Submitted:
20 April 2024
Posted:
23 April 2024
You are already at the latest version
Abstract
Keywords:
Introduction
Materials and Methods
Results
Discussion
Strengths and Limitations
Conclusion
Acknowledgments
Conflicts of Interest
References
- Basta, M.; Lipsett, B.J. , Anatomy, Abdomen and Pelvis: Umbilical Cord. StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing: 2023.
- Gaccioli, F.; Lager, S. Placental Nutrient Transport and Intrauterine Growth Restriction. Front Physiol 2016, 7, 40. [Google Scholar] [CrossRef]
- Gumina, D.L.; Su, E.J. Mechanistic insights into the development of severe fetal growth restriction. Clinical Science 2023, 137, 679–695. [Google Scholar] [CrossRef]
- Colson, A.; Sonveaux, P.; Debiève, F.; Sferruzzi-Perri, A.N. Adaptations of the human placenta to hypoxia: opportunities for interventions in fetal growth restriction. Human Reproduction Update 2020, 27, 531–569. [Google Scholar] [CrossRef]
- Ramirez Zegarra, R.; Dall’Asta, A.; Ghi, T. Mechanisms of Fetal Adaptation to Chronic Hypoxia following Placental Insufficiency: A Review. Fetal Diagn Ther 2022, 49, 279–292. [Google Scholar] [CrossRef] [PubMed]
- Brosens, I.; Puttemans, P.; Benagiano, G. Placental bed research: I. The placental bed: from spiral arteries remodeling to the great obstetrical syndromes. Am J Obstet Gynecol 2019, 221, 437–456. [Google Scholar] [CrossRef]
- Ghesquière, L.; Perbet, R.; Lacan, L.; Hamoud, Y.; Stichelbout, M.; Sharma, D.; Nguyen, S.; Storme, L.; Houfflin-Debarge, V.; De Jonckheere, J.; et al. Associations between fetal heart rate variability and umbilical cord occlusions-induced neural injury: An experimental study in a fetal sheep model. Acta Obstetricia et Gynecologica Scandinavica 2022, 101, 758–770. [Google Scholar] [CrossRef] [PubMed]
- Agrawal, S.; Parks, W.T.; Zeng, H.D.; Ravichandran, A.; Ashwal, E.; Windrim, R.C.; Hobson, S.R.; Melamed, N.; Kingdom, J.C. Diagnostic utility of serial circulating placental growth factor levels and uterine artery Doppler waveforms in diagnosing underlying placental diseases in pregnancies at high risk of placental dysfunction. Am J Obstet Gynecol 2022, 227, 618–e1. [Google Scholar] [CrossRef] [PubMed]
- Levytska, K.; Higgins, M.; Keating, S.; Melamed, N.; Walker, M.; Sebire, N.J.; Kingdom, J.C. Placental Pathology in Relation to Uterine Artery Doppler Findings in Pregnancies with Severe Intrauterine Growth Restriction and Abnormal Umbilical Artery Doppler Changes. Am J Perinatol 2017, 34, 451–457. [Google Scholar]
- Kingdom, J.C.; Audette, M.C.; Hobson, S.R.; Windrim, R.C.; Morgen, E. A placenta clinic approach to the diagnosis and management of fetal growth restriction. Am J Obstet Gynecol 2018, 218, S803–S817. [Google Scholar] [CrossRef]
- Redline, R.W. Classification of placental lesions. Am J Obstet Gynecol 2015, 213 (Suppl. S4), S21–S28. [Google Scholar] [CrossRef]
- Rocha, A.S.; Andrade, A.R. A.; Moleiro, M.L.; Guedes-Martins, L. Doppler Ultrasound of the Umbilical Artery: Clinical Application. Rev Bras Ginecol Obstet 2022, 44, 519–531. [Google Scholar] [CrossRef] [PubMed]
- Paranavitana, L.; Walker, M.; Chandran, A.R.; Milligan, N.; Shinar, S.; Whitehead, C.L.; Hobson, S.R.; Serghides, L.; Parks, W.T.; Baschat, A.A.; et al. Sex differences in uterine artery Doppler during gestation in pregnancies complicated by placental dysfunction. Biology of Sex Differences 2021, 12, 19. [Google Scholar] [CrossRef] [PubMed]
- Gudmundsson, S.; Flo, K.; Ghosh, G.; Wilsgaard, T.; Acharya, G. Placental pulsatility index: a new, more sensitive parameter for predicting adverse outcome in pregnancies suspected of fetal growth restriction. Acta Obstet Gynecol Scand 2017, 96, 216–222. [Google Scholar] [CrossRef] [PubMed]
- Todumrong, N.; Charoenvidhya, D.B.U. Use of Placental Pulsatility Index in High Risk Pregnancy to Predict Fetal Growth Restriction. Thai J. Obstet. Gynaecol. 2022, 30, 8. [Google Scholar]
- Stampalija, T.; Monasta, L.; Barbieri, M.; Chiodo, A.; Quadrifoglio, M.; Fantasia, I.; Bello, L.L.; Barresi, V.; Ottaviani, C.; Di Martino, D.D.; et al. Late-term fetuses with reduced umbilical vein blood flow volume: An under-recognized population at increased risk of growth restriction. Eur J Obstet Gynecol Reprod Biol 2022, 272, 182–187. [Google Scholar] [CrossRef] [PubMed]
- Hamidi, O.P.; Driver, C.; Steller, J.G.; Peek, E.E.; Monasta, L.; Stampalija, T.; Gumina, D.L.; DeVore, G.R.; Hobbins, J.C.; Galan, H.L. Umbilical Venous Volume Flow in Late-Onset Fetal Growth Restriction. J Ultrasound Med 2023, 42, 173–183. [Google Scholar] [CrossRef] [PubMed]
- Barbieri, M.; Di Martino, D.D.; Ferrazzi, E.M.; Stampalija, T. Umbilical vein blood flow: State-of-the-art. J Clin Ultrasound 2023, 51, 318–325. [Google Scholar] [CrossRef] [PubMed]
- Barbieri, M.; Zamagni, G.; Fantasia, I.; Monasta, L.; Lo Bello, L.; Quadrifoglio, M.; Ricci, G.; Maso, G.; Piccoli, M.; Di Martino, D.D.; et al. Umbilical Vein Blood Flow in Uncomplicated Pregnancies: Systematic Review of Available Reference Charts and Comparison with a New Cohort. J Clin Med 2023, 12. [Google Scholar] [CrossRef] [PubMed]
- Najafzadeh, A.; Dickinson, J.E. Umbilical venous blood flow and its measurement in the human fetus. J Clin Ultrasound 2012, 40, 502–11. [Google Scholar] [CrossRef]
- Lees, C.; Visser, G.H. A.; Hecher, K. , Placental-Fetal Growth Restriction. Cambridge University Press: Cambridge, 2018.
- Wang, L.; Zhou, Q.; Zhou, C.; Wang, J.; Shi, C.; Long, B.; Hu, L.; Peng, Y.; Liu, Y.; Xu, G. Z-Score Reference Ranges for Umbilical Vein Diameter and Blood Flow Volume in Normal Fetuses. Journal of Ultrasound in Medicine 2022, 41, 907–916. [Google Scholar] [CrossRef]
- Opheim, G.L.; Moe Holme, A.; Blomhoff Holm, M.; Melbye Michelsen, T.; Muneer Zahid, S.; Paasche Roland, M.C.; Henriksen, T.; Haugen, G. The impact of umbilical vein blood flow and glucose concentration on blood flow distribution to the fetal liver and systemic organs in healthy pregnancies. The FASEB Journal 2020, 34, 12481–12491. [Google Scholar] [CrossRef] [PubMed]
- Figueras, F.; Fernandez, S.; Hernandez-Andrade, E.; Gratacos, E. Umbilical venous blood flow measurement: accuracy and reproducibility. Ultrasound Obstet Gynecol 2008, 32, 587–91. [Google Scholar] [CrossRef] [PubMed]
- Flo, K.; Wilsgaard, T.; Acharya, G. Longitudinal reference ranges for umbilical vein blood flow at a free loop of the umbilical cord. Ultrasound Obstet Gynecol 2010, 36, 567–72. [Google Scholar] [CrossRef]
- Bhide, A.; Acharya, G.; Baschat, A.; Bilardo, C.M.; Brezinka, C.; Cafici, D.; Ebbing, C.; Hernandez-Andrade, E.; Kalache, K.; Kingdom, J.; et al. ISUOG Practice Guidelines (updated): use of Doppler velocimetry in obstetrics. Ultrasound Obstet Gynecol 2021, 58, 331–339. [Google Scholar] [CrossRef]
- AIUM Practice Parameter for the Performance of Detailed Second- and Third-Trimester Diagnostic Obstetric Ultrasound Examinations. Journal of Ultrasound in Medicine 2019, 38, 3093–3100. [CrossRef]
- Salomon, L.J.; Alfirevic, Z.; Berghella, V.; Bilardo, C.M.; Chalouhi, G.E.; Da Silva Costa, F.; Hernandez-Andrade, E.; Malinger, G.; Munoz, H.; Paladini, D.; et al. ISUOG Practice Guidelines (updated): performance of the routine mid-trimester fetal ultrasound scan. Ultrasound Obstet Gynecol 2022, 59, 840–856. [Google Scholar] [CrossRef]
- Dev Maulik; Lees, C.C., Doppler Ultrasound in Obstetrics and Gynecology, 3 ed.; Springer: Cham, 2023; p XI, 649.
- DeVore, G.R.; Epstein, A. Computing Z-Score Equations for Clinical Use to Measure Fetal Umbilical Vein Size and Flow Using Six Independent Variables of Age and Size. J Ultrasound Med 2022, 41, 1949–1960. [Google Scholar] [CrossRef]
- Jaiman, S.; Romero, R.; Bhatti, G.; Jung, E.; Gotsch, F.; Suksai, M.; Gallo, D.M.; Chaiworapongsa, T.; Kadar, N. The role of the placenta in spontaneous preterm labor and delivery with intact membranes. J Perinat Med 2022, 50, 553–566. [Google Scholar] [CrossRef] [PubMed]
- Preston, M.; Hall, M.; Shennan, A.; Story, L. The role of placental insufficiency in spontaneous preterm birth: A literature review. Eur J Obstet Gynecol Reprod Biol 2024, 295, 136–142. [Google Scholar] [CrossRef]
- Mecke, L.; Ignatov, A.; Redlich, A. The importance of the cerebroplacental ratio for the prognosis of neonatal outcome in AGA fetuses. Arch Gynecol Obstet 2023, 307, 311–317. [Google Scholar] [CrossRef]
- Malhotra, A.; Allison, B.J.; Castillo-Melendez, M.; Jenkin, G.; Polglase, G.R.; Miller, S.L. Neonatal Morbidities of Fetal Growth Restriction: Pathophysiology and Impact. Front Endocrinol (Lausanne) 2019, 10, 55. [Google Scholar] [CrossRef] [PubMed]
| Variables | Value | 10th | 90th |
| Maternal age (years) | 30.00 | NA | NA |
| Gravidity | 2.00 | NA | NA |
| GA at measurement (weeks) | 27.14 | NA | NA |
| GA at delivery (weeks) | 38.67±2.43 | NA | NA |
| PTB | 44(8.94%) | NA | NA |
| Birth weight (g) | 3118.75±596.18 | 2520.00 | 3738.00 |
| LBW at delivery | 34(6.91%) | NA | NA |
| UVBF (ml/min) | 151.58±80.69 | 63.86 | 265.00 |
| UA PI | 1.05±0.23 | 0.77 | 1.35 |
| UA RI | 0.65±0.09 | 0.54 | 0.76 |
| mUt A PI | 0.81±0.26 | 0.55 | 1.11 |
| mUt A RI | 0.51±0.09 | 0.40 | 0.62 |
| MCA PI | 1.93±0.43 | 1.42 | 2.50 |
| MCA RI | 0.83±0.08 | 0.74 | 0.91 |
| PPI | 0.93±0.20 | 0.71 | 1.17 |
| UVBF/PPI | 180.45±119.32 | 59.28 | 336.06 |
| CPR | 1.92±0.58 | 1.26 | 2.69 |
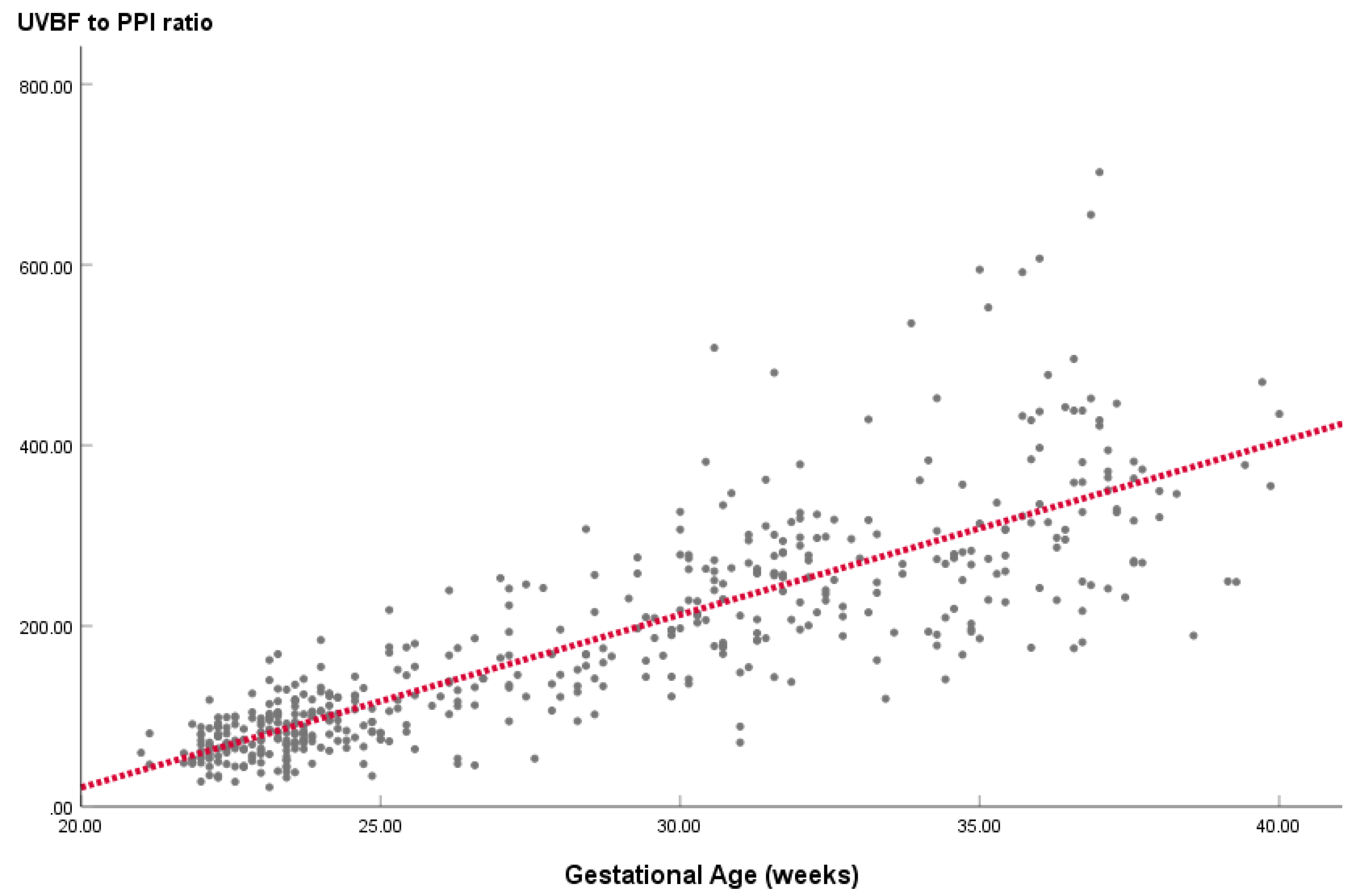
| GA(week) | n | UVBF to PPI ratio | |
| Mean | SD | ||
| 21+0 – 21+6 | 9 | 59.85 | 15.83 |
| 22+0 – 22+6 | 64 | 68.84 | 21.16 |
| 23+0 – 23+6 | 86 | 84.86 | 28.74 |
| 24+0 – 24+6 | 40 | 100.38 | 29.67 |
| 25+0 – 25+6 | 21 | 121.96 | 44.77 |
| 26+0 – 26+6 | 18 | 127.73 | 48.79 |
| 27+0 – 27+6 | 17 | 166.07 | 59.32 |
| 28+0 – 28+6 | 19 | 164.22 | 51.51 |
| 29+0 – 29+6 | 15 | 192.35 | 42.02 |
| 30+0 – 30+6 | 33 | 248.26 | 74.35 |
| 31+0 – 31+6 | 34 | 240.78 | 79.07 |
| 32+0 – 32+6 | 24 | 265.06 | 50.03 |
| 33+0 – 33+6 | 13 | 273.73 | 109.41 |
| 34+0 – 34+6 | 23 | 257.91 | 76.95 |
| 35+0 – 35+6 | 20 | 338.56 | 124.11 |
| 36+0 – 36+6 | 27 | 357.16 | 120.69 |
| 37+0 – 37+6 | 19 | 360.73 | 103.74 |
| 38+0 – 38+6 | 4 | 301.37 | 75.83 |
| 39+0 – 39+6 | 5 | 340.31 | 93.74 |
| 40+0 – 40+6 | 1 | 434.81 | NA |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




