Submitted:
05 June 2024
Posted:
06 June 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Patient Selection
2.2. Intervention
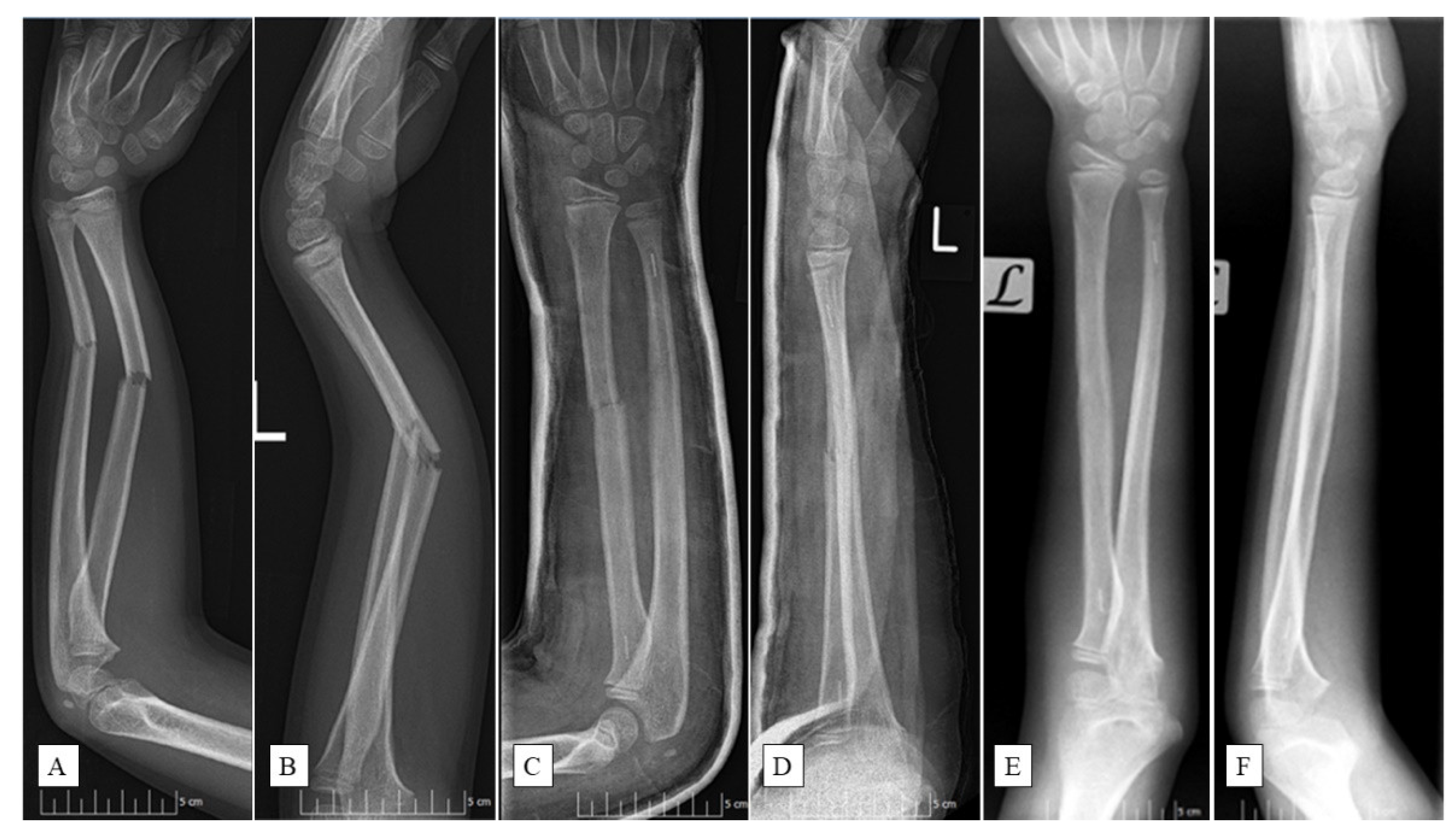
2.3. Surgical Protocol
2.5. Evaluated Metrics
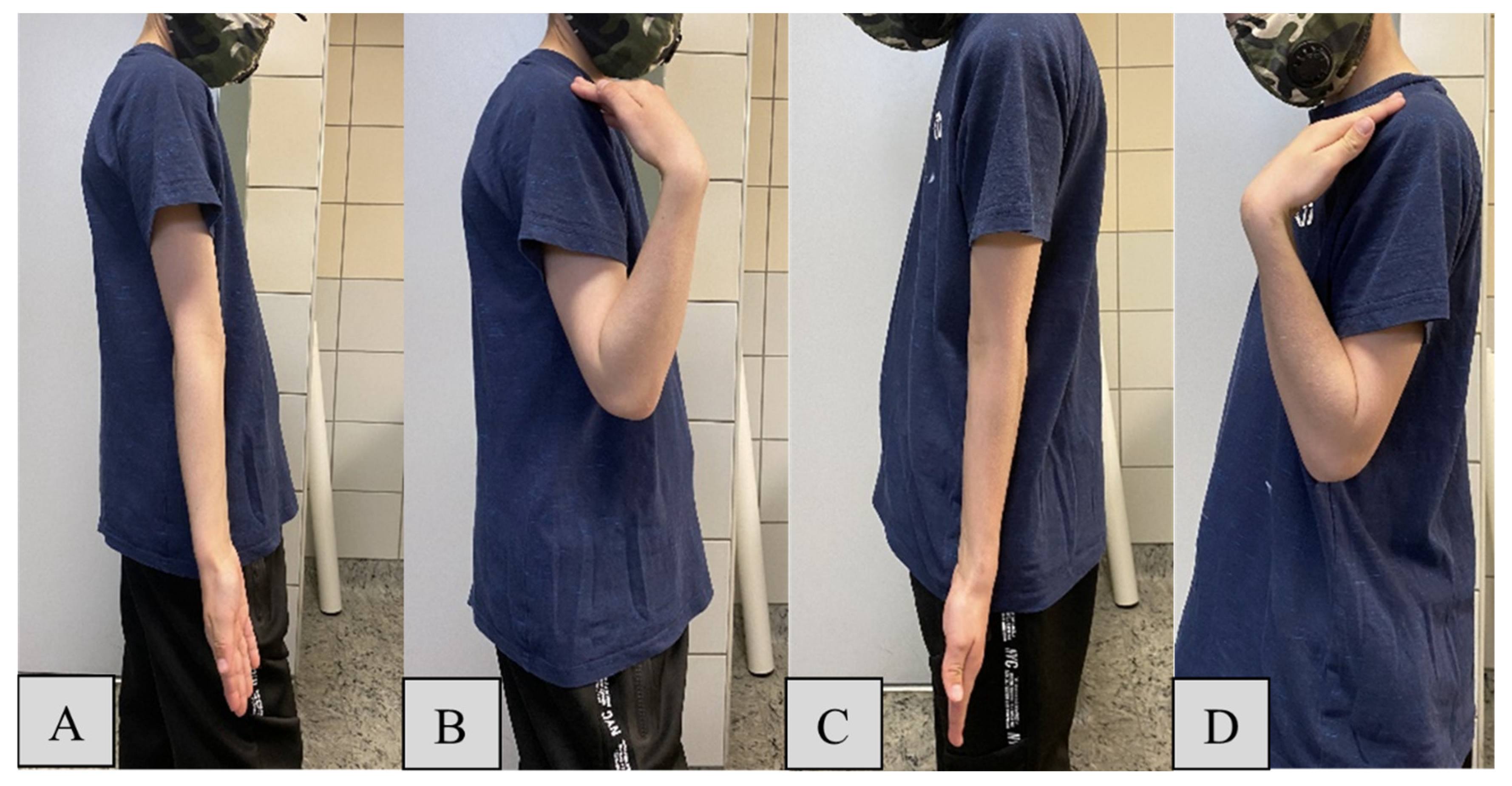
- Elbow Flexion and Extension: normal range is -10 to 150 degrees (°). Patients were instructed to fully extend and flex their elbows while standing with arms at their sides.
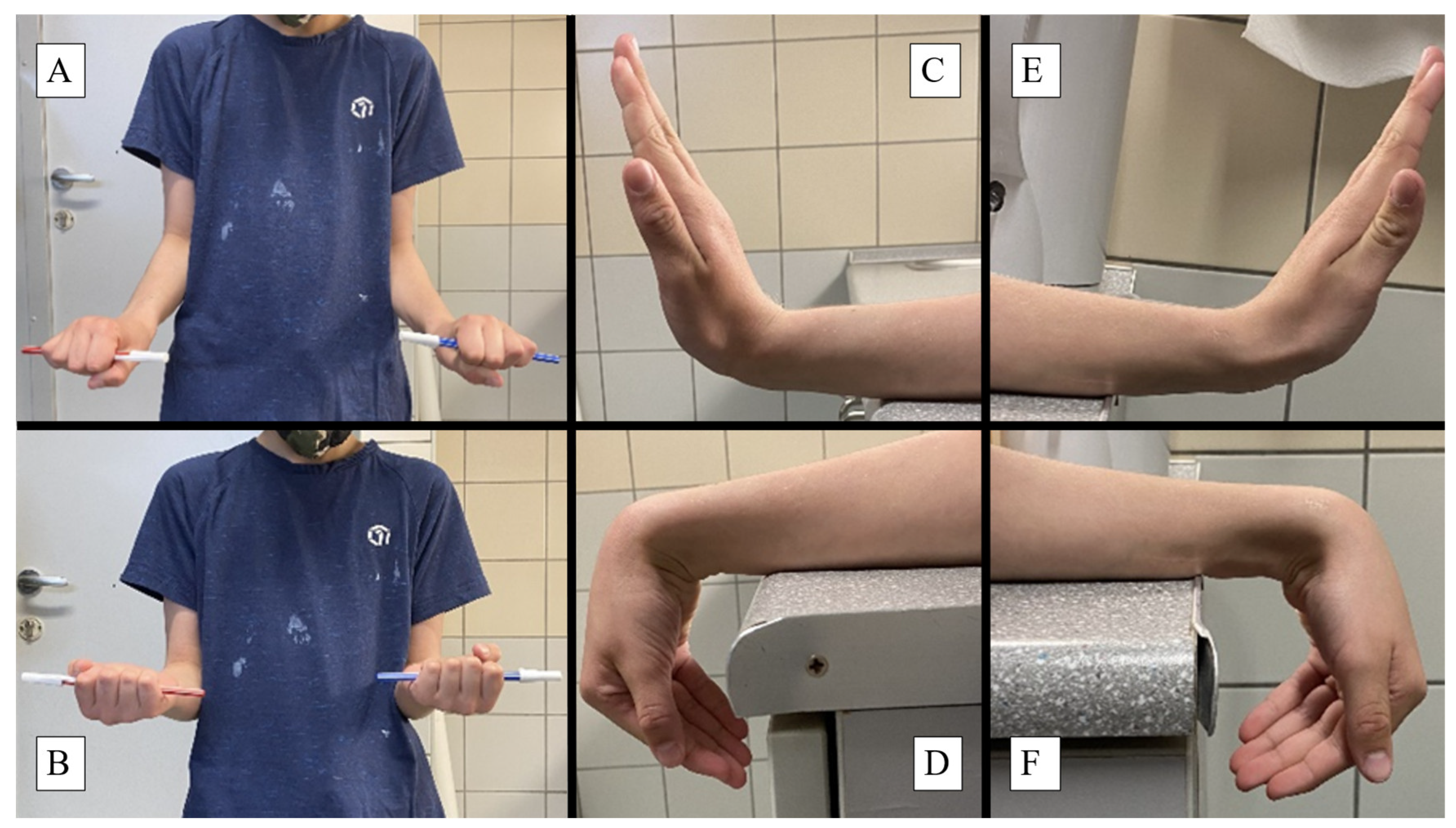
- Forearm Pronation and Supination: standard interval is 80 to 90° in both directions from the neutral position. Children held a pen in a fist with elbows at 90°, rotating their forearms to achieve maximum pronation and supination.
- Wrist Palmar Flexion and Dorsiflexion: typical ROM is 80° dorsiflexion and 70° palmar flexion. Patients placed their forearms on a horizontal surface, moving their wrists to the maximum palmar and dorsiflexion positions.
- Pigmentation: scored from 0 (normal) to 2 (severe hyperpigmentation).
- Vascularity: counted from 0 (normal) to 3 (severe vascularity).
- Pliability: graded from 0 (normal) to 5 (severe contracture).
- Height: recorded from 0 (flat) to 3 (more than 5 mm).
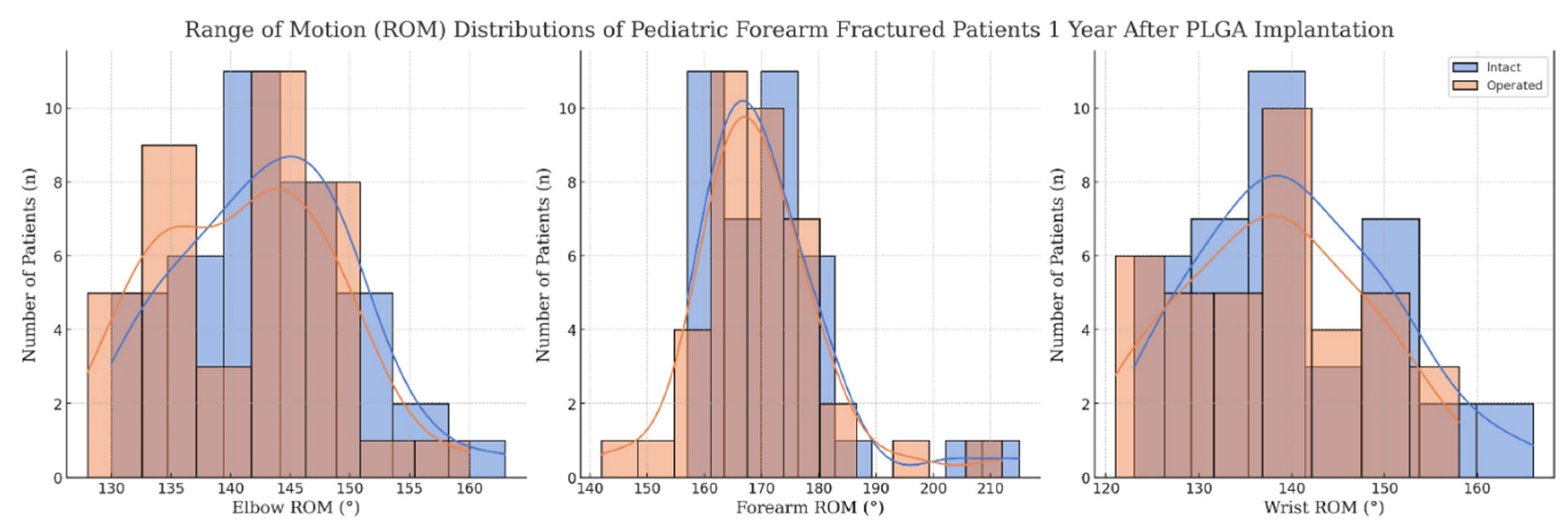
2.6. Data Analysis and Visualization
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Naranje, S.M.; Erali, R.A.; Warner, W.C.J.; Sawyer, J.R.; Kelly, D.M. Epidemiology of Pediatric Fractures Presenting to Emergency Departments in the United States. J. Pediatr. Orthop. 2016, 36, e45. [Google Scholar] [CrossRef] [PubMed]
- Chia, B.; Kozin, S.H.; Herman, M.J.; Safier, S.; Abzug, J.M. Complications of Pediatric Distal Radius and Forearm Fractures. Instr. Course Lect. 2015, 64, 499–507. [Google Scholar] [PubMed]
- Salvi, A.E. Forearm Diaphyseal Fractures: Which Bone to Synthesize First? Orthopedics 2006, 29, 669–671. [Google Scholar] [CrossRef] [PubMed]
- Manson, T.T.; Pfaeffle, H.J.; Herdon, J.H.; Tomaino, M.M.; Fischer, K.J. Forearm Rotation Alters Interosseous Ligament Strain Distribution. J. Hand Surg. 2000, 25, 1058–1063. [Google Scholar] [CrossRef] [PubMed]
- Widnall, J.; Bruce, C. Paediatric Forearm Fractures. Orthop. Trauma 2018, 32, 372–377. [Google Scholar] [CrossRef]
- Noonan, K.J.; Price, C.T. Forearm and Distal Radius Fractures in Children. J. Am. Acad. Orthop. Surg. 1998, 6, 146–156. [Google Scholar] [CrossRef] [PubMed]
- Epema, A.C.; Spanjer, M.J.B.; Ras, L.; Kelder, J.C.; Sanders, M. Point-of-Care Ultrasound Compared with Conventional Radiographic Evaluation in Children with Suspected Distal Forearm Fractures in the Netherlands: A Diagnostic Accuracy Study. Emerg. Med. J. EMJ 2019, 36, 613–616. [Google Scholar] [CrossRef] [PubMed]
- Caruso, G.; Caldari, E.; Sturla, F.D.; Caldaria, A.; Re, D.L.; Pagetti, P.; Palummieri, F.; Massari, L. Management of Pediatric Forearm Fractures: What Is the Best Therapeutic Choice? A Narrative Review of the Literature. Musculoskelet. Surg. 2021, 105, 225–234. [Google Scholar] [CrossRef] [PubMed]
- The AO Pediatric Comprehensive Classification of Long Bone Fractures (PCCF) | Acta Orthopaedica. Available online: https://actaorthop.org/actao/article/view/9669 (accessed on 31 May 2024).
- Randsborg, P.-H.; Sivertsen, E.A. Distal Radius Fractures in Children: Substantial Difference in Stability between Buckle and Greenstick Fractures. Acta Orthop. 2009, 80, 585–589. [Google Scholar] [CrossRef] [PubMed]
- Atanelov, Z.; Bentley, T.P. Greenstick Fracture. In StatPearls; StatPearls Publishing: Treasure Island (FL), 2024. [Google Scholar]
- Poutoglidou, F. Flexible Intramedullary Nailing in the Treatment of Forearm Fractures in Children and Adolescents, a Systematic Review. J. Orthop. 2020, 20. [Google Scholar] [CrossRef] [PubMed]
- Flynn, J.M.; Jones, K.J.; Garner, M.R.; Goebel, J. Eleven Years Experience in the Operative Management of Pediatric Forearm Fractures. J. Pediatr. Orthop. 2010, 30, 313–319. [Google Scholar] [CrossRef] [PubMed]
- Heye, P.; Matissek, C.; Seidl, C.; Varga, M.; Kassai, T.; Jozsa, G.; Krebs, T. Making Hardware Removal Unnecessary by Using Resorbable Implants for Osteosynthesis in Children. Child. Basel Switz. 2022, 9, 471. [Google Scholar] [CrossRef] [PubMed]
- Helber, M.U.; Ulrich, C. External Fixation in Forearm Shaft Fractures. Injury 2000, 31 Suppl 1, 45–47. [Google Scholar] [CrossRef]
- Elhalawany, A.S.; Afifi, A.; Anbar, A.; Galal, S. Hybrid Fixation for Adolescent Both-Bones Diaphyseal Forearm Fractures: Preliminary Results of a Prospective Cohort Study. J. Clin. Orthop. Trauma 2020, 11, S46–S50. [Google Scholar] [CrossRef] [PubMed]
- Korhonen, L.; Perhomaa, M.; Kyrö, A.; Pokka, T.; Serlo, W.; Merikanto, J.; Sinikumpu, J.-J. Intramedullary Nailing of Forearm Shaft Fractures by Biodegradable Compared with Titanium Nails: Results of a Prospective Randomized Trial in Children with at Least Two Years of Follow-Up. Biomaterials 2018, 185, 383–392. [Google Scholar] [CrossRef] [PubMed]
- Perhomaa, M.; Pokka, T.; Korhonen, L.; Kyrö, A.; Niinimäki, J.; Serlo, W.; Sinikumpu, J.-J. Randomized Controlled Trial of the Clinical Recovery and Biodegradation of Polylactide-Co-Glycolide Implants Used in the Intramedullary Nailing of Children’s Forearm Shaft Fractures with at Least Four Years of Follow-Up. J. Clin. Med. 2021, 10, 995. [Google Scholar] [CrossRef] [PubMed]
- Varga, M.; Józsa, G.; Hanna, D.; Tóth, M.; Hajnal, B.; Krupa, Z.; Kassai, T. Bioresorbable Implants vs. Kirschner-Wires in the Treatment of Severely Displaced Distal Paediatric Radius and Forearm Fractures - a Retrospective Multicentre Study. BMC Musculoskelet. Disord. 2022, 23, 362. [Google Scholar] [CrossRef] [PubMed]
- Elm, E. von; Altman, D.G.; Egger, M.; Pocock, S.J.; Gøtzsche, P.C.; Vandenbroucke, J.P. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) Statement: Guidelines for Reporting Observational Studies. J. Clin. Epidemiol. 2008, 61, 344–349. [Google Scholar] [CrossRef] [PubMed]
- Fearmonti, R.; Bond, J.; Erdmann, D.; Levinson, H. A Review of Scar Scales and Scar Measuring Devices. Eplasty 2010, 10, e43. [Google Scholar] [PubMed]
- Chereddy, K.K.; Payen, V.L.; Préat, V. PLGA: From a Classic Drug Carrier to a Novel Therapeutic Activity Contributor. J. Control. Release Off. J. Control. Release Soc. 2018, 289, 10–13. [Google Scholar] [CrossRef] [PubMed]
- Żywicka, B.; Krucińska, I.; Garcarek, J.; Szymonowicz, M.; Komisarczyk, A.; Rybak, Z. Biological Properties of Low-Toxic PLGA and PLGA/PHB Fibrous Nanocomposite Scaffolds for Osseous Tissue Regeneration. Evaluation of Potential Bioactivity. Mol. J. Synth. Chem. Nat. Prod. Chem. 2017, 22, 1852. [Google Scholar] [CrossRef] [PubMed]
- Paterson, N.; Waterhouse, P. Risk in Pediatric Anesthesia: Risk in Pediatric Anesthesia. Pediatr. Anesth. 2011, 21, 848–857. [Google Scholar] [CrossRef] [PubMed]
- Roeder, C.; Alves, C.; Balslev-Clausen, A.; Canavese, F.; Gercek, E.; Kassai, T.; Klestil, T.; Klingenberg, L.; Lutz, N.; Varga, M.; et al. Pilot Study and Preliminary Results of Biodegradable Intramedullary Nailing of Forearm Fractures in Children. Children 2022, 9, 754. [Google Scholar] [CrossRef] [PubMed]
- Józsa, G.; Kassai, T.; Varga, M. Preliminary Experience with Bioabsorbable Intramedullary Nails for Paediatric Forearm Fractures: Results of a Mini-Series. Genij Ortop. 2023, 29, 640–644. [Google Scholar] [CrossRef]
- Nudelman, H.; Lőrincz, A.; Lamberti, A.G.; Varga, M.; Kassai, T.; Józsa, G. Management of Juvenile Osteochondral Fractures Utilising Absorbable PLGA Implants. J. Clin. Med. 2024, 13, 375. [Google Scholar] [CrossRef] [PubMed]
- Válik, A.; Harangozó, K.; Garami, A.; Juhász, Z.; Józsa, G.; Lőrincz, A. Mid-Term Follow-Up Study of Children Undergoing Autologous Skin Transplantation for Burns. Life 2023, 13, 762. [Google Scholar] [CrossRef] [PubMed]
- Navratilova, P.; Emmer, J.; Tomas, T.; Ryba, L.; Burda, J.; Loja, T.; Veverkova, J.; Valkova, L.; Pavkova Goldbergova, M. Plastic Response of Macrophages to Metal Ions and Nanoparticles in Time Mimicking Metal Implant Body Environment. Environ. Sci. Pollut. Res. 2024, 31, 4111–4129. [Google Scholar] [CrossRef]
- Sun, C.W.Y.; Lau, L.C.M.; Cheung, J.P.Y.; Choi, S.-W. Cancer-Causing Effects of Orthopaedic Metal Implants in Total Hip Arthroplasty. Cancers 2024, 16, 1339. [Google Scholar] [CrossRef] [PubMed]
- Hedelin, H.; Larnert, P.; Antonsson, P.; Lagerstrand, K.; Brisby, H.; Hebelka, H.; Laine, T. Stability in Pelvic Triple Osteotomies in Children Using Resorbable PLGA Screws for Fixation. J. Pediatr. Orthop. 2021, 41, e787–e792. [Google Scholar] [CrossRef] [PubMed]
- Landes, C.A.; Ballon, A.; Roth, C. Maxillary and Mandibular Osteosyntheses with PLGA and P(L/DL)LA Implants: A 5-Year Inpatient Biocompatibility and Degradation Experience. Plast. Reconstr. Surg. 2006, 117, 2347–2360. [Google Scholar] [CrossRef] [PubMed]
- Xu, L.; Fukumura, D.; Jain, R.K. Acidic Extracellular pH Induces Vascular Endothelial Growth Factor (VEGF) in Human Glioblastoma Cells via ERK1/2 MAPK Signaling Pathway: MECHANISM OF LOW pH-INDUCED VEGF*. J. Biol. Chem. 2002, 277, 11368–11374. [Google Scholar] [CrossRef] [PubMed]
- Davis, R.; Singh, A.; Jackson, M.J.; Coelho, R.T.; Prakash, D.; Charalambous, C.P.; Ahmed, W.; da Silva, L.R.R.; Lawrence, A.A. A Comprehensive Review on Metallic Implant Biomaterials and Their Subtractive Manufacturing. Int. J. Adv. Manuf. Technol. 2022, 120, 1473–1530. [Google Scholar] [CrossRef] [PubMed]
- Jaspers, M.E.H.; Moortgat, P. Objective Assessment Tools: Physical Parameters in Scar Assessment. In Textbook on Scar Management: State of the Art Management and Emerging Technologies; Téot, L., Mustoe, T.A., Middelkoop, E., Gauglitz, G.G., Eds.; Springer: Cham (CH), 2020 ISBN 978-3-030-44765-6.
| Variable | Category | Count | Percentage |
| Sex | Female | 29 | 76.32% |
| Male | 9 | 23.68% | |
| Affected side | Left | 17 | 44.74% |
| Right | 21 | 55.26% | |
| Fracture type | Radius | 5 | 13.16% |
| Both | 32 | 84.21% | |
| Ulna | 1 | 2.63% | |
| Dominant hand | Right | 18 | 85.71% |
| Left | 3 | 14.29% | |
| Satisfaction | Satisfied | 38 | 100.00% |
| Endpoint (Unit) | Region | Status | Mean | SD | Min | Max | Median | IQR | IQR25 | IQR75 |
|---|---|---|---|---|---|---|---|---|---|---|
| Age (years) | ∞ | Child | 9.71 | 2.69 | 5.00 | 15.00 | 10.00 | 4.00 | 8.00 | 12.00 |
| Flexion (°) | Elbow | Operated | 139.30 | 6.20 | 130.00 | 155.00 | 140.50 | 8.25 | 136.50 | 144.75 |
| Intact | 140.80 | 6.20 | 130.00 | 155.00 | 140.50 | 8.25 | 136.50 | 144.75 | ||
| Extension (°) | Operated | -1.10 | 2.90 | -10.00 | 0.00 | 0.00 | 3.00 | -3.00 | 0.00 | |
| Intact | -1.30 | 2.90 | -10.00 | 0.00 | 0.00 | 3.00 | -3.00 | 0.00 | ||
| Pronation (°) | Forearm | Operated | 80.80 | 6.60 | 70.00 | 90.00 | 85.00 | 6.75 | 83.25 | 90.00 |
| Intact | 83.70 | 6.60 | 75.00 | 90.00 | 85.00 | 6.75 | 83.25 | 90.00 | ||
| Supination (°) | Operated | 83.50 | 6.60 | 72.00 | 110.00 | 84.00 | 5.00 | 80.00 | 85.00 | |
| Intact | 85.70 | 6.60 | 75.00 | 90.00 | 85.00 | 6.75 | 83.25 | 90.00 | ||
| Palmar Flexion (°) | Wrist | Operated | 64.90 | 6.70 | 50.00 | 75.00 | 68.00 | 5.75 | 65.00 | 70.75 |
| Intact | 68.60 | 6.10 | 50.00 | 80.00 | 70.00 | 7.00 | 66.50 | 73.50 | ||
| Dorsiflexion (°) | Operated | 73.20 | 6.70 | 60.00 | 86.00 | 68.00 | 6.00 | 65.00 | 71.00 | |
| Intact | 74.20 | 6.40 | 64.00 | 86.00 | 72.00 | 5.00 | 70.00 | 75.00 | ||
| VSS (total score) | Upper Limb | Guardian | 1.13 | 1.14 | 0.00 | 4.00 | 1.00 | 2.00 | 0.00 | 2.00 |
| Doctor | 0.55 | 0.80 | 0.00 | 3.00 | 0.00 | 1.00 | 0.00 | 1.00 |
| Measurement | Absolute Difference | Relative Difference | Test Used | p-value |
|---|---|---|---|---|
| Elbow Flexion (°) | -1.45 | 1.03% | Two-sample t | 0.282 |
| Elbow Extension (°) | 0.05 | 3.70% | Two-sample t | 0.098 |
| Pronation (°) | -1.61 | 1.31% | Mann-Whitney U | 0.166 |
| Supination (°) | 0.24 | -3.55% | Mann-Whitney U | 0.141 |
| Palmar Flexion (°) | -0.89 | 1.31% | Two-sample t | 0.563 |
| Dorsiflexion (°) | -1.55 | -3.55% | Mann-Whitney U | 0.070 |
| Dominant Hand Fracture (n) | -1 | -4.74% | Chi (χ²)-squared | 0.513 |
| VSS (Total Score) | 0.58 | 104.76% | Mann-Whitney U | 0.020 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




