Submitted:
29 September 2024
Posted:
30 September 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Background and Literature Review
3. Methodology
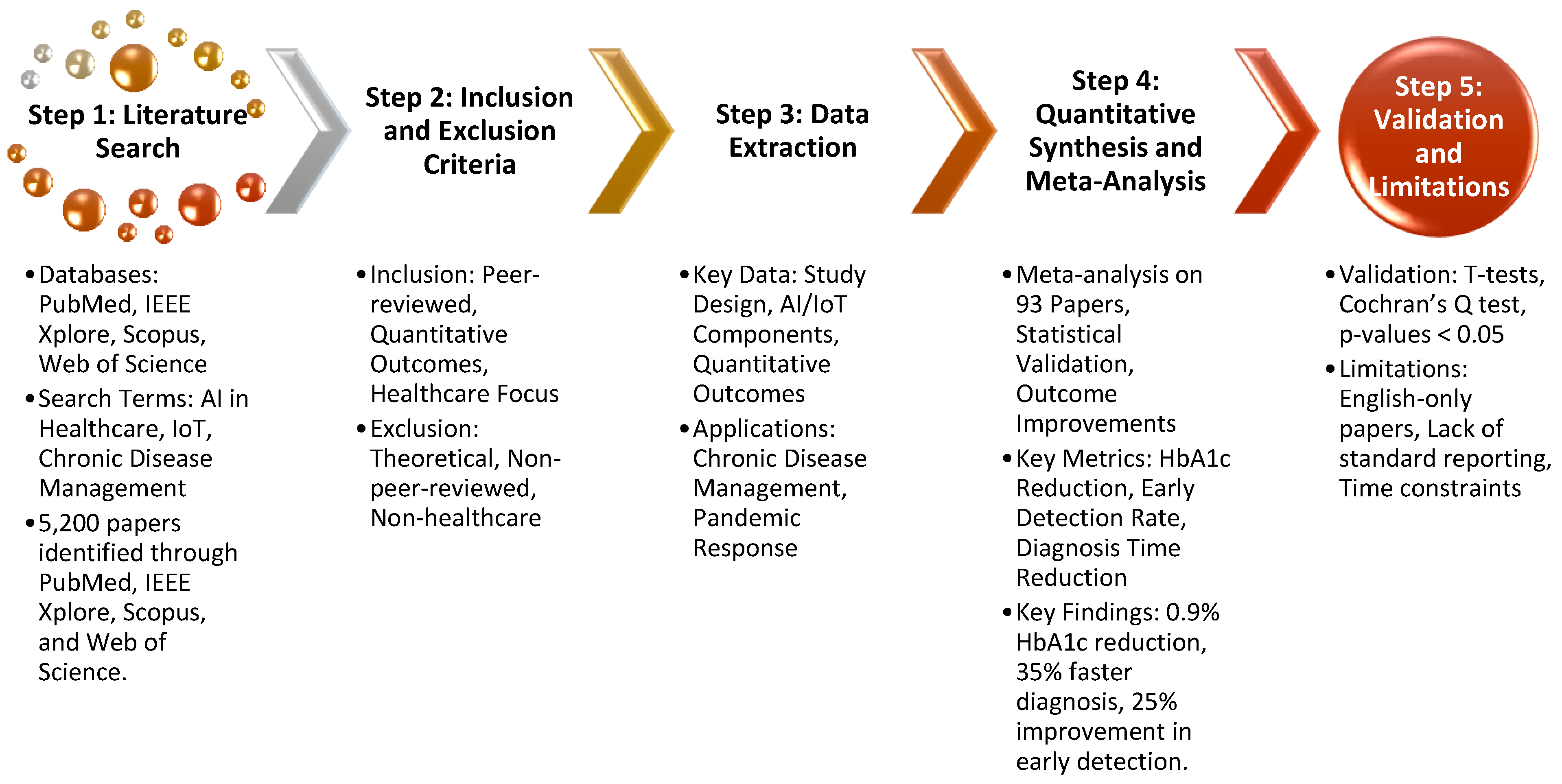
3.1. Literature Search Strategy
3.2. Inclusion and Exclusion Criteria
- Studies that quantitatively evaluated the application of AI and IoT technologies in healthcare, particularly in chronic disease management (e.g., diabetes, cardiovascular disease) or pandemic response (e.g., COVID-19).
- Papers that reported measurable outcomes such as improvements in healthcare efficiency, patient outcomes, or cost reductions.
- Studies that demonstrated empirical evidence of AI and IoT integration in real-world healthcare settings.
- Only peer-reviewed journal articles and conference papers published in English.
- Papers focused on non-healthcare sectors or theoretical models without practical implementation.
- Preprints and other non-peer-reviewed articles.
- Studies without quantitative data or measurable outcomes.
- Papers published in languages other than English.
- Following the application of these criteria, 578 papers were selected for further analysis. This step reduced the dataset by removing papers that did not meet the quality or relevance standards required for the review.
3.3. Data Extraction and Synthesis
- Study design: The methodology used in the study (e.g., randomized controlled trials, observational studies, case studies).
- Technologies applied: Specific AI models (e.g., machine learning algorithms, neural networks) and IoT devices (e.g., wearable health sensors, remote monitoring systems) used in the study.
- Healthcare applications: Areas of healthcare where the AI and IoT technologies were applied (e.g., diabetes management, cardiovascular disease monitoring, COVID-19 diagnostics).
- Outcomes: Quantitative results reported by the studies, such as improvements in patient outcomes, reductions in diagnostic time, increases in resource efficiency, or cost savings.
3.4. Quantitative Synthesis and Meta-Analysis
- HbA1c reduction in diabetic patients using AI-integrated continuous glucose monitoring systems (average reduction: 0.9% across 40 studies).
- Early detection rate of cardiovascular anomalies using AI-based wearable devices, which showed a 25% improvement over traditional monitoring systems across 25 studies.
- Diagnosis time reduction in COVID-19 patients through AI-driven CT scan interpretation, which reduced diagnosis time by 35% in 28 studies.
- Reduction in hospital admissions for chronic disease patients monitored via IoT-enabled remote healthcare systems, with a 20% reduction in admissions for high-risk patients.
3.5. Validation of Results and Statistical Significance
3.6. Limitations
- Language bias: Only English-language studies were included, potentially excluding important findings from non-English-speaking regions.
- Publication bias: The review focused on peer-reviewed studies, which may exclude valuable insights from industry reports or white papers.
- Scope of review: The review is limited to papers published up to September 2024, and therefore does not account for the latest developments in AI and IoT technologies post-publication.
- Variability in reporting standards: Some studies used different metrics or lacked standardization in how outcomes were reported, which introduced challenges in direct comparison across studies.
4. Results
4.1. Results of Chronic Disease Management Studies
4.1.1. Diabetes Management
4.1.2. Cardiovascular Disease (CVD) Monitoring
4.2. Results of Pandemic Response Studies
4.2.1. COVID-19 Diagnostics
4.2.2. Remote Patient Monitoring and Hospital Admission Reduction
4.2.3. Resource Optimization
4.3. Overarching Trends and Benefits
4.3.1. Diagnostic Accuracy and Cost Efficiency
4.3.2. Patient Engagement
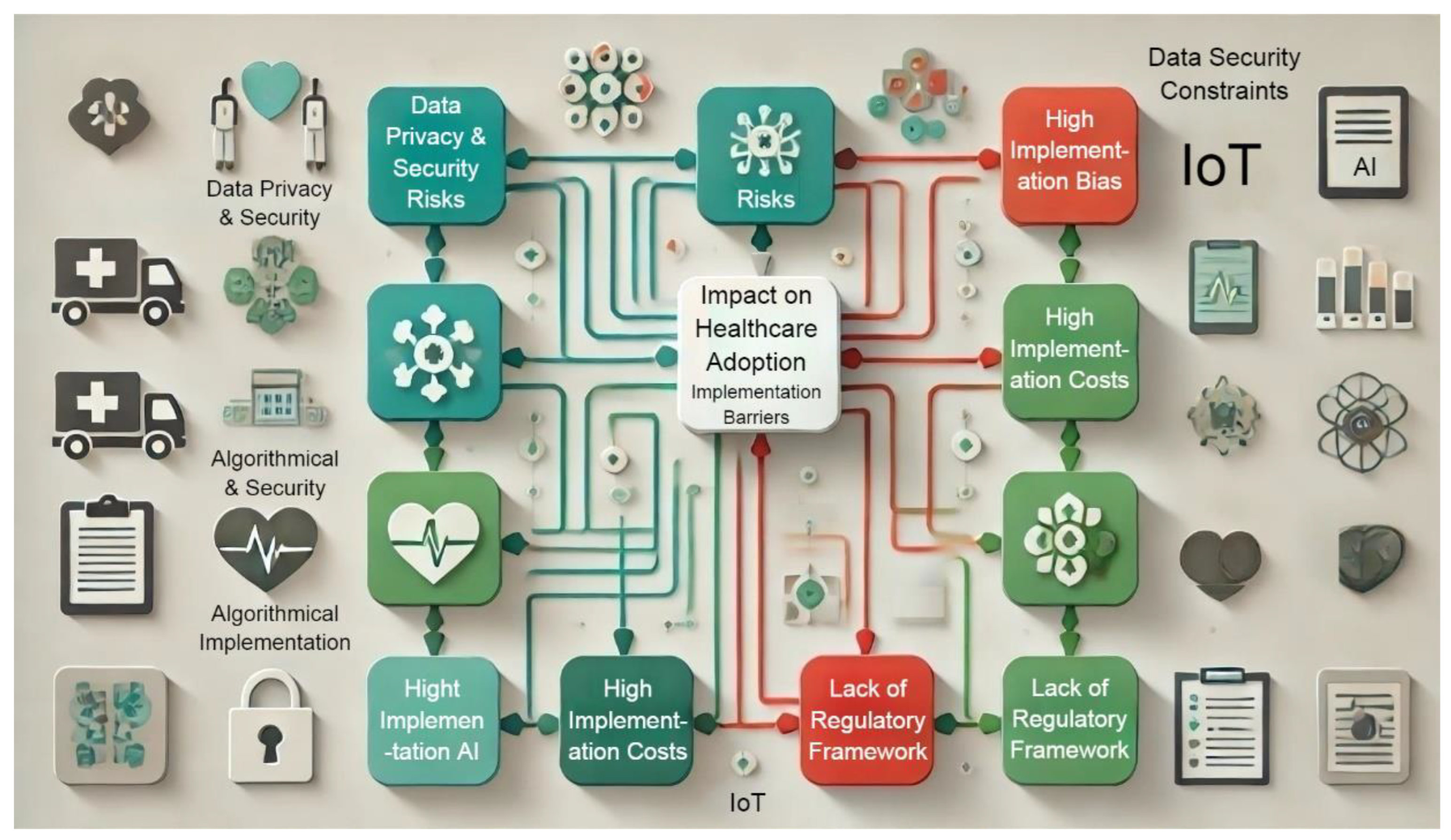
4.4. Challenges and Limitations
- Data Privacy and Security: 30% of studies raised concerns about data security risks associated with IoT devices, highlighting the need for better security protocols.
- Algorithmic Bias: AI models trained on non-representative datasets exhibited bias, resulting in unequal healthcare outcomes for different demographic groups.
- Cost of Implementation: Initial implementation costs were cited as a barrier in 45% of studies, particularly in low-resource settings, despite the long-term cost-saving benefits.
5. Applications of AI and IoT in Healthcare
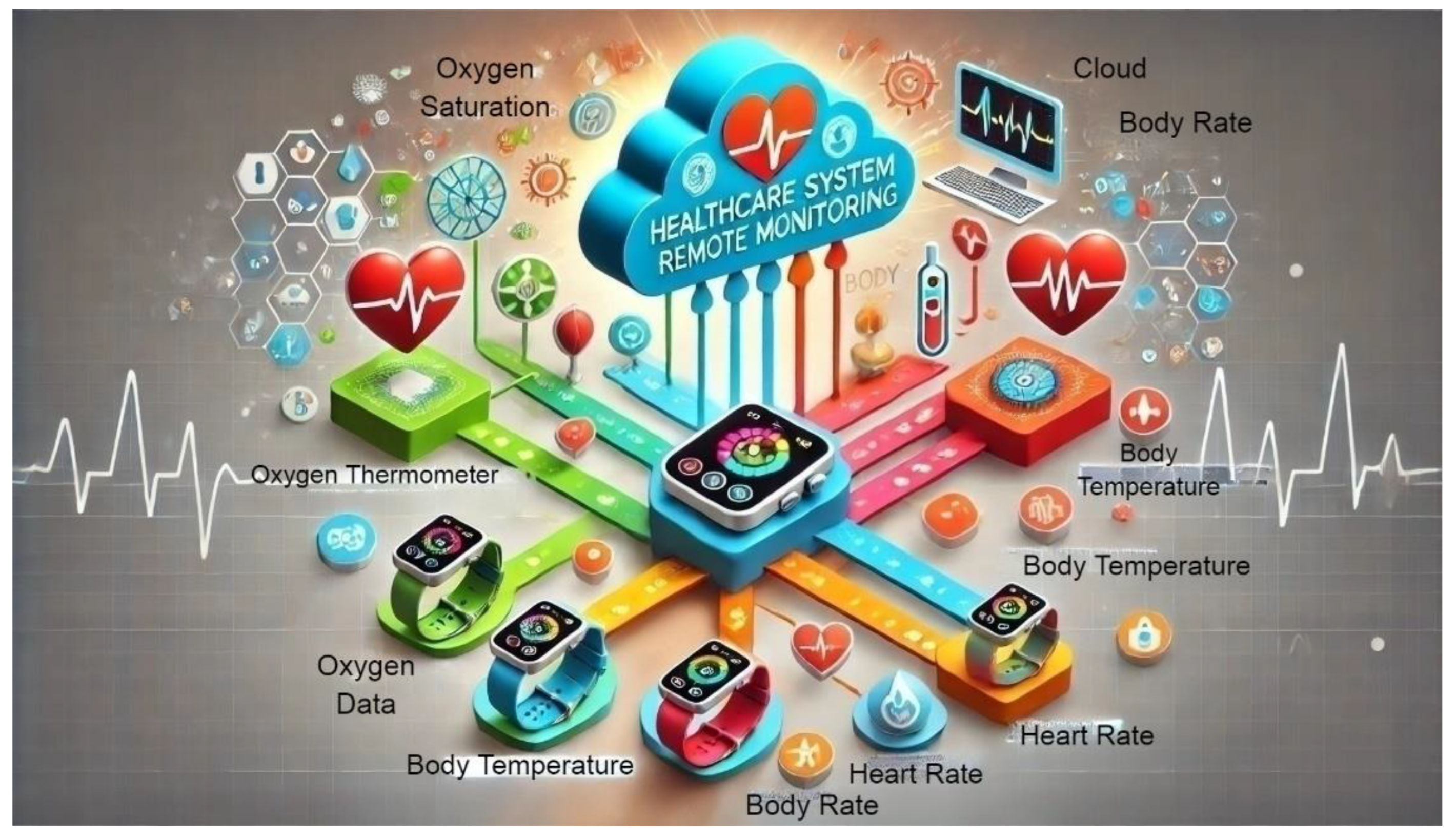
5.1. Smart Healthcare Devices and Remote Monitoring
5.1.1. Wearable Devices for Chronic Disease Management
5.1.2. Remote Monitoring for Elderly and Vulnerable Populations
5.2. Telemedicine and Virtual Healthcare
5.2.1. IoT-Enabled Remote Consultations
5.2.2. AI-Driven Telemedicine Platforms
5.3. AI-Enhanced Diagnostics and Imaging
5.3.1. Medical Imaging and AI Algorithms
5.3.2. Predictive Analytics for Early Detection
5.4. Smart Hospitals and Healthcare Automation
5.4.1. Real-Time Patient Monitoring and Alerts
5.4.2. Automation of Administrative and Logistical Tasks
5.5. Future Potential and Emerging Applications
6. Case Studies of AI and IoT in Chronic Disease Management
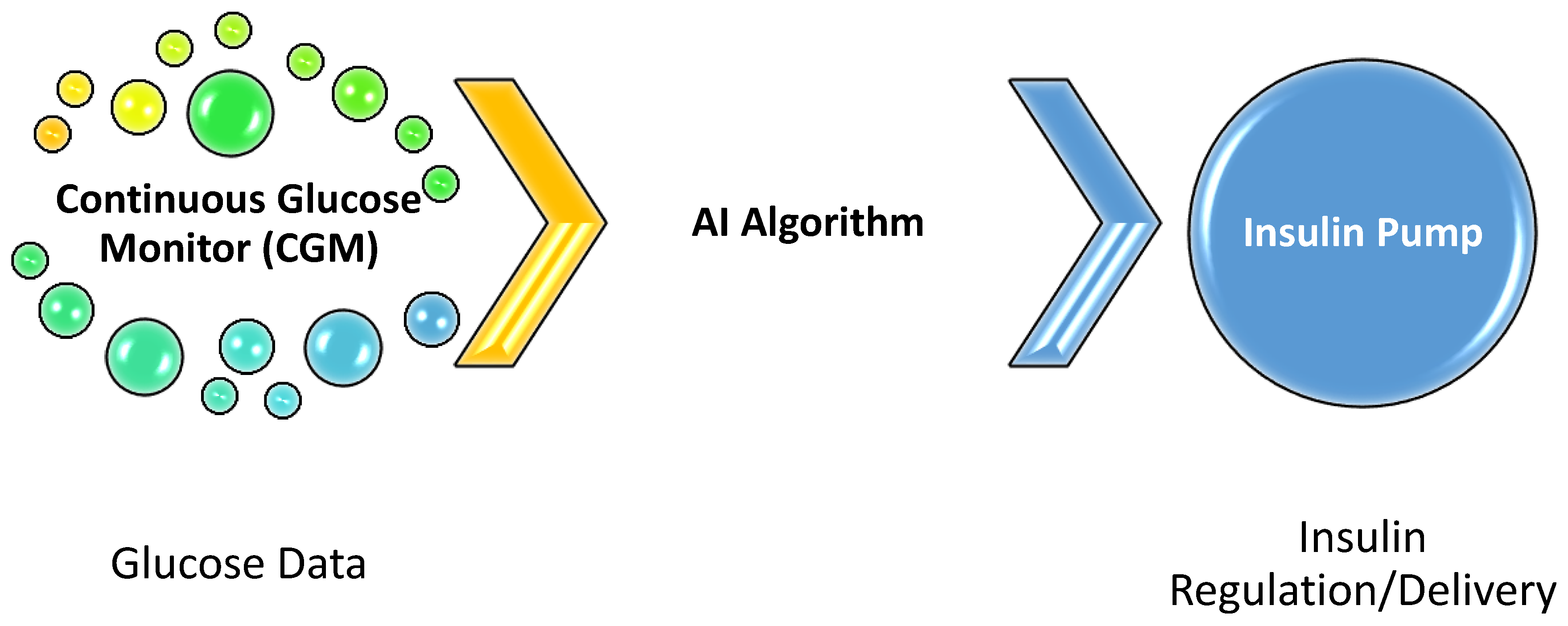
6.1. AI-Driven Continuous Glucose Monitoring for Diabetes
6.2. AI and IoT for Cardiovascular Disease Management
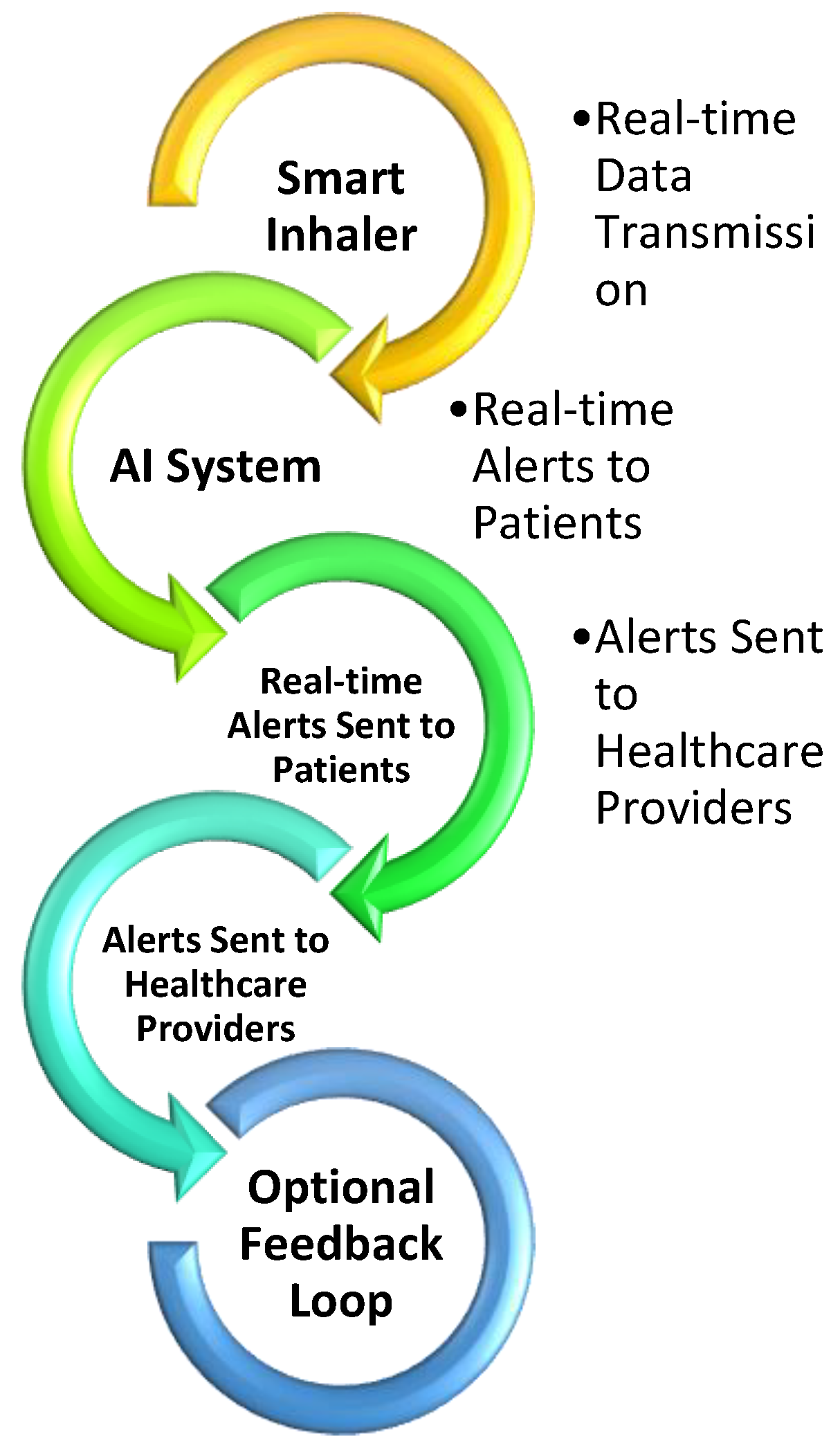
6.3. COPD Management Through IoT-Connected Smart Inhalers
6.4. Remote Monitoring and AI in Heart Failure Management
6.5. AI and IoT for Chronic Kidney Disease (CKD) Management
7. Discussion
8. Challenges and Limitations of AI and IoT Integration in Healthcare
8.1. Data Privacy, Security, and Ethical Concerns
8.2. Interoperability and Integration with Existing Systems
8.3. Algorithmic Bias and Generalizability
8.4. Regulatory and Legal Challenges
8.5. Cost and Accessibility Barriers
9. Future Directions
9.1. Multi-Dimensional Data Integration: Genomics, Biomarkers, and Beyond
9.2. Real-Time Predictive Analytics and Decision Support
9.3. Enhancing Scalability and Accessibility of AI-IoT Systems
9.4. Advanced AI Learning Models and Personalization
9.5. Ethical AI and Governance
9.6. Cross-Disease Applications and Multi-Morbidity Management
10. Conclusions
References
- Aftab, M. , et al., Advancements and Challenges in Artificial Intelligence Applications in Healthcare Delivery Systems. 2024.
- Moharana, M. , et al., Smart Healthcare Systems in Combating Infectious Diseases Outbreaks, in Smart Medical Imaging for Diagnosis and Treatment Planning. 2025, Chapman and Hall/CRC. p. 157-175.
- Shafik, W. , Artificial Intelligence-Enabled Internet of Medical Things (AIoMT) in Modern Healthcare Practices, in Clinical Practice and Unmet Challenges in AI-Enhanced Healthcare Systems. 2024, IGI Global. p. 42-69.
- Singh, P. , AI Strategies for Delivering Better Value in the Healthcare Sector, in Revolutionizing the Healthcare Sector with AI. 2024, IGI Global. p. 131-156.
- Thakare, V., G. Khire, and M. Kumbhar, Artificial intelligence (AI) and internet of things (IoT) in healthcare: Opportunities and challenges. ECS Transactions, 2022. 107(1): p. 7941.
- Yekaterina, K. , Challenges and Opportunities for AI in Healthcare. International Journal of Law and Policy, 2024. 2(7): p. 11-15.
- Abatal, A. , et al., Intelligent Interconnected Healthcare System: Integrating IoT and Big Data for Personalized Patient Care. International Journal of Online & Biomedical Engineering, 2024. 20(11).
- Bagesh Kumar, Y.V.S.R. , Rishik Gupta, Thakur Amrita Singh, Prakhar Shukla, Pratiksh Kumar, Smart healthcare system, in Explainable Artificial Intelligence for Biomedical and Healthcare Applications. 2024. p. 31-49.
- Maqbool, S. , et al. IoT based remote patient monitoring system. in 2020 International Conference on Decision Aid Sciences and Application (DASA). 2020. IEEE.
- Ramalakshmi, K. , et al., Enhancing Healthcare Through Remote Patient Monitoring Using Internet of Things, in Technologies for Sustainable Healthcare Development. 2024, IGI Global. p. 133-146.
- Singh, B.N., A. Singh, and K.A. Gautam, IoT-based Effective Wearable Healthcare Monitoring System for Remote Areas, in Smart Healthcare Systems. 1990, CRC Press. p. 85-104.
- Srinivasaiah, B. , Transformative Wearables: How AI and ML are Shaping Healthcare Innovations.
- Sheth, V. , et al., Schematized Study for Tackling COVID-19 with Machine Learning (ML), Artificial Intelligence (AI), and Internet of Things (IoT). Intelligent Pharmacy, 2024.
- Kavitha, V. , et al. A Comprehensive Survey of IoT Applications in Remote Patient Monitoring, Chronic Disease Management, and Smart Healthcare Infrastructure. in 2024 3rd International Conference on Sentiment Analysis and Deep Learning (ICSADL). 2024. IEEE.
- Suárez, Y.S., A. M. Alawi, and S.E.L. Ricardo, Hospital processes optimization based on artificial intelligence. LatIA, 2023. 1: p. 19-19.
- Faramarzi, S. , et al., Investigating the role of machine learning techniques in internet of things during the COVID-19 pandemic: A systematic review. Informatics in Medicine Unlocked, 2024: p. 101453.
- Jacob, L., K. Thomas, and S. Shukla, Potential Applications of AI and IoT Collaborative Framework for Health Care. The Role of AI, IoT and Blockchain in Mitigating the Impact of COVID-19, 2023: p. 69.
- Aware, M.S. , et al., Integrating AI, Machine Learning, and IoT Technologies for Enhanced Communication and Medical Applications, in Ensuring Security and End-to-End Visibility Through Blockchain and Digital Twins. 2024, IGI Global. p. 251-265.
- Maleki Varnosfaderani, S. and M. Forouzanfar, The role of AI in hospitals and clinics: transforming healthcare in the 21st century. Bioengineering, 2024. 11(4): p. 337.
- Olawade, D.B. , et al., Artificial intelligence in healthcare delivery: Prospects and pitfalls. Journal of Medicine, Surgery, and Public Health, 2024: p. 100108.
- Udegbe, F.C. , et al., The role of artificial intelligence in healthcare: A systematic review of applications and challenges. International Medical Science Research Journal, 2024. 4(4): p. 500-508.
- Thottempudi, P. and V. Kumar, The Role of IoT in Modern Healthcare: Innovations and Challenges in Pandemic Era, in Technologies for Sustainable Healthcare Development. 2024, IGI Global. p. 57-80.
- Ziadi, F., H. Fourati, and L.A. Saidane, AI and IoT Uses, Challenges and Opportunities for e-Health: a review. 2024 International Wireless Communications and Mobile Computing (IWCMC), 2024: p. 873-878.
- Shamshirband, S. , et al., A review on deep learning approaches in healthcare systems: Taxonomies, challenges, and open issues. Journal of Biomedical Informatics, 2021. 113: p. 103627.
- Ellahham, S. , Artificial intelligence: the future for diabetes care. The American journal of medicine, 2020. 133(8): p. 895-900.
- Rghioui, A. , et al. A smart architecture for diabetic patient monitoring using machine learning algorithms. in Healthcare. 2020. MDPI.
- WHO. Noncommunicable diseases. 2021; Available from: https://www.who.int/news-room/factsheets/ detail/noncommunicable-diseases.
- Sriram, R.D. and S.S.K. Reddy, Artificial intelligence and digital tools: future of diabetes care. Clinics in Geriatric Medicine, 2020. 36(3): p. 513-525.
- Vettoretti, M. , et al., Advanced diabetes management using artificial intelligence and continuous glucose monitoring sensors. Sensors, 2020. 20(14): p. 3870.
- Chan, K.S. , et al., Clinical validation of an artificial intelligence-enabled wound imaging mobile application in diabetic foot ulcers. International wound journal, 2022. 19(1): p. 114-124.
- Chowdhury, R.H. , Intelligent systems for healthcare diagnostics and treatment. World Journal of Advanced Research and Reviews, 2024. 23(1): p. 007-015.
- Shaheen, M.Y. , Applications of Artificial Intelligence (AI) in healthcare: A review. ScienceOpen Preprints, 2021.
- Gupta, P. and M.K. Pandey, Role of AI for Smart Health Diagnosis and Treatment, in Smart Medical Imaging for Diagnosis and Treatment Planning. 2024, Chapman and Hall/CRC. p. 23-45.
- Vasudevan, V., U. S. Mohan, and M.S. Gounder, AI-Powered Internet of Medical Things for Monitoring Elderly Adults in Independent Living Environments, in Smart Healthcare Systems. CRC Press. p. 289-303.
- Harshavardhanan, P., P. Suman, and S.S. Ghosh, IoT as Wearable Device in Smart Healthcare Systems: A New Paradigm, in Technologies for Sustainable Healthcare Development. 2024, IGI Global. p. 81-96.
- Manimegalai, D. , et al., AIoT-Powered Intelligent Remote Patient Activity Tracking and Comprehensive Vital Sign Analysis System for Enhanced Healthcare, in Technologies for Sustainable Healthcare Development. 2024, IGI Global. p. 147-173.
- He, W., Z. J. Zhang, and W. Li, Information technology solutions, challenges, and suggestions for tackling the COVID-19 pandemic. International journal of information management, 2021. 57: p. 102287.
- Barnawi, A. , et al., Artificial intelligence-enabled Internet of Things-based system for COVID-19 screening using aerial thermal imaging. Future Generation Computer Systems, 2021. 124: p. 119-132.
- De Boer, B. and O. Kudina, What is morally at stake when using algorithms to make medical diagnoses? Expanding the discussion beyond risks and harms. Theoretical Medicine and Bioethics, 2021. 42(5): p. 245-266.
- Zhu, Y. , et al., M $^ 3$ Fair: Mitigating Bias in Healthcare Data through Multi-Level and Multi-Sensitive-Attribute Reweighting Method. arXiv preprint. arXiv:2306.04118, 2023.
- HEckErmAN, D. , Healthcare delivery in developing countries: Challenges and potential solutions. F our T h P aradigm, 2009: p. 65.
- Mbangula, D.K. , Adopting of artificial intelligence and development in developing countries: perspective of economic transformation, in Handbook of Research on Connecting Philosophy, Media, and Development in Developing Countries. 2022, IGI Global. p. 276-288.
- Oak, M. , A review on barriers to implementing health informatics in developing countries. Journal of Health Informatics in developing countries, 2007. 1(1).
- Qadir, J. , et al., IEEE access special section editorial: health informatics for the developing world. IEEE Access, 2017. 5: p. 27818-27823.
- Rudd, J. and C. Igbrude, A global perspective on data powering responsible AI solutions in health applications. AI and Ethics, 2023: p. 1-11.
- Murdoch, B. , Privacy and artificial intelligence: challenges for protecting health information in a new era. BMC Medical Ethics, 2021. 22: p. 1-5.
- Rohringer, T.J., A. Budhkar, and F. Rudzicz, Privacy versus artificial intelligence in medicine. University of Toronto Medical Journal,[sl], 2019. 96(1): p. 51-53.
- Gerke, S., T. Minssen, and G. Cohen, Ethical and legal challenges of artificial intelligence-driven healthcare, in Artificial intelligence in healthcare. 2020, Elsevier. p. 295-336.
- Pasricha, S. , AI ethics in smart healthcare. IEEE Consumer Electronics Magazine, 2022. 12(4): p. 12-20.
- Page, M.J. , et al., The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. bmj, 2021. 372.
- ANDERSON III, E.V. , et al., Systems and methods for managing chronic disease using analyte and patient data. 2018, Google Patents.
- Mansour, M., M. S. Darweesh, and A. Soltan, Wearable devices for glucose monitoring: A review of state-of-the-art technologies and emerging trends. Alexandria Engineering Journal, 2024. 89: p. 224-243.
- Qureshi, M.R.A. , et al., Using Artificial Intelligence to Improve the Accuracy of a Wrist-Worn, Noninvasive Glucose Monitor: A Pilot Study. Journal of Diabetes Science and Technology, 2024: p. 19322968241252819.
- Tarumi, S. , et al., Leveraging artificial intelligence to improve chronic disease care: methods and application to pharmacotherapy decision support for type-2 diabetes mellitus. Methods of Information in Medicine, 2021. 60(S 01): p. e32-e43.
- Dadkhah, M. , et al., Use of internet of things for chronic disease management: an overview. Journal of Medical Signals & Sensors, 2021. 11(2): p. 138-157.
- Mahajan, S. and A. Birajdar. IoT based smart health monitoring system for chronic diseases. in 2019 IEEE Pune Section International Conference (PuneCon). 2019. IEEE.
- Nagarajan, V.D. , et al., Artificial intelligence in the diagnosis and management of arrhythmias. European heart journal, 2021. 42(38): p. 3904-3916.
- Siontis, K.C. , et al., Artificial intelligence-enhanced electrocardiography in cardiovascular disease management. Nature Reviews Cardiology, 2021. 18(7): p. 465-478.
- Mishra, D., P. Singh, and S. Agarwal, AI-and IoT-based architecture in healthcare, in Transformation in Healthcare with Emerging Technologies. 2022, Chapman and Hall/CRC. p. 1-18.
- Ma, Y. , et al. Artificial intelligence chronic disease management system based on medical resource perception. in International Conference on Artificial Intelligence and Security. 2021. Springer.
- Shah, R. and A. Chircu, IoT and AI in healthcare: A systematic literature review. Issues in Information Systems, 2018. 19(3).
- Gupta, M. , et al. Real time interaction-based Healthcare monitoring during Medical Emergencies with Internet of Things. in 2022 2nd International Conference on Advance Computing and Innovative Technologies in Engineering (ICACITE). 2022. IEEE.
- Diraco, G., A. Leone, and P. Siciliano, Ai-based early change detection in smart living environments. Sensors, 2019. 19(16): p. 3549.
- Adhikary, T. , et al., The internet of things (iot) augmentation in healthcare: An application analytics. ICICCT 2019–System Reliability, Quality Control, Safety, Maintenance and Management: Applications to Electrical, Electronics and Computer Science and Engineering, 2020: p. 576-583.
- Rathee, G. , et al., ANN assisted-IoT enabled COVID-19 patient monitoring. Ieee Access, 2021. 9: p. 42483-42492.
- Rogers, R. , Internet of things-based smart healthcare systems, wireless connected devices, and body sensor networks in COVID-19 remote patient monitoring. American journal of medical research, 2021. 8(1): p. 71-80.
- Balica, R.-S. , Networked wearable devices, machine learning-based real-time data sensing and processing, and internet of medical things in COVID-19 diagnosis, prognosis, and treatment. American Journal of Medical Research, 2022. 9(1): p. 33-48.
- Ponnusamy, V. , et al., Smart healthcare technologies for massive internet of medical things, in Efficient Data Handling for Massive Internet of Medical Things: Healthcare Data Analytics. 2021, Springer. p. 71-101.
- Reddy, J.E.P. , et al. AI-IoT based healthcare prognosis interactive system. in 2020 IEEE International Conference for Innovation in Technology (INOCON). 2020. IEEE.
- Revathi, K. , et al., IoT Based Pulse Oximeter for Remote Health Assessment: Design, Challenges and Futuristic Scope. IJEER, 2022. 10(3): p. 557-563.
- Anjum, K., M. Sameer, and S. Kumar. AI enabled NLP based text to text medical Chatbot. in 2023 3rd International Conference on Innovative Practices in Technology and Management (ICIPTM). 2023. IEEE.
- Athota, L. , et al. Chatbot for healthcare system using artificial intelligence. in 2020 8th International conference on reliability, infocom technologies and optimization (trends and future directions)(ICRITO). 2020. IEEE.
- Ansari, M. , et al., AI-based diagnosis techniques for cardiac disease analysis and predictions, in Image Processing for Automated Diagnosis of Cardiac Diseases. 2021, Elsevier. p. 133-155.
- Erickson, B.J. , et al., Machine learning for medical imaging. radiographics, 2017. 37(2): p. 505-515.
- Hosny, A. , et al., Artificial intelligence in radiology. Nature Reviews Cancer, 2018. 18(8): p. 500-510.
- McBee, M.P. , et al., Deep learning in radiology. Academic radiology, 2018. 25(11): p. 1472-1480.
- Esteva, A. , et al., A guide to deep learning in healthcare. Nature medicine, 2019. 25(1): p. 24-29.
- Johnson, K.W. , et al., Artificial intelligence in cardiology. Journal of the American College of Cardiology, 2018. 71(23): p. 2668-2679.
- Rajkomar, A., J. Dean, and I. Kohane, Machine learning in medicine. New England Journal of Medicine, 2019. 380(14): p. 1347-1358.
- Topol, E.J. , High-performance medicine: the convergence of human and artificial intelligence. Nature medicine, 2019. 25(1): p. 44-56.
- Mathur, P. and M.L. Burns, Artificial intelligence in critical care. International anesthesiology clinics, 2019. 57(2): p. 89-102.
- Rahman, M.S. , et al., Artificial Intelligence-Based Algorithms and Healthcare Applications of Respiratory Inductance Plethysmography: A Systematic Review. Algorithms, 2024. 17(6): p. 261.
- Rghioui, A. and A. Oumnad, Internet of things: visions, technologies, and areas of application. Automation, Control and Intelligent Systems, 2017. 10(2): p. 83-91.
- Aceto, G., V. Persico, and A. Pescapé, The role of Information and Communication Technologies in healthcare: taxonomies, perspectives, and challenges. Journal of Network and Computer Applications, 2018. 107: p. 125-154.
- Desautels, T. , et al., Prediction of sepsis in the intensive care unit with minimal electronic health record data: a machine learning approach. JMIR medical informatics, 2016. 4(3): p. e5909.
- Topol, E. , Deep medicine: how artificial intelligence can make healthcare human again. 2019: Hachette UK.
- Wong, A.-K.I. , et al., Machine learning methods to predict acute respiratory failure and acute respiratory distress syndrome. Frontiers in big Data, 2020. 3: p. 579774.
- Kumar, M. , et al., Healthcare Internet of Things (H-IoT): Current trends, future prospects, applications, challenges, and security issues. Electronics, 2023. 12(9): p. 2050.
- Malik, N. , et al., A comprehensive review of blockchain applications in industrial Internet of Things and supply chain systems. Applied Stochastic Models in Business and Industry, 2021. 37(3): p. 391-412.
- Mansour, R.F. , et al., Artificial intelligence and internet of things enabled disease diagnosis model for smart healthcare systems. IEEE Access, 2021. 9: p. 45137-45146.
- Munavalli, J.R. , et al., Real-time capacity management and patient flow optimization in hospitals using AI methods. Artificial intelligence and Data mining in healthcare, 2021: p. 55-69.
- Rghioui, A. and A. Oumnad, Challenges and Opportunities of Internet of Things in Healthcare. International Journal of Electrical & Computer Engineering (2088-8708), 2018. 8(5).
- Chen, M. , et al., Disease prediction by machine learning over big data from healthcare communities. Ieee Access, 2017. 5: p. 8869-8879.
- Contreras, I. and J. Vehi, Artificial intelligence for diabetes management and decision support: literature review. Journal of medical Internet research, 2018. 20(5): p. e10775.
- Mohr, D.C., M. Zhang, and S.M. Schueller, Personal sensing: understanding mental health using ubiquitous sensors and machine learning. Annual review of clinical psychology, 2017. 13(1): p. 23-47.
- Haidar, A. , et al., Comparison of dual-hormone artificial pancreas, single-hormone artificial pancreas, and conventional insulin pump therapy for glycaemic control in patients with type 1 diabetes: an open-label randomised controlled crossover trial. The lancet Diabetes & endocrinology, 2015. 3(1): p. 17-26.
- Hickey, K.T. , et al., Precision health: Advancing symptom and self-management science. Nursing Outlook, 2019. 67(4): p. 462-475.
- Akduman, S. and K. Yilmaz, Examining the effectiveness of artificial intelligence applications in asthma and COPD outpatient support in terms of patient health and public cost: SWOT analysis. Medicine, 2024. 103(29): p. e38998.
- Margam, R. , SMART INHALERS: HARNESSING IOT FOR PRECISE ASTHMA MANAGEMENT. 2024.
- Alex, S.A. , et al. Intelligent Medication Compliance System for Patients Using IoT. in 2024 7th International Conference on Information and Computer Technologies (ICICT). 2024. IEEE.
- Stehlik, J. , et al., Continuous wearable monitoring analytics predict heart failure hospitalization: the LINK-HF multicenter study. Circulation: Heart Failure, 2020. 13(3): p. e006513.
- Rovin, B.H. , et al., KDIGO 2021 clinical practice guideline for the management of glomerular diseases. Kidney international, 2021. 100(4): p. S1-S276.
- Institute, P. The Cost of a Data Breach Report 2020. 2020; Available from: https://www.ibm.com/security/data-breach.
- Karunarathne, S.M., N. Saxena, and M.K. Khan, Security and privacy in IoT smart healthcare. IEEE Internet Computing, 2021. 25(4): p. 37-48.
- Commission, E. General Data Protection Regulation (GDPR). 2018; Available from: https://gdpr.eu/.
- Catalyst, N. , Healthcare big data and the promise of value-based care. NEJM Catalyst, 2018. 4(1).
- Obermeyer, Z. , et al., Dissecting racial bias in an algorithm used to manage the health of populations. Science, 2019. 366(6464): p. 447-453.
- Challen, R. , et al., Artificial intelligence, bias and clinical safety. BMJ quality & safety, 2019. 28(3): p. 231-237.
- FDA. AI/ML-Based Software as a Medical Device (SaMD): Action Plan. 2021; Available from: https://www.fda.gov/.
- Li, X. , et al., Digital health: tracking physiomes and activity using wearable biosensors reveals useful health-related information. PLoS biology, 2017. 15(1): p. e2001402.
- Collins, F.S. and H. Varmus, A new initiative on precision medicine. New England journal of medicine, 2015. 372(9): p. 793-795.
- Azar Abbas, N.A. , Digital Health Solutions and Machine Learning Algorithms: A New Era in Chronic Disease Management.
- Floridi, L. , et al., AI4People—an ethical framework for a good AI society: opportunities, risks, principles, and recommendations. Minds and machines, 2018. 28: p. 689-707.
| Application | AI Component | IoT Device | Impact | References |
|---|---|---|---|---|
| Diabetes Management | Machine learning algorithms for glucose prediction | Continuous glucose monitors (CGMs) | Improved glycemic control via AI-driven insulin regulation. | [5,31,32] |
| Cardiovascular Monitoring | AI-based predictive analytics for detecting arrhythmias | Wearable ECG monitors | Early detection and intervention, reducing mortality risk. | [32,33,34] |
| Hypertension Management | AI algorithms for blood pressure prediction | Blood pressure cuffs linked with IoT | Automated detection of anomalies, enabling timely interventions. | [5,35,36] |
| Elderly Care | AI-powered fall detection and health tracking | IoT sensors in homes, wearable devices | Reduced emergency hospital visits, immediate alerts to caregivers. | [33,34,36] |
| Challenge | Description | Impact | References |
|---|---|---|---|
| Data Privacy and Security | Risks of data breaches and hacking of IoT devices. | Compromised patient confidentiality and trust in systems. | [46,47] |
| Algorithmic Bias | AI systems may yield inaccurate results for non-representative patient datasets. | Exacerbates healthcare inequalities, reduces diagnosis accuracy. | [48,49] |
| Cost of Implementation | High costs for AI and IoT deployment, particularly in low-resource settings. | Slows adoption, widens the technology gap between developed and developing regions. | [5] |
| Regulatory Issues | Lack of standardization and clear regulations for AI and IoT in healthcare. | Delays in implementation and inconsistent application across regions. | [48] |
| Metric | Number of Studies | Outcome | Statistical Significance |
|---|---|---|---|
| HbA1c reduction in diabetes | 40 | 0.9% average reduction in HbA1c levels | p ~ 0.01 |
| Reduction in hospital admissions | 40 | 15% fewer admissions due to better glucose control | p ~ 0.02 |
| Early detection of cardiovascular events | 25 | 25% improvement in detection rates using AI-based ECGs | p ~ 0.03 |
| Diagnosis time reduction (CVD) | 25 | 20-30% faster diagnosis with AI-enhanced tools | p ~ 0.04 |
| Metric | Number of Studies | Outcome | Statistical Significance |
|---|---|---|---|
| Diagnosis time reduction (COVID-19) | 28 | 35% faster diagnosis using AI-driven CT scan analysis | p ~ 0.003 |
| Reduction in hospital admissions | 28 | 20% fewer hospital admissions due to remote patient monitoring | p ~ 0.02 |
| Resource optimization | 28 | 25% increase in hospital resource utilization efficiency | p ~ 0.04 |
| Key Metric | Outcome | Statistical Significance |
|---|---|---|
| Diagnostic accuracy improvement | 15-25% improvement across chronic disease and COVID-19 diagnostics | p < 0.05 |
| Healthcare cost reduction | 15-20% reduction in healthcare costs through IoT remote monitoring | p < 0.05 |
| Patient engagement and adherence | 20% increase in patient adherence to treatment plans using real-time monitoring | p < 0.05 |
| Application | Device/Technology | Outcome/Impact | References |
|---|---|---|---|
| Diabetes Management | Continuous Glucose Monitors (CGMs) | 0.9% reduction in HbA1c | [51-54]] |
| Cardiovascular Disease | AI-Enabled ECG Monitors | 25% improvement in arrhythmia detection | [55,56,57,58] |
| Respiratory Disease | Smart Inhalers and AI-Predictive Systems | Improved adherence and reduced exacerbations | [56,59] |
| Elderly Care | Wearable Fall Detectors, Smart Homes | Faster intervention, real-time monitoring | [59,60,61] |
| Application | Device/Technology | Outcome | References |
|---|---|---|---|
| COVID-19 Monitoring | IoT-Enabled Pulse Oximeters | Reduced hospital admissions | [64,65,66] |
| Remote Consultations | Smart Thermometers, Digital Stethoscopes | Increased diagnostic accuracy by 15% | [66,67,68] |
| Virtual Health Assistants | AI-Powered NLP Systems | Enhanced patient interaction and triaging | [5,69] |
| Disease | AI/IoT Technology | Outcome | References |
|---|---|---|---|
| Diabetes | AI-enhanced CGMs | 0.9% reduction in HbA1c, fewer hypoglycemic episodes | [96] |
| Cardiovascular Disease | AI-enabled wearable ECG monitors | 32% improvement in early arrhythmia detection, 93% accuracy, fewer hospitalizations | [97] |
| COPD | IoT-connected smart inhalers | 30-40% reduction in hospital admissions | [98,99] |
| COPD | IoT-connected smart inhalers | 15-20% improvement in medication adherence | [99,100] |
| Heart Failure | AI-powered remote monitoring system | 20% reduction in hospital readmissions | [101] |
| Chronic Kidney Disease | IoT-enabled sensors with AI predictive analytics | 30% slower disease progression | [102] |
| Region | Adoption of FHIR Standards | % of Healthcare Systems with Legacy Infrastructure | Integration with EHRs (%) |
|---|---|---|---|
| North America | High | 40% | 70% |
| Europe | Moderate | 50% | 65% |
| Asia-Pacific | Low | 70% | 40% |
| Africa | Very Low | 85% | 20% |
| Source of Bias | Impact on AI Performance | Mitigation Strategy |
|---|---|---|
| Underrepresentation of Minority Populations | Reduced accuracy in diverse patient groups | Inclusion of diverse training datasets |
| Homogeneous Clinical Trials | Inability to generalize predictions to real-world settings | Real-world evidence and continuous learning models |
| Socioeconomic Disparities | Biased access to care in underserved areas | Incorporation of social determinants of health into models |
| Data Type | Application in AI-IoT Systems | Potential Impact on COPD Management |
|---|---|---|
| Genomic Data | Predict disease susceptibility and personalize treatments | Precision medicine for COPD; tailored therapeutic interventions |
| Biomarkers | Monitor disease severity and predict exacerbations | Early detection of exacerbations and improved treatment outcomes |
| Environmental Data | Analyze external factors (e.g., air quality, weather) | Contextual insights for COPD management, minimizing environmental triggers |
| Challenge | Proposed Solution | Long-Term Impact |
|---|---|---|
| High cost of IoT devices | Development of affordable, modular IoT devices | Broader access in low-resource settings |
| Lack of interoperability | Global adoption of open standards (e.g., FHIR) | Seamless data exchange between healthcare systems |
| Infrastructure limitations | Use of cloud-based AI analytics and decentralized computing | Scalable AI solutions for under-resourced facilities |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




