Submitted:
22 July 2024
Posted:
24 July 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Material and Methods
2.1. Patients
2.2. Treatment
2.3. Follow-Up
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed consent
Data Availability Statement
Conflicts of Interest
References
- Sanderson RJ, Ironside JA. Squamous cell carcinomas of the head and neck. BMJ. 2002, 325, 822-827. [CrossRef]
- Eckel HE. Recent advances in the treatment of laryngeal and hypopharyngeal carcinoma. HNO. 2012, 60, 6-18. [CrossRef]
- Che J et al. Comparative efficacy of six therapies for Hypopharyngeal and laryngeal neoplasms. a network meta-analysis. BMC Cancer. 2019, 19, 282. [CrossRef]
- Yujiao Li, Chaosu Hu. Clinical manifestations of hypopharynx squamous cell carcinoma and treatment outcomes. International Journal of Clinical Practice. 2021, 75, e14059 . [CrossRef]
- Hans EE, Patrick JB. Treatment Options for Hypopharyngeal Cancer. Adv Otorhinolaryngol. 2019, 83, 7-53. [CrossRef]
- Patricia GC et al. Matched-Pair Analysis of Survival in the Patients with Advanced Laryngeal and Hypopharyngeal Squamous Cell Carcinoma Treated with Induction Chemotherapy Plus Chemo-Radiation or Total Laryngectomy. Cancers. 2021, 13, 1735. [CrossRef]
- Kuo P, Chen MM, Decker RH, Wendell GY, Benjamin LJ. Hypopharyngeal cancer incidence, treatment, and survival: temporal trends in the United States. Laryngoscope. 2014, 124, 2064-2069. [CrossRef]
- Blanchard P. et al. Meta-analysis of chemotherapy in head and neck cancer (MACH-NC): A comprehensive analysis by tumour site. Radiother. Oncol. 2011, 100, 33-40. [CrossRef]
- Lacas B. et al. Meta-analysis of chemotherapy in head and neck cancer (MACH-NC): An update on 107 randomized trials and 19,805 patients, on behalf of MACH-NC Group. Radiother. Oncol. 2021, 156, 281-293. [CrossRef]
- Al-Mamgani A et al. Toxicity, quality of life, and functional outcomes of 176 hypopharyngeal cancer patients treated by (chemo)radiation: the impact of treatment modality and radiation technique. Laryngoscope. 2012, 122, 1789–1795. [CrossRef]
- Blanchard P. et al. Definitive radiotherapy for squamous cell carcinoma of the pyriform sinus. Radiother. Oncol. 2012, 105, 232–237. [CrossRef]
- Forastiere AA. et al. Long-term results of Intergroup RTOG 91-11: A phase III trial to preserve the larynx Induction cisplatin/5-FU and radiation therapy versus concurrent cisplatin and radiation therapy versus radiation therapy. Journal of Clinical Oncology 2006, 5517, 18S. [CrossRef]
- Lefebvre JL. et al. Larynx preservation in pyriform sinus cancer: preliminary results of a European Organization for Research and Treatment of Cancer phase III trial. EORTC Head and Neck Cancer Cooperative Group. J. Natl. Cancer Inst. 1996, 88, 890–899. [CrossRef]
- Lefebvre JL. et al. Laryngeal preservation with induction chemotherapy for hypopharyngeal squamous cell carcinoma: 10-year results of EORTC trial 24891. Annals of Oncology. 2012, 23, 2708–2714. [CrossRef]
- Edge, S. American Joint Committee on Cancer (AJCC). Cancer staging handbook 7th ed. 2010, 41-56 (Lippincott Williams & Wilkins).
- Eisenhauer EA. et al. New response evaluation criteria in solid tumours: Revised RECIST guideline (version 1.1). European Journal of Cancer. 2009, 45, 228–47. pmid:19097774. [CrossRef]
- Newman JR. et al. Survival trends in hypopharyngeal cancer: a population-based review. Laryngoscope. 2015, 125, 624-629. [CrossRef]
- Takes RP. et al. Current trends in initial management of hypopharyngeal cancer: the declining use of open surgery. Head Neck. 2012, 34, 270-281. [CrossRef]
- Taguchi T. et al. Treatment results and prognostic factors for advanced squamous cell carcinoma of the hypopharynx treated with concurrent chemoradiotherapy. Cancer Chemother. Pharmacol. 2014, 73, 1147-1154. [CrossRef]
- Wang YL. et al. Impact of lymph node ratio on the survival of patients with hypopharyngeal squamous cellcarcinoma: a population-based analysis. PLoS One 8. 2013, e56613. [CrossRef]
- Krstevska V, Stojkovski I, Zafirova-Ivanovska B, Crvenkova S. Prognostic factors in patients with advanced hypopharyngeal squamous cell carcinoma treated with concurrent chemoradiotherapy. J. BUON. 2012, 17, 327-336. PMID: 22740214.
- Forastiere AA. et al. Concurrent chemotherapy and radiotherapy for organ preservation in advanced laryngeal cancer. N. Engl. J. Med. 2003, 349, 2091-2098. [CrossRef]
- Prades JM. et al. Randomized phase III trial comparing induction chemotherapy followed by radiotherapy to concomitant chemoradiotherapy for laryngeal preservation in T3M0 pyriform sinus carcinoma. Acta Otolaryngol. 2010, 130, 150-155. [CrossRef]
- Lefebvre JL. et al. Laryngeal preservation with induction chemotherapy for hypopharyngeal squamous cell carcinoma: 10-year results of EORTC trial 24891. Ann. Oncol. 2012, 23, 2708-2714. [CrossRef]
- Lefebvre J. et al. Phase 3 randomized trial on larynx preservation comparing sequential vs alternating chemotherapy and radiotherapy. J. Natl. Cancer Inst. 2009, 101, 142-152. [CrossRef]
- Pignon JP, le Maitre A, Maillard E, Jean B. Meta-analysis of chemotherapy in head and neck cancer (MACH-NC): An update on 93 randomised trials and 17,346 patients. Radiother. Oncol. 2009, 92, 4–14. [CrossRef]
- Hall SF, Griffiths R. Did the addition of concomitant chemotherapy to radiotherapy improve outcomes in hypopharyngeal cancer? A population-based study. Curr. Oncol. 2016, 23, 266-72. [CrossRef]
- Gupta T. et al. Squamous cell carcinoma of the hypopharynx: single-institution outcome analysis of a large cohort of patients treated with primary non-surgical approaches. Acta Oncol. 2009, 48, 541–548. [CrossRef]
- Huang WY. et al. Intensity modulated radiotherapy with concurrent chemotherapy for larynx preservation of advanced resectable hypopharyngeal cancer. Radiat. Oncol. 2010, 5, 37. [CrossRef]
- Reis I. et al. Locally advanced hypopharyngeal squamous cell carcinoma: single-institution outcomes in a cohort of patients curatively treated either with or without larynx preservation. Radiol. Bras. 2016, 49, 21–25. [CrossRef]
- Mok G. et al. Outcomes of intensity-modulated radiotherapy versus conventional radiotherapy for hypopharyngeal cancer. Head Neck. 2015, 37, 655-661. [CrossRef]
- Evangelia K. et al. Hypopharyngeal Squamous Cell Carcinoma: Three-Dimensional or Intensity-Modulated Radiotherapy? A Single Institution’s Experience. Laryngoscope. 2016, 126, 620–626. [CrossRef]
- Bertelsen A, Hansen CR, Johansen J, Carsten B. Single Arc Volumetric Modulated Arc Therapy of head and neck cancer. Radiother. Oncol. 2010, 95, 142-148. [CrossRef]
- Suat K. et al. Radiotherapy modality as a predictor of survival in hypopharyngeal cancer. Head Neck. 2018, 40, 2441-2448. [CrossRef]
- Olmi P et al. Staging and follow-up of nasopharyngeal carcinoma: magnetic resonance imaging versus computerized tomography. Int J Radiat Oncol Biol Phys. 1995, 32, 795-800. [CrossRef]
- Vellayappan BA et al. Accuracy of (18)Fflurodeoxyglucose- positron emission tomography/computed tomography in the staging of newly diagnosed nasopharyngeal carcinoma: A systematic review and meta-analysis. Radiol Oncol. 2014, 48, 331-338. [CrossRef]
- Nguyen NP. et al. Feasibility of intensity-modulated and image-guided radiotherapy for functional organ preservation in locally advanced laryngeal cancer. PLoS One. 2012, 7, e42729. [CrossRef]
- Nguyen NP. et al. Feasibility of tomotherapy-based image-guided radiotherapy for locally advanced oropharyngeal cancer. PLoS One. 2013, 8, e60268. [CrossRef]
- Fang FM. et al. Intensity-modulated or Conformal Radiotherapy Improves the Quality of Life of Patients With Nasopharyngeal Carcinoma. Comparisons of Four Radiotherapy Techniques. Cancer. 2007, 109, 313-321. [CrossRef]
- Eisbruch A. et al. Chemo-IMRT of oropharyngeal cancer aiming to reduce dysphagia: swallowing organs late complication probabilities and dosimetric correlates. Int. J. Radiat. Oncol. Biol. Phys. 2011, 81, e93–e99. [CrossRef]
- Schwartz DL. et al. Candidate dosimetric predictors of long-term swallowing dysfunction after oropharyngeal intensity modulated radiotherapy. Int. J. Radiat. Oncol. Biol. Phys. 2010, 78, 1356–1365. [CrossRef]
- Lee WT. et al. Risk factors for hypopharyngeal/upper esophageal stricture formation after concurrent chemoradiation. Head Neck 2006, 28, 808–812. [CrossRef]
| Convantionally 2DRT Group 1 n (%) |
3DCRT/VMAT Radiotherapy Group 2 n (%) | Total n (%) |
P Value | |
|---|---|---|---|---|
| Gender Female Male |
9 (29.0) 22 (71.0) |
18 (36.0) 32 (64.0) |
27 (33.3) 54 (66.7) |
p=0.345 |
| Age < 60 ≥60 |
22 (71.0) 9 (29.0) |
21 (42.0) 29 (58.0) |
43 (53.1) 38 (46.9) |
p=0.013 |
| KPS ≥90 70-80 |
9 (29.0) 22 (71.0) |
31 (62.0) 19 (38.0) |
40 (49.4) 41 (50.6) |
p=0.004 |
| Clinical T stage T2-T3 T4 |
3 (9.7) 28 (90.3) |
23 (46.0) 27 (54.0) |
26 (32.1) 55 (67.9) |
p<0.01 |
| Clinical N stage N0 N1-N2 N3 |
11 (35.5) 11 (35.5) 9 (29.0) |
25 (50.0) 23 (46.0) 2 (4.0) |
36 (44.4) 35 (42.0) 11 (13.6) |
p=0.012 |
| Clinical stage Stage 3 Stage 4a Stage 4b |
1 (3.2) 21 (67.8) 9 (29.0) |
11 (22.0) 36 (72.0) 3 (6.0) |
12 (14.8) 57 (70.4) 12 (14.8) |
p=0.013 |
| Chemotherapy No chemotherapy Neoadjuvant chemotherapy + concurrent chemotherapy Concurrent chemotherapy |
22 (71.0) 3 (9.7) 6 (19.4) |
14 (28.0) 2 (4.0) 34 (68.0) |
36 (44.4) 5 (6.2) 40 (49.4) |
p<0.01 |
| Total | 31 (100) | 50 (100) | 81 (100) |
| Variables | Overall Survival | Local-Regional Relapse-Free Survıval | Disease-Specific Survival | |||||||
|---|---|---|---|---|---|---|---|---|---|---|
| N. (%) | 2 Years (%) | 5 Years (%) | P Value | 2 Years (%) | 5 Years (%) | P Value | 2 Years (%) | 5 Years (%) | P Value | |
|
Gender Male Female |
54 (66.7) 27 (33.3) |
52.7 37.6 |
35.1 32.9 |
0.354 |
63.4 51.8 |
58.2 51.8 |
0.200 |
51.8 45.0 |
42.9 45.0 |
0.310 |
|
Age (years) <60 ≥60 |
43 (53.1) 38 (46.9) |
55.1 38.7 |
36.0 31.4 |
0.364 |
72.6 51.3 |
62.2 47.4 |
0.108 |
56.6 44.9 |
42.0 41.4 |
0.428 |
|
KPS ≥90 70-80 |
40 (49.4) 41 (50.6) |
73.8 22.2 |
57.6 11.9 |
<0.001 |
78.0 41.9 |
78.0 31.4 |
<0.001 |
67.0 32.8 |
63.8 20.5 |
<0.001 |
|
T stage T2-3 T -4 |
26 (32.1) 68 (67.9) |
79.3 30.2 |
48.0 25.7 |
0.002 |
89.8 44.4 |
89.8 40.0 |
<0.001 |
78.3 34.3 |
73.0 28.3 |
<0.001 |
|
N stage No N (+) |
36 (44.4) 45 (55.6) |
53.7 40.0 |
43.8 25.5 |
0.012 |
67.1 53.3 |
67.1 45.6 |
0.049 |
64.1 37.1 |
64.1 26.4 |
0.014 |
|
Stage Stage 2-3 Stage 4 |
12 (14.8) 69 (85.2) |
75.0 41.2 |
56.3 30.0 |
0.047 |
100 51.5 |
100 47.5 |
0.005 |
83.3 42.0 |
83.3 34.7 |
0.010 |
|
Chemotherapy Yes No |
44 (54.3) 37 (45.7) |
58.3 31.3 |
43.2 21.9 |
0.045 |
73.0 42.1 |
67.0 42.1 |
0.024 |
62.6 31.3 |
54.4 27.4 |
0.010 |
|
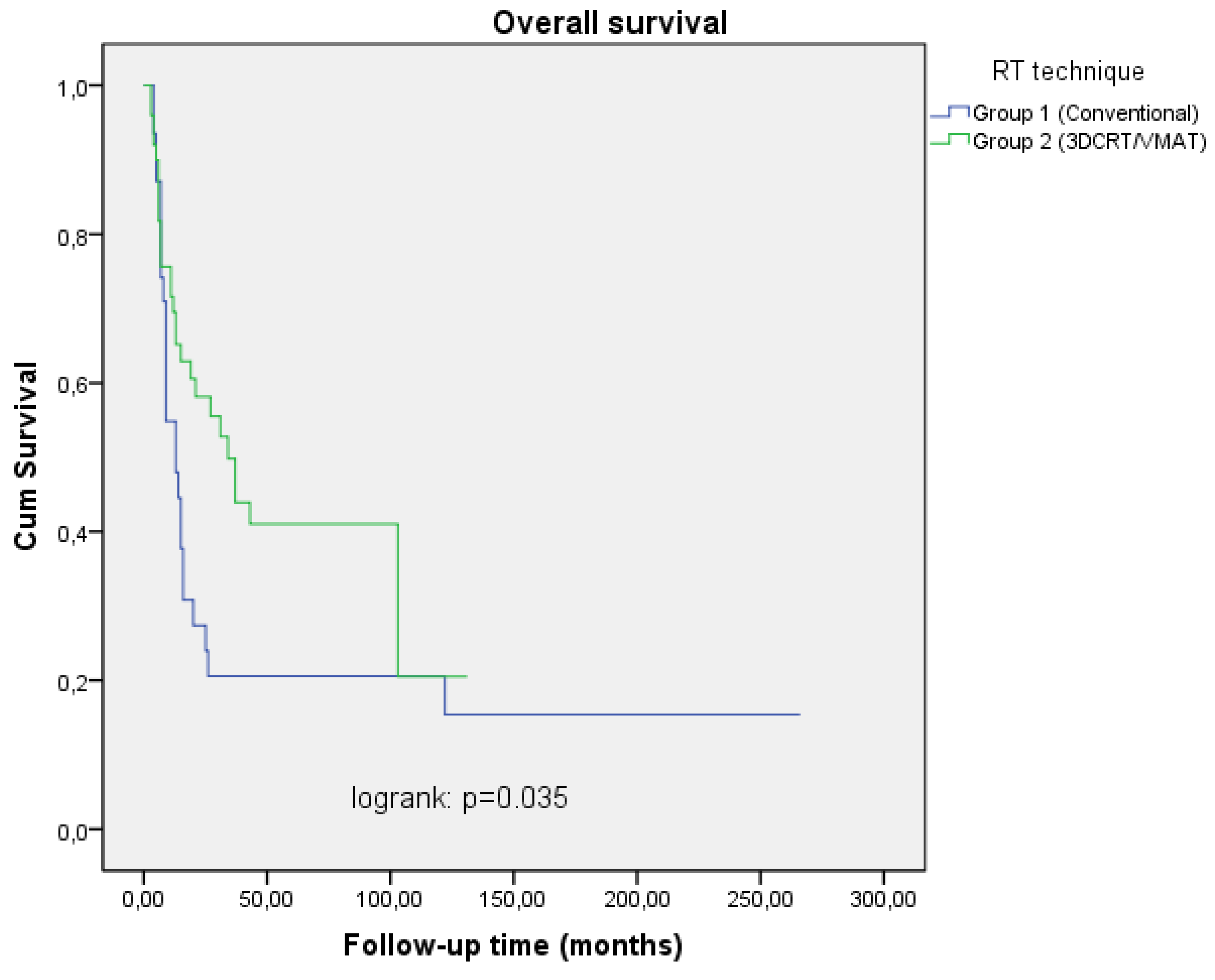
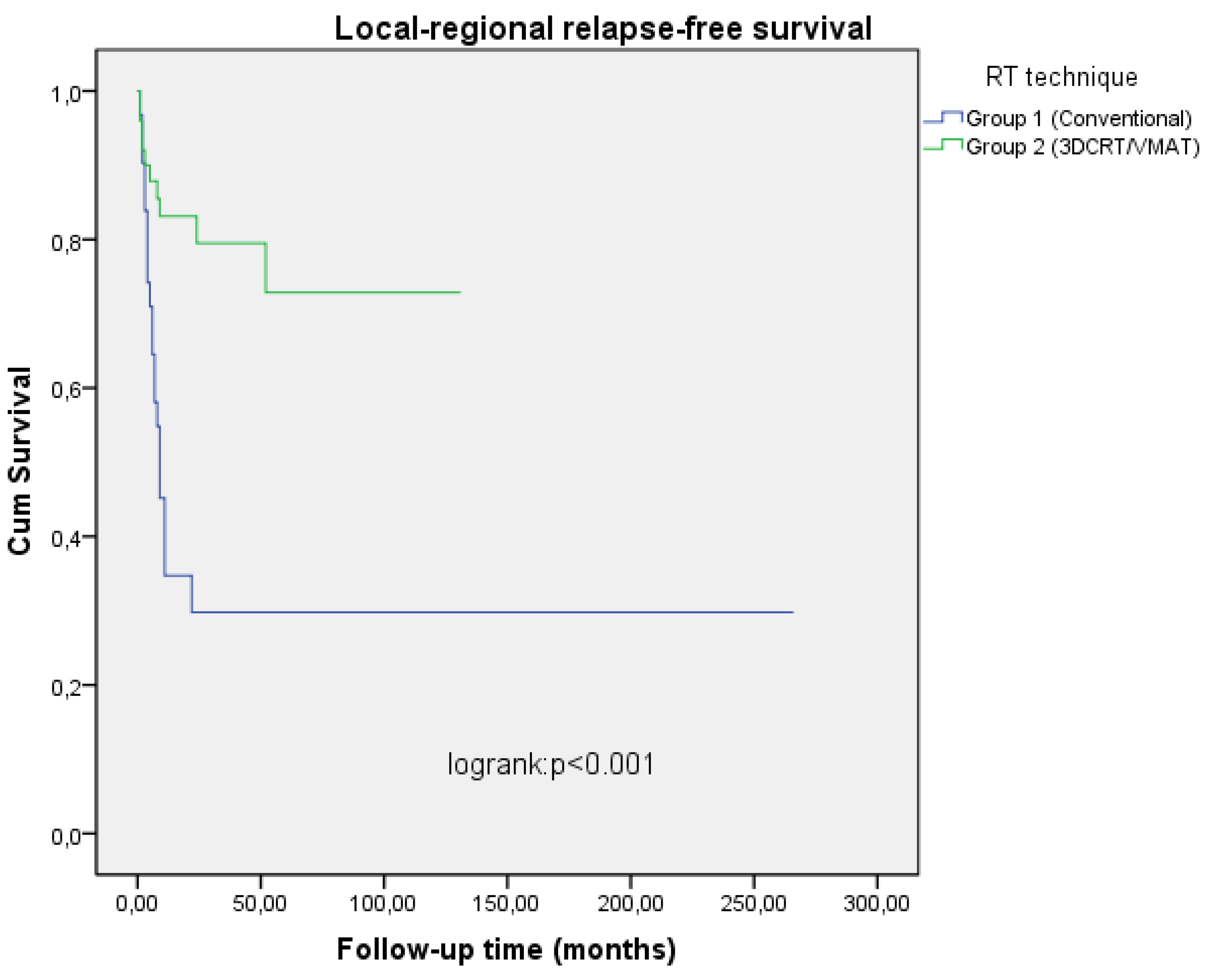
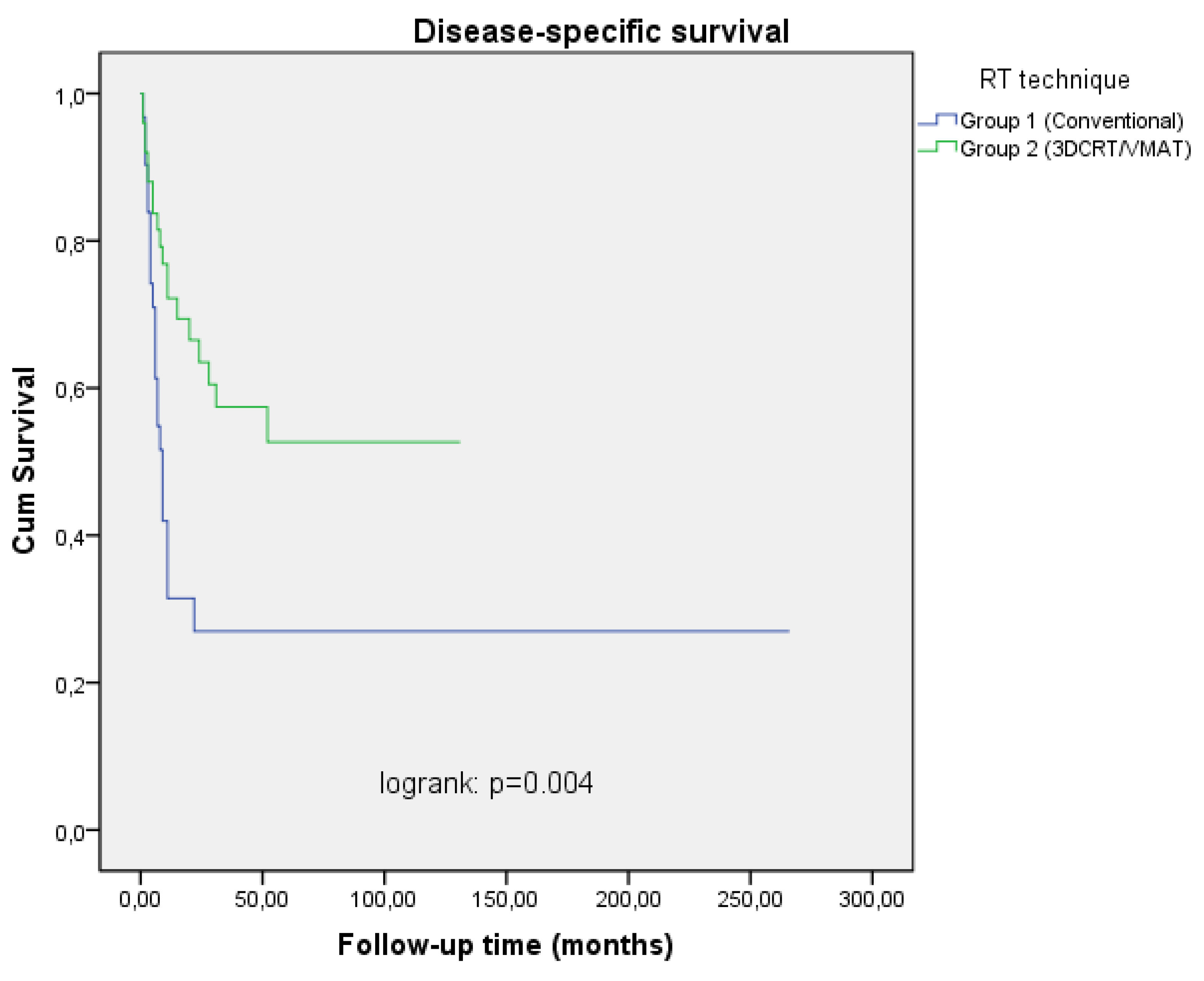
RT technique Conventionally 3DCRT/VMAT |
31 (38.3) 50 (61.7) |
27.4 58.3 |
20.6 42.1 |
0.035 |
34.7 79.5 |
29.8 72.9 |
<0.001 |
31.5 63.5 |
27.0 52.7 |
0.004 |
| Variable | Overall Survival | local-Regional Relapse-Free Survival | Disease-Spesific Survival |
|---|---|---|---|
| P Value | P Value | P Value | |
| Gender | 0.142 | 0.373 | 0.135 |
| Age | 0.027 | 0.477 | 0.213 |
| KPS | <0.001 | 0.002 | 0.001 |
| Clinical T stage | 0.001 | 0.020 | 0.001 |
| Clinical N stage | 0.013 | 0.026 | 0.018 |
| Stage | 0.072 | 0.741 | 0.210 |
| Chemotherapy | 0.531 | 0.239 | 0.213 |
| Radiotherapy Technique | 0.048 | 0.025 | 0.106 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




