Submitted:
06 November 2024
Posted:
06 November 2024
You are already at the latest version
Abstract
Purpose: This study evaluates the impact of Medicaid expansion under the Affordable Care Act (ACA) on melanoma staging at diagnosis, treatment utilization, and 3-year mortality outcomes. The objective is to determine whether Medicaid expansion led to earlier melanoma diagnosis and improved survival rates among non-elderly adults (ages 40-64) by analyzing data from the National Cancer Database (NCDB). Methods: A total of 12,667 patients, aged 40-64, diagnosed with melanoma from 2010 to 2020 were identified using the NCDB. Difference-in-difference (DID) analysis was performed to analyze tumor staging at presentation between Medicaid expansion states and non-Medicaid expansion states both prior to the expansion and after the expansion. Results: Of the total patients 2,307 were from the pre-expansion time period residing in Medicaid Expansion states (MES) and 1,804 in non-Medicaid expansion states. In the post-expansion time period there were 5,571 residing in the MES and 2,985 in the non-MES. DID analysis revealed a decrease in stage IV melanoma at diagnosis (DID -0.222, p <0.001) between MES and non-MES before and after Medicaid expansion. After expansion, in stage IV, the occurrence of primary surgery was 0.42 in non-MES and 0.44 (difference 0.02), DID analysis was not statistically significant. The use of immunotherapy in MES was significantly higher than non-MES after expansion (p<0.001), although DID analysis did not reveal a statistically significant difference. DID analysis showed a statistically significant decrease in 3-year mortality (DID -0.05, p=0.001) between MES and non-MES before and after Medicaid expansion. Conclusions: This study revealed the positive impact of the ACA’s Medicaid expansion on melanoma stage at presentation showing improved access to healthcare services can facilitate the diagnosis of early-stage melanoma and decrease mortality rate.
Keywords:
1. Introduction
2. Materials and Methods
3. Results
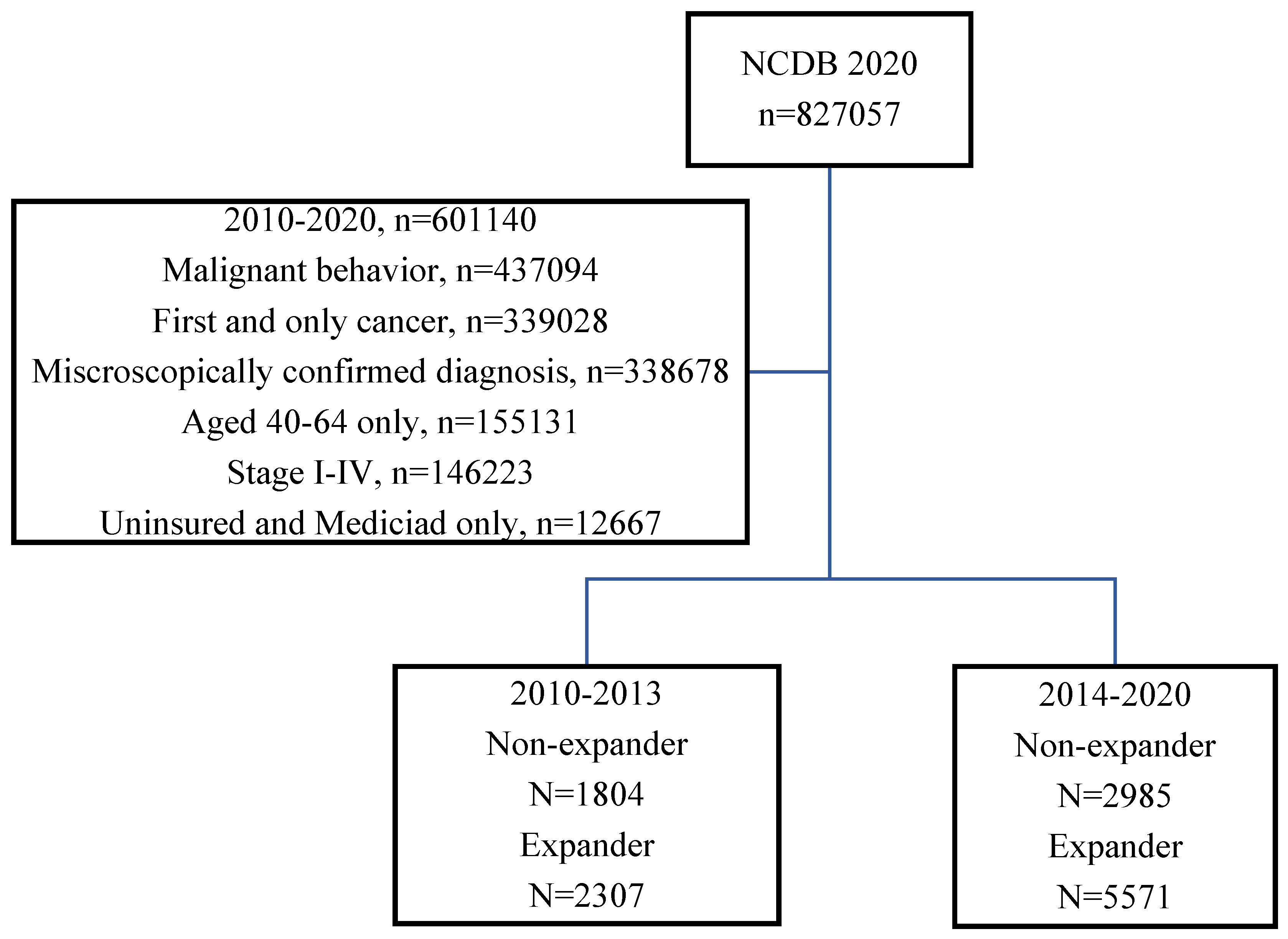
3.1. Study Population
3.2. Change in Insurance Coverage Over Time
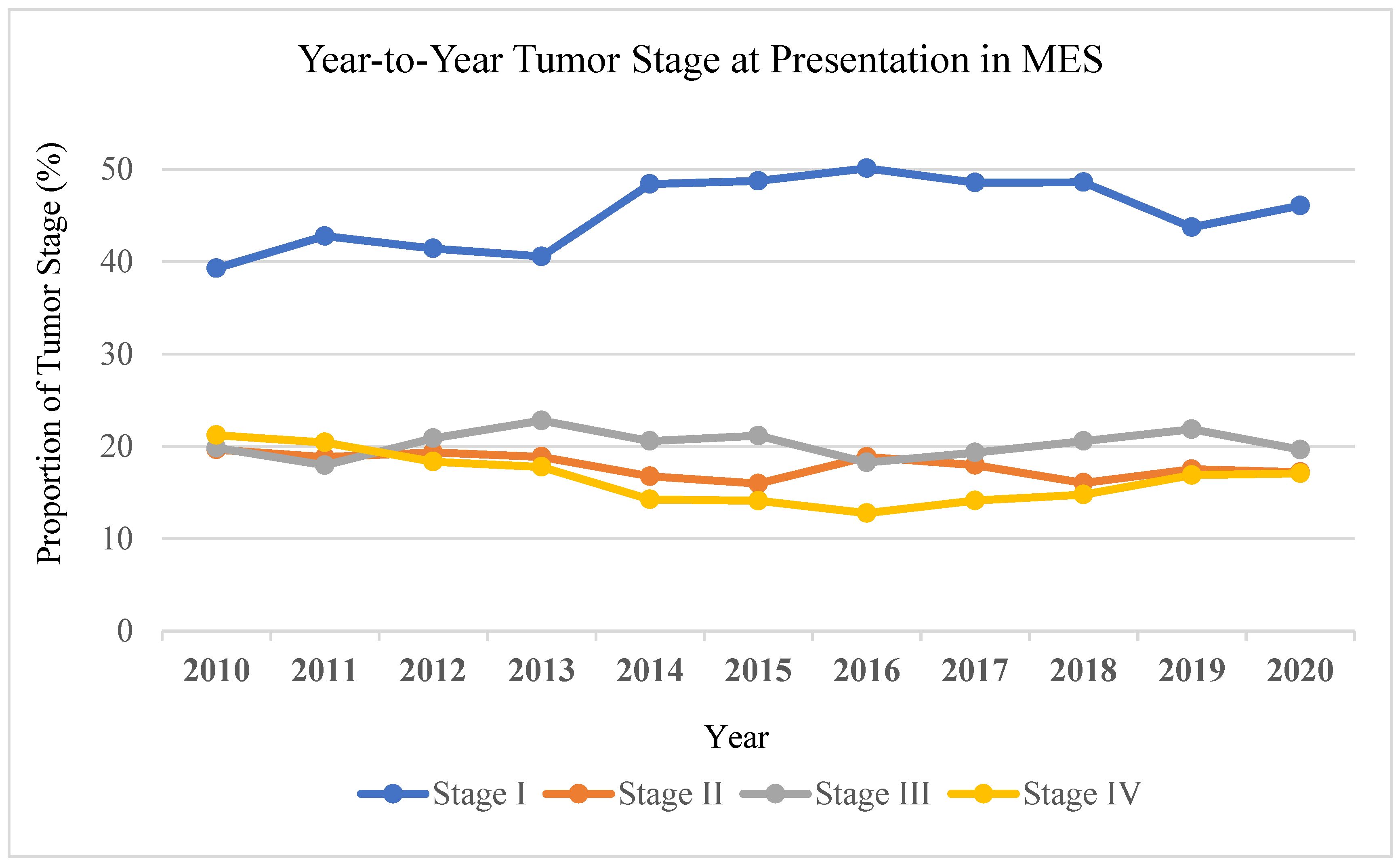
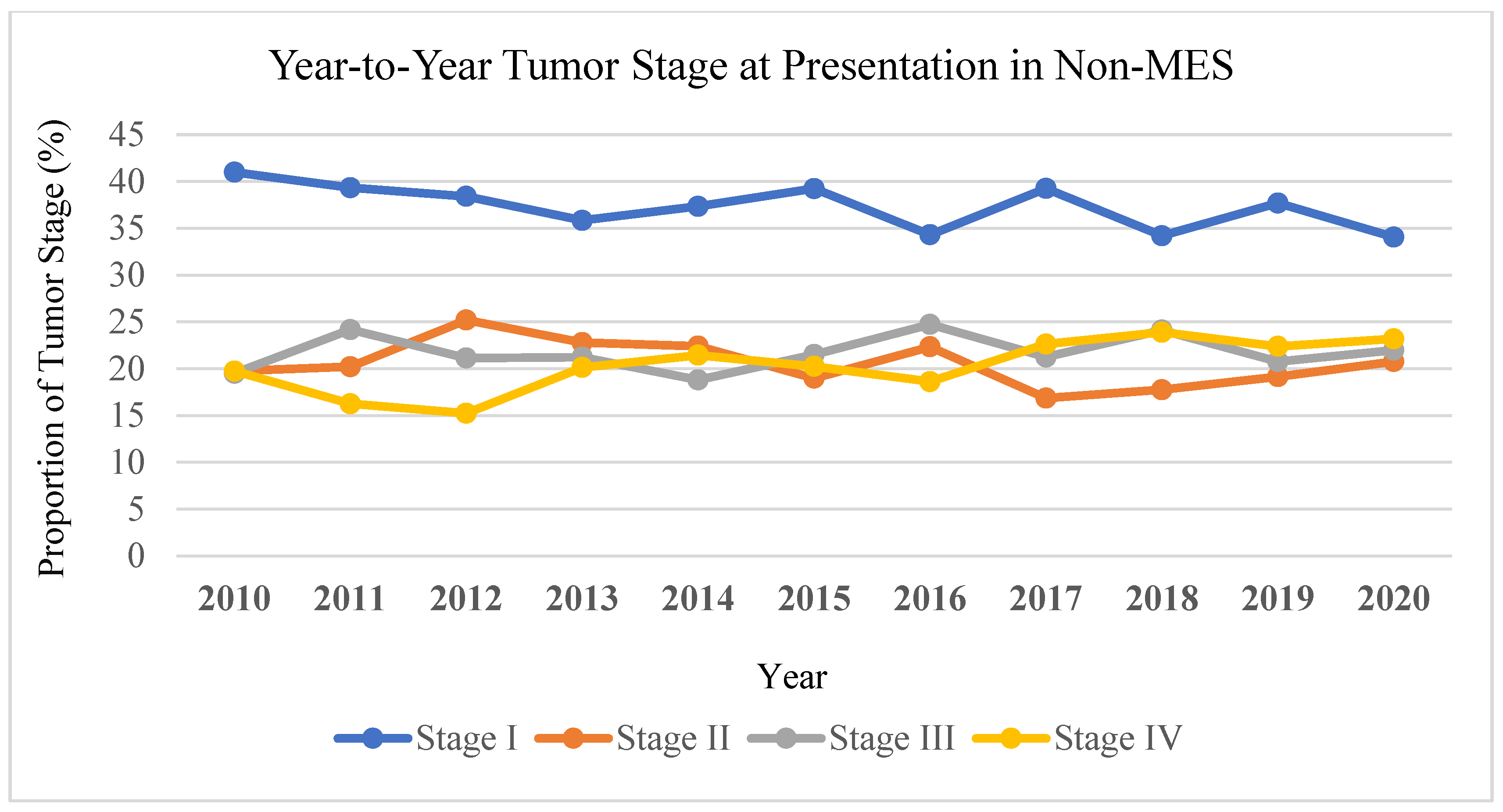
3.3. Trend Analysis
3.4. DID Analysis
3.4.1. Tumor Stage
3.4.2. Definitive Surgery
3.4.3. Use of Systemic Immunotherapy
3.4.4. 3-Year Mortality
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Kim, U.; Koroukian, S.; Statler, A.; Rose, J. The Effect of Medicaid Expansion among Adults from Low-income Communities on Stage at Diagnosis in Those with Screening-amenable Cancers. Cancer 2020, 126, 4209–4219. [CrossRef]
- Fedewa, S.A.; Yabroff, K.R.; Smith, R.A.; Goding Sauer, A.; Han, X.; Jemal, A. Changes in Breast and Colorectal Cancer Screening After Medicaid Expansion Under the Affordable Care Act. Am. J. Prev. Med. 2019, 57, 3–12. [CrossRef]
- Lee, G.; Dee, E.C.; Orav, E.J.; Kim, D.W.; Nguyen, P.L.; Wright, A.A.; Lam, M.B. Association of Medicaid Expansion and Insurance Status, Cancer Stage, Treatment and Mortality among Patients with Cervical Cancer. Cancer Rep. 2021, 4, e1407. [CrossRef]
- Hendryx, M.; Luo, J. Increased Cancer Screening for Low-Income Adults Under the Affordable Care Act Medicaid Expansion. Med. Care 2018, 56, 944–949. [CrossRef]
- Zhao, J.; Mao, Z.; Fedewa, S.A.; Nogueira, L.; Yabroff, K.R.; Jemal, A.; Han, X. The Affordable Care Act and Access to Care across the Cancer Control Continuum: A Review at 10 Years. CA. Cancer J. Clin. 2020, 70, 165–181. [CrossRef]
- Snyder, R.A.; Hu, C.; DiBrito, S.R.; Chang, G.J. Association of Medicaid Expansion with Racial Disparities in Cancer Stage at Presentation. Cancer 2022, 128, 3340–3351. [CrossRef]
- Osazuwa-Peters, N.; Barnes, J.M.; Megwalu, U.; Adjei Boakye, E.; Johnston, K.J.; Gaubatz, M.E.; Johnson, K.J.; Panth, N.; Sethi, R.K.V.; Varvares, M.A. State Medicaid Expansion Status, Insurance Coverage and Stage at Diagnosis in Head and Neck Cancer Patients. Oral Oncol. 2020, 110, 104870. [CrossRef]
- Hoehn, R.S.; Rieser, C.J.; Phelos, H.; Sabik, L.M.; Nassour, I.; Paniccia, A.; Zureikat, A.H.; Tohme, S.T. Association Between Medicaid Expansion and Diagnosis and Management of Colon Cancer. J. Am. Coll. Surg. 2021, 232, 146-156e1. [CrossRef]
- Saginala, K.; Barsouk, A.; Aluru, J.S.; Rawla, P.; Barsouk, A. Epidemiology of Melanoma. Med. Sci. 2021, 9, 63. [CrossRef]
- Siegel, R.L.; Miller, K.D.; Jemal, A. Cancer Statistics, 2019. CA. Cancer J. Clin. 2019, 69, 7–34. [CrossRef]
- NCCN Clinical Practice Guidelines in Oncology. 2024.
- Breitbart, E.W.; Waldmann, A.; Nolte, S.; Capellaro, M.; Greinert, R.; Volkmer, B.; Katalinic, A. Systematic Skin Cancer Screening in Northern Germany. J. Am. Acad. Dermatol. 2012, 66, 201–211. [CrossRef]
- Brunssen, A.; Waldmann, A.; Eisemann, N.; Katalinic, A. Impact of Skin Cancer Screening and Secondary Prevention Campaigns on Skin Cancer Incidence and Mortality: A Systematic Review. J. Am. Acad. Dermatol. 2017, 76, 129-139.e10. [CrossRef]
- Kovalyshyn, I. The Impact of Physician Screening on Melanoma Detection. Arch. Dermatol. 2011, 147, 1269. [CrossRef]
- Swetter, S.M.; Pollitt, R.A.; Johnson, T.M.; Brooks, D.R.; Geller, A.C. Behavioral Determinants of Successful Early Melanoma Detection: Role of Self and Physician Skin Examination. Cancer 2012, 118, 3725–3734. [CrossRef]
- Ercia, A. The Impact of the Affordable Care Act on Patient Coverage and Access to Care: Perspectives from FQHC Administrators in Arizona, California and Texas. BMC Health Serv. Res. 2021, 21, 920. [CrossRef]
- Marchetti, M.A.; Adamson, A.S.; Halpern, A.C. Melanoma and Racial Health Disparities in Black Individuals—Facts, Fallacies, and Fixes. JAMA Dermatol. 2021, 157, 1031. [CrossRef]
- Weinstock, M.A. Early Detection of Melanoma. JAMA 2000, 284, 886. [CrossRef]
- Gershenwald, J.E.; Scolyer, R.A.; Hess, K.R.; Sondak, V.K.; Long, G.V.; Ross, M.I.; Lazar, A.J.; Faries, M.B.; Kirkwood, J.M.; McArthur, G.A.; et al. Melanoma Staging: Evidence-based Changes in the American Joint Committee on Cancer Eighth Edition Cancer Staging Manual. CA. Cancer J. Clin. 2017, 67, 472–492. [CrossRef]
- Buccafusca, G.; Proserpio, I.; Tralongo, A.C.; Rametta Giuliano, S.; Tralongo, P. Early Colorectal Cancer: Diagnosis, Treatment and Survivorship Care. Crit. Rev. Oncol. Hematol. 2019, 136, 20–30. [CrossRef]
- Crosby, D.; Bhatia, S.; Brindle, K.M.; Coussens, L.M.; Dive, C.; Emberton, M.; Esener, S.; Fitzgerald, R.C.; Gambhir, S.S.; Kuhn, P.; et al. Early Detection of Cancer. Science 2022, 375, eaay9040. [CrossRef]
- Henrikson, N.B.; Ivlev, I.; Blasi, P.R.; Nguyen, M.B.; Senger, C.A.; Perdue, L.A.; Lin, J.S. Skin Cancer Screening: Updated Evidence Report and Systematic Review for the US Preventive Services Task Force. JAMA 2023, 329, 1296. [CrossRef]
- Zheng, D.X.; Cwalina, T.B.; Mulligan, K.M.; Levoska, M.A.; Scott, J.F.; Mostaghimi, A. Prevalence and Predictors of Transportation Barriers to Health Care among US Adults with a History of Skin Cancer. J. Am. Acad. Dermatol. 2023, 88, 201–203. [CrossRef]
- Cortez, J.L.; Vasquez, J.; Wei, M.L. The Impact of Demographics, Socioeconomics, and Health Care Access on Melanoma Outcomes. J. Am. Acad. Dermatol. 2021, 84, 1677–1683. [CrossRef]
- Obama, B. United States Health Care Reform: Progress to Date and Next Steps. JAMA 2016, 316, 525. [CrossRef]
- Levine, D.M.; Chalasani, R.; Linder, J.A.; Landon, B.E. Association of the Patient Protection and Affordable Care Act With Ambulatory Quality, Patient Experience, Utilization, and Cost, 2014-2016. JAMA Netw. Open 2022, 5, e2218167. [CrossRef]
| Characteristic | Pre-Expansion (2010 - 2013) N = 4111 |
Post-Expansion (2014 - 2020) N = 5571 |
|||||
| Non-MES N = 1804 |
MES N = 2307 |
P Value | Non-MES N = 2985 |
MES N = 5571 |
P Value | ||
| Age at diagnosis (years) – no. (%) | p=0.09 | p=0.004 | |||||
| 40 - 49 (0-29 censored) 50 - 64 |
654 (36) 1,150 (64) |
777 (34) 1,530 (66) |
959 (32) 2,026 (68) |
1,622 (29) 3,949 (71) |
|||
| Sex – no. (%) | p=0.80 | p=0.009 | |||||
| Male Female |
1,039 (58) 765 (42) |
1,338 (58) 969 (42) |
1,696 (57) 1,289 (43) |
3,002 (54) 2,569 (46) |
|||
| Race – no. (%) | p=0.29 | p=1.02 | |||||
| White Others |
1,739 (96) 65 (4) |
2,209 (96) 98 (4) |
2,858 (95.7) 127 (4.3) |
5,290 (95) 281 (5) |
|||
| Insurance – no. (%) | p<0.001 | p<0.001 | |||||
| Uninsured Medicaid |
1,227 (68) 577 (32) |
1,132 (49) 1,175 (51) |
1,804 (60) 1,181 (40) |
991 (18) 4,580 (82) |
|||
| Charleson-Deyo comorbidity index – no. (%) | p=0.01 | p=0.1 | |||||
| 0 1 2 3+ |
1,468 (82) 257 (14) 55 (3) 24 (1) |
1,960 (85) 258 (11) 56 (3) 33 (1) |
2,442 (82) 373 (13) 103 (3) 67 (2) |
4,647 (83) 664 (12) 145 (3) 115 (2) |
|||
| Median household income – no. (%) | p<0.001 | p<0.001 | |||||
| <$40,227 $40,227 - $50,353 $50,354 - $63,332 >$63,332 N/A |
452 (25) 523 (29) 338 (19) 248 (14) 243 (13) |
300 (13) 435 (19) 532 (23) 693 (30) 347 (15) |
748 (26) 762 (28) 594 (21) 468 (12) 412 (13) |
874 (16) 1,241 (22) 1,441 (26) 1,074 (19) 941 (17) |
|||
| Education % without high school – no. (%) | p<0.001 | p<0.001 | |||||
| 17.6% or more 10.9% - 17.5% 6.3% - 10.8% <6.3% N/A |
453 (25) 545 (30) 372 (21) 52 (11) 36 (13) |
375 (16) 532 (23) 590 (26) 467 (20) 343 (15) |
760 (26) 845 (28) 615 (21) 363 (12) 402 (13) |
874 (16) 1,241 (22) 1,441 (26) 1,074 (19) 941 (17) |
|||
| Population density – no. (%) | p<0.001 | p<0.001 | |||||
| Metro Urban Rural N/A |
1,358 (75) 358 (20) 52 (3) 36 (2) |
1,885 (82) 334 (14) 47 (2) 41 (2) |
2,258 (76) 586 (20) 79 (2) 62 (2) |
4,404 (79) 998 (18) 90 (2) 79 (1) |
|||
| Facility type – no. (%) | p<0.001 | p<0.001 | |||||
| Community Comprehensive Academic/research Integrated network |
102 (5) 553 (31) 828 (46) 321 (18) |
167 (7) 540 (23) 1,213 (53) 387 (17) |
131 (4) 1,000 (33) 1,362 (46) 492 (17) |
424 (7) 1,374 (25) 2,897 (52) 876 (16) |
|||
| Tumor stage – no. (%) | p=0.049 | p<0.001 | |||||
| 1 2 3 4 |
696 (38) 399 (22) 389 (22) 320 (18) |
947 (41) 442 (19) 472 (21) 446 (19) |
1,093 (36) 587 (20) 652 (22) 653 (22) |
2,661 (48) 968 (17) 1,125 (20) 827 (15) |
|||
| Models | 2010-2013 | 2014-2020 | DID (p) | ||||
| Non-MES | MES | Difference (p) | Non-MES | MES | Difference (p) | ||
| Tumor stage | |||||||
| Unadjusted | 2.19 | 2.18 | -0.004 (0.92) | 2.29 | 2.02 | -0.27 (<.001) | -0.27 (<.001) |
| Adjusted* | 1.71 | 1.77 | 0.06 (0.08) | 1.85 | 1.68 | -0.17 (<.001) | -0.22 (<.001) |
| Definitive surgery | |||||||
| Stage I-III | |||||||
| Unadjusted | 0.87 | 0.89 | 0.02 (0.06) | 0.89 | 0.92 | 0.03 (<.001) | 0.012 (0.37) |
| Adjusted* | 0.85 | 0.86 | 0.01 (0.28) | 0.86 | 0.88 | 0.02 (0.002) | 0.013 (0.33) |
| Immunotherapy (stage III & IV only) | |||||||
| Unadjusted | 0.20 | 0.23 | 0.03 (0.27) | 0.43 | 0.50 | 0.06 (<.001) | 0.04 (0.23) |
| Adjusted* | 0.17 | 0.20 | 0.03 (0.29) | 0.41 | 0.47 | 0.06 (<.001) | 0.04 (0.20) |
| 3-year mortality | |||||||
| Unadjusted | 0.27 | 0.28 | 0.01 (0.27) | 0.19 | 0.15 | -0.04 (<.001) | -0.06 (<.001) |
| Adjusted* | 0.21 | 0.24 | 0.03 (0.02) | 0.14 | 0.12 | -0.02 (0.03) | -0.06 (0.001) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




