Submitted:
23 October 2024
Posted:
23 October 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
- -
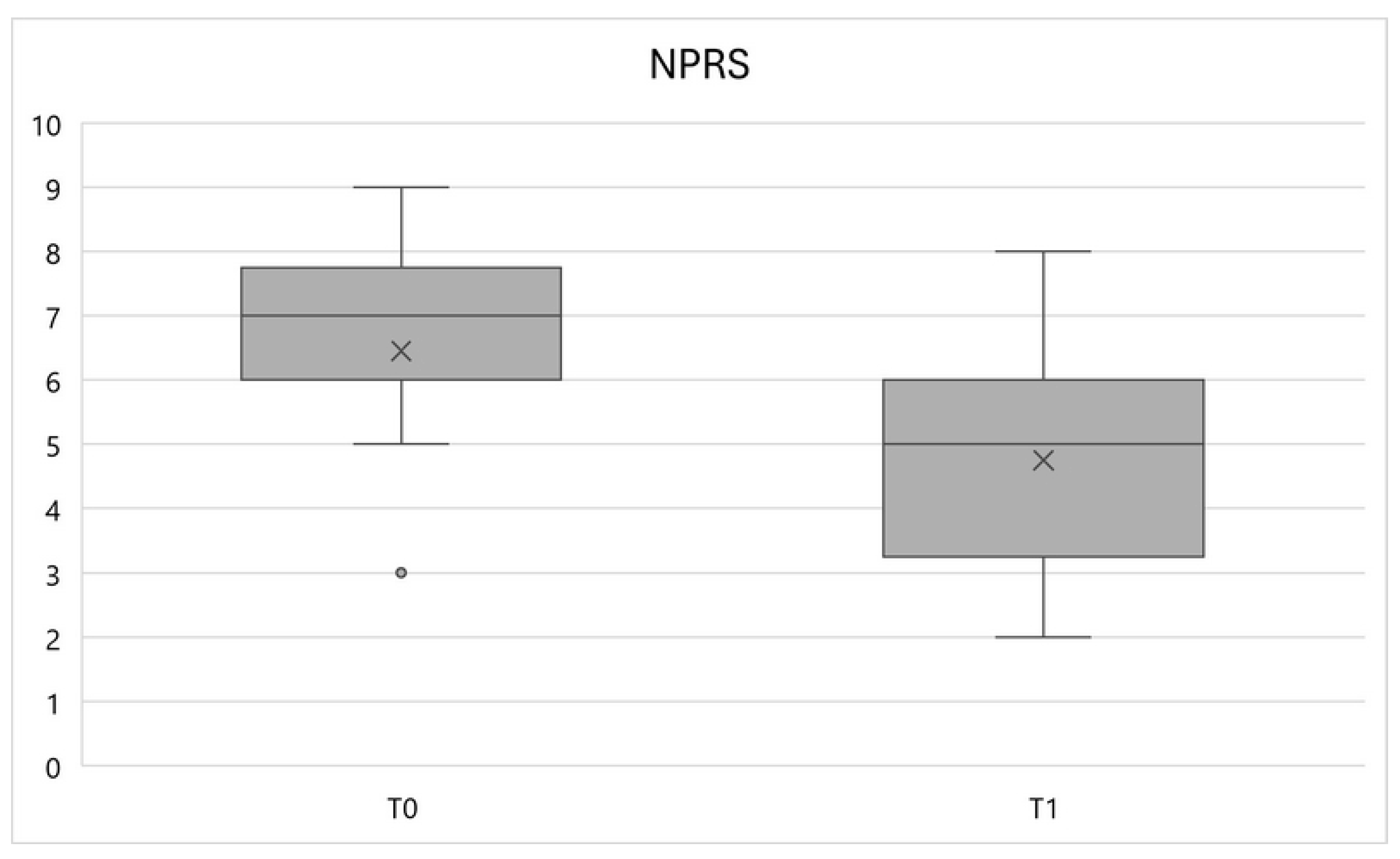
- Numeric Pain Rating Scale (NPRS): it is one of the most common tools for measuring the pain subjectively perceived by patients. It is a derivate of the Visual-Analogue Scale (VAS) divided into ten levels, usually distributed equidistant on a 10 cm long strip, which correspond to the level of pain perceived by the patient at the time of the evaluation, where 0 is the total absence of pain and 10 is the maximum level of pain imaginable and/or ever experienced by the patient [26]. This scale is reliable, effective and easy to apply even in the presence of dysfunctions of the general musculoskeletal system [26]. In the case of the present study, patients were asked to express a value from 0 to 10 corresponding to the maximum level of pain perceived at the site of the body which was more painful for them following the surgery;
- -
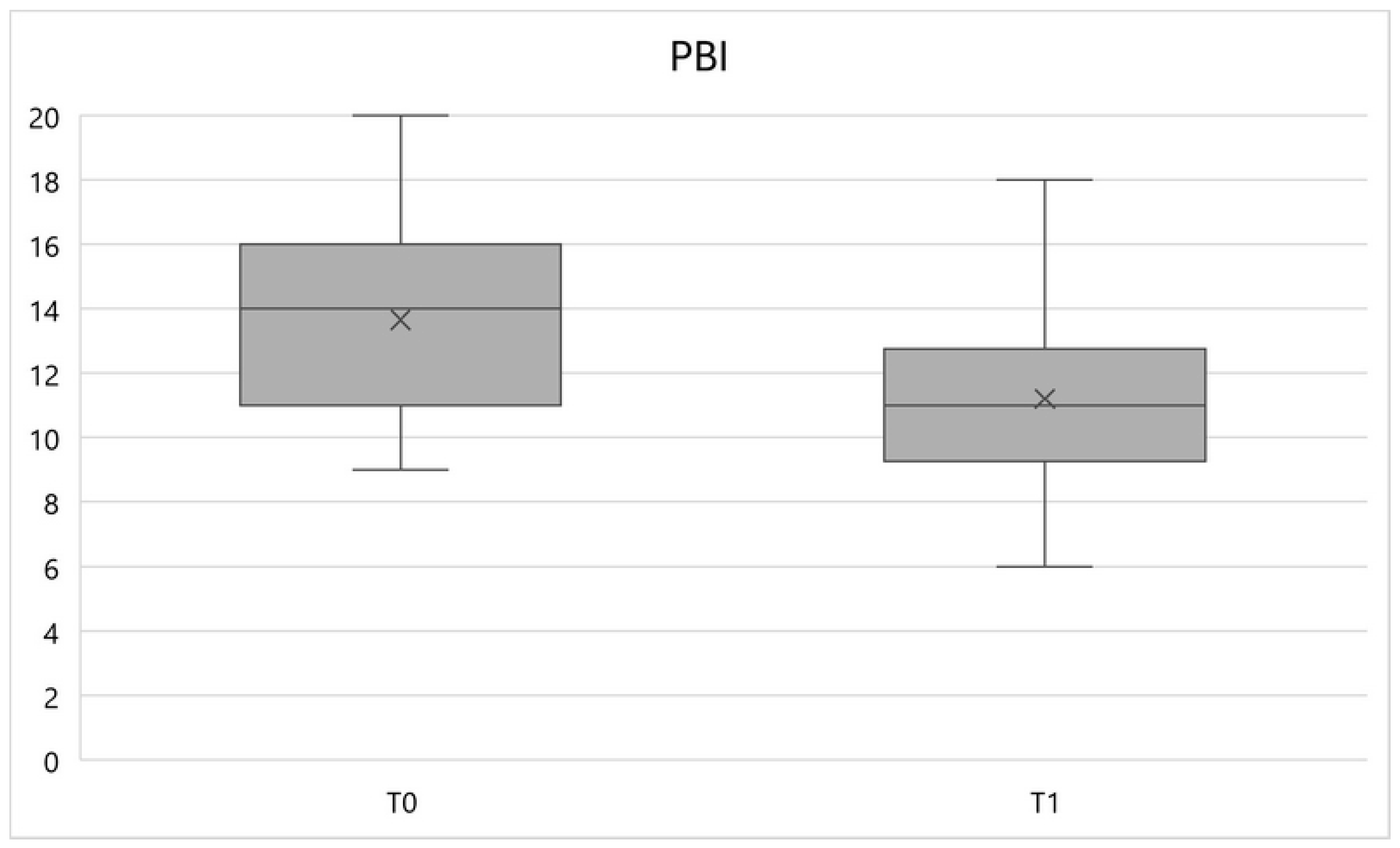
- Postural Biometric Index (PBI): this is an index calculated by the proprietary software of the Milletrix 3.0 platform (Diasu Health Technologies, Rome, Italy) on the basis of a stabilometric evaluation carried out using the same device [9]. This index takes into account the parameters of Center of Pressure, Symmetry of Bipodalic Load, Symmetry of Retro-Forefoot Load, Angle of Centers of Pressure, Podalic Angle, Location of Maximum Pressure Point, Symmetry of Support Surface and Center of Gravity Deviation - Center of Pressure [9]. These parameters are then correlated to obtain an index that quantifies the postural state of the patient [9]. The PBI value is considered healthy from 0 to 10 and dysfunctional if >10.
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Vervoort, D.; Lee, G.; Ghandour, H.; Guetter, C.R.; Adreak, N.; Till, B.M.; Lin, Y. Global cardiac surgical volume and gaps: trends, targets, and way forward. Annals of Thoracic Surgery Short Reports 2024, 2, 320–324. [Google Scholar] [CrossRef]
- Saunders, A.C.; Mutebi, M.; Rao, T.S. A review of the current state of global surgical oncology and the role of surgeons who treat cancer: our profession’s imperative to act upon a worldwide crisis in evolution. Annals of Surgical Oncology 2023, 30, 3197–3205. [Google Scholar] [CrossRef] [PubMed]
- Correa-Rodríguez, M.; Abu Ejheisheh, M.; Suleiman-Martos, N.; Membrive-Jiménez, M.J.; Velando-Soriano, A.; Schmidt-RioValle, J.; Gómez-Urquiza, J.L. Prevalence of depression in coronary artery bypass surgery: A systematic review and meta-analysis. Journal of clinical medicine 2020, 9, 909. [Google Scholar] [CrossRef] [PubMed]
- Antoni, M.H.; Jacobs, J.M.; Bouchard, L.C.; Lechner, S.C.; Jutagir, D.R.; Gudenkauf, L.M.; Blomberg, B.B.; Glück, S.; Carver, C.S. Post-surgical depressive symptoms and long-term survival in non-metastatic breast cancer patients at 11-year follow-up. General hospital psychiatry 2017, 44, 16–21. [Google Scholar] [CrossRef]
- Rosenberger, D.C.; Pogatzki-Zahn, E.M. Chronic post-surgical pain–update on incidence, risk factors and preventive treatment options. BJA education 2022, 22, 190–196. [Google Scholar] [CrossRef]
- Fagundes, C.P.; Shi, Q.; Vaporciyan, A.A.; Rice, D.C.; Popat, K.U.; Cleeland, C.S.; Wang, X.S. Symptom recovery after thoracic surgery: Measuring patient-reported outcomes with the MD Anderson Symptom Inventory. The Journal of thoracic and cardiovascular surgery 2015, 150, 613–619. [Google Scholar] [CrossRef]
- Wang, L.; Cohen, J.C.; Devasenapathy, N.; Hong, B.Y.; Kheyson, S.; Lu, D.; Oparin, Y.; Kennedy, S.A.; Romerosa, B.; Arora, N.; Kwon, H.Y. Prevalence and intensity of persistent post-surgical pain following breast cancer surgery: a systematic review and meta-analysis of observational studies. British journal of anaesthesia. 2020, 125, 346–357. [Google Scholar] [CrossRef]
- Mangone, M.; Bernetti, A.; Agostini, F.; Paoloni, M.; De Cicco, F.A.; Capobianco, S.V.; Bai, A.V.; Bonifacino, A.; Santilli, V.; Paolucci, T. Changes in spine alignment and postural balance after breast cancer surgery: a rehabilitative point of view. BioResearch open access 2019, 8, 121–128. [Google Scholar] [CrossRef]
- Barassi, G.; Di Simone, E.; Galasso, P.; Cristiani, S.; Supplizi, M.; Kontochristos, L.; Colarusso, S.; Visciano, C.P.; Marano, P.; Di Iulio, A.; Giancola, P. Posture and health: are the biomechanical postural evaluation and the postural evaluation questionnaire comparable to and predictive of the digitized biometrics examination? International Journal of Environmental Research and Public Health 2021, 18, 3507. [Google Scholar] [CrossRef]
- Lee, J.S.; Park, E.; Lee, J.H.; Lee, J.; Park, H.Y.; Yang, J.D.; Jung, T.D. Alteration in skeletal posture between breast reconstruction with latissimus dorsi flap and mastectomy: a prospective comparison study. Gland surgery 2021, 10, 1587. [Google Scholar] [CrossRef]
- Kocjan, J.; Gzik-Zroska, B.; Nowakowska-Lipiec, K.; Burkacki, M.; Suchoń, S.; Michnik, R.; Czyżewski, D.; Adamek, M. Thoracic surgery may alter body static balance via diaphragm dysfunction. Plos one 2022, 17, e0273641. [Google Scholar] [CrossRef] [PubMed]
- Stiller, K.; McInnes, M.; Huff, N.; Hall, B. Do exercises prevent musculoskeletal complications after cardiac surgery? Physiotherapy Theory and Practice 1997, 13, 117–126. [Google Scholar] [CrossRef]
- Filbay, S.R.; Hayes, K.; Holland, A.E. Physiotherapy for patients following coronary artery bypass graft (CABG) surgery: limited uptake of evidence into practice. Physiotherapy theory and practice 2012, 28, 178–187. [Google Scholar] [CrossRef] [PubMed]
- Cheville, A.L. , Tchou, J. Barriers to rehabilitation following surgery for primary breast cancer. Journal of surgical oncology 2007, 95, 409–418. [Google Scholar] [CrossRef] [PubMed]
- Barassi, G.; Di Stefano, G.; Pellegrino, R.; Di Iulio, A.; Gildone, V.; Pensa, G.; Cipriano, M.; Matarese, M.; d’Alessandro, F.; Sacco, F.; Prosperi, L. Focused Mechano-Acoustic Vibrations: Bio-Physico-Metric Approach in Neuromuscular Diseases. Eur J Musculoskel Dis 2024, 13, 41–45. [Google Scholar]
- Saggini, R.; Carmignano, S.M.; Palermo, T.; Bellomo, R.G. Mechanical vibration in rehabilitation: state of the art. Journal of novel physiotherapies 2016, 6, 314. [Google Scholar] [CrossRef]
- Pietrangelo, T.; Mancinelli, R.; Toniolo, L.; Cancellara, L.; Paoli, A.; Puglielli, C.; Iodice, P.; Doria, C.; Bosco, G.; d'Amelio, L.; Di Tano, G. Effects of local vibrations on skeletal muscle trophism in elderly people: mechanical, cellular, and molecular events. International journal of molecular medicine 2009, 24, 503–512. [Google Scholar] [CrossRef]
- Iodice, P.; Bellomo, R.G.; Migliorini, M.; Megna, M.; Saggini, R. Flexible flatfoot treatment in children with mechanical sound vibration therapy. International Journal of Immunopathology and Pharmacology 2012, 25(1_suppl), 9-15.
- Costantino, C.; Galuppo, L.; Romiti, D. Efficacy of mechano-acoustic vibration on strength, pain, and function in poststroke rehabilitation: a pilot study. Topics in Stroke Rehabilitation 2014, 21, 391–399. [Google Scholar] [CrossRef]
- Casale, R.; Ring, H.; Rainoldi, A. High frequency vibration conditioning stimulation centrally reduces myoelectrical manifestation of fatigue in healthy subjects. Journal of electromyography and Kinesiology 2009, 19, 998–1004. [Google Scholar] [CrossRef]
- Prosperi, L.; Barassi, G.; Panunzio, M.; Pellegrino, R.; Marinucci, C.; Di Iulio, A.; Colombo, A.; Licameli, M.; Moccia, A.; Melchionna, M. Bio-Physics approach to urinary incontinence disabilities. International Journal of Environmental Research and Public Health 2022, 19, 12612. [Google Scholar] [CrossRef]
- Sancilio, S.; Nobilio, S.; Ruggiero, A.G.; Di Filippo, E.S.; Stati, G.; Fulle, S.; Bellomo, R.G.; Saggini, R.; Di Pietro, R. Effects of Focused Vibrations on Human Satellite Cells. International Journal of Molecular Sciences 2022, 23, 6026. [Google Scholar] [CrossRef] [PubMed]
- Dessy, L.A.; Monarca, C.; Grasso, F.; Saggini, A.; Buccheri, E.M.; Saggini, R.; Scuderi, N. The use of mechanical acoustic vibrations to improve abdominal contour. Aesthetic Plastic Surgery 2008, 32, 339–345. [Google Scholar] [CrossRef] [PubMed]
- De Sanctis, V.; Soliman, A.T.; Daar, S.; Tzoulis, P.; Fiscina, B.; Kattamis, C. Retrospective observational studies: Lights and shadows for medical writers. Acta Bio Medica Atenei Parm. 2022, 93, e2022319. [Google Scholar]
- Winter, E.M.; Maughan, R.J. Requirements for ethics approvals. J. Sports Sci. 2009, 27, 985. [Google Scholar] [CrossRef]
- Cheatham, S.W.; Kolber, M.J.; Mokha, M.; Hanney, W.J. Concurrent validity of pain scales in individuals with myofascial pain and fibromyalgia. Journal of Bodywork and Movement Therapies 2018, 22, 355–360. [Google Scholar] [CrossRef]
- Alentorn-Geli, E.; Padilla, J.; Moras, G.; Haro, C.L.; Fernández-Solà, J. Six weeks of whole-body vibration exercise improves pain and fatigue in women with fibromyalgia. The Journal of Alternative and Complementary Medicine 2008, 14, 975–981. [Google Scholar] [CrossRef]
- Dong, Y.; Wang, W.; Zheng, J.; Chen, S.; Qiao, J.; Wang, X. Whole body vibration exercise for chronic musculoskeletal pain: a systematic review and meta-analysis of randomized controlled trials. Archives of physical medicine and rehabilitation 2019, 100, 2167–2178. [Google Scholar] [CrossRef]
- Yilmaz Menek, M.; Dansuk, E.; Tayboga, U.I. Effect of Local Vibration Therapy on Pain, Joint Position Sense, Kinesiophobia, and Disability in Cervical Disc Herniation: A Randomized Controlled Trial. Journal of Clinical Medicine 2024, 13, 4566. [Google Scholar] [CrossRef]
- Chu, Y.; Zhao, Y.; Hu, S.; Wang, Q.; Semeah, L.M.; Jia, H.; Lv, T.; Li, X.; Wang, R. Immediate effect of local vibration therapy for sport-induced fatigue based on traditional Chinese medicine’s holistic theory. Journal of Multidisciplinary Healthcare 2020, 13, 1993–2001. [Google Scholar] [CrossRef]
- Hollins, M.; Corsi, C.; Sloan, P. Pacinian signals determine the direction and magnitude of the effect of vibration on pain. Perception 2017, 46, 987–999. [Google Scholar] [CrossRef]
- Casale, R.; Hansson, P. The analgesic effect of localized vibration: a systematic review: Part 1: the neurophysiological basis. European Journal of Physical and Rehabilitation Medicine 2022, 58, 306. [Google Scholar] [CrossRef] [PubMed]
- Alashram, A.R.; Padua, E.; Romagnoli, C.; Raju, M.; Annino, G. Clinical effectiveness of focal muscle vibration on gait and postural stability in individuals with neurological disorders: A systematic review. Physiotherapy Research International 2022, 27, e1945. [Google Scholar] [CrossRef] [PubMed]
- Ferrara, P.E.; Gatto, D.M.; Codazza, S.; Zordan, P.; Stefinlongo, G.; Coraci, D.; Lo Monaco, M.R.; Ricciardi, D.; Ronconi, G. Effects of focal muscle vibration on gait and balance in Parkinson patients: preliminary results. Applied Sciences 2022, 12, 10486. [Google Scholar] [CrossRef]
- Germann, D.; El Bouse, A.; Shnier, J.; Abdelkader, N.; Kazemi, M. Effects of local vibration therapy on various performance parameters: a narrative literature review. The Journal of the Canadian Chiropractic Association 2018, 62, 170. [Google Scholar] [PubMed]
- Fattorini, L.; Rodio, A.; Pettorossi, V.E.; Filippi, G.M. Is the focal muscle vibration an effective motor conditioning intervention? A systematic review. Journal of functional morphology and kinesiology 2021, 6, 39. [Google Scholar] [CrossRef]
- Barassi, G.; Prosperi, L.; Marinucci, C.; Di Iorio, A.; Panunzio, M. Focused Mechano-Acoustic Vibrations in Chronic Pain: Bio-Physico-Metric Approach, Key Trigger Points and Posture. Medical Science Pulse 2024, 18, 30. [Google Scholar]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



