Submitted:
13 November 2024
Posted:
15 November 2024
You are already at the latest version
Abstract
Keywords:
What Is Known
- Chronic disease self-management (CDSM) programs have proven benefits in the management of many chronic diseases
- CDSM programs benefits in improving MACE in CHF remains unclear
- CDSM can be delivered as generic or disease specific programs, the former has been tested widely in CHF.
What Is New
- Generic CDSM programs can be used in CHF
- Generic short form tools derived from gold standard CDSM can risk stratify poor and good self-managers
- Self-managers with borderline and average abilities require greater understanding when designing randomized trials to further analyse these findings.
1. Introduction
2. Methods
2.1. Design
2.3. Participants
2.4. Sample Size Calculations
2.5. Trial Instruments and Procedures
2.5.1. CFPI Program and PIH Tools
2.5.2. Data Collection
2.5.3. Ethical Considerations
2.5.4. Statistical Aspects and Data Analysis
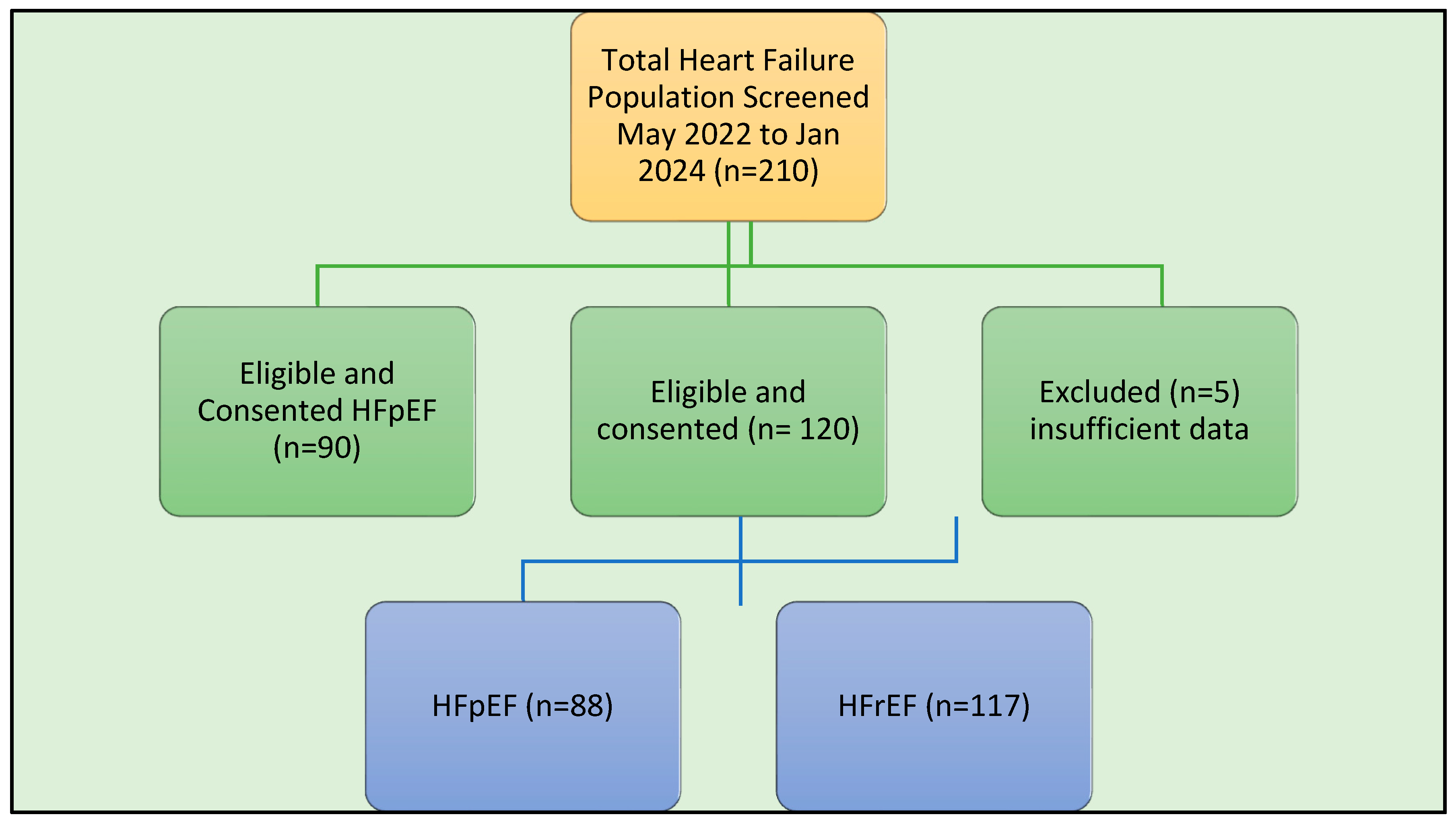
3. Results
Patient Demographic and Characteristics
Baseline Characteristics (HFrEF)
Baseline Characteristics (HFpEF)
BCFA Model
Discussion
Summary of PIH and Theoretical Framework, of Generic Self-Management, Scale
Summary of Self-Management in Heart Failure and Comparing Relevant Research
| BSEM- CFA 4-factor model |
BSEM with cross-loadings N (0, 0.005) and residual covariances IW(200*D,200 ) | |||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Item | K | P | M | C | K | P | M | C | ||||||||
| Loadings | ||||||||||||||||
| 1 | 0.916* | 0 | 0 | 0 | 0.831* | -0.019 | 0.037 | 0.013 | ||||||||
| 2 | 0.918* | 0 | 0 | 0 | 0.869* | 0.024 | -0.020 | -0.011 | ||||||||
| 3 | 0 | 0.915* | 0 | 0 | -0.040 | 0.538* | 0.065 | -0.060 | ||||||||
| 4 | 0 | 0.517* | 0 | 0 | 0.057 | 0.772* | -0.036 | 0.012 | ||||||||
| 5 | 0 | 0.551* | 0 | 0 | 0.022 | 0.854* | -0.072 | 0.012 | ||||||||
| 6 | 0 | 0.836* | 0 | 0 | -0.063 | 0.604* | 0.082 | 0.017 | ||||||||
| 7 | 0 | 0 | 0.860* | 0 | 0.024 | 0.008 | 0.906* | -0.023 | ||||||||
| 8 | 0 | 0 | 0.885* | 0 | -0.003 | 0.009 | 0.850* | 0.045 | ||||||||
| 9 | 0 | 0 | 0 | 0.761* | 0.014 | 0.024 | 0.067 | 0.622* | ||||||||
| 10 | 0 | 0 | 0 | 0.950* | -0.001 | -0.026 | -0.070 | 0.971* | ||||||||
| 11 | 0 | 0 | 0 | 0.964* | -0.003 | 0.010 | -0.019 | 0.915* | ||||||||
| 12 | 0 | 0 | 0 | 0.523* | -0.020 | 0.001 | 0.101 | 0.414* | ||||||||
| Factor correlations | ||||||||||||||||
| K | - | - | ||||||||||||||
| P | 0.275* | - | 0.641* | - | ||||||||||||
| M | 0.350* | 0.842* | - | 0.409* | 0.662* | - | ||||||||||
| C | 0.540* | 0.358* | 0.609* | - | 0.576* | 0.641* | 0.597* | - | ||||||||
Current Findings and Future Research
Limitations
5. Conclusions
6. Patents
Author Contributions
Funding
Informed Consent Statement
Acknowledgments
Conflicts of Interest
References
- Ramachandran, J.; Smith, D.; Woodman Muller, K.; Wundke, R.; McCormick, R.; et al. Psychometric validation of the Partners in Health scale as a self-management tool in patients with liver cirrhosis. Internal Medicine Journal. 2021, 51, 2104–2110. [Google Scholar] [CrossRef] [PubMed]
- Roger, V.L. Epidemiology of heart failure: a contemporary perspective. Circ Res. 2021, 128, 1421–1434. [Google Scholar] [CrossRef] [PubMed]
- Heidenreich, P.A.; Bozkurt, B.; Aguilar, D.; et al. 2022 AHA/ACC/HFSA Guideline for the Management of Heart Failure: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. J Am Coll Cardiol. 2022, 79, e263–e421. [Google Scholar] [PubMed]
- McDonagh, T.A.; Metra, M.; Adamo, M.; et al. ESC Scientific Document Group, 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: Developed by the Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC) With the special contribution of the Heart Failure Association (HFA) of the ESC. EHJ. 2021, 42, 3599–3726. [Google Scholar]
- Heidenreich, P.A.; Fonarow, G.C.; Breathett, K.; et al. 2020 ACC/AHA Clinical Performance and Quality Measures for Adults With Heart Failure: A Report of the American College of Cardiology/American Heart Association Task Force on Performance Measures. J Am Coll Cardiol. 2020, 76, 2527–2564. [Google Scholar] [CrossRef]
- Wagner, E.H. Chronic disease management: what will it take to improve care for chronic illness? Eff Clin Pract. 1998, 1, 2–4. [Google Scholar]
- Cameron, J.; Worrall-Carter, L.; Driscoll, A.; Stewart, S. Measuring self-care in chronic heart failure: a review of the psychometric properties of clinical instruments. J Cardiovasc Nurs. 2009, 24, E10–E22. [Google Scholar] [CrossRef] [PubMed]
- Riegel, B.; Driscoll, A.; Suwanno, J.; Moser, D.K.; Lennie, T.A.; Chung, M.L.; et al. Heart Failure Self-Care in Developed and Developing Countries. Journal of Cardiac Failure. 2009, 15, 508–516. [Google Scholar] [CrossRef]
- Riegel, B.; Lee, C.; Dickson, V. Self care in patients with chronic heart failure. Nat Rev Cardiol. 2011, 8, 644–654. [Google Scholar] [CrossRef]
- Lainscak, M.; Blue, L.; Clark, A.; et al. Self-care management of heart failure: practical recommendations from the Patient Care Committee of the Heart Failure Association of the European Society of Cardiology. European Journal of Heart Failure. 2011, 13, 115–12. [Google Scholar] [CrossRef]
- Riegel, B.; Moser, D.K.; Buck, H.G.; et al. Self-Care for the Prevention and Management of Cardiovascular Disease and Stroke: A Scientific Statement for Healthcare Professionals From the American Heart Association. J Am Heart Assoc. 2017, 6, e006997. [Google Scholar] [CrossRef] [PubMed]
- Jaarsma, T.; Hill, H.; Bayes-Genis, A.; et al. Self-care of heart failure patients: practical management recommendations from the Heart Failure Association of the European Society of Cardiology. Eur J Heart Fail. 2021, 23, 157–174. [Google Scholar] [CrossRef] [PubMed]
- https://www.flindersprogram.com.
- Battersby, M.; Ask, A.; Reece, M.; Markwick, M.; Collins, J. The partners in health scale: the development and psychometric properties of a generic assessment scale for chronic condition self-management? Australian Journal of Primary Health. 2003, 9, 41–52. [Google Scholar] [CrossRef]
- Harvey, P.W.; Petkov, J.; Misan, G.; Warren, K.; Fuller, J.; Battersby, M.; et al. Self-management support and training for patients with chronic and complex conditions improves health related behaviour and health outcomes. Australian Health Review. 2008, 32, 330–338. [Google Scholar] [CrossRef]
- Iyngkaran, P.; Toukhsati, S.R.; Harris, M.; Connors, C.; Kangaharan, N.; Ilton, M.; et al. Self Managing Heart Failure in Remote Australia - Translating Concepts into Clinical Practice. Curr Cardiol Rev. 2016, 12, 270–284. [Google Scholar] [CrossRef] [PubMed]
- Grady, P.A.; Gough, L.L. Self-management: a comprehensive approach to management of chronic conditions. Am J Public Health. 2014, 104, e25–e31. [Google Scholar] [CrossRef]
- Schrijver, J.; Lenferink, A.; Brusse-Keizer, M.; Zwerink, M.; van der Valk, P.D.L.P.M.; van der Palen, J.; et al. Self-management interventions for people with chronic obstructive pulmonary disease. Cochrane Database of Systematic Reviews 2022, CD002990. [Google Scholar] [CrossRef]
- Portz, J.D. A review of web-based chronic disease self-management for older adults. Gerontechnology. 2017, 16, 12–20. [Google Scholar] [CrossRef]
- Reynolds, R.; Dennis, S.; Hasan, I.; et al. A systematic review of chronic disease management interventions in primary care. BMC Fam Pract. 2018, 19, 11. [Google Scholar] [CrossRef]
- Allegrante, J.P.; Wells, M.T.; Peterson, J.C. Interventions to Support Behavioral Self-Management of Chronic Diseases. Annual Review of Public Health. 2019, 40, 127–146. [Google Scholar] [CrossRef]
- Kim, S.; Park, M.; Song, R. Effects of self-management programs on behavioral modification among individuals with chronic disease: A systematic review and meta-analysis of randomized trials. PLoS ONE. 2021, 16, e0254995. [Google Scholar] [CrossRef] [PubMed]
- O’Connell, S.; Mc Carthy, V.J.C.; Savage, E. Frameworks for self-management support for chronic disease: a cross-country comparative document analysis. BMC Health Serv Res. 2018, 18, 583. [Google Scholar] [CrossRef] [PubMed]
- Iyngkaran, P.; Hanna, F.; Andrew, S.; Horowitz, J.D.; Battersby, M.; De Courten, M.P. Comparison of short and long forms of the Flinders program of chronic disease SELF-management for participants starting SGLT-2 inhibitors for congestive heart failure (SELFMAN-HF): protocol for a prospective, observational study. Front Med (Lausanne). 2023, 10, 1059735. [Google Scholar] [CrossRef] [PubMed]
- Battersby, M.; Korff, M.V.; Schaefer, J.; et al. Twelve evidence-based principles for implementing self-management support in primary care. Jt Comm J Qual Patient Saf 2010, 36, 561–570. [Google Scholar] [CrossRef]
- Petkov, J.; Harvey, P.; Battersby, M. The internal consistency and construct validity of the Partners in Health Scale:validation of a patient rated chronic condition self-management measure. Qual Life Res 2010, 19, 1079–1085. [Google Scholar] [CrossRef]
- Lenferink, A.; Effing, T.; Harvey, P.; et al. Construct validity of the Dutch version of the 12-item Partners in Health Scale: measuring patient self-management behaviour and knowledge in patients with chronic obstructive pulmonary disease. PLoS One. 2016, 11, e161595. [Google Scholar] [CrossRef]
- Battersby, M.; Harris, M.; Smith, D.; Reed, R.; Woodman, R. A pragmatic randomized controlled trial of the Flinders Program of chronic condition management in community health care services. Patient. Educ Couns 2015, 98, 1367–1375. [Google Scholar] [CrossRef] [PubMed]
- Smith, D.; Harvey, P.; Lawn, S.; Harris, M.; Battersby, M. Measuring chronic condition self-management in an Australian community: factor structure of the revised Partners in Health (PIH) scale. Qual Life Res 2017, 26, 149–159. [Google Scholar] [CrossRef]
- Hudon, M.; Chouinard, M.C.; Krieg, C.; et al. The French adaptation and validation of the Partners in Health(PIH)Scale among patients with chronic conditions seen in primary care. PLoS One. 2019, 14, e0224191. [Google Scholar] [CrossRef] [PubMed]
- Jeon, M.K.; Ahn, J.W.; Park, Y.H.; et al. Validity and reliability of the Korean version of the Partners in Health Scale(PIH-K). J Korean Crit Care Nurs 2019, 12, 1–12. [Google Scholar] [CrossRef]
- Muthén, B.; Asparouhov, T. Bayesian structural equation modeling: a more flexible representation of substantive theory. Psychol Methods. 2012, 17, 313–335. [Google Scholar] [CrossRef] [PubMed]
- Asparouhov, T.; Muthén, B.; Morin, A.J.S. Bayesian structural equation modeling with cross-loadings and residual covariances: Comments on Stromeyer et al. Journal of Management. 2015, 41, 1561–1577. [Google Scholar] [CrossRef]
- Depaoli, S. (2021). Bayesian structural equation modeling. Guilford Publications.
- Zhang, Z.; Hamagami, F.; Lijuan Wang, L.; Nesselroade, J.R.; Grimm, K.J. Bayesian analysis of longitudinal data using growth curve models. International Journal of Behavioral Development. 2007, 31, 374–383. [Google Scholar] [CrossRef]
- Depaoli, S.; Rus, H.M.; Clifton, J.P.; van de Schoot, R.; Tiemensma, J. An introduction to Bayesian statistics in health psychology. Health Psychology Review. 2017, 11, 248–264. [Google Scholar] [CrossRef] [PubMed]
- Gelman, A.; Rubin, D.B. Inference from Iterative Simulation Using Multiple Sequences. Statistical Science. 1992, 7, 457–472. [Google Scholar] [CrossRef]
- Asparouhov, T.; Muthén, B. Advances in Bayesian model fit evaluation for structural equation models. Structural Equation Modeling: A Multidisciplinary Journal. 2021, 28, 1–14. [Google Scholar] [CrossRef]
- Hu, L.t.; Bentler, P.M. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Structural Equation Modeling: A Multidisciplinary Journal. 1999, 6, 1–55. [Google Scholar] [CrossRef]
- Spiegelhalter, D.J.; Best, N.G.; Carlin, B.P.; Van Der Linde, A. Bayesian measures of model complexity and fit. Journal of the Royal Statistical Society Series B. 2002, 64, 583–639. [Google Scholar] [CrossRef]
- McNeish, D. Thanks coefficient alpha, we'll take it from here. Psychol Methods. 2018, 23, 412–433. [Google Scholar] [CrossRef]
- Muthén, L.; Muthén, B. (1998-2017). Mplus Users Guide. Eighth Edition. Los Angeles, CA: Muthén, & Muthén.
- Kim, Y.J.; Soeken, K.L. A meta-analysis of the effect of hospital-based case management on hospital length-of-stay and readmission. Nurs Res. 2005, 54, 255–264. [Google Scholar] [CrossRef]
- McDonald, K. Disease management programs for heart failure. Curr Treat Options Cardiovasc Med. 2010, 12, 578–586. [Google Scholar] [CrossRef] [PubMed]
- Savard, L.A.; Thompson, D.R.; Clark, A.M. A meta-review of evidence on heart failure disease management programs: the challenges of describing and synthesizing evidence on complex interventions. Trials. 2011, 12, 194. [Google Scholar] [CrossRef] [PubMed]
- Whellan, D.J.; Hasselblad, V.; Peterson, E.; O’Connor, C.M.; Schulman, K.A. Metaanalysis and review of heart failure disease management randomized controlled clinical trials. Am Heart J. 2005, 149, 722–729. [Google Scholar] [CrossRef]
- Jovicic, A.; Holroyd-Leduc, J.M.; Straus, S.E. Effects of self-management intervention on health outcomes of patients with heart failure: a systematic review of randomized controlled trials. BMC Cardiovasc Disord. 2006, 6, 43. [Google Scholar] [CrossRef] [PubMed]
- Koshman, S.L.; Charrois, T.L.; Simpson, S.H.; McAlister, F.A.; Tsuyuki, R.T. Pharmacist care of patients with heart failure: a systematic review of randomized trials. Arch Intern Med. 2008, 168, 687–694. [Google Scholar] [CrossRef] [PubMed]
- Gohler, A.; Januzzi, J.L.; Worrell, S.S.; Osterziel, K.J.; Gazelle, G.S.; Dietz, R.; et al. A systematic meta-analysis of the efficacy and heterogeneity of disease management programs in congestive heart failure. J Card Fail. 2006, 12, 554–567. [Google Scholar] [CrossRef]
- Konstam, M.A.; Konstam, V. Heart failure disease management a sustainable energy source for the health care engine. J Am Coll Cardiol. 2010, 56, 379–381. [Google Scholar] [CrossRef] [PubMed]
- Ferrante, D.; Varini, S.; Macchia, A.; Soifer, S.; Badra, R.; Nul, D.; et al. Long-term results after a telephone intervention in chronic heart failure: DIAL (Randomized Trial of Phone Intervention in Chronic Heart Failure) follow-up. J Am Coll Cardiol. 2010, 56, 372–378. [Google Scholar] [CrossRef] [PubMed]
- Wu, J.R.; Moser, D.K.; Chung, M.L.; Lennie, T.A. Objectively measured, but not self-reported, medication adherence independently predicts event-free survival in patients with heart failure. J Card Fail. 2008, 14, 203–210. [Google Scholar] [CrossRef]
- Wu, J.R.; Moser, D.K.; De Jong, M.J.; Rayens, M.K.; Chung, M.L.; Riegel, B.; Lennie, T.A. Defining an evidence-based cutpoint for medication adherence in heart failure. Am Heart J. 2009, 157, 285–291. [Google Scholar] [CrossRef]
- Wu, J.R.; Corley, D.J.; Lennie, T.A.; Moser, D.K. Effect of a medication-taking behavior feedback theory-based intervention on outcomes in patients with heart failure. J Card Fail. 2012, 18, 1–9. [Google Scholar] [CrossRef] [PubMed]
- vanderWal, M.H.; vanVeldhuisen, D.J.; Veeger, N.J.; Rutten, F.H.; Jaarsma, T. Compliance with non-pharmacological recommendations and outcome in heart failure patients. Eur Heart J. 2010, 31, 1486–1493. [Google Scholar] [CrossRef] [PubMed]
- Lee, C.S.; Moser, D.K.; Lennie, T.A.; Riegel, B. Event-free survival in adults with heart failure who engage in self-care management. Heart Lung. 2011, 40, 12–20. [Google Scholar] [CrossRef] [PubMed]
- Buck, H.G.; Lee, C.S.; Moser, D.K.; Albert, N.M.; Lennie, T.; Bentley, B.; et al. Relationship between self-care and health-related quality of life in older adults with moderate to advanced heart failure. J Cardiovasc Nurs. 2012, 27, 8–15. [Google Scholar] [CrossRef] [PubMed]
- Wang, S.P.; Lin, L.C.; Lee, C.M.; Wu, S.C. Effectiveness of a self-care program in improving symptom distress and quality of life in congestive heart failure patients: a preliminary study. J Nurs Res. 2011, 19, 257–266. [Google Scholar] [CrossRef]
- Seto, E.; Leonard, K.J.; Cafazzo, J.A.; Masino, C.; Barnsley, J.; Ross, H.J. Self-care and quality of life of heart failure patients at a multidisciplinary heart function clinic. J Cardiovasc Nurs. 2011, 26, 377–385. [Google Scholar] [CrossRef]
- Feng, C.; Wang, Y.; Li, S.; Qu, Z.; Zheng, S. Effect of self-management intervention on prognosis of patients with chronic heart failure: A meta-analysis. Nurs Open. 2023, 10, 2015–2029. [Google Scholar] [CrossRef]
- Yu, D.S.; Thompson, D.R.; Lee, D.T. Disease management programmes for older people with heart failure: crucial characteristics which improve post-discharge outcomes. Eur Heart J. 2006, 27, 596–612. [Google Scholar] [CrossRef]
| Variable |
HFrEF n = 117 |
% |
HFpEF n = 88 |
% |
| Age (yo) | 66.8 mean | SD 13.5 | 71.3 | SD 9.76 |
| Sex, (men) | 88 | 75 | 46 | 52 |
| Ethnicity Caucasian South Asian Asian African Aboriginal/ Pacific Is |
90 7 3 10 7 |
77 6 3 8 6 |
71 6 4 6 1 |
81 7 4 7 1 |
| Social Married Spouse support High School |
75 71 63 |
85 82 71 |
NA | NA |
| Smoking history No Ex/ Yes |
53 64 |
45 55 |
59 29 |
67 33 |
| Comorbidities CRF (eGFR ml/m) >60 30-60 15-30 <15 CAD DM HT Chol OSA |
69 39 7 2 51 42 79 73 31 |
59.0 33.3 6.0 1.7 44.0 36.0 68.0 62.4 26.5 |
65 17 6 0 30 29 76 67 21 |
74 19.3 6.7 0 41 33 87 76 24 |
| Years with HF diagnosis Less than 1 year 1-4 years 5-10 years |
83 21 13 |
71 18.0 11.0 |
81 7 |
92 8 |
| LVEF Grade 1 (>50%) Grade 2 (40-49) Grade 3 (30-39) Grade 4 (20-29) Grade 5 <20) |
0 1 84 29 4 |
0 0.8 71.2 25 3 |
88 0 0 0 0 |
100 0 0 0 0 |
| NYHA classification at discharge I II III IV |
0 73 41 3 |
0 62.4 35.0 2.6 |
0 68 20 0 |
0 77 23 0 |
| Difference between observed and replicated χ [2] 95% CI CI |
||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| PIH model | PPP p | PP p | Lower 2.5% |
Upper 2.5% |
# Par. | pD | DIC | RMSEA (90% CI) | CFI (90% CI) | TLI (90% CI) |
| CFA | <0.001 | 128.5 | 213.3 | 42 | 47.1 | 2987 | 0.189 (0.178-0.206) | 0.836 (0.804-0.855) | 0.748 (0.699-0.777) | |
| BCFA with cross loadings | ||||||||||
| xload N(0, 0.001) | <0.001 | <0.001 | 80 | 151.3 | 78 | 46.5 | 5605 | 0.117 (0.107-0.127) | 0.913 (0.897-0.928) | 0.869 (0.843-0.890) |
| xload N(0, 0.005) | 0.007 | <0.001 | 44.5 | 119.7 | 78 | 52.9 | 5577 | 0.107 (0.092-0.121) | 0.938 (0.920-0.954) | 0.890 (0.858-0.918) |
| xload N(0, 0.01) | 0.121 | <0.001 | 31.4 | 106 | 78 | 56 | 5568 | 0.103 (0.087-0.118) | 0.948 (0.930-0.963) | 0.898 (0.864-0.927) |
| xload N(0, 0.015) | 0.304 | <0.001 | 28 | 101.3 | 78 | 57 | 5565 | 0.101 (0.085-0.117) | 0.951 (0.934-0.965) | 0.901 (0.867-0.930) |
| xload N(0, 0.02) | 0.451 | <0.001 | 26.7 | 99.9 | 78 | 58 | 5563 | 0.100 (0.084-0.116) | 0.952 (0.936-0.966) | 0.903 (0.869-0.932) |
| xload N(0, 0.03) | 0.654 | <0.001 | 26.1 | 97.8 | 78 | 56 | 5560 | 0.097 (0.081-0.114) | 0.953 (0.937-0.967) | 0.908 (0.876-0.936) |
| BCFA with cross loadings and residual covariances | ||||||||||
| xload N(0, 0.005) res corr (d=50) | 0.858 | 0.493 | -37.7 | 37.6 | 144 | 73 | 5515 | 0.023 (0.000-0.088) | 0.999 (0.981-1.0) | 0.995 (0.925-1.0) |
| xload N(0, 0.005) res corr (d=100) | 0.776 | 0.330 | -29.3 | 46.4 | 144 | 67 | 5517 | 0.047 (0.000-0.087) | 0.993 (0.974-1.0) | 0.979 (0.927-1.0) |
| xload N(0, 0.005) res corr (d=200) | 0.545 | 0.144 | -17.4 | 59.4 | 144 | 60 | 5522 | 0.061 (0.014-0.089) | 0.984 (0.965-0.999) | 0.965 (0.924-0.998) |
| xload N(0, 0.005) res corr (d=300) | 0.382 | 0.072 | -10.1 | 67.3 | 144 | 56 | 5527 | 0.067 (0.037-0.090) | 0.978 (0.960-0.993) | 0.957 (0.923-0.987) |
| xload N(0, 0.005) res corr (d=400) | 0.283 | 0.038 | -3.2 | 73.2 | 144 | 54 | 5531 | 0.071 (0.045-0.092) | 0.973 (0.955-0.989) | 0.951 (0.918-0.980) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




