Submitted:
15 July 2024
Posted:
16 July 2024
You are already at the latest version
Abstract
Keywords:
Introduction
Methods
Study Design, Study Population, and Data Collection
Retrospective Clinical Cohort
Prospective Exploratory Cohort
Data Collection
Endpoints
Immunophenotyping
Serum Analyses
Statistical Analysis
Results
Study Population
Retrospective Clinical Cohort
Prospective Exploratory Cohort
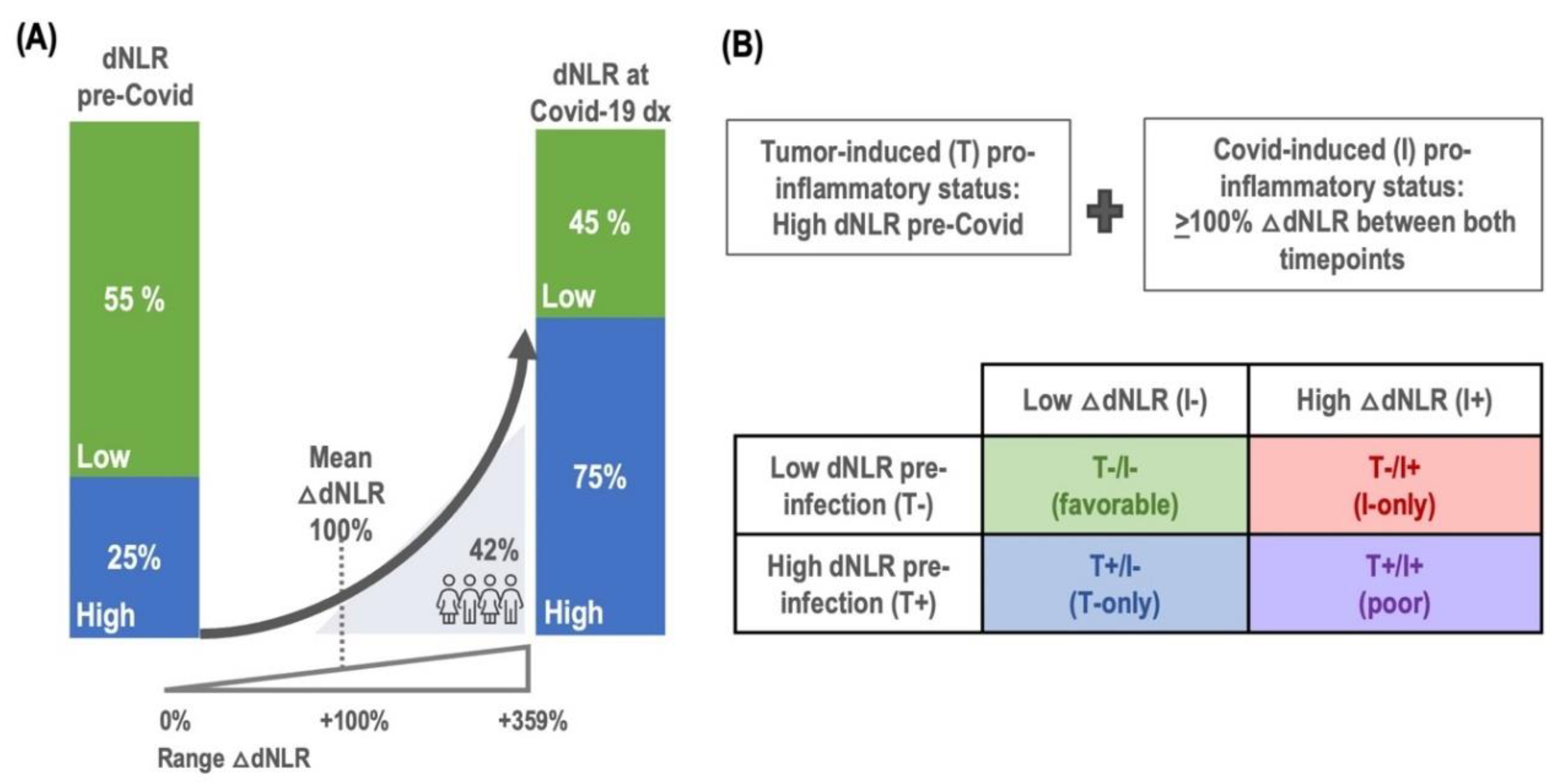
dNLR in Patients with Cancer and Covid-19 Infection
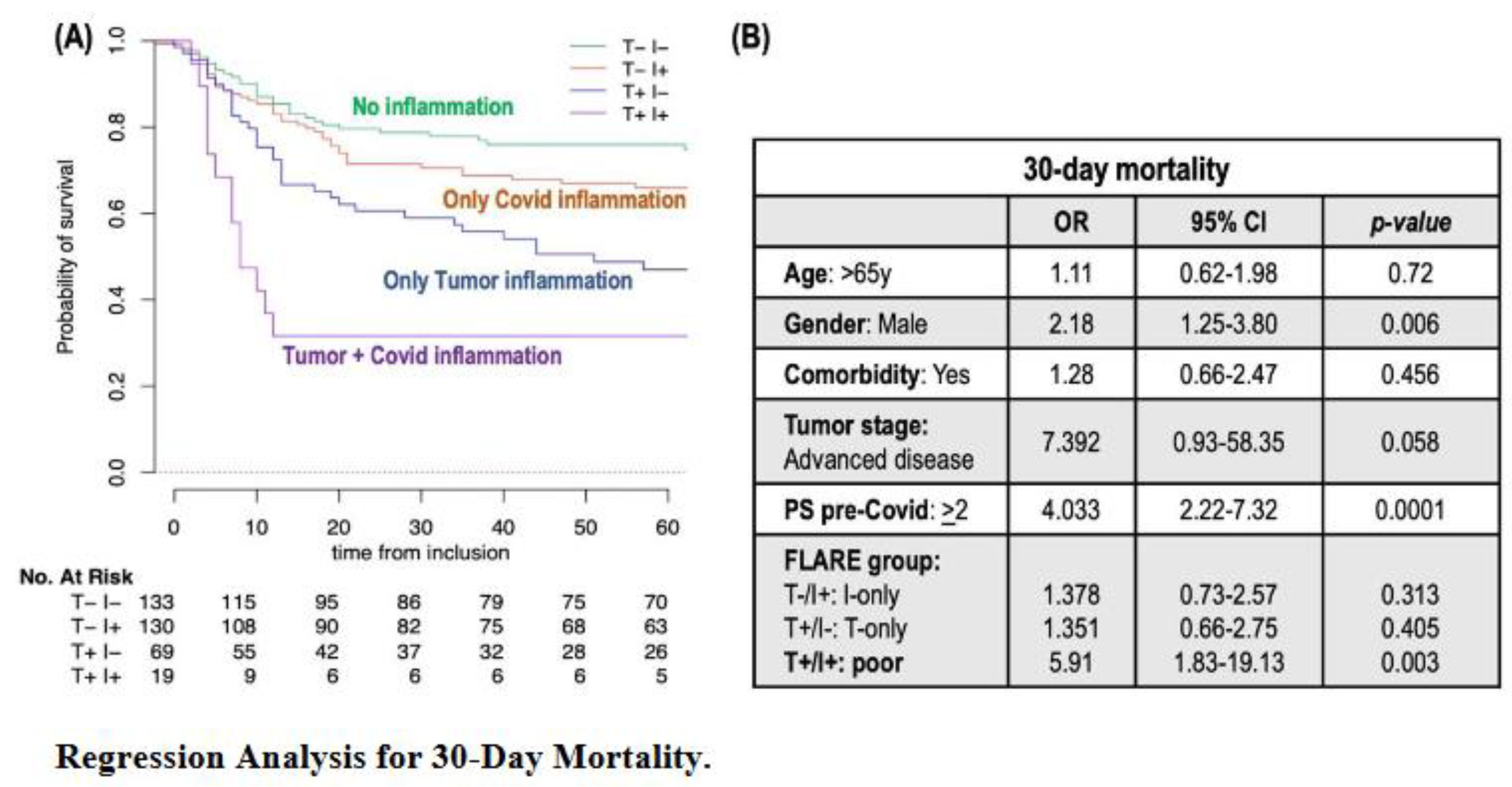
Building of the FLARE Score
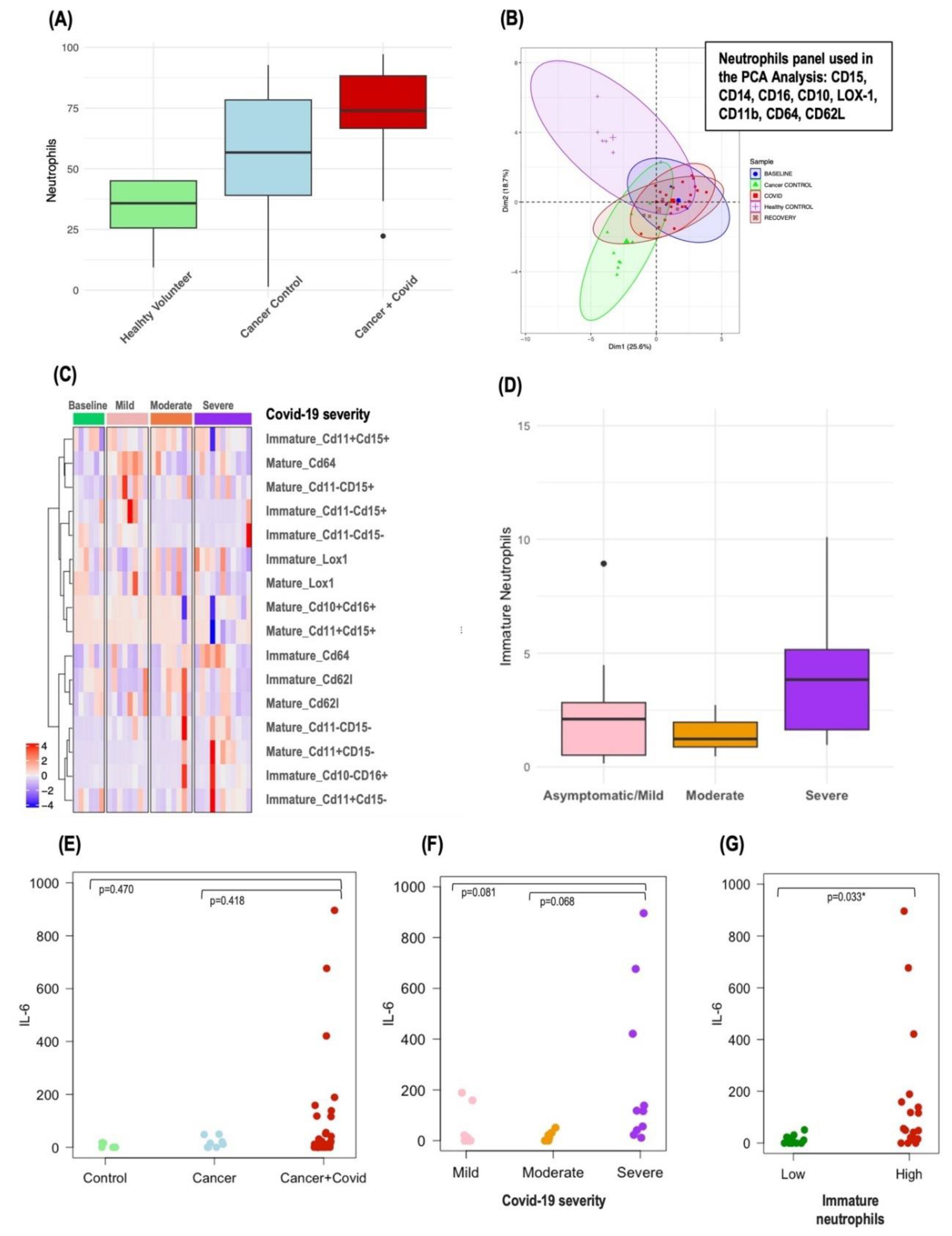
Circulating Neutrophils in Patients with Cancer and Covid-19 Infection
Circulating Immature Neutrophils in Patients with Cancer and Covid-19 Infection
Correlation between Circulating Inflammatory Cytokines, Circulating Immature Neutrophils, and Circulating Inflammatory Markers (dNLR) in Patients with Cancer and Covid-19 Infection
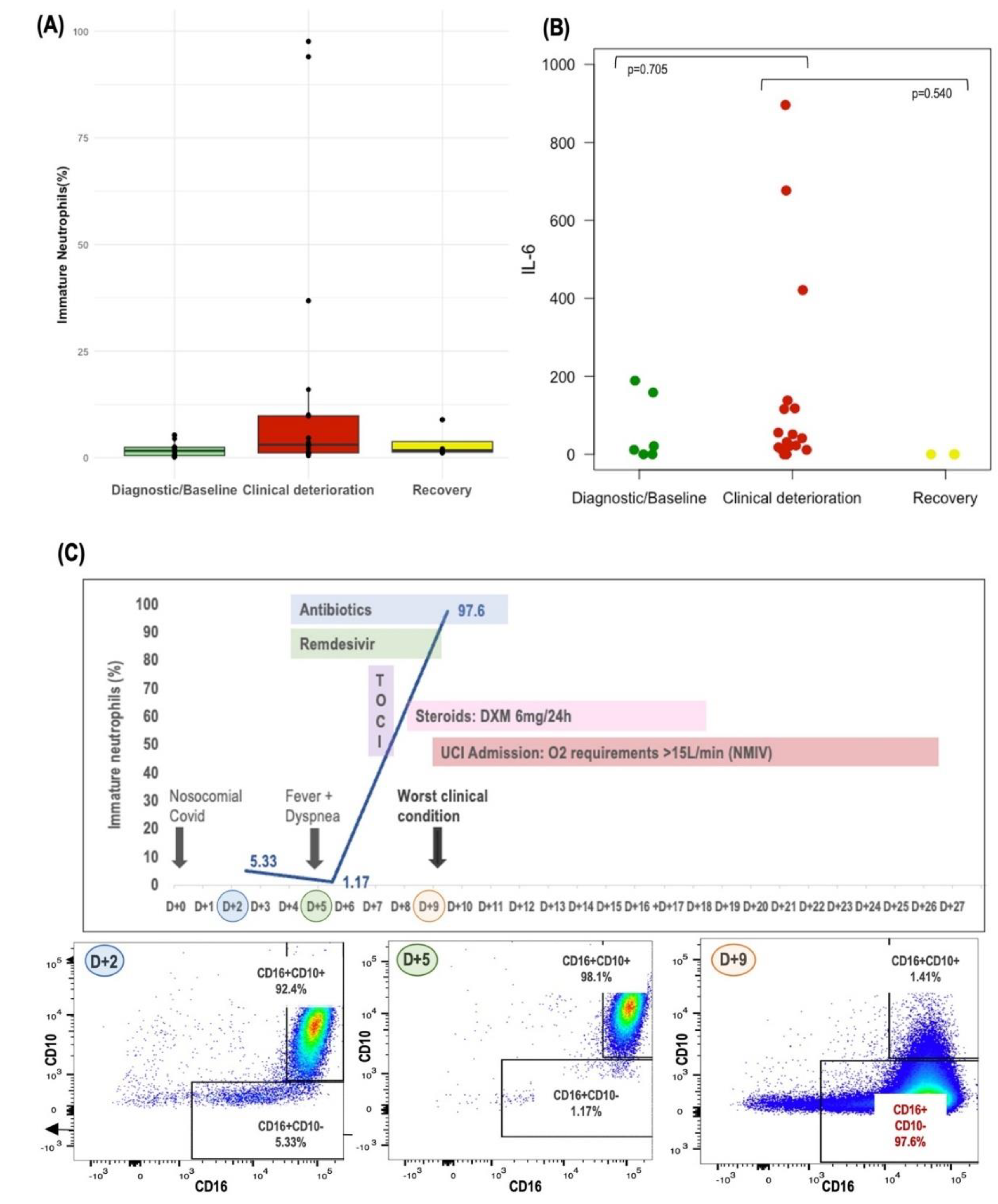
Monitoring of Circulating Neutrophils and IL-6
Discussion
Conclusions
Ethic statement
Declaration of Interest
Data sharing statement
Code availability statement
Declaration of generative AI in scientific writing:
Author Contributions
Funding
Acknowledgments
References
- Pinato DJ, Zambelli A, Aguilar-Company J, et al. Clinical portrait of the SARS-CoV-2 epidemic in European cancer patients. Cancer Discov. 2020;10(10):1465-1474.
- Pinato DJ, Lee AJX, Biello F, et al. Presenting features and early mortality from SARS-CoV-2 infection in cancer patients during the initial stage of the COVID-19 pandemic in Europe. Cancers. 2020;12.
- Kuderer NM, Choueiri TK, Shah DP, et al. COVID-19 and Cancer Consortium. Clinical impact of COVID-19 on patients with cancer (CCC19): a cohort study. Lancet. 2020;395(10241):1907-1918.
- Meizlish ML, Pine AB, Bishai JD, et al. A neutrophil activation signature predicts critical illness and mortality in COVID-19. Blood Adv. 2021;5(5):1164-1177. [CrossRef]
- Schulte-Schrepping J, Reusch N, Paclik D, et al. Severe COVID-19 Is Marked by a Dysregulated Myeloid Cell Compartment. Cell. 2020;182(6):1419-1440.e23.
- Barnes BH, Adrover JM, Baxter-Stoltzfus A, et al. Targeting potential drivers of COVID-19: Neutrophil extracellular traps. J Exp Med. 2020;217(6).
- Aschenbrenner AC, Mouktaroudi M, Krämer B, et al. Disease severity-specific neutrophil signatures in blood transcriptomes stratify COVID-19 patients. Genome Med. 2021;13(1):7.
- Liu J, Liu Y, Xiang P, et al. Neutrophil-to-Lymphocyte Ratio Predicts Severe Illness Patients with 2019 Novel Coronavirus in the Early Stage. J Transl Med. 2020;18(1):206.
- Hazeldine J, Lord JM. Neutrophils and COVID-19: Active Participants and Rational Therapeutic Targets. Front Immunol. 2021;12:680134.
- García de Guadiana-Romualdo L, Rodríguez Rojas C, et al. Circulating levels of calprotectin, a signature of neutrophil activation in prediction of severe respiratory failure in COVID-19 patients: a multicenter, prospective study (CalCov study). Inflamm Res. 2022;71(1):57-67.
- Templeton AJ, Mairéad G, Mc Namara MG, et al. Prognostic Role of Neutrophil-to-Lymphocyte Ratio in Solid Tumors: A Systematic Review and Meta-Analysis. J Natl Cancer Inst. 2014;106(6).
- Mackey JB, Coffelt SB, Carlin LM. Neutrophil Maturity in Cancer. Front Immunol. 2019.
- Mezquita L, Preeshagul I, Auclin E, et al. Predicting immunotherapy outcomes under therapy in patients with advanced NSCLC using dNLR and its early dynamics. Eur J Cancer. 2021;151:211-220. [CrossRef]
- Dettorre GM, Dolly S, Loizidou A, et al. Systemic pro-inflammatory response identifies patients with cancer with adverse outcomes from SARS-CoV-2 infection: the OnCovid Inflammatory Score. J Immunother Cancer. 2021;9(3):e002277.
- Cortellini A, Gennari A, Pommeret F, et al. COVID-19 Sequelae and the Host Proinflammatory Response: An Analysis From the OnCovid Registry. JNCI 2022; 114(7): 979–987.
- Mc Millan, DC. The systemic inflammation-based Glasgow Prognostic Score: a decade of experience in patients with cancer. Cancer Treat Rev. 2013;39(5):534-540.
- Charrier M, Mezquita L, Lueza B, et al. Circulating innate immune markers and outcomes in treatment-naïve advanced non-small cell lung cancer patients. Eur J Cancer. 2019;108:88-96.
- Suzuki R, Takagi T, Hikichi T, et al. Derived neutrophil/lymphocyte ratio predicts gemcitabine therapy outcome in unresectable pancreatic cancer. Oncol Lett. 2016;11(5):3441-3445.
- vanKessel KEM, de Haan LM, Fransen van de Putte EE, et al. Elevated derived neutrophil-to-lymphocyte ratio corresponds with poor outcomes in patients undergoing pre-operative chemotherapy in muscle-invasive bladder cancer. Bladder Cancer. 2016;2(3):351-360.
- Amato RJ, Flaherty A, Zhang Y, et al. Clinical prognostic factors associated with outcome in patients with renal cell cancer with prior tyrosine kinase inhibitors or immunotherapy treated with everolimus. Urol Oncol. 2014;32(3):345-354.
- Silvestre-Roig C, Fridlender ZG, Glogauer M, Scapini P. Neutrophil Diversity in Health and Disease. Trends Immunol. 2019;40(7):565-583.
- Arasanz H, Bocanegra AI, Morilla I, et al. Circulating Low Density Neutrophils Are Associated with Resistance to First Line Anti-PD1/PDL1 Immunotherapy in Non-Small Cell Lung Cancer. Cancers. 2022;14(16):3846.
- Daix T, Guerin E, Tavernier E, et al. Multicentric standardized flow cytometry routine assessment of patients with sepsis to predict clinical worsening. Chest. 2018;154(3):617-627.
- Coffelt SB, Wellenstein MD, de Visser KE. Neutrophils in cancer: neutral no more. Nat Rev Cancer. 2016;16(7):431-446.
- Shaul ME, Eyal O, Guglietta S, et al. Circulating neutrophil subsets in advanced lung cancer patients exhibit unique immune signature and relate to prognosis. FASEB J. 2020;34(3):4204-4218.
- Rice CM, Lewis P, Ponce-Garcia FM, et al. Neutrophils in severe COVID-19 are characterized by a hyperactive immature state and maintained CXCR2 expression. Life Sci Alliance. 2023;6(2):e202201658.
- Carissimo G, Xu W, Kwok I, et al. Whole blood immunophenotyping uncovers immature neutrophil-to-VD2 T-cell ratio as an early marker for severe COVID-19. Nat Commun. 2020;11(1):5243.
- Combadiere B, Adam L, Quentric P, et al. LOX-1+ immature neutrophils predict severe COVID-19 patients at risk of thrombotic complications. Front Immunol. 2021;12:752612.
- Townsend L, Dyer AH, Naughton A, et al. Severe COVID-19 is characterised by inflammation and immature myeloid cells early in disease progression. Heliyon. 2022;8:e09230.
- Han H, Ma Q, Li C, et al. Profiling serum cytokines in COVID-19 patients reveals IL-6 and IL-10 are disease severity predictors. Emerg Microbes Infect. 2020;9(1):1123-1130.
- Herold T, Jurinovic V, Arnreich C, et al. Elevated levels of IL-6 and CRP predict the need for mechanical ventilation in COVID-19. J Allergy Clin Immunol. 2020;146(1):128-136.e4.
- Giamarellos-Bourboulis EJ, Netea MG, Rovina N, et al. Complex Immune Dysregulation in COVID-19 Patients with Severe Respiratory Failure. Cell Host Microbe. 2020;27:992-1000.
- Kumari N, Dwarakanath BS, Das A, Bhatt AN. Role of interleukin-6 in cancer progression and therapeutic resistance. Tumour Biol. 2016;37(9):11553-11572.
- Weber R, Groth C, Lasser S, et al. IL-6 as a major regulator of MDSC activity and possible target for cancer immunotherapy. Cell Immunol. 2021;359:104254.
- Huseni MA, Wang L, Klementowicz JE, et al. CD8+ T cell-intrinsic IL-6 signaling promotes resistance to anti-PD-L1 immunotherapy. Cell Rep Med. 2023;4(1):100878.
- E. Seguí, E. Auclin, D. Casadevall et al. Change of circulating pro-inflammatory markers between preCOVID-19 condition and COVID-19 diagnosis predicts early death in cancer patients: The FLARE score. ESMO 2020. Ann Oncol, September 2020; 31(4):S1008.
- E. Seguí, JM Torres, E. Auclin et al. The FLARE score, circulating neutrophils, and association with COVID-19 outcomes in patients with solid tumors. ASCO 2022. Journal of Clinical Oncology, June 2022; 40(16): suppl.
| FLARE T-/I- razmak(n=140) | FLARE T-/I+razmak(n=136) | FLARE T+/I- razmak(n=74) | FLARE T+/I+razmak(n=19) | p-value | |||||
|---|---|---|---|---|---|---|---|---|---|
| Age (median; range) | 68 (39-93) | 69 (41-96) | 69 (37-88) | 69 (43-82) | 0.852 | ||||
| Gender: male | 60 (43%) | 90 (66%) | 41 (55%) | 12 (63%) | 0.001 | ||||
| Current or former smokers | 73 (53%) | 86 (65%) | 44 (62%) | 7 (44%) | --- | ||||
| ECOG PS <1 | 111 (80%) | 103 (82%) | 44 (62%) | 14 (78%) | <0.001 | ||||
| Comorbidity | |||||||||
| Hypertension | 67 (48%) | 60 (44%) | 43 (60%) | 11 (58%) | 0.166 | ||||
| Cardiovascular | 33 (24%) | 24 (18%) | 16 (22%) | 5 (26%) | 0.613 | ||||
| Cancer-type | |||||||||
| Thoracic | 31 (22%) | 40 (30%) | 28 (38%) | 5 (26%) | --- | ||||
| Genitourinary | 15 (11%) | 17 (13%) | 9 (12%) | 3 (16%) | --- | ||||
| Gastrointestinal | 37 (27%) | 33 (25%) | 15 (20%) | 5 (26%) | --- | ||||
| Breast | 30 (22%) | 20 (15%) | 7 (9%) | 3 (16%) | --- | ||||
| Advanced stage | 88 (63%) | 94 (69%) | 62 (84%) | 18 (95%) | --- | ||||
| Systemic therapy | 89 (64%) | 83 (61%) | 45 (62%) | 15 (79%) | 0.518 | ||||
| Chemotherapy | 59 (54%) | 47 (55%) | 28 (58%) | 13 (87%) | 0.143 | ||||
| Immunotherapy | 17 (19%) | 12 (14%) | 9 (19%) | 1 (7%) | 0.637 | ||||
| Covid-symptoms at diagnosis | |||||||||
| Fever | 97 (69%) | 97 (71%) | 47 (64%) | 13 (68%) | 0.782 | ||||
| Cough | 80 (58%) | 68 (50%) | 39 (53%) | 8 (42%) | 0.494 | ||||
| Dyspnea | 59 (42%) | 64 (47%) | 40 (54%) | 12 (63%) | 0.207 | ||||
| Covid-treatment | |||||||||
| Antibiotics | 99 (73%) | 115 (86%) | 59 (80%) | 16 (89%) | 0.045 | ||||
| Antiviral therapy | 29 (31%) | 37 (38%) | 18 (32%) | 4 (25%) | 0.21 | ||||
| Steroids | 32 (24%) | 27 (21%) | 28 (38%) | 8 (44%) | --- | ||||
| Immunomodulators | 7 (7%) | 12 (13%) | 5 (9%) | 4 (31%) | 0.081 | ||||
| Median hospital stay duration (range) | 18.5 (4-57) | 11.5 (2-44) | 18 (2-73) | 6 (2-23) | 0.177 | ||||
| Table 1B. Covid-19 outcomes across FLARE groups. | |||||||||
| FLARE T-/I- razmak(n=140) | FLARE T-/I+razmak(n=136) | FLARE T+/I- razmak(n=74) | FLARE T+/I+razmak(n=19) | p-value | |||||
| Admission to ICU | 7 (8 %) | 11 (14%) | 7 (15%) | 2 (18%) | 0.425 | ||||
| Severe acute respiratory failure | 25 (20%) | 36 (30%) | 18 (27%) | 6 (38%) | 0.19 | ||||
| Covid-19 complications | 67 (54%) | 91 (75%) | 53 (79%) | 14 (88%) | <0.001 | ||||
| 30-day mortality | 29 (23%) | 42 (33%) | 27 (39%) | 13 (68%) | <0.001 | ||||
| FLARE # | Age | Gender | Cancer-type | Stage | ECOG PS | Days since diagnosis | dNLR | Immature neutrophils (%) | IL-6 | Covid-19 severity | 30-day mortality |
|---|---|---|---|---|---|---|---|---|---|---|---|
| FLARE #1 | 66 | Female | Colorectal | IV | 2 | D+6 | 2.66 | - | - | Moderate | No |
| FLARE #2 | 60 | Male | Prostate | IV | 1 | D+10 | 4.63 | - | - | Moderate | No |
| FLARE #3 | 82 | Male | Prostate | IV | 1 | D+3 | 0.19 | - | - | Moderate | No |
| FLARE #4 | 61 | Male | Bladder | IV | 2 | D+15 | 10.73 | - | - | Severe | Yes |
| FLARE #5 | 49 | Male | Suprarenal | IV | 0 | D+3 | 2.31 | 1.03 | 0 | Moderate | No |
| FLARE #6 | 65 | Female | Breast | IV | 1 | D+2 | 2.59 | 2.72 | 21.93 | Severe | No |
| D+6 | 2.92 | 3.09 | 41.37 | ||||||||
| FLARE #7 | 66 | Female | Lung | IV | 3 | D+3 | 18.69 | 1.15 | 22.76 | Severe | Yes |
| FLARE #8 | 59 | Male | Esophagus | IV | 1 | D+3 | 0.47 | 0.15 | - | As/Mild | No |
| D+6 | 2.21 | 0.59 | - | ||||||||
| FLARE #9 | 57 | Male | Colorectal | IV | 0 | D+5 | 0.27 | 4.48 | 21.04 | As/Mild | No |
| FLARE #10 | 77 | Female | Gastric | III | 2 | D+9 | 6.42 | 0.23 | - | As/Mild | No |
| FLARE #11 | 56 | Female | Breast | IV | 2 | D+2 | 8.49 | 0.71 | - | Moderate | No |
| D+9 | 12.4 | 2.14 | - | ||||||||
| D+16 | 12.53 | 1.4 | 0 | ||||||||
| FLARE #12 | 55 | Female | Colorectal | IV | 1 | D+1 | 3.21 | 2.19 | 188.85 | As/Mild | No |
| FLARE #13 | 74 | Female | Lung | II | 2 | D+1 | 1.97 | 2.01 | 0 | As/Mild | No |
| D+8 | 1.72 | - | - | ||||||||
| FLARE #14 | 61 | Female | Ovarian | IV | 1 | D+8 | 1.41 | 2.39 | 158.69 | As/Mild | No |
| FLARE #15 | 60 | Male | Bladder | IV | 2 | D+2 | 7.72 | 5.33 | - | Severe | No |
| D+5 | 10.88 | 1.17 | 50.4 | ||||||||
| D+9 | 49.13 | 97.6 | 895.93 | ||||||||
| FLARE #16 | 58 | Male | Head&Neck | III | 1 | D+3 | 2.74 | 3.64 | 0 | As/Mild | No |
| D+7 | 2.55 | 8.93 | 00 | ||||||||
| D+19 | 3.31 | - | - | ||||||||
| FLARE #17 | 73 | Male | Esophagus | IV | 3 | D+4 | 7.96 | 4.58 | 676.46 | Severe | Yes |
| FLARE #18 | 71 | Male | Thyroid | IV | 1 | D+4 | 2.61 | 1.42 | 11.43 | Moderate | No |
| FLARE #19 | 54 | Female | Lung | IV | 1 | D+15 | 2.69 | 0.82 | 0 | Moderate | No |
| D+46 | 3.28 | 1.12 | - | ||||||||
| FLARE #20 | 77 | Female | Breast | IV | 3 | D+16 | 2.77 | 9.75 | 116.25 | Severe | No |
| D+23 | 6.32 | 4.64 | 55.676 | ||||||||
| D+25 | 6.32 | 3.02 | 138.22 | ||||||||
| FLARE #21 | 72 | Female | Lung | IV | 1 | D+4 | 1.22 | 94 | 17.83 | Moderate | No |
| FLARE #22 | 55 | Female | Ovarian | IV | 1 | D+3 | 1.31 | 0.28 | 11.43 | As/Mild | No |
| FLARE #23 | 73 | Female | Head&Neck | III | 3 | D+8 | 10.52 | 16 | 118.09 | Severe | No |
| D+10 | 4.64 | 10.1 | 421.18 | ||||||||
| D+17 | 3.95 | - | - | ||||||||
| FLARE #24 | 50 | Female | Breast | IV | 1 | D+12 | 2.83 | 1.23 | 0 | As/Mild | No |
| D+45 | 1.18 | 2.55 | - | ||||||||
| FLARE #25 | 62 | Male | Head&Neck | III | 1 | D+3 | 12.86 | 36.8 | - | Severe | No |
| D+10 | 4.11 | 2.08 | 0 | ||||||||
| FLARE #27 | 81 | Male | Lung | IV | 2 | D+4 | 3.91 | 0.96 | 11.43 | Severe | Yes |
| FLARE #28 | 65 | Female | Renal | IV | 0 | D+8 | 0.74 | - | - | As/Mild | No |
| FLARE #29 | 72 | Male | Prostate | IV | 2 | D+2 | 6.59 | 0.46 | 31.07 | Moderate | No |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




