Submitted:
03 January 2025
Posted:
03 January 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| COVID-19 | Coronavirus Disease 2019 |
| WHO | World Health Organization |
| SARS-CoV-2 | Severe Acute Respiratory Syndrome Coronavirus 2 |
| ICD-10 | 10th revision of the International Classification of Diseases |
| CI | Confidence Interval |
| WONDER | Wide-Ranging Online Data for Epidemiologic Research |
| ANOVA | One-Way Analysis of Variance |
| AOR | Adjusted Odds Ratio |
| APR | Adjusted Prevalence Ratio |
References
- Lippi, G.; Mattiuzzi, C.; Henry, B.M. Uncontrolled confounding in COVID-19 epidemiology. Diagnosis 2022, 10, 200–202. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. WHO COVID-19 dashboard. Available at: https://data.who.int/dashboards/covid19/cases. Last accessed, January 1, 2025.
- Msemburi, W.; Karlinsky, A.; Knutson, V.; Aleshin-Guendel, S.; Chatterji, S.; Wakefield, J. The WHO estimates of excess mortality associated with the COVID-19 pandemic. Nature 2022, 613, 130–137. [Google Scholar] [CrossRef] [PubMed]
- Sampath, S.; Khedr, A.; Qamar, S.; Tekin, A.; Singh, R.; Green, R.; Kashyap, R. Pandemics Throughout the History. Cureus 2021, 13. [Google Scholar] [CrossRef] [PubMed]
- Lippi, G.; Henry, B.M.; Favresse, J.; Plebani, M. Addressing standardized definitions of post-COVID and long-COVID. cclm 2023, 61, 1361–1362. [Google Scholar] [CrossRef]
- Gheorghita, R.; Soldanescu, I.; Lobiuc, A.; Sturdza, O.A.C.; Filip, R.; Bercu, A.C. ; Dimian, M.; Mangul, S.; Covasa, M. The knowns and unknowns of long COVID-19: from mechanisms to therapeutical approaches. Front. Immunol. 2024, 15, 1344086. [CrossRef]
- Gutzeit, J.; Weiß, M.; Nürnberger, C.; Lemhöfer, C.; Appel, K.S.; Pracht, E.; Reese, J.-P.; Lehmann, C.; Polidori, M.C.; Hein, G.; et al. Definitions and symptoms of the post-COVID syndrome: an updated systematic umbrella review. Eur. Arch. Psychiatry Clin. Neurosci. 2024, 1–12. [Google Scholar] [CrossRef]
- World Health Organization. Post COVID-19 condition (Long COVID). Available at: https://www.who.int/europe/news-room/fact-sheets/item/post-covid-19-condition. Last accessed, January 1, 2025.
- Razak, R.S.A.; Ismail, A.; Aziz, A.F.A.; Suddin, L.S.; Azzeri, A.; Sha’ari, N.I. Post-COVID syndrome prevalence: a systematic review and meta-analysis. BMC Public Heal. 2024, 24, 1–19. [Google Scholar] [CrossRef]
- da Silva, M.M.; Benites, M.N.; Castro, Y.M.; Moura, P.V.; Zhang, L. Prevalence of symptoms of post-COVID-19 condition (long COVID) in children hospitalized with COVID-19: A systematic review of observational studies. Pediatr. Pulmonol. 2024, 59, 3159–3169. [Google Scholar] [CrossRef]
- Atchley-Challenner, R.; Strasser, Z.; Krishnamoorthy, A.; Pant, D.; Chibnik, L.B.; Karlson, E.W. Long COVID: A Narrative Review and Meta-Analysis of Individual Symptom Frequencies. COVID 2024, 4, 1513–1545. [Google Scholar] [CrossRef]
- Kim, J.; Duru, E.E.; Weir, P.; Lee, S. Long COVID Is Associated with Decreased Quality of Life and Increased Mental Disability. COVID 2024, 4, 1719–1730. [Google Scholar] [CrossRef]
- Mattiuzzi, C.; Lippi, G. Long COVID: An Epidemic within the Pandemic. COVID 2023, 3, 773–776. [Google Scholar] [CrossRef]
- Scott, A.; Ansari, W.; Khan, F.; Chambers, R.; Benigno, M.; Di Fusco, M.; McGrath, L.; Malhotra, D.; Draica, F.; Nguyen, J.; et al. Substantial health and economic burden of COVID-19 during the year after acute illness among US adults at high risk of severe COVID-19. BMC Med. 2024, 22, 1–19. [Google Scholar] [CrossRef]
- Mukhida, S.; Khan, S. Does long covid-19 affect the quality of life only to Covid-19 patients or family member also? . J. Fam. Med. Prim. Care 2024, 13, 5442–5443. [Google Scholar] [CrossRef] [PubMed]
- Al-Aly, Z.; Topol, E. Solving the puzzle of Long Covid. Science 2024, 383, 830–832. [Google Scholar] [CrossRef]
- Muthuka, J.K.; Nzioki, J.M.; Kelly, J.O.; Musangi, E.N.; Chebungei, L.C.; Nabaweesi, R.; Kiptoo, M.K. Prevalence and Predictors of Long COVID-19 and the Average Time to Diagnosis in the General Population: A Systematic Review, Meta-Analysis and Meta-Regression. COVID 2024, 4, 968–981. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention, National Center for Health Statistics. National Vital Statistics System, Provisional Mortality on CDC WONDER Online Database. Data are from the final Multiple Cause of Death Files, 2018-2022, and from provisional data for years 2023-2024, as compiled from data provided by the 57 vital statistics jurisdictions through the Vital Statistics Cooperative Program. Accessed at http://wonder.cdc.gov/mcd-icd10-provisional.html on Jan 2, 2025.
- International Classification of Diseases. ICD-10-CM Diagnosis Code U09.9. Available at: https://www.icd10data.com/ICD10CM/Codes/U00-U85/U00-U49/U09-/U09.9. Last accessed, January 1, 2025.
- Global Burden of Disease Long COVID Collaborators; Hanson, S. W.; Abbafati, C.; Aerts, J.G.; Al-Aly, Z.; Ashbaugh, C.; Ballouz, T.; Blyuss, O.; Bobkova, P.; Bonsel, G.; et al. Estimated Global Proportions of Individuals With Persistent Fatigue, Cognitive, and Respiratory Symptom Clusters Following Symptomatic COVID-19 in 2020 and 2021. JAMA 2022, 328, 1604–1615. [CrossRef]
- Bai, F.; Tomasoni, D.; Falcinella, C.; Barbanotti, D.; Castoldi, R.; Mulè, G.; Augello, M.; Mondatore, D.; Allegrini, M.; Cona, A.; et al. Female gender is associated with long COVID syndrome: a prospective cohort study. Clin. Microbiol. Infect. 2021, 28, 611.e9–611e16. [Google Scholar] [CrossRef]
- Jeffrey, K.; Woolford, L.; Maini, R.; Basetti, S.; Batchelor, A.; Weatherill, D.; White, C.; Hammersley, V.; Millington, T.; Macdonald, C.; et al. Prevalence and risk factors for long COVID among adults in Scotland using electronic health records: a national, retrospective, observational cohort study. eClinicalMedicine 2024, 71, 102590. [Google Scholar] [CrossRef]
- Robertson, M.M.; A Qasmieh, S.; Kulkarni, S.G.; A Teasdale, C.; E Jones, H.; McNairy, M.; Borrell, L.N.; Nash, D. The Epidemiology of Long Coronavirus Disease in US Adults. Clin. Infect. Dis. 2022, 76, 1636–1645. [Google Scholar] [CrossRef]
- Hastie, C.E.; Lowe, D.J.; McAuley, A.; Mills, N.L.; Winter, A.J.; Black, C.; Scott, J.T.; O’donnell, C.A.; Blane, D.N.; Browne, S.; et al. True prevalence of long-COVID in a nationwide, population cohort study. Nat. Commun. 2023, 14, 1–6. [Google Scholar] [CrossRef]
- Ford, N.D.; Slaughter, D.; Edwards, D.; Dalton, A.; Perrine, C.; Vahratian, A.; Saydah, S. Long COVID and Significant Activity Limitation Among Adults, by Age — United States, June 1–13, 2022, to June 7–19, 2023. Mmwr-Morbidity Mortal. Wkly. Rep. 2023, 72, 866–870. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Zhong, X.; Wang, Y.; Zeng, X.; Luo, T.; Liu, Q. Clinical determinants of the severity of COVID-19: A systematic review and meta-analysis. PLOS ONE 2021, 16, e0250602. [Google Scholar] [CrossRef]
- Au, L.; Capotescu, C.; Eyal, G.; Finestone, G. Long covid and medical gaslighting: Dismissal, delayed diagnosis, and deferred treatment. SSM - Qual. Res. Heal. 2022, 2, 100167–100167. [Google Scholar] [CrossRef] [PubMed]
- Sunkersing, D.; Ramasawmy, M.; A Alwan, N.; Clutterbuck, D.; Mu, Y.; Horstmanshof, K.; Banerjee, A.; Heightman, M. What is current care for people with Long COVID in England? A qualitative interview study. BMJ Open 2024, 14, e080967. [Google Scholar] [CrossRef] [PubMed]
- Russell, C.D.; Lone, N.I.; Baillie, J.K. Comorbidities, multimorbidity and COVID-19. Nat. Med. 2023, 29, 334–343. [Google Scholar] [CrossRef]
- Reynard, C.; Campling, J.; Gordon, A.L.; Kassianos, G.; Liu, H.-H.; Richter, A.; Vyse, A.; Wiseman, D.J.; Wright, H.; Ellsbury, G. Adult risk groups for vaccine preventable respiratory infections: an overview of the UK environment. Expert Rev. Vaccines 2024, 23, 1052–1067. [Google Scholar] [CrossRef]
- Choe, E.Y.; Du, Y.; Sun, G. Decline in older adults’ daily mobility during the COVID-19 pandemic: the role of individual and built environment factors. BMC Public Heal. 2022, 22, 1–10. [Google Scholar] [CrossRef]
- Kim, Y.K.; Ang, S. Older Adults With Functional Limitations and Their Use of Telehealth During COVID-19. Res. Aging 2022, 45, 609–619. [Google Scholar] [CrossRef]
- Frenk, J.; Chen, L.C.; Chandran, L.; Groff, E.O.H.; King, R.; Meleis, A.; Fineberg, H.V. Challenges and opportunities for educating health professionals after the COVID-19 pandemic. Lancet 2022, 400, 1539–1556. [Google Scholar] [CrossRef]
| Groups | Death rate | p-value |
|---|---|---|
| Cumulative mortality (×100,000) | 0.089 (95% CI, 0.085-0.092 | |
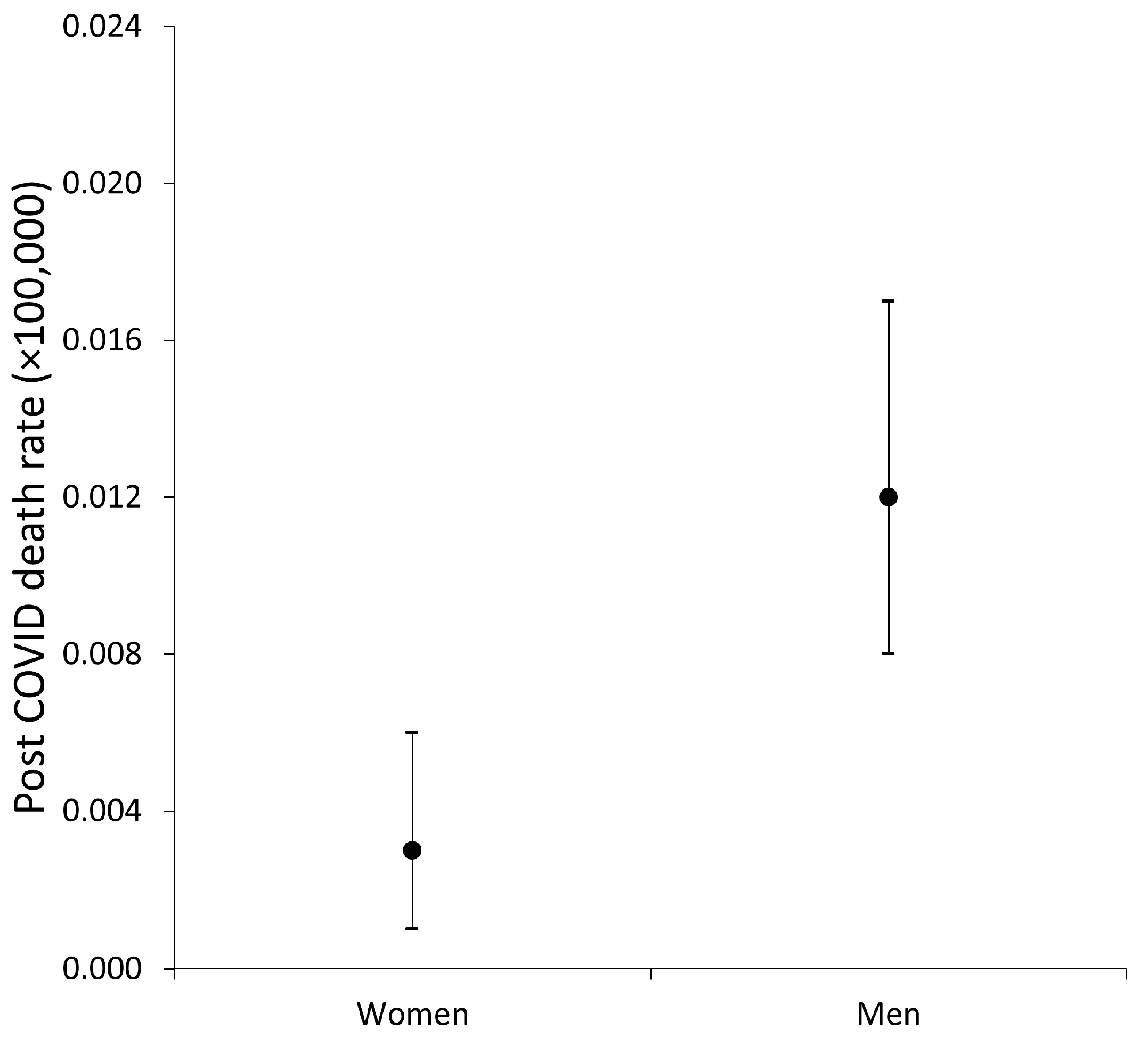
| Gender (age adjusted mortality ×100,000) | ||
| - Males | 0.098 (95% CI, 0.092-0.104) | <0.001 |
| - Females | 0.081 (95% CI, (0.077-0.086) | |
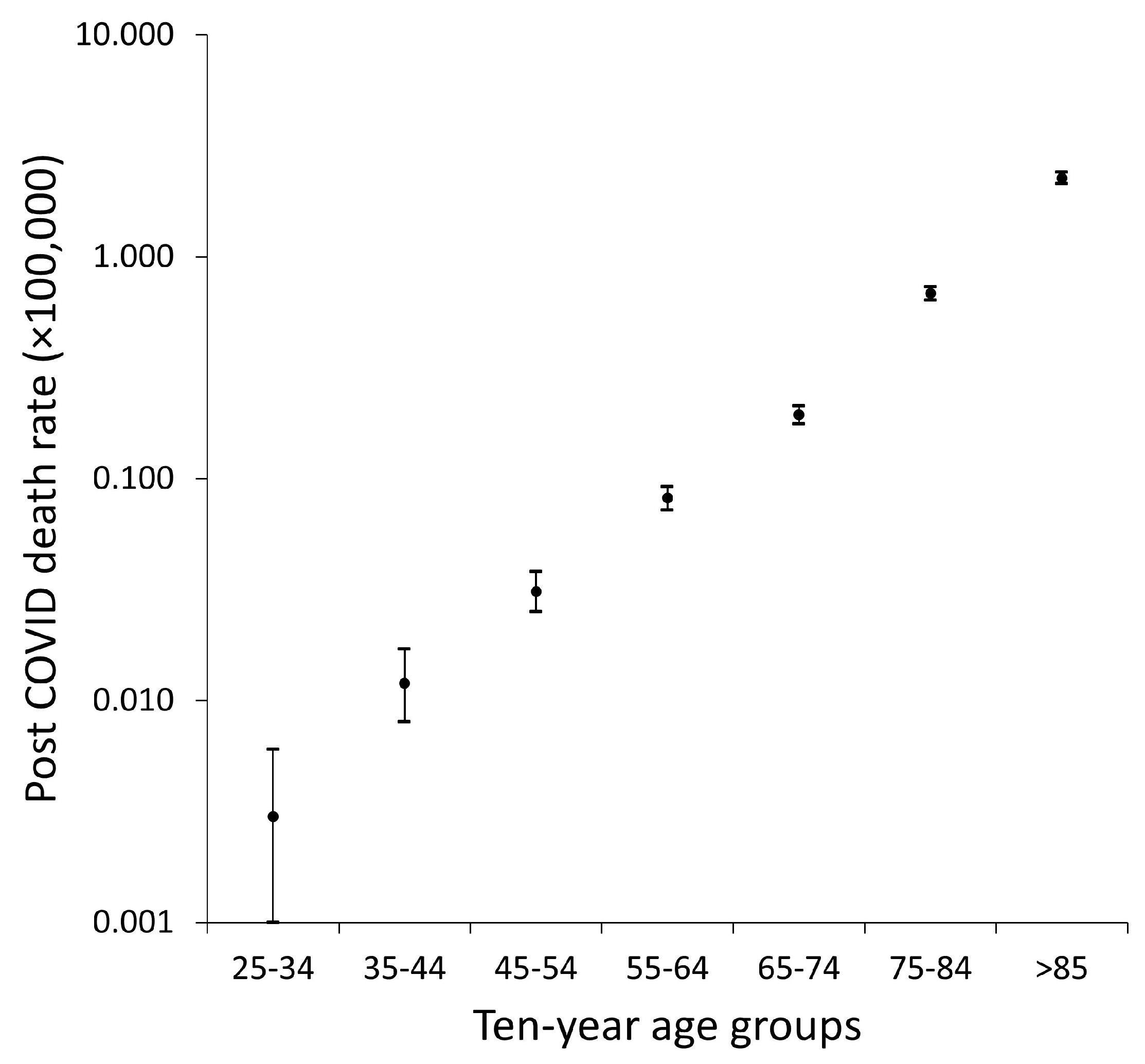
| Age (crude mortality ×100,000) | ||
| - 25-34 years | 0.003 (95% CI, 0.001-0.006) | <0.001 |
| - 35-44 years | 0.012 (95% CI, 0.008-0.017) | |
| - 45-54 years | 0.031 (95% CI, 0.025-0.038) | |
| - 55-64 years | 0.082 (95% CI, 0.072-0.092) | |
| - 65-74 years | 0.194 (95% CI, 0.176-0.212) | |
| - 75-84 years | 0.683 (95% CI, 0.635-0.730) | |
| - Over 85 years | 2.263 (95% CI, 2.125-2.402) | |
| Place of death (total number of deaths; %) | ||
| - Descent’s home | 873 (33.0%) | - |
| - Nursing home/long term care | 698 (26.3%) | |
| - Medical facility (inpatient) | 638 (24.1%) | |
| - Hospice facility | 204 (7.7%) | |
| - Medical facility (outpatient) | 98 (98%) | |
| - Other | 138 (5.2%) | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




