Submitted:
26 August 2024
Posted:
27 August 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
3.1. Demographics
3.2. Knowledge of Disrespectful Care
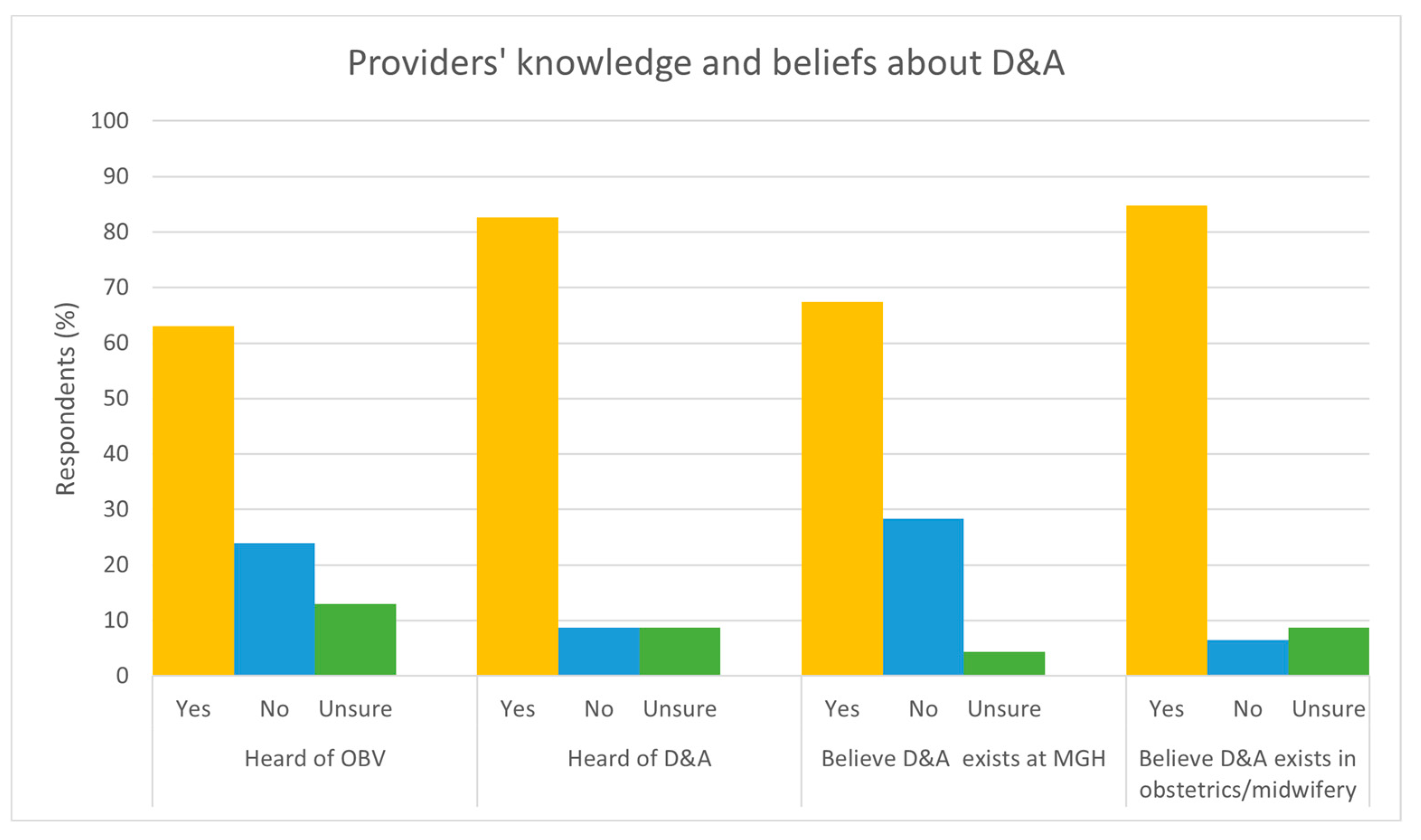
3.3. Disrespectful Care Witnessed
“There are times when I feel the language people use, whether intentionally or not, can sound rude and disrespectful.”
“Conversations outside of the room about a patient or family member that is judgmental or unkind.”
“Adequate consenting by providers for medications and procedures in labor feels inadequate. Many of the information that I hear providers offer to patients during care planning feels incomplete and biased towards what the provider most wants the patient to do/feels most convenient.”
“Trying multiple times to place cook balloons on patients who are uncomfortable”
“After traumatic cook balloon placement, MD agreed he wasn’t going to put balloon to tension right away and then pulled balloon so hard that patient had vagal response and prolonged deceleration that resulted in unnecessary intervention and unnecessary emotional and physical trauma to patient”
“Often a lack of respect and consideration of patients whose primary language is not English - increasing volume, not addressing them directly, making side comments to staff.”
3.4. Respectful Care Performed
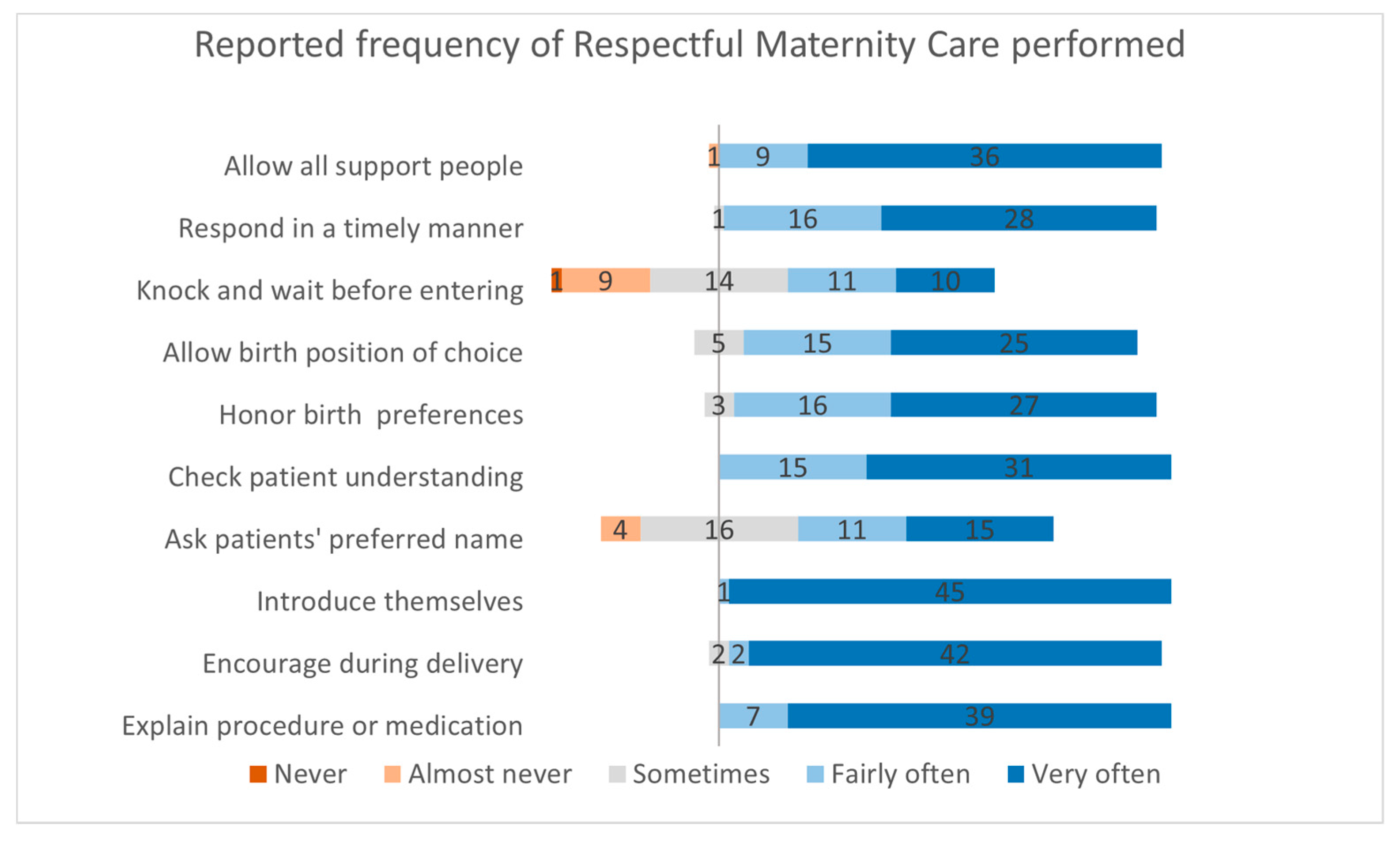
3.5. Stress & Support Factors
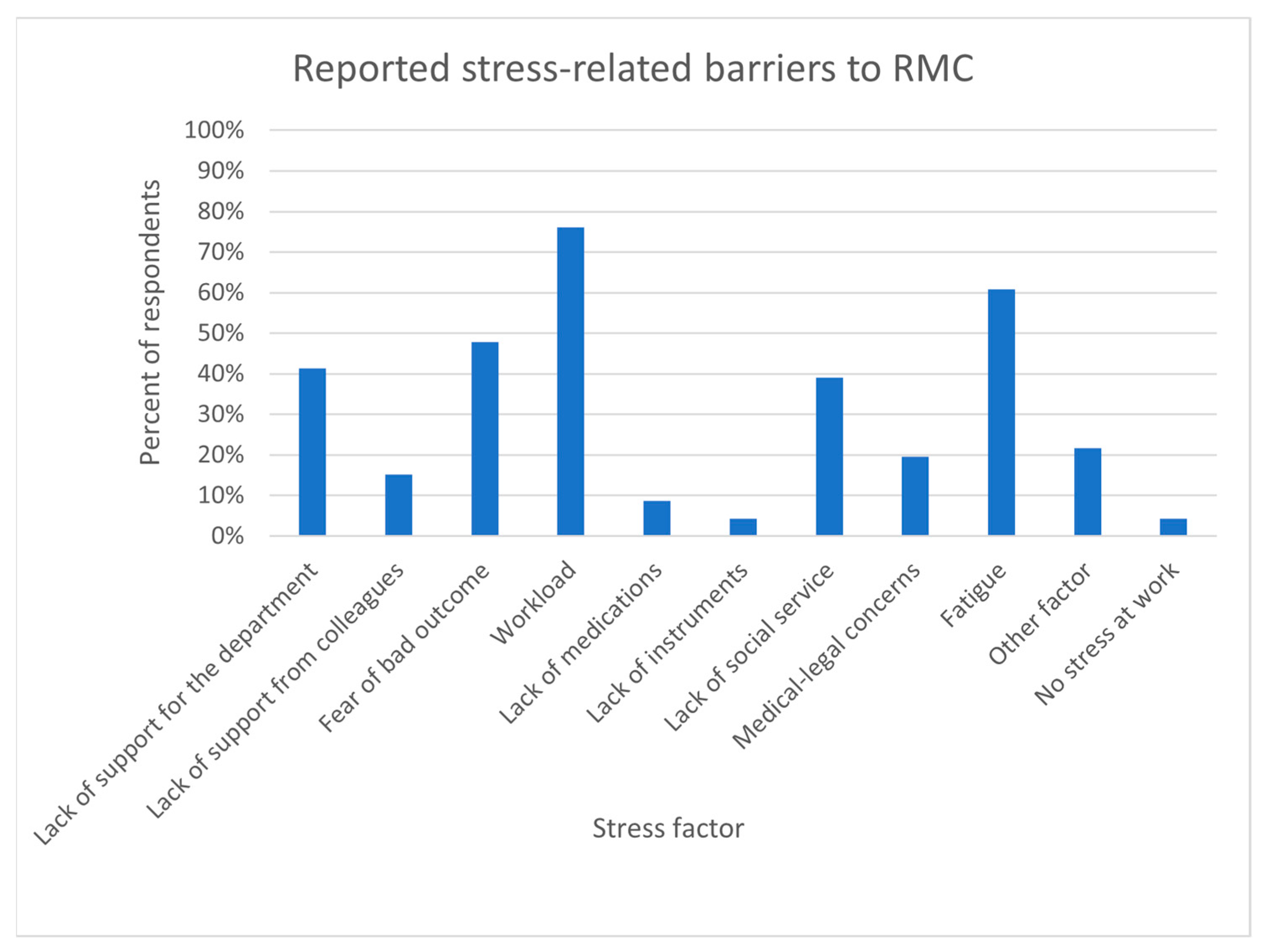
4. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Hoyert D. Maternal mortality rates in the United States, 2021 [Internet]. National Center for Health Statistics (U.S.); 2023 Mar [cited 2023 Sep 29]. Available from: https://stacks.cdc.gov/view/cdc/124678.
- Trost S, Beauregard J, Nije F. Atlanta, GA: Centers for Disease Control and Prevention, US Department of Health and Human Services. 2022 [cited 2023 Sep 29]. Pregnancy-Related Deaths: Data from Maternal Mortality Review Committees in 36 US States, 2017–2019. Available from: https://www.cdc.gov/reproductivehealth/maternal-mortality/erase-mm/data-mmrc.html.
- Maternal deaths and mortality rates: Each state, the District of Columbia, United States, 2018-2021. Center for Disease Control and Prevention, National Center for Health Ststistics (NCHS), National Vital Statistics System.
- Hollier LM, Busacker A, Njie F, Syverson C, Goodman DA. Pregnancy-Related Deaths Due to Hemorrhage: Pregnancy Mortality Surveillance System, 2012–2019. Obstet Gynecol. 2024 Aug;144(2):252. [CrossRef]
- Wallace M, Gillispie-Bell V, Cruz K, Davis K, Vilda D. Homicide During Pregnancy and the Postpartum Period in the United States, 2018–2019. Obstet Gynecol. 2021 Nov;138(5):762–9. [CrossRef]
- Crear-Perry J, Correa-de-Araujo R, Lewis Johnson T, McLemore MR, Neilson E, Wallace M. Social and Structural Determinants of Health Inequities in Maternal Health. J Womens Health. 2021 Feb;30(2):230–5. [CrossRef]
- Howell EA, Zeitlin J. Improving hospital quality to reduce disparities in severe maternal morbidity and mortality. Semin Perinatol. 2017 Aug 1;41(5):266–72. [CrossRef]
- Kheyfets A, Dhaurali S, Feyock P, Khan F, Lockley A, Miller B, et al. The impact of hostile abortion legislation on the United States maternal mortality crisis: a call for increased abortion education. Front Public Health [Internet]. 2023 Dec 5 [cited 2024 Apr 19];11. Available from: https://www.frontiersin.org/journals/public-health/articles/10.3389/fpubh.2023.1291668/full.
- Bhatia, R. Family Leave and Maternal Mortality in the US. JAMA. 2023 Oct 10;330(14):1387. [CrossRef]
- Eliason, EL. Adoption of Medicaid Expansion Is Associated with Lower Maternal Mortality. Womens Health Issues. 2020 May 1;30(3):147–52. [CrossRef]
- Vilda D, Wallace ME, Daniel C, Evans MG, Stoecker C, Theall KP. State Abortion Policies and Maternal Death in the United States, 2015‒2018. Am J Public Health. 2021 Sep;111(9):1696–704. [CrossRef]
- Goyal M, Singh P, Singh K, Shekhar S, Agrawal N, Misra S. The effect of the COVID-19 pandemic on maternal health due to delay in seeking health care: Experience from a tertiary center. Int J Gynaecol Obstet. 2021 Feb;152(2):231–5. [CrossRef]
- Davis NL, Hoyert DL, Goodman DA, Hirai AH, Callaghan WM. Contribution of maternal age and pregnancy checkbox on maternal mortality ratios in the United States, 1978–2012. Am J Obstet Gynecol. 2017 Sep;217(3):352.e1-352.e7.
- World Health Organization. The prevention and elimination of disrespect and abuse during facility-based childbirth: WHO statement. 2014.
- Bowser D, Hill K. Exploring Evidence for Disrespect and Abuse in Facility-Based Childbirth: Report of a Landscape Analysis. USAID-Tract Proj. 2010.
- Bekele W, Bayou NB, Garedew MG. Magnitude of disrespectful and abusive care among women during facility-based childbirth in Shambu town, Horro Guduru Wollega zone, Ethiopia. Midwifery. 2020 Apr 1;83:102629. [CrossRef]
- Perrotte V, Chaudhary A, Goodman A. “At Least Your Baby Is Healthy” Obstetric Violence or Disrespect and Abuse in Childbirth Occurrence Worldwide: A Literature Review. Open J Obstet Gynecol. 2020;10(11):1544–62. [CrossRef]
- Liese KL, Davis-Floyd R, Stewart K, Cheyney M. Obstetric iatrogenesis in the United States: the spectrum of unintentional harm, disrespect, violence, and abuse. Anthropol Med. 2021 Jun;28(2):188–204. [CrossRef]
- Morton CH, Henley MM, Seacrist M, Roth LM. Bearing witness: United States and Canadian maternity support workers’ observations of disrespectful care in childbirth. Birth Berkeley Calif. 2018 Sep;45(3):263–74. [CrossRef]
- Vedam S, Stoll K, Taiwo TK, Rubashkin N, Cheyney M, Strauss N, et al. The Giving Voice to Mothers study: inequity and mistreatment during pregnancy and childbirth in the United States. Reprod Health. 2019 Jun 11;16(1):77. [CrossRef]
- Afulani PA, Altman MR, Castillo E, Bernal N, Jones L, Camara T, et al. Adaptation of the Person-Centered Maternity Care Scale in the United States: Prioritizing the Experiences of Black Women and Birthing People. Womens Health Issues. 2022 Jul 1;32(4):352–61. [CrossRef]
- Cohen S, Kamarck T, Mermelstein R. A global measure of perceived stress. J Health Soc Behav. 1983;24(4):385–96. [CrossRef]
- Shannon G, Minckas N, Tan D, Haghparast-Bidgoli H, Batura N, Mannell J. Feminisation of the health workforce and wage conditions of health professions: an exploratory analysis. Hum Resour Health. 2019 Dec;17(1):72.
- Patel SJ, Truong S, DeAndrade S, Jacober J, Medina M, Diouf K, et al. Respectful Maternity Care in the United States-Characterizing Inequities Experienced by Birthing People. Matern Child Health J. 2024 Jul;28(7):1133–47. [CrossRef]
- Green CL, Perez SL, Walker A, Estriplet T, Ogunwole SM, Auguste TC, et al. The Cycle to Respectful Care: A Qualitative Approach to the Creation of an Actionable Framework to Address Maternal Outcome Disparities. Int J Environ Res Public Health. 2021 May 6;18(9):4933. [CrossRef]
- Cantor AG, Jungbauer RM, Skelly AC, Hart EL, Jorda K, Davis-O’Reilly C, et al. Respectful Maternity Care : A Systematic Review. Ann Intern Med. 2024 Jan;177(1):50–64.
- Afulani PA, Kelly AM, Buback L, Asunka J, Kirumbi L, Lyndon A. Providers’ perceptions of disrespect and abuse during childbirth: a mixed-methods study in Kenya. Health Policy Plan. 2020 Jun 1;35(5):577–86. [CrossRef]
- Mohamoud YA. Vital Signs: Maternity Care Experiences — United States, April 2023. MMWR Morb Mortal Wkly Rep [Internet]. 2023 [cited 2023 Oct 2];72. Available from: https://www.cdc.gov/mmwr/volumes/72/wr/mm7235e1.htm.
- L’Ecuyer KM, Subramaniam DS, Swope C, Lach HW. An Integrative Review of Response Rates in Nursing Research Utilizing Online Surveys. Nurs Res. 2023 Dec;72(6):471. [CrossRef]
- Chervenak FA, McLeod-Sordjan R, Pollet SL, De Four Jones M, Gordon MR, Combs A, et al. Obstetric violence is a misnomer. Am J Obstet Gynecol. 2024 Mar;230(3S):S1138–45. [CrossRef]
- Salter C, Wint K, Burke J, Chang JC, Documet P, Kaselitz E, et al. Overlap between birth trauma and mistreatment: a qualitative analysis exploring American clinician perspectives on patient birth experiences. Reprod Health. 2023 Apr 21;20(1):63. [CrossRef]
- Khatri N, Brown GD, Hicks LL. From a blame culture to a just culture in health care. Health Care Manage Rev. 2009;34(4):312–22. [CrossRef]
| Variable | N (%) |
|---|---|
| Occupation | |
| Nurse | 23 (50.0%) |
| Midwife | 8 (17.4%) |
| Physician | 15 (32.6%) |
| Age | |
| Less than 30 years old | 10 (21.7%) |
| 30-39 years old | 17 (37%) |
| 40-49 years old | 8 (17.4%) |
| 50 or older | 11 (23.9%) |
| Gender | |
| Man | 4 (8.7%) |
| Woman | 42 (91.3%) |
| Other | 0 (0%) |
| Education | |
| Associate’s degree or diploma program (ex: ADN) | 1 (2.2%) |
| Bachelor’s degree (ex: BSN) | 19 (41.3%) |
| Master’s degree (ex: MSN, CNM) | 11 (23.9%) |
| Doctorate degree (ex: MD, DNP) | 15 (32.6%) |
| Race | |
| Asian or Pacific Islander | 3 (6.5%) |
| Black or African American | 3 (6.5%) |
| White | 37 (80.4%) |
| Multiracial/Other race | 2 (4.3%) |
| NA | 1 (2.2%) |
| Ethnicity | |
| Hispanic or Latino | 3 (6.5%) |
| Non-Hispanic or non-Latino | 42 (91.3%) |
| NA | 1 (2.2%) |
| Years of Experience at MGH | |
| 1-4 years | 27 (58.7%) |
| 5-9 years | 5 (10.9%) |
| 10-14 years | 1 (2.2%) |
| 15+ years | 13 (28.3%) |
| Years of Experience in Obstetric Care | |
| 1-4 years | 18 (39.1%) |
| 5-9 years | 9 (19.6%) |
| 10-14 years | 3 (6.5%) |
| 15+ years | 16 (34.8%) |
| Domain of disrespect | Item | N (%) |
|---|---|---|
| Verbal disrespect | Dismissing/disbelieving a patient’s reports of pain | 40 (87.0%) |
| Scolding | 29 (63.0%) | |
| Threatening with unnecessary C-Section | 19 (41.3%) | |
| Other verbal/psychological disrespect | 19 (41.3%) | |
| Derogatory comment | 14 (30.4%) | |
| Physical disrespect | Vigorous/uncomfortable vaginal examinations | 30 (65.2%) |
| Not allowing patients position of choice in birth | 29 (63.0%) | |
| Other physical disrespect | 9 (19.6%) | |
| Restraining | 4 (8.7%) | |
| Privacy violations/ Neglect/ Unnecessary procedures | Asking private questions in the presence of others | 27 (58.7%) |
| Leaving patients unattended for long periods of time | 25 (54.3%) | |
| Neglecting a patient | 24 (52.2%) | |
| Medically unnecessary C-section | 15 (32.6%) | |
| Medically unnecessary episiotomy | 13 (28.3%) | |
| Delivery or examination in public | 3 (6.5%) | |
| Other disrespectful/abusive actions | 2 (4.3%) | |
| Discriminatory care | Discriminatory care based on physical characteristics | 31 (67.4%) |
| Discriminatory care based on race | 30 (65.2%) | |
| Discriminatory care based on culture | 28 (60.9%) | |
| Discriminatory care based on language | 21 (45.7%) | |
| Discriminatory care based on age | 20 (43.5%) | |
| Discriminatory care based on immigration status | 14 (30.4%) | |
| Discriminatory care based on number of children | 14 (30.4%) | |
| Discriminatory care based on socio-economic status | 13 (28.3%) | |
| Discriminatory care based on gender identity or sexual orientation | 12 (26.1%) | |
| Discriminatory care based on marital status | 6 (13%) | |
| Discriminatory care based on insurance status | 4 (8.7%) | |
| Discriminatory care based on other patient characteristic | 3 (6.5%) | |
| Performance of procedures without explanation | Artificial rupture of membrane | 18 (39.1%) |
| Episiotomy | 16 (34.8%) | |
| Stripping membrane | 16 (34.8%) | |
| Rectal exam | 11 (23.9%) | |
| Vaginal exam | 11 (23.9%) | |
| Placement of FSE or IUPC | 10 (21.7%) | |
| Placement of Foley catheter | 7 (15.2%) | |
| C-section | 6 (13%) | |
| Shaving | 6 (13%) | |
| Stitching | 5 (10.9%) | |
| Placement of straight catheter | 5 (10.9%) | |
| Injection | 4 (8.7%) | |
| Use of assistive device for delivery | 3 (6.5%) | |
| Blood transfusion | 1 (2.2%) | |
| Sterilization | 1 (2.2%) | |
| Other procedure | 1 (2.2%) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




