Submitted:
17 April 2024
Posted:
18 April 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Data Sources and Study Design
2.2. Exposure Ascertainment
2.3. Outcome Ascertainment
2.4. Covariate Ascertainment
2.5. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Jia, H.; Lubetkin, E.I.; DeMichele, K.; Stark, D.S.; Zack, M.M.; Thompson, W.W. Prevalence, risk factors, and burden of disease for falls and balance or walking problems among older adults in the US. Preventive medicine 2019, 126, 105737. [Google Scholar] [CrossRef] [PubMed]
- Choi, N.G.; Choi, B.Y.; DiNitto, D.M.; Marti, C.N.; Kunik, M.E. Fall-related emergency department visits and hospitalizations among community-dwelling older adults: examination of health problems and injury characteristics. BMC Geriatr. 2019, 19, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Vaishya, R.; Vaish, A. Falls in older adults are serious. Indian journal of orthopaedics 2020, 54, 69–74. [Google Scholar] [CrossRef]
- Seppala, L.J.; Wermelink, A.M.; de Vries, M.; Ploegmakers, K.J.; van de Glind, E.M.; Daams, J.G.; van der Velde, N.; Blain, H.; Bousquet, J.; Bucht, G.; et al. Fall-Risk-Increasing Drugs: A Systematic Review and Meta-Analysis: II. Psychotropics. J. Am. Med Dir. Assoc. 2018, 19, 371–e11. [Google Scholar] [CrossRef]
- Seppala, L.J.; van de Glind, E.M.; Daams, J.G.; Ploegmakers, K.J.; de Vries, M.; Wermelink, A.M.; van der Velde, N.; Blain, H.; Bousquet, J.; Bucht, G.; et al. Fall-Risk-Increasing Drugs: A Systematic Review and Meta-analysis: III. Others. J. Am. Med Dir. Assoc. 2018, 19, 372–e1. [Google Scholar] [CrossRef] [PubMed]
- Maust, D.T.; Bohnert, A.S.B.; Strominger, J.; Alexander, N.; Min, L.; Hoffman, G.J.; Goldstick, J.E. Prescription characteristics associated with fall-related injury risk among older adults prescribed benzodiazepines: a cohort study. BMC Geriatr. 2022, 22, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Panel, A.G.S.B.C.U.E.; Fick, D.M.; Semla, T.P.; Steinman, M.; Beizer, J.; Brandt, N.; Dombrowski, R.; DuBeau, C.E.; Pezzullo, L.; Epplin, J.J. American Geriatrics Society 2019 updated AGS Beers Criteria® for potentially inappropriate medication use in older adults. Journal of the American Geriatrics Society 2019, 67, 674–694. [Google Scholar]
- Rhee, T.G. Coprescribing of Benzodiazepines and Opioids in Older Adults: Rates, Correlates, and National Trends. Journals Gerontol. Ser. A 2018, 74, 1910–1915. [Google Scholar] [CrossRef] [PubMed]
- Guerriero, F. Guidance on opioids prescribing for the management of persistent non-cancer pain in older adults. World J. Clin. Cases 2017, 5, 73–81. [Google Scholar] [CrossRef]
- Tannenbaum, C. Inappropriate benzodiazepine use in elderly patients and its reduction. J. Psychiatry Neurosci. 2015, 40, E27–E28. [Google Scholar] [CrossRef]
- Centers for Medicare and Medicaid Services. Concurrent use of opioids and benzodiazepines in a Medicare Part D population. https://www.cms.gov/Medicare/Prescription-Drug-Coverage/PrescriptionDrugCovContra/Downloads/Concurrent-Use-of-Opioids-and-Benzodiazepines-in-a-Medicare-Part-D-Population-CY-2015.pdf. Published , 2016. Accessed January 13, 2024. 12 May.
- Mues, K.; Liede, A.; Liu, J.; Wetmore, J.B.; Zaha, R.; Bradbury, B.D.; Collins, A.J.; Gilbertson, D.T. Use of the Medicare database in epidemiologic and health services research: a valuable source of real-world evidence on the older and disabled populations in the US. Clin. Epidemiology 2017, ume 9, 267–277. [Google Scholar] [CrossRef]
- Creighton, S.; Duddy-Tenbrunsel, R.; Michel, J. The promise and pitfalls of Medicare Advantage encounter data. Health Affairs Forefront 2019.
- Von Elm, E.; Altman, D.G.; Egger, M.; Pocock, S.J.; Gøtzsche, P.C.; Vandenbroucke, J.P. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: Guidelines for reporting observational studies. J. Clin. Epidemiol. 2008, 61, 344–349. [Google Scholar] [CrossRef] [PubMed]
- Twisk, J.; Hoekstra, T. Classifying developmental trajectories over time should be done with great caution: a comparison between methods. J. Clin. Epidemiology 2012, 65, 1078–1087. [Google Scholar] [CrossRef] [PubMed]
- Jones, B.L.; Nagin, D.S. Advances in Group-Based Trajectory Modeling and an SAS Procedure for Estimating Them. Sociol. Methods Res. 2007, 35, 542–571. [Google Scholar] [CrossRef]
- Nagin, D.S.; Jones, B.L.; Passos, V.L.; E Tremblay, R. Group-based multi-trajectory modeling. Stat. Methods Med Res. 2016, 27, 2015–2023. [Google Scholar] [CrossRef] [PubMed]
- Zhou, L.; Bhattacharjee, S.; Kwoh, C.K.; Tighe, P.J.; Reisfield, G.M.; Malone, D.C.; Slack, M.; Wilson, D.L.; Chang, C.; Lo-Ciganic, W. Dual-trajectories of opioid and gabapentinoid use and risk of subsequent drug overdose among Medicare beneficiaries in the United States: a retrospective cohort study. Addiction 2020, 116, 819–830. [Google Scholar] [CrossRef] [PubMed]
- Center for Disease Control and Prevention. Guideline for Prescribing Opioids for Chronic Pain. Available online: https://www.cdc.gov/drugoverdose/pdf/guidelines_at-a-glance-a.pdf (accessed on 4 March).
- Brandt, J.; Alkabanni, W.; Alessi-Severini, S.; Leong, C. Translating Benzodiazepine Utilization Data into Meaningful Population Exposure: Integration of Two Metrics for Improved Reporting. Clin. Drug Investig. 2018, 38, 565–572. [Google Scholar] [CrossRef]
- Farinde, A.; Medscape Benzodiazepine Equivalency Chart. Medscape. Available online: https://emedicine.medscape.com/article/2172250-overview#showall (accessed on 20 October).
- Psychiatric Disorders. Conn’s current therapy 2016, Bope, E.T., Kellerman, R.D., Eds.; Elsevie: Philadelphia, PA, 2016; pp. 969–1004. [Google Scholar]
- MDCalc. Benzodiazepine Conversion Calculator. Available online: https://www.mdcalc.com/benzodiazepine-conversion-calculator#evidence (accessed on 21 October).
- Lo-Ciganic, W.; Hincapie-Castillo, J.; Wang, T.; Ge, Y.; Jones, B.L.; Huang, J.L.; Chang, C.; Wilson, D.L.; Lee, J.K.; Reisfield, G.M.; et al. Dosing profiles of concurrent opioid and benzodiazepine use associated with overdose risk among US Medicare beneficiaries: group-based multi-trajectory models. Addiction 2022, 117, 1982–1997. [Google Scholar] [CrossRef]
- Schwarz, G. Estimating the Dimension of a Model. Ann. Stat. 1978, 6, 461–464. [Google Scholar] [CrossRef]
- Nagin, D.S.; Nagin, D.; Nagin, T.H. Group-Based Modeling of Development; Harvard University Press: 2005.
- Vittinghoff, E.; McCulloch, C.E. Relaxing the Rule of Ten Events per Variable in Logistic and Cox Regression. Am. J. Epidemiology 2006, 165, 710–718. [Google Scholar] [CrossRef] [PubMed]
- Lo-Ciganic, W.-H.; Huang, J.L.; Zhang, H.H.; Weiss, J.C.; Wu, Y.; Kwoh, C.K.; Donohue, J.M.; Cochran, G.; Gordon, A.J.; Malone, D.C.; et al. Evaluation of Machine-Learning Algorithms for Predicting Opioid Overdose Risk Among Medicare Beneficiaries With Opioid Prescriptions. JAMA Netw. Open 2019, 2, e190968. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.-B.; Zingmond, D.S.; Keeler, E.B.; Jennings, L.A.; Wenger, N.S.; Reuben, D.B.; Ganz, D.A. Development of an algorithm to identify fall-related injuries and costs in Medicare data. Inj. Epidemiology 2016, 3, 1–11. [Google Scholar] [CrossRef]
- Ganz, D.A.; Kim, S.; Zingmond, D.S.; Ramirez, K.D.; Roth, C.P.; Jennings, L.A.; Mori, T.; Keeler, E.B.; Wenger, N.S.; Reuben, D.B. Effect of a Falls Quality Improvement Program on Serious Fall-Related Injuries. J. Am. Geriatr. Soc. 2015, 63, 63–70. [Google Scholar] [CrossRef] [PubMed]
- Hoffman, G.J.; Hays, R.D.; Shapiro, M.F.; Wallace, S.P.; Ettner, S.L. Claims-based Identification Methods and the Cost of Fall-related Injuries Among US Older Adults. Med Care 2016, 54, 664–671. [Google Scholar] [CrossRef] [PubMed]
- Meara, E.; Horwitz, J.R.; Powell, W.; McClelland, L.; Zhou, W.; O'Malley, A.J.; Morden, N.E. State Legal Restrictions and Prescription-Opioid Use among Disabled Adults. New Engl. J. Med. 2016, 375, 44–53. [Google Scholar] [CrossRef] [PubMed]
- Health, U.D.o.; Services, H. Falls and Fractures in Older Adults: Causes and Prevention. 2023.
- Deandrea, S.; Lucenteforte, E.; Bravi, F.; Foschi, R.; La Vecchia, C.; Negri, E. Risk factors for falls in community-dwelling older people:” a systematic review and meta-analysis”. Epidemiology 2010, 658–668. [Google Scholar] [CrossRef] [PubMed]
- Chesnaye, N.C.; Stel, V.S.; Tripepi, G.; Dekker, F.W.; Fu, E.L.; Zoccali, C.; Jager, K.J. An introduction to inverse probability of treatment weighting in observational research. Clin. Kidney J. 2021, 15, 14–20. [Google Scholar] [CrossRef] [PubMed]
- Andrade, C. Mean difference, standardized mean difference (SMD), and their use in meta-analysis: as simple as it gets. The Journal of clinical psychiatry 2020, 81, 11349. [Google Scholar] [CrossRef]
- Funk, M.J.; Westreich, D.; Wiesen, C.; Stürmer, T.; Brookhart, M.A.; Davidian, M. Doubly Robust Estimation of Causal Effects. Am. J. Epidemiology 2011, 173, 761–767. [Google Scholar] [CrossRef]
- Grambsch PM, Therneau TM. Proportional hazards tests and diagnostics based on weighted residuals. Biometrika 1994, 81, 515–526.
- VanderWeele, T.J.; Ding, P. Sensitivity Analysis in Observational Research: Introducing the E-Value. Ann. Intern. Med. 2017, 167, 268–274. [Google Scholar] [CrossRef] [PubMed]
- Miller, M.; Stürmer, T.; Azrael, D.; Levin, R.; Solomon, D.H. Opioid Analgesics and the Risk of Fractures in Older Adults with Arthritis. J. Am. Geriatr. Soc. 2011, 59, 430–438. [Google Scholar] [CrossRef]
- Saunders, K.W.; Dunn, K.M.; Merrill, J.O.; Sullivan, M.; Weisner, C.; Braden, J.B.; Psaty, B.M.; Von Korff, M. Relationship of Opioid Use and Dosage Levels to Fractures in Older Chronic Pain Patients. J. Gen. Intern. Med. 2010, 25, 310–315. [Google Scholar] [CrossRef] [PubMed]
- Ray, W.A.; Thapa, P.B.; Gideon, P. Benzodiazepines and the Risk of Falls in Nursing Home Residents. J. Am. Geriatr. Soc. 2000, 48, 682–685. [Google Scholar] [CrossRef]
- Na, I.; Seo, J.; Park, E.; Lee, J. Risk of Falls Associated with Long-Acting Benzodiazepines or Tricyclic Antidepressants Use in Community-Dwelling Older Adults: A Nationwide Population-Based Case–Crossover Study. Int. J. Environ. Res. Public Heal. 2022, 19, 8564. [Google Scholar] [CrossRef] [PubMed]
- Dowell, D.; Ragan, K.R.; Jones, C.M.; Baldwin, G.T.; Chou, R. CDC Clinical Practice Guideline for Prescribing Opioids for Pain—United States, 2022. MMWR. Recomm. Rep. 2022, 71, 1–95. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Wilson, D.L.; Fernandes, D.; Adkins, L.E.; Bantad, A.; Copacia, C.; Dharma, N.; Huang, P.-L.; Joseph, A.; Park, T.W.; et al. Deprescribing Strategies for Opioids and Benzodiazepines with Emphasis on Concurrent Use: A Scoping Review. J. Clin. Med. 2023, 12, 1788. [Google Scholar] [CrossRef]
- Wang, Y.; Wilson, D.L.; Fernandes, D.; Adkins, L.E.; Bantad, A.; Copacia, C.; Dharma, N.; Huang, P.-L.; Joseph, A.; Park, T.W.; et al. Deprescribing Strategies for Opioids and Benzodiazepines with Emphasis on Concurrent Use: A Scoping Review. J. Clin. Med. 2023, 12, 1788. [Google Scholar] [CrossRef]
- Hickson, R.P.; Annis, I.E.; Killeya-Jones, L.A.; Fang, G. Opening the black box of the group-based trajectory modeling process to analyze medication adherence patterns: An example using real-world statin adherence data. Pharmacoepidemiol. Drug Saf. 2019, 29, 357–362. [Google Scholar] [CrossRef]
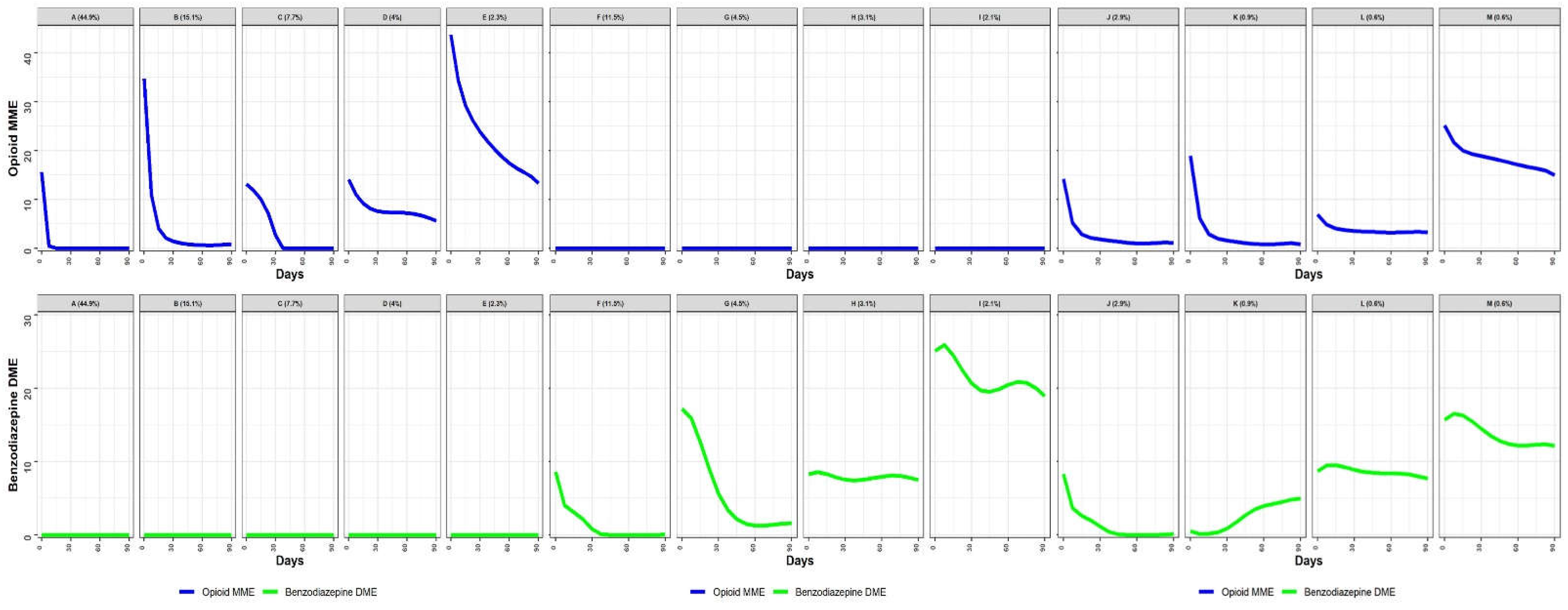
| Trajectory groups* | Overall: n=622,588 (100.0%) | OPI use only† | BZD use only† | OPI-BZD use only† | SMD‡ | |||||||||||
| A: n=279,263 (44.9%) | B: n=93,703 (15.1%) | C: n=47,851 (7.7%) | D: n=24,952 (4.0%) | E: n=14,225 (2.3%) | F: n=71,715 (11.5%) | G: n=28,109 (4.5%) | H: n=19,230 (3.1%) | I: n=13,013 (2.1%) | J: n=17,750 (2.9%) | K: n=5,601 (0.9%) | L: n=3,729 (0.6%) | M: n=3,447 (0.6%) | before IPTW | after IPTW |
||
| Age ≥65 years, % | 84.6 | 85.5 | 85.1 | 87.3 | 82.8 | 78.0 | 85.7 | 82.0 | 83.9 | 69.3 | 85.7 | 81.6 | 79.5 | 64.5 | 0.18 | 0.01 |
| Female, % | 58.1 | 53.8 | 53.3 | 64.3 | 62.9 | 52.9 | 70.9 | 66.3 | 59.5 | 56.8 | 63.8 | 65.5 | 63.0 | 57.3 | 0.14 | 0.02 |
| Race/ethnicity group, % | ||||||||||||||||
| White | 82.7 | 82.2 | 83.7 | 76.3 | 77.2 | 83.4 | 86.8 | 84.4 | 84.3 | 82.9 | 86.8 | 84.1 | 85.3 | 84.4 | 0.09 | 0.02 |
| Black | 9.0 | 9.5 | 9.3 | 12.5 | 13.1 | 10.2 | 5.7 | 6.2 | 5.9 | 6.7 | 6.3 | 7.7 | 6.5 | 8.2 | 0.10 | 0.03 |
| Others | 8.3 | 8.2 | 6.9 | 11.1 | 9.7 | 6.4 | 7.5 | 9.4 | 9.7 | 10.4 | 6.9 | 8.2 | 8.2 | 7.5 | 0.06 | 0.01 |
| Disability status, % | 21.6 | 19.8 | 21.1 | 21.6 | 27.4 | 30.9 | 19.5 | 24.3 | 22.9 | 38.1 | 19.6 | 25.1 | 28.2 | 43.9 | 0.18 | 0.01 |
| LIS/Dual eligibility, % | ||||||||||||||||
| No LIS/dual eligibility | 72.9 | 75.5 | 76.1 | 66.6 | 58.9 | 69.6 | 74.8 | 68.1 | 65.9 | 56.3 | 78.3 | 70.2 | 63.4 | 58.6 | 0.18 | 0.02 |
| LIS or dual eligibility | 5.1 | 5.0 | 4.8 | 5.4 | 7.0 | 7.9 | 4.2 | 5.1 | 5.2 | 7.8 | 4.0 | 4.9 | 7.5 | 11.9 | 0.09 | 0.01 |
| LIS and dual eligibility | 22.0 | 19.5 | 19.1 | 27.9 | 34.1 | 22.5 | 21.1 | 26.9 | 29.0 | 35.9 | 17.7 | 24.9 | 29.1 | 29.4 | 0.16 | 0.02 |
| Metropolitan residence | 81.9 | 81.6 | 80.0 | 81.6 | 79.2 | 79.4 | 85.5 | 84.4 | 80.6 | 83.8 | 84.3 | 82.8 | 80.2 | 80.1 | 0.07 | 0.02 |
| Elixhauser Comorbidity Index, mean (SD) | 3.3 (2.7) | 3.1 (2.6) | 3.6 (2.7) | 3.8 (2.7) | 4.1 (2.9) | 3.6 (2.8) | 3.1 (2.5) | 3.3 (2.7) | 3.4 (2.6) | 3.5 (2.8) | 3.2 (2.7) | 3.8 (2.9) | 4.0 (3.1) | 3.7 (3.1) | 0.14 | 0.01 |
| Opioid use disorder, % | 0.4 | 0.2 | 0.4 | 0.3 | 0.5 | 1.5 | 0.3 | 0.5 | 0.3 | 1.6 | 0.4 | 0.5 | 0.6 | 2.6 | 0.07 | 0.01 |
| Alcohol use disorders, % | 1.2 | 1.0 | 1.2 | 0.9 | 1.4 | 1.8 | 1.1 | 1.9 | 1.2 | 2.8 | 1.5 | 1.4 | 1.3 | 3.5 | 0.06 | 0.02 |
| Other SUD, % | 0.8 | 0.6 | 0.7 | 0.5 | 0.7 | 1.2 | 0.7 | 1.5 | 0.9 | 3.2 | 0.8 | 1.2 | 1.3 | 2.4 | 0.07 | 0.01 |
| Anxiety disorders, % | 11.1 | 6.7 | 8.3 | 7.3 | 9.3 | 9.7 | 20.8 | 26.1 | 19.2 | 30.7 | 14.7 | 17.8 | 24.6 | 25.7 | 0.27 | 0.02 |
| Mood disorders, % | 12.3 | 9.5 | 11.6 | 10.8 | 15.0 | 14.3 | 14.6 | 20.2 | 16.9 | 29.4 | 13.0 | 17.5 | 20.6 | 24.3 | 0.17 | 0.02 |
| Sleep disorders, % | 15.1 | 13.2 | 16.8 | 14.4 | 16.6 | 19.5 | 14.3 | 18.7 | 16.3 | 24.0 | 16.6 | 19.2 | 21.9 | 21.7 | 0.10 | 0.01 |
| Musculoskeletal conditions, % | 47.4 | 41.3 | 58.8 | 59.6 | 63.3 | 71.4 | 43.1 | 40.3 | 36.6 | 36.3 | 51.9 | 54.4 | 48.7 | 58.5 | 0.27 | 0.03 |
| Pain conditions, % | ||||||||||||||||
| Osteoarthritis | 36.8 | 32.4 | 46.3 | 44.8 | 47.3 | 53.1 | 34.0 | 31.2 | 28.9 | 27.1 | 40.2 | 42.2 | 37.6 | 41.9 | 0.20 | 0.02 |
| Low back pain | 21.2 | 17.5 | 25.2 | 31.7 | 36.0 | 36.6 | 17.7 | 16.3 | 14.2 | 15.9 | 25.7 | 27.2 | 24.1 | 36.9 | 0.23 | 0.02 |
| Neck pain | 8.0 | 6.6 | 9.0 | 10.7 | 11.3 | 12.5 | 7.8 | 7.0 | 5.8 | 6.5 | 10.6 | 10.5 | 9.3 | 15.1 | 0.11 | 0.01 |
| Chest pain | 12.4 | 11.5 | 13.5 | 12.9 | 13.5 | 12.1 | 12.2 | 14.0 | 11.2 | 12.1 | 13.8 | 15.7 | 17.4 | 15.5 | 0.06 | 0.01 |
| Abdominal pain | 17.5 | 19.3 | 20.2 | 15.5 | 16.3 | 14.7 | 13.2 | 13.5 | 11.5 | 12.5 | 16.5 | 21.8 | 19.4 | 20.1 | 0.11 | 0.01 |
| Rheumatoid arthritis | 2.6 | 2.1 | 2.9 | 4.5 | 4.9 | 3.9 | 2.0 | 2.2 | 1.9 | 2.0 | 2.7 | 3.1 | 2.7 | 3.3 | 0.07 | 0.01 |
| Pelvic pain | 3.1 | 3.1 | 3.1 | 2.7 | 2.5 | 2.5 | 3.6 | 3.1 | 2.1 | 2.5 | 4.1 | 4.3 | 3.6 | 4.4 | 0.05 | 0.01 |
| Headache/migraine | 5.2 | 4.6 | 5.1 | 5.5 | 5.8 | 5.6 | 6.2 | 6.4 | 4.6 | 6.4 | 7.0 | 7.9 | 7.9 | 7.9 | 0.06 | 0.01 |
| TMJ | 0.2 | 0.2 | 0.2 | 0.2 | 0.2 | 0.1 | 0.3 | 0.3 | 0.2 | 0.2 | 0.3 | 0.4 | 0.02 | 0.02 | ||
| Others | 21.5 | 19.9 | 25.3 | 25.0 | 26.3 | 27.2 | 19.7 | 18.0 | 16.0 | 17.0 | 24.9 | 26.4 | 23.4 | 26.3 | 0.11 | 0.01 |
| Any hospitalization, % | 13.8 | 11.0 | 28.0 | 10.2 | 12.1 | 29.2 | 7.8 | 11.5 | 9.0 | 14.8 | 12.9 | 16.3 | 17.9 | 20.6 | 0.21 | 0.04 |
| ED visits, % | ||||||||||||||||
| 0 | 87.9 | 88.5 | 87.5 | 88.2 | 85.6 | 87.4 | 89.4 | 85.5 | 88.3 | 83.7 | 87.8 | 83.0 | 81.2 | 81.5 | 0.09 | 0.01 |
| 1 | 10.5 | 10.1 | 10.7 | 10.2 | 12.1 | 10.7 | 9.1 | 12.2 | 10.0 | 13.4 | 10.3 | 14.0 | 15.7 | 15.1 | 0.08 | 0.01 |
| ≥2 | 1.7 | 1.4 | 1.8 | 1.6 | 2.3 | 1.9 | 1.5 | 2.3 | 1.7 | 2.9 | 2.0 | 3.0 | 3.1 | 3.4 | 0.05 | 0.01 |
| Outpatient visits, % | ||||||||||||||||
| 0 | 38.0 | 38.3 | 29.1 | 40.3 | 37.6 | 32.0 | 42.7 | 45.1 | 43.9 | 46.8 | 38.4 | 34.2 | 37.0 | 37.8 | 0.12 | 0.02 |
| 1 | 23.4 | 23.6 | 23.3 | 22.7 | 22.3 | 23.3 | 23.6 | 23.2 | 23.2 | 23.4 | 22.9 | 23.1 | 23.0 | 22.2 | 0.01 | 0.01 |
| 2-5 | 33.3 | 32.9 | 39.9 | 32.3 | 34.2 | 38.0 | 29.8 | 28.2 | 29.4 | 26.5 | 33.3 | 35.8 | 34.1 | 33.8 | 0.10 | 0.02 |
| >5 | 5.3 | 5.2 | 7.7 | 4.7 | 5.9 | 6.7 | 3.9 | 3.6 | 3.5 | 3.3 | 5.4 | 6.9 | 6.0 | 6.2 | 0.08 | 0.01 |
| No. antidepressants | 0.8 (2.1) | 0.7 (1.9) | 0.7 (1.9) | 0.8 (2.1) | 1.1 (2.5) | 0.9 (2.2) | 1.0 (2.4) | 1.3 (2.6) | 1.2 (2.7) | 1.8 (3.2) | 0.9 (2.1) | 1.2 (2.4) | 1.2 (2.5) | 1.2 (2.6) | 0.14 | 0.01 |
| No. antipsychotics | 0.3 (1.7) | 0.2 (1.4) | 0.2 (1.2) | 0.2 (1.3) | 0.3 (1.6) | 0.2 (1.1) | 0.4 (2.1) | 0.7 (2.8) | 0.6 (2.5) | 1.4 (3.8) | 0.2 (1.2) | 0.4 (2.0) | 0.4 (2.0) | 0.5 (3.6) | 0.14 | 0.02 |
| No. gabapentinoids | 0.2 (1.0) | 0.2 (0.9) | 0.3 (1.1) | 0.4 (1.2) | 0.6 (1.6) | 0.4 (1.3) | 0.2 (0.9) | 0.2 (1.0) | 0.2 (1.0) | 0.3 (1.2) | 0.2 (0.9) | 0.3 (1.1) | 0.3 (1.2) | 0.4 (1.4) | 0.11 | 0.01 |
| No. muscle relaxants | 0.1 (0.6) | 0.1 (0.5) | 0.1 (0.6) | 0.1 (0.6) | 0.2 (0.9) | 0.2 (0.7) | 0.1 (0.6) | 0.1 (0.6) | 0.1 (0.6) | 0.1 (0.7) | 0.1 (0.6) | 0.1 (0.7) | 0.1 (0.6) | 0.2 (0.8) | 0.07 | 0.01 |
| No. naltrexone | 0.0 (0.1) | 0.0 (0.1) | 0.0 (0.1) | 0.0 (0.1) | 0.0 (0.1) | 0.0 (0.1) | 0.0 (0.1) | 0.0 (0.2) | 0.0 (0.1) | 0.0 (0.2) | 0.0 (0.1) | 0.0 (0.1) | 0.0 (0.0) | 0.0 (0.1) | 0.02 | 0.01 |
| Polypharmacy (≥5 medications including OPI/BZD), % | 87.6 | 86.1 | 88.2 | 91.7 | 91.7 | 85.6 | 87.7 | 88.5 | 90.0 | 87.0 | 87.9 | 90.9 | 88.5 | 78.0 | 0.11 | 0.01 |
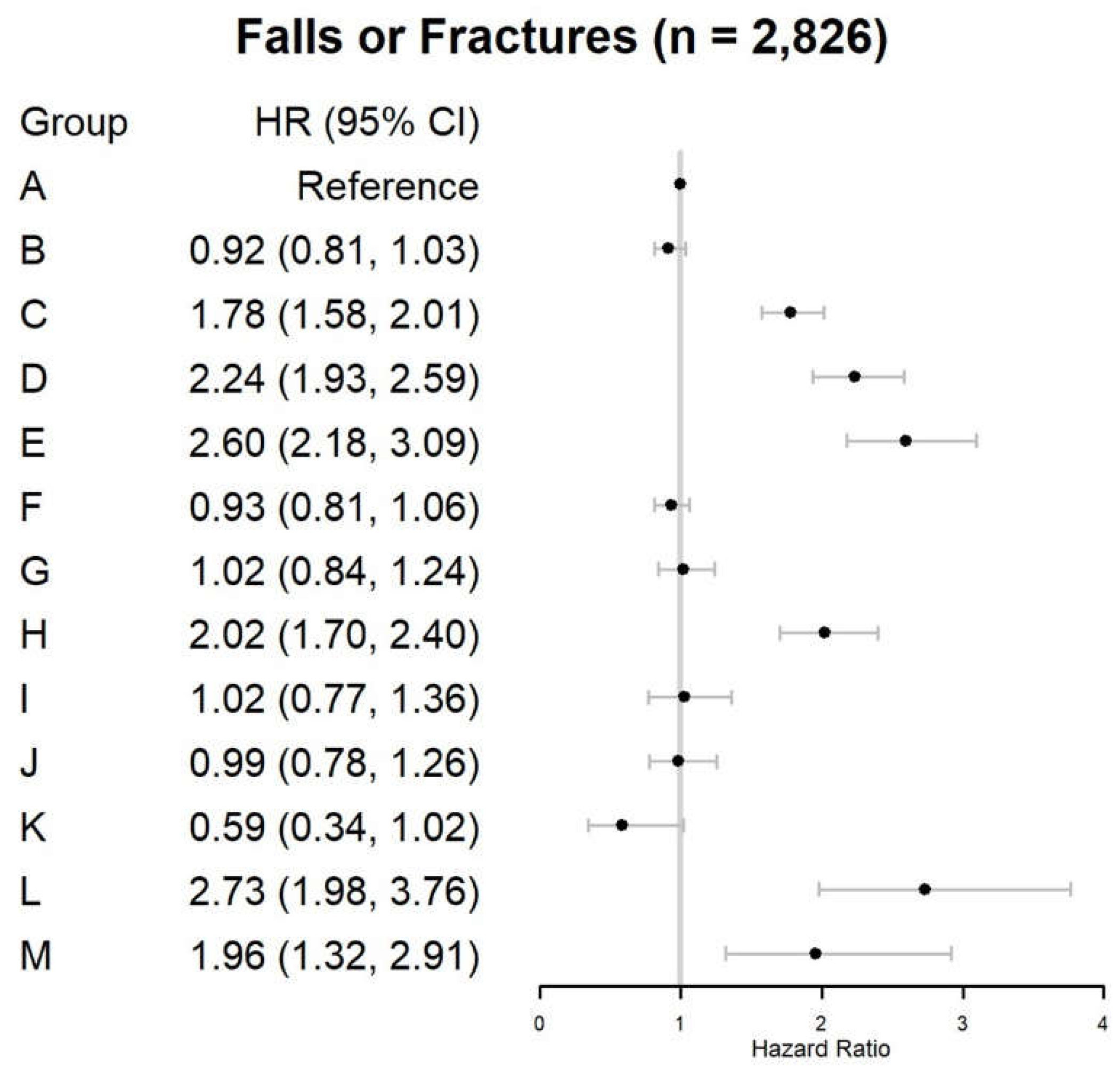
| Trajectory Groups§ | Injurious Falls (n=2,826) | |||
| N (crude rate*) | Days of follow-up, median (IQR) | HR (95%CI) | ||
| Unadjusted | Adjusted† | |||
| OPI use only | ||||
| Very-low OPI-only (early discontinuation) | 1,037 (12.4) | 44 (41.0) | Reference | Reference |
| Low OPI-only (rapid decline) | 323 (11.5) | 51 (45.0) | 0.93 (0.82, 1.05) | 0.92 (0.81, 1.03) |
| Very-low OPI-only (late discontinuation) | 360 (25.1) | 37 (46.5) | 2.03 (1.80, 2.29) | 1.78 (1.58, 2.01) |
| Low OPI-only (gradual decline) | 219 (29.3) | 48 (37.0) | 2.37 (2.05, 2.74) | 2.24 (1.93, 2.59) |
| Moderate OPI-only (rapid decline) | 122 (28.6) | 40 (41.0) | 2.32 (1.92, 2.79) | 2.60 (2.18, 3.09) |
| BZD use only | ||||
| Very-low BZD-only (late discontinuation) | 276 (12.8) | 51 (39.5) | 1.04 (0.91, 1.18) | 0.93 (0.81, 1.07) |
| Low BZD-only (rapid decline) | 122 (14.5) | 47 (46.0) | 1.17 (0.97, 1.41) | 1.02 (0.84, 1.24) |
| Low BZD-only (stable) | 147 (25.5) | 34 (38.0) | 2.06 (1.74, 2.45) | 2.02 (1.70, 2.40) |
| Moderate BZD-only (gradual decline) | 58 (14.9) | 51 (45.0) | 1.20 (0.92, 1.56) | 1.03 (0.77, 1.36) |
| OPI and BZD use | ||||
| Very-low OPI (rapid decline) / Very-low BZD (late discontinuation) | 73 (13.7) | 57 (36.0) | 1.11 (0.87, 1.40) | 0.99 (0.78, 1.26) |
| Very-low OPI (rapid decline) / Very-low BZD (increasing) | 14 (8.3) | 67 (29.0) | 0.67 (0.40, 1.14) | 0.59 (0.34, 1.02) |
| Very-low OPI (stable) / Low BZD (stable) | 48 (42.9) | 45 (51.5) | 3.48 (2.61, 4.65) | 2.73 (1.98, 3.76) |
| Low OPI (gradual decline) / Low BZD (gradual decline) | 27 (26.1) | 41 (39.0) | 2.11 (1.44, 3.10) | 1.96 (1.32, 2.91) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).




