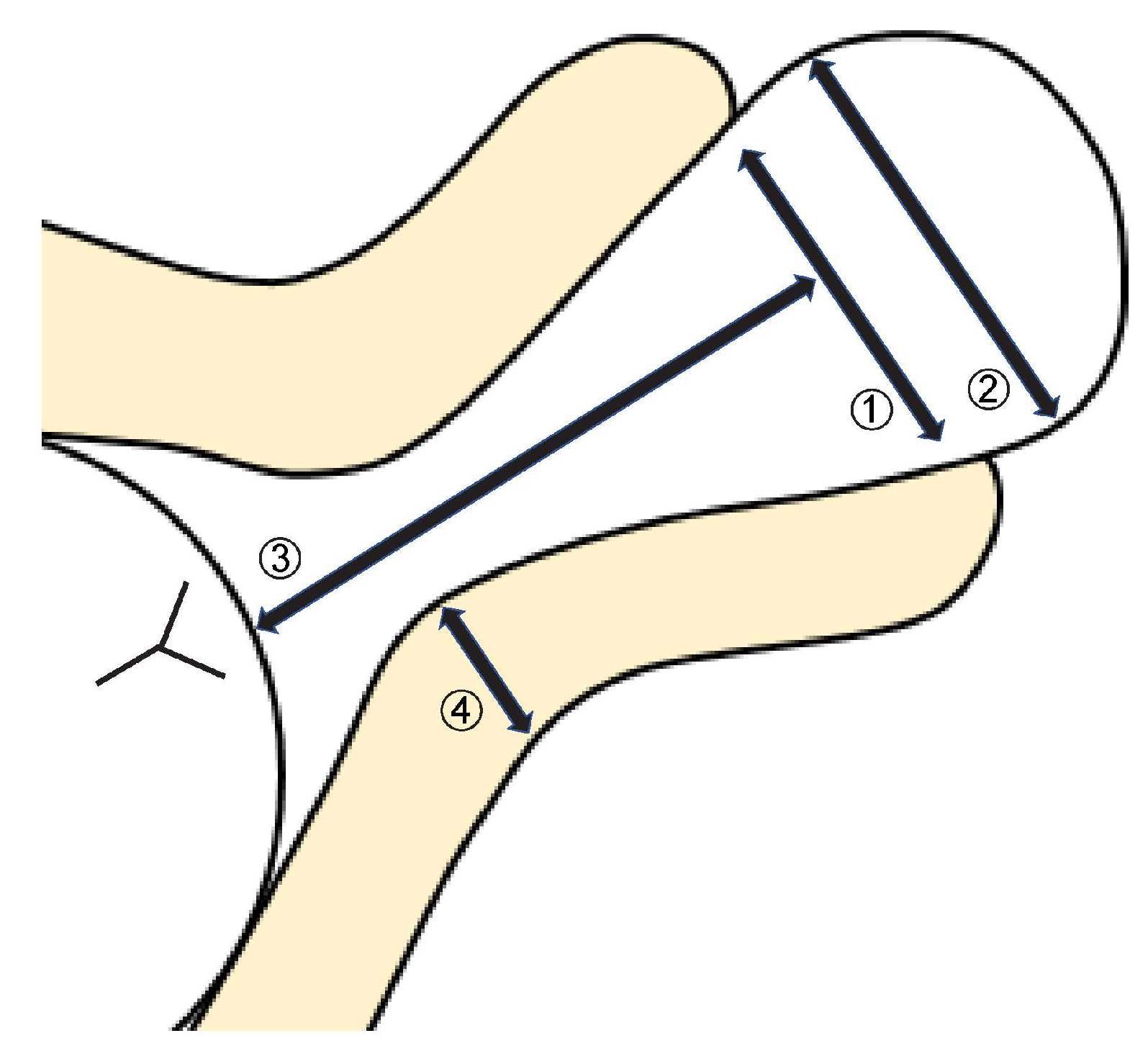
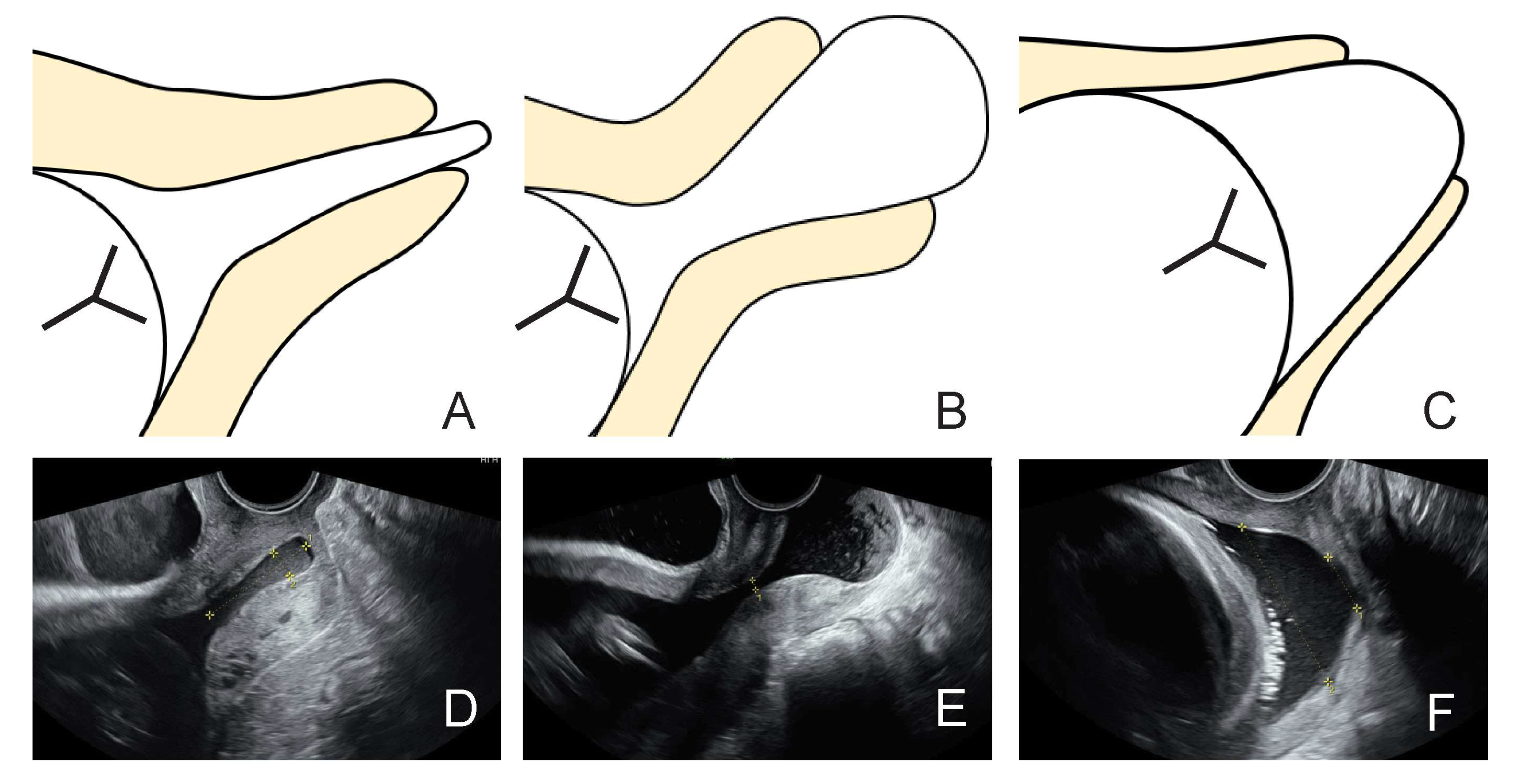
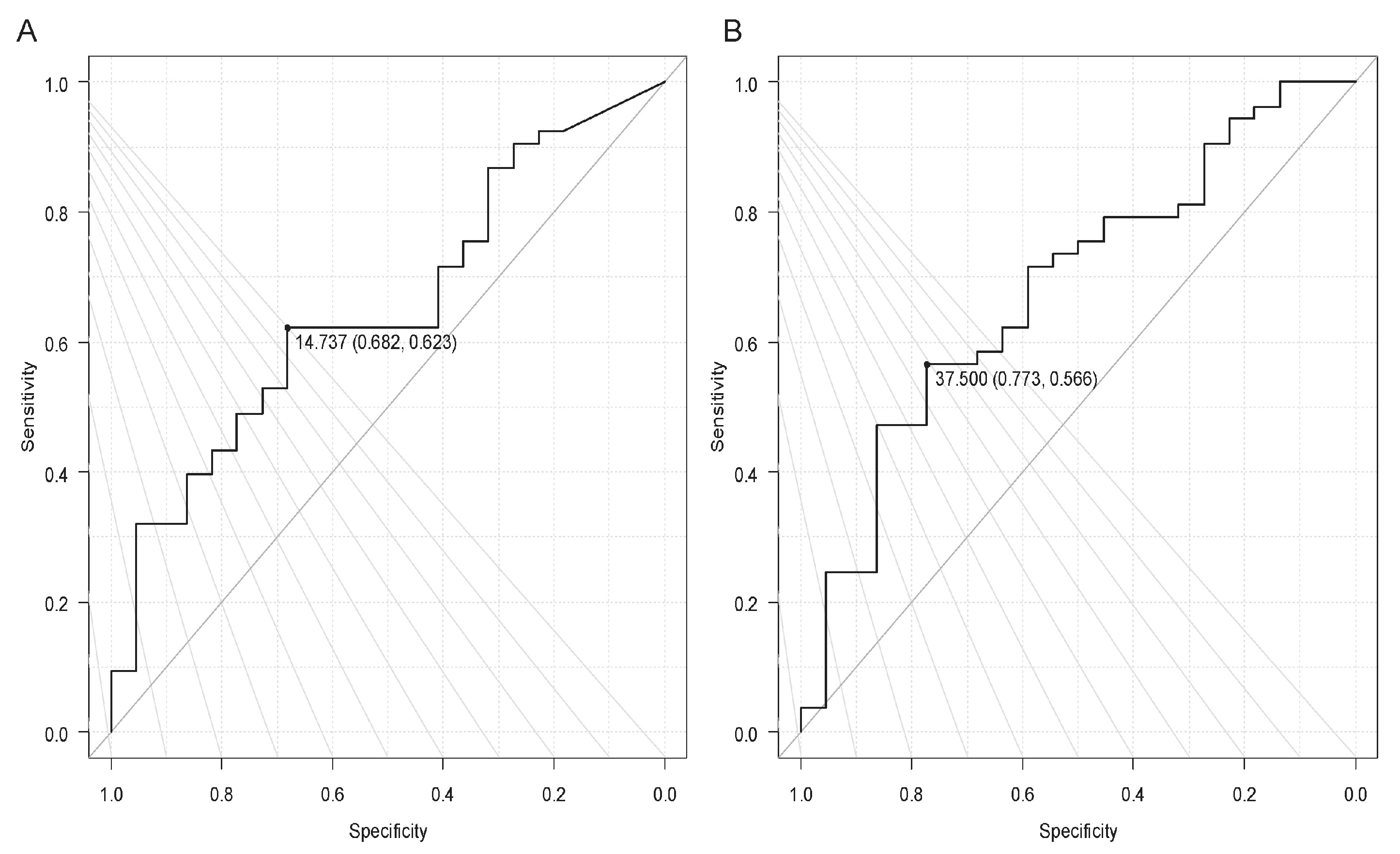
Background/Objectives: Fetal membrane prolapse can occur due to advanced cervical insufficiency. We investigated the yet unclear predictors of prolonged pregnancy in women with prolapsed fetal membranes. Methods: This retrospective observational study included 100 pregnant women with prolapsed fetal membranes between November 2017 and March 2023. We examined the correlation between transvaginal ultrasound findings at the time of admission and the duration of prolonged pregnancy, which was defined as the period from admission to delivery. We defined five trans-vaginal ultrasound indices: 1) width of the external os, 2) maximum width of the pro-lapsed fetal membrane, 3) distance from the external os to the presenting part of the fetus, 4) thickness of the posterior uterine lip, and 5) morphology of the prolapsed fetal membrane. Results: Women who underwent cervical cerclage comprised the cerclage group (n=17), while those who underwent conservative management comprised the non-cerclage group (n=83). The pregnancy period was significantly longer in the cerclage group than in the non-cerclage group (81.4 days vs. 9.1 days, P<0.001). Multiple regression analysis revealed that type A morphology was a significant factor for prolonged pregnancy in the non-cerclage group (P<0.05), which was significantly associated with a prolonged pregnancy period of over 7 days (P=0.037). Conclusions: In cases of prolapsed fetal membranes, cerclage is challenging because of the high risk of iatrogenic preterm rupture of the membrane; however, if successful, the pregnancy outcome is significantly improved. Morphological evaluation using ultrasonography is simple and easy to understand and correlates well with pregnancy outcomes, making it very useful.
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Participants
2.2. Ultrasound Findings
2.3. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| PROM | Preterm rupture of membrane |
| CI | Confidence interval |
References
- Ocal, A.; Demirci, O.; Ozgokce, C.; Kahramanoglu, O.; Dizdarogullari, G.E.; Eyisoy, O.G.; Yarsilikal Guleroglu, F. Protruding vs. visible prolapsed fetal membranes adversely affects the outcome of cervical insufficiency. Eur Rev Med Pharmacol Sci 2023, 27, 9937–9946. [Google Scholar] [CrossRef]
- ACOG Practice Bulletin, No. 142: Cerclage for the management of cervical insufficiency. Obstet Gynecol 2014, 123, 372–379. [Google Scholar] [CrossRef]
- Granese, R.; Mantegna, S.; Mondello, S.; Amadore, D.; Imbesi, G.; Calagna, G.; Marci, R.; Magro Malosso, E.R.; Triolo, O. Preterm birth: incidence, risk factors and second trimester cervical length in a single center population. A two-year retrospective study. Eur Rev Med Pharmacol Sci 2017, 21, 4270–4277. [Google Scholar] [PubMed]
- Robertson, J.E.; Lisonkova, S.; Lee, T.; De Silva, D.A.; von Dadelszen, P.; Synnes, A.R.; Joseph, K.S.; Liston, R.M.; Magee, L.A.; Canadian Perinatal Network and Canadian Neonatal Network Collaborative Groups. Fetal, infant and maternal outcomes among women with prolapsed membranes admitted before 29 weeks gestation. PLOS One 2016, 11, e0168285. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.E.; Romero, R.; Park, C.W.; Jun, J.K.; Yoon, B.H. The frequency and significance of intraamniotic inflammation in patients with cervical insufficiency. Am J Obstet Gynecol 2008, 198, 633.e1–633.e8. [Google Scholar] [CrossRef]
- Bujold, E.; Morency, A.M.; Rallu, F.; Ferland, S.; Tétu, A.; Duperron, L.; Audibert, F.; Laferrière, C. Bacteriology of amniotic fluid in women with suspected cervical insufficiency. J Obstet Gynaecol Can 2008, 30, 882–887. [Google Scholar] [CrossRef] [PubMed]
- Stupin, J.H.; David, M.; Siedentopf, J.P.; Dudenhausen, J.W. Emergency cerclage versus bed rest for amniotic sac prolapse before 27 gestational weeks. A retrospective, comparative study of 161 women. Eur J Obstet Gynecol Reprod Biol 2008, 139, 32–37. [Google Scholar] [CrossRef]
- Debby, A.; Sadan, O.; Glezerman, M.; Golan, A. Favorable outcome following emergency second trimester cerclage. Int J Gynaecol Obstet 2007, 96, 16–19. [Google Scholar] [CrossRef] [PubMed]
- Aoki, S.; Ohnuma, E.; Kurasawa, K.; Okuda, M.; Takahashi, T.; Hirahara, F. Emergency cerclage versus expectant management for prolapsed fetal membranes: a retrospective, comparative study. J Obstet Gynaecol Res 2014, 40, 381–386. [Google Scholar] [CrossRef] [PubMed]
- Hulshoff, C.C.; Bosgraaf, R.P.; Spaanderman, M.E.A.; IntHout, J.; Scholten, R.R.; Van Drongelen, J. The efficacy of emergency cervical cerclage in singleton and twin pregnancies: a systematic review with meta-analysis. Am J Obstet Gynecol MFM 2023, 5, 100971. [Google Scholar] [CrossRef] [PubMed]
- Althuisius, S.M.; Dekker, G.A.; Hummel, P.; van Geijn, H.P.; Cervical incompetence prevention randomized cerclage trial. Cervical incompetence prevention randomized cerclage trial: emergency cerclage with bed rest versus bed rest alone. Am J Obstet Gynecol 2003, 189, 907–910. [Google Scholar] [CrossRef]
- Harger, J.H. Cerclage and cervical insufficiency: an evidence-based analysis. Obstet Gynecol 2002, 100, 1313–1327. [Google Scholar] [CrossRef]
- Simcox, R.; Shennan, A. Cervical cerclage in the prevention of preterm birth. Best Pract Res Clin Obstet Gynaecol 2007, 21, 831–842. [Google Scholar] [CrossRef] [PubMed]
- Bishop, E.H. Pelvic scoring for elective induction. Obstet Gynecol 1964, 24, 266–268. [Google Scholar]
- van Dijk, C.E.; Breuking, S.H.; Jansen, S.; Limpens, J.C.E.J.M.; Kazemier, B.M.; Pajkrt, E. Perioperative complications of a transvaginal cervical cerclage in singleton pregnancies: a systematic review and meta-analysis. Am J Obstet Gynecol 2023, 228, 521–534.e19. [Google Scholar] [CrossRef] [PubMed]
- Scheerer, L.J.; Lam, F.; Bartolucci, L.; Katz, M. A new technique for reduction of prolapsed fetal membranes for emergency cervical cerclage. Obstet Gynecol 1989, 74, 408–410. [Google Scholar] [PubMed]
- Kanai, M.; Ashida, T.; Ohira, S.; Osada, R.; Konishi, I. A new technique using a rubber balloon in emergency second trimester cerclage for fetal membrane prolapse. J Obstet Gynaecol Res 2008, 34, 935–940. [Google Scholar] [CrossRef]
- Locatelli, A.; Vergani, P.; Bellini, P.; Strobelt, N.; Arreghini, A.; Ghidini, A. Amnioreduction in emergency cerclage with prolapsed membranes: comparison of two methods for reducing the membranes. Am J Perinatol 1999, 16, 73–77. [Google Scholar] [CrossRef] [PubMed]
- Fuchs, F.; Bouyer, J.; Fernandez, H.; Gervaise, A.; Frydman, R.; Senat, M.V. Ultrasound cervical length measurement for prediction of delivery before 32 weeks in women with emergency cerclage for cervical insufficiency. Int J Gynaecol Obstet 2010, 110, 245–248. [Google Scholar] [CrossRef] [PubMed]
- Roman, A.; Gulersen, M.; Boelig, R.C.; Berghella, V. Proposed staging criteria for sonographic and physical exam for cervical changes at <24 weeks gestation to predict preterm birth. Am J Obstet Gynecol MFM 2023, 5, 100753. [Google Scholar] [CrossRef] [PubMed]
- Park, J.Y.; Oh, K.J.; Lee, S.; Kim, N.K.; Lee, Y.E.; Park, Y.H.; Hong, J.S. A new quantification system for assessing the degree of acute cervical insufficiency based on physical and sonographic examination. Eur J Obstet Gynecol Reprod Biol 2021, 256, 372–378. [Google Scholar] [CrossRef]
- Zilianti, M.; Azuaga, A.; Calderon, F.; Pagés, G.; Mendoza, G. Monitoring the effacement of the uterine cervix by transperineal sonography: a new perspective. J Ultrasound Med 1995, 14, 719–724. [Google Scholar] [CrossRef]
- Aubin, A.M.; McAuliffe, L.; Williams, K.; Issah, A.; Diacci, R.; McAuliffe, J.E.; Sabdia, S.; Phung, J.; Wang, C.A.; Pennell, C.E. Combined vaginal progesterone and cervical cerclage in the prevention of preterm birth: a systematic review and meta-analysis. Am J Obstet Gynecol MFM 2023, 5, 101024. [Google Scholar] [CrossRef] [PubMed]
- Tolosa, J.E.; Boelig, R.C.; Bell, J.; Martínez-Baladejo, M.; Stoltzfus, J.; Mateus, J.; Quiñones, J.N.; Galeano-Herrera, S.; Pereira, L.; Burwick, R.; et al. Concurrent progestogen and cerclage to reduce preterm birth: a multicenter international retrospective cohort. Am J Obstet Gynecol MFM 2024, 6, 101351. [Google Scholar] [CrossRef]
| Adjusted OR | 95% CI | P-value | |
| Body mass index | 0.623 | -0.16- 1.41 | 0.117 |
| Nulliparity | 2.399 | 1.36- 6.67 | 0.007 |
| Natural pregnancy | 1.050 | -8.92- 11.02 | 0.834 |
| History of preterm birth | 7.727 | -7.55- 23.0 | 0.316 |
| Width of external os | -0.167 | -0.41- 0.07 | 0.166 |
| Width of prolapsed membrane | -0.024 | -0.28- 0.23 | 0.853 |
| Distance between external os and baby | 0.173 | -0.08- 0.43 | 0.173 |
| Thickness of Labium posterius | -0.053 | -1.13- 1.02 | 0.921 |
| Gestational weeks at admission | 0.080 | -0.07- 0.23 | 0.298 |
| Type of prolapsed fetal membrane B comparing with A C comparing with A |
-17.469 -15.369 |
-31.5- -3.47 -28.11- -2.63 |
0.0153 0.019 |
| Delivery <7 days (n=53) |
Delivery >7 days (n=22) |
P-value |
|
| Width of external os (mm) | 19.9 (0-93.5) | 13.3 (0-51.7) | 0.040 |
| Width of prolapsed fetal membrane (mm) | 38.2 (6.6-93.5) | 27.0 (0-86.1) | 0.013 |
| Distance from external os to baby (mm) | 15.7 (0-68.2) | 24.4 (2.43-60.6) | 0.067 |
| Thickness of the posterior lip (mm) | 8.50 (0-23.1) | 6.74 (0.75-14.6) | 0.093 |
| Type of prolapsed fetal membrane A B C |
3/9 (33.3%) 32/41 (78.0%) 18/25 (72%) |
6/9 (66.7%) 9/41 (22.0%) 7/25 (28%) |
0.037 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




