Submitted:
18 September 2024
Posted:
19 September 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
3.1. Optimal Excision Surgery Results
3.1.1. Figure 1: Repeat Surgery Rate, ASRM Staging & Extraneous Findings
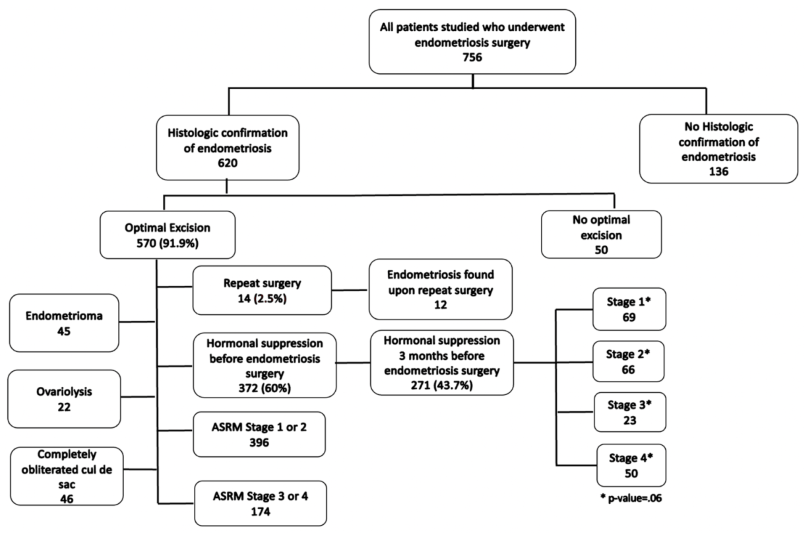
-
620 of the 756 patients in the database who underwent surgery for endometriosis from 2012-2019 had histological confirmation of endometriosis in any location excised (Table 1).91.9% received optimal endometriosis excision surgery.
- Of the 620 patients with tissue-proven endometriosis, 570 women had OES for endometriosis (Table 2).
- Of the 570 who underwent OES, only 14 patients underwent repeat surgery (2.5%).
- Endometriosis was found in 12 of these 14 women. 69.5% of the women who underwent OES were found to be in ASRM stages 1 or 2, and 30.6% in ASRM stages 3 or 4.
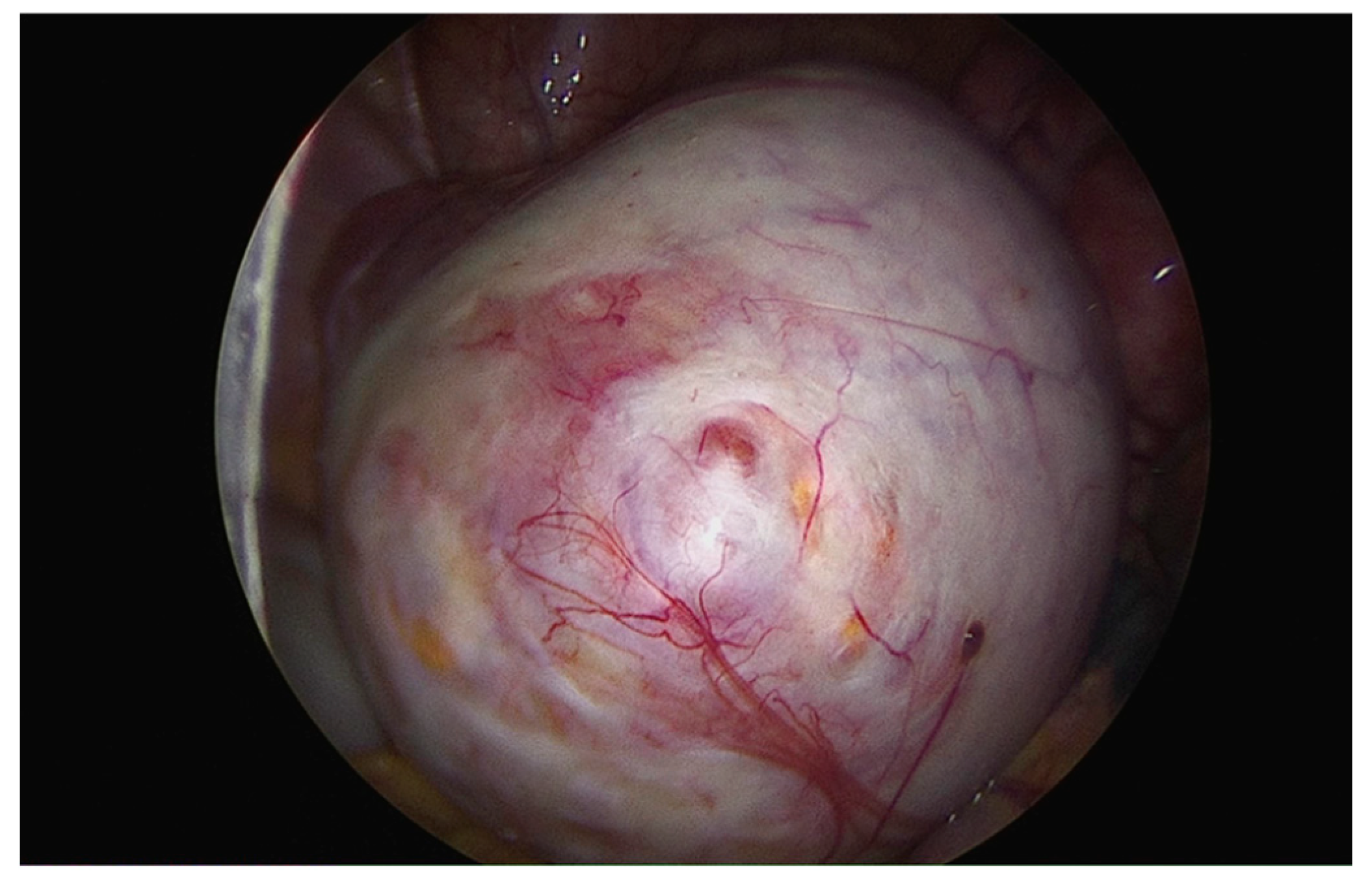
- Endometrioma was found in 45 of these women (23.1%), and ovariolysis was performed in 22 (53.7%). (Figure 2)
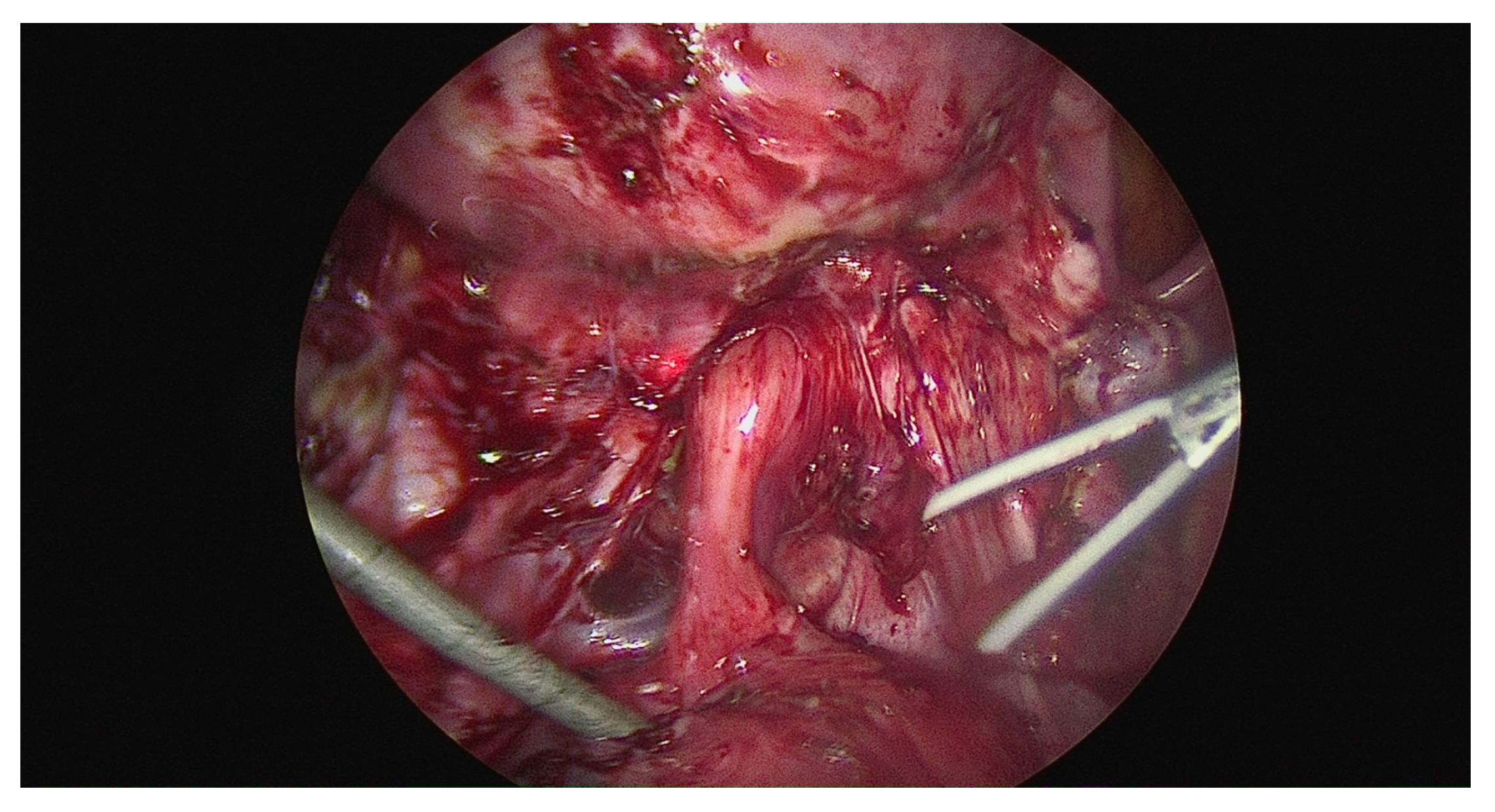
- 46 had a completely obliterated cul-de-sac (8.9%); 33 had partial (6.4%); and 440 had an absent cul-de-sac (84.8%). (Figure 3)
3.1.2. Effects of Use of Hormonal Suppression
- Of the 620 women who underwent endometriosis excision surgery, approximately 60% reported use of hormonal suppression before their surgery (Table 1).
- Hormonal contraceptives were reported by 96.4% of the women, gonadotropin-releasing agonists/antagonists/chemical menopause were reported by 29.5% of the women, and a progesterone-secreting intrauterine device (IUD) was reported by 14.6% of the women.
- The median length of hormonal suppression before endometriosis excision surgery was 36 months with a range of 1-336 months.
- The response rate of follow-up post operatively was 49% (304/620 patients).
- Use of hormonal suppression in the three months before endometriosis excision surgery was reported by 43.7% of the women.
- While no significant overall difference in the use of hormonal suppression before endometriosis excision surgery was found between women receiving OES and women not receiving OES (60.2% versus 50.0%, p=0.21, Table 2), a significantly higher proportion of women receiving OES used hormonal contraceptives (97.0% versus 87.0%, p<0.05).
- Of the 387 women with a known stage of endometriosis and known value for hormonal suppression prior to surgery, 179 reported that they did not take any hormonal suppression prior to excision surgery (Table 3).
- Of those who were known to be in stage 1, 61.6% took hormonal suppression and 38.4% did not; in stage 2, 50.4% took hormonal suppression and 49.6% did not; in stage 3, 50% took hormonal suppression and 50% did not; and in stage 4, 51% took hormonal suppression and 49% did not.
- Use of progesterone-secreting IUD before endometriosis excision surgery between women with either ASRM stage 1 (21.2%) or stage 3 (27.3%) and stage 4 (8.3%) approached statistical significance (p=0.06).
- No significant overall association was found for any hormonal suppression before endometriosis excision surgery variable with stage of endometriosis when all four endometriosis stages were examined simultaneously.
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Nirgianakis K, Ma L, McKinnon B, Mueller MD. Recurrence Patterns after Surgery in Patients with Different Endometriosis Subtypes: A Long-Term Hospital-Based Cohort Study. Journal of Clinical Medicine. 2020, 9. [Google Scholar] [CrossRef]
- Chen I, Veth VB, Choudhry AJ, Murji A, Zakhari A, Black AY, Agarpao C, Maas JW. Pre- and postsurgical medical therapy for endometriosis surgery. Cochrane Database Syst Rev. 2020, 11, CD003678. [Google Scholar] [CrossRef]
- Greene AD, Lang SA, Kendziorski JA, Sroga-Rios JM, Herzog TJ, Burns KA. Endometriosis: where are we and where are we going? Reproduction. 2016, 152, R63–R78. [Google Scholar] [CrossRef]
- Hart RJ, Hickey M, Maouris P, Buckett W. Excisional surgery versus ablative surgery for ovarian endometriomata. Cochrane Database Syst Rev 2008, CD004992. Published 2008 Apr 16. [CrossRef]
- Yeung P Jr, Tu F, Bajzak K, et al. A pilot feasibility multicenter study of patients after excision of endometriosis. JSLS. 2013, 17, 88–94. [Google Scholar] [CrossRef]
- Takenaka M, Yano R, Hiraku Y, et al. Exploratory study of pre-surgical medications with dienogest or leuprorelin in laparoscopic cystectomy of endometrial cysts. J Obstet Gynaecol Res. 2015, 41, 1234–1239. [Google Scholar] [CrossRef]
- Sutton CJ, Ewen SP, Whitelaw N, Haines P. Prospective, randomized, double-blind, controlled trial of laser laparoscopy in the treatment of pelvic pain associated with minimal, mild, and moderate endometriosis. Fertil Steril. 1994, 62, 696–700. [Google Scholar] [CrossRef]
- Alkatout I, Mettler L, Beteta C, et al. Combined surgical and hormone therapy for endometriosis is the most effective treatment: prospective, randomized, controlled trial. J Minim Invasive Gynecol. 2013, 20, 473–481. [Google Scholar] [CrossRef]
- Bozdag, G. Recurrence of endometriosis: risk factors, mechanisms and biomarkers. Womens Health (Lond). 2015, 11, 693–699. [Google Scholar] [CrossRef]
- Carmona F, Martínez-Zamora MA, Rabanal A, Martínez-Román S, Balasch J. Ovarian cystectomy versus laser vaporization in the treatment of ovarian endometriomas: a randomized clinical trial with a five-year follow-up. Fertil Steril. 2011, 96, 251–254. [Google Scholar] [CrossRef]
- Rafique S, Decherney AH. Medical Management of Endometriosis. Clin Obstet Gynecol. 2017, 60, 485–496. [Google Scholar] [CrossRef] [PubMed]
- Zondervan KT, Becker CM, Missmer SA. Endometriosis. N Engl J Med. 2020, 382, 1244–1256. [Google Scholar] [CrossRef] [PubMed]
- Sørensen SS, Colov NP, Vejerslev LO. Pre- and postoperative therapy with GnRH agonist for endometrial resection. A prospective, randomized study. Acta Obstet Gynecol Scand. 1997, 76, 340–344. [Google Scholar] [CrossRef]
- Rana N, Thomas S, Rotman C, Dmowski WP. Decrease in the size of ovarian endometriomas during ovarian suppression in stage IV endometriosis. Role of preoperative medical treatment. J Reprod Med. 1996, 41, 384–392. [Google Scholar]
- Healey M, Cheng C, Kaur H. To excise or ablate endometriosis? A prospective randomized double-blinded trial after 5-year follow-up. J Minim Invasive Gynecol. 2014, 21, 999–1004. [Google Scholar] [CrossRef]
- Bignardi T, Khong SY, Lam A. Excisional versus ablative surgery for peritoneal endometriosis. Cochrane Database Syst Rev. 2019, 2019, CD008979, Published 2019 Jul 29. [Google Scholar] [CrossRef]
- Fincham, JE. Response rates and responsiveness for surveys, standards, and the Journal. Am J Pharm Educ. 2008, 72, 43. [Google Scholar] [CrossRef]
- Stratton P, Berkley KJ. Chronic pelvic pain and endometriosis: translational evidence of the relationship and implications. Hum Reprod Update. 2011, 17, 327–346. [Google Scholar] [CrossRef]
- Yap C, Furness S, Farquhar C. Pre and post operative medical therapy for endometriosis surgery. Cochrane Database Syst Rev. 2004, 2004, CD003678. [Google Scholar] [CrossRef]
- Pecorino B, Lagana AS, Chiantera V, Ferrara M, Di Stefano AB, Di Donna MC, Sorrentino F, Nappi L, Mikus M, Scollo P. Progression Free Survival, Overall Survival, and Relapse Rate in Endometrioid Ovarian Cancer and Synchronous Endometrial-Ovarian Endometrioid Cancer (SEO-EC): Results from a Large Retrospective Analysis. Medicina (Kaunas). 2022, 58, 1706. [Google Scholar] [CrossRef]
- Martire FG, Russo C, Selntigia A, Nocita E, Soreca G, Lazzeri L, Zupi E, Exacoustos C. Early noninvasive diagnosis of endometriosis: dysmenorrhea and specific ultrasound findings are important indicators in young women. Fertil Steril. 2023, 119, 455–464. [Google Scholar] [CrossRef] [PubMed]
- Millischer AE, Santulli P, Da Costa S, Bordonne C, Cazaubon E, Marcellin L, Chapron C. Adolescent endometriosis: prevalence increases with age on magnetic resonance imaging scan. Fertil Steril. 2023, 119, 626–633. [Google Scholar] [CrossRef]
| Characteristic | N | % | |
| Histological Confirmation of Endometriosis Found Anywhere | 620 | 100.0 | |
| Optimal Excision Surgery for Endometriosis* | |||
| Yes | 570 | 91.9 | |
| No | 50 | 8.1 | |
| Hormonal Suppression Before Endometriosis Excision Surgery | |||
| No | 250 | 40.6 | |
| Yes | 366 | 59.4 | |
| Hormonal Contraceptives | 344 | 96.4 | |
| Gonadotropin-Releasing Agonists/Antagonists/Chemical Menopause | 105 | 29.5 | |
| Progesterone-secreting IUD | 52 | 14.6 | |
| Length of Hormonal Suppression Before Endometriosis Excision Surgery (mo)† | 36 (1-336) | ||
| Used Hormonal Suppression in the 3 Months Before Endometriosis Excision Surgery† | 115 | 43.7 | |
| Number of Ablation Surgeries | 0 (0-7) | ||
| Repeat Surgery | |||
| No | 605 | 97.6 | |
| Yes | 15 | 2.4 | |
| Endometriosis Found | 12 | 80.0 | |
| No Endometriosis Found | 3 | 20.0 | |
| Endometrioma | |||
| No Endometrioma Found | 153 | 74.6 | |
| Endometrioma Found: Left Ovary | 22 | 10.7 | |
| Endometrioma Found: Right Ovary | 8 | 3.9 | |
| Endometrioma Found: Both Ovaries | 22 | 10.7 | |
| Ovariolysis | |||
| No Ovariolysis Performed | 21 | 45.7 | |
| Ovariolysis Performed: Left Ovary | 5 | 10.9 | |
| Ovariolysis Performed: Right Ovary | 1 | 2.2 | |
| Ovariolysis Performed: Both Ovaries | 19 | 41.3 | |
| Obliterated Posterior Cul-de-Sac | |||
| Absent | 458 | 80.6 | |
| Partial | 38 | 6.7 | |
| Complete | 72 | 12.7 | |
| Retrocervical Endometriosis Found/Excised | 102 | 16.5 | |
| Endometriosis Stage | |||
| I | 112 | 28.6 | |
| II | 134 | 34.3 | |
| III | 46 | 11.8 | |
| IV | 99 | 25.3 | |
| N | % | N | % | P-value | ||
| Optimal Excision Surgery | 570 | 91.9 | 50 | 8.1 | ||
| Hormonal Suppression Before Endometriosis Excision Surgery | ||||||
| No | 225 | 39.8 | 25 | 50.0 | 0.21 | |
| Yes | 341 | 60.2 | 25 | 50.0 | ||
| Hormonal Contraceptives | 324 | 97.0 | 20 | 87.0 | <0.05 | |
| Gonadotropin-Releasing Agonists | 96 | 28.8 | 9 | 39.1 | 0.42 | |
| Progesterone-secreting IUD | 51 | 15.3 | 1 | 4.3 | 0.22 | |
| Hormonal Suppression Length Before Excision Surgery (mo)§ | 36 (12, 96) |
36 (6, 53) |
0.21 | |||
| Hormonal Suppression Use in 3 Months Before Excision Surgery§ | 111 | 43.7 | 4 | 44.4 | 1.00 | |
| Number of Ablation Surgeries | 0 (0, 1) | 0 (0, 0) | <0.001 | |||
| Repeat Surgery | ||||||
| No | 556 | 97.5 | 49 | 98.0 | 1.00 | |
| Yes | 14 | 2.5 | 1 | 2.0 | ||
| Endometriosis Found | 12 | 85.7 | 0 | 0.0 | 0.20 | |
| No Endometriosis Found | 2 | 14.3 | 1 | 100.0 | ||
| Endometrioma Found | ||||||
| Yes | 45 | 23.1 | 7 | 70.0 | <0.01 | |
| No | 150 | 76.9 | 3 | 30.0 | ||
| Ovariolysis Performed | ||||||
| Yes | 22 | 53.7 | 3 | 60.0 | 1.00 | |
| No | 19 | 46.3 | 2 | 40.0 | ||
| Obliterated Posterior Cul-de-Sac | ||||||
| Absent | 440 | 84.8 | 18 | 36.7 | ||
| Partial | 33 | 6.4 | 5 | 10.2 | <0.001 | |
| Complete | 46 | 8.9 | 26 | 53.1 | ||
| Retrocervical Endometriosis Excised | 86 | 15.1 | 16 | 32.0 | 0.01 | |
| Endometriosis Stage | ||||||
| I | 180 | 31.7 | 0 | 0.0 | ||
| II | 216 | 38.1 | 6 | 12.0 | <0.001 | |
| III | 68 | 12.0 | 3 | 6.0 | ||
| IV | 103 | 18.2 | 41 | 82.0 | ||
| Duration of Follow-up (mo) | 25(13, 48) | 36 (12, 71) | 0.10 | |||
| Endometriosis Stage | N | % | N | % | P-value | |
| I or II* | III or IV† | |||||
| 399 | 65.1 | 214 | 34.9 | |||
| Hormonal Suppression Before Excision Surgery | ||||||
| No | 151 | 37.8 | 99 | 46.3 | 0.05 | |
| Yes | 248 | 62.2 | 115 | 53.7 | ||
| Hormonal Contraceptives | 234 | 96.7 | 107 | 95.5 | 0.56 | |
| Gonadotropin-Releasing Agonists/CM | 69 | 28.6 | 34 | 30.4 | 0.84 | |
| Progesterone-secreting IUD | 38 | 15.8 | 14 | 12.5 | 0.52 | |
| Hormonal Suppression Length Before Excision Surgery (mo) | 32.0 (12.0, 84.3) | 36.0 (9.0, 108.0) |
0.69 | |||
| Hormonal Suppression in 3 mos Before Excision Surgery | 79 | 45.4 | 35 | 40.7 | 0.56 | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




