Submitted:
30 October 2024
Posted:
30 October 2024
You are already at the latest version
Abstract
Background/Objectives: Stroke patients generally have balance and gait dysfunction due to decreased range of motion (ROM) and muscle strength of the ankle joint. A therapist can apply a floss band to enhance ROM, pain control, jumping performance, strength, myofascial release, and recovery from fatigue. This study compared the immediate effects of floss band application on ankle ROM, balance, and gait ability in stroke patients.; Methods: This study randomized 40 chronic stroke patients to either the floss (n = 20) or sham (n = 20) band group. Outcome measures were ankle ROM, weight bearing lunge test (WBLT) performance, standing balance, and gait ability. Outcome measures were assessed at baseline and immediately after applying the floss or placebo band.; Results: There were significant improvements in dorsiflexion (DF), WBLT, static balance, and foot strike in those who used the floss band compared to the sham group (all p < 0.05).; Conclusions: The floss band improved ankle DF, balance, and gait, indicating that it is a feasible therapeutic method for improving ankle DF, balance, and gait in chronic stroke patients.
Keywords:
1. Introduction
2. Materials and Methods
2.1. Participants
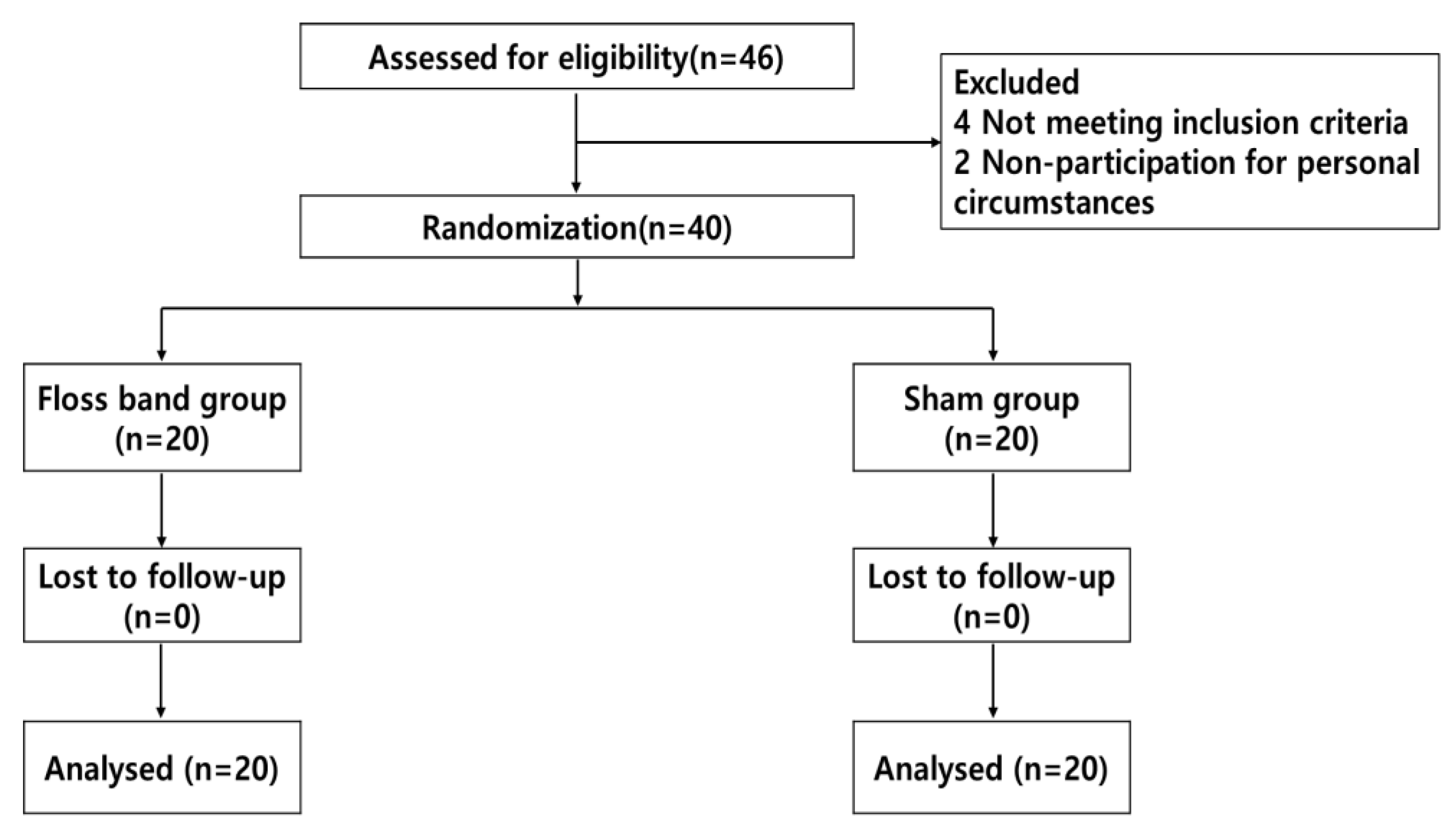
2.2. Procedures
2.3. Interventions
2.3.1. Floss Band intervention
2.3.2. Sham Floss Band Intervention
2.4. Outcome Measurements
2.4.1. Ankle Passive Range of Motion
2.4.2. Weight-Bearing Lunge Test
2.4.3. Static Balance Ability
2.4.4. Gait Ability
2.5. Statistical Analysis
3. Results
3.1. Baseline
3.2. Passive ROM
3.3. WBLT
3.4. Balance ability
3.5. Gait ability
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Conflicts of Interest
References
- Choi, S.H.; Lim, C.G. Immediate effects of ankle non-elastic taping on balance and gait ability in patients with chronic stroke: a randomized, controlled trial. Journal of Manipulative and Physiological Therapeutics 2020, 43, 922–929. [Google Scholar] [CrossRef] [PubMed]
- Patrick, J.H.; Keenan, M.A. Gait analysis to assist walking after stroke. The Lancet 2007, 369, 256–257. [Google Scholar] [CrossRef] [PubMed]
- Song, S.; Park, J.; Song, G.; Lee, S.; Jo, Y.; Jin, M.; Lee, G. Usability of the Thera-Band® to improve foot drop in stroke survivors. NeuroRehabilitation 2018, 42, 505–510. [Google Scholar] [CrossRef]
- Park, D.; Lee, J. H.; Kang, T.W.; Cynn, H.S. Immediate effects of talus-stabilizing taping on balance and gait parameters in patients with chronic stroke: A cross-sectional study. Topics in Stroke Rehabilitation 2018, 25, 417–423. [Google Scholar] [CrossRef]
- Boffeli, T.J.; Collier, R.C. Minimally invasive soft tissue release of foot and ankle contracture secondary to stroke. The Journal of Foot and Ankle Surgery 2014, 53, 369–375. [Google Scholar] [CrossRef] [PubMed]
- Ravichandran, H.; Janakiraman, B. The Effects of Ankle Joint Mobilization on Dorsiflexion Range and Gait Parameters in Chronic Stroke Survivors: A Systematic Review and Meta-analysis. Journal of Stroke Medicine 2021, 4, 15–24. [Google Scholar] [CrossRef]
- Mirshams Shahshahani, P.; Ashton-Miller, J.A. On the importance of the hip abductors during a clinical one legged balance test: A theoretical study. Plos one 2020, 15, e0242454. [Google Scholar] [CrossRef] [PubMed]
- Gao, F.; Ren, Y.; Roth, E.J.; Harvey, R.; Zhang, L.Q. Effects of repeated ankle stretching on calf muscle–tendon and ankle biomechanical properties in stroke survivors. Clinical biomechanics 2011, 26, 516–522. [Google Scholar] [CrossRef] [PubMed]
- Cho, K.H.; Park, S.J. Effects of joint mobilization and stretching on the range of motion for ankle joint and spatiotemporal gait variables in stroke patients. Journal of Stroke and Cerebrovascular Diseases 2020, 29, 104933. [Google Scholar] [CrossRef]
- Choo, Y.J.; Kim, J.K.; Kim, J.H.; Chang, M.C.; Park, D. Machine learning analysis to predict the need for ankle foot orthosis in patients with stroke. Scientific Reports 2021, 11, 1–7. [Google Scholar] [CrossRef]
- Johnston, T.E.; Keller, S.; Denzer-Weiler, C.; Brown, L. A Clinical Practice Guideline for the Use of Ankle-Foot Orthoses and Functional Electrical Stimulation Post-Stroke. Journal of Neurologic Physical Therapy 2021, 45, 112–196. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Q.; Wang, Y.; Zhou, M.; Li, D.; Yan, J.; Liu, Q.; Long, J. Ankle rehabilitation robot training for stroke patients with foot drop: Optimizing intensity and frequency. NeuroRehabilitation 2023, 53, 567–57. [Google Scholar] [CrossRef] [PubMed]
- Kalc, M.; Mikl, S.; Žökš, F.; Vogrin, M.; Stöggl, T. Effects of different tissue flossing applications on range of motion, maximum voluntary contraction, and h-reflex in young martial arts fighters. Frontiers in Physiology 2021, 12, 752641. [Google Scholar] [CrossRef] [PubMed]
- Rodrigues, S.; Forte, P.; Dewaele, E.; Branquinho, L.; Teixeira, J.E.; Ferraz, R.; Monteiro, A.M. Effect of blood flow restriction technique on delayed onset muscle soreness: a systematic review. Medicina 2022, 58, 1154. [Google Scholar] [CrossRef] [PubMed]
- Driller, M.W.; Overmayer, R.G. The effects of tissue flossing on ankle range of motion and jump performance. Physical Therapy in Sport 2017, 25, 20–24. [Google Scholar] [CrossRef]
- Vogrin, M.; Novak, F.; Licen, T.; Greiner, N.; Mikl, S.; Kalc, M. Acute effects of tissue flossing on ankle range of motion and tensiomyography parameters. Journal of Sport Rehabilitation 2020, 30, 129–135. [Google Scholar] [CrossRef]
- Rosier, E. The Long-Term Effects of Tissue Flossing on Ankle Dorsiflexion Range of Motion in Athletes with Chronic Ankle Instability, Illinois State University, Illinois, USA, March 31 2020.
- Koshino, Y.; Takabayashi, T.; Akuzawa, H.; Mizota, T.; Numasawa, S.; Kobayashi, T.; Edama, M. Differences and relationships between weightbearing and non-weightbearing dorsiflexion range of motion in foot and ankle injuries. Journal of Orthopaedic Surgery and Research 2024, 19, 115. [Google Scholar] [CrossRef]
- Clapper, M.P.; Wolf, S.L. Comparison of the reliability of the Orthoranger and the standard goniometer for assessing active lower extremity range of motion. Physical Therapy 1988, 68, 214–218. [Google Scholar] [CrossRef]
- Abu El Kasem, S.T.; Aly, S.M.; Kamel, E.M.; Hussein, H.M. Normal active range of motion of lower extremity joints of the healthy young adults in Cairo, Egypt. Bulletin of Faculty of Physical Therapy 2020, 25, 1–7. [Google Scholar] [CrossRef]
- Cady, K.; Croix, M.D.S.; Deighan, M. Back foot influence on dorsiflexion using three different positions of the weight bearing lunge test. Physical Therapy in Sport 2021, 47, 1–6. [Google Scholar] [CrossRef]
- Mancini, M.; Horak, F.B. Potential of APDM mobility lab for the monitoring of the progression of Parkinson’s disease. Expert Review of Medical Devices 2016, 13, 455–462. [Google Scholar] [CrossRef] [PubMed]
- Hou, Y.; Wang, S.; Li, J.; Komal, S.; Li, K. Reliability and Validity of a Wearable Inertial Sensor System for Gait Assessment in Healthy Young Adults. In 2021 14th International Congress on Image and Signal Processing, BioMedical Engineering and Informatics (CISP-BMEI) 2021, 1-6.
- Kaneda H; Takahira N; Tsuda K; Tozaki K; Kudo S; Takahashi Y. Effects of tissue flossing and dynamic stretching on hamstring muscles function. Journal of Sports Science & Medicine 2020, 19, 681–689. [Google Scholar]
- Stevenson, P.J.; Stevenson, R.K.; Duarte, K.W. Acute effects of the voodoo flossing band on ankle range of motion. J Med Biomed Appl Sci 2019, 7, 244–253. [Google Scholar]
- Vogrin, M.; Kalc, M.; Ličen, T. Acute effects of tissue flossing around the upper thigh on neuromuscular performance: a study using different degrees of wrapping pressure. Journal of Sport Rehabilitation 2020, 30, 601–608. [Google Scholar] [CrossRef] [PubMed]
- Reeves, G.; Kraemer, R.; Hollander, D.; Clavier, J.; Thomas, C.; Francois, M. Comparison of hormone responses following light resistance exercise with partial vascular occlusion and moderately difficult resistance exercise without occlusion. Journal of Applied Physiology 2006, 101, 1616–1622. [Google Scholar] [CrossRef]
- In, T.; Jin, Y.; Jung, K.; Cho, H.Y. Treadmill training with Thera-Band improves motor function, gait and balance in stroke patients. NeuroRehabilitation 2017, 40, 109–114. [Google Scholar] [CrossRef]
- Cho, J.E.; Lee, W.H.; Shin, J.H.; Kim, H. Effects of bi-axial ankle strengthening on muscle co-contraction during gait in chronic stroke patients: a randomized controlled pilot study. Gait & Posture 2021, 87, 177–183. [Google Scholar]
- Yoo, D.; Kim, D.H.; Seo, K.H.; Lee, B.C. The effects of technology-assisted ankle rehabilitation on balance control in stroke survivors. IEEE transactions on neural systems and rehabilitation engineering 2019, 27, 1817–1823. [Google Scholar] [CrossRef]
- Cho, J.E.; Kim, H. Ankle proprioception deficit is the strongest factor predicting balance impairment in patients with chronic stroke. Archives of rehabilitation research and clinical translation 2021, 3, 100165. [Google Scholar] [CrossRef]
- Kim, S. G.; Kim, W. S. Effect of ankle range of motion (ROM) and lower-extremity muscle strength on static balance control ability in young adults: a regression analysis. Medical science monitor: international medical journal of experimental and clinical research 2018, 24, 3168. [Google Scholar] [CrossRef]
- Chang, N.J.; Hung, W.C.; Lee, C.L.; Chang, W.D.; Wu, B.H. Effects of a single session of floss band intervention on flexibility of thigh, knee joint proprioception, muscle force output, and dynamic balance in young adults. Applied Sciences 2021, 11, 12052. [Google Scholar] [CrossRef]
- Aali, S.; Rezazadeh, F.; Badicu, G.; Grosz, W.R. Effect of heel-first strike gait on knee and ankle mechanics. Medicina 2021, 57, 657. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Li, H.; Liu, Y.; Liang, W.; Zhang, L.; Zhou, F.; Yuan, X. The effect of electromyographic feedback functional electrical stimulation on the plantar pressure in stroke patients with foot drop. Frontiers in Neuroscience 2024, 18, 1377702. [Google Scholar] [CrossRef] [PubMed]
- Kaneda, H.; Takahira, N.; Tsuda, K.; Tozaki, K.; Sakai, K.; Kudo, S.; Kenmoku, T. The effects of tissue flossing and static stretching on gastrocnemius exertion and flexibility. Isokinetics and Exercise Science 2020, 28, 205–213. [Google Scholar] [CrossRef]
- Inai, T.; Kobayashi, Y.; Huang, C.; Fujita, K.; Fujimoto, M.; Nihey, F.; Kudo, S. Identification of characteristics of foot position and angle during swing phase in fallers using principal component analysis. Frontiers in Bioengineering and Biotechnology 2023, 11, 1117884. [Google Scholar] [CrossRef]

| Floss band group (n=20) | Sham group (n=20) | t/χ2 | p | ||||||||
| Age(years) | 58.15 | ± | 11.93 | 60.4 | ± | 10.29 | -579 | .566 | |||
| Height(㎝) | 164.8 | ± | 8.08 | 167.4 | ± | 8.28 | -1.16 | .253 | |||
| Weight(㎏) | 64.34 | ± | 11.02 | 66.4 | ± | 8.56 | -175 | .862 | |||
| Gender (male/female) | 10 | / | 10 | 12 | / | 8 | .241 | .623 | |||
| Affected side (R/L) | 9 | / | 11 | 6 | / | 14 | 1.336 | .248 | |||
| Stroke type (hemorrhage / ischemia) | 5 | / | 15 | 9 | / | 11 | 2.046 | .153 | |||
| K-MMSE | 25.65 | ± | 2.11 | 24.75 | ± | 2.47 | 1.136 | .263 | |||
| MAS | .8 | ± | .5 | .53 | ± | .54 | 1.757 | .087 | |||
| BRS | 4.6 | ± | .48 | 4.4 | ± | .50 | 1.087 | .284 | |||
| BBS | 42.15 | ± | 6.24 | 39.85 | ± | 9.28 | .721 | .475 | |||
| MBI | 63.55 | ± | 9.53 | 60.1 | ± | 14.23 | .756 | .454 | |||
| TUG | 10.16 | ± | 1.07 | 10.18 | ± | 1.18 | .011 | .991 | |||
| Pre | Post | Effect size | Factor | F | p | |||||||||
| DF(︒) | Sham | 3.10 | ± | 2.38 | 3.40 | ± | 2.16 | 0.19 | T | 146.745 | .000* | |||
| G | 13.728 | .002* | ||||||||||||
| Floss | 2.60 | ± | 1.47 | 8.90 | ± | 2.10* | 4.92 | |||||||
| T×G | 114.000 | .000* | ||||||||||||
| PF(︒) | Sham | 52.90 | ± | 1.94 | 53.10 | ± | 1.62 | 0.10 | T | .322 | .577 | |||
| G | 4.135 | .056 | ||||||||||||
| Floss | 53.85 | ± | 1.95 | 54.00 | ± | 2.34 | 0.16 | |||||||
| T×G | .007 | .933 | ||||||||||||
| WBLT(㎝) | Sham | 7.65 | ± | 1.84 | 7.90 | ± | 1.80 | 0.19 | T | 27.143 | .000* | |||
| G | 6.234 | .022* | ||||||||||||
| Floss | 8.65 | ± | 1.50 | 9.40 | ± | 1.43 | 0.72 | |||||||
| T×G | 3.276 | .086 | ||||||||||||
| SB(㎟) | Sham | 7.39 | ± | 3.87 | 7.25 | ± | 3.47 | 0.05 | T | 27.143 | .000* | |||
| G | 6.234 | .022* | ||||||||||||
| Floss | 7.00 | ± | 5.25 | 4.31 | ± | 3.16* | 0.88 | |||||||
| T×G | 7.878 | .011* | ||||||||||||
| FS(︒) | Sham | 9.38 | ± | 6.47 | 9.58 | ± | 5.74 | 0.05 | T | 15.422 | .001* | |||
| G | 2.076 | .166 | ||||||||||||
| Floss | 10.20 | ± | 4.16 | 13.09 | ± | 4.95* | 0.89 | |||||||
| T×G | 12.694 | .002* | ||||||||||||
| TO(︒) | Sham | 14.96 | ± | 3.91 | 15.04 | ± | 4.18 | 0.03 | T | .665 | .425 | |||
| G | .124 | .729 | ||||||||||||
| Floss | 15.74 | ± | 5.81 | 15.04 | ± | 4.16 | 0.20 | |||||||
| T×G | .401 | .534 | ||||||||||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




