Submitted:
27 September 2024
Posted:
30 September 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
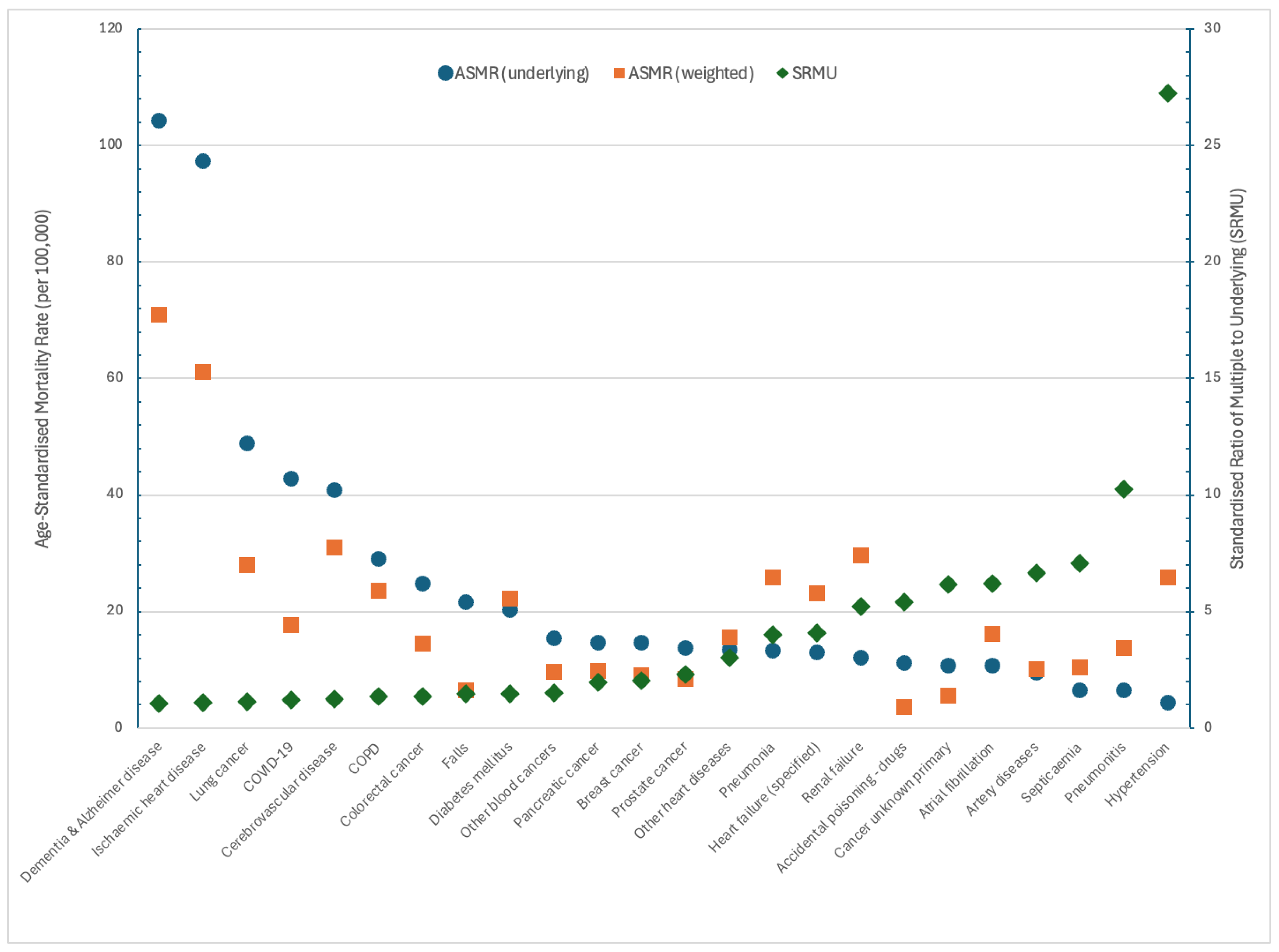
| Rank | Cause of Death | ASMR | Change | Cause of Death | ASMRw1 |
|---|---|---|---|---|---|
| 1 | Dementia & Alzheimer’s disease | 104.24 | 0 | Dementia & Alzheimer’s disease | 79.98 |
| 2 | Ischemic heart disease | 97.29 | 0 | Ischemic heart disease | 71.45 |
| 3 | Lung cancer | 48.87 | 2 | Cerebrovascular disease | 33.66 |
| 4 | COVID-19 | 42.86 | −1 | Lung cancer | 32.79 |
| 5 | Cerebrovascular disease | 40.88 | 1 | COPD | 25.48 |
| 6 | COPD | 29.09 | −2 | COVID-19 | 24.88 |
| 7 | Colorectal cancer | 24.79 | 10 | Renal failure | 23.86 |
| 8 | Falls | 21.68 | 7 | Pneumonia | 22.97 |
| 9 | Diabetes mellitus | 20.32 | 0 | Diabetes mellitus | 22.32 |
| 10 | Other blood cancers | 15.43 | n/a | Cancer secondary site | 20.81 |
| 11 | Pancreatic cancer | 14.70 | 5 | Heart failure (specified) | 20.05 |
| 12 | Breast cancer | 14.64 | 50 | Hypertension | 18.99 |
| 13 | Prostate cancer | 13.69 | −6 | Colorectal cancer | 17.00 |
| 14 | Other heart diseases | 13.45 | 0 | Other heart diseases | 14.90 |
| 15 | Pneumonia | 13.3 | 5 | Atrial fibrillation | 14.12 |
| 16 | Heart failure (specified) | 12.99 | 36 | Pneumonitis | 12.18 |
| 17 | Renal failure | 12.08 | −9 | Falls | 11.40 |
| 18 | Accidental poisoning—drugs | 11.17 | −8 | Other blood cancers | 11.16 |
| 19 | Cancer unknown primary | 10.78 | −8 | Pancreatic cancer | 10.70 |
| 20 | Atrial fibrillation | 10.67 | −8 | Breast cancer | 10.42 |
| Change | Cause of Death | ASMRw2 | Change | Cause of Death | ASMRw3 |
|---|---|---|---|---|---|
| 0 | Dementia & Alzheimer’s disease | 70.92 | 0 | Dementia & Alzheimer’s disease | 78.16 |
| 0 | Ischemic heart disease | 61.06 | 0 | Ischemic heart disease | 68.57 |
| 2 | Cerebrovascular disease | 31.03 | 2 | Cerebrovascular disease | 33.16 |
| 13 | Renal failure | 29.68 | −1 | Lung cancer | 32.9 |
| -2 | Lung cancer | 27.98 | 12 | Renal failure | 26.35 |
| 9 | Pneumonia | 25.93 | 0 | COPD | 24.59 |
| 55 | Hypertension | 25.8 | −3 | COVID-19 | 23.03 |
| n/a | Cancer secondary site | 25.77 | 7 | Pneumonia | 22.98 |
| -3 | COPD | 23.63 | 53 | Hypertension | 21.61 |
| 6 | Heart failure (specified) | 23.2 | −1 | Diabetes mellitus | 21.46 |
| -2 | Diabetes mellitus | 22.28 | 5 | Heart failure (specified) | 21.26 |
| -8 | COVID-19 | 17.74 | n/a | Cancer secondary site | 19.32 |
| 7 | Atrial fibrillation | 16.2 | −6 | Colorectal cancer | 16.93 |
| 0 | Other heart diseases | 15.5 | 6 | Atrial fibrillation | 15.36 |
| -8 | Colorectal cancer | 14.53 | −1 | Other heart diseases | 15.04 |
| 36 | Pneumonitis | 13.79 | 36 | Pneumonitis | 12.01 |
| 33 | Septicemia | 10.46 | −7 | Other blood cancers | 10.91 |
| 23 | Artery diseases | 10.11 | −7 | Pancreatic cancer | 10.81 |
| -8 | Pancreatic cancer | 9.84 | −7 | Breast cancer | 10.43 |
| -10 | Other blood cancers | 9.59 | 21 | Artery diseases | 10.13 |
4. Discussion
5. Conclusions
Author Contributions
Acknowledgments
Funding:
Institutional Review Board Statement
Data Availability Statement
Conflicts of Interest
References
- World Health Organization Global Health Estimates: Leading Causes of Death. Available online: https://www.who.int/data/gho/data/themes/mortality-and-global-health-estimates/ghe-leading-causes-of-death (accessed on 23 September 2024).
- Gerhardt, T.; Gerhardt, L.M.S.; Ouwerkerk, W.; Roth, G.A.; Dickstein, K.; Collins, S.P.; Cleland, J.G.F.; Dahlstrom, U.; Tay, W.T.; Ertl, G.; et al. Multimorbidity in Patients with Acute Heart Failure across World Regions and Country Income Levels (REPORT-HF): A Prospective, Multicentre, Global Cohort Study. Lancet Glob. Heal. 2023, 11, e1874–e1884. [Google Scholar] [CrossRef] [PubMed]
- Tran, J.; Norton, R.; Conrad, N.; Rahimian, F.; Canoy, D.; Nazarzadeh, M.; Rahimi, K. Patterns and Temporal Trends of Comorbidity among Adult Patients with Incident Cardiovascular Disease in the UK between 2000 and 2014: A Population-Based Cohort Study. PLoS Med. 2018, 15, e1002513. [Google Scholar] [CrossRef] [PubMed]
- Rahimi, K.; Lam, C.S.P.; Steinhubl, S. Cardiovascular Disease and Multimorbidity: A Call for Interdisciplinary Research and Personalized Cardiovascular Care. PLoS Med. 2018, 15, e1002545. [Google Scholar] [CrossRef]
- Désesquelles, A.; Salvatore, M.A.; Frova, L.; Pace, M.; Pappagallo, M.; Meslé, F.; Egidi, V. Revisiting the Mortality of France and Italy with the Multiple-Cause-of-Death Approach. Demogr. Res. 2010, 23, 771–806. [Google Scholar] [CrossRef]
- Désesquelles, A.; Demuru, E.; Pappagallo, M.; Frova, L.; Meslé, F.; Egidi, V. After the Epidemiologic Transition: A Reassessment of Mortality from Infectious Diseases among over-65s in France and Italy. Int. J. Public Heal. 2015, 60, 961–967. [Google Scholar] [CrossRef]
- Bishop, K.; Moreno-Betancur, M.; Balogun, S.; Eynstone-Hinkins, J.; Moran, L.; Rao, C.; Banks, E.; Korda, R.J.; Gourley, M.; Joshy, G. Quantifying Cause-Related Mortality in Australia, Incorporating Multiple Causes: Observed Patterns, Trends and Practical Considerations. Int. J. Epidemiology 2023, 52, 284–294. [Google Scholar] [CrossRef]
- Fedeli, U.; Schievano, E.; Avossa, F.; Pitter, G.; Amidei, C.B.; Grande, E.; Grippo, F. Different Approaches to the Analysis of Causes of Death during the COVID-19 Epidemic. Eur. Rev. Méd. Pharmacol. Sci. 2021, 25, 3610–3613. [Google Scholar] [CrossRef]
- Santo, A.H. Potencial Epidemiológico Da Utilização Das Causas Múltiplas de Morte Por Meio de Suas Menções Nas Declarações de Óbito, Brasil, 2003. Rev. Panam. Salud Pública 2007, 22, 178–186. [Google Scholar] [CrossRef] [PubMed]
- Santo, A.H. Causas Mal Definidas de Morte e Óbitos Sem Assistência. Revista da Associação Médica Brasileira 2008, 54, 23–28. [Google Scholar] [CrossRef]
- Bishop, K.; Balogun, S.; Eynstone-Hinkins, J.; Moran, L.; Martin, M.; Banks, E.; Rao, C.; Joshy, G. Analysis of Multiple Causes of Death: A Review of Methods and Practices. Epidemiology 2023, 34, 333–344. [Google Scholar] [CrossRef]
- Désesquelles, A.F.; Salvatore, M.A.; Pappagallo, M.; Frova, L.; Pace, M.; Meslé, F.; Egidi, V. Analysing Multiple Causes of Death: Which Methods For Which Data? An Application to the Cancer-Related Mortality in France and Italy. Eur. J. Popul. Rev. Eur. Démographie 2012, 28, 467–498. [Google Scholar] [CrossRef]
- Frova, L.; Salvatore, M.A.; Pappagallo, M.; Egidi, V. The Multiple Cause of Death Approach to Analyse Mortality Patterns. Genus 2009, 1, 1–21. [Google Scholar]
- Santos, D.A.D.; Deutsch, R. The Positive Matching Index: A New Similarity Measure with Optimal Characteristics. Pattern Recognit. Lett. 2010, 31, 1570–1576. [Google Scholar] [CrossRef]
- Piffaretti, C.; Moreno-Betancur, M.; Lamarche-Vadel, A.; Rey, G. Quantifying Cause-Related Mortality by Weighting Multiple Causes of Death. Bull. World Heal. Organ. 2016, 94, 870–879. [Google Scholar] [CrossRef] [PubMed]
- Moreno-Betancur, M.; Sadaoui, H.; Piffaretti, C.; Rey, G. Survival Analysis with Multiple Causes of Death. Epidemiology 2017, 28, 12–19. [Google Scholar] [CrossRef] [PubMed]
- Ukolova, E.; Burcin, B. What Can Multiple Causes of Death Tell about Cardiovascular Mortality during COVID-19 Pandemic in the United States? J. Public Heal. 2024, 46, 97–106. [Google Scholar] [CrossRef]
- Grundy, E.M.; Stuchbury, R. Multimorbidity as Assessed by Reporting of Multiple Causes of Death: Variations by Period, Sociodemographic Characteristics and Place of Death among Older Decedents in England and Wales, 2001–2017. J. Epidemiology Community Heal. 2022, 76, 699–706. [Google Scholar] [CrossRef]
- Trias-Llimós, S.; Permanyer, I. Cause-of-Death Diversity From a Multiple-Cause Perspective in the United States. Demography 2023, 60, 73–98. [Google Scholar] [CrossRef]
- Breger, T.L.; Edwards, J.K.; Cole, S.R.; Saag, M.; Rebeiro, P.F.; Moore, R.D.; Eron, J.J. Estimating a Set of Mortality Risk Functions with Multiple Contributing Causes of Death. Epidemiology 2020, 31, 704–712. [Google Scholar] [CrossRef]
- Fihel, A.; Janicka, A.; Buschner, A.; Ustinavičienė, R.; Trakienė, A. Unrecognised COVID-19 Deaths in Central Europe: The Importance of Cause-of-Death Certification for the COVID-19 Burden Assessment. PLoS ONE 2024, 19, e0307194. [Google Scholar] [CrossRef]
- Fihel, A.; Muszyńska-Spielauer, M. Using Multiple Cause of Death Information to Eliminate Garbage Codes. Demogr. Res. 2021, 45, 345–360. [Google Scholar] [CrossRef]
- Wilkins, K.; Wysocki, M.; Morin, C.; Wood, P. Multiple Causes of Death. Health Reports 1997, 9, 19–29. [Google Scholar]
- Park, J.; Peters, P.A. Mortality from Diabetes Mellitus, 2004 to 2008: A Multiple-Cause-of-Death Analysis. Heal. Rep. 2014, 25, 12–16. [Google Scholar]
- Park, J. Mortality from Alzheimer’s Disease in Canada: A Multiple-Cause-of-Death Analysis Mortality from Alzheimer’s Disease in Canada: A Multiple-Cause-of-Death Analysis, 2004 to 2011; Statistics Canada; 2015; pp. 17–21.
- Statistics Canada Canadian Vital Statistics—Death Database (CVSD). Available online: https://www23.statcan.gc.ca/imdb/p2SV.pl?Function=getSurvey&SDDS=3233 (accessed on 23 September 2024).
- Speizer, F.E.; Trey, C.; Parker, P. The Uses of Multiple Causes of Death Data to Clarify Changing Patterns of Cirrhosis Mortality in Massachusetts. Am. J. Public Heal. 2011, 67, 333–336. [Google Scholar] [CrossRef]
- Creamer, A.W.; Barratt, S.L. Prognostic Factors in Chronic Hypersensitivity Pneumonitis. Eur. Respir. Rev. 2020, 29, 190167. [Google Scholar] [CrossRef] [PubMed]
- Dasgupta, S.; Bhattacharya, A.; Abhijit, R.D.; Chowdhury, S.R.; Chaudhury, K. Risk Factors Associated with Mortality in Hypersensitivity Pneumonitis: A Meta-Analysis. Expert Rev. Respir. Med. 2022, 16, 801–811. [Google Scholar] [CrossRef]
- Rittig, A.H.; Hilberg, O.; Ibsen, R.; Løkke, A. Incidence, Comorbidity and Survival Rate of Hypersensitivity Pneumonitis: A National Population-Based Study. ERJ Open Res. 2019, 5, 00259–02018. [Google Scholar] [CrossRef] [PubMed]
- Kolte, D.; Lakshmanan, S.; Jankowich, M.D.; Brittain, E.L.; Maron, B.A.; Choudhary, G. Mild Pulmonary Hypertension Is Associated with Increased Mortality: A Systematic Review and Meta-Analysis. J. Am. Hear. Assoc. 2018, 7, e009729. [Google Scholar] [CrossRef] [PubMed]
- Gardner, W.M.; Razo, C.; McHugh, T.A.; Hagins, H.; Vilchis-Tella, V.M.; Hennessy, C.; Taylor, H.J.; Perumal, N.; Fuller, K.; Cercy, K.M.; et al. Prevalence, Years Lived with Disability, and Trends in Anaemia Burden by Severity and Cause, 1990–2021: Findings from the Global Burden of Disease Study 2021. Lancet Haematol. 2023, 10, e713–e734. [Google Scholar] [CrossRef]
- Vlagopoulos, P.T.; Tighiouart, H.; Weiner, D.E.; Griffith, J.; Pettitt, D.; Salem, D.N.; Levey, A.S.; Sarnak, M.J. Anemia as a Risk Factor for Cardiovascular Disease and All-Cause Mortality in Diabetes: The Impact of Chronic Kidney Disease. J. Am. Soc. Nephrol. 2005, 16, 3403–3410. [Google Scholar] [CrossRef]
- Omran, A.R. The Epidemiologic Transition: A Theory of the Epidemiology of Population Change. Milbank Q. 2005, 83, 731–757. [Google Scholar] [CrossRef] [PubMed]
- Armstrong, G.L.; Conn, L.A; Pinner, R.W. Trends in Infectious Disease Mortality in the United States during the 20th Century. Journal of the American Medical Association 1999, 281, 61–66. [Google Scholar] [CrossRef] [PubMed]
- Anderson, R.N. International Handbook of Adult Mortality. Int. Handb. Popul. 2011, 467–489. [Google Scholar] [CrossRef]
- Kempker, J.A.; Kramer, M.R.; Waller, L.A.; Martin, G.S. Risk Factors for Septicemia Deaths and Disparities in a Longitudinal US Cohort. Open Forum Infect. Dis. 2018, 5, ofy305. [Google Scholar] [CrossRef]
- Janssen, T.A. Importance of Tabulating Multiple Causes of Death. American Journal of Public Health 1940, 5, 871–879. [Google Scholar] [CrossRef] [PubMed]
- Dorn, H.F.; Moriyama, I.M. Uses and Significance of Multiple Cause Tabulations for Mortality Statistics. Am. J. Public Heal. Nations Heal. 1964, 54, 400–406. [Google Scholar] [CrossRef]
- Israel, R.L.; Rosenberg, H.M.; Curtin, L.R. Analytical Potential for Multiple Cause-of-Death Data. Am. J. Epidemiology 1986, 124, 161–179. [Google Scholar] [CrossRef]
| Indicator | 2018 | 2019 | 2020 | 2021 |
|---|---|---|---|---|
| ASMR (males) ASMR (females) Deaths (#) Mentions (#) |
810.7 | 786.0 | 832.5 | 828.3 |
| 568.6 | 550.0 | 575.3 | 562.7 | |
| 283,330 | 283,685 | 306,780 | 301,830 | |
| 923,330 | 937,045 | 1,008,370 | 966,440 | |
|
Percent of Deaths with 1 cause 2 causes 3 causes 4 causes >4 causes |
||||
| 20.25 | 20.17 | 20.40 | 24.56 | |
| 23.40 | 22.38 | 22.67 | 21.27 | |
| 19.20 | 19.26 | 18.93 | 17.59 | |
| 14.36 | 14.67 | 14.49 | 13.60 | |
| 22.79 | 23.53 | 23.51 | 22.99 | |
|
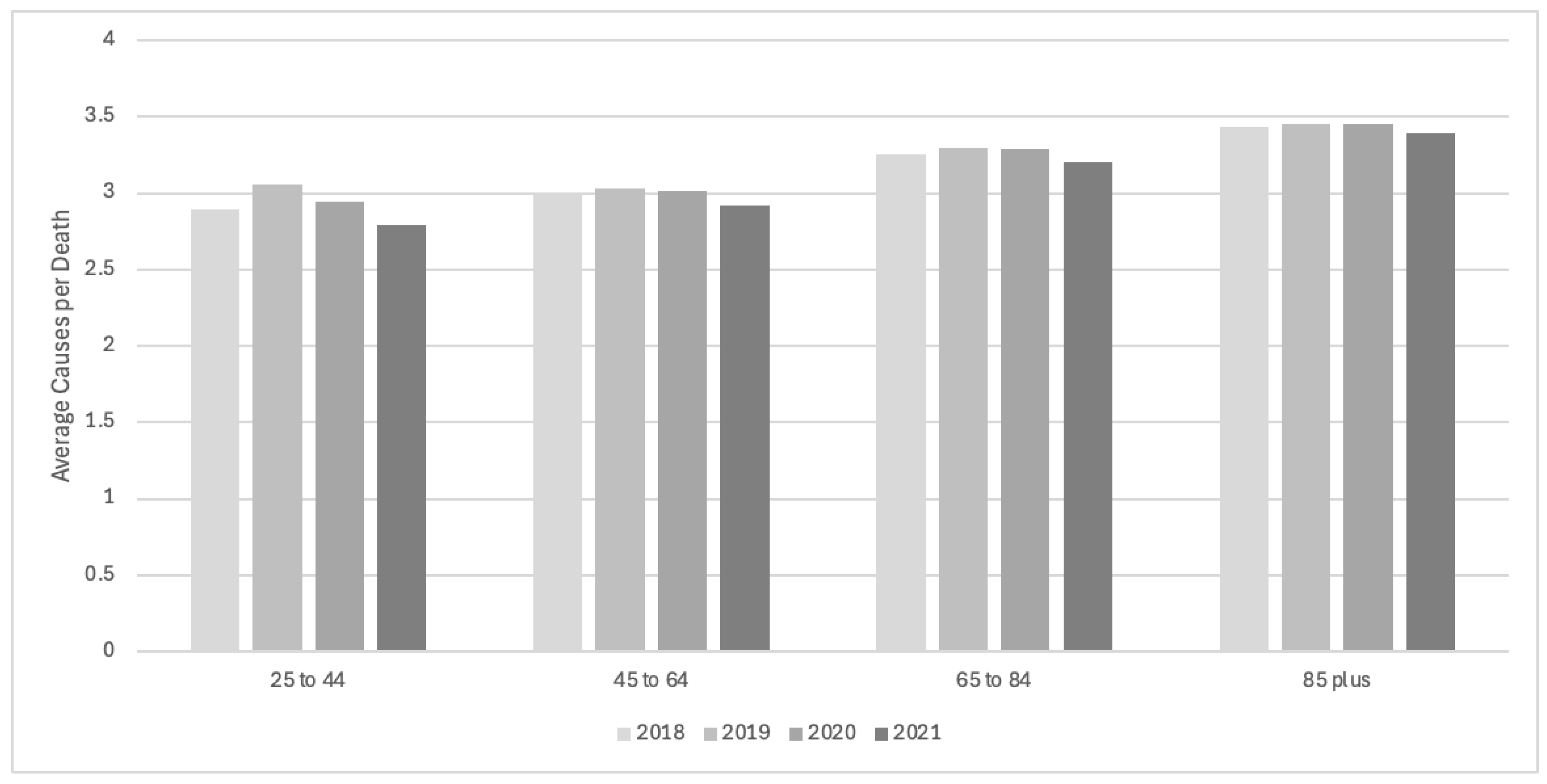
Average Causes by Income Quintile (#) Lowest (1) Mid-Low (2) Middle (3) Mid-High (4) Highest (5) All deaths |
||||
| 3.35 | 3.41 | 3.38 | 3.30 | |
| 3.28 | 3.33 | 3.31 | 3.21 | |
| 3.24 | 3.27 | 3.28 | 3.18 | |
| 3.19 | 3.22 | 3.24 | 3.13 | |
| 3.17 | 3.21 | 3.19 | 3.11 | |
| 3.26 | 3.30 | 3.29 | 3.20 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




