Submitted:
03 June 2024
Posted:
04 June 2024
You are already at the latest version
Abstract
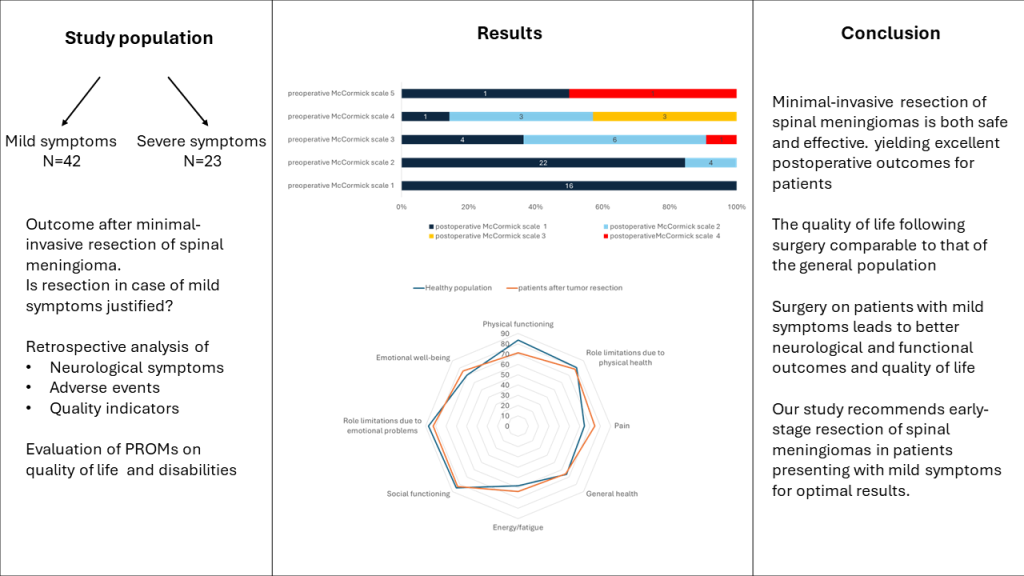
Keywords:
1. Introduction
2. Materials and Methods
Study Design
Surgical Intervention
Evaluation of Images
Statistical Analysis
3. Results
3.1. Patients’ Characteristics
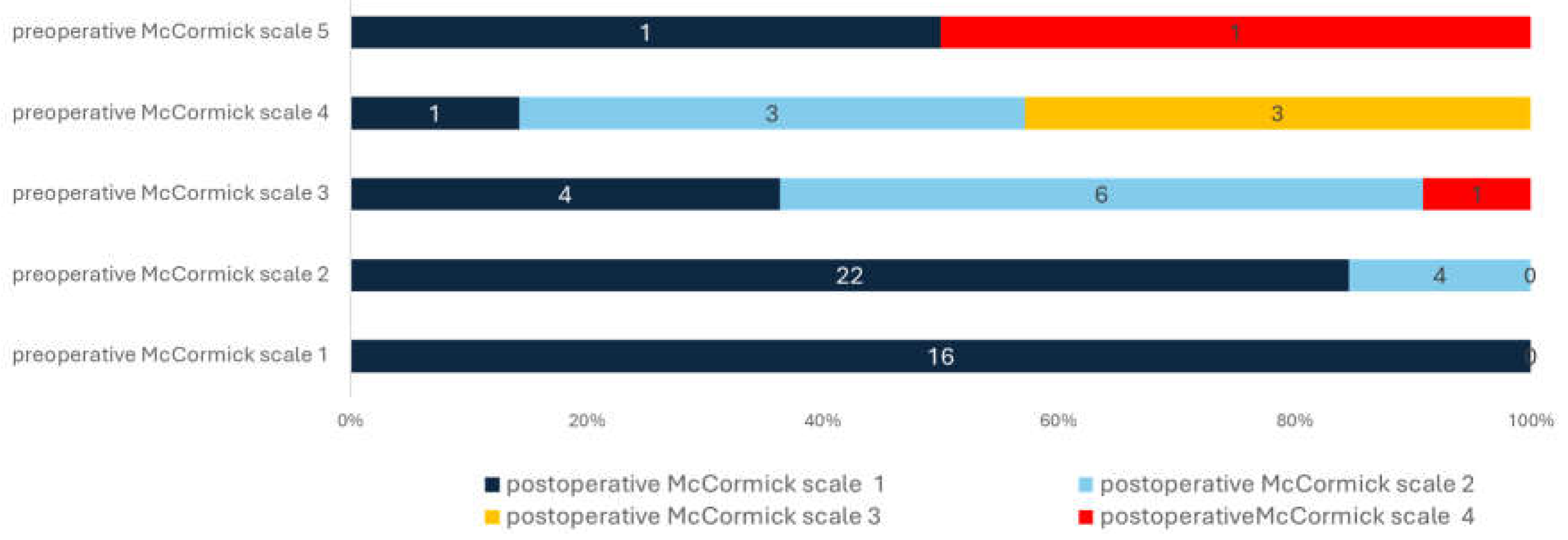
3.2. Neurological Outcome and Quality Indicators
| Variable | Mild symptoms (N = 42) | Severe symptoms (N = 23) | P Value |
|---|---|---|---|
| Duration of surgery (min, mean, SD) | 238.34 (±111.77) | 231.13 (±68.51) | .785 |
| Uni-lateral approach (N, %) | 37 (88.1%) | 22 (95.65%) | .411 |
| Bilateral approach (N, %) | 5 (11.9%) | 1 (4.35%) | .411 |
| Extent of resection | |||
| Simpson grade 2 (N, %) | 40 (95.24%) | 22 (95.65%) | >.99 |
| Simpson grade 3 (N, %) | 2 (4.76%) | 1 (4.35%) | |
| Estimated blood loss (ml, mean, SD) | 236.72 (±315.70) | 356.13 (±384) | .191 |
| Length of hospital stay (days, mean, SD) | 7.07 (±2.4) | 10.04 (±5.36) | .003 |
| Adverse events (N, %) | 2 (4.76%) | 2 (8.7%) | >.99 |
| CSF leak (N, %) | 1 (2.38%) | 0 | >.99 |
| Pulmonary embolism (N, %) | 1 (2.38%) | 0 | >.99 |
| Cardial decompensation (N, %) | 0 | 1 (4.35%) | .354 |
| Urinary tract infection | 0 | 1 (4.35%) | .354 |
| Histology WHO 1 (N, %) | 42 (100%) | 23 (100%) | >.99 |
| Karnofsky performance scale postoperative (Median, IQR) | 90 (90-100) | 80 (70-90) | .004 |
| Postoperative McCormick scale (Median, IQR) | 1 (1-1) | 2 (1-2) | .001 |
| Postoperative McCormick scale 1 (N, %) | 38 (90.48%) | 9 (39.13%) | <.001 |
| Postoperative McCormick scale 2 (N, %) | 4 (9.52%) | 10 (43.48%) | .003 |
| Postoperative McCormick scale 3 (N, %) | 0 | 3 (13.04%) | .037 |
| Postoperative McCormick scale 4 (N, %) | 0 | 1 (4.35%) | .354 |
| Postoperative McCormick scale 5 (N, %) | 0 | 0 | >.99 |
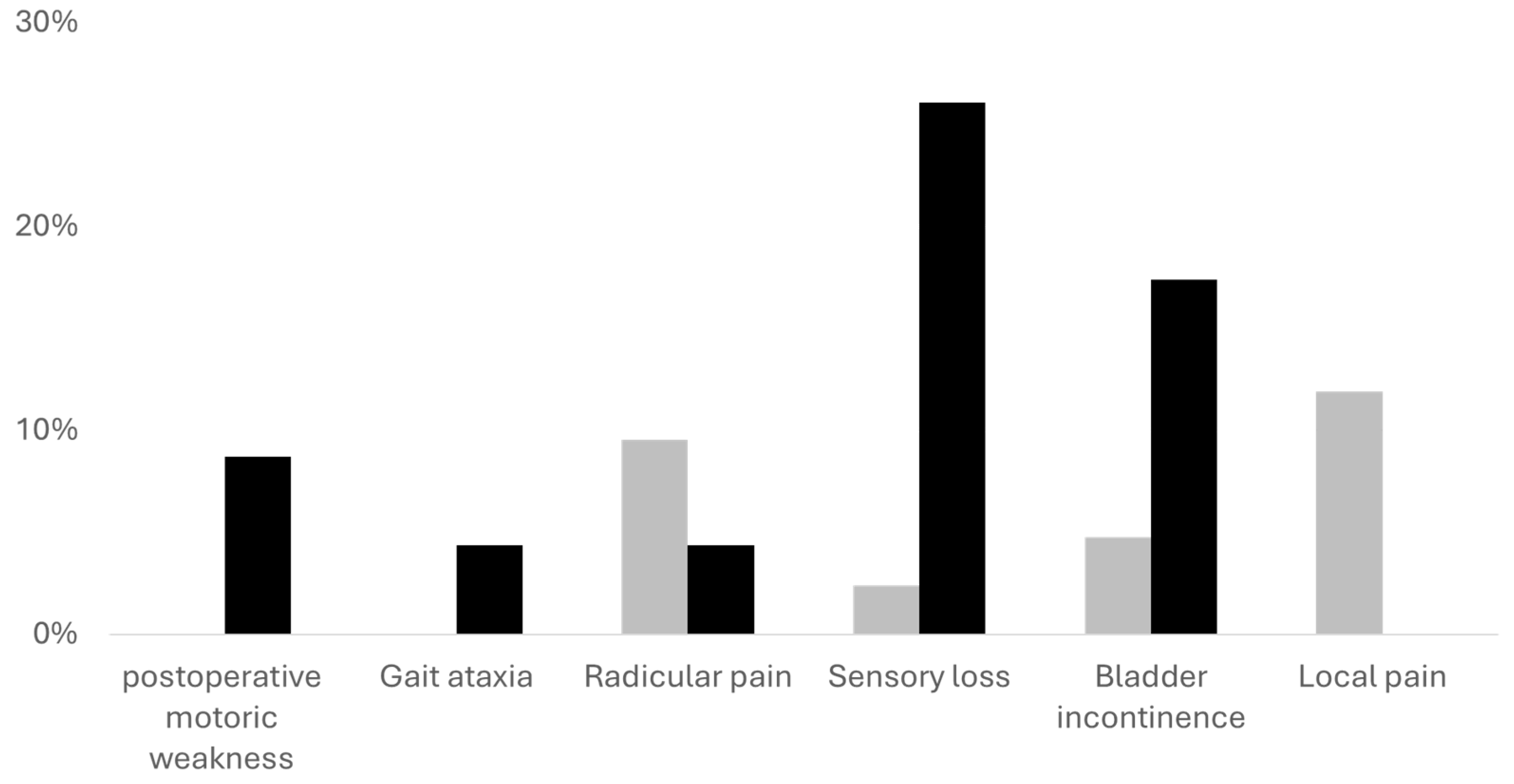
| Postoperative motoric weakness (N, %) | 0 | 2 (8.70%) | .122 |
| Gait ataxia (N, %) | 1 (2.38%) | 1 (4.35%) | >.99 |
| Radicular pain (N, %) | 4 (9.52%) | 1 (4.35%) | .649 |
| Sensory loss (N, %) | 1 (2.38%) | 6 (26.09%) | .006 |
| Bladder incontinence (N, %) | 2 (4.76%) | 4 (17.39%) | .174 |
| Local pain (N, %) | 5 (11.90%) | 0 | .152 |
| Readmission in 90 days (N, %) | 1 (2.38%) | 0 | >.99 |
| Re-Surgery in 90 days (N, %) | 1 (2.38%) | 0 | >.99 |
| Tumor recurrence (N, %) | 3 (7.14%) | 0 | .547 |
| Progression free survival (years, mean, SD) | 7.45 (±3.95) | 6 (±3.40) | .121 |
3.3. Functionality and Quality of Life
3.4. Tumor Recurrence and Progression
4. Discussion
Neurological Outcome after Minimal-Invasive Resection
Effect of Neurological Outcome on Functionality and Quality of Life
Quality Indicators and Adverse Events
Minimal Invasive Surgery
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Capo, G.; Moiraghi, A.; Baro, V.; Tahhan, N.; Delaidelli, A.; Saladino, A.; Paun, L.; DiMeco, F.; Denaro, L.; Meling, T.R.; et al. Surgical Treatment of Spinal Meningiomas in the Elderly (≥75 Years): Which Factors Affect the Neurological Outcome? An International Multicentric Study of 72 Cases. Cancers 2022, 14, 4790. [Google Scholar] [CrossRef] [PubMed]
- Schwake, M.; Adeli, A.; Sporns, P.; Ewelt, C.; Schmitz, T.; Sicking, J.; Hess, K.; Cäcilia Spille, D.; Paulus, W.; Stummer, W.; et al. Spinal Meningiomas - Risks and Potential of an Increasing Age at the Time of Surgery. Journal of Clinical Neuroscience 2018, 57, 86–92. [Google Scholar] [CrossRef] [PubMed]
- Setzer, M.; Vatter, H.; Marquardt, G.; Seifert, V.; Vrionis, F.D. Management of Spinal Meningiomas: Surgical Results and a Review of the Literature. Neurosurg Focus 2007, 23. [Google Scholar] [CrossRef]
- Pettersson-Segerlind, J.; Fletcher-Sandersjöö, A.; Tatter, C.; Burström, G.; Persson, O.; Förander, P.; Mathiesen, T.; Bartek, J.; Edström, E.; Elmi-Terander, A. Long-Term Follow-Up and Predictors of Functional Outcome after Surgery for Spinal Meningiomas: A Population-Based Cohort Study. Cancers 2021, 13, 3244. [Google Scholar] [CrossRef] [PubMed]
- Schipmann, S.; Schwake, M.; Suero Molina, E.; Stummer, W. Markers for Identifying and Targeting Glioblastoma Cells during Surgery. J Neurol Surg A Cent Eur Neurosurg 2019, 80. [Google Scholar] [CrossRef] [PubMed]
- Spille, D.C.; Lohmann, S.; Schwake, M.; Spille, J.H.; Alsofy, S.Z.; Stummer, W.; Brokinkel, B.; Schipmann, S. Can Currently Suggested Quality Indicators Be Transferred to Meningioma Surgery?-A Single-Centre Pilot Study. J Neurol Surg A Cent Eur Neurosurg 2022. [Google Scholar] [CrossRef] [PubMed]
- Schipmann, S.; Sletvold, T.P.; Wollertsen, Y.; Schwake, M.; Raknes, I.C.; Miletić, H.; Mahesparan, R. Quality Indicators and Early Adverse in Surgery for Atypical Meningiomas: A 16-Year Single Centre Study and Systematic Review of the Literature. Brain & Spine 2023, 3, 101739. [Google Scholar] [CrossRef] [PubMed]
- Kilinc, F.; Setzer, M.; Marquardt, G.; Keil, F.; Dubinski, D.; Bruder, M.; Seifert, V.; Behmanesh, B. Functional Outcome and Morbidity after Microsurgical Resection of Spinal Meningiomas. Neurosurg Focus 2021, 50, 1–7. [Google Scholar] [CrossRef]
- Viereck, M.J.; Ghobrial, G.M.; Beygi, S.; Harrop, J.S. Improved Patient Quality of Life Following Intradural Extramedullary Spinal Tumor Resection. J Neurosurg Spine 2016, 25, 640–645. [Google Scholar] [CrossRef]
- Newman, W.C.; Berry-Candelario, J.; Villavieja, J.; Reiner, A.S.; Bilsky, M.H.; Laufer, I.; Barzilai, O. Improvement in Quality of Life Following Surgical Resection of Benign Intradural Extramedullary Tumors: A Prospective Evaluation of Patient-Reported Outcomes. Neurosurgery 2021, 88, 989–995. [Google Scholar] [CrossRef]
- Said, W.; Maragno, E.; Leibrandt, L.; Spille, D.; Schipmann, S.; Stummer, W.; Gallus, M.; Schwake, M. A Retrospective Cohort Study Evaluating the Comparative Effectiveness of Unilateral Hemilaminectomy and Bilateral Laminectomy in the Resection of Spinal Meningiomas. Oper Neurosurg (Hagerstown) 2024. [Google Scholar] [CrossRef] [PubMed]
- Chiou, S.M.; Eggert, H.R.; Laborde, G.; Seeger, W. Microsurgical Unilateral Approaches for Spinal Tumour Surgery: Eight Years’ Experience in 256 Primary Operated Patients. Acta Neurochir (Wien) 1989, 100, 127–133. [Google Scholar] [CrossRef] [PubMed]
- Schöller, K.; Alimi, M.; Cong, G.T.; Christos, P.; Härtl, R. Lumbar Spinal Stenosis Associated With Degenerative Lumbar Spondylolisthesis: A Systematic Review and Meta-Analysis of Secondary Fusion Rates Following Open vs Minimally Invasive Decompression. Neurosurgery 2017, 80, 355–367. [Google Scholar] [CrossRef] [PubMed]
- Javid, M.J.; Hadar, E.J. Long-Term Follow-up Review of Patients Who Underwent Laminectomy for Lumbar Stenosis: A Prospective Study. J Neurosurg 1998, 89, 1–7. [Google Scholar] [CrossRef]
- Simpson, D. The Recurrence of Intracranial Meningiomas after Surgical Treatment. J Neurol Neurosurg Psychiatry 1957, 20, 22–39. [Google Scholar] [CrossRef] [PubMed]
- Fairbank, J.C.T.; Pynsent, P.B. The Oswestry Disability Index. Spine (Phila Pa 1976) 2000, 25, 2940–2953. [Google Scholar] [CrossRef] [PubMed]
- Vernon, H. The Neck Disability Index: State-of-the-Art, 1991-2008. J Manipulative Physiol Ther 2008, 31, 491–502. [Google Scholar] [CrossRef] [PubMed]
- McCormick, P.C.; Torres, R.; Post, K.D.; Stein, B.M. Intramedullary Ependymoma of the Spinal Cord. J Neurosurg 1990, 72, 523–532. [Google Scholar] [CrossRef] [PubMed]
- Maurischat, C.; Ehlebracht-König, I.; Kühn, A.; Bullinger, M. [Structural Validity of the Short Form 36 (SF-36) in Patients with Rheumatic Diseases]. Z Rheumatol 2005, 64, 255–264. [Google Scholar] [CrossRef]
- Jankovic, D.; Kalasauskas, D.; Othman, A.; Brockmann, M.A.; Sommer, C.J.; Ringel, F.; Keric, N. Predictors of Neurological Worsening after Resection of Spinal Meningiomas. Cancers 2023, 15, 5408. [Google Scholar] [CrossRef]
- Schwake, M.; Ricchizzi, S.; Krahwinkel, S.; Maragno, E.; Schipmann, S.; Stummer, W.; Gallus, M.; Holling, M. Resection of Intramedullary Hemangioblastoma: Timing of Surgery and Its Impact on Neurological Outcome and Quality of Life. Medicina 2023, 59, 1611. [Google Scholar] [CrossRef] [PubMed]
- El-Hajj, V.G.; Pettersson-Segerlind, J.; Fletcher-Sandersjöö, A.; Edström, E.; Elmi-Terander, A. Current Knowledge on Spinal Meningiomas-Surgical Treatment, Complications, and Outcomes: A Systematic Review and Meta-Analysis (Part 2). Cancers 2022, 14, 6221. [Google Scholar] [CrossRef] [PubMed]
- Wach, J.; Banat, M.; Schuss, P.; Güresir, E.; Vatter, H.; Scorzin, J. Age at Diagnosis and Baseline Myelomalacia Sign Predict Functional Outcome After Spinal Meningioma Surgery. Front Surg 2021, 8. [Google Scholar] [CrossRef]
- Raco, A.; Pesce, A.; Toccaceli, G.; Domenicucci, M.; Miscusi, M.; Delfini, R. Factors Leading to a Poor Functional Outcome in Spinal Meningioma Surgery: Remarks on 173 Cases. Neurosurgery 2017, 80, 602–609. [Google Scholar] [CrossRef] [PubMed]
- Jesse, C.M.; Alvarez Abut, P.; Wermelinger, J.; Raabe, A.; Schär, R.T.; Seidel, K. Functional Outcome in Spinal Meningioma Surgery and Use of Intraoperative Neurophysiological Monitoring. Cancers 2022, 14, 3989. [Google Scholar] [CrossRef] [PubMed]
- Yamaguchi, S.; Menezes, A.H.; Shimizu, K.; Woodroffe, R.W.; Helland, L.C.; Hitchon, P.W.; Howard, M.A. Differences and Characteristics of Symptoms by Tumor Location, Size, and Degree of Spinal Cord Compression: A Retrospective Study on 53 Surgically Treated, Symptomatic Spinal Meningiomas. J Neurosurg Spine 2020, 32, 931–940. [Google Scholar] [CrossRef] [PubMed]
- Boström, A.; Bürgel, U.; Reinacher, P.; Krings, T.; Rohde, V.; Gilsbach, J.M.; Hans, F.J. A Less Invasive Surgical Concept for the Resection of Spinal Meningiomas. Acta Neurochir (Wien) 2008, 150, 551–556. [Google Scholar] [CrossRef] [PubMed]
- Harati, A.; Satopää, J.; Mahler, L.; Billon-Grand, R.; Elsharkawy, A.; Niemelä, M.; Hernesniemi, J. Early Microsurgical Treatment for Spinal Hemangioblastomas Improves Outcome in Patients with von Hippel-Lindau Disease. Surg Neurol Int 2012, 3. [Google Scholar] [CrossRef]
- Butenschoen, V.M.; Gloßner, T.; Hostettler, I.C.; Meyer, B.; Wostrack, M. Quality of Life and Return to Work and Sports after Spinal Ependymoma Resection. Sci Rep 2022, 12. [Google Scholar] [CrossRef]
- Goodwin, C.R.; Price, M.; Goodwin, A.N.; Dalton, T.; Versteeg, A.L.; Sahgal, A.; Rhines, L.D.; Schuster, J.M.; Weber, M.H.; Lazary, A.; et al. Gender and Sex Differences in Health-Related Quality of Life, Clinical Outcomes and Survival after Treatment of Metastatic Spine Disease. Spine (Phila Pa 1976) 2023. [Google Scholar] [CrossRef]
- Bond, M.R.; Versteeg, A.L.; Sahgal, A.; Rhines, L.D.; Sciubba, D.M.; Schuster, J.M.; Weber, M.H.; Fehlings, M.G.; Lazary, A.; Clarke, M.J.; et al. Surgical or Radiation Therapy for the Treatment of Cervical Spine Metastases: Results From the Epidemiology, Process, and Outcomes of Spine Oncology (EPOSO) Cohort. Global Spine J 2020, 10, 21–29. [Google Scholar] [CrossRef]
- Guarino, A.; Polini, C.; Forte, G.; Favieri, F.; Boncompagni, I.; Casagrande, M. The Effectiveness of Psychological Treatments in Women with Breast Cancer: A Systematic Review and Meta-Analysis. J Clin Med 2020, 9, 209. [Google Scholar] [CrossRef] [PubMed]
- Rick, O.; Dauelsberg, T.; Kalusche-Bontemps, E.M. Oncological Rehabilitation. Oncol Res Treat 2017, 40, 772–777. [Google Scholar] [CrossRef]
- Boersma, I.; Miyasaki, J.; Kutner, J.; Kluger, B. Palliative Care and Neurology: Time for a Paradigm Shift. Neurology 2014, 83, 561–567. [Google Scholar] [CrossRef]
- Mummaneni, P.V.; Park, P.; Shaffrey, C.I.; Wang, M.Y.; Uribe, J.S.; Fessler, R.G.; Chou, D.; Kanter, A.S.; Okonkwo, D.O.; Mundis, G.M.; et al. The MISDEF2 Algorithm: An Updated Algorithm for Patient Selection in Minimally Invasive Deformity Surgery. J Neurosurg Spine 2019, 32, 221–228. [Google Scholar] [CrossRef] [PubMed]
- Debono, B.; Wainwright, T.W.; Wang, M.Y.; Sigmundsson, F.G.; Yang, M.M.H.; Smid-Nanninga, H.; Bonnal, A.; Le Huec, J.C.; Fawcett, W.J.; Ljungqvist, O.; et al. Consensus Statement for Perioperative Care in Lumbar Spinal Fusion: Enhanced Recovery After Surgery (ERAS®) Society Recommendations. Spine J 2021, 21, 729–752. [Google Scholar] [CrossRef] [PubMed]
- Dobran, M.; Paracino, R.; Nasi, D.; Aiudi, D.; Capece, M.; Carrassi, E.; Lattanzi, S.; Rienzo, A.D.I.; Iacoangeli, M. Laminectomy versus Unilateral Hemilaminectomy for the Removal of Intraspinal Schwannoma: Experience of a Single Institution and Review of Literature. J Neurol Surg A Cent Eur Neurosurg 2021, 82, 552–555. [Google Scholar] [CrossRef] [PubMed]
- Acosta, F.L.; Aryan, H.E.; Chi, J.; Parsa, A.T.; Ames, C.P. Modified Paramedian Transpedicular Approach and Spinal Reconstruction for Intradural Tumors of the Cervical and Cervicothoracic Spine: Clinical Experience. Spine (Phila Pa 1976) 2007, 32. [Google Scholar] [CrossRef]
- Onken, J.; Obermüller, K.; Staub-Bartelt, F.; Meyer, B.; Vajkoczy, P.; Wostrack, M. Surgical Management of Spinal Meningiomas: Focus on Unilateral Posterior Approach and Anterior Localization. J Neurosurg Spine 2018, 30, 308–313. [Google Scholar] [CrossRef]
- Thakur, J.; Ulrich, C.T.; Schär, R.T.; Seidel, K.; Raabe, A.; Jesse, C.M. The Surgical Challenge of Ossified Ventrolateral Spinal Meningiomas: Tricks and Pearls for Managing Large Ossified Meningiomas of the Thoracic Spine. J Neurosurg Spine 2021, 35, 516–526. [Google Scholar] [CrossRef]
- Liao, D.; Li, D.; Wang, R.; Xu, J.; Chen, H. Hemilaminectomy for the Removal of the Spinal Tumors: An Analysis of 901 Patients. Front Neurol 2022, 13, 1094073. [Google Scholar] [CrossRef] [PubMed]
- Krahwinkel, S.; Schipmann, S.; Spille, D.; Maragno, E.; Al Barim, B.; Warneke, N.; Stummer, W.; Gallus, M.; Schwake, M. The Role of Prolonged Bed Rest in Postoperative Cerebrospinal Fluid Leakage After Surgery of Intradural Pathology—A Retrospective Cohort Study. 2023. [Google Scholar] [CrossRef] [PubMed]
- Schwake, M.; Krahwinkel, S.; Gallus, M.; Schipmann, S.; Maragno, E.; Neuschmelting, V.; Perrech, M.; Müther, M.; Lenschow, M. Does Early Mobilization Following Resection of Spinal Intra-Dural Pathology Increase the Risk of Cerebrospinal Fluid Leaks?-A Dual-Center Comparative Effectiveness Research. Medicina (Kaunas) 2024, 60, 171. [Google Scholar] [CrossRef] [PubMed]
- Müther, M.; Lüthge, S.; Gerwing, M.; Stummer, W.; Schwake, M. Management of Spinal Dumbbell Tumors via a Minimally Invasive Posterolateral Approach and Carbon Fiber-Reinforced Polyether Ether Ketone Instrumentation: Technical Note and Surgical Case Series. World Neurosurg 2021, 151, 277–283. [Google Scholar] [CrossRef] [PubMed]
- Schwake, M.; Maragno, E.; Gallus, M.; Schipmann, S.; Spille, D.; Al Barim, B.; Stummer, W.; Müther, M. Minimally Invasive Facetectomy and Fusion for Resection of Extensive Dumbbell Tumors in the Lumbar Spine. Medicina (Kaunas) 2022, 58, 1613. [Google Scholar] [CrossRef]
| Variable | Mild symptoms (N = 42) | Severe symptoms (N = 23) | P Value |
|---|---|---|---|
| Age (years, mean ± SD) | 55.29 (±13.52) | 64.09 (±13.62) | .015 |
| Female patients (N, %) | 28 (90.48%) | 21 (91.30%) | |
| Karnofsky performance scale preoperative (median, IQR) | 80 (70-80) | 70 (60-70) | <.001 |
| Other spine procedures in the past (N, %) | 1 (2.38%) | 2 (8.70%) | .284 |
| Other neurological diseases (N, %) | 2 (4,76%) | 2 (8.70%) | .603 |
| Psychological disorders (N, %) | 1 (2.38%) | 1 (4.35%) | >.99 |
| Other meningiomas in different localization (N, %) | 4 (9.52%) | 3 (13.04%) | .691 |
| Preoperative McCormick scale (median, IQR) | 2 (1-2) | 3 (3-4) | <.001 |
| Preoperative McCormick scale 1 (N, %) | 16 (38.1%) | 0 | <.001 |
| Preoperative McCormick scale 2 (N, %) | 26 (61.3%) | 0 | <.001 |
| Preoperative McCormick scale 3 (N, %) | 0 | 15 (65.22%) | <.001 |
| Preoperative McCormick scale 4 (N, %) | 0 | 6 (26.09%) | <.001 |
| Preoperative McCormick scale 5 (N, %) | 0 | 2 (8.70%) | .114 |
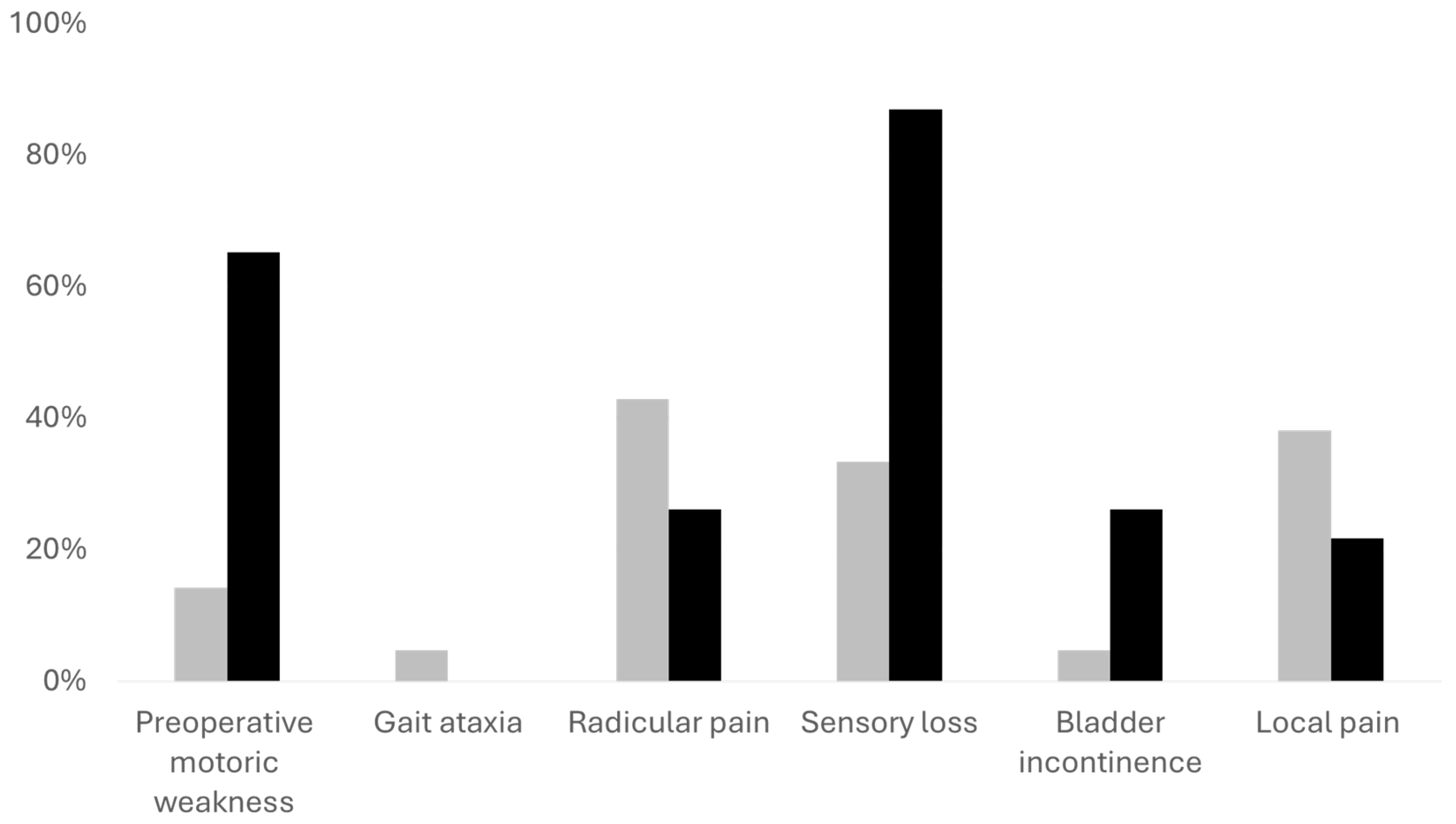
| Motor weakness (N, %) | 6 (14.29%) | 15 (65.22%) | <.001 |
| Gait ataxia (N, %) | 2 (4.76%) | 16 (69.57%) | <.001 |
| Radicular pain (N, %) | 18 (42.86%) | 6 (26.09%) | .282 |
| Sensory deficit (N, %) | 14 (33.33%) | 20 (86.96%) | <.001 |
| Bladder incontinence (N, %) | 2 (4.76%) | 6 (26.09%) | .016 |
| Local pain (N, %) | 16 (38.10%) | 5 (21.74%) | .275 |
| Duration of Symptoms (N, %) | .093 | ||
| More than 6 months (N, %) | 12 (28.57%) | 8 (34.78%) | .780 |
| Less than 6 months (N, %) | 19 (45.24%) | 14 (60.87%) | .302 |
| Unknown (N, %) | 11 (26.19%) | 1 (4.35%) | .043 |
| Primary case (N, %) | 38 (90.48%) | 23 (100%) | .290 |
| Recurrent tumor (N, %) | 4 (9.52%) | 0 | |
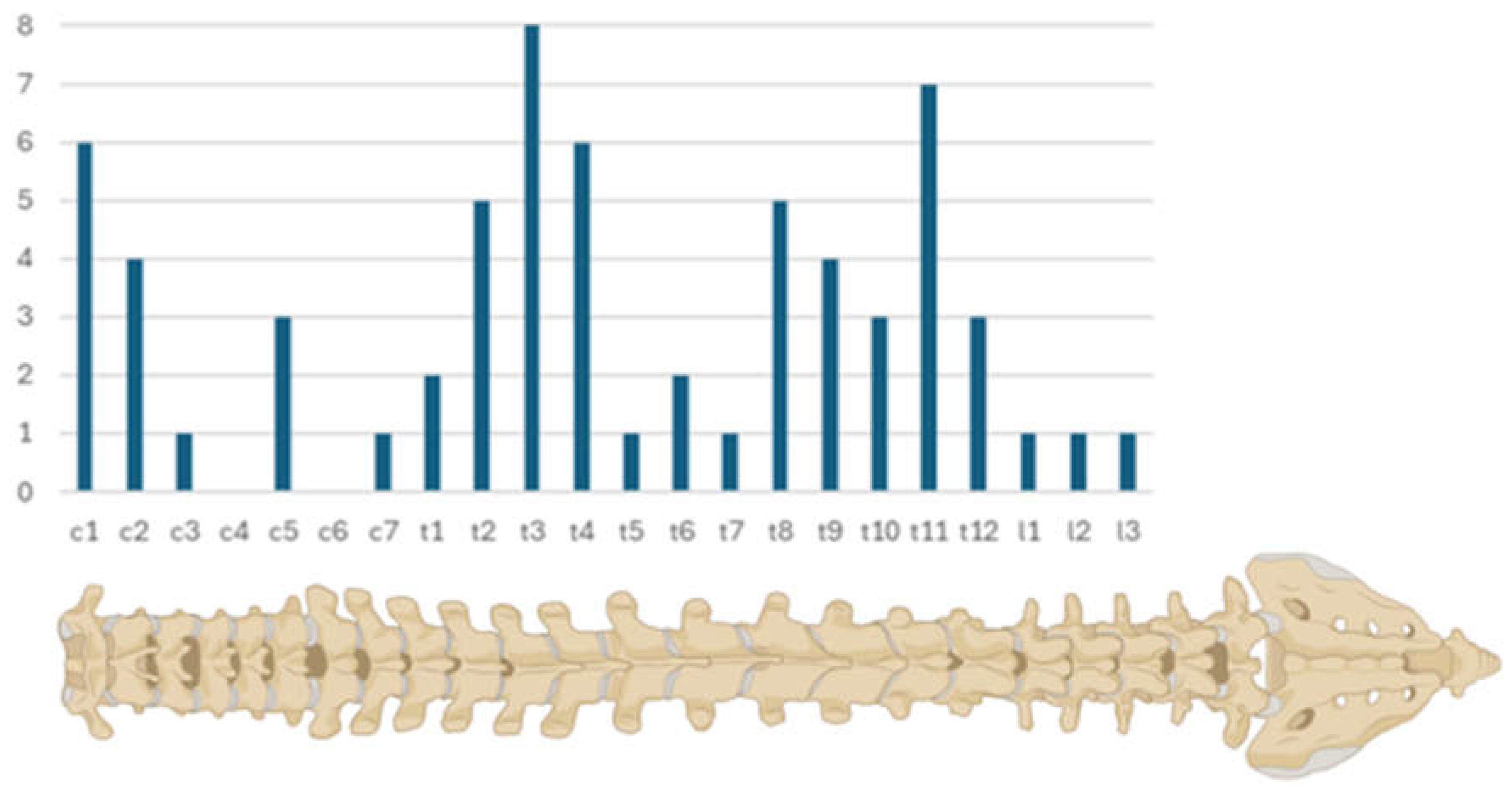
| Localization within the spinal canal | .087 | ||
| cervical spine (N, %) | 14 (33.33%) | 3 (13.04%) | .087 |
| Thoracic spine (N, %) | 25 (59.52%) | 20 (86.96%) | .026 |
| Lumbar spine (N, %) | 3 (7.14%) | 0 | .546 |
| Tumor volume (ml, mean, SD) | 1.13 (±0.79) | 1.36 (±0.95) | .294 |
| Tumor/spinal canal ratio (%, mean, SD) | 47.25% (±17.77%) | 59.73 (±21.07%) | .016 |
| Compression of spinal cord (N, %) | 36 (85.71%) | 23 (100%) | .082 |
| Spinal cord edema (N, %) | 5 (11.90%) | 8 (34.78%) | .049 |
| Variable | Favorable neurological outcome (N = 27) | Incomplete neurological outcome (N = 11) | P Value |
|---|---|---|---|
| Age at time of surgery (years, mean ± SD) | 56.93 ± 12.62 | 64.64 ± 12.04 | .092 |
| Age at present (years, mean ± SD) | 63.15 ± 12.77 | 68.73 ± 12.06 | .223 |
| Female patients (N, %) | 25 (93%) | 10 (91%) | >.99 |
| Karnofsky performance scale preoperative (median, IQR) | 80 (70-80) | 70 (70) | <.001 |
| Other spine procedures in the past (N, %) | 3 (11%) | 2 (18%) | .615 |
| Other neurological diseases (N, %) | 2 | 1 (9%) | >.99 |
| Psychological disorders (N, %) | 0 | 1 (9%) | .290 |
| Other meningiomas (N, %) | 1 | 2 | .196 |
| McCormick scale (median, IQR) | |||
| McCormick scale 1 (N, %) | 6 | 0 | .154 |
| McCormick scale 2 (N, %) | 16 | 1 | .010 |
| McCormick scale 3 (N, %) | 3 | 6 | .009 |
| McCormick scale 4 (N, %) | 1 | 4 | .019 |
| McCormick scale 5 (N, %) | 0 | 0 | >.99 |
| McCormick scale 1-2 (N, %) | 22 | 1 | <.001 |
| Preoperative motoric weakness (N, %) | 6 (22%) | 5 (45%) | .238 |
| Gait ataxia (N, %) | 0 | 10 (91%) | <.001 |
| Radicular pain (N, %) | 13 (48%) | 3 (27%) | .296 |
| Sensory loss (N, %) | 10 (37%) | 9 (32%) | .029 |
| Bladder incontinence (N, %) | 1 (4%) | 2 (18%) | .196 |
| Local pain (N, %) | 11 (41%) | 1 (9%) | .121 |
| Duration of Symptoms (N, %) | |||
| More than 6 months (N, %) | 5 | 5 | .116 |
| Less than 6 months (N, %) | 17 | 5 | .471 |
| Unknown (N, %) | 4 | 1 | >.99 |
| Primary case (N, %) | 24 | 11 (100%) | .542 |
| Recurrent tumor (N, %) | 3 | 0 | .542 |
| Localization with spinal canal | |||
| cervical spine (N, %) | 7 | 1 | .395 |
| Thoracic spine (N, %) | 17 | 10 | .124 |
| Lumbar spine (N, %) | 3 | 0 | .542 |
| Tumor volume (ml, mean, SD) | 1.17 ± 0.81 | 1.26 ± 1.10 | .787 |
| Tumor/spinal canal ratio (%, mean, SD) | 52 ± 17% | 59% ± 22% | .468 |
| Compression of spinal cord (N, %) | 25 (93%) | 11 (100%) | >.99 |
| Spinal cord edema (N, %) | 1 (4%) | 4 (36%) | 0.019 |
| Variable | Favorable neurological outcome (N = 27) | Incomplete neurological outcome (N = 11) | P Value |
|---|---|---|---|
| Duration of surgery (min, mean, SD) | 211.48 ± 95.87 | 236.09 ± 88.07 | 0.468 |
| Uni-lateral approach (N, %) | 26 | 11 (11%) | >.99 |
| Bilateral approach (N, %) | 1 | 0 | >.99 |
| Extent of resection | |||
| Simpson grade 2 (N, %) | 24 (89%) | 10 (91%) | >.99 |
| Simpson grade 3 (N, %) | 3 (11%) | 1 (9%) | >.99 |
| Estimated blood loss (ml, mean, SD) | 260.78 ± 382.88 | 203.73 ± 218.18 | .647 |
| Length of hospital stay (days, mean, SD) | 6.85 ± 1.26 | 9 ± 4.29 | .022 |
| Adverse events (N, %) | 0 | 0 | |
| Histology WHO 1 (N, %) | 27 | 11 | >.99 |
| Karnofsky scale postoperative (Median, IQR) | 100 (90-100) | 80 (70-90) | <.001 |
| McCormick scale (Median, IQR) | |||
| McCormick scale 1 (N, %) | 27 | 0 | <.001 |
| McCormick scale 2 (N, %) | 0 | 9 | <.001 |
| McCormick scale 3 (N, %) | 0 | 2 (18%) | 0.078 |
| postoperative motoric weakness (N, %) | 0 | 1 (9%) | .290 |
| Gait ataxia (N, %) | 0 | 1 (9%) | .290 |
| Radicular pain (N, %) | 2 (7%) | 2 (18%) | .564 |
| Sensory loss (N, %) | 0 | 3 (27%) | .020 |
| Bladder incontinence (N, %) | 0 | 0 | >.99 |
| Local pain (N, %) | 1 (4%) | 1 (9%) | .501 |
| Readmission in 90 days (N, %) | 0 | 0 | >.99 |
| Re-Surgery in 90 days (N, %) | 0 | 0 | >.99 |
| Tumor recurrence (N, %) | 2 (7%) | 0 | >.99 |
| Progression free survival (years, mean, SD) | 6.78 ± 4.14 | 4.09 ± 1.64 | .046 |
| Variable | Favorable neurological outcome (N = 27) | Incomplete neurological outcome (N = 11) | P Value |
|---|---|---|---|
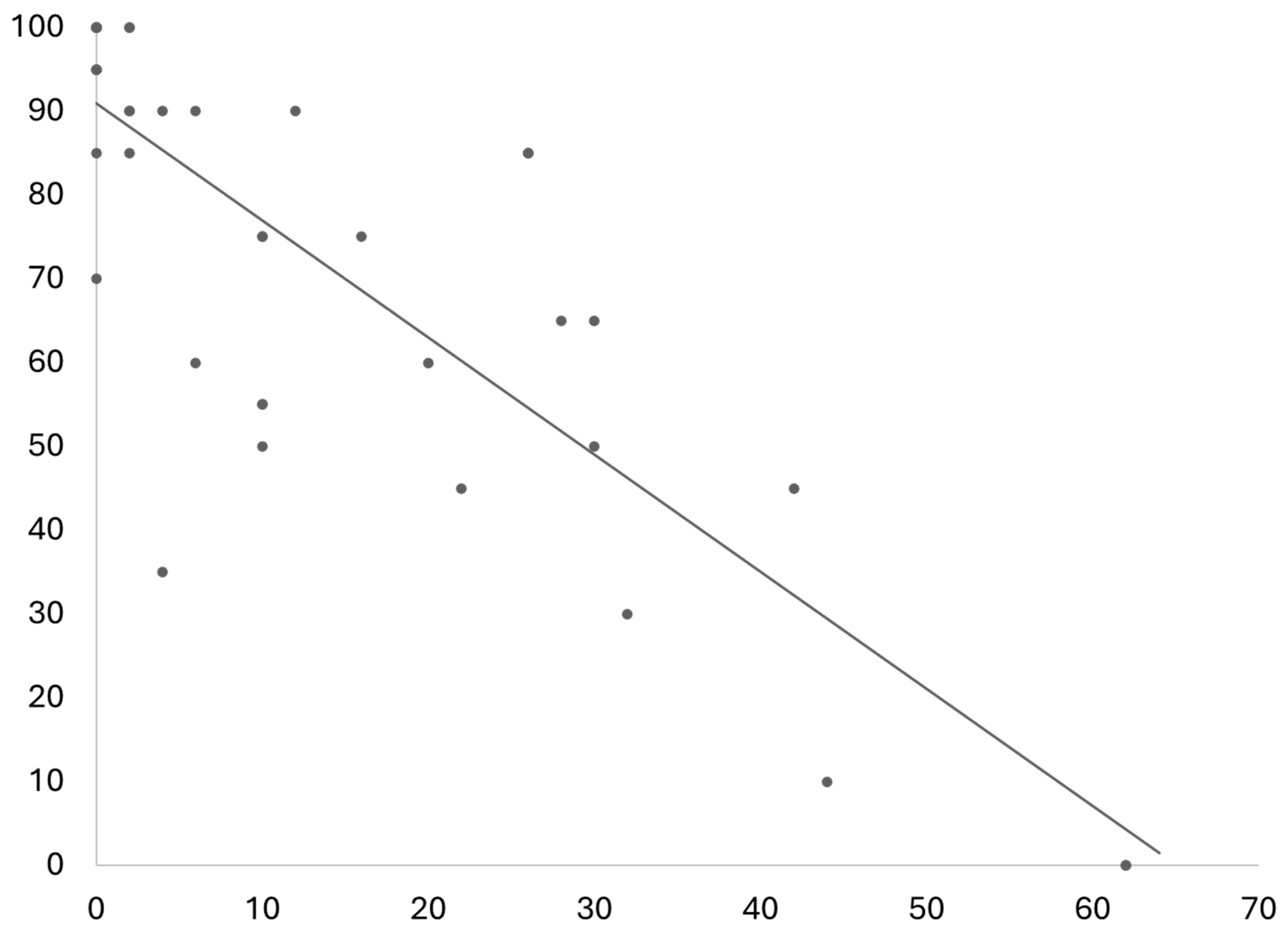
| ODI/NDI (mean, SD) | 9.26% ± 11.60% | 23.27% ± 24.10% | .020 |
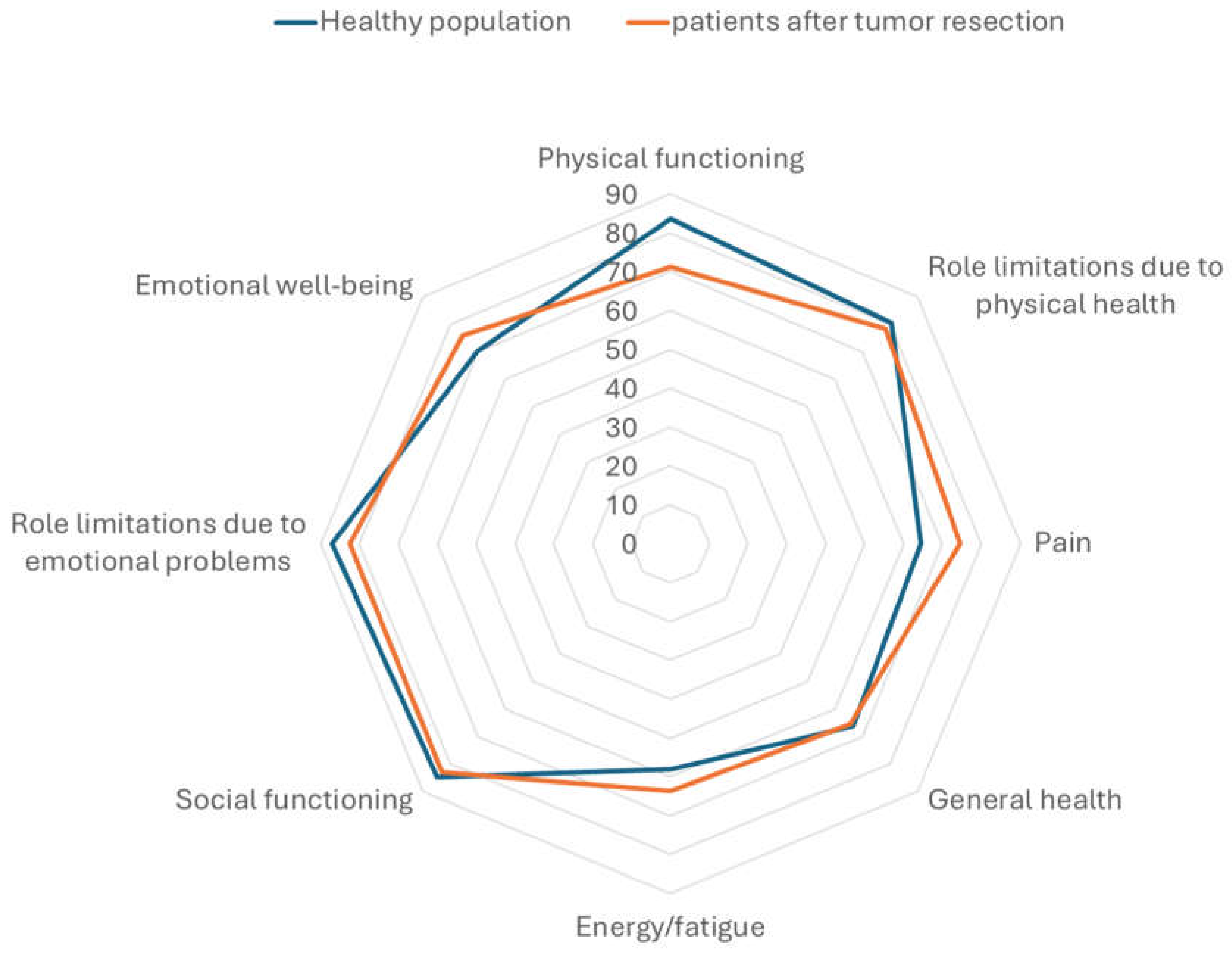
| Physical functioning (mean, SD) | 79.26 ± 20.03 | 51.82 ± 37.97 | .019 |
| Role limitations due to physical health (mean, SD) | 86.11 ± 27.15 | 59.09 ± 45.10 | .029 |
| Role limitations due to emotional problems (mean, SD) | 85.19 ± 29.72 | 75.75 ± 42.41 | .604 |
| Energy/fatigue (mean, SD) | 66.11 ± 21.81 | 57.27 ± 23.06 | .272 |
| Emotional well-being (mean, SD) | 78.48 ± 17.83 | 69.09 ± 22.42 | .180 |
| Social functioning (mean, SD) | 87.04 ± 18.50 | 73.86 ± 29.82 | .106 |
| Pain (mean, SD) | 80.19 ± 24.35 | 60.68 ± 32.66 | .050 |
| General health (mean, SD) | 68.33 ± 21.75 | 58.64 ± 22.59 | .226 |
| Health change (mean, SD) | 65.74 ± 25.14 | 61.36 ± 23.35 | .623 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




