Submitted:
02 December 2024
Posted:
04 December 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Related Work
3. 3. LOCKED dataset
3.1. Preprocessing Stage
3.2. Data Labeling
- Hostility (items 7, 34, 35, 39, 43): This dimension reflects anger, irritability, and aggression. A high score may suggest a tendency to react with anger or experience feelings of hostility toward others.
- Somatization (items 18, 23, 26, 29, 31): This refers to the experience of physical symptoms without an apparent medical cause, often linked to emotional or psychological factors. A high score may indicate a tendency to report multiple physical complaints.
- Depression (items 9, 10, 11, 27, 42): This scale measures symptoms of depression, including profound sadness, loss of interest, fatigue, and hopelessness. A high score suggests a significant presence of depressive symptoms.
- Obsessive-Compulsive (items 16, 20, 21, 25, 28): T This dimension relates to the presence of intrusive thoughts (obsessions) or ritualistic behaviors (compulsions). A high score indicates a greater tendency toward obsessive-compulsive patterns.
- Anxiety (items 6, 12, 30, 38, 41): This scale assesses symptoms of anxiety, such as excessive worry, tension, and fear. A high score reflects a high presence of anxiety symptoms. (11 features)
- Interpersonal Sensitivity (items 14, 15, 17, 32, 36): This dimension evaluates feelings of inferiority and self-criticism in social interactions. A high score indicates heightened sensitivity to criticism and feelings of inadequacy in social situations.
- Agoraphobia (items 3, 8, 22, 24, 37): This refers to the fear of being in situations where escape might be difficult or help unavailable, particularly in the case of a panic attack. A high score suggests a stronger presence of these fears.
- Paranoid Ideation (items 2, 5, 19, 40, 44): This scale measures paranoid thoughts, such as excessive distrust or beliefs of being persecuted. A high score reflects a significant tendency toward paranoia.
- Psychoticism (items 1, 4, 13, 33, 45): This dimension assesses symptoms associated with psychotic disorders, such as hallucinations, unusual thoughts, and eccentric behaviors. A high score indicates a greater presence of psychotic symptoms.
3.3. 3.3 Studied features
4. Experimental Benchmarks
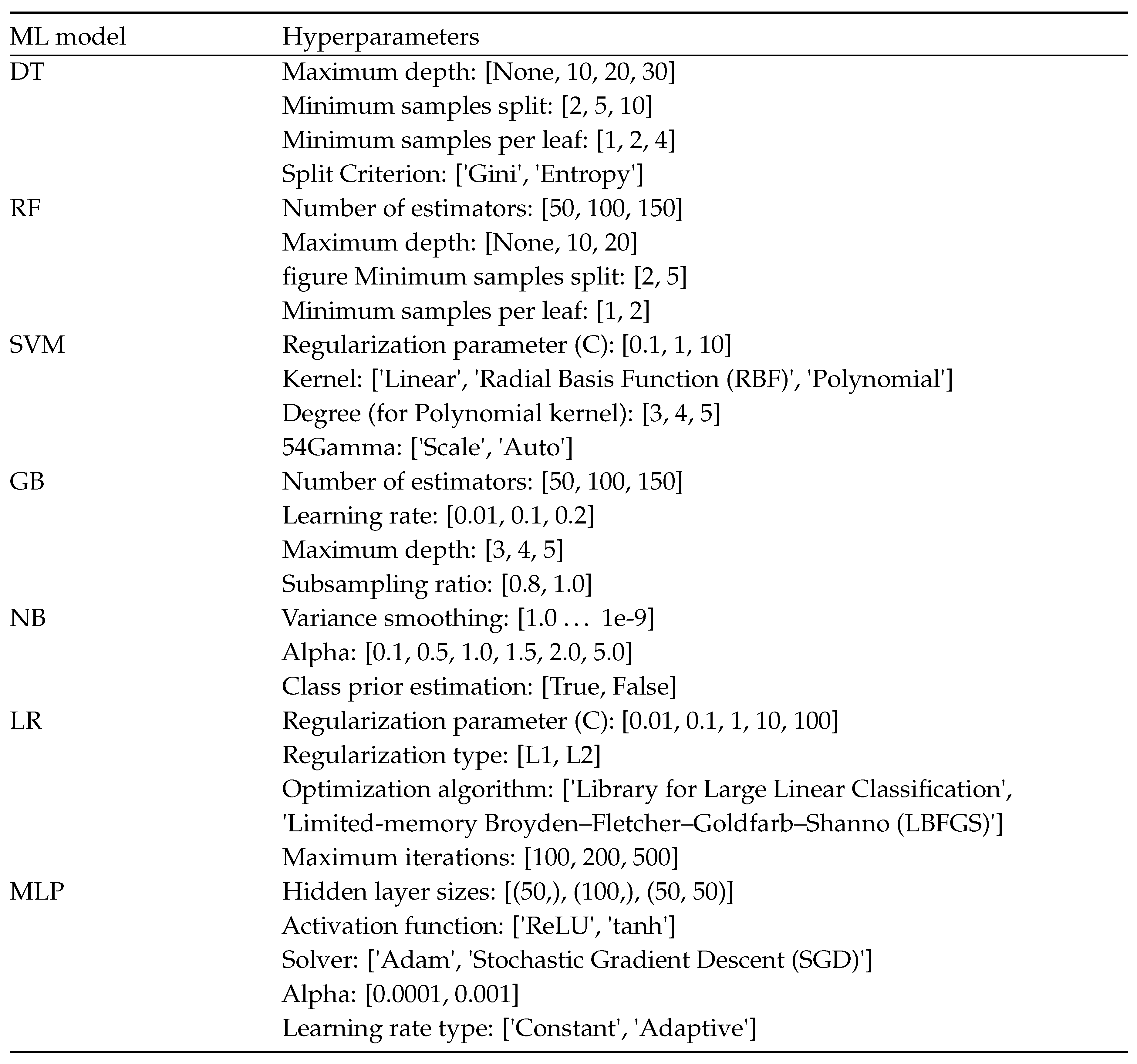 |
| ML model | Training set | Test set |
| Hostility | 233 | 59 |
| Somatization | 252 | 64 |
| Depression | 252 | 64 |
| Obsession-Compulsion | 267 | 67 |
| Anxiety | 270 | 68 |
| Interpersonal Sensitivity | 270 | 68 |
| Agoraphobia | 198 | 50 |
| Paranoid Ideation | 208 | 52 |
| Psychoticism | 224 | 56 |
| Training subset | Binary classifier | Best ML model | Train | Validation | Test |
| Hostility | DT | 91.15% ± 2.50 | 85.16% ± 1.48 | 81.36% | |
| Somatization | SVM | 81.70% ± 5.86 | 76.36% ± 3.09 | 87.50% | |
| Depression | SVM | 85.09% ± 4.47 | 80.27% ± 2.85 | 87.50% | |
| Obsession-Compulsion | RF | 90.96% ± 2.40 | 82.40% ± 1.50 | 89.55% | |
| Demographic characteristics | Anxiety | SVM | 81.89% ± 5.42 | 77.81% ± 3.47 | 89.71% |
| Interpersonal Sensitivity | DT | 89.60% ± 2.42 | 87.59% ± 1.01 | 85.29% | |
| Agoraphobia | RF | 92.76% ± 1.25 | 85.89% ± 0.53 | 90% | |
| Paranoid Ideation | DT | 92.23% ± 1.69 | 84.52% ± 1.1 | 92.31% | |
| Psychoticism | MLP | 86.83% ± 7.37 | 79.95% ± 3.07 | 87.50% | |
| Hostility | SMV | 83.94% ± 10.16 | 76.75% ± 6.93 | 88.14% | |
| Somatization | SVM | 84.14% ± 9.7 | 76.85% ± 7.98 | 87.5% | |
| Depression | MLP | 73.34% ± 3.67 | 71.04% ± 3.46 | 84.38% | |
| Obsession-Compulsion | RF | 95.35% ± 2.12 | 88.36% ± 0.78 | 89.55% | |
| Living environment | Anxiety | SVM | 82.2% ± 10.67 | 75.35% ± 7.49 | 94.12% |
| Interpersonal Sensitivity | GB | 94.44% ± 5.40 | 80.75% ± 1.74 | 83.82% | |
| Agoraphobia | MLP | 90.60% ± 7.83 | 81.22% ± 3.77 | 90.00% | |
| Paranoid Ideation | RF | 96.09% ± 1.98 | 85.63% ± 0.67 | 90.38% | |
| Psychoticism | RF | 96.50% ± 1.63 | 79.53% ± 1.35 | 92.86% | |
| Hostility | SVM | 89.22% ± 7.89 | 83.76% ± 5.56 | 91.52% | |
| Somatization | RF | 96.3% ± 1.3 | 87.86% ± 0.91 | 87.5% | |
| Depression | DT | 93.12% ± 2.29 | 78.73% ± 1.25 | 85.29% | |
| Obsession-Compulsion | RF | 97.64% ± 0.98 | 88.20% ± 0.71 | 88.06% | |
| Economic status | Anxiety | RF | 97.17% ± 1.12 | 85.75% ± 0.51 | 85.29% |
| Interpersonal Sensitivity | DT | 91.98% ± 3.01 | 81.55% ± 1.48 | 91.18% | |
| Agoraphobia | SVM | 87.94% ± 9.88 | 80.12% ± 6.78 | 94% | |
| Paranoid Ideation | RF | 95.66% ± 1.56 | 85.4% ± 1.37 | 96.15% | |
| Psychoticism | NB | 83.92% ± 4.15 | 82.60% ± 3.74 | 87.50% | |
| Hostility | DT | 95.74% ± 1.15 | 93.12% ± 0.35 | 96.61% | |
| Somatization | RF | 96.7% ± 0.15 | 96.15% ± 0.68 | 92.19% | |
| Depression | GB | 96.84% ± 0.79 | 95.37% ± 0.78 | 95.31% | |
| Health impacts | Obsession-Compulsion | DT | 94.01% ± 0.61 | 93.51% ± 0.7 | 98.51% |
| undersampling | Anxiety | RF | 95.4% ± 0.16 | 95.31% ± 0.41 | 92.65% |
| Interpersonal Sensitivity | DT | 95.68% ± 0.63 | 94..69% ± 0.7 | 92.65% | |
| Agoraphobia | NB | 92.79% ± 8.67 | 92.61% ± 8.91 | 98% | |
| Paranoid Ideation | DT | 92.3% ± 0.68 | 92% ± 1.13 | 100% | |
| Psychoticism | SVM | 87.33% ± 7.45 | 85.89% ± 7.39 | 91.07% |
| Training subset | Binary classifier | Train | Validation | Test | |
| Hostility | 88.61% ± 0.19 | 81.76% ± 0.84 | 65.52% | ||
| Somatization | 78.19% ± 0.09 | 72.03% ± 1.01 | 81.25% | ||
| Depression | 97.81% ± 0.02 | 94.09% ± 0.14 | 81.25% | ||
| Obsession-Compulsion | 83.02% ± 0.06 | 75.55% ± 0.79 | 81.82% | ||
| Demographic characteristics | Anxiety | 76.77% ± 0.05 | 98.10% ± 0.04 | 79.41% | |
| Interpersonal Sensitivity | 83.40% ± 0.16 | 67.63% ± 0.22 | 73.53% | ||
| Agoraphobia | 91.67 % ± 0.01 | 96.41% ± 0.02 | 90.00% | ||
| Paranoid Ideation | 89.41% ± 0.05 | 78.61% ± 1.77 | 96.15% | ||
| Psychoticism | 96.26% ± 0.05 | 87.44% ± 0.53 | 82.14% | ||
| Hostility | 82.28% ± 0.04 | 78.52% ± 1.22 | 79.31% | ||
| Somatization | 83.13% ± 0.03 | 77.86% ± 0.43 | 81.25% | ||
| Depression | 74.38% ± 2.72 | 69.23% ± 2.71 | 84.38% | ||
| Obsession-Compulsion | 88.25% ± 0.05 | 81.33% ± 0.54 | 87.88% | ||
| Living environment | Anxiety | 83.25% ± 0.04 | 76.32% ± 0.56 | 91.18% | |
| Interpersonal Sensitivity | 88.26% ± 0.02 | 75.43% ± 0.78 | 81.25% | ||
| Agoraphobia | 86.85% ± 0.06 | 78.68% ± 0.18 | 88.00% | ||
| Paranoid Ideation | 95.13% ± 0.03 | 78.07% ± 0.24 | 92.31% | ||
| Psychoticism | 94.37% ± 0.04 | 80.58% ± 0.21 | 89.29% | ||
| Hostility | 90.60% ± 0.01 | 86.11% ± 1.20 | 86.21% | ||
| Somatization | 93.43% ± 0.01 | 83.05% ± 0.29 | 84.38% | ||
| Depression | 90.04% ± 0.04 | 71.44% ± 0.48 | 78.13% | ||
| Obsession-Compulsion | 97.76% ± 0.00 | 88.09% ± 0.30 | 93.94% | ||
| Economic status | Anxiety | 96.32% ± 0.00 | 86.70% ± 0.25 | 82.35% | |
| Interpersonal Sensitivity | 88.31% ± 0.03 | 78.29% ± 0.06 | 88.24% | ||
| Agoraphobia | 93.43% ± 0.01 | 90.21% ± 0.29 | 88.00% | ||
| Paranoid Ideation | 89.66% ± 0.01 | 80.03% ± 0.58 | 92.31% | ||
| Psychoticism | 76.33% ± 0.05 | 76.70% ± 0.40 | 75.00% | ||
| Hostility | 94.02% ± 0.00 | 91.05% ± 0.15 | 93.10% | ||
| Somatization | 93.66% ± 0.01 | 93.71% ± 0.22 | 84.38% | ||
| Depression | 94.44% ± 0.00 | 92.00% ± 0.29 | 90.63% | ||
| Health impacts | Obsession-Compulsion | 90.29% ± 0.02 | 86.31% ± 0.65 | 96.97% | |
| Anxiety | 91.87% ± 0.00 | 91.94% ± 0.06 | 91.18% | ||
| Interpersonal Sensitivity | 93.28% ± 0.02 | 90.19% ± 0.28 | 88.24% | ||
| Agoraphobia | 92.88% ± 0.02 | 92.22% ± 0.22 | 96.00% | ||
| Paranoid Ideation | 85.61% ± 0.03 | 86.18% ± 0.64 | 100.00% | ||
| Psychoticism | 83.98% ± 0.08 | 83.92% ± 0.92 | 82.14% | ||
| Training subset | Binary classifier | Train | Validation | Test |
| Hostility | 94.35% ± 0.07 | 91.92% ± 0.50 | 96.67% | |
| Somatization | 99.19% ± 0.01 | 92.69% ± 0.20 | 93.75% | |
| Depression | 97.81% ± 0.02 | 94.09% ± 0.14 | 93.75% | |
| Obsession-Compulsion | 97.93% ± 0.01 | 94.09% ± 0.44 | 97.06% | |
| Demographic characteristics | Anxiety | 98.10% ± 0.04 | 95.86% ± 0.08 | 100.00% |
| Interpersonal Sensitivity | 95.56% ± 0.05 | 90.28% ± 0.45 | 97.06% | |
| Agoraphobia | 96.41% ± 0.02 | 90.09% ± 0.50 | 92.00% | |
| Paranoid Ideation | 97.82% ± 0.01 | 90.34% ± 0.50 | 88.46% | |
| Psychoticism | 96.89% ± 0.02 | 82.98% ± 0.76 | 92.86% | |
| Hostility | 100.00% ± 0.00 | 99.26% ± 0.02 | 96.67% | |
| Somatization | 99.41% ± 0.00 | 97.46% ± 0.10 | 93.75% | |
| Depression | 88.41% ± 1.24 | 81.01% ± 3.88 | 84.38% | |
| Obsession-Compulsion | 98.30% ± 0.01 | 92.49% ± 0.17 | 91.18% | |
| Living environment | Anxiety | 98.68% ± 0.01 | 95.54% ± 0.15 | 97.06% |
| Interpersonal Sensitivity | 98.11% ± 0.02 | 85.69% ± 0.59 | 94.12% | |
| Agoraphobia | 94.96% ± 0.02 | 88.03% ± 0.84 | 92.00% | |
| Paranoid Ideation | 100.00% ± 0.00 | 87.03% ± 0.63 | 88.46% | |
| Psychoticism | 98.00% ± 0.03 | 83.93% ± 0.58 | 96.43% | |
| Hostility | 100.00% ± 0.00 | 99.00% ± 0.04 | 96.67% | |
| Somatization | 98.82% ± 0.01 | 86.01% ± 0.56 | 93.75% | |
| Depression | 98.41% ± 0.01 | 86.70% ± 0.02 | 93.75% | |
| Obsession-Compulsion | 98.13% ± 0.01 | 89.41% ± 0.09 | 82.35% | |
| Economic status | Anxiety | 99.28% ± 0.00 | 87.16% ± 0.35 | 88.24% |
| Interpersonal Sensitivity | 94.39% ± 0.05 | 85.42% ± 0.60 | 94.12% | |
| Agoraphobia | 100.00% ± 0.00 | 96.67% ± 0.44 | 100.00% | |
| Paranoid Ideation | 100.00% ± 0.00 | 91.89% ± 0.37 | 100.00% | |
| Psychoticism | 93.76% ± 0.01 | 93.87% ± 0.09 | 100.00% | |
| Hostility | 100.00% ± 0.00 | 100.00% ± 0.00 | 100.00% | |
| Somatization | 100.00% ± 0.00 | 100.00% ± 0.00 | 100.00% | |
| Depression | 100.00% ± 0.00 | 100.00% ± 0.00 | 100.00% | |
| Health impacts | Obsession-Compulsion | 99.25% ± 0.00 | 99.29% ± 0.02 | 100.00% |
| Anxiety | 99.26% ± 0.00 | 99.33% ± 0.02 | 94.12% | |
| Interpersonal Sensitivity | 99.26% ± 0.00 | 99.33% ± 0.02 | 97.06% | |
| Agoraphobia | 100.00% ± 0.00 | 100.00% ± 0.00 | 100.00% | |
| Paranoid Ideation | 100.00% ± 0.00 | 100.00% ± 0.00 | 100.00% | |
| Psychoticism | 100.00% ± 0.00 | 100.00% ± 0.00 | 100.00% |
5. Conclusions and Future Works
Acknowledgments
Appendix A Personal questionnaire
Appendix B SA-45 Test
Appendix C Distribution of initial features among the four subsets
- Gender
- Age
- Nationality
- Marital Status
- Current Documentation Status
- Education Level
- Family Structure before COVID
- Family Structure during COVID
- Change in Family Structure
- Number of Minors in Care During COVID
- Adults in Care Over 18
- Type of Living Space During Confinement
- Property Ownership
- Square Meters of Living Space
- Light During Quarantine
- Ventilation During Quarantine
- Number of Rooms
- Number of Cohabitants
- Number of Cohabitants in the Same Room
- Outings During Quarantine
- Assessment of COVID Measures
- Employment Status Before Quarantine
- Employment Status During Quarantine
- Employment Status After Quarantine
- Change in Employment Status
- Working Hours Before Quarantine
- Occupation of the Person with the Highest Economic Contribution
- Net Monthly Income Before COVID
- Net Monthly Income During COVID
- Change in Net Monthly Income
- Financial Sufficiency and Situation During COVID
- Financial Sufficiency and Situation After COVID
- Health Condition and Specific Needs
- Disability Degree
- Suicide Attempt
- COVID Diagnosis
- COVID Severity
- Isolation During COVID Diagnosis
- Family Member Diagnosed with COVID
- Family Member COVID Severity
- Co-living with a Diagnosed Family Member
Appendix D Information related to computational resources used for the best ML models.
| Training subset | Binary classifier | Time (s) | Memory space (KB) | Tunned hyperparameters |
| Hostility | 0.750003 | 6 | - | |
| Somatization | 25.170890 | 15 | - | |
| Depression | 32.415980 | 13 | - | |
| Obsession-Compulsion | 10.62998 | 457 | - | |
| Demographic characteristics | Anxiety | 89.17416 | 16 | - |
| Interpersonal Sensitivity | 0.842999 | 7 | - | |
| Agoraphobia | 8.176015 | 262 | - | |
| Paranoid Ideation | 0.715997 | 9 | - | |
| Psychoticism | 43.589999 | 89 | - | |
| Hostility | 40.453997 | 15 | - | |
| Somatization | 42.414486 | 13 | - | |
| Depression | 16.899999 | 87 | - | |
| Obsession-Compulsion | 8.106001 | 514 | - | |
| Living environment | Anxiety | 48.644653 | 15 | - |
| Interpersonal Sensitivity | 13.537016 | 98 | - | |
| Agoraphobia | 47.707595 | 74 | - | |
| Paranoid Ideation | 8.211001 | 285 | - | |
| Psychoticism | 8.212002 | 250 | - | |
| Hostility | 14.565359 | 10 | - | |
| Somatization | 9.50388 | 813 | - | |
| Depression | 0.887095 | 10 | - | |
| Obsession-Compulsion | 8.809057 | 809 | - | |
| Economic status | Anxiety | 13.53503 | 547 | - |
| Interpersonal Sensitivity | 0.772601 | 7 | - | |
| Agoraphobia | 17.598321 | 8 | - | |
| Paranoid Ideation | 8.533304 | 546 | - | |
| Psychoticism | 3.693993 | 4 | - | |
| Hostility | 0.646555 | 4 | - | |
| Somatization | 11.578461 | 76 | - | |
| Depression | 9.281631 | 426 | - | |
| Health impacts | Obsession-Compulsion | 0.664224 | 5 | - |
| Anxiety | 8.356251 | 99 | - | |
| Interpersonal Sensitivity | 0.827175 | 5 | - | |
| Agoraphobia | 7.309343 | 3 | - | |
| Paranoid Ideation | 0.716712 | 4 | - | |
| Psychoticism | 8.846613 | 10 | - |
References
- Radovanovic, D.; Rizzi, M.; Pini, S.; Saad, M.; Chiumello, D.A.; Santus, P. Helmet CPAP to treat acute hypoxemic respiratory failure in patients with COVID-19: a management strategy proposal. Journal of clinical medicine 2020, 9, 1191. [Google Scholar] [CrossRef]
- Grant, M.C.; Geoghegan, L.; Arbyn, M.; Mohammed, Z.; McGuinness, L.; Clarke, E.L.; Wade, R.G. The prevalence of symptoms in 24,410 adults infected by the novel coronavirus (SARS-CoV-2; COVID-19): A systematic review and meta-analysis of 148 studies from 9 countries. PloS one 2020, 15, e0234765. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, F.; Zviedrite, N.; Uzicanin, A. Effectiveness of workplace social distancing measures in reducing influenza transmission: a systematic review. BMC public health 2018, 18, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Livingston, E.; Bucher, K.; Rekito, A. Coronavirus disease 2019 and influenza 2019-2020. Jama 2020, 323, 1122–1122. [Google Scholar] [CrossRef]
- Shah, S.G.S.; Nogueras, D.; Van Woerden, H.C.; Kiparoglou, V. The COVID-19 pandemic: a pandemic of lockdown loneliness and the role of digital technology. Journal of medical Internet research 2020, 22, e22287. [Google Scholar] [CrossRef]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The psychological impact of quarantine and how to reduce it: rapid review of the evidence. The lancet 2020, 395, 912–920. [Google Scholar] [CrossRef]
- Rodríguez-Rey, R.; Garrido-Hernansaiz, H.; Collado, S. Psychological impact of COVID-19 in Spain: Early data report. Psychological Trauma: Theory, Research, Practice, and Policy 2020, 12, 550. [Google Scholar] [CrossRef]
- Gismero-González, E.; Bermejo-Toro, L.; Cagigal, V.; Roldán, A.; Martínez-Beltrán, M.J.; Halty, L. Emotional impact of COVID-19 lockdown among the Spanish population. Frontiers in Psychology 2020, 11, 616978. [Google Scholar] [CrossRef] [PubMed]
- González-Sanguino, C.; Ausín, B.; Castellanos, M.Á.; Saiz, J.; López-Gómez, A.; Ugidos, C.; Muñoz, M. Mental health consequences during the initial stage of the 2020 Coronavirus pandemic (COVID-19) in Spain. Brain, behavior, and immunity 2020, 87, 172–176. [Google Scholar] [CrossRef] [PubMed]
- Miranda-Mendizabal, A.; Recoder, S.; Calbo Sebastian, E.; Casajuana Closas, M.; Leiva Ureña, D.; Manolov, R.; Matilla Santander, N.; Forero, C.G.; Castellví, P. Socio-economic and psychological impact of COVID-19 pandemic in a Spanish cohort BIOVAL-D-COVID-19 study protocol. Gaceta Sanitaria 2022, 36, 70–73. [Google Scholar] [CrossRef]
- Sadegh-Zadeh, S.A.; Bahrami, M.; Najafi, A.; Asgari-Ahi, M.; Campion, R.; Hajiyavand, A.M. Evaluation of COVID-19 pandemic on components of social and mental health using machine learning, analysing United States data in 2020. Frontiers in Psychiatry 2022, 13, 933439. [Google Scholar] [CrossRef]
- Wang, X.; Li, H.; Sun, C.; Zhang, X.; Wang, T.; Dong, C.; Guo, D. Prediction of mental health in medical workers during COVID-19 based on machine learning. Frontiers in public health 2021, 9, 697850. [Google Scholar] [CrossRef] [PubMed]
- Samuelson, K.W.; Dixon, K.; Jordan, J.T.; Powers, T.; Sonderman, S.; Brickman, S. Mental health and resilience during the coronavirus pandemic: A machine learning approach. Journal of Clinical Psychology 2022, 78, 821–846. [Google Scholar] [CrossRef] [PubMed]
- Rezapour, M.; Hansen, L. A machine learning analysis of COVID-19 mental health data. Scientific reports 2022, 12, 14965. [Google Scholar] [CrossRef] [PubMed]
- Prout, T.A.; Zilcha-Mano, S.; Aafjes-van Doorn, K.; Békés, V.; Christman-Cohen, I.; Whistler, K.; Kui, T.; Di Giuseppe, M. Identifying predictors of psychological distress during COVID-19: a machine learning approach. Frontiers in psychology 2020, 11, 586202. [Google Scholar] [CrossRef]
- Herbert, C.; El Bolock, A.; Abdennadher, S. How do you feel during the COVID-19 pandemic? A survey using psychological and linguistic self-report measures, and machine learning to investigate mental health, subjective experience, personality, and behaviour during the COVID-19 pandemic among university students. BMC psychology 2021, 9, 90. [Google Scholar]
- Glowacz, F.; Schmits, E. Psychological distress during the COVID-19 lockdown: The young adults most at risk. Psychiatry research 2020, 293, 113486. [Google Scholar] [CrossRef] [PubMed]
- Simjanoski, M.; Ballester, P.L.; da Mota, J.C.; De Boni, R.B.; Balanzá-Martínez, V.; Atienza-Carbonell, B.; Bastos, F.I.; Frey, B.N.; Minuzzi, L.; Cardoso, T.d.A.; others. Lifestyle predictors of depression and anxiety during COVID-19: a machine learning approach. Trends in Psychiatry and Psychotherapy 2022, 44, e20210365. [Google Scholar] [CrossRef]
- Tubío-Fungueiriño, M.; Cernadas, E.; Gonçalves, Ó.F.; Segalas, C.; Bertolín, S.; Mar-Barrutia, L.; Real, E.; Fernández-Delgado, M.; Menchón, J.M.; Carvalho, S.; others. Viability study of machine learning-based prediction of covid-19 pandemic impact in obsessive-compulsive disorder patients. Frontiers in Neuroinformatics 2022, 16, 807584. [Google Scholar] [CrossRef] [PubMed]
- Alonso, P.; Bertolín, S.; Segalàs, J.; Tubío-Fungueiriño, M.; Real, E.; Mar-Barrutia, L.; Fernández-Prieto, M.; Carvalho, S.; Carracedo, A.; Menchón, J. How is COVID-19 affecting patients with obsessive–compulsive disorder? A longitudinal study on the initial phase of the pandemic in a Spanish cohort. European Psychiatry 2021, 64, e45. [Google Scholar] [CrossRef] [PubMed]
- Aguilar-Latorre, A.; Oliván-Blázquez, B.; Porroche-Escudero, A.; Méndez-López, F.; García-Gallego, V.; Benedé-Azagra, B.; Magallón-Botaya, R. The impact of the COVID-19 lockdown on depression sufferers: a qualitative study from the province of Zaragoza, Spain. BMC Public Health 2022, 22, 780. [Google Scholar] [CrossRef] [PubMed]
- Holgado-Tello, F.P.; Vila-Abad, E.; Barbero-Garcia, M. Estructura interna del Symptom Assessment-45 Questionnaire (SA-45). Acción psicológica 2019, 16, 31–42. [Google Scholar] [CrossRef]
- Sandín, B.; Valiente, R.M.; Chorot, P.; Santed, M.A.; Lostao, L. SA-45: a brief form of the SCL-90. Psicothema 2008, 20, 290–296. [Google Scholar] [PubMed]
- Davison, M.L.; Bershadsky, B.; Bieber, J.; Silversmith, D.; Maruish, M.E.; Kane, R.L. Development of a brief, multidimensional, self-report instrument for treatment outcomes assessment in psychiatric settings: Preliminary findings. Assessment 1997, 4, 259–276. [Google Scholar] [CrossRef]
- Breiman, L. Classification and regression trees; Routledge, 2017.
- Breiman, L. Random forests. Machine learning 2001, 45, 5–32. [Google Scholar] [CrossRef]
- Cortes, C. Support-Vector Networks. Machine Learning 1995. [Google Scholar] [CrossRef]
- Friedman, J.H. Stochastic gradient boosting. Computational statistics & data analysis 2002, 38, 367–378. [Google Scholar]
- Mitchell, H. Bayesian Decision Theory. In Multi-Sensor Data Fusion: An Introduction; Springer, 2007; pp. 201–219.
- McCullagh, P. Generalized linear models; Routledge, 2019.
- Rumelhart, D.E.; Hinton, G.E.; Williams, R.J. Learning representations by back-propagating errors. nature 1986, 323, 533–536. [Google Scholar] [CrossRef]
- Bergstra, J.; Bardenet, R.; Bengio, Y.; Kégl, B. Algorithms for hyper-parameter optimization. Advances in neural information processing systems 2011, 24. [Google Scholar]
- Belkin, M.; Hsu, D.; Ma, S.; Mandal, S. Reconciling modern machine-learning practice and the classical bias–variance trade-off. Proceedings of the National Academy of Sciences 2019, 116, 15849–15854. [Google Scholar] [CrossRef]
| 1 | |
| 2 | |
| 3 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).





