Submitted:
16 December 2024
Posted:
18 December 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Intervention
2.3. Measures
2.4. Statistical Analysis
3. Results
3.1. Changes in Inflammatory and Oxidative Stress Markers
4. Discussion
4.1. Future Directions
4.2. Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Guo, J.; Huang, X.; Dou, L.; et al. Aging and aging-related diseases: from molecular mechanisms to interventions and treatments. Sig Transduct Target Ther. 2022, 7, 391. [Google Scholar] [CrossRef] [PubMed]
- López-Otín, C.; Blasco, M.A.; Partridge, L.; Serrano, M.; Kroemer, G. Hallmarks of aging: An expanding universe. Cell. 2023, 186, 243–278. [Google Scholar] [CrossRef] [PubMed]
- Liguori, I.; Russo, G.; Curcio, F.; et al. Oxidative stress, aging, and diseases. Clin Interv Aging. 2018, 13, 757–772. [Google Scholar] [CrossRef] [PubMed]
- Kökten, T.; Hansmannel, F.; Ndiaye, N.C.; et al. Calorie Restriction as a New Treatment of Inflammatory Diseases. Adv Nutr. 2021, 12, 1558–1570. [Google Scholar] [CrossRef]
- Bosch-Sierra, N.; Grau-del Valle, C.; Salom, C.; et al. Effect of a Very Low-Calorie Diet on Oxidative Stress, Inflammatory and Metabolomic Profile in Metabolically Healthy and Unhealthy Obese Subjects. Antioxidants. 2024, 13, 302. [Google Scholar] [CrossRef]
- Dorling, J.L.; Das, S.K.; Racette, S.B.; et al. Changes in body weight, adherence, and appetite during 2 years of calorie restriction: the CALERIE 2 randomized clinical trial. Eur J Clin Nutr. 2020, 74, 1210–1220. [Google Scholar] [CrossRef]
- Ezzati, A.; Rosenkranz, S.K.; Phelan, J.; et al. The Effects of Isocaloric Intermittent Fasting vs Daily Caloric Restriction on Weight Loss and Metabolic Risk Factors for Noncommunicable Chronic Diseases: A Systematic Review of Randomized Controlled or Comparative Trials. J Acad Nutr Diet. 2023, 123, 318–329.e1. [Google Scholar] [CrossRef]
- Ezzati, A.; McLaren, C.; Bohlman, C.; et al. Does time-restricted eating add benefits to calorie restriction? A systematic review. Obesity (Silver Spring). 2024, 32, 640–654. [Google Scholar] [CrossRef]
- Sampieri, A. , Paoli, A., Spinello, G. et al. Impact of daily fasting duration on body composition and cardiometabolic risk factors during a time-restricted eating protocol: a randomized controlled trial. J Transl Med 2024, 22, 1086. [CrossRef]
- Lin S, Cienfuegos S, Ezpeleta M.; et al. Time-restricted eating without calorie counting for weight loss in a racially diverse population: a randomized controlled trial. Ann Intern Med. 2023, 176, 885–895.
- Wilkinson, M.J.; Manoogian, E.N.C.; Zadourian, A.; et al. Ten-Hour Time-Restricted Eating Reduces Weight, Blood Pressure, and Atherogenic Lipids in Patients with Metabolic Syndrome. Cell Metab. 2020, 31, 92–104.e5. [Google Scholar] [CrossRef] [PubMed]
- Xie, Z.; Sun, Y.; Ye, Y.; et al. Randomized controlled trial for time-restricted eating in healthy volunteers without obesity. Nat Commun. 2022, 13, 1003. [Google Scholar] [CrossRef] [PubMed]
- Moro, T.; Tinsley, G.; Pacelli, F.Q.; Marcolin, G.; Bianco, A.; Paoli, A. Twelve Months of Time-restricted Eating and Resistance Training Improves Inflammatory Markers and Cardiometabolic Risk Factors. Med Sci Sports Exerc. 2021, 53, 2577–2585. [Google Scholar] [CrossRef] [PubMed]
- Cienfuegos S, Gabel K, Kalam F; et al. Effects of 4- and 6-h time-restricted feeding on weight and cardiometabolic health: a randomized controlled trial in adults with obesity. Cell Metab. 2020, 32, 366–378.e3. [CrossRef]
- Sutton, E.F.; Beyl, R.; Early, K.S.; et al. Early time-restricted feeding improves insulin sensitivity, blood pressure, and oxidative stress even without weight loss in men with prediabetes. Cell Metab. 2018, 27, 1212–1221.e3. [Google Scholar] [CrossRef]
- Ezzati, A.; Pak, V.M. The effects of time-restricted eating on sleep, cognitive decline, and Alzheimer's disease. Exp Gerontol. 2023, 171, 112033. [Google Scholar] [CrossRef]
- Ezzati, A.; Rosenkranz, S.K.; Horne, B.D. Importance of Intermittent Fasting Regimens and Selection of Adequate Therapy on Inflammation and Oxidative Stress in SARS-CoV-2 Infection. Nutrients. 2022, 14, 4299. [Google Scholar] [CrossRef]
- Gabel, K.; Hoddy, K.K.; Haggerty, N.; et al. Effects of 8-hour time restricted feeding on body weight and metabolic disease risk factors in obese adults: a pilot study. Nutr Healthy Aging. 2018, 4, 345–353. [Google Scholar] [CrossRef]
- Haganes, K.L.; Silva, C.P.; Eyjólfsdóttir, S.K.; et al. Time-restricted eating and exercise training improve HbA1c and body composition in women with overweight/obesity: a randomized controlled trial. Cell Metab. 2022, 34, 1457–1471.e4. [Google Scholar] [CrossRef]
- Peters, B.; Vahlhaus, J.; Pivovarova-Ramich, O. Meal timing and its role in obesity and associated diseases. Front Endocrinol. 2024, 15, 1359772. [Google Scholar] [CrossRef]
- Anton, S.D.; Lee, S.A.; Donahoo, W.T.; McLaren, C.; Manini, T.; Leeuwenburgh, C.; Pahor, M. The Effects of Time Restricted Feeding on Overweight, Older Adults: A Pilot Study. Nutrients. 2019, 11, 1500. [Google Scholar] [CrossRef] [PubMed]
- Li, C.; Xing, C.; Zhang, J.; Zhao, H.; Shi, W.; He, B. Eight-hour time-restricted feeding improves endocrine and metabolic profiles in women with anovulatory polycystic ovary syndrome. J Transl Med. 2021, 19, 148. [Google Scholar] [CrossRef] [PubMed]
- Martens, C.R.; Rossman, M.J.; Mazzo, M.R.; Jankowski, L.R.; Nagy, E.E.; Denman, B.A.; Richey, J.J.; Johnson, S.A.; Ziemba, B.P.; Wang, Y.; Peterson, C.M.; Chonchol, M.; Seals, D.R. Short-term time-restricted feeding is safe and feasible in non- obese healthy midlife and older adults. GeroScience. 2020, 42, 667–686. [Google Scholar] [CrossRef] [PubMed]
- Akasheh, R.T.; Ankireddy, A.; Gabel, K.; Ezpeleta, M.; Lin, S.; Tamatam, C.M.; Reddy, S.P.; Spring, B.; Cheng, T.-Y.D.; Fontana, L.; et al. Effect of Time-Restricted Eating on Circulating Levels of IGF1 and Its Binding Proteins in Obesity: An Exploratory Analysis of a Randomized Controlled Trial. Nutrients 2024, 16, 3476. [Google Scholar] [CrossRef]
- Lee, S.A.; Sypniewski, C.; Bensadon, B.A.; McLaren, C.; Donahoo, W.T.; Sibille, K.T.; Anton, S. Determinants of adherence in time-restricted feeding in older adults: lessons from a pilot study. Nutrients. 2020, 12, 874. [Google Scholar] [CrossRef]
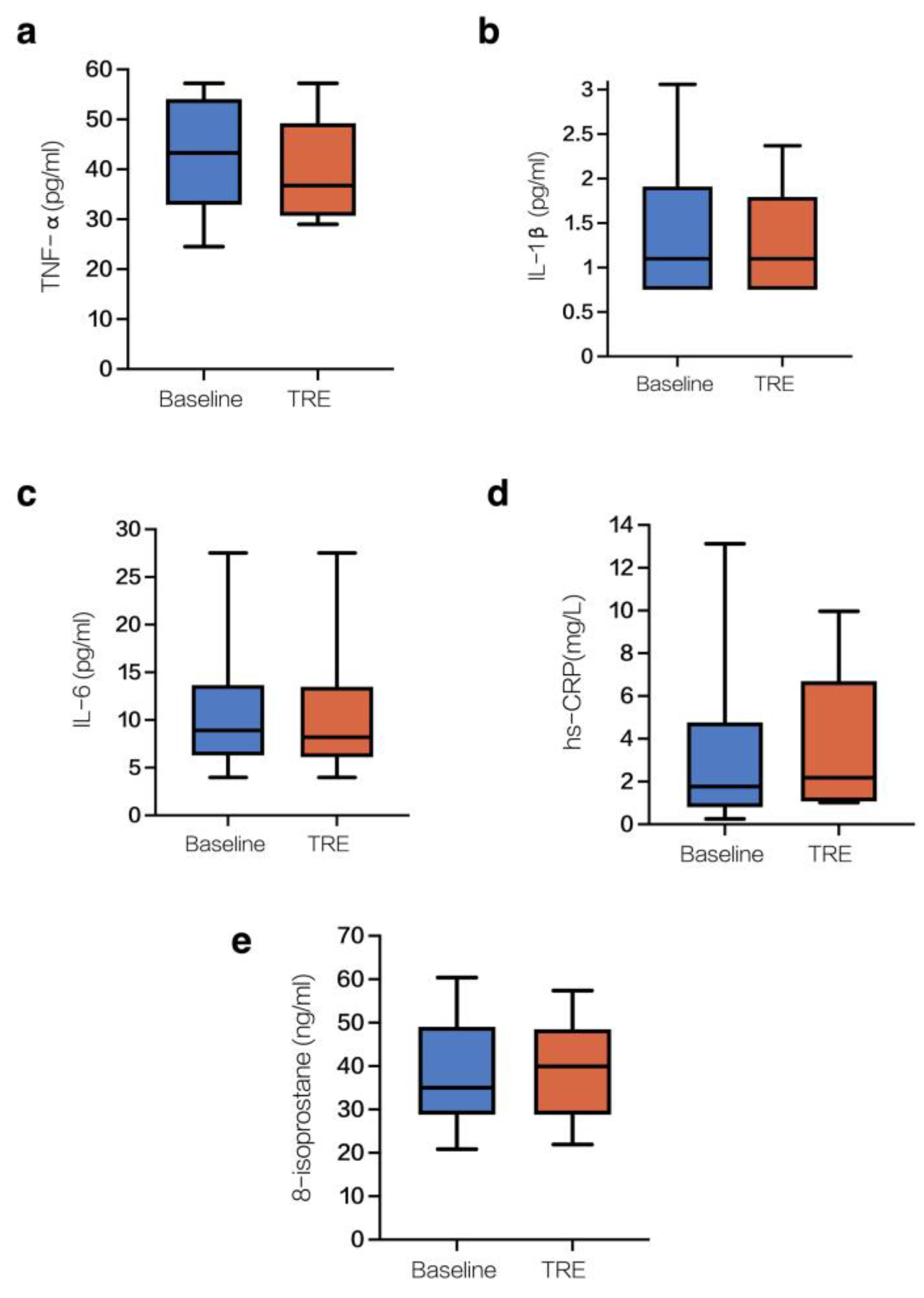
| Study Measures | Baseline M (SD) | TRE M (SD) | Δ Mean (SD) | %Change | Cohen’s d | p-Value |
| TNF-alpha (pg/ml) | 43.2 (11.2) | 39.7 (10.0) | −3.5 (5.7) | −8% | 0.33 | 0.101 |
| IL-1β (pg/ml) | 1.4 (0.8) | 1.3 (0.6) | −0.1 (0.7) | −11% | 0.23 | 0.499 |
| IL-6 (pg/ml) | 10.8 (7.2) | 10.8 (7.2) | −0.001 (2.4) | 0% | 0.03 | 0.998 |
| hs-CRP (mg/L) | 3.3 (4.1) | 3.6 (3.4) | 0.3 (1.8) | 10% | 0.01 | 0.596 |
| 8-isoprostane (ng/mL) | 41.3 (13.8) | 38.7 (11.6) | -0.4 (12.2) | -1% | 0.07 | 0.919 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




