Submitted:
26 September 2024
Posted:
27 September 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Procedure
2.2. Adaptation of the SPICT-TW
2.3. The Validity and Reliability of the SPICT-TW
2.4. Other Measurements
2.5. Participants
2.6. Statistical Analysis
3. Results
3.1. Background Information of Patients and Evaluators
3.2. The Reliability and Validity of the SPICT-TW
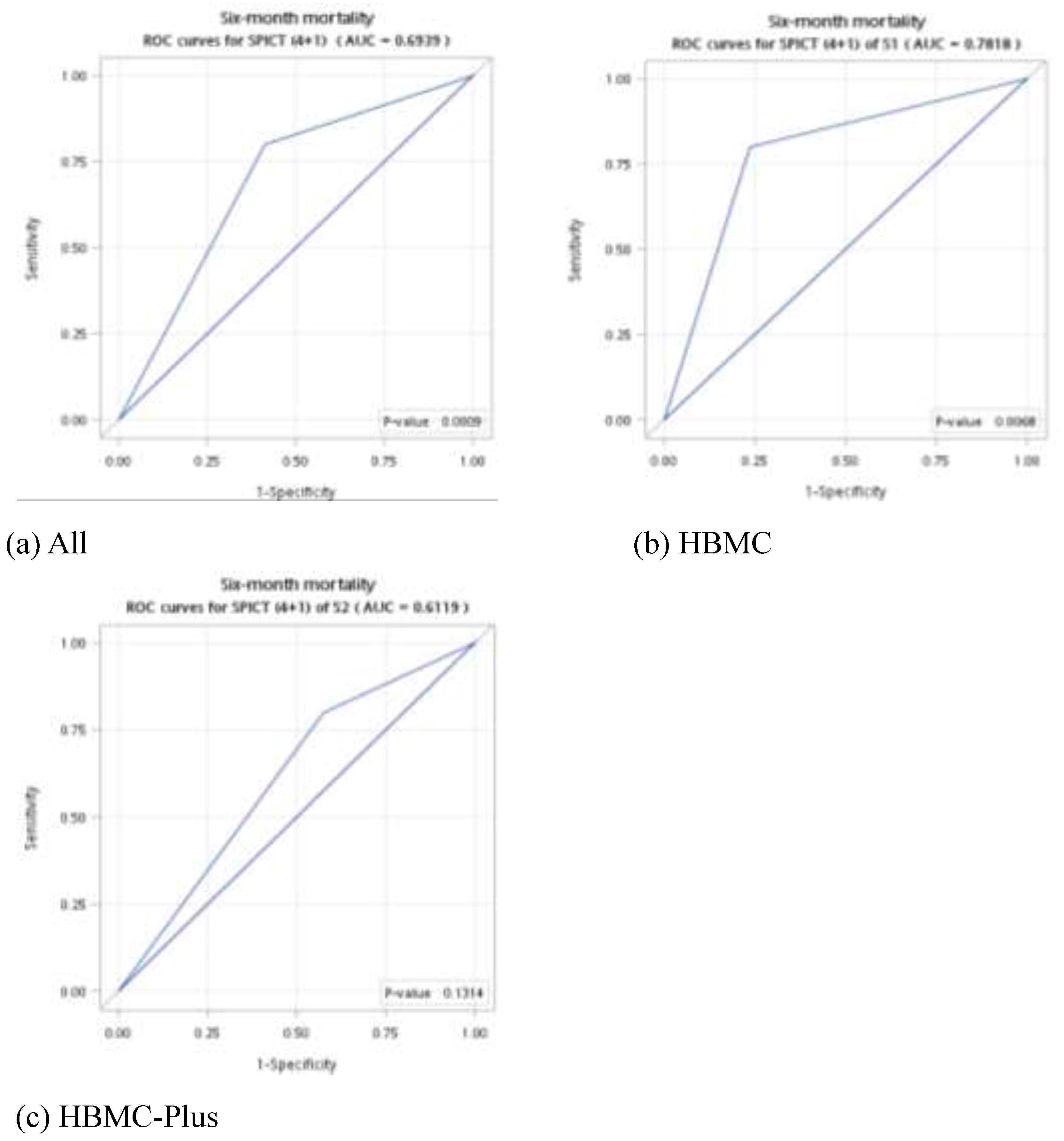
3.3. Association between the SPICT-TW and Six-Month Mortality
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Boyd K, Murray SA: Recognising and managing key transitions in end of life care. BMJ, 2010; 341, c4863.
- Fachado AA, Martínez NS, Roselló MM, Rial JJV, Oliver EB, García RG, García JMF: Spanish adaptation and validation of the supportive & palliative care indicators tool - SPICT-ESTM. Rev Saude Publica, 2018; 52, 3.
- Afshar K, Feichtner A, Boyd K, Murray S, Jünger S, Wiese B, Schneider N, Müller-Mundt G: Systematic development and adjustment of the German version of the Supportive and Palliative Care Indicators Tool (SPICT-DE). BMC Palliat Care, 2018; 17, 27.
- Casale G, Magnani C, Fanelli R, Surdo L, Goletti M, Boyd K, D'Angelo D, Mastroianni C: Supportive and palliative care indicators tool (SPICT™): content validity, feasibility and pre-test of the Italian version. BMC Palliat Care, 2020; 19, 79.
- Sripaew S, Fumaneeshoat O, Ingviya T: Systematic adaptation of the Thai version of the supportive and palliative care indicators tool for low-income setting (SPICT-LIS). BMC Palliat Care, 2021; 20, 35.
- Bergenholtz H, Weibull A, Raunkiær M: Supportive and palliative care indicators tool (SPICT™) in a Danish healthcare context: translation, cross-cultural adaptation, and content validation. BMC Palliat Care, 2022; 21, 41.
- Highet G, Crawford D, Murray SA, Boyd K: Development and evaluation of the Supportive and Palliative Care Indicators Tool (SPICT): a mixed-methods study. BMJ Support Palliat Care, 2014; 4, 285–290.
- De Bock R, Van Den Noortgate N, Piers R: Validation of the supportive and palliative care indicators tool in a geriatric population. J Palliat Med, 2018; 21, 220–224.
- Mudge AM, Douglas C, Sansome X, Tresillian M, Murray S, Finnigan S, Blaber CR: Risk of 12-month mortality among hospital inpatients using the surprise question and SPICT criteria: a prospective study. BMJ Support Palliat Care, 2018; 8, 213–220.
- Piers R, De Brauwer I, Baeyens H, Velghe A, Hens L, Deschepper E, Henrard S, De Pauw M, Van Den Noortgate N, De Saint-Hubert M: Supportive and Palliative Care Indicators Tool prognostic value in older hospitalised patients: a prospective multicentre study. BMJ Support Palliat Care, 2021; bmjspcare-2021-003042.
- Effendy C, Silva JFDS, Padmawati RS: Identifying palliative care needs of patients with non-communicable diseases in Indonesia using the SPICT tool: a descriptive cross-sectional study. BMC Palliat Care, 2022; 21, 13.
- Mitchell GK, Senior HE, Rhee JJ, Ware RS, Young S, Teo PC, Murray S, Boyd K, Clayton JM: Using intuition or a formal palliative care needs assessment screening process in general practice to predict death within 12 months: A randomised controlled trial. Palliat Med, 2018; 32, 384–394.
- van Wijmen MPS, Schweitzer BPM, Pasman HR, Onwuteaka-Philipsen BD: Identifying patients who could benefit from palliative care by making use of the general practice information system: the Surprise Question versus the SPICT. Fam Pract, 2020; 37, 641–647.
- van Baal K, Wiese B, Müller-Mundt G, Stiel S, Schneider N, Afshar K: Quality of end-of-life care in general practice – a pre–post comparison of a two-tiered intervention. BMC Prim Care, 2022; 23, 90.
- Liyanage T, Mitchell G, Senior H: Identifying palliative care needs in residential care. Aust J Prim Health, 2018; 24, 524–529.
- Mondor L, Maxwell CJ, Hogan DB, Bronskill SE, Gruneir A, Lane NE, Wodchis WP: Multimorbidity and healthcare utilization among home care clients with dementia in Ontario, Canada: A retrospective analysis of a population-based cohort. PLoS Med, 2017; 14, e1002249.
- Harrison KL, Leff B, Altan A, Dunning S, Patterson CR, Ritchie CS: What's happening at home: a claims-based approach to better understand home clinical care received by older adults. Med Care, 2020; 58, 360–367.
- Ritchie CS, Leff B: Population health and tailored medical care in the home: the roles of home-based primary care and home-based palliative care. J Pain Symptom Manage, 2018; 55, 1041–1046.
- Chang HT, Lai HY, Hwang IH, Ho MM, Hwang SJ: Home healthcare services in Taiwan: a nationwide study among the older population. BMC Health Serv Res, 2010; 10, 274.
- Landers S, Madigan E, Leff B, Rosati RJ, McCann BA, Hornbake R, MacMillan R, Jones K, Bowles K, Dowding D et al: The future of home health care: a strategic framework for optimizing value. Home Health Care Manag Pract, 2016; 28, 262–278.
- Shih CY, Chen YM, Huang SJ: Survival and characteristics of older adults receiving home-based medical care: A nationwide analysis in Taiwan. J Am Geriatr Soc, 2023; 71, 1526–1535.
- Su MC, Chen YC, Huang MS, Lin YH, Lin LH, Chang HT, Chen TJ: LACE score-based risk management tool for long-term home care patients: a proof-of-concept study in Taiwan. Int J Environ Res Public Health, 2021; 18.
- Liao JY, Chen PJ, Wu YL, Cheng CH, Yu SJ, Huang CH, Li CM, Wang YW, Zhang KP, Liu IT et al: HOme-based Longitudinal Investigation of the multidiSciplinary Team Integrated Care (HOLISTIC): protocol of a prospective nationwide cohort study. BMC Geriatr, 2020, 20(1):511.
- World Health Organization. Process of translation and adaptation of instruments. 2009 [http://www who int/substance_abuse/research_tools/translation/en/ 2009].
- Shrout PE, Fleiss JL: Intraclass correlations: uses in assessing rater reliability. Psychological Bulletin, 1979, 86(2):420-42.
- Bonsignore M, Barkow K, Jessen F, Heun R: Validity of the five-item WHO Well-Being Index (WHO-5) in an elderly population. Eur Arch Psychiatry Clin Neurosci, 2001, 251 Suppl 2:Ii27-31.
- Rockwood K, Song X, MacKnight C, Bergman H, Hogan DB, McDowell I, Mitnitski A: A global clinical measure of fitness and frailty in elderly people. CMAJ, 2005, 173(5):489-495.
- Shrout PE, Fleiss JL: Intraclass correlations: uses in assessing rater reliability. Psychological Bulletin, 1979, 86(2):420.
- McHugh ML: Interrater reliability: the kappa statistic. Biochem Med (Zagreb), 2012, 22(3):276-282.
- Hosmer DW, Lemeshow S, Sturdivant RX: Applied Logistic Regression; 2013.
- Bourmorck D, de Saint-Hubert M, Desmedt M, Piers R, Flament J, De Brauwer I: SPICT as a predictive tool for risk of 1-year health degradation and death in older patients admitted to the emergency department: a bicentric cohort study in Belgium. BMC palliat care, 2023, 22(1):79.
| Total, N=129 | HBMC Type | |||
| HBMC, n=60 |
HBMC-Plus, n=69 | P-value | ||
| Age, mean (SD) | 82.4 (12.0) | 81.7 (11.9) | 83.0 (12.2) | .516 |
| Sex (Female), n (%) | 69 (53.5) | 33 (55.0) | 36 (52.2) | .748 |
| Comorbidity, n (%) | .259 | |||
| <5 | 43 (33.3) | 22 (36.7) | 21 (30.4) | |
| 5-6 | 49 (38.0) | 25 (41.7) | 24 (34.8) | |
| ≥ 7 | 37 (28.7) | 13 (21.7) | 24 (34.8) | |
| Hospitalization in past 30 days, n (%) | 13 (10.0) | 3 (5.0) | 10 (14.5) | .086 |
| WHO-5, n (%) | <.001 | |||
| Good | 64 (49.6) | 40 (66.7) | 24 (34.8) | |
| Poor | 65 (50.4) | 20 (33.3) | 45 (65.2) | |
| Clinical Frailty Scale, n (%) | <.001 | |||
| ≤ 5 | 22 (17.1) | 17 (28.3) | 5 (7.3) | |
| 6 | 34 (26.4) | 26 (43.3) | 8 (11.6) | |
| 7 | 48 (37.2) | 13 (21.7) | 35 (50.7) | |
| 8-9 | 25 (19.4) | 4 (6.7) | 21 (30.4) | |
| Six-month mortality, n (%) | 15 (12.3) | 5 (8.3) | 10 (14.5) | .276 |
| Total (N=35) | |||
| Age, mean (SD) a | 40.6 (10.0) | ||
| Years of work experience, median (IQR)b | 15 (4.6-24.5) | ||
| Professional of evaluator, n (%) | |||
| Physician | 11 (31.4) | ||
| Nurse | 19 (54.3) | ||
| Others | 5 (14.3) | ||
| Type of affiliation, n (%) | |||
| Hospital | 21 (60.0) | ||
| Clinic | 14 (40.0) | ||
| SPICT-TW | |||
| All indicators | General health indicators | Clinical indicators | |
| KR-20 | |||
| All (n=129) | 0.84 | 0.67 | 0.80 |
| physician (n=53) | 0.83 | 0.61 | 0.77 |
| Nurse (n=55) | 0.86 | 0.66 | 0.82 |
| Others (n=21) | 0.77 | 0.71 | 0.80 |
| ICC (95% CI) | 0.92 (0.89-0.95) | 0.91 (0.87-0.93) | 0.87 (0.82-0.91) |
| Number of indicators | Sensitivity | Specificity | Youden Index | AUC (95% CI) | |
| General indicators | 1 | 0.93 | 0.07 | 0.003 | 0.73 (0.58-0.88) |
| 2 | 0.93 | 0.18 | 0.108 | P=0.002 | |
| 3 | 0.87 | 0.36 | 0.227 | ||
| 4 | 0.80 | 0.56 | 0.361 | ||
| 5 | 0.53 | 0.83 | 0.358 | ||
| 6 | 0.20 | 0.97 | 0.165 | ||
| 7 | 0.07 | 0.99 | 0.058 | ||
| Clinical indicators | 1 | 0.87 | 0.25 | 0.113 | 0.61 (0.46-0.76) |
| 2 | 0.67 | 0.49 | 0.158 | P=0.154 | |
| 3 | 0.20 | 0.90 | 0.095 | ||
| 4 | 0.13 | 0.98 | 0.115 | ||
| 5 | 0.13 | 0.99 | 0.124 | ||
| 6 | 0.07 | 1.00 | 0.067 |
| Variable | Univariate model | Full model I | Full model II | ||||||
| OR | 95% CI | P | OR | 95% CI | P | OR | 95% CI | P | |
| SPICT (4+1) | |||||||||
| Negative | [Ref] | [Ref] | N/A | ||||||
| Positive | 5.70 | (1.53-21.3) | 0.010 | 8.30 | (1.17-58.82) | 0.034 | |||
| SPICT (2+1) | |||||||||
| Negative | [Ref] | N/A | [Ref] | ||||||
| Positive | 3.12 | (0.67-14.55) | 0.147 | 6.24 | (0.57-68.29) | 0.134 | |||
| Age | |||||||||
| <75 | [Ref] | [Ref] | [Ref] | ||||||
| 75-84 | 1.92 | (0.19-19.6) | 0.583 | 1.16 | (0.08-16.01) | 0.914 | 1.34 | (0.11-17.18) | 0.822 |
| ≧85 | 4.60 | (0.56-37.7) | 0.155 | 4.46 | (0.42-47.28) | 0.215 | 5.11 | (0.50-52.31) | 0.169 |
| Sex | |||||||||
| Male | [Ref] | [Ref] | [Ref] | ||||||
| Female | 0.99 | (0.34-2.92) | 0.990 | 0.34 | (0.08-1.54) | 0.162 | 0.31 | (0.07-1.44) | 0.134 |
| Comorbidity | |||||||||
| <5 | [Ref] | [Ref] | [Ref] | ||||||
| 5-6 | 0.55 | (0.14-2.09) | 0.378 | 0.38 | (0.07-2.08) | 0.263 | 0.33 | (0.06-1.70) | 0.184 |
| ≧7 | 0.96 | (0.27-3.46) | 0.955 | 1.19 | (0.21-6.74) | 0.848 | 0.95 | (0.18-5.17) | 0.954 |
| HBMC Type | |||||||||
| HBMC | [Ref] | [Ref] | [Ref] | ||||||
| HBMC-Plus | 1.86 | (0.60-5.80) | 0.282 | 0.49 | (0.09-2.57) | 0.395 | 0.56 | (0.11-2.87) | 0.491 |
| Hospitalization in past 30 days | |||||||||
| No | [Ref] | [Ref] | [Ref] | ||||||
| Yes | 2.60 | (0.63-10.78) | 0.188 | 2.14 | (0.31-14.88) | 0.441 | 2.75 | (0.37-20.49) | 0.323 |
| WHO-5 wellbeing index | |||||||||
| Good | [Ref] | [Ref] | [Ref] | ||||||
| Poor | 4.60 | (1.23-17.2) | 0.023 | 3.09 | (0.50-19.13) | 0.226 | 3.24 | (0.56-18.62) | 0.188 |
| Clinical Frailty Scale | |||||||||
| 1-5 | [Ref] | [Ref] | [Ref] | ||||||
| 6 | 2.03 | (0.20-20.89) | 0.551 | 0.63 | (0.04-11.07) | 0.754 | 0.82 | (0.05-13.44) | 0.888 |
| 7 | 0.91 | (0.08-10.64) | 0.942 | 0.09 | (0.01-2.85) | 0.170 | 0.12 | (0.01-3.74) | 0.229 |
| 8-9 | 11.8 | (1.35-103.04) | 0.026 | 2.14 | (0.09-49.52) | 0.636 | 2.70 | (0.12-60.56) | 0.531 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




