Submitted:
13 April 2024
Posted:
15 April 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
- -
- The study group that includes all newborns who required resuscitation at birth and were admitted to the NICU section.
- -
- The control group consisted of newborns who did not have the necessary criteria for admission to the NICU, newborns who were cared for in the rooming-in system.
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Bjorland, P.A.; Øymar, K.; Ersdal, H.L.; Rettedal, S.I. Incidence of newborn resuscitative interventions at birth and short-term outcomes: A regional population-based study. BMJ Paediatr Open 2019, 3, e000592. [Google Scholar] [CrossRef]
- Skåre, C.; Kramer-Johansen, J.; Steen, T.; Ødegaard, S.; Niles, D.E.; Nakstad, B.; Solevåg, A.L.; Nadkarni, V.M.; Olasveengen, T.M. Incidence of Newborn Stabilization and Resuscitation Measures and Guideline Compliance during the First Minutes of Life in Norway. Neonatology 2015, 108, 100–107. [Google Scholar] [CrossRef]
- Quinn, C.E.; Sivasubramaniam, P.; Blevins, M.; Al Hajajra, A.; Znait, A.T.; Khuri-Bulos, N.; Faouri, S.; Halasa, N. Risk factors for neonatal intensive care unit admission in Amman, Jordan. East Mediterr Health J. 2016, 22, 163–174. [Google Scholar] [CrossRef] [PubMed]
- Bizzego, A.; Gabrieli, G. Predictors of Contemporary under-5 Child Mortality in Low- and Middle-Income Countries: A Machine Learning Approach. Int J Environ Res Public Health. 2021, 18, 1315. [Google Scholar] [CrossRef]
- Aziz, K.; Chadwick, M.; Baker, M.; Andrews, W. Ante- and intra-partum factors that predict increased need for neonatal resuscitation. Resuscitation 2008, 79, 444–452. [Google Scholar] [CrossRef]
- Chadha, I.A. Neonatal resuscitation: Current issues. Indian J Anaesth. 2010, 54, 428–438. [Google Scholar] [CrossRef] [PubMed]
- Yangthara, B.; Horrasith, S.; Paes, B.; Kitsommart, R. Predictive factors for intensive birth resuscitation in a developing-country: A 5-year, single-center study. J Matern Fetal Neonatal Med. 2020, 33, 570–576. [Google Scholar] [CrossRef] [PubMed]
- Weiner, G.M. Textbook of neonatal resuscitation. 7th Edn. American Academy of Pediatrics; Elk Grove Village, I: 2016.
- Dorobanțu, F.R.; Hodoșan, V.; Tîrb, A.M.; Zaha, D.C.; Galușca, D.; Pop, N.O.; Dorobanțu, C.D. Pattern of Newborn Antibiotic Use in a Tertiary Level Maternity for Five Years. Pharmacophore, 2020, 13, 57–63. [Google Scholar] [CrossRef]
- WHO. Levels and trends in child mortality: Report 2021. https://www.who.int/publications/m/item/levels-and-trends-in-child-mortality-report-2021.
- https://ec.europa.eu/eurostat/web/products-eurostat-news/w/ddn-20230309-1.
- Woodd, S.L.; Montoya, A.; Barreix, M.; Pi, L.; Calvert, C.; Rehman, A.M.; Chou, D.; Campbell, O.M.R. Incidence of maternal peripartum infection: A systematic review and meta-analysis. PLoS Med. 2019, 16, e1002984. [Google Scholar] [CrossRef]
- https://ec.europa.eu/eurostat/statistics-explained/index.php?title=Fertility_statistics.
- https://stacks.cdc.gov/view/cdc/23435.
- Zeitlin, J.; Szamotulska, K.; Drewniak, N.; Mohangoo, A.D.; Chalmers, J.; Sakkeus, L.; Irgens, L.; Gatt, M.; Gissler, M.; Blondel, B. Euro-Peristat Preterm Study Group. Preterm birth time trends in Europe: A study of 19 countries. BJOG. 2013, 120, 1356–1365. [Google Scholar] [CrossRef]
- Smith, L.K.; Hindori-Mohangoo, A.D.; Delnord, M.; Durox, M.; Szamotulska, K.; Macfarlane, A. Quantifying the burden of stillbirths before 28 weeks of completed gestational age in high-income countries: A population-based study of 19 European countries. Lancet 2018, 392, 1639–1646. [Google Scholar] [CrossRef]
- Kappy, B.; Berkowitz, D.; Isbey, S.; Breslin, K.; McKinley, K. Characteristics and patient impact of boarding in the pediatric emergency department, 2018-2022. Am J Emerg Med. 2024, 77, 139–146. [Google Scholar] [CrossRef]
- Yadav, S.; Lee, B.; Kamity, R. Neonatal Respiratory Distress Syndrome. 2023. In StatPearls [Internet]; StatPearls Publishing: Treasure Island, FL, USA, 2024. [Google Scholar]
- McPherson, C.; Wambach, J.A. Prevention and Treatment of Respiratory Distress Syndrome in Preterm Neonates. Neonatal Netw. 2018, 37, 169–177. [Google Scholar] [CrossRef]
- McCrossan, P.M.; Sweet, D.G. Surfactant therapy–past, present and future. Infant 2018, 14, 218–222. [Google Scholar]
- Suard, C.; Flori, A.; Paoli, F.; Loundou, A.; Fouilloux, V.; Sigaudy, S.; Michel, F.; Antomarchi, J.; Moceri, P.; Paquis-Flucklinger, V.; D’Ercole, C.; Bretelle, F. Accuracy of prenatal screening for congenital heart disease in population: A retrospective study in Southern France. PLoS ONE. 2020, 15, e0239476. [Google Scholar] [CrossRef]
- Daalderop, L.A.; Been, J.V.; Steegers, E.A.P.; Bertens, L.C.M. Impact of the EURO-PERISTAT Reports on obstetric management: A difference-in-regression-discontinuity analysis. Eur J Public Health. 2023, 33, 342–348. [Google Scholar] [CrossRef]
- Wu, W.; Shao, X. Incidence and mortality trend of congenital heart disease at the global, regional, and national level, 1990–2017. Medicine 2020, 99, e20593. [Google Scholar] [CrossRef]
- Liu, Y.; Chen, S.; Zühlke, L.; Black, G.C.; Choy, M.K.; Li, N.; Keavney, B.D. Global birth prevalence of congenital heart defects 1970–2017: Updated systematic review and meta-analysis of 260 studies. Int J Epidemiol 2019, 48, 455–463. [Google Scholar] [CrossRef]
- Schlapbach, L.J.; Kissoon, N. Defining Pediatric Sepsis. JAMA Pediatr. 2018, 172, 313–314. [Google Scholar] [CrossRef]
- Menon, K.; Schlapbach, L.J.; Akech, S.; Argent, A.; Biban, P.; Carrol, E.D.; Chiotos, K.; Jobayer Chisti, M.; Evans, I.V.R.; Inwald, D.P.; et al. Pediatric Sepsis Definition Taskforce of the Society of Critical Care Medicine. Criteria for Pediatric Sepsis-A Systematic Review and Meta-Analysis by the Pediatric Sepsis Definition Taskforce. Crit Care Med. 2022, 50, 21–36. [Google Scholar] [CrossRef]
- Carcillo, J.A.; Berg, R.A.; Wessel, D.; Pollack, M.; Meert, K.; Hall, M.; Newth, C.; Lin, J.C.; Doctor, A.; Shanley, T.; et al. Eunice Kennedy Shriver National Institute of Child Health and Human Development Collaborative Pediatric Critical Care Research Network. A Multicenter Network Assessment of Three Inflammation Phenotypes in Pediatric Sepsis-Induced Multiple Organ Failure. Pediatr Crit Care Med. 2019, 20, 1137–1146. [Google Scholar] [CrossRef]
- Shah, B.A.; Padbury, J.F. Neonatal sepsis: An old problem with new insights. Virulence. 2014, 5, 170–178. [Google Scholar] [CrossRef]
- Stanescu, A.L.; Liszewski, M.C.; Lee, E.Y.; Phillips, G.S. Neonatal Gastrointestinal Emergencies: Step-by-Step Approach. Radiol Clin North Am. 2017, 55, 717–739. [Google Scholar] [CrossRef]
- Suciu, L.M.; Puscasiu, L.; Szabo, B.; Cucerea, M.; Ognean, M.L.; Oprea, I.; Bell, E.F. Mortality and morbidity of very preterm infants in Romania: How are we doing? Pediatr. Int. 2014, 56, 200–206. [Google Scholar] [CrossRef]
- Coran, A.G.; Adzick, N.S.; Krummel, T.M.; Laberge, J.M.; Shamberger, R.; Caldamone, A. Pediatric Surgery E-Book: Expert Consult-Online and Print (Vol. 2). Elsevier Health Sciences, 2012.
- Xu, C.; Li, Y.; Zhang, W.; Wang, Q. Analysis of perinatal coagulation function in preeclampsia. Medicine 2021, 100, e26482. [Google Scholar] [CrossRef]
- Kher, P.; Verma, R.P. Hemorrhagic Disease of Newborn. [Updated 2023 Jun 26]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK558994/.
- Murariu, M.G.; Dorobanțu, F.R.; Tărniceriu, D. A Novel Automated Empirical Mode Decomposition (EMD) Based Method and Spectral Feature Extraction for Epilepsy EEG Signals Classification. Electronics. 2023, 12, 1958. [Google Scholar] [CrossRef]
- Araki, S.; Shirahata, A. Vitamin K Deficiency Bleeding in Infancy. Nutrients. 2020, 12, 780. [Google Scholar] [CrossRef]
- Ng, E.; Loewy, A.D. Document de principes: Lignes directrices sur la prophylaxie à la vitamine K chez les nouveau-nés: Une déclaration conjointe de la Société canadienne de pédiatrie et du Collège des médecins de famille du Canada. Can Fam Physician. 2018, 64, e431–e434. [Google Scholar]
- El Hasbaoui, B.; Karboubi, L.; Benjelloun, B.S. Newborn haemorrhagic disorders: About 30 cases. Pan African Medical Journal 2017, 28, 123–123. [Google Scholar] [CrossRef]
- WHO. Global health observatory data repository world health organization. 2015. August 2019. https://apps.who.int/ghodata/.
- Odd, D.; Heep, A.; Luyt, K.; Draycott, T. Hypoxic-ischemic brain injury: Planned delivery before intrapartum events. J Neonatal Perinatal Med. 2017, 10, 347–353. [Google Scholar] [CrossRef]
- Gebregziabher, G.T.; Hadgu, F.B.; Abebe, H.T. Prevalence and Associated Factors of Perinatal Asphyxia in Neonates Admitted to Ayder Comprehensive Specialized Hospital, Northern Ethiopia: A Cross-Sectional Study. Int J Pediatr. 2020, 2020, 4367248. [Google Scholar] [CrossRef] [PubMed]
- Phaloprakarn, C.; Manusirivithaya, S.; Boonyarittipong, P. Risk score comprising maternal and obstetric factors to identify late preterm infants at risk for neonatal intensive care unit admission. J Obstet Gynaecol Res. 2015, 41, 680–688. [Google Scholar] [CrossRef] [PubMed]
- Bouvier, D.; Forest, J.C.; Blanchon, L.; Bujold, E.; Pereira, B.; Bernard, N.; Gallot, D.; Sapin, V.; Giguère, Y. Risk Factors and Outcomes of Preterm Premature Rupture of Membranes in a Cohort of 6968 Pregnant Women Prospectively Recruited. J. Clin. Med. 2019, 8, 1987. [Google Scholar] [CrossRef] [PubMed]
- Ilyes, S.-G.; Chiriac, V.D.; Gluhovschi, A.; Valcovici, M.; Dahma, G.; Mocanu, A.G.; Neamtu, R.; Silaghi, C.; Radu, D.; Bernad, E.; Craina, M. The Influence of Maternal Factors on Neonatal Intensive Care Unit Admission and In-Hospital Mortality in Premature Newborns from Western Romania: A Population-Based Study. Medicina. 2022, 58, 709. [Google Scholar] [CrossRef] [PubMed]
| Parameter | 2012 | 2013 | 2014 | 2015 | 2016 | 2017 | 2018 | 2019 | 2020 | 2021 | Total |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Delivered on term | 4151 | 3922 | 3662 | 3405 | 3414 | 3276 | 3264 | 2913 | 2939 | 3154 | 34100 |
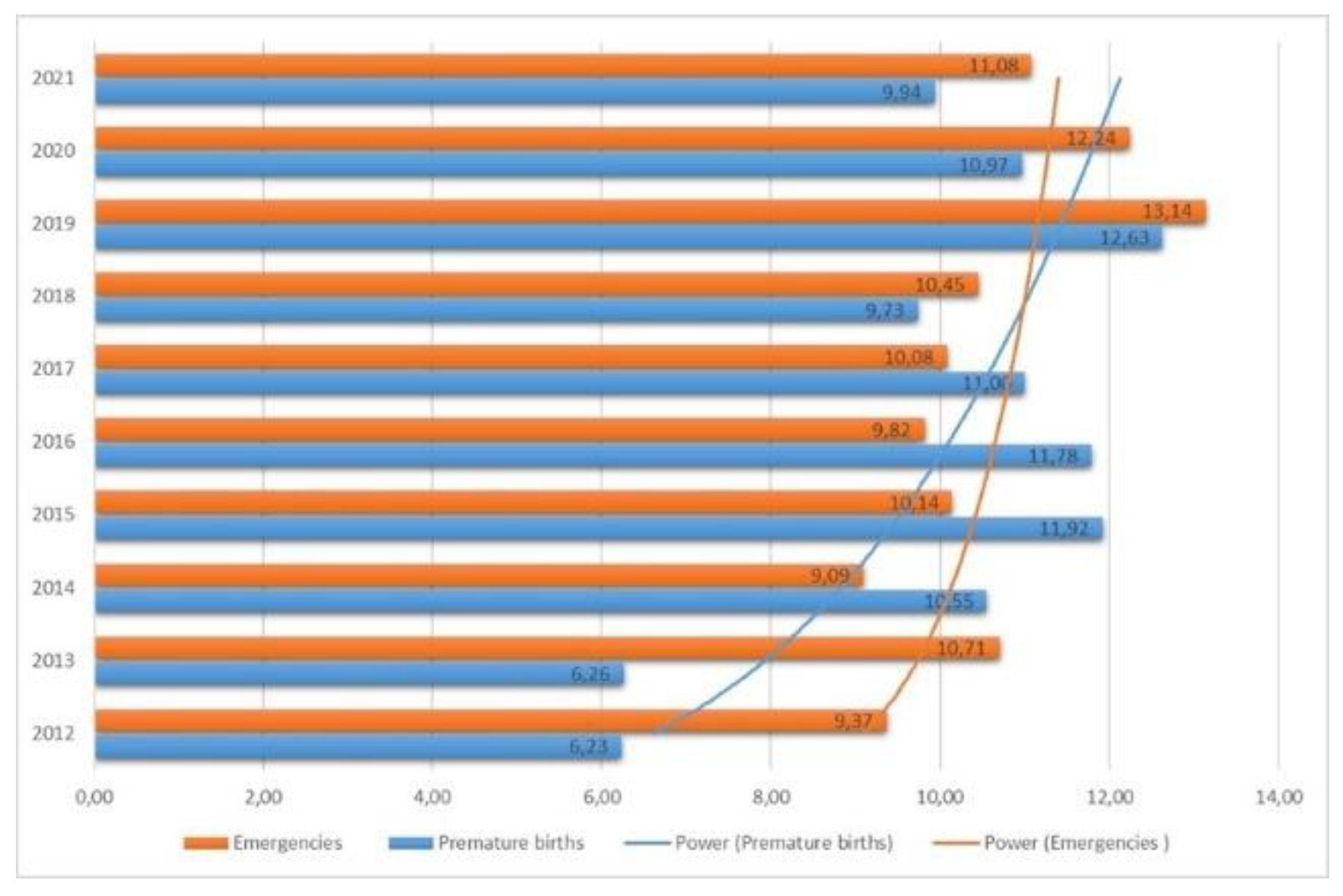
| Premature births | 276 | 262 | 432 | 461 | 456 | 405 | 352 | 421 | 362 | 348 | 3775 |
| Extreme prematurity | 17 | 26 | 22 | 31 | 28 | 30 | 20 | 34 | 30 | 15 | 253 |
| Emergencies | 415 | 448 | 372 | 392 | 380 | 371 | 378 | 438 | 404 | 388 | 3986 |
| Total births | 4427 | 4184 | 4094 | 3866 | 3870 | 3681 | 3616 | 3334 | 3301 | 3502 | 37875 |
| Type of emergency | 2012 | 2013 | 2014 | 2015 | 2016 | 2017 | 2018 | 2019 | 2020 | 2021 | Total |
|---|---|---|---|---|---|---|---|---|---|---|---|
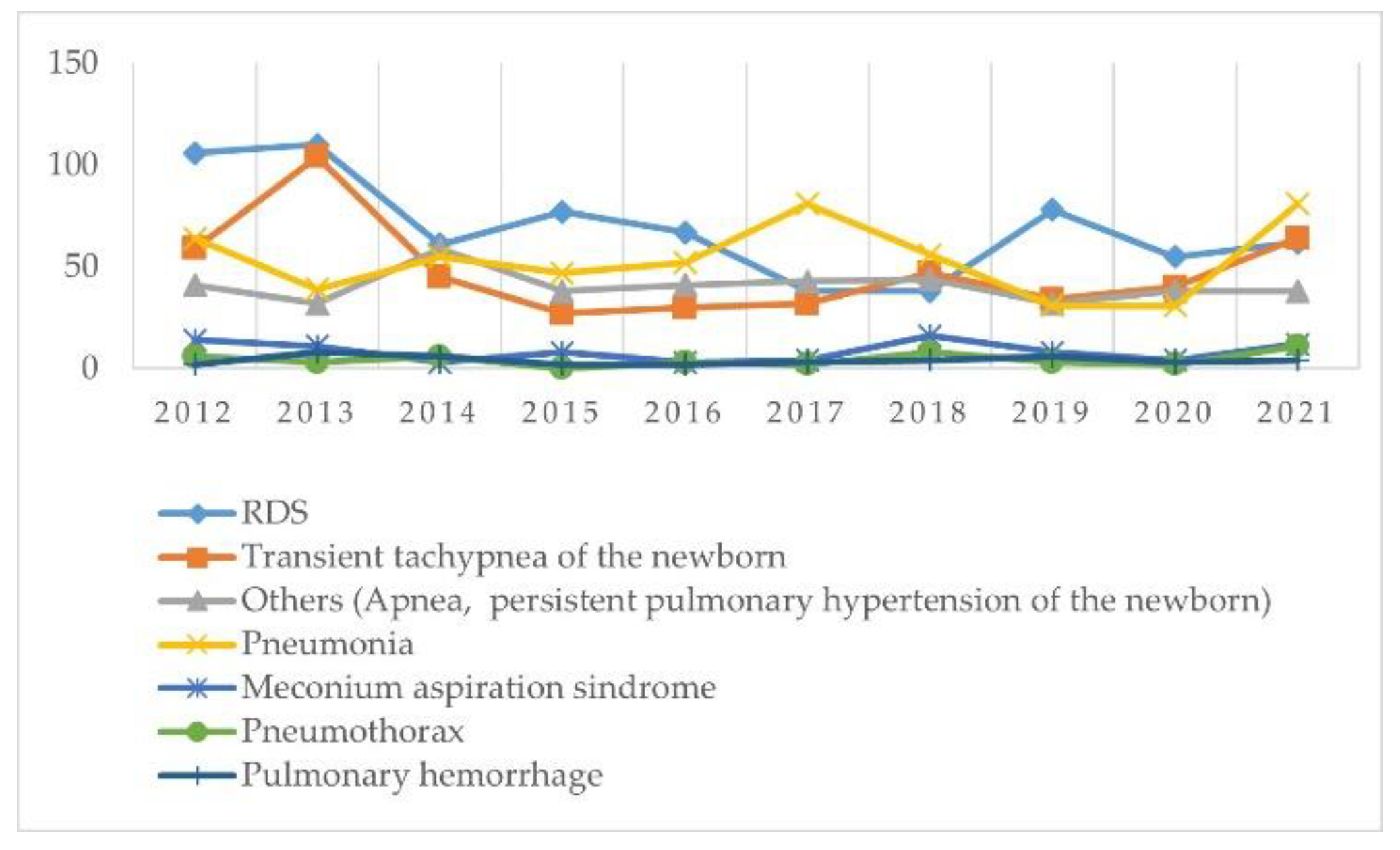
| Respiratory | 292 | 307 | 235 | 199 | 198 | 203 | 213 | 192 | 173 | 272 | 2284 |
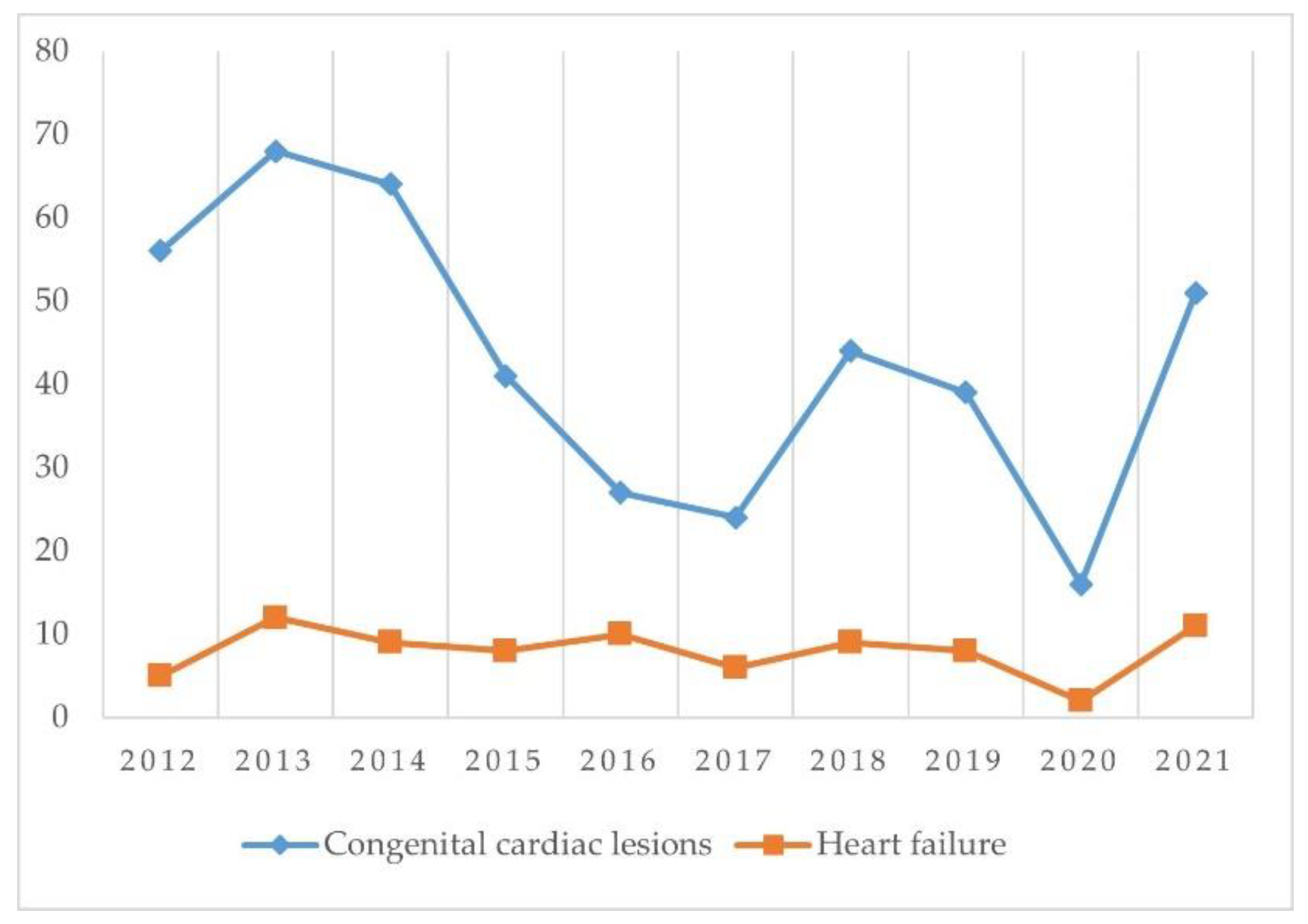
| Cardiovascular | 61 | 80 | 73 | 49 | 37 | 30 | 53 | 47 | 18 | 62 | 510 |
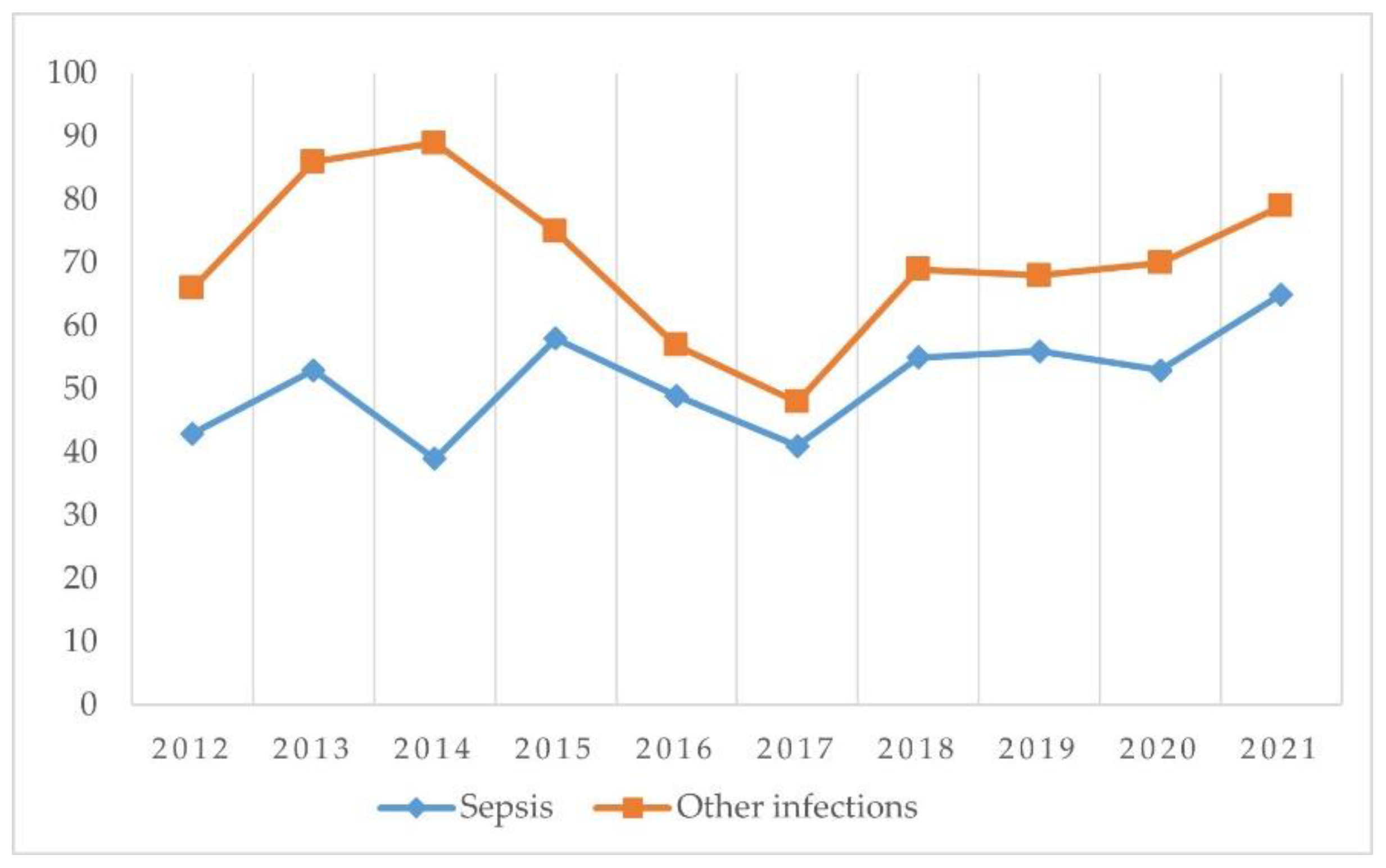
| Sepsis and other infections | 66 | 86 | 89 | 75 | 57 | 48 | 69 | 68 | 70 | 79 | 707 |
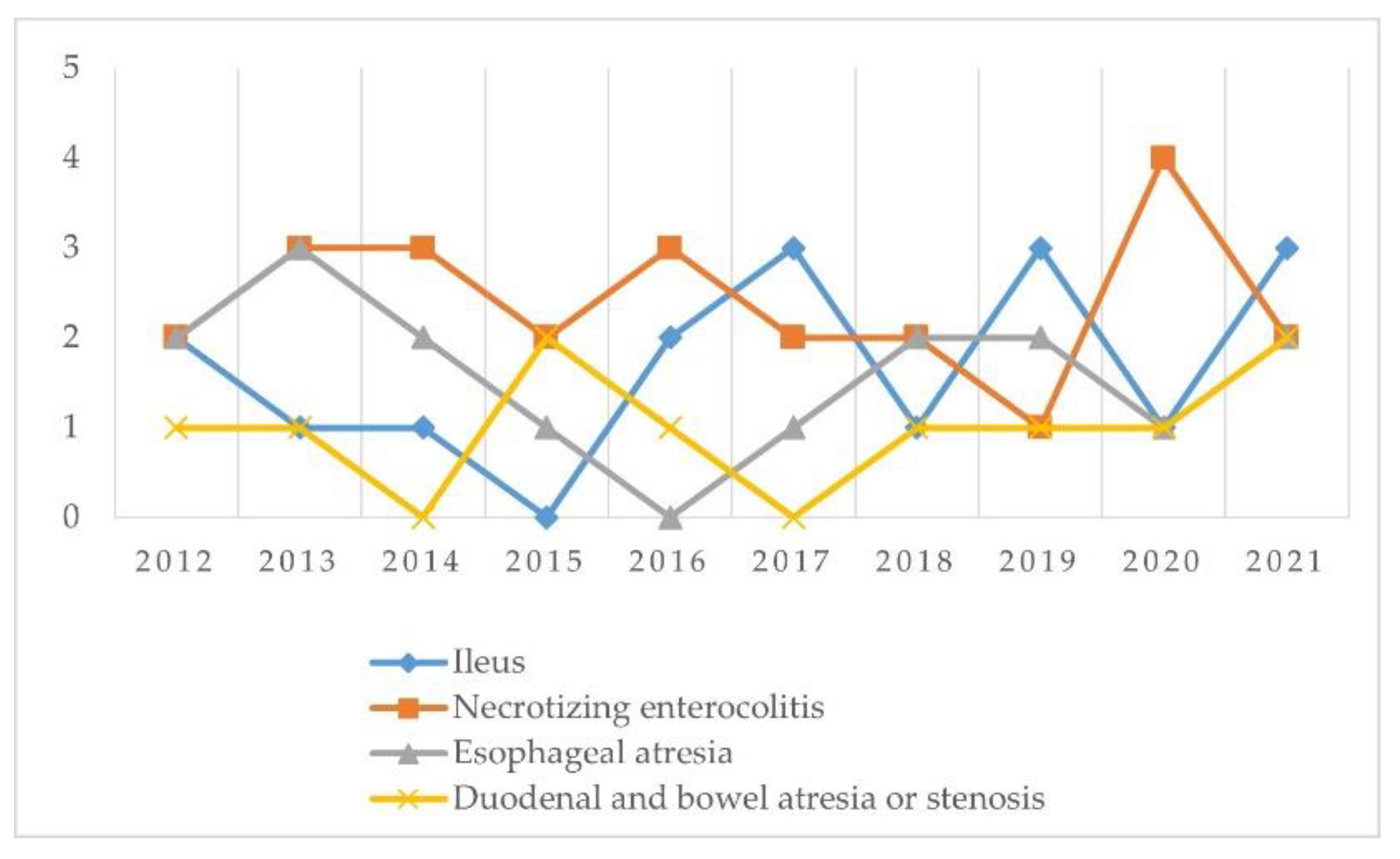
| Gastrointestinal | 7 | 8 | 6 | 5 | 6 | 6 | 6 | 7 | 7 | 9 | 67 |
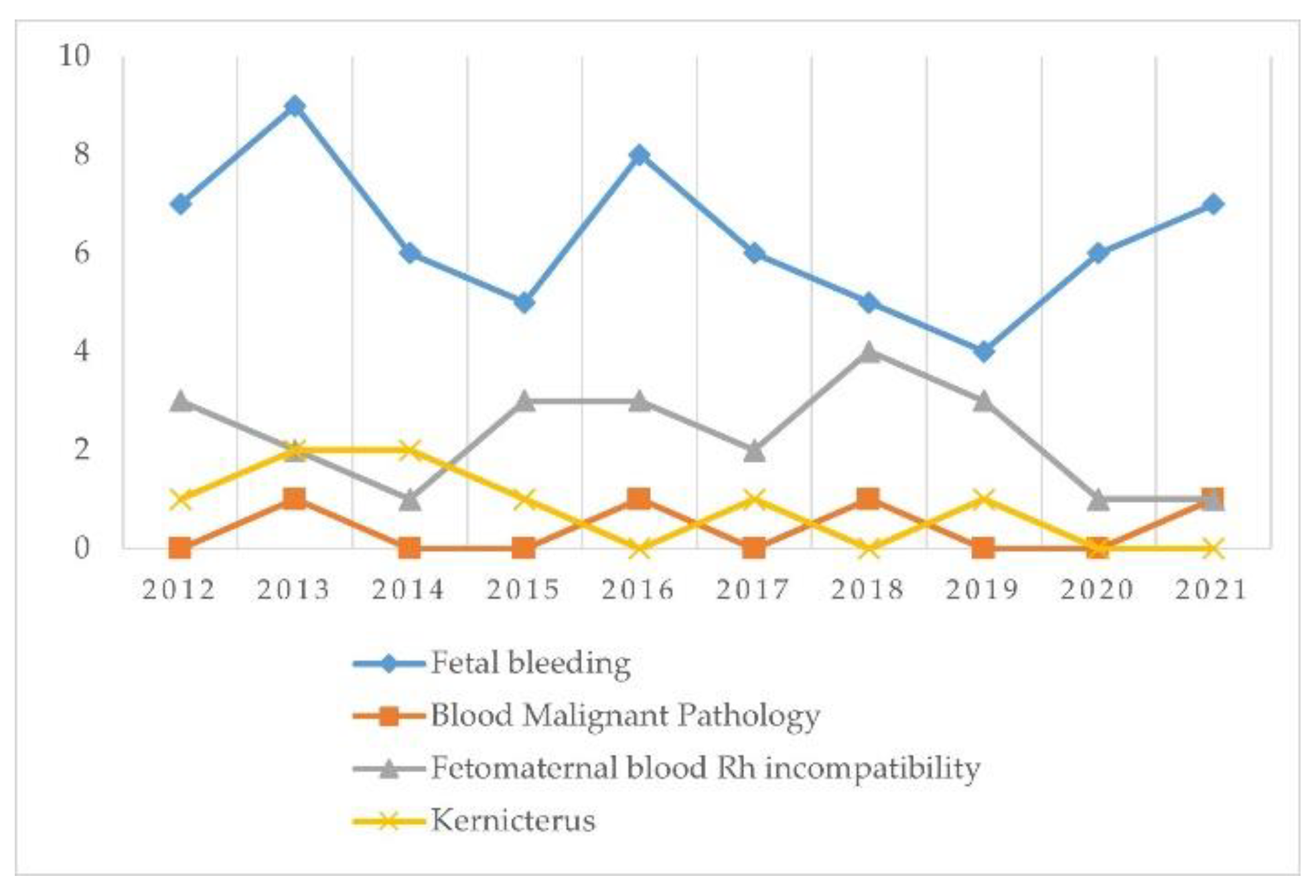
| Haematological | 11 | 14 | 9 | 9 | 12 | 9 | 10 | 8 | 7 | 9 | 98 |
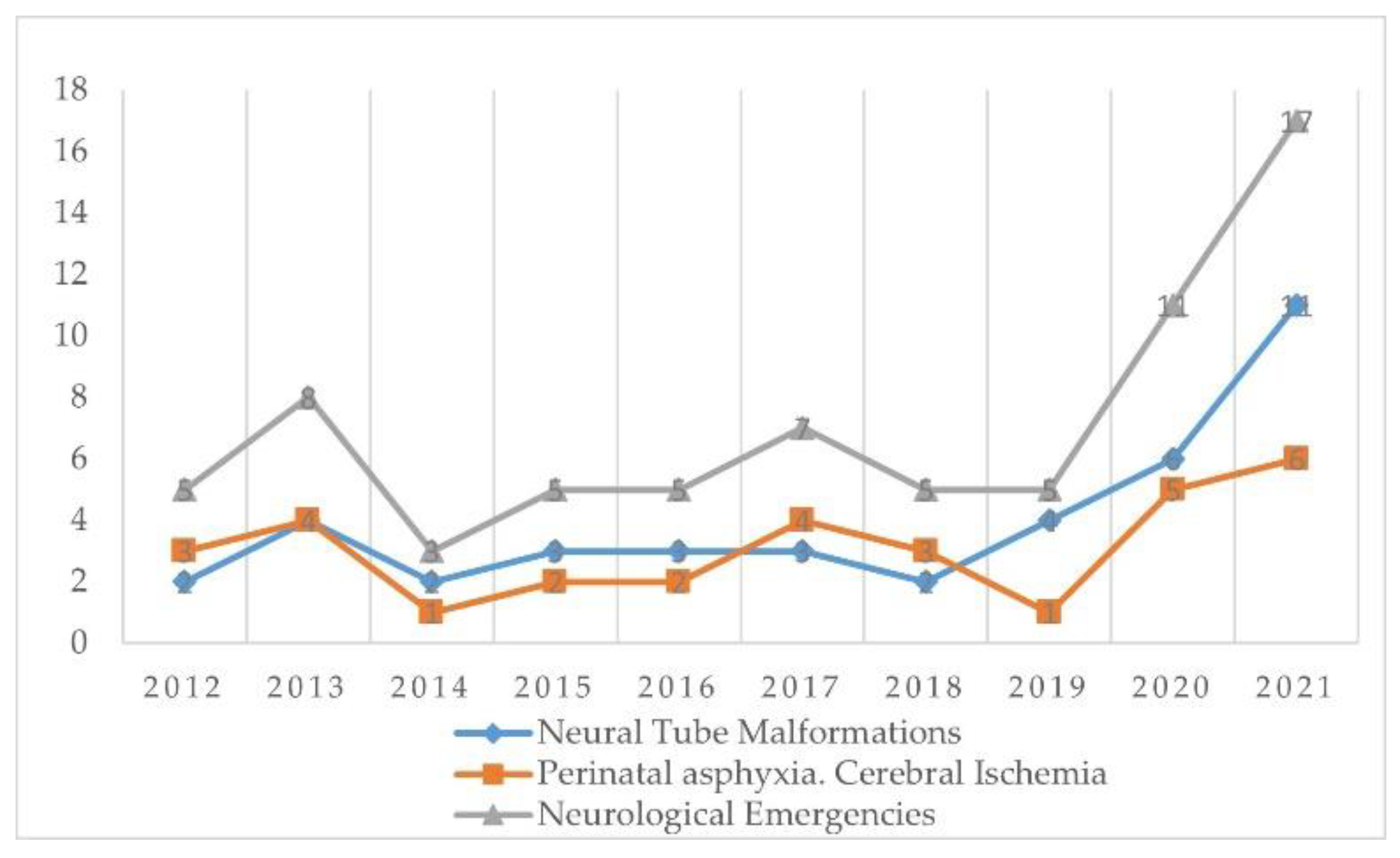
| Neurological | 5 | 8 | 3 | 5 | 5 | 7 | 5 | 5 | 11 | 17 | 71 |
| Extreme prematurity | 17 | 26 | 22 | 31 | 28 | 30 | 20 | 34 | 30 | 15 | 253 |
| Case n (%) |
Control n (%) |
Odds ratio (95% CI) |
p | |
|---|---|---|---|---|
| Mother’s age 18-34 years | 2678 (67.19) | 23567 (62.45) | 0.84 (0.47-1.49) | <0.001 |
| Mother’s age over 35 years | 1308 (32.81) | 14169 (37.54) | 1.19 (0.66-2.12) | |
| Low level of education | 1549 (38.86) | 13817 (36.61) | 2.02 (1.14-3.57) | <0.001 |
| Medium level of education | 2099 (52.66) | 12873 (34.11) | 1.08 (0.61-1.92) | |
| Higher level of education | 398 (9.98) | 11044 (29.26) | 0.27 (0.12-0.59) | |
| Country | 2559 (64.2) | 22591 (59.86) | 1.18 (0.66-2.09) | 0.354 |
| Urban | 1427 (35.8) | 15145 (40.13) | 0.84 (0.47-1.49) | |
| Primiparous | 1521 (38.16) | 11949 (31.66) | 0.34 (0.25-0.44) | |
| Second/more pregnancy | 2465 (61.84) | 25787 (68.33) | 1.09 (0.6-1.97) | <0.001 |
| Female gender | 1977(49.6) | 18273 (48.42) | 2.15 (1.22-3.79) | 0.743 |
| Male gender | 2009 (50.4) | 19463 (51.57) | 0.42 (0.24-0.75) | |
| Weight under 2500 g | 2340 (58.71) | 634 (1.68) | 2.26 (1.21-4.21) | <0.001 |
| Weight over 2500 g | 1646 (41.29) | 37102 (98.31) | 0.44 (0.23-0.82) | |
| Apgar score under 7 | 2144 (53.79) | 793 (2.10) | 2.79 (1.45-2.35) | <0.001 |
| Apgar score over 7 | 1842 (46.21) | 36943 (97.89) | 0.35 (0.18-0.68) | |
| Detachment from the placenta | 264 (6.62) | 27 (0.07) | 3.06 (0.31-3.87) | 0.662 |
| Premature rupture of membranes | 1123 (28.17) | 4 (0.01) | 2.11 (0.92- 4.8) | 0.02 |
| Multiple pregnancy | 211 (5.29) | 196 (0.51) | 1.05 (1-1.17) | 0.06 |
| Meconium amniotic fluid | 164 (4.11) | 14 (0.03) | 1 (0.13-6.24) | 0.70 |
| Macrosomia | 417 (10.46) | 4605 (12.20) | 2.43 (0.61-6.69) | 0.01 |
| Mother’s infectious pathology | 2246 (56.35) | 1158 (3.06) | 1.69 (1.43-1.99) | <0.001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




