Submitted:
21 June 2024
Posted:
24 June 2024
You are already at the latest version
Abstract
Keywords:
Introduction
A History of Surgical Education
Teaching for Rare Surgical Methods
3D Modeling for Educational Insight
Functional 3D Models Enable On-Demand Practice
Materials and Methods
Results
Discussion
Current Challenges & Future Directions
Biomimicry of Surrogate Materials
Local Production, Customization, and Training for Enhanced Accessibility
Anticipated Challenges and Strategies for Refinement
Accessible & Equitable Practice
Global Implications in Surgical Education
Impact on Patient Care Outcomes
Conclusion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- G. A. Appuhamillage, S. S. Ambagaspitiya, R. S. Dassanayake, and A. Wijenayake, “3D and 4D printing of biomedical materials: Current trends, challenges, and future outlook,” Explor. Med., vol. 5, no. 1, pp. 17–47, Feb. 2024. [CrossRef]
- R. Michaels et al., “3D printing in surgical simulation: Emphasized importance in the COVID-19 pandemic era,” J. 3D Print. Med., vol. 5, no. 1, pp. 5–9, Mar. 2021. [CrossRef]
- R. E. Michaels et al., “Development of a High-Fidelity, 3D-Printed Veau Class II Cleft Palate Simulator with Patient-Specific Capabilities,” J. 3D Print. Med., vol. 6, no. 2, pp. 69–75, Jun. 2022. [CrossRef]
- J. J. E. Choi et al., “Mechanical properties of human oral mucosa tissues are site dependent: A combined biomechanical, histological and ultrastructural approach,” Clin. Exp. Dent. Res., vol. 6, no. 6, pp. 602–611, Dec. 2020. [CrossRef]
- J. Choi, E. J. Lee, W. B. Jang, and S.-M. Kwon, “Development of Biocompatible 3D-Printed Artificial Blood Vessels through Multidimensional Approaches,” J. Funct. Biomater., vol. 14, no. 10, p. 497, Oct. 2023. [CrossRef]
- L. Camison, J. E. Brooker, S. Naran, J. R. Potts, and J. E. Losee, “The History of Surgical Education in the United States: Past, Present, and Future,” Ann. Surg. Open, vol. 3, no. 1, p. e148, Mar. 2022. [CrossRef]
- S. V. Kotsis and K. C. Chung, “Application of the ‘See One, Do One, Teach One’ Concept in Surgical Training:,” Plast. Reconstr. Surg., vol. 131, no. 5, pp. 1194–1201, May 2013. [CrossRef]
- S. Shebrain, N. Ferrin, C. Cookenmaster, E. Norman, and R. Sawyer, “History of surgical training in Kalamazoo,” Ann. Med. Surg., vol. 73, Jan. 2022. [CrossRef]
- D. Nikkhah and J. Rawlins, “Training and mentorship in plastic surgery,” J. Plast. Reconstr. Aesthet. Surg., vol. 72, no. 9, pp. 1576–1606, Sep. 2019. [CrossRef]
- G. Chen et al., “Insight into the history and trends of surgical simulation training in education: A bibliometric analysis,” Int. J. Surg., vol. 109, no. 8, pp. 2204–2213, Aug. 2023. [CrossRef]
- C. I. Lauer et al., “The Value of Surgical Graduate Medical Education (GME) Programs Within An Integrated Health Care System,” J. Surg. Educ., vol. 76, no. 6, pp. e173–e181, Nov. 2019. [CrossRef]
- M. S. Ryan, E. S. Holmboe, and S. Chandra, “Competency-Based Medical Education: Considering Its Past, Present, and a Post–COVID-19 Era,” Acad. Med., vol. 97, no. 3S, pp. S90–S97, Mar. 2022. [CrossRef]
- L. B. Kaban, R. Hale, and D. H. Perrott, “Oral and Maxillofacial Surgery Training in the United States,” Oral Maxillofac. Surg. Clin. N. Am., vol. 34, no. 4, pp. 495–503, Nov. 2022. [CrossRef]
- K. Liu et al., “Anatomical education and surgical simulation based on the Chinese Visible Human: A three-dimensional virtual model of the larynx region,” Anat. Sci. Int., vol. 88, no. 4, pp. 254–258, Sep. 2013. [CrossRef]
- D. G. Alemayehu, Z. Zhang, E. Tahir, D. Gateau, D.-F. Zhang, and X. Ma, “Preoperative Planning Using 3D Printing Technology in Orthopedic Surgery,” BioMed Res. Int., vol. 2021, pp. 1–9, Oct. 2021. [CrossRef]
- R. Sud and S. Khanduja, “Implementing competency-based medical education in post-graduate ophthalmology training: Understanding key concepts and methodologies and overcoming challenges,” Indian J. Ophthalmol., vol. 70, no. 10, p. 3701, 2022. [CrossRef]
- T. R. Meling and T. R. Meling, “The impact of surgical simulation on patient outcomes: A systematic review and meta-analysis,” Neurosurg. Rev., vol. 44, no. 2, pp. 843–854, Apr. 2021. [CrossRef]
- L. Heskin, C. Simms, O. Traynor, and R. Galvin, “Designing a synthetic simulator to teach open surgical skills for limb exploration in trauma: A qualitative study exploring the experiences and perspectives of educators and surgical trainees,” BMC Surg., vol. 21, no. 1, p. 417, Dec. 2021. [CrossRef]
- K. Oxford, G. Walsh, J. Bungay, S. Quigley, and A. Dubrowski, “Development, manufacture and initial assessment of validity of a 3-dimensional-printed bowel anastomosis simulation training model,” Can. J. Surg., vol. 64, no. 5, pp. E484–E490, Sep. 2021. [CrossRef]
- P. Saba, E. Belfast, R. Melnyk, A. Patel, R. Kashyap, and A. Ghazi, “Development of a High-Fidelity Robot-Assisted Kidney Transplant Simulation Platform Using Three-Dimensional Printing and Hydrogel Casting Technologies,” J. Endourol., vol. 34, no. 10, pp. 1088–1094, Oct. 2020. [CrossRef]
- T. Muelleman, J. Peterson, N. Chowdhury, J. Gorup, P. Camarata, and J. Lin, “Individualized Surgical Approach Planning for Petroclival Tumors Using a 3D Printer,” J. Neurol. Surg. Part B Skull Base, vol. 77, no. 03, pp. 243–248, Nov. 2015. [CrossRef]
- R. J. Mobbs, M. Coughlan, R. Thompson, C. E. Sutterlin, and K. Phan, “The utility of 3D printing for surgical planning and patient-specific implant design for complex spinal pathologies: Case report,” J. Neurosurg. Spine, vol. 26, no. 4, pp. 513–518, Apr. 2017. [CrossRef]
- R. Foresti et al., “Surgical Medical Education via 3D Bioprinting: Modular System for Endovascular Training,” Bioengineering, vol. 11, no. 2, p. 197, Feb. 2024. [CrossRef]
- K. Qiu, G. Haghiashtiani, and M. C. McAlpine, “3D Printed Organ Models for Surgical Applications,” Annu. Rev. Anal. Chem., vol. 11, no. 1, pp. 287–306, Jun. 2018. [CrossRef]
- X. Huang et al., “An intelligent grasper to provide real-time force feedback to shorten the learning curve in laparoscopic training,” BMC Med. Educ., vol. 24, no. 1, p. 161, Feb. 2024. [CrossRef]
- J. Xu et al., “A Deep Learning Approach to Classify Surgical Skill in Microsurgery Using Force Data from a Novel Sensorised Surgical Glove,” Sensors, vol. 23, no. 21, p. 8947, Nov. 2023. [CrossRef]
- V. R. Talanki, Q. Peng, S. B. Shamir, S. H. Baete, T. Q. Duong, and N. Wake, “Three - Dimensional Printed Anatomic Models Derived From Magnetic Resonance Imaging Data: Current State and Image Acquisition Recommendations for Appropriate Clinical Scenarios,” J. Magn. Reson. Imaging, vol. 55, no. 4, pp. 1060–1081, Apr. 2022. [CrossRef]
- S. Maloney and T. Haines, “Issues of cost-benefit and cost-effectiveness for simulation in health professions education,” Adv. Simul., vol. 1, no. 1, p. 13, Jan. 2016. [CrossRef]
- M. S. Tjønnås et al., “Stress responses in surgical trainees during simulation-based training courses in laparoscopy,” BMC Med. Educ., vol. 24, no. 1, p. 407, Apr. 2024. [CrossRef]
- M. S. Tjønnås, A. Das, C. Våpenstad, and S. O. Ose, “Simulation-based skills training: A qualitative interview study exploring surgical trainees’ experience of stress,” Adv. Simul., vol. 7, no. 1, p. 33, Oct. 2022. [CrossRef]
- Z. Ye et al., “The role of 3D printed models in the teaching of human anatomy: A systematic review and meta-analysis,” BMC Med. Educ., vol. 20, no. 1, p. 335, Dec. 2020. [CrossRef]
- S. Şenel, “An Overview of Physical, Microbiological and Immune Barriers of Oral Mucosa,” Int. J. Mol. Sci., vol. 22, no. 15, p. 7821, Jul. 2021. [CrossRef]
- M. Waasdorp, B. P. Krom, F. J. Bikker, P. P. M. Van Zuijlen, F. B. Niessen, and S. Gibbs, “The Bigger Picture: Why Oral Mucosa Heals Better Than Skin,” Biomolecules, vol. 11, no. 8, p. 1165, Aug. 2021. [CrossRef]
- M. L. Carnevale, J. Phair, J. E. Indes, and I. Koleilat, “Digital Footprint of Vascular Surgery Training Programs in the United States and Canada,” Ann. Vasc. Surg., vol. 67, pp. 115–122, Aug. 2020. [CrossRef]
- R. G. Nagassa, P. G. McMenamin, J. W. Adams, M. R. Quayle, and J. V. Rosenfeld, “Advanced 3D printed model of middle cerebral artery aneurysms for neurosurgery simulation,” 3D Print. Med., vol. 5, no. 1, p. 11, Dec. 2019. [CrossRef]
- C. Tenewitz, R. T. Le, M. Hernandez, S. Baig, and T. E. Meyer, “Systematic review of three-dimensional printing for simulation training of interventional radiology trainees,” 3D Print. Med., vol. 7, no. 1, p. 10, Dec. 2021. [CrossRef]
- Q. Gao, Q. Wang, M. Li, and C. Lu, “Feasibility and impact of three-dimensional (3D) printing technology in simulated teaching of congenital malformations,” BMC Med. Educ., vol. 24, no. 1, p. 499, May 2024. [CrossRef]
- S. M. Simkovich et al., “Resources and Geographic Access to Care for Severe Pediatric Pneumonia in Four Resource-limited Settings,” Am. J. Respir. Crit. Care Med., vol. 205, no. 2, pp. 183–197, Jan. 2022. [CrossRef]
- J.-Y. Kim, Y.-C. Lee, S.-G. Kim, and U. Garagiola, “Advancements in Oral Maxillofacial Surgery: A Comprehensive Review on 3D Printing and Virtual Surgical Planning,” Appl. Sci., vol. 13, no. 17, p. 9907, Sep. 2023. [CrossRef]
- P. García-Robles, I. Cortés-Pérez, F. A. Nieto-Escámez, H. García-López, E. Obrero-Gaitán, and M. C. Osuna-Pérez, “Immersive virtual reality and augmented reality in anatomy education: A systematic review and meta-analysis,” Anat. Sci. Educ., vol. 17, no. 3, pp. 514–528, Apr. 2024. [CrossRef]
- F. Von Bechtolsheim et al., “The development of tissue handling skills is sufficient and comparable after training in virtual reality or on a surgical robotic system: A prospective randomized trial,” Surg. Endosc., vol. 38, no. 5, pp. 2900–2910, May 2024. [CrossRef]
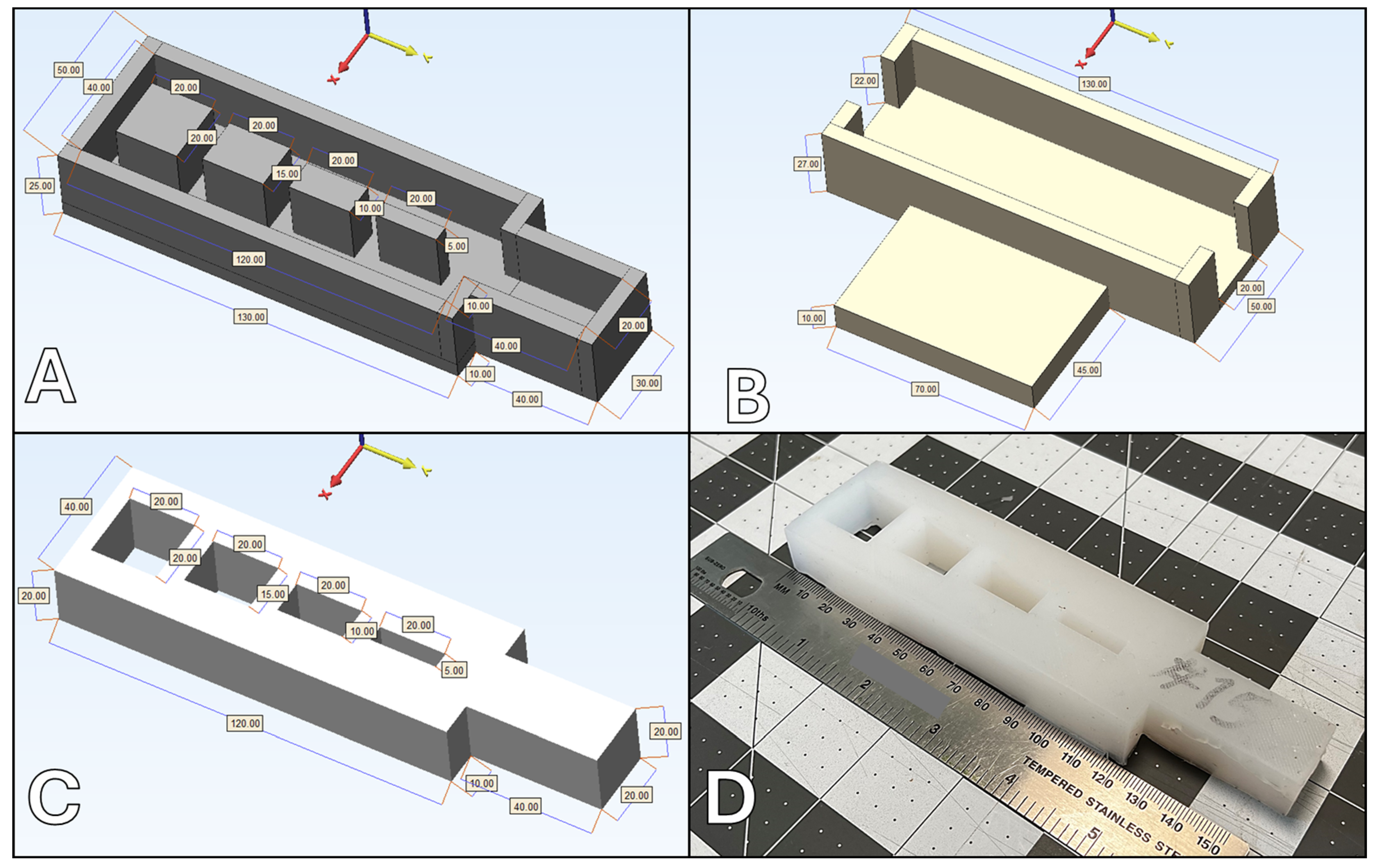
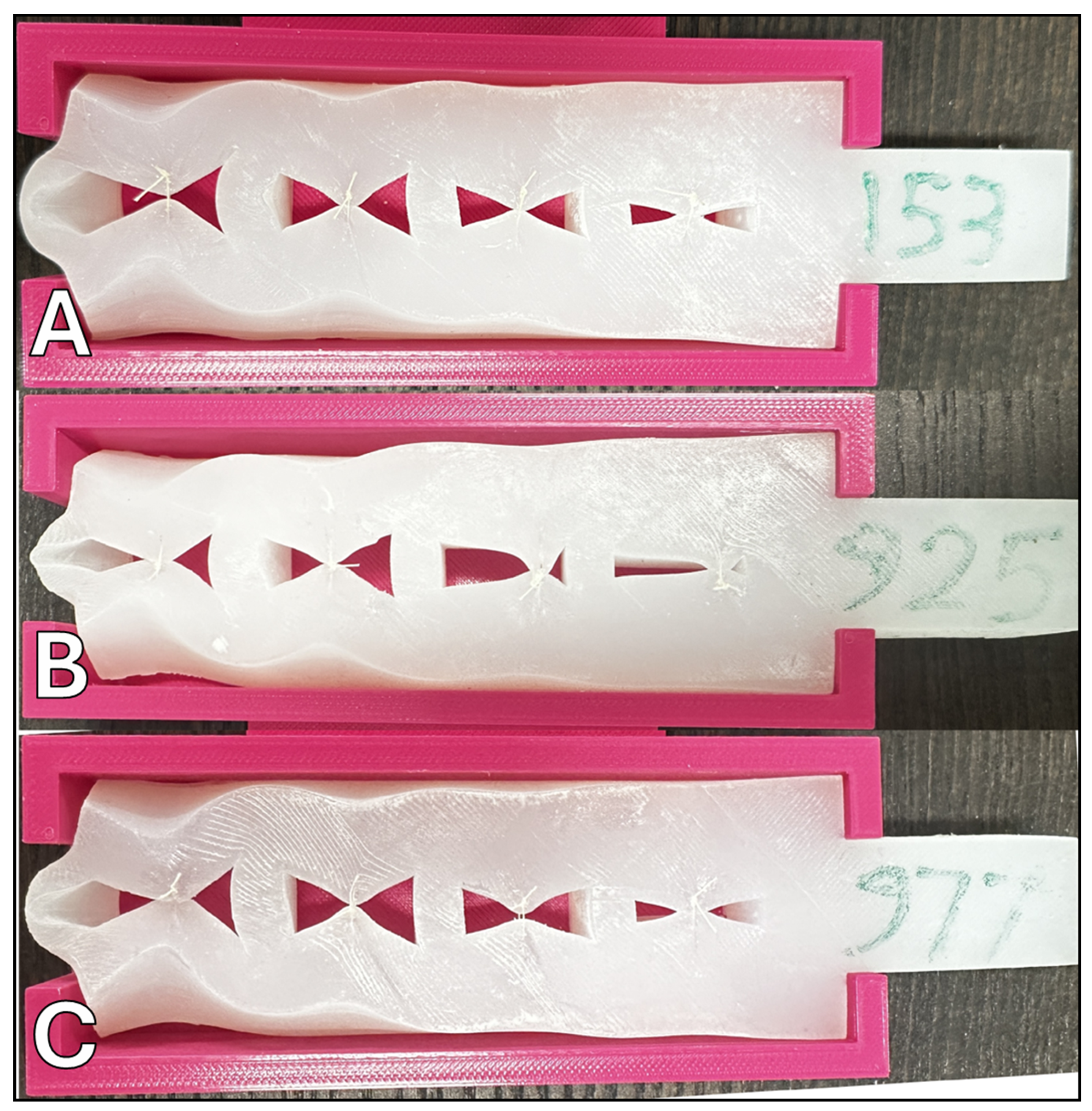
| Sample # | Silicone 10A | Silicone 00-45 | Slacker (%) |
| 810 | 100g | 0g | 10g (10) |
| 456 | 100g | 0g | 20g (20) |
| 925 | 100g | 0g | 30g (30) |
| 926 | 75g | 25g | 10g (10) |
| 153 | 75g | 25g | 20g (20) |
| 370 | 75g | 25g | 30g (30) |
| 977 | 50g | 50g | 10g (10) |
| 445 | 50g | 50g | 20g (20) |
| 642 | 50g | 50g | 30g (30) |
| 966 | 25g | 75g | 10g (10) |
| 876 | 25g | 75g | 20g (20) |
| 864 | 25g | 75g | 30g (30) |
| 643 | 0g | 100g | 10g (10) |
| 498 | 0g | 100g | 20g (20) |
| 745 | 0g | 100g | 30g (30) |
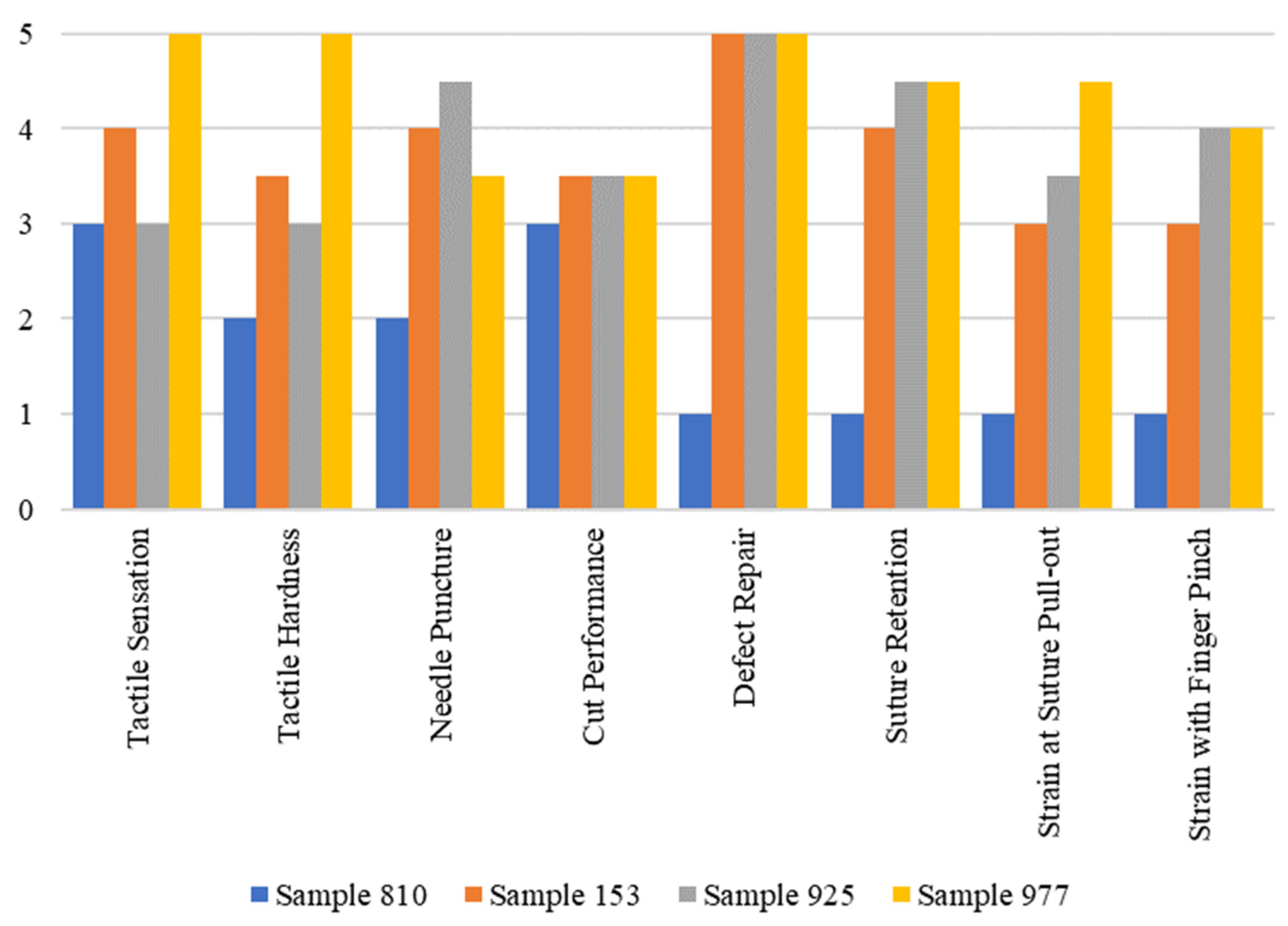
| Sample | 153 | 925 | 977 |
| Tactile Sensation | 4.0 | 3.0 | 5.0 |
| Tactile Hardness | 3.5 | 3.0 | 5.0 |
| Needle Puncture Performance | 4.0 | 4.5 | 3.5 |
| Cut Performance | 3.5 | 3.5 | 3.5 |
| Defect Repair Performance | 5.0 | 5.0 | 5.0 |
| Suture Retention to Manual Pull-out | 4.0 | 4.5 | 4.5 |
| Strain at Suture Pull-out | 3.0 | 3.5 | 4.5 |
| Strain with Finger Pinch | 3.0 | 4.0 | 4.0 |
| Average | 3.75 | 3.88 | 4.38 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




